ABOS Part I Orthopaedic Review: Spondylolisthesis, Scoliosis & Spinal Deformity Management | Part 22224
Key Takeaway
This ABOS Part I review module provides 21 advanced multiple-choice questions on spondylolisthesis and scoliosis. It covers diagnosis, classification systems (Wiltse-Newman, Meyerding), conservative and surgical management strategies (fusion, decompression), and key considerations for spinal deformities in orthopaedic practice, preparing candidates for board examinations.
ABOS Part I Comprehensive Review - Batch 101
This module contains 21 advanced orthopedic multiple-choice questions developed to mirror the American Board of Orthopaedic Surgery (ABOS) Part I and AAOS OITE examinations. Questions are derived directly from high-yield clinical teaching cases.
Generated MCQ Transcript
Question 1:
A 14-year-old competitive gymnast presents with insidious onset low back pain exacerbated by extension and hyperextension activities. Physical examination reveals hamstring tightness and a palpable step-off at L5. AP and lateral radiographs of the lumbar spine show a defect in the pars interarticularis at L5 with an anterior translation of L5 on S1. Which of the following is the most appropriate classification for this condition?
- A: Type I Dysplastic
- B: Type II Isthmic, Lytic
- C: Type III Degenerative
- D: Type IV Traumatic
- E: Type V Pathologic
Explanation:
Correct Answer: B
The patient's age, activity (gymnast), pars defect, and anterior translation are classic for an isthmic spondylolisthesis. The Wiltse-Newman classification Type II isthmic is characterized by a lesion in the pars interarticularis. Given the insidious onset and high-impact repetitive extension activities, it's most likely a stress fracture (lytic) rather than an acute traumatic fracture (Type IV) or congenital dysplastic anomaly (Type I). Degenerative (Type III) is typically seen in older adults, and pathologic (Type V) is due to bone disease.
Question 2:
Which of the following Meyerding grades of spondylolisthesis indicates a slip of 50-75% of the vertebral body's width?
- A: Grade I
- B: Grade II
- C: Grade III
- D: Grade IV
- E: Grade V
Explanation:
Correct Answer: C
The Meyerding classification system grades spondylolisthesis based on the percentage of anterior displacement of the superior vertebral body over the inferior one. Grade I is 0-25%, Grade II is 25-50%, Grade III is 50-75%, Grade IV is 75-100%, and Grade V (spondyloptosis) is complete displacement (>100%). Therefore, 50-75% displacement corresponds to Grade III.
Question 3:
A 55-year-old female presents with a long history of low back pain and bilateral leg pain, worse with standing and walking, relieved by sitting or leaning forward. Radiographs show L4-L5 degenerative spondylolisthesis (Grade I) with associated spinal stenosis. She has failed 6 months of comprehensive conservative management including physical therapy, NSAIDs, and epidural steroid injections. Neurological exam reveals mild quadriceps weakness (4+/5) bilaterally but no frank motor deficit. What is the most appropriate next step in management?
- A: Continue conservative management, add opioid analgesics
- B: L4-L5 posterior decompression alone
- C: L4-L5 posterior decompression and instrumented posterolateral fusion
- D: L4-L5 anterior lumbar interbody fusion alone
- E: L4-L5 transforaminal lumbar interbody fusion (TLIF) without decompression
Explanation:
Correct Answer: C
For symptomatic degenerative spondylolisthesis with spinal stenosis that has failed conservative management, surgical intervention is often indicated. The Spine Patient Outcomes Research Trial (SPORT) demonstrated superior outcomes for surgical treatment compared to non-operative care in patients with degenerative spondylolisthesis and stenosis. While decompression alone can address stenosis, studies like SPORT have shown that adding fusion to decompression significantly improves outcomes and reduces reoperation rates for degenerative spondylolisthesis, especially in the presence of instability or significant back pain. Quadriceps weakness suggests L4 nerve root compression, making decompression necessary. Anterior fusion alone does not address the posterior decompression requirement. TLIF typically includes decompression. The best option combining decompression and stabilization is decompression with instrumented posterolateral fusion.
Question 4:
A 30-year-old male with chronic L5-S1 isthmic spondylolisthesis (Grade II) complains of persistent low back pain and bilateral S1 radiculopathy despite 9 months of conservative treatment. On examination, he has bilateral hamstring tightness and a positive straight leg raise test at 45 degrees. Which of the following imaging modalities is most crucial for evaluating potential nerve root compression and planning surgical decompression?
- A: Plain radiographs (AP/Lateral/Oblique)
- B: CT scan of the lumbar spine
- C: MRI of the lumbar spine
- D: Bone scintigraphy
- E: Electromyography (EMG)
Explanation:
Correct Answer: C
While plain radiographs define the slip, and CT can better visualize bony stenosis, MRI is superior for evaluating soft tissue structures, including nerve roots, discs, and the spinal cord, and identifying nerve root compression by hypertrophic soft tissue, disc herniation, or foraminal stenosis, which is critical for surgical planning in patients with radiculopathy. EMG assesses nerve function but isn't an imaging modality for structural compression.
Question 5:
Which of the following describes the anatomical defect in Type IIB isthmic spondylolisthesis?
- A: Elongation of the pars interarticularis without fracture
- B: Lytic stress fracture of the pars interarticularis
- C: Acute fracture of the pars interarticularis
- D: Degeneration of the facet joints
- E: Congenital dysplastic elements
Explanation:
Correct Answer: A
Wiltse-Newman Type II isthmic spondylolisthesis is subdivided: Type IIA is a lytic (stress) fracture of the pars, Type IIB is an elongated but intact pars (often a healed stress fracture with elongation), and Type IIC is an acute fracture of the pars. Therefore, Type IIB specifically refers to an elongated pars without a clear lytic defect.
Question 6:
What is the most common neurological complication following reduction of a high-grade spondylolisthesis?
- A: Cauda equina syndrome
- B: L5 nerve root palsy
- C: S1 nerve root palsy
- D: Foot drop (peroneal nerve palsy)
- E: Femoral nerve palsy
Explanation:
Correct Answer: B
The L5 nerve root is most vulnerable during the reduction of a high-grade L5-S1 spondylolisthesis. This is due to its course over the sacral ala and the potential for stretch injury during the reduction maneuver, especially with attempts to correct lumbosacral kyphosis. While other nerve injuries can occur, L5 radiculopathy/palsy is the most frequently reported neurological complication.
Question 7:
What is the typical radiological feature that differentiates degenerative spondylolisthesis from isthmic spondylolisthesis?
- A: Sacral spina bifida occulta
- B: Pars interarticularis defect
- C: Intact pars interarticularis with facet joint degeneration
- D: Trapezoidal L5 vertebral body
- E: High-grade slip (>50%)
Explanation:
Correct Answer: C
Degenerative spondylolisthesis (Wiltse-Newman Type III) is characterized by an intact pars interarticularis, with anterior slippage resulting from chronic instability due to degenerative changes in the facet joints and intervertebral disc. Isthmic spondylolisthesis (Type II) is defined by a defect in the pars. Type I (Dysplastic) can have a trapezoidal L5 and spina bifida. High-grade slips can occur in both types, though less common in Type III.
Question 8:
A 12-year-old active child presents with an L5-S1 Grade II spondylolisthesis that has shown progression from Grade I over the past 6 months. He has moderate back pain but no neurological deficits. Conservative treatment has been initiated but the slip continues to progress. What is the most appropriate next step in management?
- A: Continue conservative management indefinitely
- B: Perform L5-S1 posterolateral fusion in situ
- C: Attempt aggressive reduction and fusion
- D: Decompression alone at L5-S1
- E: Initiate high-dose corticosteroid therapy
Explanation:
Correct Answer: B
In a child with a progressive spondylolisthesis (especially Grade II or higher) despite conservative management, surgical stabilization is indicated to prevent further slip and potential neurological complications. L5-S1 in situ posterolateral fusion is generally preferred for these cases. Aggressive reduction is associated with higher risks of neurological injury, and decompression alone would not address the instability or progression. Corticosteroids are not indicated.
Question 9:
In an adult patient with isthmic spondylolisthesis, which muscle group is characteristically tight and often contributes to sagittal imbalance and altered gait?
- A: Quadriceps femoris
- B: Gluteus maximus
- C: Hamstrings
- D: Psoas major
- E: Rectus abdominis
Explanation:
Correct Answer: C
Hamstring tightness is a common clinical finding in patients with spondylolisthesis, particularly in children and adolescents, but also in adults. It is thought to be a compensatory mechanism to maintain sagittal balance and prevent further anterior shear forces on the unstable segment, often leading to a 'pelvic tilt' or 'waddling' gait.
Question 10:
What is the primary advantage of a Transforaminal Lumbar Interbody Fusion (TLIF) over a Posterior Lumbar Interbody Fusion (PLIF) for spondylolisthesis correction?
- A: Allows for wider central canal decompression
- B: Requires less posterior muscle dissection
- C: Provides better lordosis restoration
- D: Offers a lower risk of dural tear and nerve root injury
- E: Enables multi-level fusion more easily
Explanation:
Correct Answer: D
TLIF offers a unilateral approach to the disc space, allowing for disc excision and cage placement through the foramen. This typically involves less retraction of the thecal sac and nerve roots compared to PLIF, which requires bilateral laminectomy and retraction, thereby generally carrying a lower risk of dural tear and nerve root injury. While both can restore lordosis and achieve fusion, the safety profile regarding dural injury is a key advantage of TLIF.
Question 11:
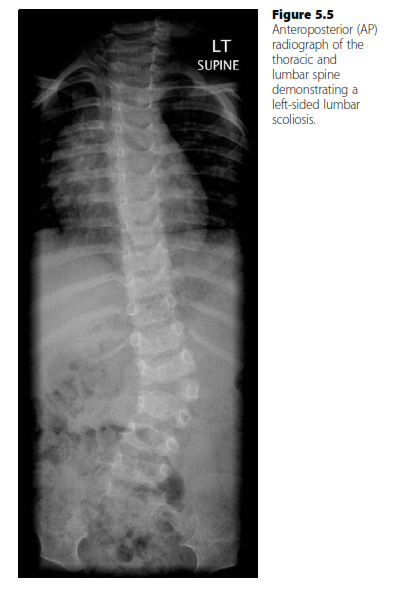
A 6-year-old male presents with a progressive spinal deformity. An AP radiograph, similar to the one shown, reveals a left-sided lumbar scoliosis with a fully segmented hemivertebra at L2 and a contralateral unsegmented bar from L1 to L3. The Cobb angle measures 35 degrees. Based on the natural history of congenital scoliosis, what is the most likely prognosis for this patient's curve progression?
- A: A. The curve is likely to stabilize or resolve spontaneously due to the patient's young age.
- B: B. The curve will likely progress slowly, approximately 1 degree per year, after skeletal maturity.
- C: C. The curve has a benign prognosis and is unlikely to progress beyond 20 degrees.
- D: D. The curve has the least balanced growth potential and the worst prognosis for progression.
- E: E. The curve will likely respond well to bracing and prevent the need for surgical intervention.
Explanation:
Correct Answer: D
Explanation:
The case describes a fully segmented hemivertebra in connection with a contralateral unsegmented bar. According to the provided text, this specific combination of congenital vertebral anomalies has the least balanced growth potential and the worst prognosis for progression. This is because a fully segmented hemivertebra has growth plates cranial and caudal to it, allowing for significant growth, while the contralateral unsegmented bar acts as a tether, preventing growth on the concave side. This imbalance leads to severe and progressive deformity.
- A. The curve is likely to stabilize or resolve spontaneously due to the patient's young age. This is incorrect. While some infantile idiopathic scoliosis curves may resolve, congenital scoliosis, especially with significant vertebral anomalies like a fully segmented hemivertebra and unsegmented bar, rarely resolves spontaneously and typically progresses.
- B. The curve will likely progress slowly, approximately 1 degree per year, after skeletal maturity. This rate of progression (1 degree per year) is typically associated with adolescent idiopathic scoliosis after skeletal maturity. Congenital scoliosis with severe anomalies can progress much more rapidly, especially during growth spurts, and its progression is not solely tied to post-maturity rates of idiopathic curves.
- C. The curve has a benign prognosis and is unlikely to progress beyond 20 degrees. This is incorrect. A benign prognosis, rarely progressing beyond 20 degrees, is characteristic of a block vertebra, not a fully segmented hemivertebra with a contralateral unsegmented bar.
- E. The curve will likely respond well to bracing and prevent the need for surgical intervention. Bracing is generally less effective for congenital scoliosis, particularly those caused by significant bony anomalies like hemivertebrae and unsegmented bars, because the deformity is structural and driven by differential bone growth. Surgical intervention is often required for progressive congenital curves with severe anomalies.
Question 12:
A 12-year-old female presents with a 42-degree right thoracic scoliosis. She is premenarchal and has a Risser sign of 0. Her parents report a recent growth spurt. Based on the provided information, which of the following factors is the strongest indicator of a high likelihood of curve progression in this patient?
- A: A. The curve's location in the thoracic spine.
- B: B. The patient's female gender.
- C: C. The current Cobb angle of 42 degrees.
- D: D. Her premenarchal status and Risser 0.
- E: E. The presence of a right-sided curve.
Explanation:
Correct Answer: D
Explanation:
The provided text explicitly lists features that indicate an increased likelihood of curve progression in adolescent idiopathic scoliosis. These include: young age at onset, premenarchal status, physical immaturity (like Risser 0), large curves, and female gender. Among these, premenarchal status and a low Risser sign (indicating significant remaining growth potential) are critical indicators of ongoing skeletal immaturity and thus a high risk for rapid progression during the adolescent growth spurt.
- A. The curve's location in the thoracic spine. While thoracic curves are common in AIS, the location itself is not listed as the strongest predictor of progression compared to skeletal maturity.
- B. The patient's female gender. Female gender is indeed a risk factor for progression, especially for curves over 20 degrees (F:M 5.4:1). However, in the context of a 12-year-old premenarchal girl with Risser 0, the immaturity indicators (premenarchal status, Risser 0) are more direct and stronger predictors of future progression than gender alone, as they signify the peak growth period.
- C. The current Cobb angle of 42 degrees. A large curve (over 40 degrees) is a risk factor for progression. However, the potential for further rapid progression is most strongly linked to the remaining growth. A 42-degree curve in a skeletally mature individual would progress much less than a 42-degree curve in a skeletally immature individual.
- E. The presence of a right-sided curve. A right thoracic curve is the most common pattern in AIS and is not considered an atypical feature indicating higher progression risk compared to, for example, a left-sided curve which might suggest underlying pathology.
Question 13:
A 10-year-old patient with Duchenne muscular dystrophy develops a progressive scoliosis, similar to the pattern of a collapsing long 'C' shaped curve. The patient has recently lost ambulatory function. The orthopedic team is considering surgical intervention. What is the primary goal of surgical treatment for neuromuscular scoliosis in this patient?
- A: A. Complete correction of the spinal deformity to achieve a Cobb angle less than 10 degrees.
- B: B. Prevention of future progression to avoid the need for nocturnal ventilation.
- C: C. Improvement of quality of life, maintenance of function, and sitting balance.
- D: D. Excision of any underlying vertebral anomalies contributing to the curve.
- E: E. Restoration of ambulatory function and independent mobility.
Explanation:
Correct Answer: C
Explanation:
The text explicitly states that the goals of treatment in neuromuscular scoliosis are improved quality of life, maintenance of function, maintenance of respiratory function, and sitting balance. These patients often have significant comorbidities and limited functional potential, so the goals are focused on improving their daily living and preventing further deterioration rather than achieving a 'normal' spine.
- A. Complete correction of the spinal deformity to achieve a Cobb angle less than 10 degrees. While correction is a goal, 'complete correction' to less than 10 degrees is often unrealistic and not the primary or sole goal in neuromuscular scoliosis, where functional outcomes are prioritized over radiographic perfection.
- B. Prevention of future progression to avoid the need for nocturnal ventilation. While maintaining respiratory function is a goal, and surgery can delay deterioration, it does not necessarily 'avoid' the need for nocturnal ventilation, especially in a progressive disease like Duchenne muscular dystrophy. The text mentions surgery having an 'additive effect with nocturnal ventilation in delaying the deterioration of respiratory function.'
- D. Excision of any underlying vertebral anomalies contributing to the curve. This is a treatment strategy for congenital scoliosis (e.g., hemivertebra excision), not typically for neuromuscular scoliosis, which is caused by muscle weakness and lack of spinal support, not vertebral malformations.
- E. Restoration of ambulatory function and independent mobility. In Duchenne muscular dystrophy, scoliosis often develops after the loss of ambulatory function. Surgery aims to improve sitting balance and overall function, but it does not restore lost ambulatory function.
Question 14:
An 8-year-old boy presents with a left-sided thoracic scoliosis and severe back pain. Physical examination reveals abnormal abdominal reflexes and a hairy patch over his lower back. An AP radiograph, similar to the one shown, confirms the scoliosis. Which of the following investigations is most strongly indicated given these atypical findings?

- A: A. Full-length standing lateral X-ray to assess sagittal balance.
- B: B. Risser sign assessment to determine skeletal maturity.
- C: C. Surface topography to objectively assess curve progression.
- D: D. MRI scanning of the spine to detect underlying intraspinal anomalies.
- E: E. Electromyography (EMG) to evaluate muscle function.
Explanation:
Correct Answer: D
Explanation:
The case describes several 'atypical features' for scoliosis: a left-sided thoracic curve (most common is right thoracic), severe back pain (scoliosis is not typically painful, severe pain indicates underlying cause), abnormal abdominal reflexes (most commonly associated with intraspinal anomalies), and a hairy patch on the back (a feature of spinal dysraphism). The text explicitly states that MRI scanning of the spine can be used to detect underlying intraspinal anomalies such as diastomatomyelia, syringomyelia, and Arnold–Chiari malformations, particularly in atypical curves.
- A. Full-length standing lateral X-ray to assess sagittal balance. While a lateral X-ray is part of a standard scoliosis workup, it would not directly identify intraspinal anomalies suggested by the atypical findings.
- B. Risser sign assessment to determine skeletal maturity. Risser sign is important for predicting progression in idiopathic scoliosis but does not address the underlying pathology suggested by the atypical features.
- C. Surface topography to objectively assess curve progression. Surface topography is used for follow-up and objective assessment of curves but does not diagnose intraspinal anomalies.
- E. Electromyography (EMG) to evaluate muscle function. EMG might be considered if a neuromuscular cause was suspected, but the specific combination of atypical curve direction, pain, abnormal reflexes, and skin changes points more directly to structural intraspinal anomalies, making MRI the priority.
Question 15:
An orthopedic surgeon is performing a hemivertebra excision in the lumbar spine using a thoraco-abdominal (Hodgson's) approach, as described in the case. After incising the skin, fat, serratus anterior, external oblique, and latissimus dorsi, and removing the 10th rib subperiosteally, the parietal pleura is incised. What is the next critical step in gaining access to the retroperitoneum for this specific approach?
- A: A. Ligation of segmental vessels.
- B: B. Division of the diaphragm 2 cm from its origin.
- C: C. Excision of the discs above and below the hemivertebra.
- D: D. Splitting the costal cartilage to enter the retroperitoneum.
- E: E. Sweeping away retroperitoneal fascia with swabs.
Explanation:
Correct Answer: D
Explanation:
The case provides a detailed description of the thoraco-abdominal (Hodgson's) approach. After the initial steps of skin incision, muscle division, rib removal, and parietal pleura incision, the text explicitly states: 'A key step in this procedure is splitting the costal cartilage to enter the retroperitoneum.' This is the direct next step mentioned to transition from the thoracic cavity (after incising pleura) to the retroperitoneal space where the lumbar vertebrae are accessed.
- A. Ligation of segmental vessels. Ligation of segmental vessels occurs later in the procedure, after the retroperitoneum is entered and the diaphragm is divided, to allow for safe vertebral body work.
- B. Division of the diaphragm 2 cm from its origin. This step occurs after entering the retroperitoneum and sweeping away fascia, to expose the vertebral column more fully.
- C. Excision of the discs above and below the hemivertebra. This is a step performed once the vertebral body is exposed, prior to the hemivertebra excision itself.
- E. Sweeping away retroperitoneal fascia with swabs. This occurs immediately after entering the retroperitoneum, but the entry itself is achieved by splitting the costal cartilage.
Question 16:
A 14-year-old female presents with a 30-degree thoracolumbar idiopathic scoliosis. She is post-menarchal with a Risser sign of 3. The curve has shown 5 degrees of progression over the last 6 months. The patient and her parents are concerned about the deformity. Based on the provided guidelines, what is the most appropriate initial management strategy?
- A: A. Immediate surgical correction with posterior spinal fusion.
- B: B. Observation with serial radiographs every 12 months.
- C: C. Initiation of bracing, worn 23 hours a day.
- D: D. Anterior spinal fusion due to the thoracolumbar curve location.
- E: E. Referral for physical therapy and exercise program only.
Explanation:
Correct Answer: C
Explanation:
The text states that bracing is 'Applied for progressive curves measuring 25–40. Not thought of as corrective but aims to prevent progression of the curve whilst growth continues aiming to reduce the need for surgery.' This patient has a 30-degree curve, which falls within the 25-40 degree range, and has shown progression. Although she is post-menarchal, a Risser 3 indicates some remaining growth potential, making bracing a suitable option to prevent further progression.
- A. Immediate surgical correction with posterior spinal fusion. Surgery is generally reserved for curves with a magnitude > 50 degrees or earlier intervention in curves with greater potential for progression. A 30-degree curve, even with some progression, is typically managed with bracing first, especially with some remaining growth.
- B. Observation with serial radiographs every 12 months. Given the documented progression and the curve magnitude (30 degrees), simple observation is insufficient. More frequent monitoring and intervention (like bracing) are indicated.
- D. Anterior spinal fusion due to the thoracolumbar curve location. While the text mentions considering an anterior approach for thoracolumbar curves, surgery itself is not the initial management for a 30-degree progressive curve in this age group with remaining growth potential.
- E. Referral for physical therapy and exercise program only. Physical therapy alone is not considered an effective treatment for preventing progression of structural scoliosis of this magnitude.
Question 17:
A 7-year-old patient presents with a 55-degree idiopathic scoliosis. The patient's parents report that the curve was first noticed when the child was 5 years old. The orthopedic surgeon is particularly concerned about the potential for cardiorespiratory compromise. What classification of scoliosis best describes this patient's condition, highlighting the surgeon's primary concern?
- A: A. Adolescent Idiopathic Scoliosis (AIS).
- B: B. Juvenile Idiopathic Scoliosis (JIS).
- C: C. Infantile Idiopathic Scoliosis (IIS).
- D: D. Early-Onset Scoliosis (EOS).
- E: E. Late-Onset Scoliosis (LOS).
Explanation:
Correct Answer: D
Explanation:
The text defines 'Early-onset scoliosis' as having its onset before the age of 7 (or 5 by some classifications). It specifically highlights that EOS is 'associated with a high risk of cardiorespiratory compromise as the developing heart and lungs may be affected.' This patient's curve was noticed at age 5, placing it squarely in the early-onset category, and the surgeon's concern directly aligns with the key risk factor for EOS.
- A. Adolescent Idiopathic Scoliosis (AIS). AIS has its onset after age 10 to maturity. This patient's onset was at age 5, so it does not fit AIS.
- B. Juvenile Idiopathic Scoliosis (JIS). JIS has its onset between 3 and 10 years. While the onset at age 5 falls within this range, the term 'Early-Onset Scoliosis' is a broader classification specifically used to group all idiopathic scoliosis cases with onset before age 7 (or 5) due to the shared risk of cardiorespiratory compromise, which is the primary concern in the question.
- C. Infantile Idiopathic Scoliosis (IIS). IIS has its onset between 0 and 3 years. This patient's onset at age 5 is outside this range.
- E. Late-Onset Scoliosis (LOS). LOS has its onset after the age of 7. This patient's onset was at age 5, so it is not late-onset.
Question 18:
A 16-year-old male presents with a 60-degree right thoracic scoliosis. He is skeletally mature with a Risser sign of 5. The curve has shown minimal progression (1 degree per year) since skeletal maturity. He reports significant cosmetic concerns due to rib prominence. Based on the provided treatment guidelines, what is the most appropriate management option?
- A: A. Continued observation with annual radiographs.
- B: B. Initiation of bracing to prevent further progression.
- C: C. Surgical correction with posterior spinal fusion.
- D: D. Anterior spinal fusion due to the large curve magnitude.
- E: E. Physical therapy and chiropractic adjustments.
Explanation:
Correct Answer: C
Explanation:
The text states that surgery is 'Usually reserved for curves with a magnitude > 50.' This patient has a 60-degree curve, which clearly exceeds this threshold. Additionally, 'unacceptable deformity' is listed as an indication for surgery, and the patient reports significant cosmetic concerns due to rib prominence, which is a common associated problem with scoliosis. Given the large, structural curve, surgical correction is the most appropriate management.
- A. Continued observation with annual radiographs. While progression slows after skeletal maturity, a 60-degree curve is already severe and warrants intervention, especially with cosmetic concerns. Observation alone is not sufficient for curves of this magnitude.
- B. Initiation of bracing to prevent further progression. Bracing is typically used for progressive curves between 25-40 degrees in skeletally immature patients to prevent progression. It is not effective for curves over 40-50 degrees or in skeletally mature individuals.
- D. Anterior spinal fusion due to the large curve magnitude. While anterior approaches can be considered for thoracolumbar curves, the text notes a recent trend towards posterior approach with 'third-generation' instrumentation (segmental pedicle screws). The choice of anterior vs. posterior is secondary to the indication for surgery itself, and for a thoracic curve, posterior is often preferred.
- E. Physical therapy and chiropractic adjustments. These modalities are not effective in correcting or preventing the progression of structural scoliosis of this magnitude.
Question 19:
A 13-year-old girl presents with a 28-degree right thoracic scoliosis. Her Risser sign is 2, and she is 6 months post-menarche. Her parents are concerned about the curve's progression. During the examination, the Adam's forward bend test is performed. What is the primary purpose of the Adam's forward bend test in the assessment of scoliosis?
- A: A. To determine the patient's skeletal maturity.
- B: B. To measure the Cobb angle accurately.
- C: C. To assess the flexibility of the spinal curve.
- D: D. To detect rotational deformity and rib prominence.
- E: E. To identify underlying intraspinal anomalies.
Explanation:
Correct Answer: D
Explanation:
The Adam's forward bend test is a clinical screening tool primarily used to detect rotational deformity of the trunk, which manifests as a rib hump or prominence in the thoracic spine or a lumbar prominence. This prominence is a key indicator of the three-dimensional nature of scoliosis, where lateral curvature is accompanied by vertebral rotation.
- A. To determine the patient's skeletal maturity. Skeletal maturity is assessed using radiographic indicators like the Risser sign, not the Adam's forward bend test.
- B. To measure the Cobb angle accurately. The Cobb angle is a radiographic measurement, not determined by physical examination.
- C. To assess the flexibility of the spinal curve. Curve flexibility is typically assessed with lateral bending radiographs, not the Adam's forward bend test.
- E. To identify underlying intraspinal anomalies. Intraspinal anomalies are typically identified through MRI, especially in atypical curves or those with neurological signs. The Adam's test does not directly detect these.
Question 20:
A 4-year-old child is diagnosed with a progressive idiopathic scoliosis. The curve measures 40 degrees. The parents are counseled on the potential long-term complications. Which of the following is the most significant long-term risk specifically associated with this type of scoliosis, as highlighted in the case?
- A: A. Increased risk of severe back pain in adulthood.
- B: B. Development of significant leg length discrepancy.
- C: C. Progressive cardiorespiratory compromise leading to decreased life expectancy.
- D: D. Higher incidence of spondylolisthesis in later life.
- E: E. Increased likelihood of neurological deficits due to spinal cord compression.
Explanation:
Correct Answer: C
Explanation:
The patient is 4 years old with idiopathic scoliosis, which falls under the 'Early-onset scoliosis' category (onset before age 7). The text explicitly states for early-onset scoliosis: 'The developing heart and lungs may be affected by the scoliosis. Cardiorespiratory compromise may result from a progressive curve resulting in decreased life expectancy.' This is the most significant and unique long-term risk highlighted for this specific age group.
- A. Increased risk of severe back pain in adulthood. While scoliosis patients can experience back pain, the text notes that scoliosis is 'not typically thought of as a painful condition,' and severe pain may indicate an underlying cause. Cardiorespiratory compromise is a more specific and severe risk for early-onset scoliosis.
- B. Development of significant leg length discrepancy. Leg length discrepancy can mimic scoliosis but is not a direct long-term complication of idiopathic scoliosis itself.
- D. Higher incidence of spondylolisthesis in later life. Spondylolisthesis is a separate spinal condition and not a direct long-term complication of idiopathic scoliosis.
- E. Increased likelihood of neurological deficits due to spinal cord compression. While severe curves can theoretically lead to neurological issues, this is less common in idiopathic scoliosis compared to congenital scoliosis with intraspinal anomalies. Cardiorespiratory compromise is the primary concern for early-onset idiopathic scoliosis.
Question 21:
A 15-year-old patient presents with a 48-degree left-sided lumbar scoliosis, as depicted in the AP radiograph. The patient reports no pain but is concerned about the cosmetic appearance. She is skeletally mature with a Risser sign of 4. Given the curve characteristics and patient's maturity, what is the most likely natural history of this curve going forward?

- A: A. Rapid progression is expected due to the left-sided curve and lumbar location.
- B: B. The curve will likely stabilize with no further progression.
- C: C. Slow progression of approximately 1 degree per year is expected.
- D: D. Spontaneous resolution of the curve is highly probable.
- E: E. The curve will likely accelerate in progression during the next growth spurt.
Explanation:
Correct Answer: C
Explanation:
The text states: 'Once skeletal maturity is reached the scoliosis tends to stabilize and progress less rapidly (1 per year).' This patient is 15 years old and has a Risser sign of 4, indicating significant skeletal maturity. While a 48-degree curve is substantial, the key factor here is the patient's maturity. Therefore, slow progression at approximately 1 degree per year is the most likely natural history.
- A. Rapid progression is expected due to the left-sided curve and lumbar location. While left-sided curves can be atypical and warrant further investigation for underlying pathology, the primary driver of rapid progression in idiopathic scoliosis is skeletal immaturity. With a Risser 4, rapid progression is unlikely.
- B. The curve will likely stabilize with no further progression. While progression slows, it doesn't typically cease entirely. A small degree of progression (around 1 degree per year) is still expected even after skeletal maturity for larger curves.
- D. Spontaneous resolution of the curve is highly probable. Spontaneous resolution is primarily seen in a significant number of infantile idiopathic scoliosis cases (80-90% of curves before age 2), not in adolescent or mature patients with a 48-degree curve.
- E. The curve will likely accelerate in progression during the next growth spurt. With a Risser 4, the patient is past the peak of their adolescent growth spurt, so an acceleration in progression due to growth is highly unlikely.
⚠️ Unanswered Questions
You have unanswered questions in this module. Are you sure you want to submit?
You Might Also Like
