Full Question & Answer Text (for Search Engines)
Question 1:
A 7-year-old boy has short stature, unilateral coxa vara, and lack of ossification in the medial pubic rami. The most likely diagnosis is:
Options:
- Achondroplasia
- Diastrophic dysplasia
- Osteogenesis imperfecta
- C leidocranial dysplasia
- Multiple epiphyseal dysplasia
Correct Answer: C leidocranial dysplasia
Explanation:
Cleidocranial dysplasia produces the above findings, in addition to partial or complete lack of formation of the clavicles and persistent widening of the cranial fontanelles. None of these findings are present in the other conditions.
Question 2:
An 11-year-old girl injures her knee while playing lacrosse and develops a hemarthrosis. The most likely diagnosis is:
Options:
- Anterior cruciate ligament tear
- Patellar dislocation
- Physeal injury of the distal femur
- Tibial spine avulsion
- Medial meniscus tear
Correct Answer: Patellar dislocation
Explanation:
The most common cause of hemarthrosis of the knee in skeletally immature patients is a patellar dislocation. Anterior cruciate ligament injuries and tibial spine avulsions are less common. Medial meniscus tears are extremely rare in this population.
Question 3:
In order to see the articular cartilage of the knee in a child who has knee trauma, a magnetic resonance image must include:
Options:
- T1-weighted images
- T2-weighted images
- Gradient echo sequences
- Gadolinium contrast
- Flexion and extension images
Correct Answer: Gradient echo sequences
Explanation:
Articular cartilage may be injured during trauma to the knee and manifest as either osteochondral fractures or osteochondritis dissecans. The articular cartilage is best visualized using gradient echo sequences. Examples of this technique include fast lowangle shot (FLASH) imaging, fast imaging with steady precession (FISP), and short tau inversion recovery (STIR).
Question 4:
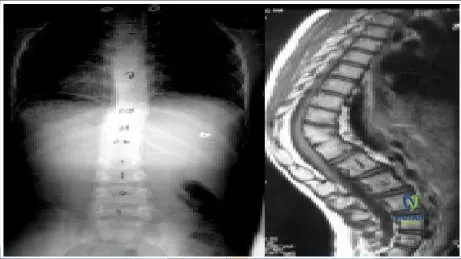
For a patient who has thoracic idiopathic scoliosis of the surgical range, the distance between the thecal sac and the apical thoracic pedicle on the concave side is:
Options:
- Less than 1 mm
- 2 mm
- 3 mm
- 4 mm
- 5 mm
Correct Answer: Less than 1 mm
Explanation:
The distance between the apical thoracic pedicle and the thecal sac is less than 1 mm on the concave side.
Question 5:
Which region (vertebral body) of the spine is the closest to the aorta:
Options:
Correct Answer: T1
Explanation:
The aorta is on the left side of the vertebra in the upper and midthoracic spine. The aorta moves to an anterior location in the lower thoracic spine. The distance from the aorta to the vertebral body is 6 mm to 7 mm in skeletally mature patients with idiopathic scoliosis between the fourth and ninth vertebral bodies. The distance becomes less than 5 mm in the thoracolumbar junction and lumbar spine. The aortic arch does not extend to the first thoracic vertebral.
Question 6:
The width of the pedicles in a patient with idiopathic scoliosis in the surgical range is narrowest in the:
Options:
- Thoracic spine on the convex side
- Lumbar spine on the convex side
- Sacral spine
- Thoracic spine on the concave side
- Lumbar spine on the concave side
Correct Answer: Thoracic spine on the convex side
Explanation:
The width of the pedicles is less in the thoracic spine than in the lumbar or sacral spine, and less on the concavity than on the convexity. The mean width of the thoracic pedicles on the concave side at the apex in skeletally mature patients is only 3 mm.
Question 7:
The angle of the pedicle with the midsagittal plane at T11 is closest to:
Options:
Correct Answer: 5°
Explanation:
The angle of the pedicles is greatest in the upper thoracic and lumbar spines (approximately 15°). The angle decreases to approximately 7° at the thoracolumbar junction.
Question 8:
Which of the following is not a common finding in the forearms of patients who have multiple hereditary exostoses:
Options:
- Radial head subluxation or dislocation
- Limitation of rotation
- Decreased slope of the distal radial articular surface
- Subluxation of the carpus toward the ulna
- Decreased length of the ulna
Correct Answer: Decreased slope of the distal radial articular surface
Explanation:
Multiple hereditary exostosis is characterized by differential growth of the two bones. There is often decreased length of the ulna. This results in increased inclination of the distal radial articular surface, radial head subluxation, and subluxation of the carpus toward the ulna. The exostoses themselves may block rotation.
Question 9:
Which of the following factors has proven to increase the risk of degenerative disease of the wrist in patients with multiple hereditary osteochondromas:
Options:
- Ulnar negative variance of 5 mm
- Ulnar negative variance of 10 mm
- Distal radial articular slope larger than 25°
- Subluxation of the radial head
- None of the above
Correct Answer: None of the above
Explanation:
The above findings are all more common in the forearms and wrists of patients with multiple hereditary exostoses than in the general population. However, there is no parameter shown to increase the risk of degenerative wrist disease.
Question 10:
Which adverse outcome is most common in adults undergoing periacetabular osteotomy for hip dysplasia:
Options:
- Sciatic nerve palsy
- Femoral nerve palsy
- Nonunion of the osteotomy
- Persistent or worsening joint pain
- Heterotopic ossification
Correct Answer: Persistent or worsening joint pain
Explanation:
Heterotopic ossification occurs in fewer than 5% of patients undergoing various types of periacetabular osteotomy. Femoral nerve palsy and sciatic nerve palsy occur in only 1% to 2% of patients. Nonunion is rare in this region because of abundant cancellous bone contact. Persistent or worsening joint pain is the most frequent adverse outcome and is least common in those patients with preoperative degenerative changes.
Question 11:
An 18-year-old woman complains of pain in her groin area. An anteroposterior radiograph reveals a dysplastic hip with a centeredge angle of 0°. The femoral head is spherical and centers better on abduction. There is a cyst in the superior acetabulum. The joint space is narrowed superiorly by 1 mm. Recommended treatment includes:
Options:
- Salter innominate osteotomy
- Total hip arthroplasty
- Pemberton osteotomy
- Hip arthrodesis
- Periacetabular osteotomy
Correct Answer: Periacetabular osteotomy
Explanation:
This patient has a high likelihood of progressive hip deterioration so surgery is warranted. The periacetabular osteotomy is preferred because the procedure can correct this high degree of hip dysplasia. The Salter osteotomy, which hinges the hemipelvis on the symphysis pubis, cannot reliably correct more than 10° of dysplasia in this age group. The Pemberton osteotomy relies on plasticity of the immature skeleton to â foldâ the pelvis on an open triradiate cartilage, therefore, it is not indicated in an 18-yearold woman who is skeletally mature. Hip arthrodesis is not indicated when there are other, better options. The same can be said for total hip arthroplasty due to the finite duration of fixation in a young person.
Question 12:
A high school basketball player dies suddenly during a game. Which of the following is the least likely cause of death:
Options:
- Hypertrophic cardiomyopathy
- Prolonged Q-T interval
- Aortic dissection from Marfan syndrome
- C oronary artery anomalies
- Substance abuse
Correct Answer: Aortic dissection from Marfan syndrome
Explanation:
Hypertrophic cardiomyopathy, coronary artery anomalies, and electrical abnormalities are the most common causes of sudden death in athletes. Substance abuse is also common. Marfan syndrome, which can be heralded by skeletal features of arachnodactyly, should also be considered when screening athletes although it is not as likely as the other choices to cause death.
Question 13:
A 15-year-old girl has anterior hip pain and she tells you that she hears periodic snapping or clicking. Bringing the hip from the flexed-abducted position to the extended position reproduces the pain. Radiographs are normal. The diagnosis is most likely:
Options:
- Trochanteric bursitis
- Acetabular dysplasia
- Snapping psoas tendon
- Torn acetabular labrum
- Femoral hernia
Correct Answer: Snapping psoas tendon
Explanation:
Snapping of the psoas tendon is more common in girls than boys. A snapped psoas tendon is characterized by anterior hip pain that can be reproduced by moving the hip from a figure 4 position to an extended position. The discomfort from trochanteric bursitis is located laterally. The symptoms of an abnormality in the labrum or the acetabulum are not associated with snapping.
Question 14:
A 15-year-old girl has a snapping psoas tendon. Abducting and adducting her hip reproduces symptoms of anterior hip pain. Her pain has not been relieved by rest and stretching. The next step of treatment is:
Options:
- Excising the bursa
- Releasing the hip from the lesser trochanter
- Intramuscular lengthening of the tendon
- Transferring the psoas tendon to the neck of the femur
- Excising the pectineal eminence
Correct Answer: Intramuscular lengthening of the tendon
Explanation:
The initial treatment of snapping psoas tendon is rest, antiinflammatory agents, and stretching. If symptoms remain significant, the next measure to offer the patient is intramuscular lengthening of the tendon.
Question 15:
A 4-year-old girl is newly diagnosed with developmental dislocations of the hips. The femoral heads are fully dislocated and located 4 cm above the acetabulum. No pseudoacetabulum is seen. Recommended treatment includes:
Options:
- No treatment
- Traction and closed reduction
- Open reduction through a medial approach
- C losed reduction and Salter osteotomy
- Open reduction through an anterolateral approach with femoral and iliac osteotomies
Correct Answer: Open reduction through a medial approach
Explanation:
At the age of 4, femoral shortening is indicated to remove the pressure on the reduced femoral head. Realignment of the bony dysplasia is achieved by femoral derotation, iliac redirection, and possible creation of varus in the proximal femur. Open reduction through a medial approach is an option during the first 2 years, but after that the anterolateral approach is preferred in order to create a stable capsulorrhaphy.
Question 16:
A 3-year-old boy falls from a swing and injures his elbow. Radiographs show posteromedial displacement of the radius and ulna. A small fleck of bone is viewed on the radiograph that does not match the contralateral elbow. The most likely diagnosis is:
Options:
- Elbow dislocation
- Salter I disruption of the distal humerus
- Lateral condyle fracture with elbow dislocation
- Supracondylar fracture of the humerus
- Radial head fracture dislocation
Correct Answer: Elbow dislocation
Explanation:
Isolated elbow dislocations are rare in very young children because the epiphysis is mostly cartilaginous. Supracondylar fractures usually occur at an older age and have an obvious fracture line. A Salter I injury does not have an osseous component. A radial head fracture-dislocation would not explain the disruption of the ulna-humerus articulation. A lateral condyle fracture-dislocation is the most likely diagnosis in this patient.
Question 17:
A 6-month-old baby is brought in for consultation because of bowing of the tibia and fibula. The apex of the bow is medial and posterior. The angulation measures 40° on the anteroposterior film and 35° on the lateral film. One of the babys legs is 1.5 cm shorter than the other one. Recommended treatment includes:
Options:
- Manipulation and cast application
- Osteoclasis
- Osteotomy and intramedullary rod fixation
- Osteotomy and lengthening
- Observation
Correct Answer: Observation
Explanation:
Posteromedial bowing of the tibia is not likely to go on to fracture. In most cases, the bowing resolves with growth. The length inequality remains proportionate throughout growth. No treatment is indicated at this time. Length equalization by standard means is indicated near maturity.
Question 18:
Which of the following bone lesions is shown to improve radiographically and clinically by use of systemic medication:
Options:
- Aneurysmal bone cyst
- Unicameral bone cyst
- Multiple exostoses
- Fibrous dysplasia
- Fibrous cortical defect
Correct Answer: Fibrous dysplasia
Explanation:
In patients with polyostotic fibrous dysplasia, there is a decrease in pain and fracture rate and an improvement in radiodensity through the use of bisphosphonates. None of the other lesions mentioned respond radiographically to systemic medication.
Question 19:
Polyostotic fibrous dysplasia is caused by a mutation in which of the following genes:
Options:
- GNAS 1
- EXT 1
- Fibroblast growth factor receptor protein
- CFBA1
- COL1A1
Correct Answer: GNAS 1
Explanation:
Fibrous dysplasia is due to a postzygotic mutation in the GNAS1 gene. By contrast, EXT 1 mutations can cause multiple exostoses, and fibroblast growth factor receptor protein mutations cause achondroplasia, among other disorders. C FBA1 mutations are responsible for cleidocranial dysplasia. C OL1A1 mutations are responsible for osteogenesis imperfecta.
Question 20:
A 17-year-old girl is newly diagnosed with an expansile lesion of the distal tibia that is causing pain. Radiographs and biopsy are consistent with an aneurysmal bone cyst. Recommended treatment includes:
Options:
- Intralesional steroid injection
- Intralesional bone marrow injection
- Curettage and bone graft
- Wide resection distal tibial osteoarticular allograft
- Local radiation
Correct Answer: Curettage and bone graft
Explanation:
Aneurysmal bone cyst is a progressively expansile lesion that does not involute with time. Treatment of aneurysmal bone cysts is curettage and bone graft. Wide resection and structural allografts have a high complication rate and are not indicated for initial treatment. Injection of marrow or steroids is effective for unicameral cysts, but not for aneurysmal cysts. Local radiation is indicated only as an adjunct for lesions that are not surgically resectable.