Proximal Tibial Diaphyseal Fracture: High-Energy Trauma Case Study, Clinical & Imaging Diagnostics
Key Takeaway
Diagnosis of high-energy proximal tibial diaphyseal fractures involves a detailed patient history, thorough clinical examination assessing deformity, swelling, and neurovascular status. Initial plain radiographs confirm the fracture, while a CT scan precisely delineates comminution, angulation, and rules out intra-articular extension. This comprehensive approach is crucial for accurate classification and surgical planning.
Patient Presentation and History
The management of high-energy proximal tibial diaphyseal fractures presents a complex biomechanical and physiological challenge for the orthopedic trauma surgeon. This case involves a 38-year-old male who presented to the Level I trauma center following a high-velocity motorcycle collision. The patient, acting as the driver, was ejected over the handlebars after striking a stationary object at an estimated speed of 45 miles per hour. This mechanism of injury involves massive kinetic energy transfer, typically resulting in complex fracture patterns, significant soft tissue envelope compromise, and a high risk for concomitant polytrauma.
Initial assessment by emergency medical services adhered to standard Advanced Trauma Life Support protocols. The patient was immobilized via cervical collar and rigid backboard. Paramedics noted an obvious clinical deformity of the right lower leg accompanied by severe localized pain and an inability to bear weight. Notably, there were no gross open wounds, hemorrhage, or active external bleeding identified at the scene. Intravenous access was established, and the patient received crystalloid fluid resuscitation and opioid analgesia during transport. Upon arrival at the trauma bay, the patient was hemodynamically stable, maintaining a blood pressure of 130/80 mmHg, a heart rate of 92 beats per minute, a respiratory rate of 16 breaths per minute, and oxygen saturation of 99% on room air.
A thorough primary survey revealed a patent and protected airway, bilateral symmetric breath sounds with no evidence of tension pneumothorax or hemothorax, and adequate perfusion. The focused assessment with sonography for trauma examination was negative for free intraperitoneal or pericardial fluid. The pelvic binder was not required as the pelvis was clinically stable to AP and lateral compression. The primary injury was isolated to the right lower extremity.
The patient’s past medical history is highly relevant to the anticipated biological healing cascade and perioperative risk stratification. He carries a diagnosis of Type 2 Diabetes Mellitus, currently managed with oral metformin, with a recent Hemoglobin A1c of 6.8%. While relatively well-controlled, diabetes inherently alters bone microarchitecture and impairs cellular responses to trauma. The accumulation of advanced glycation end-products in the collagen matrix increases bone fragility, while microvascular disease impairs the critical angiogenic response required for soft callus formation. Furthermore, the patient has a 15 pack-year smoking history. Nicotine induces profound peripheral vasoconstriction, drastically reducing cutaneous and osseous blood flow. Concurrently, carbon monoxide competitively binds to hemoglobin, shifting the oxygen dissociation curve to the left and resulting in tissue hypoxia. This combination significantly elevates the risk of delayed union, nonunion, and surgical site infection, particularly in the watershed areas of the tibial diaphysis. The patient reported no known drug allergies, no prior surgical interventions, and his last oral intake was approximately six hours prior to the trauma, clearing him for urgent surgical intervention if required.
Clinical Examination Findings
Following the primary survey, a meticulous secondary survey was conducted with a concentrated focus on the right lower extremity. The evaluation of the soft tissue envelope in high-energy tibial fractures is as critical as the analysis of the osseous injury itself, as it dictates the timing and modality of surgical fixation.
Soft Tissue Assessment
Inspection of the right lower extremity revealed gross clinical deformity with obvious apex anteromedial angulation in the proximal third of the tibia. Significant non-pitting edema and ecchymosis were present, extending from the distal thigh to the ankle joint. The skin integrity was meticulously evaluated. While the fracture was closed, the soft tissue envelope exhibited signs of severe contusion consistent with a Tscherne Grade 2 closed soft tissue injury. There was deep muscle contusion and moderate to severe abrasion, but no impending skin necrosis or tenting that would necessitate emergent reduction for skin preservation. Fracture blisters, which represent cleavage at the dermo-epidermal junction due to massive interstitial edema, had not yet formed but were highly anticipated given the energy of the injury.
Palpation elicited marked, circumferential tenderness over the proximal tibial diaphysis. Gross crepitus and abnormal mobility were appreciated with minimal manipulation, confirming the discontinuity of the tibial shaft.
Compartment Syndrome Evaluation
Given the high-energy mechanism and the rapidly accumulating edema, the patient was at an exceptionally high risk for acute compartment syndrome. The pathophysiology of acute compartment syndrome involves an increase in interstitial pressure within a closed osteofascial compartment, which eventually exceeds capillary perfusion pressure. This leads to a collapse of the arteriovenous gradient, resulting in tissue hypoxia, anaerobic metabolism, and subsequent myonecrosis.
Clinical assessment of the four compartments of the lower leg (anterior, lateral, superficial posterior, and deep posterior) was performed. The compartments were tense and swollen but remained compressible, lacking the classic "wood-like" rigidity associated with late-stage compartment syndrome. Pain out of proportion to the injury and pain with passive stretch of the ischemic muscles are the most sensitive early clinical indicators. Passive plantar flexion of the toes (stretching the anterior compartment musculature, primarily the extensor hallucis longus and extensor digitorum longus) and passive dorsiflexion (stretching the deep posterior compartment, primarily the flexor hallucis longus and flexor digitorum longus) elicited pain, but it was not deemed disproportionate to the severe underlying fracture. However, clinical examination in an alert patient with a highly painful fracture can be equivocal. Therefore, serial clinical examinations were mandated, and the threshold for invasive intracompartmental pressure monitoring via a solid-state transducer was kept exceedingly low. A Delta P calculation (diastolic blood pressure minus intracompartmental pressure) of less than 30 mmHg would serve as the absolute indication for emergent four-compartment fasciotomies.
Neurological and Vascular Status
A comprehensive neurovascular examination is paramount, particularly considering the anatomical vulnerability of the neurovascular structures traversing the proximal tibia. The popliteal artery bifurcates at the proximal border of the interosseous membrane, and the anterior tibial artery passes anteriorly through the hiatus in the interosseous membrane, tethering it and making it highly susceptible to shear forces in proximal tibial fractures.
Vascular assessment demonstrated palpable and symmetric dorsalis pedis and posterior tibial pulses (graded 2+ bilaterally). Capillary refill in the digits was brisk, occurring in less than two seconds. The skin was warm and well-perfused distally. There was no evidence of an expanding hematoma or pulsatile mass in the popliteal fossa.
Neurological assessment evaluated the motor and sensory distributions of the major peripheral nerves. The deep peroneal nerve, coursing through the vulnerable anterior compartment, was intact, evidenced by 4/5 strength in ankle dorsiflexion and great toe extension, along with intact sensation in the first dorsal web space. The superficial peroneal nerve (lateral compartment) was intact, with 4/5 strength in foot eversion and normal sensation over the dorsum of the foot. The tibial nerve (deep posterior compartment) demonstrated 4/5 strength in ankle plantarflexion and toe flexion, with intact sensation over the plantar aspect of the foot. The saphenous and sural nerve sensory distributions were also intact. The initial neurovascular exam provided a reassuring baseline, though continuous monitoring was required due to the evolving nature of the soft tissue edema.
Imaging and Diagnostics
Standard radiographic evaluation of the injured extremity is the cornerstone of initial diagnostic management. The protocol mandates orthogonal anteroposterior and lateral projections of the entire tibia, strictly incorporating the knee and ankle joints to rule out contiguous fractures or joint subluxations.
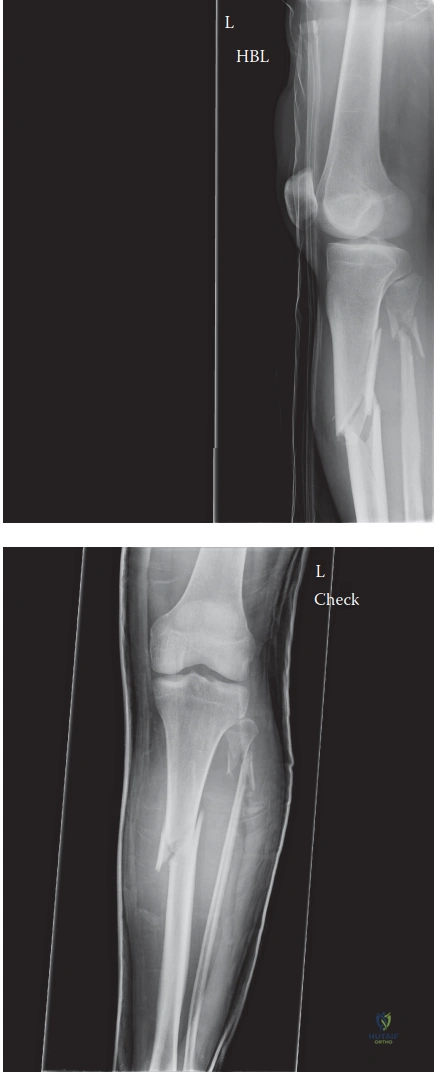
Radiographic analysis of the right lower extremity revealed a severely displaced, comminuted fracture of the proximal third of the tibial diaphysis. The fracture pattern exhibited a dominant oblique configuration with a large, laterally displaced butterfly fragment, indicative of combined axial loading and bending moments. There was approximately 15 millimeters of shortening, with significant apex anterior (procurvatum) and apex lateral (valgus) angulation. This specific deformity pattern is classic for proximal third tibial fractures and is driven by the unopposed pull of the extensor mechanism (quadriceps via the patellar tendon) on the proximal fragment, drawing it into extension, while the pes anserinus and iliotibial band exert variable varus/valgus and rotational forces. The fibula demonstrated a concomitant comminuted fracture at the same level, further compromising the inherent stability of the lower leg segment.

While plain radiographs provide the macroscopic architecture of the diaphyseal injury, they are notoriously insensitive for detecting occult intra-articular extension into the tibial plateau. Literature indicates that up to 20% to 30% of high-energy proximal third tibial shaft fractures possess an unrecognized coronal or sagittal split propagating into the articular surface. The presence of an intra-articular component drastically alters the surgical algorithm, necessitating independent anatomical reduction and absolute stability (lag screw fixation) of the articular block prior to the introduction of any intramedullary device, which could otherwise displace the intra-articular fracture and lead to catastrophic post-traumatic arthrosis.
Consequently, a dedicated computed tomography scan of the right knee and proximal tibia with fine axial cuts and multiplanar (coronal and sagittal) reconstructions was ordered. The CT scan is critical for assessing the integrity of the tibial plateau, identifying unrecognized posterior malleolar fractures (if the scan is extended distally, though less common with proximal third injuries compared to distal third spiral fractures), and evaluating the exact geometry of the medullary canal.
Preoperative templating was performed utilizing the digital radiograph suite. True magnification markers were used to determine the appropriate length and diameter of the anticipated intramedullary nail. The isthmus of the tibia was measured to guide reamer sizing, and the proximal metaphysis was scrutinized to plan the trajectory of blocking screws (Poller screws), which are essential for maintaining reduction in the wide metaphyseal flare where the intramedullary nail provides insufficient cortical contact for inherent stability.
Differential Diagnosis
The presentation of a deformed, painful lower extremity following high-energy trauma requires a systematic differentiation of specific injury patterns, as the management protocols vary significantly.
| Differential Diagnosis | Clinical Presentation | Imaging Findings | Management Implications |
|---|---|---|---|
| Proximal Tibial Diaphyseal Fracture | Severe pain, gross deformity (procurvatum/valgus), inability to bear weight, tense soft tissues. | Discontinuity of the proximal tibial shaft, often with comminution. Intact articular surface on CT. | Requires surgical stabilization, typically via intramedullary nailing or plate osteosynthesis, depending on soft tissue status. |
| Bicondylar Tibial Plateau Fracture (Schatzker VI) | Massive knee effusion (hemarthrosis), widening of the knee joint, axial instability, severe proximal pain. | Metaphyseal-diaphyseal dissociation with intra-articular extension, depression, and widening of the medial and lateral condyles. | Requires anatomical reduction of the articular surface and stable internal fixation, often utilizing dual plating constructs. IM nailing is contraindicated. |
| Acute Compartment Syndrome (Isolated) | Pain out of proportion, pain with passive muscle stretch, tense "wood-like" compartments, paresthesia (late). | Radiographs may be normal or show minimal osseous injury. Diagnosis is primarily clinical and via intracompartmental pressure monitoring. | Emergent surgical emergency requiring four-compartment fasciotomies. Delay leads to irreversible myonecrosis and Volkmann's ischemic contracture. |
| Proximal Tibiofibular Joint Dislocation | Lateral knee pain, prominence of the fibular head, possible common peroneal nerve palsy (foot drop). | Asymmetry of the proximal tibiofibular joint on AP/Lateral knee radiographs. CT confirms subluxation/dislocation. | Closed reduction under sedation. If irreducible or highly unstable, open reduction and temporary screw fixation or ligamentous reconstruction is required. |
Proximal Tibial Diaphyseal Fracture
This is the primary working diagnosis. The clinical deformity and plain radiographs definitively demonstrate the diaphyseal discontinuity. The challenge lies not in the diagnosis, but in the execution of the surgical plan, as the proximal third of the tibia is notorious for malalignment during intramedullary nailing due to the mismatch between the narrow nail and the wide metaphyseal canal.
Bicondylar Tibial Plateau Fracture
High-energy axial loads can drive the femoral condyles into the tibial plateau, causing severe articular comminution and metaphyseal dissociation. Clinically, these present with massive hemarthrosis and severe instability of the knee joint proper. While our patient has proximal tibial swelling, the primary deformity is diaphyseal. The mandatory CT scan definitively rules out articular involvement, confirming this is an extra-articular diaphyseal injury. If articular extension were present, the treatment paradigm would shift entirely towards articular reconstruction and dual plating, abandoning the intramedullary nail approach.
Acute Compartment Syndrome
While acute compartment syndrome is a complication rather than a primary osseous diagnosis, it must be considered as an independent entity that dictates immediate management. A patient can sustain a severe soft tissue crush injury resulting in compartment syndrome without a concomitant fracture. In this case, the patient has a highly concerning soft tissue envelope, but serial examinations and the absence of disproportionate pain with passive stretch currently keep ACS as a high-risk impending complication rather than the primary immediate surgical indication. Vigilance remains paramount.
Proximal Tibiofibular Joint Dislocation
This injury is often missed in the setting of polytrauma. It occurs via sudden twisting motions of the flexed knee. Patients present with lateral knee pain and a palpable prominence of the fibular head. The common peroneal nerve wraps directly around the fibular neck and is at extreme risk in these dislocations. Our patient’s intact peroneal nerve function and the clear diaphyseal nature of the injury on radiographs make this diagnosis less likely, though the proximal fibula fracture noted on imaging requires assessment to ensure the joint itself is not entirely disrupted.
Surgical Decision Making and Classification
The fracture was classified according to the AO/OTA alphanumeric system as a 42-B3 injury (Tibia, Diaphysis, Wedge fracture, Fragmented wedge). Given the closed nature of the injury, the Gustilo-Anderson classification is inapplicable; instead, the Tscherne classification of Grade 2 was assigned, denoting significant deep soft tissue contusion and impending blister formation.
The decision-making process for proximal third tibial diaphyseal fractures is inherently complex. Non-operative management via long-leg casting is contraindicated for this patient. High-energy, displaced, comminuted fractures of the proximal third treated conservatively carry an unacceptably high rate of malunion, nonunion, and prolonged immobilization leading to joint stiffness and deep vein thrombosis. The deforming forces are too immense to be controlled by external splintage alone.
Surgical stabilization is unequivocally indicated. The debate centers on the modality of fixation: external fixation, plate osteosynthesis, or intramedullary nailing.
External fixation is generally reserved for damage control orthopedics in the hemodynamically unstable polytrauma patient or in the presence of massive, contaminated soft tissue defects (e.g., severe Gustilo IIIB or IIIC open fractures). Given this patient’s hemodynamic stability and closed soft tissue envelope, definitive internal fixation is preferred.
Minimally Invasive Percutaneous Plate Osteosynthesis (MIPPO) is a viable option for proximal third fractures. It allows for excellent anatomical reduction and avoids the intra-articular risks of nailing. However, plating the tibia, particularly on the subcutaneous anteromedial surface, requires significant soft tissue stripping (even with percutaneous techniques) and introduces bulky hardware under a traumatized soft tissue envelope, significantly increasing the risk of wound dehiscence and deep infection. Furthermore, plates are load-bearing devices in the diaphysis and are highly susceptible to fatigue failure prior to fracture union, particularly in non-compliant patients or those with delayed healing biology (such as this diabetic, smoking patient).
Intramedullary Nailing (IMN) remains the gold standard for tibial diaphyseal fractures. It is a load-sharing device that preserves the extraosseous blood supply, offers superior biomechanical stability against bending and torsional forces, and allows for earlier weight-bearing. However, nailing proximal third fractures is notoriously treacherous. The proximal tibial metaphysis is wide and funnel-shaped. When a standard intramedullary nail is inserted via a traditional infrapatellar approach, the knee must be hyper-flexed past 90 degrees. This hyper-flexion maximizes the tension on the patellar tendon, which inserts on the tibial tubercle. As the nail is driven down the canal, the patellar tendon pulls the proximal fragment anteriorly. Simultaneously, the nail tends to direct itself towards the posterior cortex of the distal fragment due to the "wedge effect" of the posterior proximal tibial cortex. This combination inevitably leads to the classic apex anterior (procurvatum) and valgus malalignment.
To mitigate these severe deforming forces, advanced surgical techniques must be employed. The surgical plan for this patient involves a Suprapatellar Intramedullary Nailing technique combined with the strategic placement of blocking (Poller) screws.
Surgical Technique and Intervention
The patient was taken to the operating room and placed in the supine position on a radiolucent flat Jackson table. General endotracheal anesthesia was administered, and a preoperative dose of intravenous cefazolin was given for surgical prophylaxis. A sterile tourniquet was placed on the proximal right thigh but not inflated, reserved only for catastrophic hemorrhage.
The critical advantage of the suprapatellar approach is patient positioning. The limb is positioned with the knee in a semi-extended posture, resting on a sterile bump at approximately 15 to 20 degrees of flexion. This semi-extended position dramatically reduces the tension on the extensor mechanism, neutralizing the primary deforming force that causes procurvatum. It also facilitates easier acquisition of orthogonal fluoroscopic images without needing to constantly manipulate the injured limb.
Approach and Entry Portal
A 3-centimeter longitudinal incision was made approximately 2 centimeters proximal to the superior pole of the patella. Dissection was carried down through the subcutaneous tissue to the quadriceps tendon. A midline longitudinal split was created in the quadriceps tendon, and the underlying suprapatellar pouch was entered. A specialized retropatellar cannula system with a protective Teflon sleeve was carefully advanced deep to the patella and seated on the anterior aspect of the proximal tibia. This cannula is absolutely critical to protect the articular cartilage of the patellofemoral joint from iatrogenic damage during reaming and nail insertion.
The starting point is paramount in proximal third fractures. Under fluoroscopic guidance, a rigid guide pin was placed perfectly centered on the AP view (in line with the anatomical axis of the medullary canal) and highly proximal and anterior on the lateral view, just extra-articular to the anterior margin of the tibial plateau. An eccentric starting point will invariably dictate a malreduced trajectory. The starting hole was opened using a cannulated opening reamer over the guide pin.
Reduction and Blocking Screws
The cardinal rule of proximal tibial nailing is that the nail does not reduce the fracture; the fracture must be anatomically reduced prior to the passage of the reamer or the nail. Due to the "bell-clapper effect" in the wide metaphysis, the nail will simply follow the path of least resistance, cementing any existing deformity.
To achieve and maintain reduction, percutaneous pointed reduction clamps were utilized. However, to permanently narrow the metaphyseal canal and force the nail into the correct central trajectory, blocking screws (Poller screws) were employed. The biomechanical principle of a blocking screw is to place it on the concave side of the anticipated deformity. To prevent the classic valgus and procurvatum deformity, two blocking screws were placed in the proximal fragment. One screw was placed in the posterior half of the proximal fragment (viewed laterally) to block the nail from translating posteriorly, thereby preventing procurvatum. A second screw was placed in the lateral half of the proximal fragment (viewed on AP) to prevent the nail from translating laterally, thereby preventing valgus.
Reaming and Nail Insertion
With the fracture anatomically reduced and the trajectory secured by the blocking screws, a ball-tipped guide wire was passed down the medullary canal to the level of the distal tibial epiphyseal scar. Sequential flexible reaming was performed in 0.5-millimeter increments. Reaming generates autologous bone graft (osteogenic reamings) that is deposited at the fracture site, promoting secondary bone healing. Care was taken to monitor for excessive intramedullary pressure, which can lead to fat embolization syndrome, though the risk is mitigated by the open nature of the fracture hematoma. The canal was over-reamed by 1.0 to 1.5 millimeters larger than the selected nail diameter.
A 10-millimeter diameter, appropriately templated titanium tibial nail with a proximal Herzog bend was selected. The nail was advanced over the guide wire through the protective cannula. Because the knee was semi-extended and the blocking screws were properly positioned, the nail passed smoothly across the fracture site without displacing the proximal fragment.
Interlocking and Closure
Proximal fixation in a wide metaphysis requires maximum stability. The nail was locked proximally utilizing three multi-planar interlocking screws (two medial-to-lateral, one oblique) to control rotation and angular displacement. Distal interlocking was performed utilizing a perfect-circle freehand fluoroscopic technique, placing two medial-to-lateral screws.
Final fluoroscopic images confirmed excellent orthogonal alignment, restoration of length, and appropriate hardware placement. The wounds were copiously irrigated. The quadriceps tendon split was meticulously repaired with heavy absorbable suture to ensure extensor mechanism integrity. The skin was closed precisely without tension. A sterile, bulky Jones dressing was applied to accommodate anticipated postoperative swelling.
Post Operative Protocol and Rehabilitation
The immediate postoperative period requires extreme vigilance for the development of delayed acute compartment syndrome. The trauma of reaming and nail insertion introduces additional volume and inflammatory mediators into the closed fascial spaces. The patient was admitted to the orthopedic trauma unit with strict instructions for hourly neurovascular and compartment checks for the first 24 hours. The limb was elevated precisely at the level of the heart—elevation
