Pilon Fracture Case: Critical Steps for High-Energy Injury
Key Takeaway
Learn more about Pilon Fracture Case: Critical Steps for High-Energy Injury and how to manage it. A case pilon fracture involves a comminuted and displaced intra-articular injury of the distal tibia. Typically resulting from a high-energy axial load, like a fall or MVA, it often presents with articular and metaphyseal comminution. Initial management prioritizes soft tissue assessment, neurovascular integrity, and closed reduction, followed by a CT scan for surgical planning.
Patient Presentation and History
Mechanism of Injury and Energy Transfer
The patient is a 42-year-old male construction worker who presents to the Level I Trauma Center following a high-energy fall from a height of approximately 15 feet. The patient reports landing primarily on his right lower extremity with the ankle in a neutral to slightly dorsiflexed position. This specific mechanism of injury represents a classic axial loading force vector, which drives the talar dome directly into the tibial plafond, resulting in a severe pilon fracture. The magnitude of the kinetic energy transferred through the osseous and soft tissue structures is immense, leading to profound comminution of the distal tibial articular surface and extensive damage to the surrounding soft tissue envelope. The energy dissipation in such injuries typically results in a combination of shear and impaction forces, creating a complex fracture morphology characterized by metaphyseal impaction, central die-punch fragments, and significant displacement of the major articular columns.
Patient Demographics and Comorbidities
The demographic profile and medical history of the patient are critical determinants in the surgical decision-making process and overall prognosis. The patient is a daily tobacco user, consuming approximately one pack per day for the past twenty years. Nicotine acts as a potent vasoconstrictor, significantly diminishing microvascular perfusion to the distal extremities. Furthermore, carbon monoxide competitively binds to hemoglobin, reducing oxygen delivery to the healing tissues. This combination drastically elevates the risk of postoperative wound complications, flap necrosis, delayed union, and nonunion. Additional medical history reveals poorly controlled type 2 diabetes mellitus with a recent Hemoglobin A1c of 8.4 percent. Hyperglycemia impairs leukocyte function, specifically neutrophil chemotaxis and phagocytosis, thereby exponentially increasing the susceptibility to deep surgical site infections. The patient has a Body Mass Index of 32, adding further mechanical stress to the planned fixation construct and complicating the soft tissue management. No history of peripheral vascular disease or neuropathy is reported, but the combination of smoking and diabetes necessitates a meticulous evaluation of the vascular status and dictates a highly conservative approach to soft tissue handling.
Clinical Examination Findings
Soft Tissue Envelope Assessment
Upon initial evaluation in the trauma bay, the right lower extremity exhibits gross deformity, profound edema, and ecchymosis extending from the proximal third of the leg down to the midfoot. The soft tissue envelope, which is the primary limiting factor in the definitive management of pilon fractures, demonstrates classic signs of severe trauma. The skin is tense and tight, with a loss of normal skin wrinkling. Within the first six hours of injury, the patient developed extensive fracture blisters over the anterior and medial aspects of the distal tibia. These blisters are a manifestation of dermo-epidermal junction separation secondary to profound interstitial edema. Both clear fluid-filled blisters (indicating cleavage within the epidermis) and hemorrhagic blisters (indicating a deeper cleavage plane involving the dermal vascular plexus) are present. The presence of hemorrhagic blisters signifies a more severe soft tissue insult and strictly precludes any immediate surgical incisions through these zones. The injury is classified as a Tscherne Grade III closed soft tissue injury, characterized by severe skin contusion, extensive subcutaneous degloving, and impending compartment syndrome.
Neurological and Vascular Evaluation
A comprehensive neurovascular examination is paramount and must be documented meticulously prior to any intervention. Vascular assessment reveals palpable but bounding dorsalis pedis and posterior tibial pulses. Capillary refill in the digits is brisk, occurring in less than two seconds. Despite the palpable pulses, the high-energy nature of the injury warrants a low threshold for obtaining Ankle-Brachial Indices or formal angiography if any asymmetry or deterioration is noted, as intimal tears or arterial vasospasm can occur. Neurological examination demonstrates intact motor function of the Extensor Hallucis Longus, Tibialis Anterior, Peroneus Longus and Brevis, and the gastrocnemius-soleus complex, though testing is limited by pain. Sensory evaluation reveals intact light touch and pinprick sensation across all five major dermatomal distributions of the foot. Specifically, the deep peroneal nerve (first web space), superficial peroneal nerve (dorsum of foot), tibial nerve (plantar aspect), sural nerve (lateral border), and saphenous nerve (medial border) are all functionally intact. The integrity of the superficial peroneal nerve is particularly important to document, as it is frequently stretched during the initial deformity or at risk during the anterolateral surgical approach.
Compartment Syndrome Screening
Given the high-energy axial load and the resultant massive soft tissue swelling, the patient is at an exceptionally high risk for developing acute compartment syndrome of the leg. The clinical examination focuses on the classic "Pain out of proportion" and "Pain with passive stretch" of the involved compartments. Passive plantarflexion of the toes elicits severe pain in the anterior compartment, while passive dorsiflexion causes significant discomfort in the deep posterior compartment. However, distinguishing between pain secondary to the highly comminuted fracture and true ischemic pain from compartment syndrome is clinically challenging. The compartments are palpably tense, described as "wood-like." Due to the equivocal clinical findings in an obtunded or highly agonized patient, intracompartmental pressure monitoring is indicated. Using a side-port needle and a continuous pressure monitor, the anterior compartment pressure measures 42 mmHg, lateral is 38 mmHg, superficial posterior is 35 mmHg, and deep posterior is 45 mmHg. The patient's diastolic blood pressure is 85 mmHg. The delta pressure (Diastolic BP minus Compartment Pressure) for the deep posterior compartment is exactly 40 mmHg, and the anterior compartment is 43 mmHg. While these delta pressures hover near the generally accepted threshold of 30 mmHg for fasciotomy, the dynamic nature of the swelling necessitates continuous serial examinations. A decision is made to proceed with immediate spanning external fixation to restore length and alignment, which often significantly decreases intracompartmental pressures by reducing the volumetric mismatch caused by the shortened, displaced fracture.
Imaging and Diagnostics
Standard Radiographic Evaluation
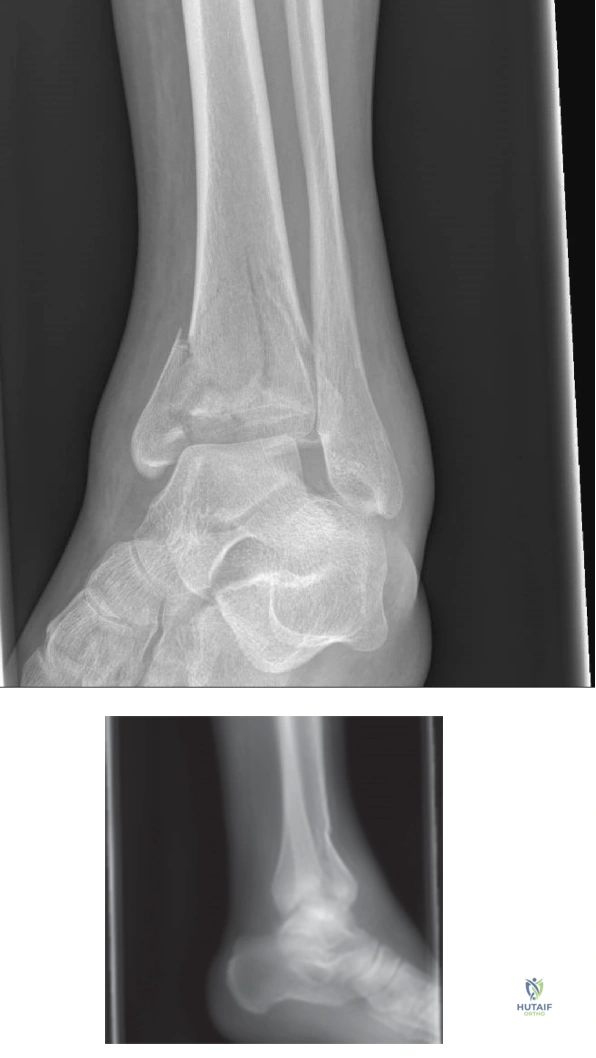
The initial radiographic series includes orthogonal views of the tibia and fibula, as well as dedicated Anteroposterior, Lateral, and Mortise views of the ankle joint. The radiographs reveal a highly comminuted, complete articular fracture of the distal tibia. The fracture pattern demonstrates significant metaphyseal comminution with a varus collapse of the distal articular block. The fibula is fractured at the level of the syndesmosis, exhibiting a short oblique pattern consistent with a supination-adduction or high-energy axial loading mechanism. The talus is proximally migrated and driven into the central portion of the tibial plafond, creating a massive central die-punch fragment. The medial malleolus is fractured at its base with vertical extension, and there is gross displacement of the anterolateral (Chaput) fragment. The disruption of the syndesmotic ligaments is evident by the widening of the tibiofibular clear space and the loss of the normal tibiofibular overlap. These standard radiographs provide a macroscopic overview of the injury, confirming the diagnosis of a severe pilon fracture and dictating the immediate need for damage control orthopedics.
Advanced Cross Sectional Imaging
Following the application of a spanning external fixator, a high-resolution Computed Tomography scan with fine axial cuts (1.0 mm or less) and multiplanar reconstructions (coronal and sagittal) is mandatory. The CT scan is the gold standard for defining the complex articular topography and is indispensable for preoperative planning.

The axial slices at the level of the joint line reveal the classic three-fragment pattern originally described by Topliss et al., but with further comminution. The major articular fragments identified include the medial malleolar fragment, the anterolateral (Chaput) fragment, and the posterolateral (Volkmann) fragment. Additionally, the CT scan clearly delineates a large, central die-punch fragment that is impacted 15 millimeters proximally into the metaphyseal void. The sagittal reconstructions are particularly useful for assessing the size of the anterior and posterior articular fragments and determining the degree of anterior or posterior subluxation of the talus. The coronal reconstructions provide excellent visualization of the medial malleolar extension and the central impaction. The CT scan also allows for the assessment of the fibular fracture morphology and its relationship to the syndesmotic incisura. Furthermore, the 3D reconstructions provide a spatial understanding of the fracture fragments, allowing the surgeon to conceptualize the injury as an exploded puzzle that must be meticulously reassembled.
Preoperative Templating and Three Dimensional Planning
Based on the advanced imaging, formal preoperative templating is performed. This involves digitally tracing the fracture fragments and simulating the reduction sequence. The templating process helps in selecting the appropriate surgical approaches, determining the sequence of fragment reduction, and choosing the optimal implant sizes and configurations. For this specific case, the templating indicates the need for a dual incision approach to address both the medial and lateral columns of the distal tibia. The planning also highlights the massive metaphyseal void that will remain after the articular surface is elevated, necessitating the procurement of autogenous bone graft or the use of an osteoconductive bone graft substitute. The precise location of the external fixator pins is also mapped out to ensure they will not interfere with the planned definitive incisions or plate placement.
Differential Diagnosis
The presentation of a high-energy distal tibia fracture necessitates a careful differentiation from other complex ankle and hindfoot injuries. While the radiographic appearance of a pilon fracture is often unmistakable, understanding the nuances between similar pathologies is critical for appropriate surgical planning and patient counseling.
Comparative Pathologies
| Diagnostic Entity | Mechanism of Injury | Key Clinical Features | Radiographic Hallmarks | Management Strategy |
|---|---|---|---|---|
| Tibial Plafond (Pilon) Fracture | High-energy axial load (fall from height, MVC). Talar impaction into tibia. | Severe soft tissue compromise, rapid swelling, fracture blisters. High risk of compartment syndrome. | Complete articular involvement, metaphyseal comminution, central die-punch fragments, proximal talar migration. | Staged protocol: Span, Scan, and Plan. Definitive ORIF delayed 10-21 days until soft tissues recover. |
| Trimalleolar Ankle Fracture | Low to moderate energy rotational forces (supination-external rotation, pronation-abduction). | Moderate swelling, visible deformity usually related to talar subluxation. Less severe soft tissue envelope damage. | Fractures of medial, lateral, and posterior malleoli. Articular involvement is peripheral, lacking central impaction. | Often amenable to early definitive ORIF if soft tissues permit. Standard plate and screw fixation. |
| Distal Tibial Shaft Fracture with Intra-articular Extension | Torsional or direct bending forces to the tibial diaphysis. | Deformity primarily in the supramalleolar region. Soft tissue injury depends on open vs closed status. | Primary fracture line in the diaphysis/metaphysis with a non-displaced or minimally displaced split extending into the joint. | Intramedullary nailing or MIPO. The articular split is often stabilized percutaneously prior to diaphyseal fixation. |
| Talar Body/Neck Fracture | Extreme dorsiflexion with axial load (classic "aviator's astragalus"). | Deep ankle pain, inability to bear weight. Swelling localized to the hindfoot and anterior ankle. | Disruption of talar trabeculae, subluxation/dislocation of the subtalar or tibiotalar joints. Hawkins sign on follow-up. | Emergent reduction if dislocated. ORIF with dual approaches. High risk of avascular necrosis (AVN). |
Surgical Decision Making and Classification
Fracture Classification Systems
Accurate classification of the fracture is essential for standardizing communication, guiding treatment algorithms, and predicting clinical outcomes. The injury is evaluated using the two most widely recognized systems: the Rüedi-Allgöwer classification and the AO/OTA alphanumeric system.
Under the Rüedi-Allgöwer system, this injury is classified as a Type III fracture. This indicates a highly comminuted articular surface with significant metaphyseal impaction and displacement of the major weight-bearing columns. Type III injuries are historically associated with the highest rates of complications, including post-traumatic osteoarthritis, deep infection, and nonunion.
Utilizing the more comprehensive AO/OTA classification, the fracture is designated as a 43-C3. The "43" denotes the distal tibia segment. The "C" indicates a complete articular fracture, meaning the articular surface is completely separated from the diaphysis. The "3" specifies that both the articular surface and the metaphyseal region are multifragmentary. This classification underscores the extreme complexity of the injury, highlighting the lack of any intact cortical bridge connecting the joint surface to the tibial shaft, which fundamentally dictates the requirement for rigid, bridging fixation constructs.
Indications for Staged Management
The paramount principle in the management of high-energy pilon fractures is the absolute respect for the soft tissue envelope. Historically, early attempts at immediate definitive Open Reduction and Internal Fixation (ORIF) through swollen, compromised tissues led to catastrophic complication rates, including wound dehiscence, deep osteomyelitis, and subsequent amputations, with historical infection rates approaching 30 to 50 percent.
Consequently, the standard of care has evolved to a staged protocol, universally referred to as "Span, Scan, and Plan." The rationale for this approach is multifactorial. First, the immediate application of a spanning external fixator restores limb length, corrects angular deformity, and provides skeletal stability. This reduction in volumetric mismatch significantly decreases interstitial pressure, mitigates the risk of compartment syndrome, and halts ongoing trauma to the soft tissues from mobile, sharp bone fragments. Second, it allows the soft tissue envelope to heal and the profound edema to resolve over a period of 10 to 21 days. The definitive indicator of soft tissue readiness is the appearance of the "wrinkle sign"—the return of normal skin creases upon dorsiflexion of the ankle, indicating that the interstitial edema has sufficiently subsided to allow for tension-free wound closure. Third, the temporizing period provides the necessary time to obtain high-resolution CT imaging, perform detailed 3D preoperative templating, and optimize the patient's medical comorbidities, specifically addressing glycemic control and implementing smoking cessation protocols.
Surgical Technique and Intervention
Stage One Damage Control Orthopedics
The initial surgical intervention is performed emergently to stabilize the skeletal structures and protect the soft tissues. The patient is brought to the operating room and positioned supine on a radiolucent Jackson table. Under general anesthesia, a thorough debridement of any superficial abrasions is performed. The application of a delta-configuration spanning external fixator is initiated.
Two 5.0 mm half-pins are placed in the anterior tibial diaphysis, strictly outside the anticipated zone of definitive fixation and well proximal to the fracture hematoma. These pins are placed via a minimally invasive technique, utilizing a drill sleeve to protect the anterior tibial neurovascular bundle and the extensor tendons. A centrally threaded transfixion pin is then placed through the calcaneal tuberosity, entering from medial to lateral to avoid the neurovascular bundle at the medial malleolus. The medial entry point must be meticulously chosen, typically two fingerbreadths inferior and two fingerbreadths posterior to the medial malleolus, to avoid the posterior tibial artery and the tibial nerve.
Once the pins are secured, longitudinal traction is applied through the calcaneal pin to restore tibial length and disimpact the talus from the tibial plafond. The frame is constructed using carbon fiber rods and multi-pin clamps. The ankle is held in a neutral position to prevent equinus contracture, and the frame is rigidly tightened.
The management of the fibula during this primary stage remains a topic of ongoing debate. While early fibular plating can restore the lateral column and assist in indirect reduction of the tibial plafond through the syndesmotic attachments, it requires an incision through potentially compromised lateral skin. In this specific case, due to the severe soft tissue contusion laterally, a decision is made to defer fibular fixation to the second stage to minimize the risk of wound complications.
Stage Two Definitive Reconstruction
Fourteen days post-injury, the patient's soft tissue envelope demonstrates significant improvement. The massive edema has resolved, fracture blisters have re-epithelialized, and a positive wrinkle sign is clearly present. The patient is medically optimized, and definitive reconstruction is scheduled.
The patient is positioned supine on a radiolucent flat table with a bump placed under the ipsilateral hip to internally rotate the leg, bringing the lateral malleolus forward. A thigh tourniquet is applied but not inflated, reserving its use for critical portions of the procedure to minimize ischemic time to the already traumatized soft tissues. The external fixator is prepped into the surgical field to maintain length and alignment during the initial surgical exposure.
Surgical Approaches and Internervous Planes
Based on the preoperative CT templating, a dual incision strategy is employed to address the complex articular comminution. The primary approach is an anterolateral incision, which provides excellent exposure of the Chaput fragment, the central die-punch fragment, and the lateral aspect of the tibial plafond.
The anterolateral incision is centered over the distal tibia, starting approximately 7 centimeters proximal to the ankle joint and extending distally toward the base of the fourth metatarsal. The superficial dissection requires meticulous identification and protection of the superficial peroneal nerve, which frequently crosses the operative field from medial to lateral in the distal third of the leg. The deep dissection utilizes the internervous plane between the extensor digitorum longus (innervated by the deep peroneal nerve) and the peroneus tertius. The extensor retinaculum is incised, and the anterior neurovascular bundle (deep peroneal nerve and anterior tibial artery) is carefully mobilized and retracted medially along with the extensor hallucis longus and tibialis anterior tendons.
A second, supplemental posteromedial approach is planned to address the posterior malleolar extension and the medial column. It is an absolute biomechanical and biological imperative that a minimum skin bridge of 7 centimeters is maintained between the two incisions to preserve the delicate angiosomal blood supply and prevent catastrophic skin necrosis. The posteromedial incision is placed midway between the posterior border of the medial malleolus and the Achilles tendon. The saphenous nerve and vein are protected anteriorly. The deep dissection proceeds between the posterior tibial tendon and the flexor digitorum longus, allowing access to the posterior aspect of the medial malleolus and the Volkmann fragment.
Articular Reduction Strategies
The fundamental philosophy of pilon fracture reconstruction follows a specific, sequential algorithm: reconstruction of the fibula (if not already done), reconstruction of the articular surface (from peripheral to central), grafting of the metaphyseal void, and finally, rigid connection of the articular block to the tibial diaphysis.
The procedure begins with the open reduction and internal fixation of the fibula using a standard lateral approach, ensuring the incision is carefully planned relative to the anterolateral tibial incision. A one-third tubular plate or a specialized distal fibular locking plate is utilized to restore the exact length, alignment, and rotation of the lateral column. This step is critical, as the fibula acts as a template for the tibial reduction through the intact anterior and posterior inferior tibiofibular ligaments.
Attention is then directed to the anterolateral tibial approach. The joint capsule is opened, and the fracture hematoma is thoroughly irrigated and debrided. A femoral distractor or a lamina spreader is often utilized to open the joint space and visualize the articular surface. The reduction proceeds from the periphery to the center. The anterolateral (Chaput) fragment is mobilized and reduced to the reconstructed fibula. The posterolateral (Volkmann) fragment is then reduced, often requiring manipulation through the fracture site or via the posteromedial approach. Once the peripheral rim is re-established, the central die-punch fragments are elevated. These fragments are devoid of soft tissue attachments and must be handled with extreme care to preserve their precarious blood supply. They are elevated using a periosteal elevator or a bone tamp until they are flush with the talar dome. The articular reduction is provisionally stabilized with multiple 1.6 mm
