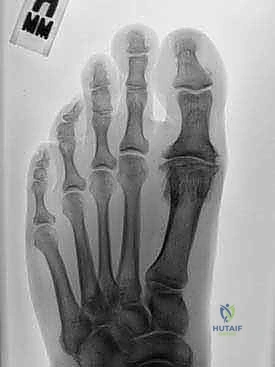
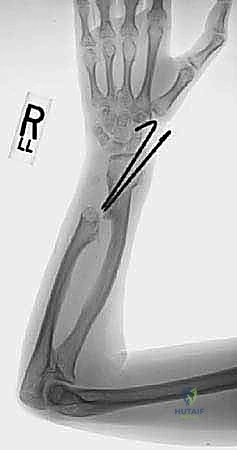
Flexion Intertrochanteric Osteotomy for Severe Slipped Capital Femoral Epiphysis: An Intraoperative Masterclass
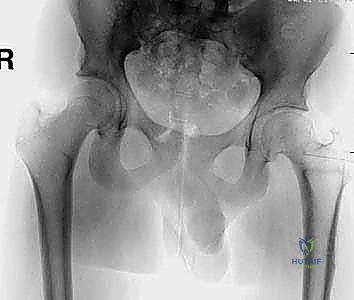
Key Takeaway
This masterclass details the flexion intertrochanteric osteotomy for severe slipped capital femoral epiphysis (SCFE). We cover comprehensive surgical anatomy, meticulous preoperative planning, and a granular, step-by-step intraoperative execution from the surgeon's perspective. Critical pearls, potential pitfalls, and a robust postoperative rehabilitation protocol are extensively discussed, ensuring fellows gain a deep understanding of this complex hip realignment procedure.
Introduction and Epidemiology
Slipped capital femoral epiphysis (SCFE) represents one of the most common adolescent hip disorders, characterized by the displacement of the proximal femoral epiphysis relative to the femoral neck. While the term implies a slippage of the capitis, the biomechanical reality is that the femoral neck and shaft displace anteriorly and externally rotate while the epiphysis remains tethered within the acetabulum by the ligamentum teres. The true etiology of SCFE remains multifactorial and incompletely understood. However, epidemiological data demonstrate a strong predilection for adolescent males, accounting for approximately 80% of cases. Endocrine factors, particularly the interplay between growth hormone and sex hormones during the pubertal growth spurt, significantly influence physeal stability.
During the transition from juvenile to adolescent development, the orientation of the proximal femoral physis becomes increasingly vertical. This anatomic shift dramatically increases shear stress across the hypertrophic zone of the physis. Concurrently, this developmental period is frequently associated with rapid weight gain, leading to the stereotypical obese body habitus observed in the vast majority of SCFE patients. The combination of increased mechanical load and altered physeal geometry creates a biomechanical environment highly susceptible to failure.
Undetected or inadequately treated SCFE invariably alters the natural history of the hip joint, frequently culminating in early-onset osteoarthritis. The classic "pistol grip" deformity—a pathognomonic radiographic finding representing the abnormal contour of the head-neck junction—precipitates severe anterior femoroacetabular impingement (FAI). Murray's seminal longitudinal studies suggested that up to 40% of hips presenting with idiopathic degenerative arthritis exhibit a "tilt deformity" or subtle morphologic abnormalities attributable to subclinical or undetected SCFE. Further corroborating this, Aronson's epidemiological review demonstrated that 15% to 20% of patients with a history of SCFE developed painful, functionally limiting osteoarthritis by the fifth decade of life, and 11% of all patients presenting with end-stage hip osteoarthritis had a pre-existing SCFE.
For severe, chronic, or healed SCFE with residual posterior displacement of the epiphysis, in situ pinning alone fails to address the mechanical impingement. In these complex scenarios, realignment of the proximal femur via a flexion intertrochanteric osteotomy (ITO), often combined with a surgical hip dislocation and femoral head-neck osteoplasty, is indicated to restore the anterior head-neck offset, clear the impingement, and optimize joint kinematics.
Surgical Anatomy and Biomechanics
Pathoanatomy of Slipped Capital Femoral Epiphysis
The primary pathoanatomic consequence of a severe SCFE is the creation of a massive anterior metaphyseal prominence. As the femoral neck displaces anteriorly and superiorly relative to the epiphysis, the anterolateral metaphysis abuts the anterior acetabular rim during hip flexion and internal rotation. This creates a severe cam-type femoroacetabular impingement.
Repeated impingement leads to predictable patterns of intra-articular derangement. The acetabular labrum is subjected to massive shear forces, leading to tearing, intrasubstance degeneration, and eventual detachment. Concurrently, the adjacent acetabular articular cartilage undergoes delamination from the subchondral bone, a phenomenon often referred to as the "carpet delamination" lesion.

Biomechanically, the hip joint experiences a profound loss of internal rotation and flexion. To accommodate the anterior metaphyseal bump, the lower extremity adopts an obligate external rotation during hip flexion. This kinematic compensation allows the prominent metaphysis to bypass the anterior acetabular rim but severely limits the physiologic arc of motion required for activities of daily living.
Vascular Anatomy of the Proximal Femur
A rigorous understanding of the extraosseous and intraosseous vascular supply to the proximal femur is paramount when performing surgical hip dislocation and intertrochanteric osteotomies. The primary blood supply to the femoral head is derived from the medial femoral circumflex artery (MFCA).
The deep branch of the MFCA courses posterior to the obturator externus and anterior to the superior gemellus and obturator internus tendons. It crosses the posterior capsule and perforates the joint capsule distal to the reflected head of the rectus femoris, transitioning into the retinacular vessels. These vessels run along the posterosuperior aspect of the femoral neck within the synovial folds (retinacula of Weitbrecht) to enter the epiphysis.
Surgical approaches, particularly the trochanteric flip osteotomy utilized in surgical hip dislocation, are specifically designed to protect this vascular leash. The intact obturator externus tendon protects the MFCA from excessive tension during dislocation, provided the dislocation is performed with controlled flexion and external rotation.
Indications and Contraindications
The decision to proceed with a flexion intertrochanteric osteotomy requires careful patient selection, balancing the severity of the deformity against the inherent risks of complex proximal femoral reconstruction. Patients typically present with insidious-onset groin or anterior thigh pain, often misdiagnosed initially as a muscle strain. Physical examination reveals an antalgic gait, an externally rotated foot progression angle, and a positive anterior impingement test (pain elicited with combined flexion, adduction, and internal rotation).
Normal physiologic hip flexion required for standard activities of daily living is at least 90 degrees. Patients with chronic, severe SCFE will reliably demonstrate less than 90 degrees of true hip flexion and will exhibit obligate external rotation as the hip is passively flexed.
The primary indication for a flexion ITO is a severe, healed SCFE (typically a Southwick slip angle greater than 50 to 60 degrees) where the resultant extension and external rotation deformity of the femoral neck precludes functional range of motion and causes symptomatic impingement.
| Parameter | Operative Indications (Flexion ITO / SHD) | Non-Operative / Alternative Management |
|---|---|---|
| Slip Severity | Severe (>50-60 degrees), Moderate with severe impingement | Mild (<30 degrees) - Typically managed with in situ pinning |
| Symptomatology | Refractory groin pain, obligate external rotation, severe ROM deficit | Asymptomatic (rare in severe slips), medically unfit for major surgery |
| Joint Space | Preserved joint space (Tönnis Grade 0 or 1) | Advanced Osteoarthritis (Tönnis Grade 2 or 3) - Arthroplasty indicated |
| Physeal Status | Closed or closing physis (chronic/healed slip) | Open physis with acute instability (Subcapital realignment may be preferred) |
| Articular Cartilage | Localized delamination amenable to debridement | Widespread full-thickness chondrolysis (Salvage procedures indicated) |
Contraindications include advanced degenerative joint disease, active joint infection, established avascular necrosis (AVN) of the femoral head, and severe osteopenia that would preclude stable hardware fixation.
Pre Operative Planning and Patient Positioning
Clinical Evaluation and Kinematic Assessment
Preoperative planning begins with a meticulous clinical examination. The degree of obligate external rotation and the absolute limits of flexion and internal rotation must be documented. This clinical assessment dictates the exact degree of flexion and internal rotation required in the osteotomy to restore a functional arc of motion.
Radiographic Analysis and Templating
Standard radiographic evaluation mandates high-quality anteroposterior (AP) views of the pelvis and a frog-leg lateral view of the involved hip. The Southwick slip angle is calculated to quantify the magnitude of the deformity.

While plain radiographs provide baseline metrics, computed tomography (CT) with two-dimensional and three-dimensional surface rendering is the gold standard for preoperative templating in severe SCFE.

CT imaging allows for precise quantification of femoral retroversion, the volume and location of the anterior metaphyseal cam lesion, and the spatial relationship between the epiphysis and the metaphysis.
Templating the osteotomy involves calculating the necessary wedge resection. Because the deformity in a severe SCFE is essentially an extension and external rotation deformity of the femoral neck relative to the shaft, the corrective osteotomy must impart flexion and internal rotation. This is achieved by planning an anteriorly and laterally based closing wedge osteotomy at the intertrochanteric level. The angle of the wedge corresponds directly to the required degrees of correction determined during the clinical and radiographic assessment.
Patient Positioning
The procedure is typically performed with the patient in the lateral decubitus position on a radiolucent operative table. This position facilitates the surgical hip dislocation approach and allows for unhindered fluoroscopic imaging in both the AP and axial planes. Rigid pelvic fixation using a peg board or lateral supports is critical to ensure the pelvis does not roll during the dislocation or the execution of the osteotomy, which would compromise the accuracy of the triplanar correction.
Detailed Surgical Approach and Technique
Surgical Hip Dislocation Approach
The operation commences with a surgical hip dislocation, popularized by Ganz, to allow direct visual access to the femoral head-neck junction and the intra-articular space. A straight lateral incision is made centered over the greater trochanter. The fascia lata is incised in line with the skin incision, and the Gibson interval (between the gluteus maximus and gluteus medius) is developed.

A trochanteric flip osteotomy (digastric osteotomy) is performed. The osteotomy begins at the posterosuperior border of the greater trochanter and exits distally at the vastus ridge, ensuring a maximum thickness of approximately 1.5 cm. This osteotomy preserves the continuity of the gluteus medius and vastus lateralis aponeurosis. The trochanteric fragment is mobilized anteriorly, exposing the superior capsule.
The piriformis tendon is identified and preserved. The interval between the piriformis and the gluteus minimus is developed to expose the superior joint capsule. The capsule is meticulously cleared of overlying soft tissue.

A Z-shaped capsulotomy is performed. The longitudinal limb of the capsulotomy is placed along the anterosuperior axis of the femoral neck. This placement is critical to avoid injury to the main retinacular vessels coursing posterosuperiorly. The hip is then dislocated anteriorly by applying flexion, adduction, and external rotation to the leg. The ligamentum teres is sharply transected.
Femoral Head Neck Osteoplasty
Once dislocated, the joint is thoroughly inspected. The labrum is evaluated for tears or detachments, and the articular cartilage is probed for delamination. Labral repair or debridement is performed as indicated.

Attention is then directed to the proximal femur. The massive anterior metaphyseal prominence is visualized. An aggressive femoral head-neck osteoplasty is performed using curved osteotomes and a high-speed burr. The goal is to resect the cam lesion and recreate a concave anterior head-neck offset. The resection must be carefully contoured to avoid excessive narrowing of the femoral neck, which could precipitate a stress fracture. Dynamic examination of the hip through a simulated range of motion is performed to confirm the clearance of the impingement.
If the osteoplasty successfully restores greater than 90 degrees of impingement-free flexion and adequate internal rotation, the intertrochanteric osteotomy may be aborted. However, in severe slips, osteoplasty alone is frequently insufficient, necessitating the flexion ITO.
Execution of the Flexion Intertrochanteric Osteotomy
The hip is reduced prior to the extra-articular osteotomy. The vastus lateralis is elevated from the lateral femoral shaft to expose the subtrochanteric region.

Guidewires are placed under fluoroscopic guidance to define the osteotomy planes. The seating chisel for a 90-degree or 130-degree blade plate (or the trajectory for a proximal femoral locking plate) is introduced into the femoral neck parallel to the planned axis of correction.
An anteriorly based closing wedge is outlined. The proximal cut is made parallel to the seating chisel, and the distal cut is angled to resect the predetermined wedge (typically 30 to 60 degrees, depending on the preoperative Southwick angle). The osteotomy is completed using an oscillating saw, ensuring the medial cortex is either cleanly cut or maintained as a greenstick hinge depending on the surgeon's preference for stability.

The anterior wedge is removed. The distal femoral shaft is then flexed, abducted (if a valgus correction is also planned), and internally rotated to close the osteotomy site. This maneuver effectively reorients the proximal femoral articular surface anteriorly and superiorly, clearing the posterior displacement of the epiphysis.
The osteotomy is stabilized with the pre-selected implant. Rigid compression across the osteotomy site is achieved using an articulated tension device before final screw fixation. Fluoroscopy confirms anatomic reduction of the osteotomy, appropriate hardware placement, and restoration of the proximal femoral mechanical axis.
The trochanteric flip fragment is then reduced and secured with two or three 4.5 mm cortical screws. The vastus lateralis fascia and the iliotibial band are meticulously closed over drains.
Complications and Management
The surgical management of severe SCFE via surgical hip dislocation and intertrochanteric osteotomy is a technically demanding procedure associated with a recognized complication profile. Meticulous surgical technique and strict adherence to anatomic boundaries are required to minimize morbidity.
| Complication | Incidence / Risk Factors | Prevention and Management Strategies |
|---|---|---|
| Avascular Necrosis (AVN) | 5% - 15% (Higher in acute-on-chronic or unstable slips) | Preserve the MFCA and retinacular vessels during SHD. Avoid excessive tension during dislocation. If AVN occurs, management ranges from core decompression to total hip arthroplasty depending on collapse. |
| Chondrolysis | 2% - 7% (Associated with unrecognized intra-articular hardware penetration) | Rigorous fluoroscopic evaluation during pinning/plating. Avoid excessive intra-articular manipulation. Management includes aggressive physical therapy and NSAIDs; severe cases may require arthrodesis or arthroplasty. |
| Nonunion / Delayed Union | < 5% (Higher with inadequate fixation or early weight-bearing) | Ensure rigid compression across the osteotomy site. Utilize robust fixation constructs (blade plates or locking plates). Treat with revision internal fixation and bone grafting if nonunion is established. |
| Hardware Failure | Rare (< 2%) | Select appropriately sized implants for patient weight and activity level. Strict adherence to postoperative weight-bearing restrictions. |
| Trochanteric Nonunion | 1% - 3% | Ensure minimum 1.5 cm thickness of the trochanteric fragment. Use minimum two 4.5mm screws for fixation. Treat symptomatic nonunions with revision fixation and grafting. |
| Leg Length Discrepancy | Variable (Shortening expected due to wedge resection) | Preoperative counseling is mandatory. The flexion/valgus correction may partially offset the shortening from the wedge resection. Shoe lifts are utilized for discrepancies >1.5 cm. |

Postoperative radiographic surveillance is critical to monitor the progression of bone healing and the maintenance of correction. Any loss of fixation or signs of impending AVN (such as subchondral sclerosis or crescent signs) must be identified early to facilitate appropriate salvage interventions.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol is designed to protect the trochanteric osteotomy and the intertrochanteric osteotomy while preventing intra-articular adhesions and restoring muscle strength.
Phase I: Maximum Protection (Weeks 0-6)
* Weight-Bearing: Strict toe-touch weight-bearing (TTWB) or non-weight-bearing (NWB) using crutches or a walker.
* Range of Motion: Passive and active-assisted range of motion is initiated immediately. Continuous passive motion (CPM) machines may be utilized to prevent intra-articular adhesions, particularly if extensive osteochondroplasty or labral repair was performed. Active abduction is strictly prohibited to protect the trochanteric flip osteotomy.
* Strengthening: Isometric quadriceps, hamstring, and gluteal sets.
Phase II: Controlled Mobilization (Weeks 6-12)
* Weight-Bearing: Progression to partial weight-bearing (PWB) and eventually full weight-bearing (FWB) is permitted only after radiographic evidence of early bridging callus at both the intertrochanteric and trochanteric osteotomy sites.
* Range of Motion: Progression to full active range of motion. Gentle stretching is introduced to address capsular contractures.
* Strengthening: Isotonic strengthening of the hip flexors, extensors, and adductors. Active abduction strengthening is initiated cautiously once trochanteric union is confirmed. Closed kinetic chain exercises (e.g., mini-squats, leg presses) are introduced as weight-bearing allows.
Phase III: Advanced Strengthening and Return to Activity (Months 3-6+)
* Weight-Bearing: Full, unassisted weight-bearing.
* Strengthening: Advanced core stabilization, proprioceptive training, and plyometrics. Focus on restoring normal gait mechanics and eliminating Trendelenburg gait.
* Return to Sport: Clearance for high-impact activities or sports is typically delayed until 6 to 9 months postoperatively, contingent upon complete radiographic union, symmetric muscle strength, and a pain-free, functional arc of motion.
Summary of Key Literature and Guidelines
The evolution of surgical techniques for severe SCFE reflects a growing understanding of hip kinematics and vascular anatomy. Historically, in situ pinning was the gold standard for all SCFE, regardless of severity. However, long-term outcome studies, notably by Aronson and Murray, highlighted the unacceptably high rates of early-onset osteoarthritis in patients with severe residual deformities left in situ.
The concept of the compensatory intertrochanteric osteotomy was pioneered by Imhauser in 1956 and later refined by Southwick in 1967. The Imhauser osteotomy specifically utilized a flexion, internal rotation, and valgus correction at the intertrochanteric level to reorient the articular cartilage and clear the anterior impingement. While these extra-articular osteotomies significantly improved the arc of motion, they did not address the intra-articular pathology or the physical cam lesion.
The paradigm shifted significantly with the introduction of the surgical hip dislocation by Ganz and Leunig in 2001. This approach revolutionized the treatment of severe SCFE by allowing safe, direct visualization of the femoral head-neck junction without compromising the critical medial femoral circumflex artery.
Current academic consensus and clinical guidelines advocate for a tailored approach. For mild to moderate slips without severe impingement, in situ pinning remains appropriate. However, for severe slips (>50-60 degrees) with profound kinematic restrictions, the combination of a surgical hip dislocation, femoral head-neck osteoplasty, and a flexion intertrochanteric osteotomy represents the most comprehensive strategy to restore joint mechanics, alleviate impingement, and theoretically delay the onset of degenerative joint disease. The choice between an extra-articular compensatory osteotomy (Flexion ITO) and an intra-articular anatomic reduction (Modified Dunn procedure) remains a subject of ongoing academic debate,
Clinical & Radiographic Imaging









You Might Also Like