ABOS Part I Review: Tibia Fractures, IM Nailing & Compartment Syndrome Management | Part 22231
Key Takeaway
Tibia fracture management involves accurate classification (Gustilo-Anderson, Tscherne, AO/OTA), appropriate imaging like CT scans for intra-articular extension, and surgical stabilization, often with intramedullary nailing. Critical considerations include preventing and managing complications such as acute compartment syndrome, vascular injury, and non-union, with specific techniques like blocking screws and suprapatellar approaches.
ABOS Part I Comprehensive Review - Batch 21
This module contains 32 advanced orthopedic multiple-choice questions developed to mirror the American Board of Orthopaedic Surgery (ABOS) Part I and AAOS OITE examinations. Questions are derived directly from high-yield clinical teaching cases.
Generated MCQ Transcript
Question 1:
A 28-year-old male presents to the emergency department after a high-energy motor vehicle collision, sustaining a closed midshaft diaphyseal tibia fracture. He is hemodynamically stable, and initial neurovascular examination is intact. Given the epidemiology and anatomical considerations of high-energy tibia fractures, which of the following statements is most accurate?
- A: The incidence of diaphyseal tibia fractures is highest in elderly individuals due to low-energy falls.
- B: The primary blood supply to the tibial diaphysis is predominantly from periosteal vessels, making it less vulnerable to high-energy trauma.
- C: The anteromedial surface of the tibia has a robust soft tissue envelope, offering significant protection against open fractures.
- D: High-energy mechanisms are frequently associated with comminution and a higher propensity for open fractures, particularly in young, active males.
- E: The fibula is the primary weight-bearing bone of the lower leg, and its integrity is crucial for load sharing in midshaft tibia fractures.
Explanation:
Correct Answer: D
Explanation:
The case states that high-energy mechanisms are frequently associated with comminution, segmental defects, significant soft tissue compromise, and a higher propensity for open fractures (up to 30-40% in some series). It also notes a bimodal distribution, affecting young, active males involved in high-energy trauma. This directly supports option D.
- Option A is incorrect: While elderly individuals are affected by lower-energy falls, the bimodal distribution includes young, active males involved in high-energy trauma, which is the context of this question. The overall incidence is 16.9 per 100,000 person-years, but high-energy mechanisms are distinct.
- Option B is incorrect: The main blood supply to the tibial diaphysis is primarily from the nutrient artery (a branch of the posterior tibial artery). While periosteal vessels contribute, especially after trauma or reaming, the nutrient artery is the primary supply, and damage to it in high-energy injuries can impair healing.
- Option C is incorrect: The case explicitly states, 'The tibia has a precarious soft tissue envelope, particularly on its anteromedial surface, where it is largely subcutaneous.' This limited soft tissue coverage predisposes to open fractures and wound healing complications.
- Option E is incorrect: The case states, 'The tibia is the primary weight-bearing bone of the lower leg.' The fibula runs parallel and provides stability to the ankle joint, but is not the primary weight-bearing bone. While its integrity affects load sharing and rotational stability, its primary biomechanical importance is at the ankle and knee, not as the primary weight-bearer for the lower leg.
Question 2:
A 35-year-old construction worker sustains a high-energy closed midshaft tibia fracture after a fall from scaffolding. On presentation, he complains of severe pain, especially with passive dorsiflexion of the toes. His leg is tense to palpation, and sensation in the first web space is diminished. Which of the following neurovascular structures is most likely compromised in this scenario, and what is the immediate management?
- A: Superficial peroneal nerve; emergent surgical exploration and nerve repair.
- B: Posterior tibial artery; emergent CT angiogram to confirm injury.
- C: Deep peroneal nerve; emergent four-compartment fasciotomy.
- D: Tibial nerve; observation for neuropraxia and serial neurological exams.
- E: Peroneal artery; provisional external fixation followed by vascular repair.
Explanation:
Correct Answer: C
Explanation:
The clinical presentation of severe pain with passive stretch, tense compartment, and diminished sensation in the first web space (which is innervated by the deep peroneal nerve) are classic signs of acute compartment syndrome in the anterior compartment. The deep peroneal nerve and anterior tibial artery run in the anterior compartment. The case explicitly states that compartment syndrome is a surgical emergency requiring emergent fasciotomy.
- Option A is incorrect: The superficial peroneal nerve innervates the dorsum of the foot (except the first web space) and runs in the lateral compartment. While it can be injured, the specific symptoms point more strongly to the anterior compartment. Emergent surgical exploration for nerve repair is not the immediate management for compartment syndrome.
- Option B is incorrect: The posterior tibial artery runs in the deep posterior compartment. While vascular injury is a concern in high-energy trauma, the symptoms described are more indicative of compartment syndrome than a direct arterial transection, and emergent fasciotomy takes precedence over diagnostic imaging if compartment syndrome is clinically evident.
- Option D is incorrect: The tibial nerve runs in the deep posterior compartment. While nerve injury can occur, the constellation of symptoms (pain with passive stretch, tense compartment, specific sensory deficit) points to compartment syndrome, which requires immediate surgical intervention, not just observation.
- Option E is incorrect: The peroneal artery runs in the deep posterior compartment. Similar to option B, while vascular injury is a risk, the immediate concern with these symptoms is compartment syndrome, which requires fasciotomy, not just provisional fixation and vascular repair (unless a definitive vascular injury is confirmed and contributing to ischemia, which is not the primary presentation here).
Question 3:
A 62-year-old male presents with a Gustilo-Anderson Type IIIA open midshaft tibia fracture after being struck by a car. He has multiple other injuries, including a closed head injury and a pelvic fracture, but is hemodynamically stable after initial resuscitation. Based on the case guidelines, what is the most appropriate initial management strategy for his tibia fracture?
- A: Immediate definitive intramedullary nailing within 6 hours to achieve early total care.
- B: Non-operative management with serial casting and close monitoring for soft tissue healing.
- C: Emergent surgical debridement and provisional external fixation, followed by delayed definitive fixation.
- D: Primary plate osteosynthesis with autogenous bone grafting due to the open nature of the fracture.
- E: Delay all surgical intervention for 48-72 hours to allow for soft tissue swelling to subside.
Explanation:
Correct Answer: C
Explanation:
The case explicitly states, 'For Gustilo I, II, IIIA fractures, thorough surgical debridement of all contaminated and devitalized tissue is paramount. Pulsatile lavage. Repeat debridement ('second look') after 24-48 hours may be necessary.' It also highlights 'Damage Control Orthopedics (DCO): For unstable polytrauma patients or those with severe soft tissue swelling/compromise, provisional external fixation is performed first. Definitive fixation (usually IM nailing) is delayed until the patient is physiologically stable and soft tissue swelling has subsided (typically 5-10 days, but can be longer).' Given the Gustilo IIIA open fracture and polytrauma status, emergent debridement and provisional external fixation are the most appropriate initial steps.
- Option A is incorrect: While early total care (ETC) is an option for isolated closed fractures, for open fractures, especially in polytrauma patients, the priority is debridement and provisional stabilization (DCO) to manage contamination and systemic inflammatory response, delaying definitive internal fixation.
- Option B is incorrect: Non-operative management is generally reserved for non-displaced or minimally displaced closed fractures, which is rare in high-energy trauma, and is absolutely contraindicated for open fractures.
- Option D is incorrect: While plate osteosynthesis can be used in some open fractures, it is not the primary initial management for a Gustilo IIIA fracture, which requires debridement and often provisional external fixation first. Autogenous bone grafting is typically delayed until soft tissue healing is complete or for non-unions.
- Option E is incorrect: Delaying all surgical intervention for an open fracture is contraindicated. Emergent debridement is critical to reduce infection risk.
Question 4:
A 40-year-old male presents with a high-energy midshaft tibia fracture. Pre-operative planning is underway. The trauma surgeon notes a concern for potential intra-articular extension at the knee, as well as significant comminution not fully appreciated on plain radiographs. Which imaging modality is most appropriate to address these specific concerns?
- A: Ankle-Brachial Index (ABI) measurement.
- B: Magnetic Resonance Imaging (MRI).
- C: Computed Tomography (CT) scan.
- D: Conventional angiography.
- E: Repeat plain radiographs with oblique views.
Explanation:
Correct Answer: C
Explanation:
The case states that a CT scan is 'Useful for identifying subtle intra-articular extension at the knee or ankle, which can influence fixation strategy' and for 'Detailed assessment of comminution, bone loss, and fracture geometry.' This directly addresses both concerns mentioned in the vignette.
- Option A is incorrect: ABI is used to assess vascular status, not fracture morphology or intra-articular extension.
- Option B is incorrect: MRI is rarely indicated acutely for fracture assessment but may be useful for ligamentous injury assessment at the knee/ankle if suspected post-reduction. It is not the primary modality for bone detail or comminution in the acute setting.
- Option D is incorrect: Conventional angiography is indicated if there is suspicion of vascular injury, not for assessing intra-articular extension or comminution.
- Option E is incorrect: While oblique views on plain radiographs can provide more information than AP/lateral views, they are still limited in assessing subtle intra-articular extension or complex comminution compared to a CT scan.
Question 5:
During intramedullary nailing of a midshaft tibia fracture, the surgeon is preparing the entry point. The image below demonstrates a common approach for proximal tibial entry. Which of the following statements accurately describes a key consideration for this step?

- A: The entry point should be lateral to the lateral tibial spine to avoid the patellar tendon.
- B: Suprapatellar entry is preferred in all cases to minimize anterior knee pain.
- C: The goal is to align the entry point with the central axis of the medullary canal in both AP and lateral planes.
- D: Reaming should always precede entry point preparation to ensure adequate canal size.
- E: The entry point is typically made through the medial collateral ligament to facilitate nail insertion.
Explanation:
Correct Answer: C
Explanation:
The case states, 'The choice of entry point is critical to avoid malalignment (especially apex anterior/posterior deformity or valgus/varus) and iatrogenic injury.' It further specifies, 'Once the entry point is identified on the proximal tibia (usually medial to the lateral tibial spine and lateral to the medial tibial spine, aligning with the intercondylar notch), an awl or drill is used to open the cortex. The goal is to align with the central axis of the medullary canal in both AP and lateral planes.' This directly supports option C.
- Option A is incorrect: The entry point is usually medial to the lateral tibial spine and lateral to the medial tibial spine, aligning with the intercondylar notch, not lateral to the lateral tibial spine. Splitting the patellar tendon centrally or paratendinously is a common approach.
- Option B is incorrect: While suprapatellar nailing is a technique that may reduce anterior knee pain, the case describes it as 'a more recent technique' and does not state it is preferred in all cases. Patellar ligament splitting is also a common approach.
- Option D is incorrect: Entry point preparation (opening the cortex) always precedes reaming. Reaming is the sequential enlargement of the medullary canal after the entry point is established.
- Option E is incorrect: The entry point is made on the proximal tibia, typically through or adjacent to the patellar tendon, not through the medial collateral ligament, which is a knee stabilizer.
Question 6:
A 50-year-old male with a closed, comminuted midshaft tibia fracture is undergoing intramedullary nailing. The surgeon is debating between reamed and unreamed nailing. The patient has no other significant comorbidities, and soft tissue swelling is minimal. Based on the case, which approach is generally preferred for this type of fracture in this patient, and why?
- A: Unreamed nailing, because it preserves endosteal blood supply and reduces the risk of fat embolism.
- B: Reamed nailing, because it allows for a larger, stiffer nail, providing greater stability and enhancing callus formation.
- C: Unreamed nailing, because it is preferred for Gustilo II and IIIA open fractures to avoid spreading contamination.
- D: Reamed nailing, because it is associated with lower rates of anterior knee pain post-operatively.
- E: Unreamed nailing, because it is less technically demanding and faster to perform.
Explanation:
Correct Answer: B
Explanation:
The case states, 'Reamed intramedullary nailing is the gold standard for diaphyseal tibia fractures due to superior union rates, lower reoperation rates, and faster time to union compared to plating or casting for most patterns.' Under 'Reamed Nailing,' it lists advantages: 'Maximizes nail-to-bone contact, allowing for a larger diameter and stiffer nail, which provides greater rotational and bending stability. Enhances primary callus formation.' This aligns with the scenario of a closed, comminuted fracture in a healthy patient where stability and union are paramount.
- Option A is incorrect: While unreamed nailing does preserve endosteal blood supply and has a lower risk of fat embolism, the case indicates that reamed nailing is generally preferred for closed fractures due to superior stability and union rates.
- Option C is incorrect: Unreamed nailing is indeed preferred for Gustilo II and IIIA open fractures to avoid spreading contamination, but the patient in the vignette has a closed fracture.
- Option D is incorrect: The case mentions that anterior knee pain is a common complication of IM nailing, but it does not state that reamed nailing specifically is associated with lower rates of anterior knee pain. In fact, suprapatellar nailing techniques are discussed as potentially reducing this incidence, not reaming itself.
- Option E is incorrect: The case does not suggest that unreamed nailing is less technically demanding or faster. The choice between reamed and unreamed is based on biomechanical and biological considerations, not ease of performance.
Question 7:
A 22-year-old male presents with a high-energy midshaft tibia fracture with significant comminution and a wide medullary canal, making stable reduction challenging. The surgeon decides to use an adjunct technique to improve alignment and prevent malreduction during intramedullary nailing. The image below illustrates a technique that could be employed in this situation. Which of the following adjuncts is most appropriate for this scenario?

- A: Cerclage wires to compress all comminuted fragments around the nail.
- B: Bone grafting at the fracture site prior to nail insertion.
- C: Blocking screws (Poller screws) to guide the nail into the correct position.
- D: A temporary external fixator for definitive fixation.
- E: Plate osteosynthesis as the primary fixation method.
Explanation:
Correct Answer: C
Explanation:
The case states, 'Blocking screws (Poller Screws): Small cortical screws placed adjacent to the IM nail track to guide the nail into the correct position, preventing malalignment in specific planes (e.g., apex anterior/posterior, valgus/varus). Especially useful for metadiaphyseal fractures or wide medullary canals.' This directly matches the clinical scenario of a wide medullary canal and challenging reduction.
- Option A is incorrect: The case states, 'Cerclage Wires: Rarely used for midshaft diaphyseal fractures due to disruption of periosteal blood supply, but may be considered for large butterfly fragments that are difficult to reduce or stabilize. Use sparingly and with caution.' This suggests they are not the most appropriate primary adjunct for general comminution and wide canals.
- Option B is incorrect: Bone grafting is typically used for bone loss, delayed union, or non-union, often delayed until soft tissue healing is complete. It is not an adjunct for achieving acute reduction and alignment during IM nailing.
- Option D is incorrect: A temporary external fixator can assist with reduction, but it is typically used for provisional stabilization in damage control orthopedics or severe open fractures, not as a definitive fixation method in this context, nor is it the specific adjunct for guiding the nail in a wide canal.
- Option E is incorrect: Plate osteosynthesis is an alternative fixation method, not an adjunct to IM nailing, and is generally a secondary option for midshaft diaphyseal tibia fractures.
Question 8:
A 48-year-old male undergoes intramedullary nailing for a high-energy closed midshaft tibia fracture. Post-operatively, he develops increasing pain, swelling, and paresthesia in the foot. On examination, his foot is cool, and pedal pulses are diminished. Which of the following is the most critical early complication to rule out, and what is its immediate management?
- A: Deep vein thrombosis (DVT); initiate anticoagulation.
- B: Fat embolism syndrome (FES); provide supportive care and ventilatory support.
- C: Acute compartment syndrome; emergent four-compartment fasciotomy.
- D: Vascular injury; emergent vascular surgery consultation and repair.
- E: Infection; start broad-spectrum intravenous antibiotics.
Explanation:
Correct Answer: D
Explanation:
The symptoms of increasing pain, swelling, paresthesia, a cool foot, and diminished pedal pulses are highly suggestive of acute vascular compromise (e.g., laceration, transection, or thrombosis of major arteries). The case lists 'Vascular Injury' as an early complication, describing it as 'Laceration, transection, or thrombosis of major arteries (anterior/posterior tibial, peroneal). Presents as pulselessness, pallor, cold extremity.' The management is 'Emergent vascular surgery consultation and repair (bypass or primary repair).' While compartment syndrome can present similarly, the diminished pulses and cool extremity strongly point to a primary vascular injury requiring immediate repair to prevent limb loss.
- Option A is incorrect: DVT typically presents with swelling and pain, but usually not with a cool extremity or diminished pulses, which are signs of arterial insufficiency.
- Option B is incorrect: FES presents with a triad of respiratory insufficiency, neurological dysfunction, and petechial rash, not primarily with localized limb ischemia.
- Option C is incorrect: While acute compartment syndrome is a critical early complication, the presence of diminished pulses and a cool extremity makes vascular injury a more immediate and limb-threatening concern that must be addressed first. Compartment syndrome can be secondary to vascular injury, but the primary issue here is arterial flow.
- Option E is incorrect: Infection is a later complication unless it's an open fracture, and its acute presentation would not typically include a cool extremity and diminished pulses.
Question 9:
A 30-year-old male undergoes intramedullary nailing for a high-energy midshaft tibia fracture. Six months post-operatively, he complains of persistent pain around the knee, particularly with kneeling and stair climbing. Radiographs confirm union of the fracture, and the image below shows a typical final IM nail construct. What is the most likely diagnosis for his persistent knee pain, and what is the recommended management?
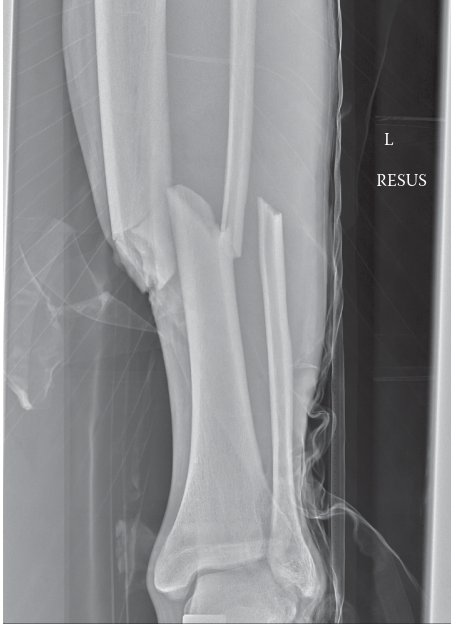
- A: Aseptic hypertrophic non-union; revision surgery with exchange nailing.
- B: Malunion; corrective osteotomy and internal fixation.
- C: Anterior knee pain post-IM nailing; physical therapy and potential hardware removal after complete union.
- D: Hardware failure; revision surgery with a new implant.
- E: Chronic regional pain syndrome (CRPS); sympathetic nerve block.
Explanation:
Correct Answer: C
Explanation:
The case specifically addresses 'Anterior Knee Pain Post-IM Nailing' as a common late complication, stating, 'Up to 50% of patients experience anterior knee pain after IM nailing of the tibia.' It describes the etiology as multifactorial and the management as 'While common, hardware removal for symptomatic pain is often effective, but should be delayed until complete union.' The vignette describes persistent knee pain after confirmed union, which is characteristic of this complication.
- Option A is incorrect: Non-union implies failure of fracture healing, but the vignette states radiographs confirm union.
- Option B is incorrect: Malunion implies the fracture healed in an unacceptable position, which is not indicated by the symptoms of knee pain after union.
- Option D is incorrect: Hardware failure would typically be associated with pain at the fracture site or loss of reduction, and the radiographs confirm union, making hardware failure less likely to be the primary cause of isolated anterior knee pain.
- Option E is incorrect: CRPS is a complex pain syndrome with distinct features (e.g., allodynia, trophic changes) not fully described in the vignette, and while possible, anterior knee pain post-IM nailing is a much more common and specific diagnosis in this context.
Question 10:
A 55-year-old female with a high-energy midshaft tibia fracture treated with reamed intramedullary nailing is 8 weeks post-operative. Radiographs show early callus formation, and she has good pain control. According to the post-operative rehabilitation protocols, what is the most appropriate progression for her weight-bearing status at this stage?
- A: Continue strict non-weight bearing (NWB) until full cortical bridging is evident.
- B: Initiate full weight bearing as tolerated (FWBAT) immediately to promote bone healing.
- C: Progress from non-weight bearing (NWB) or touch-down weight bearing (TDWB) to protected weight bearing (PWB) or weight bearing as tolerated (WBAT).
- D: Begin plyometric exercises to strengthen the quadriceps and calf muscles.
- E: Remove all assistive devices and encourage independent ambulation.
Explanation:
Correct Answer: C
Explanation:
The case's 'Phase 2 Early Mobilization & Progressive Loading (Weeks 6-12)' section states, 'Weight Bearing: Progress from NWB/TDWB to PWB/WBAT as radiological signs of healing (early callus formation) become evident and pain allows. Regular follow-up radiographs (every 4-6 weeks) guide progression.' The patient is 8 weeks post-op with early callus, fitting this phase.
- Option A is incorrect: Continuing strict NWB until full cortical bridging is too conservative for this stage, especially with early callus formation and good pain control.
- Option B is incorrect: Initiating FWBAT immediately is too aggressive. FWBAT is typically achieved later, once clinical and radiographic union are confirmed (Phase 3).
- Option D is incorrect: Plyometric exercises are part of 'Phase 3 Advanced Strengthening & Return to Activity (Weeks 12+)' and are too aggressive for 8 weeks post-op.
- Option E is incorrect: Removing all assistive devices and encouraging independent ambulation is part of later stages of rehabilitation (Phase 3), after significant progression in strength and confidence.
Question 11:
A 70-year-old male with a history of smoking and peripheral vascular disease sustains a high-energy Gustilo-Anderson Type IIIA open midshaft tibia fracture. He undergoes emergent debridement and provisional external fixation. Based on the summary of key literature and guidelines, which of the following statements regarding his definitive management and potential complications is most accurate?
- A: Unreamed intramedullary nailing is the gold standard for Gustilo IIIA open fractures to maximize stability and union rates.
- B: Delayed definitive soft tissue coverage beyond 7 days for Gustilo IIIB/IIIC fractures has been shown to reduce infection rates.
- C: Exchange nailing is a highly effective treatment for aseptic hypertrophic non-unions.
- D: Prophylactic autogenous bone grafting is routinely indicated for highly comminuted open fractures to prevent non-union.
- E: Early total care (ETC) with definitive internal fixation within 24-48 hours is preferred for all open tibia fractures.
Explanation:
Correct Answer: C
Explanation:
The 'Summary of Key Literature / Guidelines' section states, 'Exchange nailing is a highly effective treatment for aseptic hypertrophic non-unions.' This is a well-established principle in orthopedic trauma.
- Option A is incorrect: While unreamed nailing is often favored for Gustilo IIIA/B open fractures to minimize infection spread and preserve endosteal blood supply, the case states that 'Reamed nailing generally results in higher union rates and stronger constructs than unreamed nailing, particularly in closed and Gustilo I/II open fractures.' For Gustilo IIIA/B, the choice is more nuanced, and unreamed is chosen for infection control, not necessarily for maximizing stability and union rates compared to reamed nailing in general. Reamed nailing is the gold standard for diaphyseal tibia fractures overall, but unreamed has specific indications for open fractures.
- Option B is incorrect: The case states, 'For Gustilo IIIB/IIIC fractures, early definitive soft tissue coverage (within 7 days) by plastic surgery has been shown to reduce infection rates and improve outcomes.' Therefore, delaying beyond 7 days would increase, not reduce, infection rates.
- Option D is incorrect: The case states, 'Prophylactic grafting for highly comminuted open fractures is controversial but may be considered for large segmental defects.' It is not routinely indicated.
- Option E is incorrect: The case states, 'For polytrauma patients or those with severe soft tissue swelling, provisional external fixation followed by delayed definitive internal fixation (typically within 5-10 days) is supported by evidence to reduce systemic inflammatory response and improve outcomes ('early appropriate care').' This is Damage Control Orthopedics (DCO), which is often preferred for open fractures, especially in polytrauma patients, over Early Total Care (ETC).
Question 12:
A 38-year-old male presents with a high-energy proximal tibial diaphyseal fracture. His medical history includes Type 2 Diabetes Mellitus (HbA1c 6.8%) and a 15 pack-year smoking history.
Considering these comorbidities, which of the following is the MOST significant anticipated complication directly related to the patient's biological healing cascade and perioperative risk?
- A: Acute kidney injury
- B: Deep vein thrombosis
- C: Delayed union or nonunion
- D: Pulmonary embolism
- E: Myocardial infarction
Explanation:
Correct Answer: C
The case explicitly states that the patient's Type 2 Diabetes Mellitus and 15 pack-year smoking history significantly elevate the risk of delayed union, nonunion, and surgical site infection. Diabetes inherently alters bone microarchitecture and impairs cellular responses to trauma, while smoking induces profound peripheral vasoconstriction and tissue hypoxia. These factors directly compromise the biological healing cascade. While other complications listed are possible in trauma patients, delayed union or nonunion is the most directly and significantly impacted by the patient's specific comorbidities as described in the case.
Question 13:
The patient's right lower extremity exhibits gross clinical deformity, significant non-pitting edema, and ecchymosis. The skin integrity is closed, but there is deep muscle contusion and moderate to severe abrasion. The compartments are tense but compressible. Pain with passive stretch of the ischemic muscles is noted but not deemed disproportionate.
Based on these findings, what is the most appropriate Tscherne classification for the closed soft tissue injury, and what is the critical diagnostic threshold for acute compartment syndrome in this patient?
- A: Tscherne Grade 0; Absolute intracompartmental pressure > 30 mmHg
- B: Tscherne Grade 1; Delta P (diastolic BP - intracompartmental pressure) < 40 mmHg
- C: Tscherne Grade 2; Delta P (diastolic BP - intracompartmental pressure) < 30 mmHg
- D: Tscherne Grade 3; Absolute intracompartmental pressure > 45 mmHg
- E: Tscherne Grade 2; Absolute intracompartmental pressure > 30 mmHg
Explanation:
Correct Answer: C
The case describes the soft tissue envelope as exhibiting signs of severe contusion, deep muscle contusion, and moderate to severe abrasion, which is explicitly stated as consistent with a Tscherne Grade 2 closed soft tissue injury. Regarding acute compartment syndrome, the case specifies that a Delta P calculation (diastolic blood pressure minus intracompartmental pressure) of less than 30 mmHg would serve as the absolute indication for emergent four-compartment fasciotomies. Therefore, option C accurately reflects both the Tscherne classification and the critical diagnostic threshold for compartment syndrome as detailed in the case.
Question 14:
Review the provided radiograph of the patient's right lower extremity.
Based on the case and the provided image, which of the following best describes the fracture pattern and associated deformity?
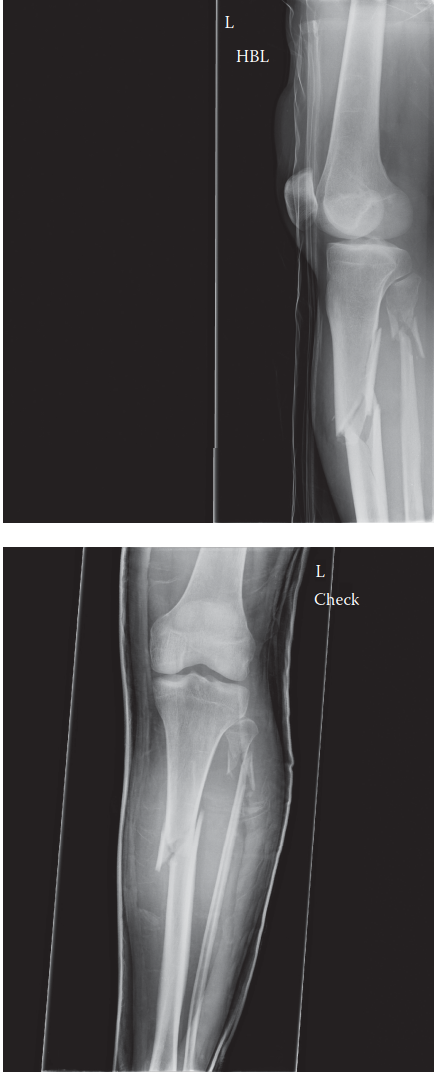
- A: Distal third spiral fracture with apex posterior angulation.
- B: Mid-diaphyseal transverse fracture with minimal displacement.
- C: Proximal third comminuted oblique fracture with apex anterior and valgus angulation.
- D: Pilon fracture with significant intra-articular involvement.
- E: Isolated fibula fracture with an intact tibia.
Explanation:
Correct Answer: C
The case explicitly states: 'Radiographic analysis of the right lower extremity revealed a severely displaced, comminuted fracture of the proximal third of the tibial diaphysis. The fracture pattern exhibited a dominant oblique configuration with a large, laterally displaced butterfly fragment... with significant apex anterior (procurvatum) and apex lateral (valgus) angulation.' The provided image clearly demonstrates these features, showing a fracture in the proximal third of the tibia with multiple fragments (comminuted), an oblique component, and the characteristic apex anterior and valgus angulation. Options A, B, D, and E describe different fracture locations, patterns, or severities that are inconsistent with both the image and the detailed description in the case.
Question 15:
The patient's proximal tibial diaphyseal fracture exhibits significant apex anterior (procurvatum) and apex lateral (valgus) angulation.
Which of the following anatomical structures is primarily responsible for the apex anterior (procurvatum) deformity observed in proximal third tibial fractures?
- A: Gastrocnemius muscle
- B: Soleus muscle
- C: Extensor mechanism (quadriceps via patellar tendon)
- D: Pes anserinus
- E: Iliotibial band
Explanation:
Correct Answer: C
The case specifically addresses the deforming forces in proximal third tibial fractures: 'This specific deformity pattern is classic for proximal third tibial fractures and is driven by the unopposed pull of the extensor mechanism (quadriceps via the patellar tendon) on the proximal fragment, drawing it into extension, while the pes anserinus and iliotibial band exert variable varus/valgus and rotational forces.' The extensor mechanism, primarily through the patellar tendon, pulls the proximal fragment anteriorly, creating the apex anterior (procurvatum) deformity. The other options are either not the primary deforming force for procurvatum or contribute more to other deformities (e.g., pes anserinus and iliotibial band for varus/valgus).
Question 16:
Following plain radiographs, a dedicated computed tomography (CT) scan of the right knee and proximal tibia with fine axial cuts and multiplanar reconstructions was ordered for this patient.
What is the MOST critical reason for obtaining a CT scan in a high-energy proximal third tibial shaft fracture, even if plain radiographs appear to show an extra-articular injury?
- A: To assess the integrity of the distal tibiofibular syndesmosis.
- B: To quantify the degree of soft tissue edema and contusion.
- C: To identify occult intra-articular extension into the tibial plateau.
- D: To evaluate for concomitant popliteal artery injury.
- E: To determine the exact length and diameter of the intramedullary canal for templating.
Explanation:
Correct Answer: C
The case emphasizes the importance of the CT scan: 'While plain radiographs provide the macroscopic architecture of the diaphyseal injury, they are notoriously insensitive for detecting occult intra-articular extension into the tibial plateau. Literature indicates that up to 20% to 30% of high-energy proximal third tibial shaft fractures possess an unrecognized coronal or sagittal split propagating into the articular surface. The presence of an intra-articular component drastically alters the surgical algorithm...' Therefore, the primary and most critical reason for the CT scan in this context is to rule out occult intra-articular extension, which would fundamentally change the surgical approach. While templating (E) is a benefit, it's not the most critical reason for the CT in terms of altering the fundamental treatment strategy for an articular injury.
Question 17:
The patient has a closed, comminuted proximal third tibial diaphyseal fracture (AO/OTA 42-B3, Tscherne Grade 2) and a history of Type 2 Diabetes and smoking. Surgical stabilization is indicated.
Considering the patient's fracture characteristics and comorbidities, which surgical fixation method is generally considered the gold standard and offers the most biomechanical advantages for this specific injury, while mitigating risks associated with his medical history?
- A: Long-leg casting for 12 weeks.
- B: External fixation as a definitive treatment.
- C: Minimally Invasive Percutaneous Plate Osteosynthesis (MIPPO).
- D: Intramedullary Nailing (IMN).
- E: Open Reduction Internal Fixation (ORIF) with a single anterior plate.
Explanation:
Correct Answer: D
The case explicitly states: 'Intramedullary Nailing (IMN) remains the gold standard for tibial diaphyseal fractures. It is a load-sharing device that preserves the extraosseous blood supply, offers superior biomechanical stability against bending and torsional forces, and allows for earlier weight-bearing.' It also discusses the disadvantages of plating (MIPPO or ORIF with plates) in this context, noting that 'plating the tibia, particularly on the subcutaneous anteromedial surface, requires significant soft tissue stripping... and introduces bulky hardware under a traumatized soft tissue envelope, significantly increasing the risk of wound dehiscence and deep infection.' This risk is particularly relevant for a diabetic, smoking patient with impaired healing. Non-operative management (A) is contraindicated for this high-energy, displaced fracture, and external fixation (B) is generally reserved for damage control or severe open fractures, not definitive treatment in a stable, closed injury.
Question 18:
The surgical plan for this patient involves a Suprapatellar Intramedullary Nailing technique.
What is the primary biomechanical advantage of utilizing a suprapatellar approach for intramedullary nailing of a proximal tibial diaphyseal fracture, compared to a traditional infrapatellar approach?
- A: It allows for easier distal interlocking.
- B: It completely eliminates the need for blocking screws.
- C: It reduces tension on the extensor mechanism, thereby neutralizing the primary deforming force causing procurvatum.
- D: It provides direct visualization of the fracture site.
- E: It significantly reduces the risk of acute compartment syndrome.
Explanation:
Correct Answer: C
The case highlights the key advantage of the suprapatellar approach: 'The critical advantage of the suprapatellar approach is patient positioning. The limb is positioned with the knee in a semi-extended posture, resting on a sterile bump at approximately 15 to 20 degrees of flexion. This semi-extended position dramatically reduces the tension on the extensor mechanism, neutralizing the primary deforming force that causes procurvatum.' This directly addresses the common challenge of apex anterior deformity in proximal tibial nailing. Options A, B, D, and E are incorrect; distal interlocking is not inherently easier, blocking screws are still often necessary, direct visualization of the fracture is not achieved, and it does not significantly reduce the risk of compartment syndrome compared to other approaches.
Question 19:
During the intramedullary nailing of this patient's proximal tibial fracture, blocking screws (Poller screws) were strategically placed in the proximal fragment.
To prevent the classic apex anterior (procurvatum) and valgus malalignment, where should the blocking screws be placed in the proximal fragment relative to the anticipated nail trajectory?
- A: Anteriorly to prevent procurvatum, and medially to prevent valgus.
- B: Posteriorly to prevent procurvatum, and laterally to prevent valgus.
- C: Anteriorly to prevent valgus, and medially to prevent procurvatum.
- D: Posteriorly to prevent valgus, and laterally to prevent procurvatum.
- E: Two screws placed directly anterior and posterior to the nail to prevent rotation.
Explanation:
Correct Answer: B
The case provides precise guidance on blocking screw placement: 'To prevent the classic valgus and procurvatum deformity, two blocking screws were placed in the proximal fragment. One screw was placed in the posterior half of the proximal fragment (viewed laterally) to block the nail from translating posteriorly, thereby preventing procurvatum. A second screw was placed in the lateral half of the proximal fragment (viewed on AP) to prevent the nail from translating laterally, thereby preventing valgus.' Blocking screws are placed on the concave side of the deformity to guide the nail centrally. For procurvatum (apex anterior), the nail tends to go posterior, so a posterior screw blocks this. For valgus (apex lateral), the nail tends to go lateral, so a lateral screw blocks this.
Question 20:
During the intramedullary nailing procedure, sequential flexible reaming was performed.
What is a recognized benefit of sequential flexible reaming during intramedullary nailing of a tibial diaphyseal fracture?
- A: It directly reduces the fracture fragments.
- B: It decreases the risk of fat embolization syndrome.
- C: It generates autologous bone graft (osteogenic reamings) that promotes secondary bone healing.
- D: It allows for a smaller diameter nail to be used.
- E: It eliminates the need for fluoroscopic guidance.
Explanation:
Correct Answer: C
The case states: 'Sequential flexible reaming was performed in 0.5-millimeter increments. Reaming generates autologous bone graft (osteogenic reamings) that is deposited at the fracture site, promoting secondary bone healing.' This is a well-known biological advantage of reamed nailing. Reaming does not directly reduce the fracture (A), it can actually increase the risk of fat embolization (B), it allows for a larger diameter nail (D), and fluoroscopic guidance is still essential (E).
Question 21:
Following intramedullary nailing for the proximal tibial diaphyseal fracture, the patient is in the immediate postoperative period.
What is the MOST critical immediate postoperative concern that requires extreme vigilance and hourly monitoring in this patient?
- A: Deep vein thrombosis (DVT)
- B: Surgical site infection (SSI)
- C: Delayed union
- D: Delayed acute compartment syndrome
- E: Hardware failure
Explanation:
Correct Answer: D
The case explicitly states: 'The immediate postoperative period requires extreme vigilance for the development of delayed acute compartment syndrome. The trauma of reaming and nail insertion introduces additional volume and inflammatory mediators into the closed fascial spaces. The patient was admitted to the orthopedic trauma unit with strict instructions for hourly neurovascular and compartment checks for the first 24 hours.' While DVT, SSI, delayed union, and hardware failure are all potential complications, delayed acute compartment syndrome is the most immediate, life-threatening, and limb-threatening complication requiring hourly monitoring in the immediate postoperative period, as emphasized in the case.
Question 22:
A 28-year-old male presents to the trauma center after a high-energy motor vehicle collision, sustaining an open right tibial diaphyseal fracture. Despite initial hemodynamic stability and palpable distal pulses, he develops excruciating, unremitting pain in his right lower leg, rated 10/10 on the VAS, unresponsive to high-dose opioids. Clinical examination reveals a tense, 'wood-hard' anterior compartment. Which of the following is the MOST sensitive and specific clinical finding for diagnosing acute compartment syndrome in this patient?
- A: A. Absence of distal pulses (dorsalis pedis and posterior tibial)
- B: B. Pallor and poikilothermia of the affected limb
- C: C. Severe pain with passive plantarflexion of the ankle and passive flexion of the great toe
- D: D. Paresthesia in the distribution of the superficial peroneal nerve
- E: E. Gross deformity and crepitus at the fracture site
Explanation:
Correct Answer: C
Explanation:
The most sensitive and specific clinical finding for diagnosing acute compartment syndrome (ACS) is severe pain with passive stretch of the muscles within the affected compartment, which is disproportionate to the injury and unrelieved by analgesia. In this case, passive plantarflexion of the ankle and passive flexion of the great toe selectively stretch the muscles of the anterior compartment (tibialis anterior, extensor hallucis longus, extensor digitorum longus), eliciting excruciating pain. This is a hallmark sign of ACS.
- A. Absence of distal pulses (dorsalis pedis and posterior tibial): Pulselessness is a very late and unreliable sign of ACS. Peripheral pulses are often maintained until intra-compartmental pressure exceeds systolic arterial pressure, which signifies irreversible damage. The case explicitly states that distal pulses remained robust and palpable, highlighting this pitfall.
- B. Pallor and poikilothermia of the affected limb: These are classic signs of acute arterial occlusion/ischemia, not typically ACS. In ACS, the limb is often warm due to the hyperemic response of early tissue distress, and pallor is not a primary feature until very late stages.
- D. Paresthesia in the distribution of the superficial peroneal nerve: While sensory changes (paresthesia, diminished two-point discrimination) are important signs of nerve ischemia in ACS, they are generally considered less sensitive and specific than pain with passive stretch, and often represent a more advanced stage of nerve compromise. The case describes this as altered sensation progressing to early paresthesia, indicating it's an evolving sign.
- E. Gross deformity and crepitus at the fracture site: Gross deformity and crepitus are expected findings with a displaced tibial fracture. They are indicative of the fracture itself, not specifically acute compartment syndrome. While the fracture is the inciting event, these findings do not differentiate between a simple fracture and one complicated by ACS.
Question 23:
The patient's clinical presentation, including escalating pain, tense compartments, and severe pain with passive stretch, led to a clinical diagnosis of acute compartment syndrome. Given the high-energy mechanism and open fracture, which of the following conditions would be the MOST critical to differentiate from acute compartment syndrome, and what specific finding in this case helped rule it out?
- A: A. Deep Vein Thrombosis (DVT); absence of Homan's sign
- B: B. Necrotizing Fasciitis; absence of crepitus and systemic toxicity
- C: C. Acute Arterial Occlusion; presence of palpable distal pulses and brisk capillary refill
- D: D. Severe Fracture Pain; pain unresponsive to high-dose opioids and disproportionate to injury
- E: E. Peripheral Neuropathy; intact light touch sensation in multiple nerve distributions
Explanation:
Correct Answer: C
Explanation:
In the setting of high-energy trauma to an extremity, acute arterial occlusion is a limb-threatening emergency that must be rapidly differentiated from acute compartment syndrome. Both can present with severe pain and potential neurological deficits. However, the case explicitly states that the dorsalis pedis and posterior tibial pulses remained robust and palpable, and capillary refill was brisk (<2 seconds). This strongly rules out a major arterial occlusion as the primary pathology.
- A. Deep Vein Thrombosis (DVT); absence of Homan's sign: DVT typically presents with generalized swelling, dull aching pain, and erythema, usually developing over a longer period (hours to days) than the acute timeline of this injury. While Homan's sign is unreliable, the acute onset and localized compartment tenseness are inconsistent with DVT.
- B. Necrotizing Fasciitis; absence of crepitus and systemic toxicity: Necrotizing fasciitis is a severe soft tissue infection. While it causes severe pain, it is typically accompanied by systemic signs of sepsis (fever, tachycardia), crepitus (indicating gas-forming organisms), and hemorrhagic bullae, which were not present in this acute setting.
- D. Severe Fracture Pain; pain unresponsive to high-dose opioids and disproportionate to injury: While severe fracture pain is a differential, the key differentiating factor from ACS is that fracture pain is usually proportional to the injury and improves with immobilization and analgesia. The patient's pain was 'excruciating, unremitting,' '10/10 on the VAS,' and 'completely unrelieved' by high-dose opioids, which strongly points away from isolated fracture pain and towards ACS. However, this option describes a finding that confirms ACS rather than ruling out a critical differential.
- E. Peripheral Neuropathy; intact light touch sensation in multiple nerve distributions: Peripheral neuropathy is a chronic condition and not an acute traumatic differential. While nerve injury can occur with trauma, the initial intact sensation followed by rapid deterioration points to an acute ischemic process, not a pre-existing neuropathy.
Question 24:
Given the patient's clear clinical signs of acute compartment syndrome, the decision was made to proceed directly to surgery without intra-compartmental pressure monitoring. However, in an equivocal case, such as an obtunded or polytraumatized patient, pressure monitoring would be indicated. Which of the following pressure measurements is the MOST reliable indicator for emergent fasciotomy?
- A: A. Absolute intra-compartmental pressure greater than 30 mmHg
- B: B. Absolute intra-compartmental pressure greater than 40 mmHg
- C: C. A Delta P (Diastolic Blood Pressure - Intra-compartmental Pressure) less than 30 mmHg
- D: D. A Delta P (Systolic Blood Pressure - Intra-compartmental Pressure) less than 30 mmHg
- E: E. A Delta P (Mean Arterial Pressure - Intra-compartmental Pressure) less than 40 mmHg
Explanation:
Correct Answer: C
Explanation:
The most reliable indicator for emergent fasciotomy, especially in equivocal cases or non-communicative patients, is the differential pressure (Delta P). Delta P is calculated as Diastolic Blood Pressure (DBP) minus the Intra-compartmental Pressure (ICP). A Delta P of less than 30 mmHg signifies inadequate tissue perfusion and is a widely accepted threshold for emergent fasciotomy. This metric accounts for the patient's systemic blood pressure, which is crucial because a hypotensive patient with a relatively low absolute compartment pressure can still be ischemic, while a hypertensive patient with a higher absolute compartment pressure might maintain adequate perfusion.
- A. Absolute intra-compartmental pressure greater than 30 mmHg: While often cited, relying solely on an absolute pressure threshold is a known pitfall. A patient with a DBP of 100 mmHg and an ICP of 35 mmHg (ΔP = 65 mmHg) may not require fasciotomy, whereas a patient with a DBP of 50 mmHg and an ICP of 25 mmHg (ΔP = 25 mmHg) is critically ischemic and requires intervention.
- B. Absolute intra-compartmental pressure greater than 40 mmHg: Similar to option A, this absolute threshold does not account for the patient's systemic blood pressure and is therefore less reliable than the Delta P.
- D. A Delta P (Systolic Blood Pressure - Intra-compartmental Pressure) less than 30 mmHg: While the concept of a differential pressure is correct, the standard and most widely accepted calculation for Delta P in the context of ACS uses Diastolic Blood Pressure, not Systolic Blood Pressure, as it more accurately reflects the pressure gradient for capillary perfusion.
- E. A Delta P (Mean Arterial Pressure - Intra-compartmental Pressure) less than 40 mmHg: While Mean Arterial Pressure (MAP) is a measure of overall perfusion, the established and validated threshold for Delta P in ACS specifically uses Diastolic Blood Pressure.
Question 25:
The patient underwent emergent dual-incision four-compartment fasciotomy and unreamed intramedullary nailing. The case highlights the critical time sensitivity of acute compartment syndrome. Skeletal muscle can tolerate ischemia for approximately 4 hours without permanent damage. Between 4 and 8 hours, irreversible myonecrosis and peripheral nerve damage begin to occur. Beyond 8 hours, the damage is essentially complete. What is the primary cellular mechanism underlying irreversible damage in acute compartment syndrome?
- A: A. Excessive calcium influx leading to muscle hypercontracture and rigor mortis
- B: B. Failure of the ATP-dependent Na+/K+ pump, leading to intracellular swelling and cell death
- C: C. Accumulation of lactic acid causing severe acidosis and enzyme denaturation
- D: D. Direct mechanical compression of muscle fibers leading to necrosis
- E: E. Reperfusion injury causing massive free radical production and inflammation
Explanation:
Correct Answer: B
Explanation:
The primary cellular mechanism underlying irreversible damage in acute compartment syndrome is the failure of the ATP-dependent Na+/K+ pump. As intra-compartmental pressure rises, it compromises capillary perfusion, leading to tissue ischemia and cellular hypoxia. Without adequate oxygen, cells cannot produce sufficient ATP through oxidative phosphorylation. The Na+/K+ pump, which actively transports sodium out of the cell and potassium into the cell, is highly ATP-dependent. Its failure leads to an accumulation of sodium and water inside the cell, causing intracellular swelling. This swelling further exacerbates the intra-compartmental pressure in a vicious cycle, ultimately leading to cell membrane rupture and myonecrosis.
- A. Excessive calcium influx leading to muscle hypercontracture and rigor mortis: While calcium dysregulation (influx of calcium) does occur in ischemic cells and contributes to muscle damage and hypercontracture, it is a downstream effect of the initial energy failure and membrane dysfunction, not the primary initiating mechanism of irreversible damage.
- C. Accumulation of lactic acid causing severe acidosis and enzyme denaturation: Lactic acid accumulation and acidosis are consequences of anaerobic metabolism during ischemia. While acidosis contributes to cellular dysfunction, the fundamental irreversible damage stems from the failure of ion pumps and subsequent cellular swelling and membrane integrity loss.
- D. Direct mechanical compression of muscle fibers leading to necrosis: While there is mechanical compression, the primary mechanism of damage is ischemic, not purely mechanical. The pressure impedes blood flow, leading to hypoxia, which then triggers the cellular cascade of pump failure and swelling.
- E. Reperfusion injury causing massive free radical production and inflammation: Reperfusion injury is a significant complication that occurs after fasciotomy when blood flow is restored to ischemic tissues. It involves the production of reactive oxygen species (free radicals) and inflammatory mediators, which can cause further tissue damage and systemic complications (e.g., rhabdomyolysis, acute kidney injury). However, it is not the mechanism of irreversible damage during the ischemic phase of ACS.
Question 26:
The patient underwent a dual-incision four-compartment fasciotomy. The surgical image below shows a typical anterolateral incision for fasciotomy. During the anterolateral incision, which nerve is at greatest risk of iatrogenic injury, and where is it typically located?

- A: A. Tibial nerve; deep posterior compartment, posterior to the tibialis posterior muscle
- B: B. Common peroneal nerve; wrapping around the fibular neck, proximal to the lateral compartment release
- C: C. Superficial peroneal nerve; exiting the lateral compartment fascia in the distal third of the leg
- D: D. Deep peroneal nerve; running with the anterior tibial artery in the anterior compartment
- E: E. Saphenous nerve; in the subcutaneous tissue along the posteromedial aspect of the leg
Explanation:
Correct Answer: C
Explanation:
During the anterolateral incision for fasciotomy, the superficial peroneal nerve is at greatest risk of iatrogenic injury. It typically exits the lateral compartment fascia to become subcutaneous in the distal third of the leg, approximately 10 to 12 cm proximal to the lateral malleolus. Care must be taken during the distal extension of the lateral compartment fascial release to identify and protect this nerve, as injury can lead to sensory loss over the lateral dorsum of the foot and potentially a painful neuroma.
- A. Tibial nerve; deep posterior compartment, posterior to the tibialis posterior muscle: The tibial nerve is located in the deep posterior compartment and is at risk during the posteromedial incision and deep posterior compartment release, not the anterolateral incision.
- B. Common peroneal nerve; wrapping around the fibular neck, proximal to the lateral compartment release: The common peroneal nerve is at risk during the proximal extension of the lateral compartment fascial release, particularly when incising near the fibular head. While important to protect, the superficial peroneal nerve is more commonly injured during the distal aspect of the anterolateral incision due to its superficial course.
- D. Deep peroneal nerve; running with the anterior tibial artery in the anterior compartment: The deep peroneal nerve is located within the anterior compartment. While it is important to avoid direct injury to this nerve during the anterior compartment release, it is generally less susceptible to iatrogenic injury from the fascial incision itself compared to the superficial peroneal nerve, which becomes subcutaneous.
- E. Saphenous nerve; in the subcutaneous tissue along the posteromedial aspect of the leg: The saphenous nerve is located in the subcutaneous tissue along the posteromedial aspect of the leg and is at risk during the posteromedial incision, not the anterolateral incision.
Question 27:
Following the emergent four-compartment fasciotomy, the open tibial fracture (Gustilo-Anderson Type II, OTA/AO 42-B3) required stabilization. The patient was physiologically stable. The surgical team opted for unreamed statically locked intramedullary nailing. Which of the following is the MOST compelling reason for choosing unreamed intramedullary nailing over spanning external fixation in this specific clinical scenario?
- A: A. External fixation is contraindicated in open fractures due to high infection rates.
- B: B. Unreamed intramedullary nailing provides superior biomechanical stability and avoids pin-tract complications, facilitating earlier definitive soft tissue coverage.
- C: C. Reamed intramedullary nailing is preferred for open fractures to enhance fracture healing.
- D: D. External fixation would further elevate intra-compartmental pressures after fasciotomy.
- E: E. Unreamed nailing allows for immediate full weight-bearing, accelerating rehabilitation.
Explanation:
Correct Answer: B
Explanation:
In a physiologically stable patient with an open tibial fracture and acute compartment syndrome, unreamed intramedullary nailing offers several advantages over external fixation. It provides superior biomechanical stability, which is crucial for fracture healing and allows for earlier mobilization. Furthermore, it avoids the complications associated with external fixator pin tracts, such as pin-tract infections, which can complicate subsequent definitive soft tissue coverage and potentially lead to osteomyelitis. The case explicitly states that modern trauma protocols often favor early definitive fixation with an unreamed IMN if the patient is physiologically stable, as it provides superior biomechanical stability and avoids pin-tract infections.
- A. External fixation is contraindicated in open fractures due to high infection rates: External fixation is a valid and often preferred method for initial stabilization of open fractures, especially in unstable patients (damage control orthopedics). While pin-tract infections are a concern, it is not an absolute contraindication for open fractures.
- C. Reamed intramedullary nailing is preferred for open fractures to enhance fracture healing: Reaming the medullary canal can further disrupt endosteal blood supply and potentially increase intra-compartmental pressures, especially in the context of recent fasciotomy. Therefore, unreamed nailing is generally preferred in open fractures and those complicated by ACS to minimize additional soft tissue and vascular insult.
- D. External fixation would further elevate intra-compartmental pressures after fasciotomy: External fixation itself does not typically elevate intra-compartmental pressures after a successful fasciotomy. The concern with external fixation relates more to pin-site issues and less stable fixation compared to IMN.
- E. Unreamed nailing allows for immediate full weight-bearing, accelerating rehabilitation: While IMN provides good stability, a comminuted diaphyseal fracture (OTA 42-B3) fixed with an unreamed nail typically requires a period of protected weight-bearing (e.g., touch-down weight-bearing for 6 weeks, as described in the case) to allow for callus formation and prevent implant failure. Immediate full weight-bearing is generally not advised.
Question 28:
The patient's postoperative course included aggressive intravenous fluid resuscitation to maintain a high urine output and monitoring of serum creatine kinase (CK) levels. This management strategy is primarily aimed at preventing which of the following complications?
- A: A. Deep vein thrombosis (DVT)
- B: B. Acute respiratory distress syndrome (ARDS)
- C: C. Acute kidney injury (AKI) secondary to rhabdomyolysis
- D: D. Compartment syndrome recurrence
- E: E. Wound infection and dehiscence
Explanation:
Correct Answer: C
Explanation:
Aggressive intravenous fluid resuscitation and monitoring of serum creatine kinase (CK) levels post-fasciotomy are critical for preventing acute kidney injury (AKI) secondary to rhabdomyolysis. Rhabdomyolysis is the breakdown of damaged muscle tissue, releasing myoglobin into the bloodstream. Myoglobin is nephrotoxic and can precipitate in the renal tubules, leading to acute tubular necrosis and AKI. Maintaining a high urine output helps to flush myoglobin through the renal tubules, while monitoring CK levels tracks the extent of muscle breakdown.
- A. Deep vein thrombosis (DVT): While DVT prophylaxis is important in trauma patients, aggressive fluid resuscitation is not its primary treatment or prevention strategy.
- B. Acute respiratory distress syndrome (ARDS): ARDS is a severe lung injury that can occur in polytrauma patients, but it is not directly addressed by fluid resuscitation for rhabdomyolysis.
- D. Compartment syndrome recurrence: Compartment syndrome recurrence is prevented by ensuring a complete fasciotomy and leaving the wounds open. While fluid management is crucial for systemic health, it does not directly prevent recurrence of local compartment pressure.
- E. Wound infection and dehiscence: Wound infection is managed with antibiotics, meticulous debridement, and proper wound care. Dehiscence is prevented by delayed primary closure or skin grafting when edema has resolved. Fluid resuscitation is not the primary intervention for these wound complications.
Question 29:
During the initial clinical examination, the patient demonstrated profound weakness in active dorsiflexion of the ankle and toe extension, with a rapid decline in motor strength from 3/5 to 1/5. Sensation was diminished in the first dorsal webspace. Which nerve is primarily affected by the acute compartment syndrome in this scenario, and what compartment does it innervate?
- A: A. Tibial nerve; superficial posterior compartment
- B: B. Superficial peroneal nerve; lateral compartment
- C: C. Deep peroneal nerve; anterior compartment
- D: D. Sural nerve; deep posterior compartment
- E: E. Saphenous nerve; medial compartment
Explanation:
Correct Answer: C
Explanation:
The deep peroneal nerve innervates the muscles of the anterior compartment of the leg, which are responsible for active dorsiflexion of the ankle (tibialis anterior) and toe extension (extensor hallucis longus, extensor digitorum longus). It also provides sensation to the first dorsal webspace. The described motor weakness and sensory deficit are classic signs of deep peroneal nerve compromise due to acute compartment syndrome in the anterior compartment.
- A. Tibial nerve; superficial posterior compartment: The tibial nerve innervates the superficial and deep posterior compartments, responsible for plantarflexion of the ankle and toe flexion. Its sensory distribution includes the sole of the foot.
- B. Superficial peroneal nerve; lateral compartment: The superficial peroneal nerve innervates the muscles of the lateral compartment (peroneus longus and brevis), which are responsible for active eversion of the ankle. Its sensory distribution is the lateral dorsum of the foot. While the case mentions altered sensation in this distribution, the profound motor weakness described points more strongly to the deep peroneal nerve.
- D. Sural nerve; deep posterior compartment: The sural nerve is a purely sensory nerve, providing sensation to the lateral aspect of the foot and ankle. It does not innervate any muscles.
- E. Saphenous nerve; medial compartment: The saphenous nerve is a purely sensory nerve, providing sensation to the medial aspect of the leg and foot. It does not innervate any muscles.
Question 30:
The patient sustained an open right tibial diaphyseal fracture. The laceration was 2 cm, without extensive soft tissue damage, avulsions, or degloving, and with adequate soft tissue coverage for the bone. Based on this description, what is the correct Gustilo-Anderson classification for this open fracture?
- A: A. Gustilo-Anderson Type I
- B: B. Gustilo-Anderson Type II
- C: C. Gustilo-Anderson Type IIIA
- D: D. Gustilo-Anderson Type IIIB
- E: E. Gustilo-Anderson Type IIIC
Explanation:
Correct Answer: B
Explanation:
The Gustilo-Anderson classification system categorizes open fractures based on the size of the wound, the extent of soft tissue damage, and the degree of contamination. In this case, the laceration was 2 cm, which is greater than 1 cm but without extensive soft tissue damage, avulsions, or degloving, and with adequate soft tissue coverage for the bone. This description perfectly matches the criteria for a Gustilo-Anderson Type II open fracture.
- A. Gustilo-Anderson Type I: Characterized by a wound less than 1 cm, with minimal soft tissue damage, and usually a clean wound.
- C. Gustilo-Anderson Type IIIA: Involves extensive soft tissue damage, but with adequate soft tissue coverage of the bone despite the damage. The wound is typically greater than 10 cm.
- D. Gustilo-Anderson Type IIIB: Characterized by extensive soft tissue damage with periosteal stripping and inadequate soft tissue coverage, requiring a flap for coverage.
- E. Gustilo-Anderson Type IIIC: Involves an arterial injury requiring repair, regardless of the size of the wound or the extent of soft tissue damage.
Question 31:
The case emphasizes a critical clinical pearl: 'Open fractures do not prevent compartment syndrome.' Which of the following statements best explains why an open tibial fracture, even with a visible laceration, does not reliably decompress the fascial compartments and prevent acute compartment syndrome?
- A: A. The fascial defect in an open fracture is rarely large enough to allow sufficient extrusion of hematoma and edematous muscle to lower intra-compartmental pressure below the ischemic threshold.
- B: B. Open fractures inherently cause more severe arterial injury, leading to compartment syndrome.
- C: C. The presence of an open wound increases the risk of infection, which directly causes compartment syndrome.
- D: D. Open fractures lead to systemic hypotension, which lowers the Delta P and precipitates compartment syndrome.
- E: E. The bone fragments in an open fracture directly compress the muscles, causing compartment syndrome regardless of fascial integrity.
Explanation:
Correct Answer: A
Explanation:
The statement 'Open fractures do not prevent compartment syndrome' is a crucial clinical pearl. The primary reason is that the fascial defect created by an open fracture, even if visible, is rarely large enough or strategically located to allow for sufficient decompression of the entire fascial compartment. The non-yielding osseous-fascial envelope remains largely intact, trapping the accumulating hematoma and edematous muscle, leading to a rise in intra-compartmental pressure above the ischemic threshold. The case explicitly states: 'The fascial defect is rarely large enough to allow sufficient extrusion of hematoma and edematous muscle to lower the intra-compartmental pressure below the ischemic threshold.'
- B. Open fractures inherently cause more severe arterial injury, leading to compartment syndrome: While severe open fractures can be associated with arterial injury (Gustilo-Anderson Type IIIC), this is not the inherent mechanism by which open fractures fail to prevent compartment syndrome. Compartment syndrome is a pressure-related phenomenon, not primarily an arterial injury.
- C. The presence of an open wound increases the risk of infection, which directly causes compartment syndrome: Infection (e.g., necrotizing fasciitis) can cause compartment syndrome, but this is a distinct pathology. The failure of an open fracture to decompress is a mechanical issue related to the fascial envelope, not primarily an infectious one.
- D. Open fractures lead to systemic hypotension, which lowers the Delta P and precipitates compartment syndrome: While systemic hypotension can lower the Delta P and make a patient more susceptible to ischemia at a given compartment pressure, open fractures do not inherently cause hypotension. The patient in this case was hemodynamically stable.
- E. The bone fragments in an open fracture directly compress the muscles, causing compartment syndrome regardless of fascial integrity: While displaced bone fragments can contribute to soft tissue injury and hematoma, the primary mechanism of compartment syndrome is the global increase in pressure within the fascial compartment, not direct compression by bone fragments. The fascial envelope's inability to expand is the key factor.
Question 32:
The patient's radiographs, shown below, revealed a displaced, comminuted fracture of the middle and distal third junction of the right tibial diaphysis, classified as an OTA/AO 42-B3. This was associated with a segmental fracture of the fibular diaphysis. What does the 'B3' in the OTA/AO classification for the tibia specifically indicate?
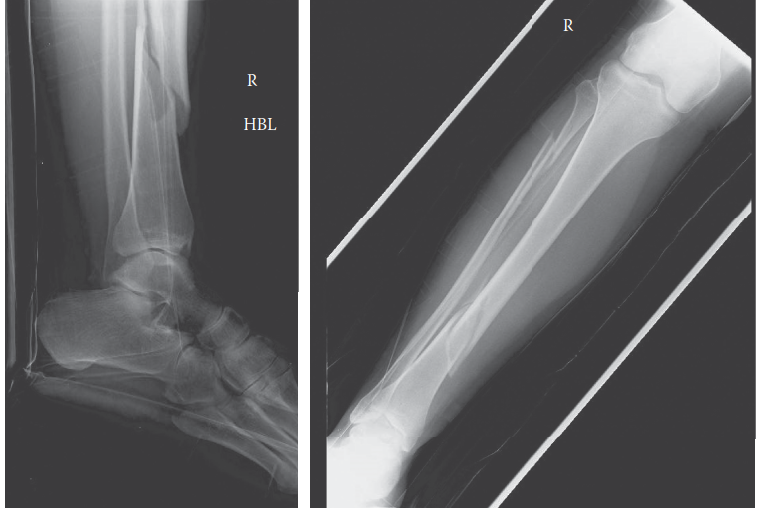
- A: A. A simple spiral fracture of the tibia
- B: B. A multifragmentary segmental fracture of the tibia
- C: C. A wedge fracture with a fragmented wedge
- D: D. A complex comminuted fracture with bone loss
- E: E. An intra-articular fracture extending into the ankle joint
Explanation:
Correct Answer: C
Explanation:
The OTA/AO classification system for long bone fractures is hierarchical. For the tibia (bone 4), diaphyseal fractures are group 2. The 'B' indicates a wedge fracture, meaning there is a third fragment (a wedge) that is still in contact with one of the main fragments after reduction. The '3' further specifies the type of wedge. A 'B3' fracture is a wedge fracture with a fragmented wedge, indicating a more comminuted and unstable wedge fragment compared to a simple wedge (B2).
- A. A simple spiral fracture of the tibia: A simple spiral fracture would typically be classified as an A1 fracture (simple, spiral).
- B. A multifragmentary segmental fracture of the tibia: A segmental fracture (two distinct fracture lines creating a free segment) would be classified as a C-type fracture (complex, multifragmentary).
- D. A complex comminuted fracture with bone loss: While the fracture is comminuted, 'bone loss' is not directly indicated by B3. Complex comminuted fractures are generally C-type fractures.
- E. An intra-articular fracture extending into the ankle joint: Intra-articular fractures are classified differently (e.g., 43-A, B, C for distal tibia). The '42' indicates a diaphyseal fracture, not an intra-articular one.
⚠️ Unanswered Questions
You have unanswered questions in this module. Are you sure you want to submit?
You Might Also Like
