OITE & ABOS Orthopedic Board Prep MCQs: Hip & Knee Arthroplasty - Part 198

Key Takeaway
This page offers Part 198 of a comprehensive OITE and AAOS Orthopedic Board Review quiz bank. Authored by Dr. Mohammed Hutaif, it features 100 verified, high-yield MCQs focused on Arthroplasty, Hip, and Knee. Designed for orthopedic surgeons and residents, this interactive set aids rigorous preparation for board certification exams.
About This Board Review Set
This is Part 198 of the comprehensive OITE and AAOS Orthopedic Surgery Board Review series authored by Dr. Mohammed Hutaif, Consultant Orthopedic & Spine Surgeon.
This set has been strictly audited and contains 100 100% verified, high-yield multiple-choice questions (MCQs) modelled on the exact format of the Orthopaedic In-Training Examination (OITE) and the American Academy of Orthopaedic Surgeons (AAOS) board examinations.
How to Use the Interactive Quiz
Two distinct learning modes are available:
- Study Mode — After selecting an answer, you immediately see whether you are correct or incorrect, together with a full clinical explanation and literature references.
- Exam Mode — All feedback is hidden until you click Submit & See Results. A live timer tracks elapsed time. A percentage score and detailed breakdown are displayed upon submission.
Pro Tip: Use keyboard shortcuts A–E to select options, F to flag a question for review, and Enter to jump to the next unanswered question.
Topics Covered in Part 198
This module focuses heavily on: Arthroplasty, Hip, Knee.
Sample Questions from This Set
Sample Question 1: What is the most frequent late complication of cementless fixation in total knee arthroplasty?...
Sample Question 2: Consider the theoretic articulation shown in Figure 11 as femoral and tibial components of a total knee prosthesis in which the components fit like a “roller in trough.” Which of the following best describes the articulation?...
Sample Question 3: Ayear-oldmanisabouttoundergorighttotalhiparthroplasty.ApreoperativeAPpelvisradiographisshowninbelow.Thefinalacetabularcomponentandpolyethylenelinerareimplanted.Withthe broachinplace,thesurgeontrialsastandardoffsetneckandneutrallengthfemoral...
Sample Question 4: A patient with rheumatoid arthritis has an unstable pseudarthrosis after undergoing C1-2 posterior fusion. No neurologic deficits are noted, and repair with posterior transarticular fixation screws and a posterior wiring technique at C1-2 i...
Sample Question 5: A 22-year-old patient has had severe groin pain for many months and is unable to engage in any physical activity. The AP radiograph of the pelvis shows minimal arthritis. The lateral radiograph of the hip is shown in Figure 33a. An MR-arthr...
Why Active MCQ Practice Works
Evidence consistently demonstrates that active recall through spaced MCQ practice yields substantially greater long-term retention than passive reading alone (Roediger & Karpicke, 2006). All questions in this specific module have been algorithmically verified for clinical integrity and complete explanations.
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
What is the most frequent late complication of cementless fixation in total knee arthroplasty?
Explanation
REFERENCES: Peters PC, Engh GA, Dwyer KA, Vinh TN: Osteolysis after total knee arthroplasty without cement. J Bone Joint Surg Am 1992;74:864-876.
Parks NL, Engh GA, Topoleski LDT, Emperado J: Modular tibial insert micromotion: A concern with contemporary knee implants. Clin Orthop 1998;356:10-15.
Question 2
Consider the theoretic articulation shown in Figure 11 as femoral and tibial components of a total knee prosthesis in which the components fit like a “roller in trough.” Which of the following best describes the articulation?
Explanation
REFERENCE: Alicea J: Scoring systems and their validation for the arthritic knee, in Insall JN, Scott WN (eds): Surgery of the Knee, ed 3. Philadelphia, PA, Churchill Livingstone, 2001, vol 2, pp 1507-1515.
Question 3
A year-old man is about to undergo right total hip arthroplasty. A preoperative AP pelvis radiograph is shown in below. The final acetabular component and polyethylene liner are implanted. With the broach in place, the surgeon trials a standard offset neck and neutral length femoral head. The leg lengths are approximately equal, but the hip is unstable. What is the best next step?
Explanation
The radiograph shows that this patient has a high offset varus femoral morphology of both hips. Preoperative templating would identify this, and the surgeon should choose an implant system that has extended offset options to help match the native anatomy and biomechanics and minimize the risk of instability. Trialing a high offset neck, rather than a standard offset neck, is the next most appropriate step. Depending on the design of the implant system, this step can be accomplished by direct medialization of the femoral head, which would not affect leg length, or by lowering the neck angle, which would affect the leg length and would require a longer femoral head, because the leg lengths had previously been equal. Placement of a longer femoral head would likely improve hip stability but would also make the leg length uneven, which is a common cause of dissatisfaction after total hip arthroplasty. An offset acetabular liner also increases the leg length and does not correct the issue, which is on the femoral side. Trochanteric
advancement is sometimes used as a treatment for instability but would be inappropriate as the next step in this setting.
Question 4
A patient with rheumatoid arthritis has an unstable pseudarthrosis after undergoing C1-2 posterior fusion. No neurologic deficits are noted, and repair with posterior transarticular fixation screws and a posterior wiring technique at C1-2 is planned. Which of the following preoperative studies offers the best visualization?
Explanation
REFERENCES: Paramore CG, Dickman CA, Sonntag VK: The anatomic suitability of the C1-2 complex for transarticular screw fixation. J Neurosurg 1996;85:221-224.
Dickman CA, Sonntag VK: Posterior C1-C2 transarticular screw fixation for atlantoaxial arthrodesis. Neurosurgery 1998;43:275-280.
Song GS, Theodore N, Dickman CA, Sonntag VK: Unilateral posterior atlantoaxial transarticular Screw fixation. J Neurosurg 1997;87:851-855.
Question 5
A 22-year-old patient has had severe groin pain for many months and is unable to engage in any physical activity. The AP radiograph of the pelvis shows minimal arthritis. The lateral radiograph of the hip is shown in Figure 33a. An MR-arthrogram is shown in Figure 33b. What is the most appropriate treatment at this stage? Review Topic
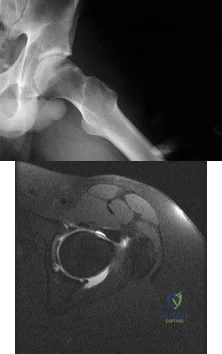
Explanation
Question 6
A 16-year-old boy who is a competitive basketball player (Figure 43)
Explanation
Question 7
A 35-year-old woman reports an 8-week history of neck pain radiating to her right upper extremity. She denies any history of trauma or provocative event. Examination reveals decreased pinprick sensation in her right middle finger, otherwise sensation is intact bilaterally. Finger flexors and interossei demonstrate 5/5 motor strength bilaterally. Finger extensors are 4/5 on the right and 5/5 on the left. The triceps reflex is 1+ on the right and 2+ on the left. The most likely diagnosis is a herniated nucleus pulposus at what level?
Explanation
REFERENCES: Houten JK, Errico TJ: Cervical spondylotic myelopathy and radiculopathy: Natural history and clinical presentation, in Clark CR (ed): The Cervical Spine, ed 4. Philadelphia, PA, Lippincott Williams & Wilkins, 2005, pp 985-990.
Hoppenfeld S: Orthopaedic Neurology: A Diagnostic Guide to Neurologic Levels. Philadelphia, PA, JB Lippincott, 1977, pp 7-43.
Question 8
Figure 37 shows a coronal T2-weighted MRI scan. What is the name of the labeled torn structure?
Explanation
are intact.
REFERENCES: Potter HG, Weiland AJ, Schatz JA, et al: Posterolateral rotatory instability of the elbow: Usefulness of MR imaging in diagnosis. Radiology 1997;204:185-189.
King JC, Spencer EE: Lateral ligamentous instability: Techniques of repair and reconstruction. Techniques in Orthopaedics 2000;8:93-104.
Question 9
A 10-year-old girl is treated for a tibia/fibula fracture with a long leg cast. The on-call resident is called to evaluate the patient for increasing pain medicine requirements and tingling in her foot. Examination of the cast reveals that the ankle has been immobilized in 10 degrees of dorsiflexion. What ankle position results in the safest compartment pressures in a casted lower leg?

Explanation
Weiner et al measured intramuscular compartment pressure in the anterior and deep posterior compartments of the leg in seven healthy adults who had long leg casts placed. They found that in a casted leg the intramuscular pressure in the anterior compartment was lowest with the ankle in neutral, and the deep posterior compartments was lowest when the ankle joint was in the resting position to approximately 37 degrees of plantar flexion. Based on this, they concluded that the safest ankle casting position regarding compartment pressure is between 0 and 37 degrees of plantar flexion. After the cast was bivalved, they noted a significant decrease in intramuscular pressure of 47 per cent in the anterior compartment and of 33 per cent in the deep posterior compartment. Constrictive casts and abberant ankle positioning can exacerbate pain/symptoms. Loosening of the cast by bivalving, spreading, and cutting underlying stockinette/softroll should always be the first step in management of possible compartment syndrome.
Question 10
Hip pain of 1-month duration has developed in a 72-year-old man with a previous total hip arthroplasty. He underwent dental work 6 weeks ago. Aspiration shows a white blood cell count of more than 6,000 cells/μL (reference range 4,500 to 11,000 cells/μL) and the presence of gram-positive cocci in clusters on Gram stain. The orthopaedic surgeon recommends urgent debridement and irrigation. Fixation of the components is judged to be stable, and the surgeon elects to retain the implants. What is this patient's prognosis for infection resolution?
Explanation
The patient has a late infection of at least 4 weeks symptomatic duration that most likely is hematogenous in etiology. This infection is not an acute hematogenous infection that can successfully be treated with irrigation and debridement. Retention of the implants with debridement and irrigation alone has been associated with a poor prognosis. In a recent study, the success rate was only 44% in a series of 104 patients at a mean 5.7-year follow-up. In one study of 50 infections attributable to MRSA or methicillin-resistant Staphylococcus epidermidis organisms treated with a two-stage protocol, the failure rate was 21%. Patients who experienced successful infection treatment had lower functional outcome measures using the Western Ontario and McMaster Universities Osteoarthritis Index, the University of California Los Angeles Activity Score, and the 12-item Oxford Knee Score, however.
Question 11
What is the most common primary malignant bone or cartilage tumor in children?
Explanation
1 million children younger than age 15 years), and Ewing’s sarcoma is second (2.1 per
1 million children). Giant cell tumor and chondrosarcoma are rare in children. Osteochondroma is more common than any of the above tumors in children, but it is not malignant.
REFERENCES: Himelstein BP, Dormans JP: Malignant bone tumors of childhood. Pediatr Clin North Am 1996;43:967-984.
Pierz KA, Womer RB, Dormans JP: Pediatric bone tumors: Osteosarcoma, Ewing’s sarcoma, and chondrosarcoma associated with multiple hereditary osteochondromatosis. J Pediatr Orthop 2001;21:412-418.
Arndt CA, Crist WM: Common musculoskeletal tumors of childhood and adolescence.
N Engl J Med 1999;341:342-352.
Question 12
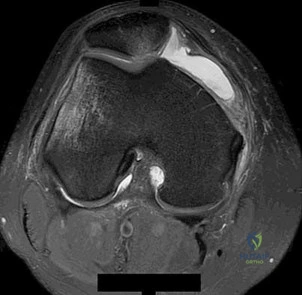
Figures 31a and 31b show the T1- and T2-weighted MRI scans of a patient’s knee joint. What is the most likely diagnosis?
Explanation
REFERENCES: Resnick D, Kang HS: Synovial joints, in Resnick D, Kang HS (eds): Internal Derangements of Joints: Emphasis on MR Imaging. Philadelphia, PA, WB Saunders, 1997, pp 49-53.
Kier R, McCarthy SM: Lipohemarthrosis of the knee: MR imaging. J Comput Assist Tomogr 1990;14:395-396.
Question 13
Use of titanium elastic nailing for treatment of pediatric femur fractures is associated with a higher complication rate among
Explanation
Studies of titanium elastic nailing for femur fractures demonstrated a higher rate of complications, including angular deformity and construct failure, among patients weighing more than 50 kg (100 pounds). Other methods of fixation are recommended for these patients. Flexible nails are not commonly needed, but they also are not associated with a higher complication rate in children younger than age 6.5. Titanium elastic nailing works well in closed or minimally open transverse midshaft fractures, even in the setting of early or immediate weight bearing.
Video 8a
Video 8b
Question 14
Figures 25a and 25b show the radiograph and MRI scan of a 48-year-old man who reports increasing unsteadiness in his gait and hand clumsiness. Examination reveals a positive Hoffmann’s reflex bilaterally, positive clonus, and a spastic gait. Management should consist of
Explanation
including directly posterior to the vertebral bodies. A multilevel diskectomy may address the cord compression at the disk level, but not posterior to the bodies, and most likely would be inadequate. The patient has significant stenosis distal to C5, necessitating a more extensive surgical approach than simply C3-C5. Because the patient’s cervical lordosis is preserved, a posterior procedure such as laminoplasty or laminectomy would allow the cord to fall away
from the anterior pathology and afford decompression. Cervical myelopathy does not tend to resolve, and there is a significant risk for progression; therefore, surgical management usually
is recommended.
REFERENCES: Edwards CC II, Riew KD, Anderson PA, et al: Cervical myelopathy: Current diagnostic and treatment strategies. Spine J 2003;3:68-81.
Edwards CC II, Heller JG, Murakami H: Corpectomy versus laminoplasty for multilevel cervical myelopathy: An independent matched-cohort analysis. Spine 2002;27:1168-1175.
Question 15
A 6-year-old girl is brought in for orthopaedic examination because she “walks funny” and occasionally trips. Her feet are normal in appearance. Internal rotation of her hips is 60 degrees and external rotation is 40 degrees bilaterally. The thigh-foot angle on the right is -20 degrees, and +10 degrees on the left. What is the source of her gait abnormality?
Explanation
Question 16
An 11-year-old boy has had a fever and pain and swelling over the lateral aspect of his right ankle for the past 3 days. Examination reveals warmth, swelling, and tenderness over the lateral malleolus, and he has a temperature of 103.2 degrees F (39.5 degrees C). Laboratory studies show a WBC count of 13,200/mm 3 with 61% neutrophils, an erythocyte sedimentation rate of 112 mm/h, and a C-reactive protein of 15.7. Radiographs and a T 2 -weighted MRI scan are shown in Figures 13a through 13c. Aspiration yields 1 mL of purulent fluid. Management should now consist of
Explanation
definitive treatment.
REFERENCES: Scott RJ, Christofersen MR, Robertson WW Jr, et al: Acute osteomyelitis in children: A review of 116 cases. J Pediatr Orthop 1990;10:649-652.
Vaughan PA, Newman NM, Rosman MA: Acute hematogenous osteomyelitis. J Pediatr Orthop 1987;7:652-655.
Question 17
A 68-year-old woman who sustained a closed distal tibia fracture 2 years ago was initially treated with an external fixator across the ankle for 12 weeks, followed by intramedullary nailing of the fibula and lag screw fixation of the tibia. She continued to report persistent pain so she was treated with a brace and a bone stimulator. She now reports pain in her ankle. Examination reveals ankle range of motion of 8 degrees of dorsiflexion to 25 degrees of plantar flexion. She is neurovascularly intact. Current radiographs are shown in Figures 9a through 9c. What is the next most appropriate step in management?
Explanation
REFERENCES: Carpenter CA, Jupiter JB: Blade plate reconstruction of metaphyseal nonunion of the tibia. Clin Orthop 1996;332:23-28.
Lonner JH, Siliski JM, Jupiter JB, Lhowe DW: Posttraumatic nonunion of the proximal tibial metaphysis. Am J Orthop 1999;28:523-528.
Stevenson S: Enhancement of fracture healing with autogenous and allogeneic bone grafts. Clin Orthop 1998;355:S239-S246.
Wiss DA, Johnson DL, Miao M: Compression plating for non-union after failed external fixation of open tibial fractures. J Bone Joint Surg Am 1992;74:1279-1285.
Question 18
What is the most significant prognostic factor in nontraumatic osteonecrosis of the humeral head?
Explanation
REFERENCES: Cruess RL: Osteonecrosis of bone: Current concepts as to etiology and pathogenesis. Clin Orthop 1986;208:30-39.
Cruess RL: Steroid-induced avascular necrosis of the humeral head: Natural history and management. J Bone Joint Surg Br 1976;58:313-317.
Rutherford CS, Cofield RH: Osteonecrosis of the shoulder. Orthop Trans 1987;11:239.
Hattrup SJ, Cofield RH: Osteonecrosis of the humeral head: Relationship of disease stage, extent, and cause to natural history. J Shoulder Elbow Surg 1999;8:559-564.
Question 19
A well-healed bulk proximal tibia osteoarticular allograft is removed 10 years after implantation due to arthropathy. Histologic examination of the host allograft junction site will most likely reveal
Explanation
Question 20
Video 1 shows a 20-year-old right-hand dominant man with a 6-month history of left wrist pain and popping that has failed nonsurgical measures. No other positive findings upon examination are noted. What is the most appropriate course of treatment?
Explanation
A. Abductor pollicis longus reconstruction with palmaris autograft
B. Extensor pollicis brevis repair
C. Extensor pollicis longus (EPL) repair
D. Extensor indicis proprius (EIP) to extensor pollicis longus tendon transfer
The EPL is the only tendon that will lift a thumb off of a table as described. It is the most frequently ruptured tendon associated with distal radius fractures. Rupture is more common with nondisplaced fractures. Rupture after a nondisplaced or minimally displaced fracture suggests an ischemic etiology. The patient will not be able to lift her thumb off of a table with her hand lying flat, palm-down. Direct repair is often difficult because of retraction of tendon ends, atrophy, and fraying. The EIP has a similar amplitude and direction of pull. Prerequisites for the use of the EIP to EPL tendon transfer include independent extension of the index finger.
15- Figure 1 is the clinical photograph of a very functional 17-year-old boy with cerebral palsy and quadriplegia. He has no active supination but has full passive supination. His ability to determine position and sensibility without visual input are good. Radiographs show no osseous malalignment. Which treatment can best improve this patient's function?
A. Physical therapy for supination strengthening
1- Figures 1 through 3 are the radiographs of a 40-year-old woman who sustained a minor injury to her left ring finger. Prior to this injury she was asymptomatic, but she now notes pain and swelling. What is the best course of treatment?
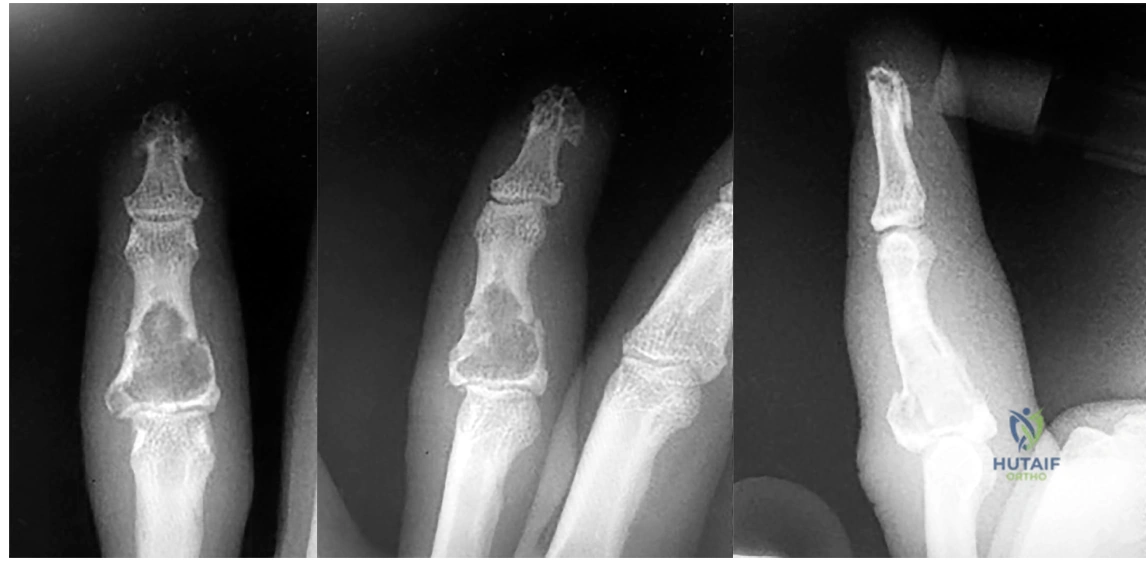
A. Observation only
B. Fluoroscopic-guided intralesional steroid injection followed by serial radiographs
C. Immediate curettage without bone grafting
D. Splint immobilization with curettage and possible grafting after the fracture has healed
This patient has a fracture of the middle phalanx attributable to the presence of an enchondroma. Enchondromas are the most common benign bone tumor affecting the hand. This particular enchondroma has thinned the cortices extensively so that even minor trauma can cause a pathologic fracture. Observation is not the best treatment because a fracture is present, and, at a minimum, the digit should be immobilized.
Question 21
A right-handed 24-year-old professional baseball player injured his left shoulder 6 weeks ago when he dove forward and landed hard with the arm extended. He reports that the shoulder “slipped out” and “went back in.” The shoulder did not need to be reduced. He now reports deep pain in the front of the shoulder when batting on either side and is hesitant to raise his left arm up over his head to catch a ball. Examination reveals no obvious deformities of the shoulder and a somewhat guarded, limited range of motion in all planes. Provocative tests for the rotator cuff and labrum are equivocal. MRI scans are shown in Figures 16a and 16b. What is the best course of action?
Explanation
REFERENCES: Abrams JS, Savoie FH III, Tauro JC, et al: Recent advances in the evaluation and treatment of shoulder instability: Anterior, posterior and multidirectional. Arthroscopy 2002;18:1-13.
DeBerardino TM, Arciero RA, Taylor DC, et al: Prospective evaluation of arthroscopic stabilization of acute, initial anterior shoulder dislocations in young athletes: Two- to five-year follow-up. Am J Sports Med 2001;29:586-592.
Question 22
A 41-year-old man who plays golf regularly has had ulnar-sided wrist pain for the past several days after striking a tree root with a golf club. Examination reveals significant pain with resisted flexion of the ring and small fingers and tenderness over the hook of the hamate. Which of the following radiographic views would be most helpful in identifying the pathology of this injury?
Explanation
REFERENCES: Green DP, Hotchkiss RN, Pederson WC (eds): Operative Hand Surgery, ed 4. New York, NY, Churchill Livingstone, 1999, p 855.
Manske PR (ed): Hand Surgery Update. Rosemont, IL, American Society for Surgery of the Hand, 1994, pp 77-84.
Question 23
In the most common condition causing a winged scapula, which of the following nerves is affected?
Explanation
REFERENCES: Kline DG, Hudson AR: Nerve Injuries: Operative Results for Major Nerve Injuries, Entrapments and Tumors. Philadelphia, PA, WB Saunders, 1995.
van Alfen N, van Engelen BG: The clinical spectrum of neuralgic amyotrophy in 246 cases. Brain 2006;129:438-450.
Question 24
What factor is associated with a high risk of developing pseudotumors after metal-on-metal hip resurfacing?
Explanation
Question 25
...Figure 74 is the radiograph of an 11-year-old boy with pain in his left arm. Prognosis is most influenced by
Explanation
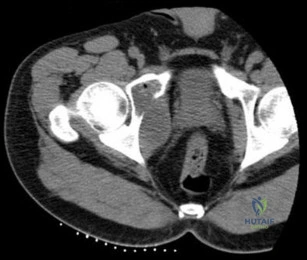
Question 26
Synovitis of the MTP joints with eventual hyperextension deformity of the MTP is a common toe deformity seen with RA.
Explanation
Jin et al conducted a meta-analysis regarding polymorphisms in the 5' flank of COL1A1 gene and the conflicting results relating to osteoporosis. They found that the COL1A1 Sp1 polymorphism is associated with a modest reduction in BMD and an increased risk of fracture.
The attached review by Huang and Kung discusses the multiple genetic and environmental determinants of osteoporosis and illustration A (from a different review by these same authors) lists the known genes currently associated with osteoporosis.
The greatest biomechanical difference between unicortical and bicortical locking screws is seen when what force is applied?
Compression
Torsion
Distraction
Bending on the side of the plate
Bending on the surface perpendicular to the plate
Torsion force has the largest biomechanical difference between unicortical locked screws and bicortical locked screws.
The first referenced article by Roberts et al noted that by replacing the farthest unicortical
screws (3 per side of the fracture) with bicortical locking screws, torsion resistance was increased by over 50%.
The second referenced article by Fulkerson et al noted decreased resistance to all applied forces with unicortical screws in a comminuted fracture model, and recommended against their use in such a fracture.
FOR ALL MCQS CLICK THE LINK ORTHO MCQ BANK
You are planning surgery on a 54-year-old female with the tibial plateau fracture seen in figures A and B. After reduction of the joint surface you plan to fill the void with a bone-graft substitute to prevent joint collapse. Which of the following bone-graft substitutes
disappears most quickly in vivo?
Collagen-based matrices
Calcium phosphate
Calcium sulfate
Synthetic calcium sulfate and tri-phosphate mixture
Coraline hydroxyapatite
Calcium sulfate disappears in vivo quickly, usually within 4-12 weeks. Calcium phosphate and coraline hydroxyapatite are resorbed slowly, somewhere between 1-10 years, depending on the manufacturer. Synthetics that combine calcium sulfate and phosphate
resorb quicker than calcium phosphate but slower than calcium sulfate. Collagen-based matrices show quick resorption of the collegen but slow resorption of their hydroxyapatite coating. Walsh et al. examined the in vivo response of calcium sulfate pellets alone or in combination with autogenous bone graft in a sheep model. They found excellent bone formation in defects filled with calcium sulfate pellets. Immunostaining for various cytokines (BMP-2, BMP-7, PDGF, or TGF-beta)
showed elevated levels in the newly formed bone. They proposed that the local environment acidity was responsible for breakdown of the calcium sulfate. Watson evaluated 8 patients with comminuted tibial metaphyseal fractures treated with an injectable calcium sulfate. They found that bone regrowth was observed in all patients and the bone substitute almost completely resorbed by
months. Bucholz reviewed the biochemical, biomechanical, and longevity characteristics of the common bone substitutes.
Which of the following Figures shows a fixation construct achieving absolute stability?
Figure A shows percutaneous pinning, Figure B shows locked bridge plating, Figure C shows intramedullary nailing, Figure D shows lag fixation and neutralization plating, and Figure E shows external fixation. All except Figure D show relative stability constructs.
Absolute stability is a construct seen in Figure D, where lag screws and a neutralization plate are shown in a postoperative clavicle. No micromotion is seen with this technique, and healing is by primary (Haversian) healing, as opposed to the other four constructs, which have relative stability and heal via callus formation. The first reference, the AO Principles textbook, covers this in depth.
The second reference by Claes et al notes that bone can still heal with bone (as opposed to fibrous union) with strain rates up to 15%.
Which immunoglobulin subtype does the rheumatoid factor target?
IgA
IgE
IgM
IgG
Rheumatoid factor does not target an immunoglobulin
Rheumatoid factor is an auto-antibody most commonly seen with rheumatoid arthritis. The presence of rheumatoid factor can also indicate generalized autoimmune activity unrelated to rheumatoid arthritis (e.g. tissue or organ rejection). Rheumatoid factor is itself an IgM antibody that is directed against the Fc portion of IgG antibody. Rheumatoid factor (IgM) attaches to IgG to form immune complexes which are deposited in tissues like the kidney and contribute to the overall disease process in rheumatoid arthritis.
James et al. assessed the occurrence and predictive factors for orthopaedic surgery in an cohort of patients with rheumatoid arthritis. Risk factors for surgery varied but the authors found that decreased inflammatory markers during the first year after diagnosis decreased the risk for subsequent surgery.
The positive predictive value is defined as which of the following?
True positives / (true positives + true negatives)
False negatives / (false negatives + true positives)
False positives / (false positives + false negatives)
(True positives + false positives) / (true negatives + false negatives)
True positives / (true positives + false positives) Corrent answer: 5
The positive predictive value is defined as the true positives divided by the sum of the positive results (true positive and false positive). It is also defined as the probability that a patient with a positive test actually has the disease; it is dependent on prevalence of disease.
The referenced articles by Wojtys and Kuhn et al are two of a series of medical statistics review papers.
An 85-year-old woman undergoes the treatment seen in Figure A for a displaced left femoral neck fracture. During wound closure, the patient becomes hypoxic and hypotensive. Despite aggressive resuscitation efforts, she passes away three hours later in the intensive care unit. The autopsy findings seen in
Figure B from the patient's lungs are most likely the result of which of the following
Reaming for the femoral component
Insertion of a femoral component after cement pressurization
Utilization of undersized broaches during canal preparation
Inadequate beta blockade
Use of spinal anesthesia
The clinical scenario is consistent with fat emboli syndrome. Figure A, shows a cemented bipolar hemiarthroplasty while Figure B shows marrow embolization into the lungs.
Studies have shown that intramedullary pressure and fat embolization are greatest during pressurization of cement and implant insertion.
Intramedullary pressure is influenced by size, shape, sharpness and insertion rate of an implant. Pressurization during cementing of a femoral component generates a large degree of pressure over a much wider surface area than in the other methods described of femoral canal instrumentation or preparation, as the entire femoral canal is
pressurized at one time. This results in the highest degree of marrow embolization to the lungs resulting in hypoxia.
Dobrjanski et al studied which variables affected intramedullary pressurization and found that lower implant insertion speed, lower hammering force, a
rubber- compared with steel-tipped hammer and a larger synthetic bone-to- implant radial gap reduced intramedullary pressure generated in a femur module.
Sustained compression applied to a growth plate under experimental conditions has what effect?
No effect
Accelerated longitudinal growth
Decelerated longitudinal growth
Decelerated apposition growth
Decreased bending strength of the bone
The Heuter-Volkmann Law states that compression across the growth plate slows longitudinal growth.
Stokes et al demonstrated that sustained compression across the growth plate can decrease longitudinal growth by 40%. Tension across the physis increases growth, but to a lesser degree.
A 13-year-old girl with a displaced proximal tibia fracture is brought into the emergency department by her adult cousin. The
fracture needs surgical management. The child is living with her cousin's family while her parents are in Germany. While the child speaks fluent English, her cousin and her parents are German-only speaking. How should you consent this patient?
No consent is needed given the urgent nature of the injury, proceed with surgery
Talk with the cousin, using the child as a translator
Talk with the cousin, using a German-translator
Call the parents in Germany, using the child as a translator over the phone
Call the parents in Germany, using a German-translator over the phone
This is an urgent (not emergent) clinical senario, and as such, the child needs to have
formal consent by speaking with her parents using a German- translator.
Wenger and Lieberman discuss the problems and potential solutions surrounding the process of informed consent in patients who either personally lack capacity to make decisions or in patients who require surrogates (like minors) to make treatment decisions.
Lindseth reviews the ethical issues encountered in pediatric orthopaedics and the problems associated with these decisions. Specifically pediatric consent is confounded because the person giving the consent is not the person who will bear the consequences of the treatment.
What is the primary mode of bisphosphonate excretion?
Renal
Gastrointestinal
Liver
Skin
Pulmonary
Bisphosphonates are a broad class of medicines used to treat osteoporosis and Paget's disease. They work by inhibiting osteoclast-mediated resorption after being absorbed into the inorganic phase of bone and taken up by osteoclasts. The paper by Lin et al provides a nice review of bisphosphonates and describe their appropriate use in enhancing bone density in patients with structurally
flawed bone. They describe the mechanism of action of bisphosphonates as pyrophosphate analogues and their renal mechanism of excretion, thus, prohibiting their use in patients with renal insufficiency. Rosier discusses the role of the orthopaedic surgeon in the diagnosis and treatment of patients with osteoporosis, now referred to as the "own the bone" initiative. Central to the treatment of osteoporosis are bisphosphonates and the anti-RANKL
monoclonal antibody, Denosumab.
The 2009 AAOS Clinical Guideline on prevention of pulmonary embolism in patients undergoing total hip or knee arthroplasty recommends classifying patients as having either a "standard" or "elevated" risk of bleeding complications. The presence of all of the following qualify a patient as having an "elevated" risk of major bleeding EXCEPT?
History of hemophilia
History of protein C deficiency
History of a recent gastrointestinal bleed
History of a recent hemorrhagic stroke
History of Von Willebrand's Disease
The 2009 AAOS Clinical Guideline on prevention of pulmonary embolism in patients undergoing total hip or knee arthroplasty recommends that all patients pre-operatively should be classified as either having an elevated or standard risk of bleeding and either an elevated or standard risk of pulmonary embolism.
A history of a bleeding disorder (e.g., hemophilia, Von Willebrand's Disease), recent GI bleed, or hemorrhagic stroke qualifies a patient as having an elevated risk of major bleeding.
A history of hypercoagulable state (such as protein C deficiency) or previous documented pulmonary embolism qualifies a patient as having an elevated risk of pulmonary embolism. Type of thromboembolism prophylaxis is recommended by weighing risk of major bleeding vs risk of PE. For those patients with a known contraindication to anticoagulation an IVC filter is considered. Mechanical prophylaxis is recommended across all risk (low to
high risk of either bleeding or pulmonary embolism) groups undergoing total hip or total knee arthroplasty. The detailed AAOS guidelines can be found on the AAOS website.
The evidence based clinical recommendations are presented in the reference by Johanson et al.
In consideration of a prosthetic knee, each of the following are advantages of choosing a polycentric knee with fluid control over a constant friction knee EXCEPT:
Allows variations in cadence
Flexes in a more controlled manner
Lighter in weight
Improved stance control allows less energy expenditure
Overall length of the limb is shortened during initiation of a step reducing the risk of stumbling
Single axis, constant friction knees function as a simple hinge. They are light, durable, and much cheaper prostheses making them ideal for growing children who will need multiple prostheses before reaching adulthood. This prosthesis allows only a single speed of walking, and relies solely on alignment for stance phase stability. Polycentric knees offer each of the advantages stated above making it a more ideal prosthesis for the active adult. Disadvantages of the polycentric knee include cost, weight, and more sophisticated maintenance.
Tang et al reviews the current prosthetic options for leg and foot amputees. Illustration A demonstrates a single axis knee prosthesis.
Illustration B demonstrates a polycentric knee prosthesis.
Which of the following biologic agents commonly used to treat rheumatoid arthritis (RA) DOES NOT target tumor necrosis factor- alpha (TNF-alpha)?
Infliximab
Rituximab
Etanercept
Golimumab
Adalimumab
Rituximab is a chimeric monoclonal antibody against the protein CD20, which is primarily found on the surface of immune system B cells. Rituximab is used in combination with methotrexate to treat RA that has not responded to one or more types of treatment, including anti-tumor necrosis factor (TNF) blockers.
In rheumatoid arthritis, and other chronic inflammatory conditions, cytokines produced by activated T-cells/macrophages contribute to the pro-inflammatory state. TNF-alpha is thought to be one of the major cytokines involved in rheumatoid arthritis pathology. As a result, many biologic agents used to treat RA are directed towards blocking TNF-alpha or its receptors. These drugs are able to reduce inflammation and stop disease progression.
Elliot et al. evaluated the safety and efficacy of infliximab in 20 patients with active RA in an open phase I/II trial lasting 8 weeks. They found that treatment with anti-TNFa was safe, well tolerated and resulted in significant clinical and laboratory improvements.
Illustration A depicts five commonly used anti-TNF alpha biologic agents for the treatment of rheumatoid arhtirits with their usual dosing regimens.
Incorrect Answers:
Receptor activator of nuclear-factor kappa-B ligand (RANKL) is
an important regulator of bone resorption. Which of the following cells is the MAJOR source of RANKL in bone remodelling?
Osteoclasts
Osteoblasts
Integrins
T cells
Macrophages
RANKL, a key osteoclastogenic protein, is expressed by osteoblasts and binds to the RANK receptor on osteoclast precursor cells.
The binding of RANKL to RANK on osteoclast precursor cells drives their differentiation into mature osteoclasts (multinucleated giant cells). Mature osteoclasts bind to the bone surfaces via integrins and resorb bone via their ruffled border within Howship's lacunae. Osteocytes orchestrate bone resorption and bone deposition by controlling osteoclast and osteoblast activity. Osteoblasts release RANKL to induce osteoclast differentiation, while
osteoblasts release osteoprotegerin (OPG) to downregulate osteoclastogenesis. Osteocytes also release fibroblast growth factor-23 (FGF-23), BMPs and sclerostin to regulate osteoblast activity. Antibodies to RANKL and Sclerostin have both been shown to increase bone density.
Compton et al. reviewed osteocyte function and the emerging importance of sclerostin, which is a glycoprotein. Sclerostin is predominantly secreted by osteocytes under physiologic conditions to act as an important negative regulator of bone mass through inhibition of bone formation by osteoblasts.
Illustration A demonstrates local bone milieu. It depicts the interplay between osteocytes, osteoblasts, and osteoclasts via the factors described above.
Incorrect answers:
A 45-year-old woman with rheumatoid arthritis is being scheduled for a total knee athroplasty in 2 weeks. She is currently taking sulfasalazine, Penicillamine, and etanercept, a tumor necrosis factor inhibitor (aTNF-a). What changes should be made to her medication regimen prior to surgery?
Discontinuation of all three medications 1 weeks prior to surgery
Discontinuation of sulfasalazine 1 weeks prior to surgery, continuation of etanercept and penicillamine
Continuation of sulfasalazine, penicillamine, and etanercept
Continuation of sulfasalazine and penicillamine, discontinuation of etanercept 1 week prior to surgery
Continuation of penicillamine, discontinuation of sulfasalazine and etanercept 1 week prior to surgery
Anticytokine disease-modifying antirheumatic drugs (DMARD) have become increasingly popular in the treatment of RA. Immunosuppression and the risk of infection are potential complications for all anti-TNF-alpha medications. Current recommendations for cessation of immunosuppressive therapy are when the drug concentrations are at their lowest levels which include the following: 3 days after etanercept injection; 2 weeks prior to infliximab infusion; 10 days after adalimumab injection. Medications such as sulfasalazine and penicillamine may be continued during the pre and post- operative period. Recent evidence and guidelines such as those reviewed by Keith's paper, suggest that anti-TNF-alpha medications should be stopped 4 weeks prior to surgery.
Giles et al report in their case control series an increased infection rate of RA patients undergoing an orthopaedic procedure who were on TNF-a inhibitors as opposed to patients on more traditional treatment regimens like methotrexate and prednisone.
Which of the following supplements affects blood clotting through its effect on platelets?
Ginkgo
Vitamin D
Ephedra
St. John's Wort
Selenium
Ginkgo and ginseng are two common supplements used in the general population that have inhibitory effects of platelet function. Adverse peri- operative complications consisting of increased bleeding and hematoma formation have been reported with the use of these two herbal supplements. The most commonly used supplements that could have an effect in the peri- operative period include echinacea, ephedra, garlic, ginkgo, ginseng, kava, St John's wort, and valerian. Bleeding has been shown to be effected by garlic, ginkgo, and ginseng; cardiovascular instability from ephedra; and hypoglycemia from ginseng. Kava and valerian have pharmacodynamic herb- drug interactions that can increase the sedative effect of anesthetics. St John's wort has been shown to alter the metabolism of certain drugs used in the perioperative period.
Ang-Lee et al review common supplements used today and their potential anesthesia/operative effects. The article places emphasis on proper history taking of not only medications but also supplements which is often times left out of documentation.
The femur radiograph of a healthy 25-year-old female is compared to the femur radiograph of a healthy 85-year-old female. Which of the following best describes the 25-year-old's femur?
Increased cortical thickness and a smaller medullary canal volume
Decreased cortical thickness and a larger medullary canal volume
Equivalent cortical thickness and medullary canal volume
Increased cortical thickness and larger medullary canal volume
Decreased cortical thickness and a smaller medullary canal volume
As the human body ages the cortical thickness/area decreases and subsequently the diameter/volume of the medullary canal increases. Therefore, a young healthy 25- year-old woman should have thicker cortices and a smaller medullary canal volume than her counterpart at 85 years. A decreased cortical bone area is linked to increased fracture risk.
Stein et al studied femurs from subjects aged 21-92 years of age. They found that a reduction in cortical area was seen in older specimens and this change was more
pronounced in female specimens.
Wrong Answers:
Which of the following is NOT a described complication of corticosteroid injections?
Local flare in surrounding tissues
Apoptosis of myocytes
Skin pigmentation changes
Fat atrophy
Facial flushing
Corticosteroids have not been shown to cause apoptosis of myocytes when injected extra-articularly. Each of the other answers have been described.
Cole and Schumacher provide a review of current uses of corticosteroid injections, and emphasize that how accurately the injection is placed affects the outcome.
Kumar and Newman report prospectively on 672 patients who received 1147 intra- and extra-articular injections. Their overall complication rate was low (16%) with injection site pain (mild) and bleeding constituting the majority of cases. There were 4 instances of fat atrophy in the extra-articular group, and
cases of syncope or dizziness in the intra-articular group. They did not discuss the efficacy of their injections.
A surgeon chooses a periarticular locking plate with unicortical proximal locking screws for an extra-articular distal femur fracture as seen in Figure A. Compared to an identical construct with bicortical unlocked proximal screw fixation, the periarticular locking plate with unicortical locking screws has which biomechanical properties?
Greater torsional and axial fixation strength
Less torsional but greater axial fixation strength
Equal torsional and axial fixation strength
Greater torsional but less axial fixation strength
Less torsional and axial fixation strength
Unicortical locking plates have characteristically less torsional strength than bicortical locking plates and bicortical non-locking plates. Axial strength is improved with locking plate fixation.
Zlowodzki et al studied the LISS periarticular locking plate with unicortical proximal fixation in a distal femur model and found superior axial fixation strength (134%) but worse torsional strength (68%) compared to a fixed angle blade plate with non- locking bicortical screw fixation.
Locked plating was reviewed by Haidukewych and Ricci which highlighted the added cost, unique complications, and they recommended the use of locked plating only in situations when unlocked constructs have demonstrated poor outcomes.
In rat models looking at the effect of malnutrition on fracture healing, amino acid supplementation in a nutritionally deprived rat increases all of the following EXCEPT
Serum albumin
Body mass
Quadriceps total protein content
Fracture callus mineralization
Insulin-like growth factor 1 (IGF-1) mRNA expression
The study by Hughes et al found that essential amino acid supplementation (glutamine, arginine, and taurine) following femoral fracture in a protein- malnourished rat model increases serum albumin, body mass, quadriceps total protein content, and fracture callus mineralization. Expression of IGF-1 and
IGF-2, myosin, actin, and VEGF mRNA were all significantly decreased in the amino acid supplemented group compared to the malnourished group. The malnourished group is thought to have upregulation of mRNA expression in attempt to increase the amount of protein product that is translated, however the lack of amino acid building blocks in the malnutrition group was a barrier to appropriate protein synthesis.
The study by Day et al created a malnourished rat femur fracture model by administering a 6% protein diet. They found that administering a 20% protein diet in the post-fracture period yielded a greater cross-sectional area of the
fracture callus and callus stiffness compared to the 6% protein malnourished group.
The statistical power of a study is best defined by?
1 - probability of type-II (beta) error
True positive/(true positive + false negative)
True negative/(false positive + true negative)
1 - probability of type-I (alpha) error
[True positive/(true positive + false negative)] / false-positive rate
The power of a study is an estimate of the probability of finding a significant association in a research study when one truly exists. The power is defined by
1 - probability of type-II (beta) error, and is often set at 80%. For example, a power of 80% means that if the intervention works, the study has an 80% chance of detecting this and a 20% chance of randomly missing it. A type-II or beta error occurs when one falsely concludes that there is no significant association when there actually is an association (resulting in a false-negative study that rejects a true alternative hypothesis). The type-II or beta error can be determined if Type I error rate and sample size are known. A type-I or alpha error occurs when a significant association is found when there is no true association (resulting in a false-positive study that rejects a true null hypothesis). The alpha level refers to the probability of a type-I (alpha) error and is usually set for most studies at 0.05. Answer 2 is the formula for sensitivity. Answer 3 is the formula for specificity. Answer 5 is the formula for the positive likelihood ratio. The references by
Kocher and Wojtys are excellent reviews of basic biostatistic principles.
A 55-year-old female with a history of metastatic breast cancer develops shoulder pain without any trauma. Which of the following is involved with the findings shown in Figures A and B?
IL-4
RANK
TNF-alpha
OPG
Sox-9
Osteoclastic bone resorption is the final common mechanism for osteolysis, whether due to a pathologic lytic lesion, macrophage activation in particle wear, or normal remodeling. The RANK-RANKL mechanism controls the coupling of osteoblast and osteoclast activation. Figures A and B show an osteolytic lesion in the humerus in a patient with known metastatic breast carcinoma.
RANKL is expressed from osteoblasts and bone-marrow stromal cells. When RANKL binds to the RANK receptor (receptor/activator of NF-[kappa]B) on the cell membrane of osteoclasts it stimulates differentiation from osteoclast progenitor cells to mature osteoclasts. Mature osteoclasts proceed with osteoclastic bone resporption.
Osteoprotegerin (OPG) acts as a decoy receptor by binding to RANKL and blocking the interaction between RANKL and the RANK-receptor and consequently inhibiting osteoclast formation and
activation.
Illustration A depicts the RANK/RANKL involvement in tumor metastatic spread.
Laboratory values of a normal serum calcium and parathyroid hormone can be found in which of the following disease states?
Primary hyperparathyroidism
Type I vitamin D deficient rickets
Type II vitamin D deficient rickets
X-linked hypophosphatemic rickets
Nutritional rickets
Hypophosphatemic rickets is caused by the inability of kidney proximal tubules to reabsorb phosphate due to a mutated PHEX gene, found on the X chromosome. PHEX is thought to protect extracellular matrix glycoproteins from proteolysis. Hypophosphatemic rickets shares many clinical similarities with nutritional rickets but shows PTH levels that are not elevated, even with calcium and phosphate abnormalities.
Pettifor reviews the advances in molecular genetics in the understanding and possible treatments in tumour-induced osteomalacia/rickets.
The review article by Carpenter discusses the X-linked disorder including its clinical manifestations, the wide spectrum of disease severity, and complications of the disease in adult patients.
Illustration A is a table that details the laboratory values associated with each type of rickets.
An 80 year-old female undergoes ORIF of her hip fracture without any complications. A hospitalist consult was obtained for medical clearance pre- operatively, and she was diagnosed with osteoporosis. Which of the following treatment scenarios will lead to the best management of the patient's osteoporosis?
Schedule a follow-up appointment with the patients primary care physician to initiate therapy
Order a physical therapy consult and initiate an exercise plan
Have the patient meet with a nutritionist to increase her calcium and vitamin D intake
Start bisphosphonates, and have the patient follow-up with her primary care physician
Perform a metabolic work-up as an inpatient, and set-up an appointment in an osteoporosis clinic
The initiation of appropriate osteoporosis treatment following hip fractures occurs at a surprisingly low rate. Physical therapy and dietary changes are not appropriate initial treatments for osteoporosis, and bisphosphonate therapy should be prescribed by the physician who will be following and managing the patient's osteoporosis.
Miki et al performed a prospective randomized trial where they compared the rates of osteoporosis treatment initiation. The percentage of patients who were on pharmacologic treatment at 6 months post-injury was 58% in the group whose treatment was directed by the orthopedic surgeon and osteoporosis clinic, and 29% when managed by the primary care physician alone.
The elements chromium, molybdenum, and cobalt are basic components of which of the following implant materials?
Aluminum oxide
Cobalt alloy
Stainless steel
PMMA
Tantalum
Cobalt alloys are extremely strong and are well-suited to applications requiring longevity. Strength of the implant is improved by the addition of molybdenum. Corrosion resistance is addressed by the addition of chromium, which also increases the hardness of the implant.
Incorrect Answers:
Which of the following scenarios of treatment of a humerus fracture best achieves low strain at the fracture site and high stiffness of the treatment construct?
Functional bracing of a transverse midshaft fracture
Comminuted midshaft fracture with locked bridge plating
Short oblique fracture with interfragmentary lag screw and locked neutralization plate
Uniplane external fixation of a spiral open fracture
Oblique fracture with intramedullary nail fixation
Strain in fractures is calculated by dividing the interfragmentary movement by the size of the fracture gap. Strain must be very low (2%) for primary bone healing to occur, and should be less than 10% for secondary bone healing to occur. Stiffness refers the ability of the construct to resist movement under applied loads. Answer 3 describes a situation where primary bone healing is
the goal. For this to occur, there must be no significant gapping at the fracture site, there must be low strain between fracture fragments, and the construct must be stiff.
None of the other answers would accomplish this. Functional bracing and intramedullary fixation both accomplish healing through formation of fracture callus, or secondary healing. A comminuted fracture treated with locked bridge plating relies on less stiffness to allow for secondary healing between fragments. However, since there are many fracture fragments, the strain is distributed among them and therefore remains low. A uniplane external fixator is very unlikely to accomplish low strain and high stiffness in this setting.
A 67-year-old man complains of low-grade fevers and calf pain 2 weeks following a total knee arthroplasty. What is the next appropriate step in management of this patient?
Plethysmography of lower extremity
MRI of lower extremity
CT angiography of lower extremity
Venous ultrasonography
Knee aspiration to evaluate for septic joint
Venous ultrasonography is the next best step in this patient's management, due to the clinical picture of a deep venous thrombosis. The most sensitive and specific recommended diagnostic procedure is a venous ultrasonography.
In their multi-center study, Haut et al. hypothesized that admission to trauma centers that use duplex ultrasound more frequently would independently predict increased DVT reporting for individual patients. They indeed found that trauma centers ultrasound practice was an independent predictor of DVT diagnosis for individual patients, controlling for patient-level risk factors, but concluded the elevated DVT rates at these centers were due to surveillance bias. As such, they recommend that surveillance for DVT should not be considered as a quality control measure in the care of trauma patients.
A patient undergoes closed reduction of a bimalleolar ankle fracture dislocation by the ER physician and is sent to your clinic for evaluation. You evaluate the patient and schedule him for surgery. According to the 2009 guidelines, which of the following scenarios would meet criteria for coding the encounter as a new patient?
You injected his knee in the office almost 3 years ago for osteoarthritis, and have not seen him since
He had an arthroscopic operation by your partner 4 years ago
You were consulted 1 year ago for shoulder pain when he was hospitalized for chronic renal failure
He was seen by your partner in clinic for a herniated disk 2 years ago, but had no procedures performed
You performed a hip replacement on him 12 years ago, and his last follow- up was 18 months ago at which time he was doing well
Only answer two is correct. The 2009 guidlines clarify that the patient can be defined as new only if he has not been seen by anyone in the physician's same group practice and of the same specialty in the past 3 years. Hand and sports medicine specialists with a CAQ, however, are an exception and are allowed to bill for patients already seen by other orthopedists in the same group as new
patients. This scenario would not qualify as a consultation, since the orthopedic surgeon
is taking over care of the patient's problem and is not merely offering advice to another physician who is already caring for the patient. Consultations do not have the same 3 year time qualification. However, Medicare and many other insurers no longer recognize consultation codes.
All the following medications binds reversibly to the enzyme COX-1 EXCEPT
Meloxicam
Diclofenac
Indomethacin
Naproxen sodium
Aspirin
Aspirin binds irreversibly to the cyclooxygenase enzyme. Aspirin acetylates platelet cyclooxygenase and permanently inhibits thromboxane (TX) A2 production leading to its antiplatelet effects. The other NSAID's listed above bind reversibly with COX-1.
Patrono et al discuss the pharmokinetics and platelet effect of both low dose and regular dose aspirin. Nonsteroidal anti-inflammatory drugs compete dose- dependently with arachidonate for binding to platelet cyclooxygenase.
In the treatment of patients with rheumatoid arthritis, TNF-alpha is blocked by which of the following agents?
Tocilizumab
Anakinra
Etanercept
Abatacept
Rituximab
Etanercept is a biochemically designed soluble p75 tumor necrosis factor receptor immunoglobulin G fusion protein, which blocks the downstream
effects of TNF.
Methotrexate is a chemotherapy agent used to inhibit lymphocytes. Gold inhibits monocytes, while sulfasalazine is an anti-inflammatory decreasing the production of
prostaglandins and leukotrienes. Rituximab inhibits B-cells as it
is a monoclonal antibody to CD20 antigen. Anakinra (Kineret) is a recombinant IL-1 receptor antagonist. Abatacept (Orencia) is a selective costimulation modulator that binds to CD-80 and CD-86 (inhibits T cells). Tocilizumab (Actemra)is an IL-6 receptor inhibitor (2nd line treatment for poor response to TNF-antagonist therapy).
Pisetsky wrote an editorial in NEJM discussing the development of TNF blockers through research, and the potential for the use of Etanercept in patients with juvenile RA through its inhibition of lymphotoxin-alpha.
Which of the following medications when combined with methotrexate has been shown to be more effective than methotrexate alone in the treatment of rheumatoid arthritis?
Nitrofurantoin
Rifampin
Azithromycin
Erythromycin
Doxycycline
Tetracycline was initially used in the treatment of rheumatoid arthritis (RA) because Mycoplasma was thought to be the causative agent. It was later found that tetracyclines have biologic effects on the inflammatory and immunologic cascade by inhibiting collagenase activity. Collagenase is an enzyme involved
in breaking down macromolecules in the connective tissue, contributing to the pathologic changes of RA.
In a prospective study, O'Dell et al found that initial therapy with methotrexate plus doxycycline was superior to treatment with methotrexate alone. Furthermore, similar results for low-dose and high-dose doxycycline suggested that antimetalloproteinase effects were more important than the antibacterial effects.
When using C-arm fluorocopy, patient radiation exposure will be increased with which of the following?
The extremity is positioned closer to the image intensifier
A larger body part is imaged compared to a smaller body part
Use of radiation beam collimation
Mini C-arm fluroscopy is used instead of large C-arm fluroscopy
Decreased duration of imaging
Patient radiation exposure will be increased if a larger body part is imaged compared to a smaller body part.
The first study by Giordano et al used radiation dosimeters for large and mini c-arm machines. They found that elevated exposure levels can be expected when larger body parts are imaged, when the extremity is positioned closer to the x-ray source, and when the large c-arm is used over the mini c-arm.
The second study by Giordano et al also used dosimeters for a mini c-arm and found that the surgical team is exposed to minimal radiation during routine
use of mini-c-arm fluoroscopy, except when they are in the direct path of the radiation beam. They list factors to decrease radiation exposure to patient and surgeon including: minimizing exposure time, reducing exposure factors, manipulating the x-ray beam with collimation, orienting the fluoroscopic beam in an inverted position relative to the patient, strategic positioning of the surgeon within the operative field, judicious use of protective shielding during imaging, and maximizing the distance of the surgeon from the radiation beam.
Illustration A shows that arrangement #1 has the body part half-way between the radiation source and image intensifier. Arrangement #2 has the the image intensifier acting as an arm table for the body part with the radiation source further away. Arrangement #1 has more radiation exposure than #2. The distance between the x-ray tube and the body part is doubled in arrangement
#2 compared to arrangement #1. This increased distance correlates to a reduction in exposure according to the inverse square law (reduction in radiation intensity with greater distance from the x-ray source).
You are seeing a 13-year-old girl for asymptomatic flat feet and recommend observation. In educating this patient/family about general bone health, you recommend what amount of daily dietary calcium for your patient?
Question 27
Osteolysis, after total knee arthroplasty performed without cement, most often occurs in the
Explanation
factors. First gravity and weight bearing through the medial side of the knee tend to localize the debris particulate polyethylene on the tibial side. Second, on the femoral side if the osteolytic process is initiated along the implant-bone interface, the flanges of the femoral implant obscure a radiographic diagnosis. Finally, the addition of screws to the tibial implant provide avenues for the migration of debris into the bone. In the patients with osteolysis all had very large amounts of polythylene and metal particles less than one micrometer in size leading to intense histiolytic response.
Question 28
A 38-year-old man has winging of the ipsilateral scapula after undergoing a transaxillary resection of the first rib 3 weeks ago. What is the most likely cause of this finding?
Explanation
REFERENCES: Leffert RD: Thoracic outlet syndrome. J Am Acad Orthop Surg 1994;2:317-325.
Todd TW: The descent of the shoulder after birth: Its significance in the production of pressure-symptoms on the lowest brachial trunk. Anat Anz 1912;41:385-397.
Question 29
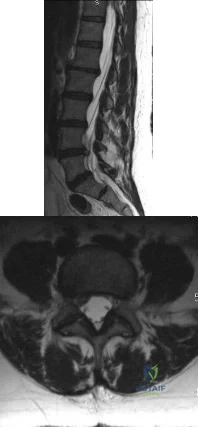
A 45-year-old female returns to your clinic with 10-weeks of severe pain that starts in her back and extends down her right leg to the top of her foot. On physical exam she has decreased sensation on the dorsal aspect of her foot and 4/5 strength in her EHL. She has a positive straight leg raise on the right. The remaining physical exam is unremarkable, including normal achilles and patellar reflexes bilaterally, no clonus, and a down-going Babinski sign. Her pain has not been relieved by NSAIDs, epidural steroids or physical therapy. Figure A is a sagittal MRI and figure B is a axial MRI through the L4/5 disc space. What is the best treatment option at this time? Review Topic
Explanation
Patients with paracentral herniated lumbar discs present with radicular pain affecting the traversing (caudal) nerve root. Unless the patient develops progressive neurologic decline, patients with herniated lumbar discs should undergo no less than 6 weeks of conservative treatment consisting of anti-inflammatory medications, rest and therapy. Most patients improve with nonoperative modalities. If appropriate conservative care fails, the correct surgical option is a unilateral microdiscectomy.
In the Spine Patient Outcomes Research Trial (SPORT) Weinstein et al. reported on the results of 501 patients with herniated lumbar discs who had failed at least six weeks of non-operative care. The patients were randomized to operative or nonoperative care, however there was a high amount of crossover between the two groups. Because of this, there was no difference reported between the two groups at final follow-up using an intent-to-treat analysis.
Weinstein et al., because of the flaws with the intent-to-treat analysis, also published an observational study on 528 patients who received surgery and 191 who received nonoperative care for a herniated lumbar disc. They reported that while both groups had an improvement from baseline, at two years, patients who elected to undergo surgery had significantly better outcomes than those who chose conservative care.
Lurie et al. reported the eight-year results from the observational group of the SPORT data, and found that the patients who underwent surgery continued to have statistically superior outcomes compared to those who underwent conservative care at long-term follow-up.
Figure A is a T2 sagittal MRI of the lumbar spine demonstrating a right sided L4/5 disc herniation, and Figure B is an axial image again demonstrating a paracentral L4/5 disc herniation.
Incorrect answers:
Question 30
A 72-year-old woman is evaluated for sacrococcygeal pain sustained after a twisting injury. Radiographic and MRI evaluation confirms the presence of a nondisplaced fracture at the sacrococcygeal junction. Over a 3-week period, the pain has gotten significantly better. No additional lesions or injuries are noted. Laboratory studies show a serum calcium level of 8.8 mg/dL (normal 8.6-10.3 mg/dL) and a 25-OH Vitamin D level of 14 ng/mL (normal 30-80 ng/mL). What is the most appropriate treatment for this patient?
Explanation
Question 31
The artery located within the substance of the coracoacromial ligament is a branch of what artery?
Explanation
REFERENCES: Esch JC, Baker CL: The shoulder and elbow, in Whipple TL (ed): Arthroscopic Surgery. Philadelphia, PA, JB Lippincott, 1993, pp 65-66.
Woodburne RT (ed): Essentials of Human Anatomy, ed 2. New York, NY, Oxford University Press, 1983, pp 75-76.
Question 32
Two major pharmacologic classes of bisphosphonates exist: nitrogen-containing and non-nitrogen-containing compounds. The nitrogen-containing compounds work by which of the following actions?
Explanation
Question 33
- Which of the following radiographic views best shows the size and displacement of a posterior wall fracture of the acetabulum?
Explanation
Question 34
A 48-year-old woman reports bilateral thigh pain that is limiting her function as a librarian. A radiograph and a bone scan are shown in Figures 23a and 23b. What is the most likely diagnosis?
Explanation
REFERENCES: Resnick D: Diagnosis of Bone and Joint Disorders, ed 3. Philadelphia, PA,
WB Saunders, 1995, pp 956-957.
Wheeless’ Textbook of Orthopaedics: Acetabular Protrusio. www.wheelessonline.com/ortho/acetabular_protrusio
Question 35
The most appropriate next surgical procedure is
Explanation
This patient’s arthritis likely has progressed to the lateral compartment. The location and degree of local pain and tenderness are the most important physical findings. History and physical findings indicate arthritis progression to the lateral and anterior compartments. This scenario suggests the need for conversion of the unicompartmental arthroplasty to TKA.
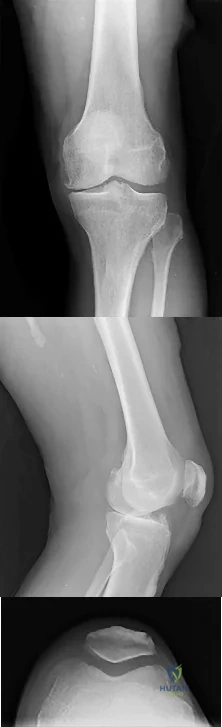
Question 36
A 50-year-old man reports left shoulder pain and weakness after undergoing a lymph node biopsy in his neck 2 years ago. Examination reveals winging of the left scapula. Electromyography shows denervation of the trapezius. Surgical treatment for this condition involves Review Topic
Explanation
Question 37
You are interested in learning a new technique for minimally invasive total knee arthroplasty. The Keyhole Genuflex system seems appealing to you because the instrumentation comes with wireless controls. Which of the following represents an acceptable arrangement?
Explanation
REFERENCES: AAOS Standard of Professionalism -Orthopaedist -Industry Conflict of Interest (Adopted 4/18/07), Mandatory Standard numbers 6, 9, 12-15. http://www3.aaos.org/member/profcomp/SOPConflictsIndustry.pdf
The Orthopaedic Surgeon’s Relationship with Industry, in Guide to the Ethical Practice of Orthopaedic Surgery, ed 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2007. http://www.aaos.org/about/papers/ethics/1204eth.asp
AdvaMed Code of Ethics on Interactions with Health Care Professionals 2005. http://www.advamed.org/MemberPortal/searchresults.htm?query=Advamed%20Code%20of%20Ethics%20on%20Interactions%20with%20Health%20Care%20Professionals%202005
Question 38
Figure 10 shows the radiograph of a 9-year-old girl who injured her left lower leg after being thrown from a horse. Examination reveals no other injuries. Which of the following forms of management will provide the lowest rate of complications and the earliest return to function?
Explanation
REFERENCES: Ligier JN, Metaizeau JP, Prevot J, Lascombes P: Elastic stable intramedullary nailing of femoral shaft fractures in children. J Bone Joint Surg Br 1988;70:74-77.
Heinrich SD, Drvaric D, Darr K, MacEwen GD: Stabilization of pediatric diaphyseal femoral fractures with flexible intramedullary nails (a technique paper). J Orthop Trauma 1992;6:452-459.
Question 39
During treatment of rupture of the subscapularis tendon with associated biceps instability, treatment of the biceps tendon should include which of the following? Review Topic
Explanation
the restraints to medial translations of the biceps have been disrupted. Attempts at recentering the biceps have not been successful, and clinical results appear to be improved when tenodesis or tenotomy is employed in the treatment of the unstable biceps associated with subscapularis tears.
Question 40
A 28-year-old woman has had pain in her hand and mild swelling of the little finger for the past 2 months. A radiograph is shown in Figure 41a, and the biopsy specimen is shown in Figures 41b and 41c. What is the most likely diagnosis?
Explanation
REFERENCES: Wold LE, Adler CP, Sim FH, et al: Atlas of Orthopedic Pathology, ed 2. Philadelphia, PA, WB Saunders, 2003, p 225.
McCarthy EF, Frassica FJ: Pathology of Bone and Joint Disorders with Clinical and Radiographic Correlation. Philadelphia, PA, WB Saunders, 1998, p 227.
Question 41
Complications following a reverse shoulder prosthesis occur most frequently when performed for what diagnosis? Review Topic
Explanation
Question 42
Which of following is pathognomonic of intervertebral disk degeneration? Review Topic
Explanation
large proteoglycan molecules in
the nucleus pulposus is
pathognomonic
of intervertebral disk
(IVD) degeneration.
Degeneration of the intervertebral disk (IVD) is a major pathological process implicated in low back pain and is often considered a prerequisite for intervertebral disc herniation. While the pathophysiologic causes of IVD degeneration at the molecular level are not fully known, there are many physical and molecular changes that are known to contribute to the disease process. The most significant is loss of large proteoglycan molecules and decreased water content.
An et al. showed that large proteoglycans (PGs), such as aggrecan and versican, decrease in patients with intervertebral disk (IVD) degeneration.
Kepler et al. reviewed IVD degeneration. They report that degeneration leads to changes in the expression of matrix proteins, cytokines, and proteinases. They suggest treatment with gene therapy, such as Growth and Differentiation Factor-5 (GDF-5), may help to promote the healing of degenerated intervertebral disks.
Illustration A shows a cadaveric image of normal disk anatomy (left) and IVD degeneration (right)
Incorrect Answers:
Question 43
A surgeon prepares a medial gastrocnemius rotational flap to cover a medial proximal tibia defect at the time of revision knee replacement surgery. To optimize coverage, the surgeon must optimally mobilize which artery?
Explanation
The medial sural arteries vascularize the gastrocnemius, plantaris, and soleus muscles proximally. These arteries arise from the popliteal artery. If this artery is not adequately mobilized, a gastrocnemius soleus flap can be devascularized.
Question 44
Figures 29a and 29b show the radiographs of a 13-year-old competitive gymnast who has had elbow pain for the past 2 weeks. The pain is worse with tumbling activities. Examination reveals a mild effusion and slight limitation of extension and forearm rotation with no locking. Initial management should consist of
Explanation
REFERENCES: Maffulli N, Chan D, Aldridge MJ: Derangement of the articular surfaces of the elbow in young gymnasts. J Pediatr Orthop 1992;12:344-350.
Bauer M, Jonsson K, Josefsson PO, Linden B: Osteochondritis dissecans of the elbow: A long-term follow-up study. Clin Orthop 1992;284:156-160.
Tivnon MC, Anzel SH, Waugh TR: Surgical management of osteochondritis dissecans of the capitellum. Am J Sports Med 1976;4:121-128.
Question 45
Where is the watershed zone for tarsal navicular vascularity?
Explanation
REFERENCES: Nunley JA, Pfeffer GB, Sanders RW, et al (eds): Advanced Reconstruction: Foot and Ankle. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004,
pp 239-242.
Sarrafian SK: Anatomy of the Foot and Ankle. Philadelphia, PA, JB Lippincott, 1983,
pp 299-302.
Question 46
During the cocking and acceleration phases of the overhand throw (pitch), there are several static and dynamic restraints to provide medial elbow support and prevent valgus instability. The dynamic structures found to be most important during these phases of the overhand throw are the flexor digitorum Review Topic
Explanation
Question 47
A 78-year-old man is seen in the emergency room 3 hours after a fall from a standing position. The patient sustained a mild scalp laceration and the injury shown in Figure 90. He reports severe neck pain and is unable to move his hands and legs. Examination reveals absent motor function in the wrist flexors, triceps, and fingers. He cannot move his lower extremities during motor testing. The patient has some sensation in the lower extremities. Bulbocavernosus reflex is absent. Based on examination findings and the imaging findings, what is the most definitive treatment option? Review Topic
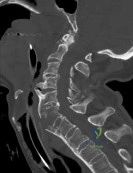
Explanation
(SBQ13PE.22) A 11-year-old male is referred for evaluation of scoliosis by his primary care physician. He has a normal birth and development history and denies any neurologic deficits or pain. On physical examination, he is neurologically intact with normal reflexes and tone. A PA radiograph is shown in Figure A. What is the next best step? Review Topic
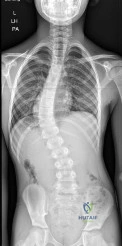
Custom orthosis prescription to initiate bracing
Physical therapy referral and observation
Bending and lumbar oblique radiographs
Total spine CT
Total spine MRI
A left thoracic curve is an abnormal finding and warrants further work-up with a total axis MRI in order to rule out concomitant neurologic abnormalities such as a spinal cord cyst and/or syrinx.
In adolescent idiopathic scoliosis (AIS), the most commonly occurring curve is a right thoracic curve. Left thoracic curves are not as common, and warrants total axis MRI in order to rule out concomitant central axis abnormalities. This is imperative not only during initial work-up, but most importantly for operative planning.
Spiegel et al. performed a a retrospective radiographic review on 41 patients with scoliosis associated with a Chiari I malformation and/or syringomyelia. Approximately 50% of patients had an "atypical" pattern (left thoracic, double thoracic, triple, long right thoracic). The authors recommend that MRI should be considered in these patients.
Gillingham et al. provides a thorough review of early onset scoliosis and notes the relatively high incidence of concurrent central axis abnormalities, even in patients with normal neurologic exams. Rates have been reported upwards of 21.7%, with malformations including Chiari Type 1, dural ectasias, syrinx, and spinal cord cysts.
Figure A exhibits a left thoracic curve. Further imaging in this patient revealed a syrinx which required decompression.
Incorrect answers:
thoracic
curve.
Question 48
What range of motion parameters are required for a patient with posttraumatic elbow stiffness to accomplish all the normal activities of daily living?
Explanation
REFERENCES: Kasser JR (ed): Orthopaedic Knowledge Update 5. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1996, pp 283-294.
Morrey BF, Askew LJ, Chao EY: A biomechanical study of normal functional elbow motion. J Bone Joint Surg Am 1981;63:872-877.
Question 49
A 40-year-old man has a palpable mass over the dorsum of the ankle. He reports no history of direct trauma but notes that he sustained a laceration to the middle of his leg 6 weeks ago. Examination reveals a 4-cm x 1-cm mass. T 1 - and T 2 -weighted MRI scans are shown in Figures 12a and 12b. An intraoperative photograph and biopsy specimen are shown in Figures 12c and 12d. What is the most likely diagnosis?
Explanation
REFERENCES: Otte S, Klinger HM, Loreaz F, Haerer T: Operative treatment in case of closed rupture of the anterior tibial tendon. Arch Orthop Traum Surg 2002;122:188-190.
Kausch T, Rutt J: Subcutaneous rupture of the tibialis anterior tendon: Review of the literature and case report. Arch Orthop Traum Surg 1998;117:290-293.
Question 50
Intraoperative frozen section analysis reveals 10 neutrophils per high-power field and a positive gram stain result. What is the best next step?
Explanation
The radiograph reveals a rotator cuff dysfunction secondary to malpositioning of the humeral stem and a nonanatomic humeral head. Glenohumeral kinematics have been altered, resulting in damage to the rotator cuff, which in turn has led to impingement with the coracoacromial arch. This single radiograph reveals excessive humeral head height, “overstuffing” of the joint, and severe narrowing of the acromiohumeral interval. Osteolysis and implant loosening are not radiographically apparent. An orthogonal view (axillary lateral) would be necessary to evaluate for shoulder instability. A CT arthrogram is the most appropriate advanced imaging test in the setting of a retained shoulder arthroplasty to evaluate the integrity of the rotator cuff. An MRI evaluation would be obfuscated by artifact. Three-phase and indium-tagged white blood cell scans may be appropriate in the setting of an occult infection evaluation, but not as a test to evaluate rotator cuff injury.
In the absence of infection with rotator cuff compromise, the most appropriate procedure(s) during revision would involve humeral component explantation and conversion to rTSA Revision anatomic hemiarthroplasty may provide pain relief, but function may not appreciably change because of the unbalanced forced couples of the rotator cuff complex. Placement of a glenoid component in the setting of an irreparable rotator cuff tear is contraindicated because rapid glenoid loosening will occur due to eccentric loading during active shoulder motion. Resection arthroplasty should be reserved for recalcitrant cases of infection because this procedure does not provide functional improvement.
In the event that frozen section analysis and positive gram stain results indicate an infection, the treating surgeon should remove all components, perform a thorough debridement and irrigation of suspect tissue, implant an antibiotic spacer, and perform a second-stage reconstruction when deemed appropriate (in light of laboratory studies, repeat shoulder aspiration, frozen section analysis, and arthroscopic soft-tissue biopsy findings). Irrigation and debridement with primary exchange/conversion of components remains inferior to 2-stage reconstruction for infection eradication. Resection arthroplasty remains a salvage procedure for resistant cases that preclude reimplantation and generally is performed for symptom control and sepsis prevention.
RECOMMENDED READINGS
Bohsali KI, Wirth MA, Rockwood CA Jr. Complications of total shoulder arthroplasty. J Bone Joint Surg Am. 2006 Oct;88(10):2279-92. Review. PubMed PMID: 17015609. View Abstract at PubMed
Florschütz AV, Lane PD, Crosby LA. Infection after primary anatomic versus primary reverse total shoulder arthroplasty. J Shoulder Elbow Surg. 2015 Aug;24(8):1296-301. doi: 10.1016/j.jse.2014.12.036. Epub 2015 Feb 19. PubMed PMID: 25704211. View Abstract at PubMed
Padegimas EM, Maltenfort M, Ramsey ML, Williams GR, Parvizi J, Namdari S. Periprosthetic shoulder infection in the United States: incidence and economic burden. J Shoulder Elbow Surg. 2015 May;24(5):741-6. doi: 10.1016/j.jse.2014.11.044. Epub 2015 Jan 13. View Abstract at PubMed
Leung B, Horodyski M, Struk AM, Wright TW. Functional outcome of hemiarthroplasty compared with reverse total shoulder arthroplasty in the treatment of rotator cuff tear arthropathy. J Shoulder Elbow Surg. 2012 Mar;21(3):319-23. doi: 10.1016/j.jse.2011.05.023. Epub 2011 Aug 26. PubMed PMID: 21872496. View Abstract at PubMed
Iannotti JP, Spencer EE, Winter U, Deffenbaugh D, Williams G. Prosthetic positioning in total shoulder arthroplasty. J Shoulder Elbow Surg. 2005 Jan-Feb;14(1 Suppl S):111S-121S. PubMed PMID: 15726070. View Abstract at PubMed
Iannotti JP, Gabriel JP, Schneck SL, Evans BG, Misra S. The normal glenohumeral relationships. An anatomical study of one hundred and forty shoulders. J Bone Joint Surg Am. 1992 Apr;74(4):491-500. PubMed PMID: 1583043.View Abstract at PubMed
Grosso MJ, Frangiamore SJ, Ricchetti ET, Bauer TW, Iannotti JP. Sensitivity of frozen section histology for identifying Propionibacterium acnes infections in revision shoulder arthroplasty. J Bone Joint Surg Am. 2014 Mar 19;96(6):442-7. doi: 10.2106/JBJS.M.00258. View Abstract at PubMed
Question 51
Closed reduction and functional bracing would lead to significant upper extremity disability due to malunion.
Explanation
The referenced review article by Michelson covers rotational ankle fractures, with a review of the diagnosis, treatment options, and patient outcomes. He notes that unstable fractures (bimalleolar, bimalleolar equivalent, etc.) usually are managed with open reduction and internal fixation for optimal outcomes.
Incorrect answers:
Figure B shows a Weber C (high fibular) ankle fracture, PER, without any evidence of a medial malleolar fracture.
Figures C (SER IV), D (PER IV), and E (isloated medial malleolar fracture) all show fractures not suitable for screw fixation of the medial malleolus parallel to the joint since their fracture lines are not vertical.
OrthoCash 2020
Which of the following is an advantage of using blocking screws for tibial nailing?
Decrease risk of nail breakage
Eliminate use of interlocking screws
Allow for larger nail use
Enhance construct stiffness
Decrease torsional rigidity Corrent answer: 4
Blocking screws can be used to help obtain and maintain reductions, increase construct stiffness, and neutralize translational forces. There are no studies as of yet that find a blocking screw to decrease nail failure.
Krettek found that medial and lateral blocking screws can increase the primary stability of distal and proximal metaphyseal fractures after nailing and can be an effective tool for selected cases that exhibit malalignment and/or instability by decreasing mechanically measured deformation.
In a later clinical study, Krettek found that after using blocking screws, tibial healing was evident radiologically at a mean of 5.4 months with a decreased
rate of malunions.
Ricci also found that blocking screws are effective to help obtain and maintain alignment of fractures of the proximal third of the tibial shaft treated with intramedullary nails.
OrthoCash 2020
Following operative repair of lower extremity long bone and periarticular fractures, what is the time frame for patients to return to normal automobile braking time?
6 weeks after initiation of weight bearing
4 weeks postoperatively
8 weeks from the date of injury
Once full range of motion of the ankle and knee exist
At the time of bony union Corrent answer: 1
According to the first referenced study by Egol et al, appropriate braking time returns at a point 6 weeks after initiation of weightbearing after treatment of lower extremity long bone and periarticular fractures, as examined with a driving simulator. No differences were seen in return of braking time between periarticular fractures and long bone injuries.
The second reference by Egol studied only operatively treated ankle fractures and found that time to appropriate braking returns at 9 weeks postoperatively. Interestingly, no significant association was found between the functional scores and normalization of total braking time.
OrthoCash 2020
A 42-year-old male sustains the injury seen in figure A. What negative sequelae would occur with displacement of this fracture in the characteristic fashion?
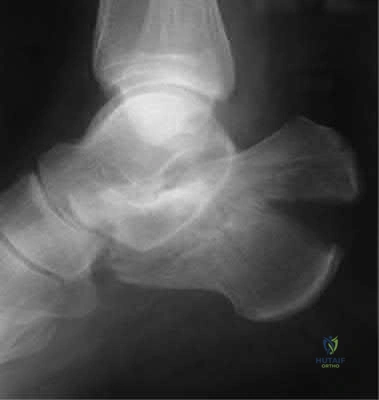
Post-traumatic subtalar arthrosis
Stress fracture of the fibula
Reflex sympathetic dystrophy
Achilles tendon rupture
Posterior skin necrosis Corrent answer: 5
The radiograph shows a tongue-type calcaneus fracture, with major displacement of the posterior calcaneal body/tuberosity. The Achilles tendon insertion here causes characteristic proximal and posterior displacement, and with increasing displacement, posterior skin necrosis can be caused in a short period. Per the references, this should be treated urgently to prevent this sequelae. Lag screw fixation is appropriate for this fracture pattern, placed perpendicular to the fracture.
OrthoCash 2020
A 34-year-old male falls 10 feet from a balcony and is brought to the emergency room with the deformity seen in Figure A. Radiographs shown are shown in Figure B and C. Which of the following structures can block closed reduction of this injury pattern?
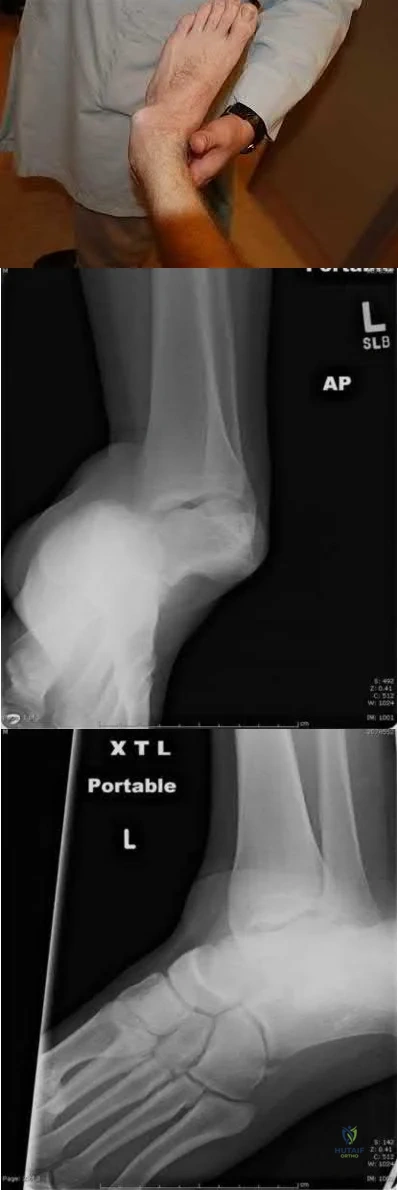
Flexor hallucis longus tendon
Extensor digitorum brevis muscle
Posterior tibial tendon
Tibialis anterior tendon
Plantar fascia
Figures A through C show a medial subtalar dislocation. Irreducible dislocations are typically the result of either inadequate sedation or interposed soft tissue structures.
In medial dislocations, the extensor digitorum brevis, the deep peroneal neurovascular bundle, or the joint capsule may block a closed reduction. In lateral dislocations, the most common structure implicated as a block to reduction is the posterior tibial tendon, although the flexor digitorum longs, posterior tibial neurovascular bundle or flexor hallucis may also block reduction.
Bibbo et al found that subtalar dislocations were irreducible 32% of the time and that 88% had ipsilateral foot and ankle injuries. At follow up, 89% of patients demonstrated radiographic changes of the subtalar joint, and had worse function on the side of the subtalar dislocation as demonstrated by lower
AOFAS scores.
Incorrect Answers:
OrthoCash 2020
Spontaneous rupture of the extensor pollicis longus tendon is most frequently associated with which of the following scenarios?
Non-displaced distal radius fracture
Non-displaced Rolando fracture
Second metacarpal base fracture
Boxer's fracture
Non-displaced radial styloid fracture Corrent answer: 1
Rupture of the extensor pollicis longus (EPL) tendon after non operative treatment for a distal radius fracture occurs with a 0.3-5% incidence. The causes of EPL rupture include mechanical irritation, attrition, and vascular impairment leading to delayed rupture. Synovitis of the extensor carpi radialis due to repetitive use may invade the EPL tendon and lead to rupture.
Recommended treatment in the pre-rupture setting includes a third dorsal compartment release with or without an extensor retinacular patch graft. Palmaris longus graft or a transfer from the extensor indicis proprius to the EPL tendon are reasonable treatment options. Results of all treatments seem to be clinically satisfactory.
The referenced article by Gelb is a review of the etiology and treatment of this injury. He reviews the above discussion and findings.
OrthoCash 2020
A 79-year-old cyclist is involved in an accident and sustains a displaced femoral neck fracture as seen in Figure A. What is the
optimal treatment?
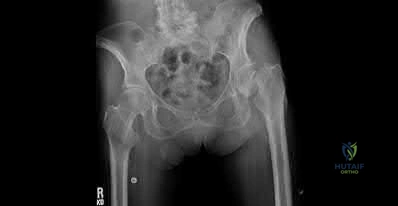
Open reduction internal fixation
Bipolar hemiarthroplasty
Unipolar hemiarthroplasty
Total hip arthoplasty
Nonoperative treatment
An AP pelvis radiographs with a displaced femoral neck fracture is seen in Figure A. It important to note that degenerative changes are seen on this image. Both references suggest that elderly active individuals should be treated with a primary total hip after displaced femoral neck fractures.
In the first study by Blomfeldt et al, the group reviewed a series of patients who underwent either an acute primary total hip arthroplasty for a femoral neck fracture or a delayed primary hip after an attempt at ORIF. They found that the group treated with an acute primary total hip arthroplasty had better Harris hip and quality of life scores.
The second reference from Blomfeldt et al, studies a population of active elderly patients randomized to either a total hip arthroplasty or bipolar for femoral neck fractures. The group found no mortality or dislocation difference between the groups, but higher Harris hip scores at 1 year in patients treated with a total hip
arthroplasty.
OrthoCash 2020
A 53-year-old man sustains the injury seen in figure A and later undergoes open reduction and internal fixation. What variable will
most significantly increase his rate of degenerative arthritis in the long-term?
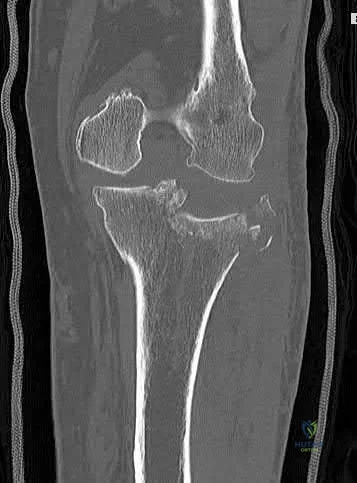
Postoperative joint stepoff
Alteration of limb mechanical axis
Fracture type
Male sex
Age greater than 50
Maintenance of mechanical axis correlates most with a satisfactory clinical outcome when managing an intra-articular fracture of the proximal tibia.
According to the study of plateau fractures with up to 27 year follow-up by Rademakers et al, malalignment of the limb by greater than 5 degrees tripled the rate of degenerative osteoarthritis (27% v. 9%). Age at time of injury had no effect on outcome; 31% had joint space narrowing but 64% of those knees were well tolerated.
Weigel and Marsh's study looked at high energy plateau fractures treated with staged external fixation followed by internal fixation, and noted a low rate of severe arthrosis even with mild to moderate joint incongruity.
Stevens et al noted a worse outcome with increasing age at presentation with these injuries; fracture type had a small influence and adequacy of reduction had no significant influence on outcome.
Figure A is a coronal CT image showing a lateral tibial plateau fracture with significant joint depression.
OrthoCash 2020
A 69-year-old male sustained a proximal humerus fracture that underwent open reduction and internal fixation nine months ago. He complains of constant pain and weakness; repeat radiographs are shown in Figures A and B. What is the most appropriate surgical treatment at this time?
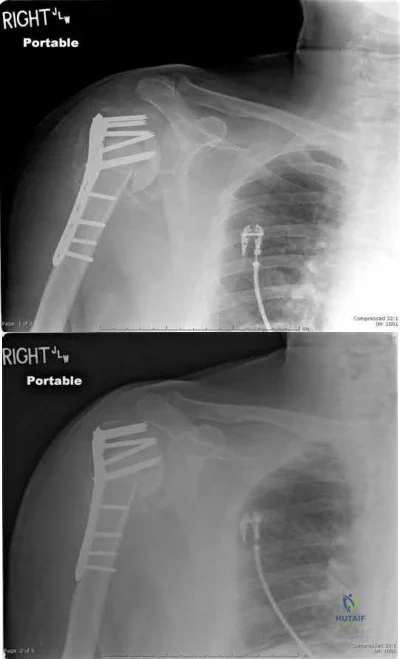
Revision open reduction and internal fixation
Valgus corrective osteotomy of proximal humerus
Shoulder arthroplasty
Shoulder arthrodesis
Humeral head resection Corrent answer: 3
Figures A and B show loss of fixation of a proximal humerus fracture. The most appropriate treatment for this scenario is a humeral arthroplasty, as the tenuous blood supply of the proximal humerus is likely chronically disrupted, leading to osteonecrosis and poor healing potential of the proximal humerus.
Traditionally, hemiarthroplasty was performed for these presentations, but reverse total shoulder arthroplasty has emerged as a potentially better
treatment method, especially if the rotator cuff function/status is unknown or poor.
According to the referenced article by Norris et al, delayed shoulder hemiarthroplasty decreased shoulder pain in 95% of patients but warned of technical difficulties and limited postoperative range of motion. A total shoulder arthroplasty is needed if glenoid erosion from the screw(s) or bone occurs.
OrthoCash 2020
During the ilioinguinal approach to the pelvis, the corona mortis artery must be identified and ligated if present. The corona mortis artery joins the external illiac artery with which other major artery?
Pudendal
Deep illiac circumflex
Hypogastric
Obturator
Testicular
The "corona mortis" (translated as “crown of death”) artery is a vascular variant that joins the external illiac and the obturator artery as it crosses the superior pubic ramus. Tornetta et al did a study where "fifty cadaver halves were dissected to determine the occurrence and location of the corona mortis. Anastomoses between the obturator and external iliac systems occurred in 84% of the specimens. Thirty-four percent had an arterial connection, 70% had a venous connection, and 20% had both. The distance from the symphysis to the anastomotic vessels averaged 6.2 cm (range, 3-9 cm)." The corona mortis can be injured in superior ramus fractures and iatrogenically while plating pelvic ring injuries using the ilioinguinal approach.
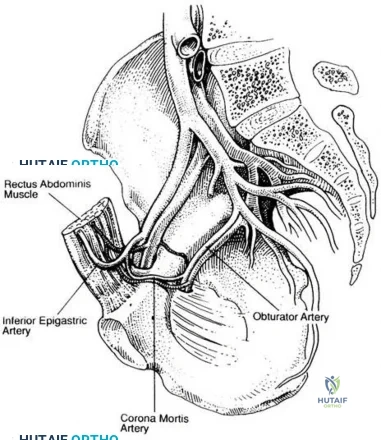
OrthoCash 2020
A 26-year-old male sustains a femoral shaft fracture treated with the implant shown in Figure A. Postoperatively, what muscular deficits can be expected at medium and long-term follow-up?
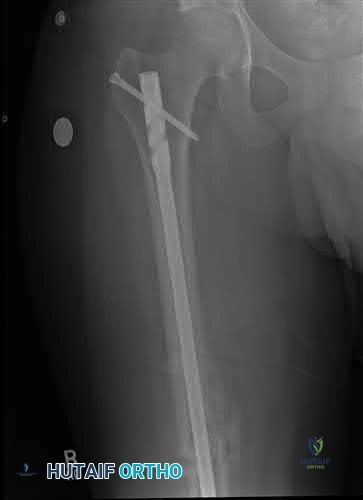
Weakness with hip abduction and knee flexion
Weakness with hip abduction and knee extension
Weakness with knee flexion and knee extension
Weakness with hip external rotation and hip abduction
Weakness with hip external rotation and hip flexion Corrent answer: 2
Figure A shows a femoral shaft fracture treated with an antegrade femoral nail. Long term deficits are weakness with knee extension (quadriceps) and hip abduction (glutei muscles).
The referenced study by Kapp et al noted long term quadriceps weakness as well as decreased bone mineral density in the femur (femoral neck by 9%, the lateral cortex by 20% and the medial cortex by 13%). It is unclear whether this is due to the injury, treatment, or a combination of both.
The second referenced study by Archdeacon et al also noted weakness in hip abduction, which showed time dependent improvement. He reports that increased early ipsilateral trunk lean is associated with worse recovery of abduction strength.
OrthoCash 2020
A 33-year-old male sustains the injury seen in Figure A as a result of a high-speed motor vehicle collision. Based on this image, what is the most likely acetabular fracture pattern?
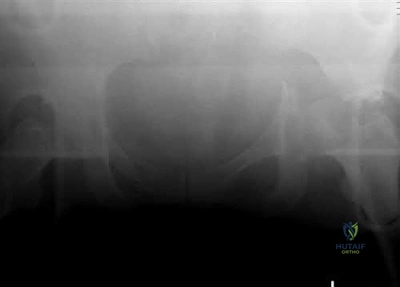
Both column
Anterior column
Anterior column posterior hemitransverse
Transverse
T-type
The radiograph in Figure A shows a transverse acetabulum fracture. The iliopectineal (anterior column) and ilioischial lines (posterior column) are interrupted, revealing bicolumnar involvement; however, this is different than the both column fracture, as a transverse pattern has articular surface still in continuity with the axial skeleton via the sacroiliac joint.
The referenced article by Patel et al showed a wide variation of inter and intra-observer agreement in interpreting radiographs of acetabular fractures, with high agreement for basic radiographic classification and only slight to moderate agreement for other radiologic variables such as impaction.
The other referenced article by Letournel is a great review article regarding the initial classification of these fractures as well as a quick summary of his outcomes.
OrthoCash 2020
A 56-year-old carpenter sustains the closed injury seen in Figures A, B, and C. After temporary spanning external fixation is performed and soft tissue conditions improve, what strategy provides the optimal fixation for this fracture pattern?
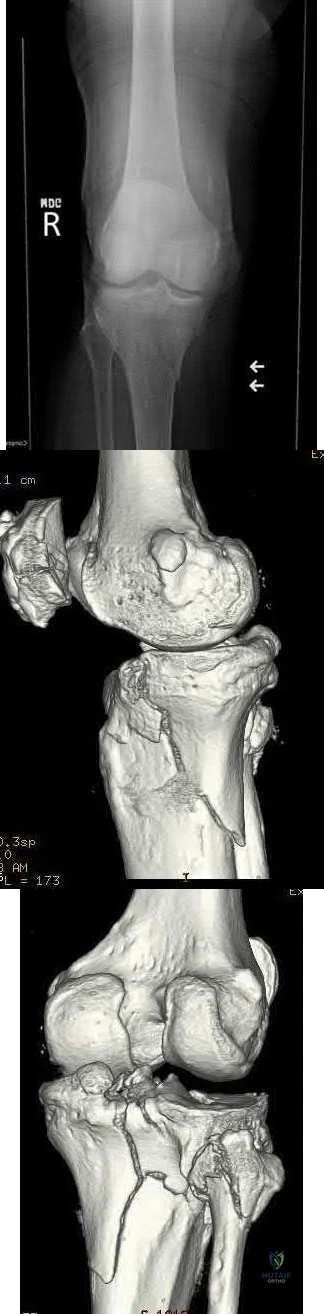
Anatomic lateral locking plate
Posteromedial and lateral plates
Anatomic medial locking plate
Conversion of the spanning external fixator to a hinged external fixator
Posterior buttress plate Corrent answer: 2
Figures A and B show a bicondylar tibial plateau fracture, with a typical appearing lateral fracture line and a posteromedial fracture line. The posteromedial sheared fracture piece is difficult, and/or sometimes impossible, to achieve appropriate stable fixation with a single lateral locking plate, as there will be limited screw purchase and fixation into the posteromedial fragment.
The referenced article by Georgiadis notes that a dual incision approach is safe and is associated with improved outcomes over their historical comparisons.
They describe the dual incisions and approaches in length, and review risks/issues with each approach.
The other referenced study by Bhattacharyya et al notes that these fractures have a typical appearance of the posteromedial fracture piece and that articular reduction quality is correlated with short-term results. They recommended buttress-type fixation of these fracture pieces.
OrthoCash 2020
A 31-year-old male sustains an irreducible ankle fracture-dislocation with the foot maintained in an externally rotated position. An AP and lateral radiograph are shown in figures A and B respectively. The attempted post reduction AP and lateral are shown in C and D. What structure is most likely preventing reduction?
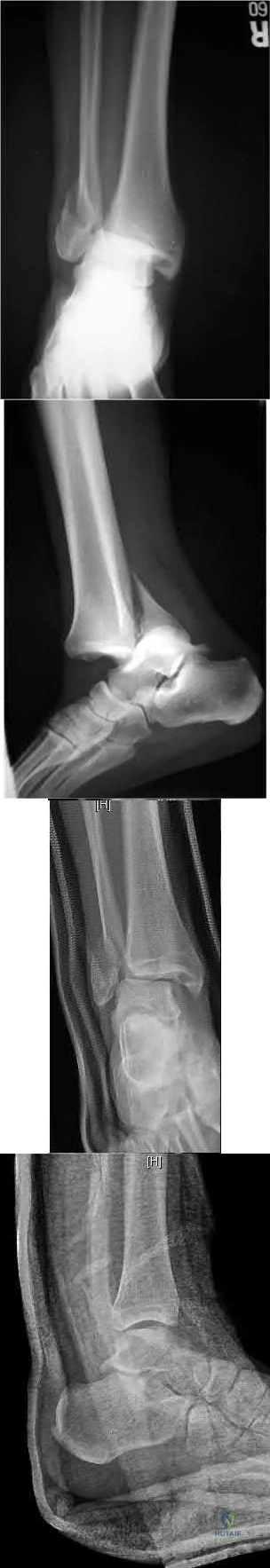
Anterior-inferior tibiofibular ligament
Posterior-inferior tibiofibular ligament
Peroneus brevis tendon
Posterolateral ridge of the tibia
Flexor hallucis longus tendon Corrent answer: 4
As described by Hoblitzell et al, the so-called "Bosworth fracture-dislocation" is a rare fracture-dislocation of the ankle where the fibula becomes entrapped behind the tibia and becomes irreducible. It can cause compartment syndrome, as reported by Beekman and Watson.
Hoblitzell et al stress the importance and difficulty of recognizing these injuries. Standard radiographs are difficult to interpret due to the often severe external rotation of the foot. Prompt treatment, though can lead to good results in patients. The posterolateral ridge of the distal tibia hinders reduction and reduction often requires an open technique
Mayer and Evarts stated AP and mortise radiographs can be hard to interpret due to the external rotation posture of the foot. In their series a closed reduction consisting of traction and medial rotation applied to the foot while the fibular shaft is pushed laterally was successful in 3/4 patients.
OrthoCash 2020
A 37-year-old female sustains the injury seen in Figures A and B. At long-term follow up, degeneration of which of the following joints has been shown to have the highest rate of patient symptoms?
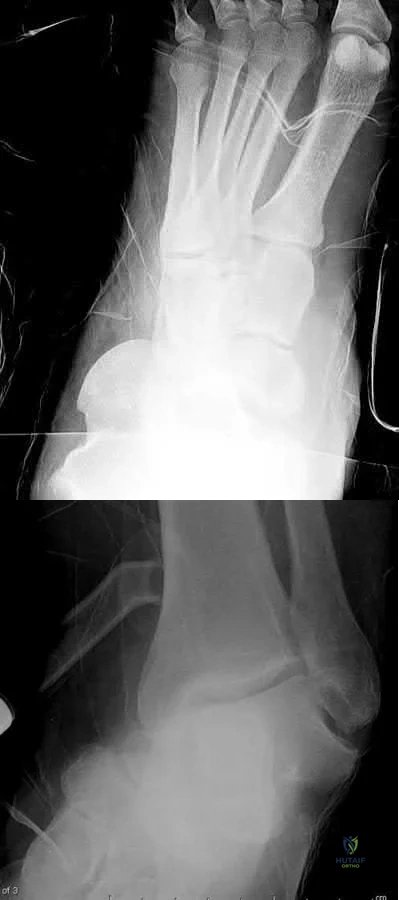
Tibiotalar joint
Talonavicular joint
Calcaneocuboid joint
Lisfranc joint
Subtalar joint
Figures A and B show a medial subtalar dislocation, which is more common than a lateral dislocation (65% vs. 35%).
The referenced article by Bibbo et al looked at long-term follow up of these patients, and noted that radiographic degeneration of the ankle and subtalar joints were 89%, although 31% of ankle joints were symptomatic and 68% of subtalar joints were symptomatic. Midfoot degeneration was seen radiographically in 72% (15% symptomatic).
OrthoCash 2020
In treating a lateral split-depression type tibial plateau fracture, which of the following adjuncts has been shown to have the least articular surface subsidence when used to fill the bony void?
Crushed cancellous allograft
Hydroxyapatite
Calcium phosphate cement
Autogenous iliac crest
Bisected diaphyseal humeral allograft Corrent answer: 3
In treating tibial plateau fractures, calcium phosphate has been shown to have the least amount of articular subsidence on follow-up examinations.
The referenced study by Russell et al noted a significantly increased rate of subsidence at 12 months with autograft as compared to calcium phosphate cement (in types I-VI).
The other referenced study by Lobenhoffer et al noted improved radiographic outcomes and earlier weightbearing with usage of calcium phosphate cement.
OrthoCash 2020
The pelvic spur sign on plain radiography is indicative of the following injuries?
Transtectal transverse acetabular fracture
Vertical shear pelvic ring injury
Displaced H-type sacral fracture
Both column acetabular fracture
Anterior-posterior type III pelvic ring injury Corrent answer: 4
The pelvic spur sign is indicative of a both column acetabular fracture. It is best seen on an AP or obturator oblique x-ray. The spur is the intact portion of the ilium, still attached to the axial skeleton and seen posterosuperior to the displaced acetabulum (typically medially displaced).
Illustration A shows the spur sign (arrows) on a CT image, while illustration B shows an obturator oblique of the pelvis and the spur sign is shown with the long tailed arrow (on the left of the image).
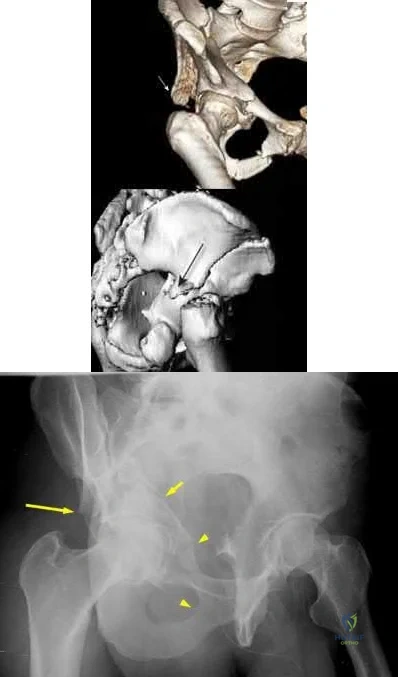
OrthoCash 2020
A 33-year-old male sustains a distal humerus fracture and is treated with open reduction and internal fixation of the distal humerus with olecranon osteotomy. A postoperative radiograph is shown in Figure A. A new deficit of the anterior interosseous nerve is now noted in the recovery room. What physical exam finding would be expected with this nerve injury?
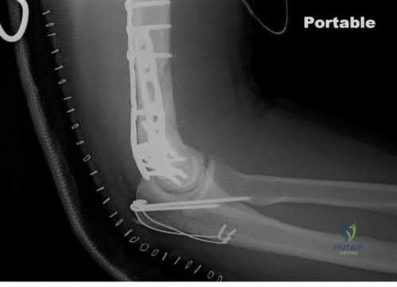
Inability to flex radiocarpal joint
Loss of sensation over palmar aspect of thumb
Loss of sensation over dorsal hand first webspace
Inability to abduct index finger
Inability to flex thumb interphalangeal joint Corrent answer: 5
A deficit in the anterior interosseous nerve (AIN) would result in an inability to flex the interphalangeal joint (IPJ) of the thumb.
Injury to the AIN can be seen with K-wires that penetrate through the anterior cortex of the proximal ulna, such as mentioned above. The AIN is a branch of the median nerve that provides motor function to forearm/hand. It branches off from the median nerve 4 cm distal to the medial epicondyle, passes between the 2 heads of the pronator teres, travels through the forearm anterior to the interosseous membrane between the flexor pollicis longs (FPL) and flexor digitorum profundus (FDP), and then terminates in the pronator quadratus (PQ). The nerve gives of branches to the FDP, FPL, and PQ enabling for flexion of the distal phalangeal joint of the index and middle fingers, flexion of the IPJ of the thumb, and aids with pronation of the forearm, respectively.
Injury to the nerve will result in weakness in motor function to these muscles.
Mekail et al. reviewed the anterior approach to the proximal radius in order to describe and identify important neurovascular and musculoskeletal structures in the area. They were specifically aiming to determine the safest anatomic orientation for plate and screw fixation in regards to the posterior interosseous nerve. The authors, however, did discuss that medial plating was especially dangerous to the AIN, and significantly increased the risk of iatrogenic injury to the branch sent to the FPL.
Parker et al. reported a case report in a patient who experienced an AIN deficit postoperatively after tension banding of an olecranon fracture.
Intraoperatively, there were multiple passes of the K-wires in an attempt to find purchase in the anterior cortex of the ulna. The authors believed that during these passes, the nerve was injured and concluded that placing K-wires should not occur without radiologic visualization.
Figure A is a postoperative lateral radiograph after tension banding of the olecranon. Perforation of the anterior ulnar cortex can be seen by the K-wire which can cause damage to the AIN nerve. Illustration A is a schematic of the path of the AIN, its branches, and its function.
Incorrect Answers:
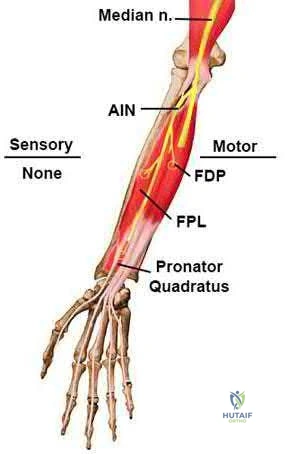
OrthoCash 2020
A computed tomography (CT) scan has been shown to be indicated for evaluation of all of the following aspects of acetabular fractures, EXCEPT:
Determination of surgical planning
Intra-articular loose bodies
Marginal impaction
Fracture piece size and position
Determination of pre-existing degenerative changes Corrent answer: 5
CT scanning is indicated in acetabular fractures for determination of surgical approach and techniques, evaluation of marginal impaction and presence of intra-articular loose bodies (especially after hip dislocation), and evaluation of fracture piece sizes and relative positions.
Kellam et al reviewed their initial experience with CT scanning and acetabular fractures, and noted a 25% change in surgical planning when CT was utilized versus plain radiographs; they also noted the ability to detect marginal impaction and fracture size/position was improved with CT.
OrthoCash 2020
A 69-year-old woman falls while getting out of her car and lands on her right shoulder sustaining a 4-part proximal humerus fracture. She subsequently undergoes surgery to treat the fracture, with immediate postoperative radiographs shown in Figure A. Six months following surgery, she denies shoulder pain, but she is unable to actively raise her hand above her shoulder. Which of the following is the most likely cause of this limitation?
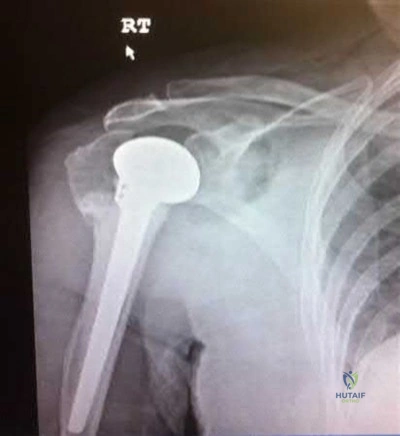
Joint infection
Retroversion of the prosthesis
Glenoid arthritis
Axillary nerve injury
Greater tuberosity malunion Corrent answer: 5
The radiograph demonstrates a humeral hemiarthroplasty. Malunion of the greater tuberosity is a known complication of this procedure, and the most likely cause for loss of shoulder elevation.
Frankle et al in 2004 reported a 25% rate of greater tuberosity malunion. They discuss surgical techniques to improve fixation of the tuberosities following hemiarthroplasty for proximal humerus fractures.
Frankle et al in 2002 evaluated 5 different techniques to reattach the tuberosities following shoulder hemiarthroplasty in human cadavers. Findings suggested that a circumferential medial cerclage should be placed around the tuberosities to enhance the stability of the tuberosity repair.
Bosch et al reviewed 39 consecutive 3 or 4 part proximal humerus fractures that were treated with either primary hemiarthroplasty or secondary hemiarthroplasty following a primary ORIF. Patients who underwent primary
hemiarthroplasty reported better clinical outcomes. The authors concluded that elderly patients with 3 or 4 part humerus fractures are best treated with early arthroplasty.
OrthoCash 2020
An acetabular fracture with all segments of the articular surface detached from the intact posterior ilium is defined as what fracture pattern?
Transverse
Both column
Anterior column posterior hemitransverse
Posterior column with posterior wall
Anterior column with anterior wall Corrent answer: 2
A both column acetabular fracture is defined as an acetabular fracture with no articular surface in continuity with the remaining posterior ilium (and therefore, axial skeleton). The spur sign is a radiological sign seen with these fractures, and is the posterio-inferior aspect of the intact posterior ilium. The spur sign and other radiographic findings consistent with a both column acetabular fracture can be seen in Illustration A (AP), Illustration B (obturator oblique), and Illustration C (iliac oblique).
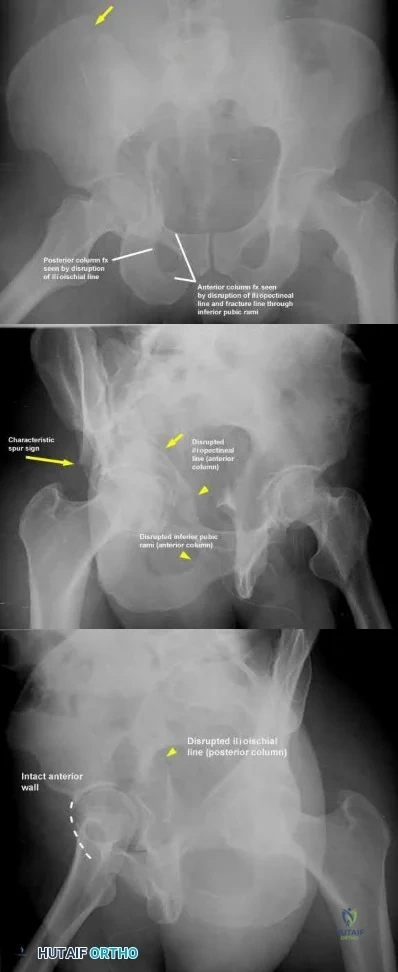
OrthoCash 2020
A large posteromedial tibial plateau fracture pattern, as seen with the bicondylar tibial plateau fracture shown in Figures A and B, is important to recognize because of which of the following factors?
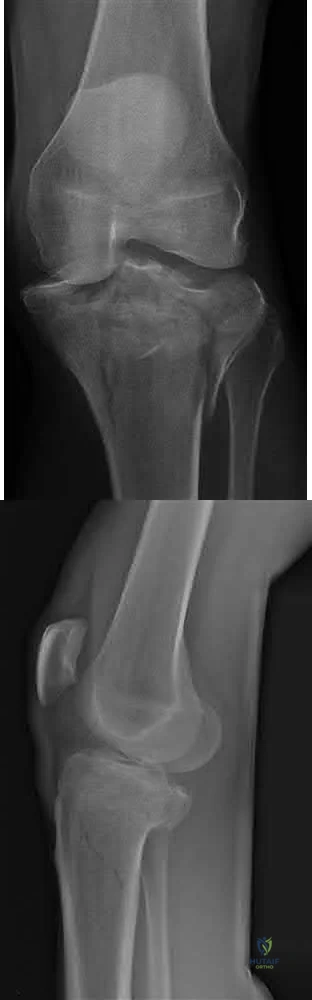
Association with posteromedial corner of the knee injury
Association with anterior tibial artery injury
Possible need for dual plate fixation
Possible need for single extensile anterior approach to the knee
Increased risk of deep venous thrombosis Corrent answer: 3
Figures A and B show a bicondylar tibial plateau fracture with a large posteromedial fracture piece. This has clinical importance, as currently available plate/screw constructs often have poor fixation of this fracture segment, and this pattern often requires a second, posteromedial, approach and placement of a second plate/screw construct.
The referenced article by Barei et al notes a prevalence of posteromedial fracture pieces of nearly 33% of all bicondylar tibial plateau fractures. They also recommend supplementary or alternative fixation techniques when this pattern is recognized.
The referenced article by Higgins et al notes a 59% incidence of this fracture pattern (consisting of nearly 25% of the total joint surface) in bicondylar tibial plateau fractures, and recommends appropriate fixation to combat the vertical shear instability through a separate approach.
The last referenced study by Higgings et al notes a significantly increased rate of late fracture displacement in a biomechanical model with a single lateral locking plate as compared to a dual plate construct.
OrthoCash 2020
At the elbow, the anterior bundle of the medial collateral ligament inserts at which site?
Radial tuberosity
3mm distal to the tip of the coronoid
Anteromedial process of the coronoid
Medial border of the olecranon fossa
Radial side of ulna at origin of annular ligament Corrent answer: 3
The anterior bundle of the medial collateral ligament of the elbow inserts at the anteromedial process of the coronoid, also known as the sublime tubercle.
Fractures at this site have been shown to have worse results with nonoperative
treatment, due to increased rates of instability and post-traumatic arthrosis.
The referenced articles by Ring and Steinmann are great reviews of the topic of coronoid fractures. They review the diagnosis, treatment options, rehabilitation, and outcomes of these injuries. They focus on the importance of the coronoid in elbow stability, especially with base fractures, or ones that involve the sublime tubercle.
Illustration A depicts the anterior bundle of the MCL inserting at the sublime tubercle.
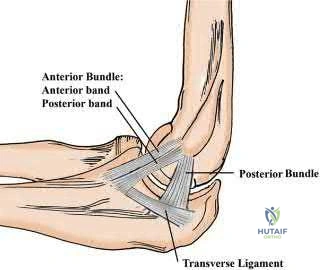
OrthoCash 2020
In the Lauge-Hansen classification system, a pronation-abduction ankle fracture has what characteristic fibular fracture pattern?
Transverse fracture below the level of the syndesmosis
Short oblique fracture running from anteroinferior to posteriosuperior
Short oblique fracture running from posteroinferior to anteriosuperior
Comminuted fracture at or above the level of the syndesmosis
Wagstaff fracture
In the Lauge-Hansen classification, the characteristic fibular fracture pattern in a pronation-abduction injury is a comminuted fibular fracture above the level of the syndesmosis. In the first stage of this injury pattern, the deltoid fails in tension, or an avulsion fracture of the medial malleolus occurs. In the second stage, the anterior inferior tibiofibular ligament ruptures, or a small bony avulsion of this ligament's insertion/origin occurs. The final stage includes the creation of a comminuted fibular fracture above the level of the syndesmosis.
The referenced article by Siegel et al noted that extraperiosteal bridge plating of these ankle injuries was safe and had excellent radiographic and clinical outcomes at final follow-up.
OrthoCash 2020
A 38-year-old male sustains the closed injury shown in Figures A and B. When treating this injury with an intramedullary nail, addition of blocking screws into which of the following positions can prevent the characteristic malunion deformity?
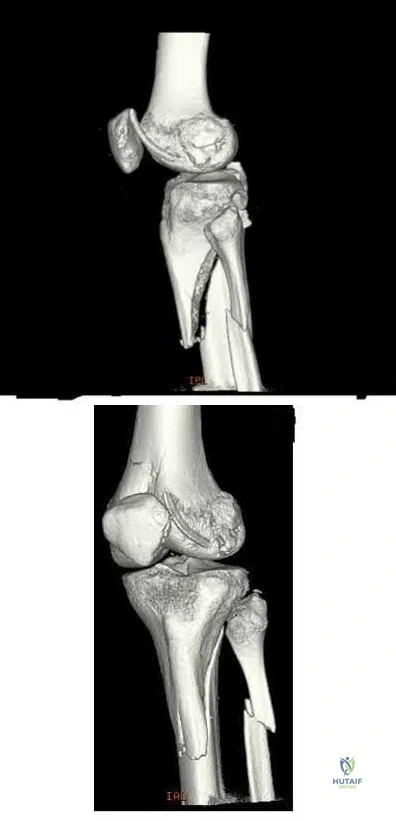
Anterior to the nail in the proximal segment; medial to the nail in the proximal segment
Anterior to the nail in the proximal segment; lateral to the nail in the proximal segment
Posterior to the nail in the proximal segment; lateral to the nail in the proximal segment
Anterior to the nail in the distal segment; lateral to the nail in the distal segment
Posterior to the nail in the distal segment; medial to the nail in the proximal segment
Figures A and B show a proximal tibia fracture, which is prone to malreduction/malunion into a characteristic valgus and procurvatum (apex anterior) deformity. Placement of screws in this instance posterior to the nail (medial to lateral) and lateral to the nail (anterior to posterior) in the proximal segment will prevent iatrogenic malalignment.
Intramedullary nails will not effect a reduction in metaphyseal proximal tibia fractures. Valgus and apex anterior deformities in these injuries may be caused by deforming muscular forces, limb positioning in hyper flexion, as well as iatrogenic deformity created by improper nail insertion technique. Blocking (Poller) screws are utilized to redirect intramedullary nails by creating an artificial cortex to guide the nail into appropriate position.
The referenced biomechanical study by Krettek et al noted that addition of blocking screws added increased stability to metaphyseal fractures.
Ricci et al noted no malalignment intraoperatively or at final follow-up of proximal tibia fractures treated with intramedullary nails if blocking screws were used.
OrthoCash 2020
In an uninjured proximal tibia which statement best describes the shape and position of the medial tibial plateau relative to the lateral tibial plateau?
More concave and more proximal
More convex and more proximal
More concave and more distal
More convex and more distal
Symetric in conture and more distal
The medial tibial plateau is more concave and more distal relative to the lateral tibial plateau.
Watson et al report "the medial tibial plateau has a more concave shape and is larger in both length and width than the lateral tibial plateau, which has a slightly convex shape. The lateral tibial plateau lies proximal to the medial plateau. The convexity of the lateral plateau helps differentiate it from the medial plateau on a lateral radiograph of the proximal tibia."
Illustration A shows the relative concavity of the medial and lateral proximal tibia.
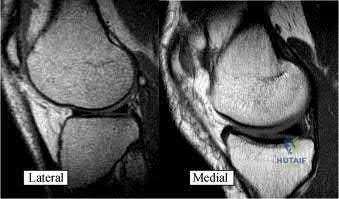
OrthoCash 2020
On average, the radial nerve travels from the posterior compartment of the arm and enters the anterior compartment at which of the following sites?
Spiral groove of the humerus
At the arcuate ligament of Osborne
10 cm distal to the lateral acromion
10 cm proximal to radiocapitellar joint
At the origin of the deep head of the triceps Corrent answer: 4
The radial nerve enters the anterior compartment through the intercompartmental fascia on average 10 cm proximal to the radiocapitellar joint. It has never been found to remain in the posterior compartment within
Question 52
A 55-year-old woman with a long history of low back and left lower extremity pain has failed to respond to exhaustive nonsurgical management. MRI scans show bulging and degeneration at L3-4 and L4-5 as well as a normal disk at L2-3 and L5-S1. She undergoes provocative lumbar diskography at L3-4, L4-5, and L5-S1. Post-diskography axial CT images of L3-4 and L4-5 are shown in Figures 6a and 6b, respectively. The injections at L3-4 and L4-5 produce no pain. The injection at L5-S1 produces 10/10 concordant back pain with radiation to the lower extremity. What is the most appropriate recommendation at this time? Review Topic
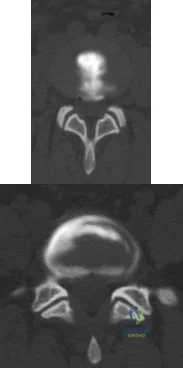
Explanation
sided radicular symptoms. The only disk that produced concordant back pain was the normal disk at the L5-S1 level and it reproduced radicular symptoms on the side opposite of her typical pain. Based on these findings, it would be difficult to select a level or levels to include in a lumbar fusion. As such, continued nonsurgical management is the safest treatment option at the current time. Brox and associates reported on a randomized clinical trial comparing lumbar fusion to cognitive intervention and exercise and found similar results in both groups, with significantly less risk in the latter.
Question 53
Figures 48a and 48b show the elbow radiographs of a 5-year-old boy who fell from a tree after dinner. Examination reveals that he is unable to extend his wrist. Management should consist of immediate
Explanation
REFERENCES: Iyengar SR, Hoffinger SA, Townsend DR: Early versus delayed reduction and pinning of type III displaced supracondylar fractures of the humerus in children: A comparative study. J Orthop Trauma 1999;13:51-55.
Leet AI, Frisancho J, Ebramzadeh E: Delayed treatment of type 3 supracondylar humerus fractures in children. J Pediatr Orthop 2002;22:203-207.
Question 54
Figures below show the AP and lateral radiographs obtained from a 54-year-old woman who has worsening groin pain 18 months after a primary left total hip arthroplasty. The pain is worst when climbing stairs, when rising from a seated position, and during resisted hip flexion. Her pain improved early after surgery but did not completely resolve. Her C-reactive protein and erythrocyte sedimentation rate results of less than 1 mg/dL and 10 mm/hr, respectively, were obtained in the office. What is the best next step?
Explanation
Iliopsoas impingement is a potential cause of persistent groin pain after a total hip arthroplasty. This patient’s history gives groin pain with resisted hip flexion and during activities that require this level of function. The radiographs depict an acetabular component with substantial retroversion. Typical options for the management of iliopsoas tendon impingement include injections, tenotomy, and acetabular revision. Recently, Chalmers and associates reported more predictable groin pain resolution with 8 mm or more of anterior acetabular component when overhang was revised. The radiographs clearly show more retroversion, with a cup prominence of more than 8 mm anteriorly. MRI with MARS could potentially help in the diagnosis of this impingement but would not help in management (option A). An ultrasound- guided injection would need to be administered into the iliopsoas tendon sheath to be of help and, in this case, would likely be performed for diagnostic purposes due to the extreme anterior overhang (option C). Option D would be useful for mild cases of iliopsoas impingement but likely would not help much in this more extreme case.
Question 55
The patient fails nonsurgical treatment for this condition. What is the best next step?
Explanation
Osgood-Schlatter disease is an apophysitis of the tibial tubercle. This condition is present in males more than females and occurs prior to fusion of the tubercle to the epiphysis of the tibia. The apophysis is cartilaginous before 11 years of age and begins to ossify between 11 and 14 years of age. The apophysis fuses to the epiphysis between 14 and 18 years of age (females before males). Symptoms are pain and swelling, and pain is worse with jumping and running. Initial treatment should consist of activity limitation, ice, quadriceps and hamstring stretching, and possible bracing. NSAIDs may be used to control symptoms. When symptoms resolve, the athlete may return to activities. In fewer than 10% of cases, symptoms persist after skeletal maturity. For these patients, excision of the ossicle will usually resolve symptoms. The ossicle is usually not part of the tendon attachment and can be resected without detaching any of the patellar tendon.
RECOMMENDED READINGS
Vergara-Amador E, Davalos Herrera D, Moreno LÁ. Radiographic features of the development of the anterior tibial tuberosity. Radiologia. 2016 Feb 22. pii: S0033-8338(16)00019-9. doi: 10.1016/j.rx.2016.01.005. [Epub ahead of print] English, Spanish. PubMed PMID: 26917430. View Abstract at PubMed
Frank JB, Jarit GJ, Bravman JT, Rosen JE. Lower extremity injuries in the skeletally immature athlete. J Am Acad Orthop Surg. 2007 Jun;15(6):356-66. Review. PubMed PMID: 17548885. View Abstract at PubMed
Question 56
A 20-year-old athlete sustains a 2- x 3-cm grade IV chondral injury to the right knee. After failure of nonsurgical management, which of the following procedures would ensure the highest percentage of hyaline-like cartilage?
Explanation
REFERENCES: Brittberg M, Lindahl A, Nilsson A, et al: Treatment of deep cartilage defects in the knee with autologous chondrocyte transplantation. N Engl J Med 1994;331:889-895.
Garrett WE, Speer KP, Kirkendall DT (eds): Principles & Practice of Orthopaedic Sports Medicine. Philadelphia, PA, Lippincott Williams & Wilkins, 2000, pp 787-804.
Question 57
A 6-year-old boy has had increasing pain and a mass in the suprapatellar region of the right femur for the past week. Examination of the mass reveals it may be firm, immobile, and tender to palpitation. The patient has no systemic symptoms. Laboratory studies show a WBC of 7000 per cubic millimeter, a hematocrit of 40%, and an erythrocyte sedimentation rate of 10 mm/hr. radiographs are normal. Figures 64a and 64b show saggital and axial T1-weighted MRI scans. Figure 64c shows frozen section pathology of the biopsy specimen. What is the most likely diagnosis?
Explanation
Question 58
A direct lateral (Hardinge) approach is used during total hip arthroplasty. The structure labeled A in Figure 7 is the
Explanation
REFERENCES: Hoppenfeld S, deBoer P: Surgical Exposures in Orthopaedics: The Anatomic Approach. Philadelphia, PA, JB Lippincott, 1984, pp 333-335.
Ramesh M, O’Byrne JM, McCarthy N, et al: Damage to the superior gluteal nerve after the Hardinge approach to the hip. J Bone Joint Surg Br 1996;78:903-906.
Question 59
Figure 242 is the anteroposterior radiograph of a 28-year-old man who underwent resection and reconstruction for an Ewing sarcoma. What is the most common functional deficit encountered during rehabilitation?
Explanation
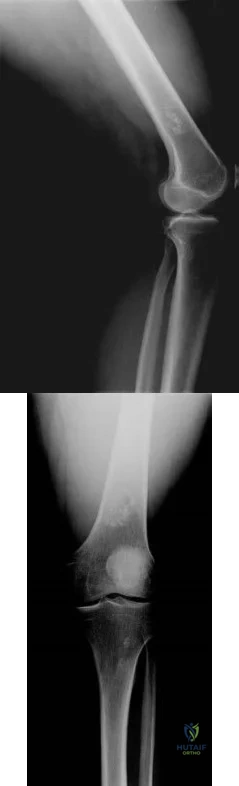
Question 60
Which treatment option will most reliably achieve long-term success?
Explanation
There are 3 types of fifth metatarsal fractures. Zone 1 is an avulsion fracture. Zone 2 fractures, also known as Jones fractures, occur in the watershed area of the fifth metatarsal. A fracture must exit the intermetatarsal articulation between the fourth and fifth metatarsals to be considered a Jones fracture. Zone 3 fractures are distal to the articulation in the diaphysis of the fifth metatarsal. Jones fractures are associated with a 15% to 20% nonunion rate with nonsurgical care. Surgical intervention is preferred in athletic patients. Fixation with a solid screw is mechanically stronger than fixation with a cannulated screw. Nonunions or failure of hardware can be attributable to inadequate fixation or an unrecognized varus heel alignment leading to lateral column overload.
RECOMMENDED READINGS
Zenios M, Kim WY, Sampath J, Muddu BN. Functional treatment of acute metatarsal fractures: a prospective randomised comparison of management in a cast versus elasticated support bandage. Injury. 2005 Jul;36(7):832-5. Epub 2005 Mar 21. PubMed PMID: 15949484. View Abstract at PubMed
Fetzer GB, Wright RW. Metatarsal shaft fractures and fractures of the proximal fifth metatarsal. Clin Sports Med. 2006 Jan;25(1):139-50, x. Review. PubMed PMID: 16324980. View Abstract at PubMed
Zwitser EW, Breederveld RS. Fractures of the fifth metatarsal; diagnosis and treatment. Injury. 2010 Jun;41(6):555-62. doi: 10.1016/j.injury.2009.05.035. Epub 2009 Jun 30. Review. PubMed PMID: 19570536. View Abstract at PubMed
Hunt KJ, Goeb Y, Esparza R, Malone M, Shultz R, Matheson G. Site-Specific Loading at the Fifth Metatarsal Base in Rehabilitative Devices: Implications for Jones Fracture Treatment. PM
R. 2014 May 28. pii: S1934-1482(14)00243-3. doi: 10.1016/j.pmrj.2014.05.011. [Epub
ahead of print] PubMed PMID: 24880059. View Abstract at PubMed
Nunley JA. Fractures of the base of the fifth metatarsal: the Jones fracture. Orthop Clin North Am. 2001 Jan;32(1):171-80. Review. PubMed PMID: 11465126. View Abstract at PubMed
Orr JD, Glisson RR, Nunley JA. Jones fracture fixation: a biomechanical comparison of partially threaded screws versus tapered variable pitch screws. Am J Sports Med. 2012 Mar;40(3):691-
Question 61
A 58-year-old male presents after a motor vehicle accident with severe pain and point tenderness over his lumbar spine. He is hemodynamically stable and full neurologic examination reveals no deficits. Radiographs showed no evidence of fracture. A CT was performed and is shown in Figure A. What is the most appropriate treatment of his injury. Review Topic
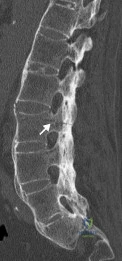
Explanation
In patients with ankylosing spondylitis (AS), the rigid spine creates a long lever arm that makes even minimally displaced fractures potentially unstable. Thus, despite being minimally displaced in a neurologically intact patient, most fractures in AS warrant a posterior instrumentation and fusion, typically of three levels above and three levels below the fracture.
Caron et al. present a retrospective review of patients with ankylosed spines (due to AS or DISH) and characterize their fractures and outcomes of treatment. Cervical fractures were most common (55%) and rates of occurrence decreased as they progressed down the spine, with lumbar fractures seen only 8% of the time. They found the most common successful surgical intervention was multilevel posterior instrumentation and fusion (with decompression when necessary for neurologic compromise).
Wang et al. reviewed 12 cases of patients with AS who presented with traumatic spinal injuries. They reviewed clinical histories and available imaging. They found that MRI was the most sensitive test for identifying occult fractures of the spine, and recommend using MRI to rule out occult fractures as well as better characterize fractures seen on radiographs or CT imaging for patients with AS.
Werner et al. present a review of spinal fractures in patients with AS. They note that non-operative treatment of these fractures is reserved only for patients who have an unacceptably high risk of undergoing surgery. For three column thoracolumbar fractures they recommend surgical stabilization with a long posterior construct.
Figure A is a sagittal CT image of the lumbar spine with marginal syndesmophytes consistent with AS. The white arrow highlights a minimally displaced fracture that extends through all three columns on the spine. Illustration A are radiographs comparing DISH (on the left) with non-marginal syndesmophytes, and AS (on the right) with marginal syndesmophytes.
Incorrect Answers:
Question 62
A 40-year-old unrestrained passenger reports chest wall pain after a motor vehicle accident. Which of the following structures is most important in preventing the injury shown in Figure 33?
Explanation
REFERENCES: Gilot GJ, Wirth MA, Rockwood CA: Injuries to the sternoclavicular joint, in Bucholz RW, Heckman JD, Court-Brown C (eds): Fractures in Adults. Philadelphia, PA, Lippincott, Williams and Wilkins, 2006, vol 2, pp 1373-1374.
Spencer EE, Kuhn JE, Huston LJ, et al: Ligamentous restraints to anterior and posterior translation of the sternoclavicular joint. J Shoulder Elbow Surg 2002;11:43-47.
Question 63
A 73-year-old woman reports a 4-month history of severe left-sided posterior buttock pain and left leg pain. The leg pain radiates into the left lateral thigh and posterior calf with cramping. Examination reveals mild difficulty with a single-leg toe raise on the left side and a diminished ankle reflex. There is also a significant straight leg raise test at 45 degrees which exacerbates symptoms. An MRI scan is shown in Figure 4. What is the most appropriate treatment at this time?
Explanation
REFERENCES: Lyons MK, Atkinson JL, Wharen RE, et al: Surgical evaluation and management of lumbar synovial cysts: The Mayo Clinic Experience. J Neurosurg
2000;93:53-57.
Khan AM, Synnot K, Cammisa FP, et al: Lumbar synovial cysts of the spine: An evaluation of surgical outcome. J Spinal Disord Tech 2005;18:127-131.
Epstein NE: Lumbar laminectomy for the resection of synovial cysts and coexisting lumbar spinal stenosis or degenerative spondylolisthesis: An outcome study. Spine 2004;29:1049-1055.
Question 64
Figure 40 shows the plain radiograph of a 30-year-old woman who has had a long history of standing bilateral anterior knee pain and a sense of patellar instability without frank dislocation. Nonsurgical management consisting of anti-inflammatory drugs and physical therapy has failed to provide relief. Examination reveals full range of motion of both knees, with moderate patellofemoral crepitance. Patellar apprehension and patellar grind tests are positive. The Q-angle measures 20°. Management should now consist of
Explanation
REFERENCES: Boden BP, Pearsall AW, Garrett We Jr, et al: Patellofemoral instability: Evaluation and management. J Am Acad Orthop Surg 1997;5:47-57.
Fulkerson JP: Patellofemoral pain disorders: Evaluation and management. J Am Acad Orthop Surg 1994;2:124-132.
Question 65
A 58-year-old man has anterior knee pain after undergoing total knee arthroplasty for osteoarthritis 2 years ago. He denies any history of trauma. A Merchant view is shown in Figure 20. What is the most likely cause of his pain?
Explanation
REFERENCES: Reuben JD, McDonald CL, Woodard PL, Hennington LJ: Effect of patella thickness on patella strain following total knee arthroplasty. J Arthroplasty 1991;6:251-258.
Hsu HC, Luo ZP, Rand JA, An KN: Influence of patellar thickness on patellar tracking and patellofemoral contact characteristics after total knee arthroplasty. J Arthroplasty 1996;11:69-80.
Greenfield MA, Insall JN, Case GC, Kelly MA: Instrumentation of the patellar osteotomy in total knee arthroplasty: The relationship of patellar thickness and lateral retinacular release. Am J Knee Surg 1996;9:129-131.
Question 66
A 47-year-old, healthy, active patient presents with a sub-acute, full-thickness supraspinatus tear. His physical examination reveals significant weakness and pain with abduction. There was no glenohumeral instability. Radiographs demonstrate a type 1 acromion. An MRI scan shows a crescent shaped tear with 2-cm of tendinous retraction and no tendinous fatty changes. A subacromial corticosteroid injection 6 weeks ago provided him with 24 hours of pain relief but no improvement in strength. What would be the most appropriate treatment option? Review Topic QID:4501
Explanation
The primary purpose of rotator cuff repair is to restore muscle function. Secondary outcomes include reduction of pain and prevention of irreversible cuff changes, specifically muscular atrophy. Non-operative treatment (exercise, therapy and pain medications) are recommended for partial thickness tears. The indication of surgical repair includes, isolated supraspinatus weakness +/- pain that correlates with MRI imaging of a respective full thickness tear. Routine acrominoplasty is not recommended in conjunction with rotator cuff repair, especially with no previous symptoms of impingement.
Pedowitz et al. developed clinical practice guidelines for the treatment of rotator cuff pathology. The strongest supporting evidence in current literature was given a grade of 'moderate' with four treatment recommendations. These were,
Exercise and non-steroidal anti-inflammatory drugs can be used to manage partial thickness tears,
Routine acromioplasty is not required the time of cuff repair,
Non-cross-linked, porcine small intestine submucosal xenograft patches should not be used to manage cuff tears, and
Surgeons can advise patients that workers' compensation status correlates with a less favorable outcome after rotator cuff surgery.
Illustration A shows the different shapes of rotator cuff tears. Incorrect Answers:
Question 67
During the anterior approach for repair of a distal biceps tendon rupture, what structure, shown under the scissors in Figure 6, is at risk for injury?
Explanation
REFERENCES: Kelly EW, Morrey BF, O’Driscoll SW: Complications of repair of the distal biceps tendon with the modified two-incision technique. J Bone Joint Surg Am 2000;82:1575-1581.
Ramsey ML: Distal biceps tendon injuries: Diagnosis and management. J Am Acad Orthop Surg 1999;7:199-207.
Question 68
An year-old African American woman who lives in a large city is scheduled for total hip arthroplasty to address primary osteoarthritis. Part of the presurgical protocol includes nasal swab screening to assess for methicillin-resistant Staphylococcus aureus (MRSA) colonization. Which demographic factor places this patient at highest risk for a positive result?
Explanation
Demographic factors are associated with increased risk for MRSA colonization, so it is important to identify vulnerable patients. Female gender and advanced age reduce the risk for colonization, whereas African American race increases this risk. Urban environments do not influence MRSA colonization.
Question 69
An 82-year-old woman reports activity-related knee pain. History reveals that she underwent total knee arthroplasty 16 years ago. AP and lateral radiographs and a bone scan are shown in Figures 38a through 38c. What is the most likely diagnosis?
Explanation
well-defined borders. Joint space narrowing medially is consistent with polyethylene wear.
The most likely diagnosis is particle-mediated osteolysis. Metastatic tumors and primary sarcomas adjacent to an arthroplasty are extremely rare. In addition, malignant tumors and infection would more likely reveal a destructive lesion with poorly defined borders and increased uptake on a bone scan. Stress shielding with massive bone loss has not been described in knee arthroplasty literature, although this entity has been observed in fully porous-coated femoral implants in total hip arthroplasty.
REFERENCES: Robinson EJ, Mulliken BD, Bourne RB, et al: Catastrophic osteolysis in total knee replacement: A report of 17 cases. Clin Orthop Relat Res 1995;321:98-105.
Archibeck MJ, Jacobs JJ, Roebuck KA, et al: The basic science of periprosthetic osteolysis. Instr Course Lect 2001;50:185-195.
Bugbee WD, Culpepper WJ, Engh CA Jr, et al: Long-term clinical consequences of stress-shielding after total hip arthroplasty without cement. J Bone Joint Surg Am 1997;79:1007-1012.
Question 70
A 40-year-old man with a history of Legg-Calve-Perthes disease underwent a right hip resurfacing 3 years ago with no perioperative complications. Hip pain has developed gradually during the last 4 months. Radiographs show no evidence of fixation loosening or any adverse changes at the femoral neck. No periarticular osteolysis is evident. A large intra-articular and intrapelvic pseudotumor has developed. What predominant histological feature(s) is/are present in such a lesion?
Explanation
Controversy persists over what exactly is the best approach to managing patients with metal-on-metal (MOM) hip arthroplasties. All patients with painful MOM hip arthroplasties should be examined for fixation loosening, wear/osteolysis, and infection—no differently than patients without MOM hip arthroplasties. It is recommended to obtain serum trace element levels. If the levels are high, cross-sectional imaging should be obtained to determine whether any pseudotumor or tissue necrosis is present around the hip arthroplasty. Hip aspiration should be considered if concern for infection exists. Adverse tissue reaction has been identified to occur around MOM hip arthroplasties. The predominant histologic feature is tissue necrosis with infiltration of lymphocytes and plasma cells.
Question 71
The subcutaneous nerve most at risk for transection during an anterior surgical exposure of the ankle is the
Explanation
The dorsal medial cutaneous nerve arising from the superficial peroneal nerve crosses the inferior extent of a routine extensile surgical exposure to the ankle joint. The extensile anterior incision develops the interval between the tibialis anterior and extensor hallucis tendons, and, although the deep peroneal nerve is lateral and posterior to the extensor hallucis longus, the nerve most at risk during this exposure is the cutaneous branch supplying the dorsal medial foot to the great toe. Ankle replacement surgery is becoming more common; consequently, surgeons must be familiar with this anatomic landmark and risks related to its transection during surgery.
The medial plantar nerve is at risk when medial hindfoot incisions are made through the
abductor hallucis muscle during tarsal tunnel release and harvest of the flexor hallucis tendon for transfer. The dorsal cutaneous branch of the sural nerve supplies the lateral dorsal
Question 72
A 4-year-old girl has knee pain after a fall. Examination reveals tenderness about the proximal tibia with modest deformity. She has no neurovascular deficits. A radiograph is seen in Figure 24. What should her parents be told? 2010 Pediatric Orthopaedic Examination Answer Book • 25
Explanation
REFERENCES: Jordan SE, Alonso JE, Cook FF: The etiology of valgus angulation after metaphyseal fractures of the tibia in children. J Pediatr Orthop 1987;7:450-457.
Tuten HR, Keeler KA, Gabos PG, et al: Posttraumatic tibia valga in children: A long-term follow-up note. J Bone
Joint Surg Am 1999;81:799-810.
Question 73
- What location is the primary source of vascular ingrowth for tendon-bone healing with rotator cuff repair?
Explanation
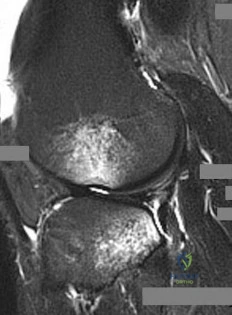
Question 74
Figures 189a through 189d are the radiograph and MR images of the right hip of a 28-year-old woman who has had right hip pain for 3 years. The pain is felt in the groin area, is exacerbated by weight-bearing activities, and interferes with her activities of daily living. She has been seen several times and has attempted anti-inflammatory medications, physical therapy, and an intra-articular steroid injection with minimal relief. What is the most appropriate next step?
Explanation
Video 189 for reference
This patient has dysplasia with a lack of lateral femoral head coverage. The MR images do not demonstrate a labral tear. There is still preserved joint space and she is young, so it would be preferable to delay THA in her case. A Ganz periacetabular osteotomy can provide more adequate coverage of the femoral head and is a multiplanar correction of the dysplastic acetabulum. This osteotomy is an effective treatment for symptomatic dysplasia in prearthritic young adult hips. A femoral osteotomy is not likely to be effective in this scenario.
CLINICAL SITUATION FOR QUESTIONS 190 THROUGH 192
Eighteen years after undergoing right total hip arthroplasty (THA), a 79-year-old woman experiences several weeks of right groin pain. A hip examination reveals that she is walking with a mild limp with a walker. Hip radiographs reveal moderate polyethylene wear with well-fixed components and mild osteolysis in the greater trochanter. Analysis of a CT scan reveals that the acetabular component is osteointegrated in 49 degrees of abduction and 25 degrees of anteversion. Erythrocyte sedimentation rate and C-reactive protein findings are within defined limits.
Question 75
Figure 38 shows the radiograph of a 5-year-old child who sustained a type III supracondylar fracture. Examination reveals the absence of a radial pulse, but an otherwise well-perfused hand. Following closed reduction and percutaneous pinning, the radial pulse remains absent; however, the hand is pink and well perfused. Management should now include
Explanation
REFERENCE: Sabharwal S, Tredwell SJ, Beauchamp RD, Mackenzie WG, Jakubec DM, Cairns R: Management of pulseless pink hand in pediatric supracondylar fractures of humerus. J Pediatr Orthop 1997;17:303-310.
Question 76
The so-called high ankle sprain from an external rotation mechanism of injury typically involves injury to which of the following structures?
Explanation
REFERENCES: Last RJ: Anatomy: Regional and Applied, ed 6. London, England, Churchill Livingstone, 1978, p 182.
Kaye RA: Stabilization of ankle syndesmosis injuries with a syndesmosis screw. Foot Ankle 1989;9:290-293.
Baxter DE: The Foot and Ankle in Sports. St Louis, MO, Mosby-Year Book, 1995, p 30.
Pfeffer GB (ed): Chronic Ankle Pain in the Athlete. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, p 11.
Question 77
A 16-year-old boy has abdominal and back pain after being involved in a high-velocity head-on motor vehicle accident. He was restrained in the rear of the automobile by a lap belt only. A radiograph and CT scan are shown in Figure 47. The patient has no other injuries. Optimal management should include
Explanation
REFERENCES: Greenwald TA, Mann DC: Pediatric seatbelt injuries: Diagnosis and treatment of lumbar flexion-distraction injuries. Paraplegia 1994;32:743-751.
Glassman SD, Johnson JR, Holt RT: Seatbelt injuries in children. J Trauma 1992;33:882-886.
Raney EM, Bennett JT: Pediatric Chance fracture. Spine 1992;17:1522-1524.
Question 78
A 16-year-old girl has had anterior leg pain and a mass for the past 8 months. Figures 2a and 2b show a radiograph and an H & E histologic specimen. Which of the following disorders is believed to be a precursor of this lesion?
Explanation
REFERENCE: Springfield DS, Rosenberg AE, Mankin HJ, et al: Relationship between osteofibrous dysplasia and adamantinoma. Clin Orthop 1994;309:234-244.
Question 79
A 20-year-old minor league baseball pitcher is diagnosed with a symptomatic torn ulnar collateral ligament (UCL) in his pitching elbow. Nonsurgical management consisting of rest and physical therapy aimed at elbow strengthening has
Explanation
Question 80
A 22-year-old college football player reports shortness of breath and dyspnea after a tackle. Examination reveals tachypnea, tachycardia, the trachea is shifted to the right, and there are decreased breath sounds on the left lung fields. The first line of treatment on the field should be
Explanation
REFERENCES: Amaral JF: Thoracoabdominal injuries in the athlete. Clin Sports Med 1997;16:739-753.
Perron AD: Chest pain in athletes. Clin Sports Med 2003;22:37-50.
Question 81
A 45-year-old recreational tennis player underwent arthroscopic decompression and mini-open repair of a small supraspinatus tendon tear 3 weeks ago after nonsurgical management failed to provide relief. He now has pain, swelling about the wound, erythema, and purulent drainage. The patient is returned to the operating room for irrigation, debridement, and cultures. What is the most common organism causing this infection?
Explanation
REFERENCES: Herrera MF, Bauer G, Reynolds F, et al: Infection after mini-open rotator cuff repair. J Shoulder Elbow Surg 2002;11:605-608.
Settecerri JJ, Pitner MA, Rock MG, et al: Infection after rotator cuff repair. J Shoulder Elbow Surg 1999;8:1-5.
Question 82
Figure 1 is the anteroposterior radiograph of a 20-year-old dancer who fell during his routine and injured his right foot. What is the most appropriate treatment?
Explanation
Question 83
0 mmol/L (normal < 2.5), 1 hour postinjury it was 3.5 mmol/L, and it is now 5 mmol/L. His core temperature is 93 degrees F (34 degrees C). What is the most appropriate management for the femoral shaft fracture at this point?
Explanation
Question 84
A 22-year-old volleyball player has atrophy of the infraspinatus muscle. This deficit is the result of entrapment of what nerve?
Explanation
REFERENCES: Ferretti A, Cerullo G, Russo G: Suprascapular neuropathy in volleyball players. J Bone Joint Surg Am 1987;69:260-263.
Bigliani LU, Dalsey RM, McCann PD, April EW: An anatomical study of the suprascapular nerve. Arthroscopy 1990;6:301-305.
Question 85
Figures 5a and 5b show the radiographs of a 21 -year-old wrestler who reports that his leg was rolled over while wrestling. The patient has decreased sensation and function in the distribution of the peroneal nerve, and he has absent pulses. What is the most appropriate initial management at this time?
Explanation
intervention of the artery, but documentation with studies would be appropriate. Delayed reconstruction of injured structures is appropriate.
REFERENCES: Fanelli GC, Orcutt DR, Edson CJ: The multiple- ligament injured knee: Evaluation, treatment, and results. Arthroscopy 2005;21:471 -486.
McDonough EB Jr, Wojtys EM: Multiligamentous injuries of the knee and associated vascular injuries.
Am J Sports Med 2009;37:156-159.
Wascher DC: High-velocity knee dislocation with vascular injury: Treatment principles. Clin Sports Med 2000;19:457-477.
Question 86
A 57-year-old woman experiences pain 1 year after total knee arthroplasty (TKA). She reports sharp anterior pain and a painful catching sensation that is aggravated by rising from a chair or climbing stairs. Physical examination reveals a mild effusion and a range of motion of 2° to 130°, with patellar crepitus. The symptoms are reproduced by resisted knee extension. Radiographs show a well-aligned posterior- stabilized TKA without evidence of component loosening. What is the most likely cause of this patient's pain?
Explanation
Patellar clunk syndrome is caused by the development of a fibrous nodule on the posterior aspect of the quadriceps tendon at its insertion into the patella. It causes a painful catching sensation when the extensor mechanism traverses over the trochlear notch as the knee extends from 45° of flexion to 30° from full extension. It characteristically occurs in posterior stabilized total knee arthroplasties and appears to be related to femoral component design. The syndrome can usually be prevented by excising the residual synovial fold just proximal to the patella. Flexion gap instability can also cause a painful total knee arthroplasty but is less common in posterior stabilized implants. Femoral component malrotation can cause pain attributable to a flexion gap imbalance or patellar tracking problems. Polyethylene wear would be unlikely after just 1 year. Patellar clunk syndrome can usually be addressed successfully with arthroscopic synovectomy. Recurrence is uncommon. Physical therapy may help to strengthen the quadriceps following synovectomy but would not resolve the clunk syndrome symptoms. Femoral or tibial insert revision is not indicated if patellar clunk syndrome is the only problem resulting in a painful
total knee arthroplasty.
Question 87
A 55-year-old woman has slowly increasing pain at the distal end of her little finger that is exacerbated by cold temperatures. She denies any history of trauma to her hands and is employed as a school teacher. The histology of the resected specimen is shown in Figure 71. What is the most likely diagnosis?
Explanation
REFERENCES: Zook EG, Brown RE: The perionychium, in Green DP, Hotchkiss RN, Pederson WC (eds): Green’s Operative Hand Surgery, ed 4. Philadelphia, PA, Churchill Livingstone, 1999, vol 2, pp 1353-1380.
McDermott EM, Weiss AP: Glomus tumors. J Hand Surg Am 2006;31:1397-1400.
Question 88
Figure 100 is the MR image of a 19-year-old man who sustains recurrent anterior shoulder dislocations. The lesion shown occupies approximately 10% of the articular surface. What is the most appropriate treatment?
Explanation
The MR image shows a bony Bankart lesion involving less than 20% of the glenoid joint surface. One series reported high success rates after arthroscopic treatment when the defect was incorporated into the repair. Anterior bony deficiencies occupying more than 25% to 30% of the glenoid joint surface treated with soft-tissue repair only are associated with high
recurrence rates. In these patients, an open or arthroscopic coracoid transfer or distal tibial allograft reconstruction should be considered. ORIF has been reported for treatment of large acute glenoid rim fractures, but is not recommended for recurrent anterior shoulder instability in the setting of a 10% glenoid rim fracture.
Question 89
An 18-year-old man sustains an injury to his lateral ankle after being kicked while playing soccer. He reports persistent pain on the lateral ankle as well as a popping sensation with attempted ankle dorsiflexion and eversion. Which of the following structures anatomically restrains the retracted structure shown in Figure 12?
Explanation
REFERENCES: Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2003, pp 81-89.
Sarrafian S: The Anatomy of the Foot and Ankle: Descriptive, Topographic, Functional, ed 2. Philadelphia, PA, JB Lippincott, 1993, pp 113-158.
Question 90
A 40-year-old woman has a symptomatic mass on the anterior aspect of the ankle. She reports no constitutional symptoms. An MRI scan is shown in Figure 12. What is the most likely diagnosis?
Explanation
REFERENCES: Kransdorf MJ, Jelinek JS, Moser RP Jr, et al: Soft tissue masses: Diagnosis using MR imaging. Am J Roentgenol 1989;153:541-547.
Wetzel LH, Levine E: Soft-tissue tumors of the foot: Value of MR imaging for specific diagnosis. Am J Roentgenol 1990;155:1025-1030.
Gerster JC, Landry M, Dufresne L, Meuwly JY: Imaging of tophaceous gout: Computed tomography provide specific images compared with magnetic resonance imaging and ultrasonography. Ann Rheum Dis 2002;61:52-54.
Question 91
Figure 83a shows an axillary radiograph and Figures 83b and 83c show axial MR arthrograms of a 20-year-old collegiate offensive lineman who has shoulder pain while pass-blocking. He sustained a shoulder injury 3 months earlier when he "jammed it." Prior to this injury, he denies any pain or instability in either shoulder. Despite undergoing rehabilitation with a physical therapist and trainer and abstaining from playing for 6 weeks, he is currently unable to play because of his symptoms. Examination reveals full active range of motion, a positive jerk test which reproduces his symptoms, and a grade 2 posterior translation of the humeral head with load and shift testing which also reproduces his symptoms. What is the best management option to allow him to return to his pre-injury function next season? Review Topic
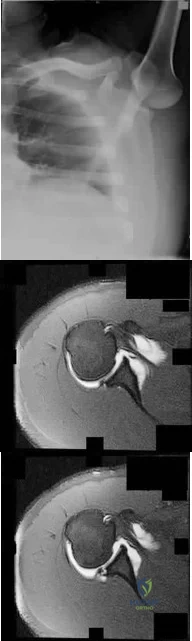
Explanation
Question 92
Which of the following is the only nonreversible effect of anabolic steroids? Review Topic
Explanation
Question 93
When performing a Green transfer for cerebral palsy—flexor carpi ulnaris (FCU) to extensor carpi radialis brevis (ECRB)—in addition to improving wrist extension, what other motion may be improved if the FCU is routed around the ulna instead of through the interosseous membrane?
Explanation
The typical upper extremity deformity in spastic hemiplegic cerebral palsy consists of shoulder internal rotation, elbow flexion, forearm pronation and wrist flexion, and ulnar deviation. The pronation position of the forearm can make bimanual activities more challenging for the child. The wrist flexion and ulnar deviation deformity interferes with finger function and therefore with grasp and release patterns. By transferring the FCU tendon to the ECRB, the deforming force is released, and central wrist extension is augmented. This transfer can lead to a supination moment when it is routed around the ulna to the ECRB insertion on the dorsum of the wrist. Thumb and finger extension are not affected by an FCU-to-ECRB tendon transfer. Forearm supination, not pronation, is potentially improved with this tendon transfer.
Question 94
What is the most appropriate treatment for a 17-year-old boy who sustained a gunshot wound to his forearm from a handgun with a muzzle-velocity of 1000 feet/second if he is neurovascularly intact and radiographs reveal no fracture?

Explanation
The two referenced articles offer guidance for treating low-velocity gunshot injuries with stable, non-operative fracture patterns. The first article by Geissler et al is a retrospective study comparing 25 patients that prospectively received local irrigation and debridement, tetanus prophylaxis and a long acting cephalosporin intramuscularly to a random retrospective sample of 25 patients with similar ballistic-induced fractures and wounds managed by local debridement and 48h of intravenous antibiotics. One infection occurred in each group, requiring further therapy. It was concluded that patients with low-velocity gunshot induced fractures can be managed without the use of short-term intravenous antibiotics with no increased risk of infection.
In the second study, Dickey et al evaluated the efficacy of an outpatient management protocol for patients with a gunshot-induced fracture with a stable, non-operative configuration. 41 patients with a grade I or II open, nonoperative fracture secondary to a low-velocity bullet were treated with 1gm of cefazolin administered in the emergency room and a 7-day course of oral cephalexin. No patient developed a deep infection. Thus, local I&D, tetanus, and oral antibiotics for 2-3 days is adequate for low velocity gunshot wounds
Question 95
A 15-year-old wrestler sustains an abduction, hyperextension, and external rotation injury to his right shoulder. The MRI scan findings shown in Figures 27a and 27b are most consistent with Review Topic
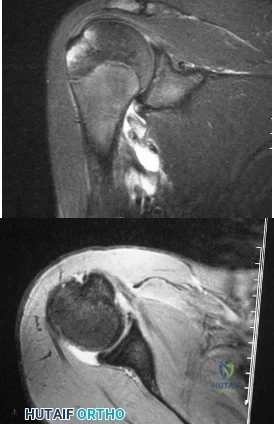
Explanation
Question 96
Which of the following conditions is associated with palmoplantar pustulosis?
Explanation
REFERENCES: Wirth MA, Rockwood CA: Disorders of the sternoclavicular joint, in Rockwood CA, Matsen FA, Wirth MA, et al (eds): The Shoulder. Philadelphia, PA,
WB Saunders, 2004, vol 2, pp 608-609.
Sonozaki H, Azuma A, Okai K, et al: Clinical features of 22 cases with inter-sterno-costo-clavicular ossification: A new rheumatic syndrome. Arch Orthop Trauma Surg 1979;95:13-22.
Question 97
A 13-year-old baseball pitcher presents with worsening medial-sided elbow pain. He pitches 7 months out of the year, throws 85 pitches per game and plays in two games per week. His fastball speed is approximately 75mph. He regularly plays outfield once he has been relieved of pitching. Which of the following is most likely contributing to his elbow pain? Review Topic
Explanation
Little League elbow is a medial-sided overuse injury that occurs in the skeletally immature athlete. During execution of the baseball pitch, tremendous valgus and extension stresses occur at the elbow. Repetitive microtrauma can ultimately injure the medial epicondyle apophysis, ulnar collateral ligament or the flexor-pronator muscle mass. Limiting the number of pitches and innings played per game, as well as the number of months of competitive pitching per year, has been recommended to prevent these overuse injuries in the young athlete.
Olsen et al performed a case control study to determine risk factors associated with the development of shoulder and elbow injuries in adolescent baseball pitchers. Greater than 8 months of competitive pitching per year, more than 80 pitches per game and a fastball speed of greater than 85mph were all associated with increased risk of injury. Continued pitching despite arm fatigue and pain, being a starting pitcher, greater number of warm-up pitches, participating in showcases and regular use of NSAIDs were also associated with injury. The type of pitch (fastball, changeups and breaking balls) and continued play in a different position once being relieved was not associated with increased risk of injury.
Andrews et al authored a review article on ulnar collateral ligament injuries in throwing athletes. According to the USA Baseball Medical/Safety Advisory Committee, young baseball pitchers should avoid breaking pitches, such as curveballs and sliders, and avoid year-round baseball. A minimum of 3 months of complete rest from pitching per year is vital. Youth pitching coaches should be educated to ensure proper pitching mechanics are being reinforced.
Illustration A is a table depicting the recommended maximum number of pitches by age group.
Incorrect Answers:
Question 98
A 62-year-old man with a long history of ankylosing spondylitis has neck pain after lightly bumping his head on the wall. Examination reveals neck pain with any attempted motion; the neurologic examination is normal. Plain radiographs show extensive ankylosis of the cervical spine and kyphosis but no fracture. What is the next most appropriate step in management?
Explanation
REFERENCES: Brigham CD: Ankylosing spondylitis and seronegative spondyloarthropathies, in Clark CR (ed): The Cervical Spine, ed 3. Philadelphia, PA, Lippincott Raven, 1998,
pp 724-727.
McDowell GS, Cammisa FP, Eismont FJ: Hyperextension injuries of the cervical spine, in Levine AM, Eismont FJ, Garfin SR, Zigler JE (eds): Spine Trauma. Philadelphia, PA,
WB Saunders, 1998, pp 372-374.
Question 99
In children with moderate to severe osteogenesis imperfecta (OI), intravenous pamidronate therapy has been shown to increase the thickness of cortical bone. This occurs primarily as a consequence of
Explanation
REFERENCES: Zeitlin L, Fassier F, Glorieux FH: Modern approach to children with osteogenesis imperfecta. J Pediatr Orthop B 2003;12:77-87.
Falk MJ, Heeger S, Lynch KA, et al: Intravenous bisphosphonate therapy in children with osteogenesis imperfecta. Pediatrics 2003;111:573-578.
Glorieux FH, Bishop NJ, Plotkin H, et al: Cyclic administration of pamidronate in children with severe osteogenesis imperfecta. N Engl J Med 1998;339:947-952.
Question 100
An AP radiograph of the pelvis is shown in Figure 4. What muscle attaches to the avulsed fragment of bone identified by the arrow?
Explanation
REFERENCES: Woodburne RT (ed): Essentials of Human Anatomy. New York, NY, Oxford University Press, 1978, pp 542-545.
Metzmaker JN, Pappas AM: Avulsion fractures of the pelvis. Am J Sports Med 1985;13:349-358.
