OITE & ABOS Orthopedic Board Exam MCQs: Hip & Knee Arthroplasty, Fracture | Part 196
Key Takeaway
This page offers Part 196 of a high-yield interactive MCQ quiz for orthopedic residents and surgeons preparing for OITE/AAOS/ABOS board certification. It contains 50 questions covering arthroplasty, fracture, hip, and knee, with study and exam modes to enhance your board exam preparation.
OITE & ABOS Orthopedic Board Exam MCQs: Hip & Knee Arthroplasty, Fracture | Part 196
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
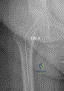
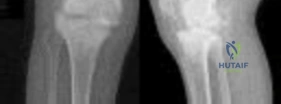
A 72-year-old female presents with thigh pain after a fall. She had a primary total hip arthroplasty 10 years ago. Radiographs demonstrate a periprosthetic fracture around the femoral stem. The stem is determined to be loose, but there is adequate proximal and distal bone stock.
What is the most appropriate management according to the Vancouver classification system?
Explanation
Question 2
During a primary posterior-stabilized total knee arthroplasty, the trial components are placed and the knee's range of motion is assessed. The knee is noted to be excessively tight in both full extension and at 90 degrees of flexion. What is the most appropriate next intraoperative step to achieve proper balancing?

Explanation
Question 3
The direct anterior approach (Smith-Petersen) to the hip is increasingly popular for total hip arthroplasty. This approach utilizes a true internervous and intermuscular plane. Deep dissection occurs between which of the following muscles?
Explanation
Question 4
In the evaluation of a persistently painful total knee arthroplasty, synovial fluid is aspirated and an alpha-defensin test is ordered.
What is the primary role and characteristic of alpha-defensin in this clinical context?

Explanation
Question 5
According to the 2018 International Consensus Meeting (ICM) criteria for periprosthetic joint infection (PJI), which of the following findings is considered a major criterion that independently confirms the diagnosis of a PJI?
Explanation
Question 6
A 65-year-old female presents with a painful catching sensation and an audible 'clunk' in her knee when extending from a flexed position. She underwent a primary posterior-stabilized total knee arthroplasty 18 months ago.
What is the most likely etiology of her symptoms?

Explanation
Question 7
Medial unicompartmental knee arthroplasty (UKA) offers a less invasive alternative to total knee arthroplasty for isolated medial compartment osteoarthritis. Which of the following is classically considered an absolute contraindication to performing a medial UKA?
Explanation
Question 8
A 55-year-old male with a metal-on-metal total hip arthroplasty placed 8 years ago presents with worsening groin pain and a palpable anterior mass. Serum cobalt and chromium levels are significantly elevated. MRI reveals a solid and cystic mass communicating with the joint space. What is the most likely diagnosis?
Explanation
Question 9
During a primary total knee arthroplasty for a severe varus deformity, the surgeon proceeds with sequential medial releases. After initial osteophyte removal and deep medial collateral ligament (MCL) release, trial components are placed. The knee is noted to be well-balanced in flexion but remains significantly tight on the medial side in full extension.
Which specific structure should be released next to achieve balance?

Explanation
Question 10
Tranexamic acid (TXA) is widely used in orthopedic arthroplasty to minimize perioperative blood loss and reduce transfusion rates. What is the precise pharmacological mechanism of action of TXA?
Explanation
Question 11
A 45-year-old male who underwent a ceramic-on-ceramic total hip arthroplasty 3 years ago reports a new, loud 'squeaking' noise emanating from his hip during ambulation. He denies pain or instability. What biomechanical or surgical factor is most strongly associated with the development of squeaking in a ceramic-on-ceramic bearing surface?
Explanation
Question 12
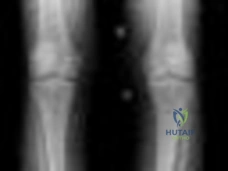
In total hip arthroplasty, the 'safe zone' for acetabular component placement described by Lewinnek is historically targeted to minimize the risk of postoperative dislocation.
What are the classically described target ranges for acetabular abduction (inclination) and anteversion in this zone?
Explanation
Question 13
A 78-year-old female sustains a closed Su Type II distal femur fracture superior to a well-fixed posterior-stabilized total knee arthroplasty (TKA). The femoral component has a closed-box design. Assuming closed reduction is possible, what is the most appropriate surgical management?
Explanation
Question 14
During a primary total knee arthroplasty, trial components are inserted. Evaluation reveals that the knee is perfectly stable and balanced in full extension, but demonstrates excessive medial and lateral laxity at 90 degrees of flexion. What is the most appropriate surgical adjustment to correct this imbalance?
Explanation
Question 15
A 65-year-old female undergoes a right total hip arthroplasty via a posterior approach. Postoperatively in the recovery room, she demonstrates a dense foot drop and diminished sensation over the dorsal aspect of her right foot and lateral leg.
Which of the following intraoperative factors is most commonly responsible for this specific nerve injury?

Explanation
Question 16
A 75-year-old female undergoes fixation of an unstable, reverse obliquity intertrochanteric femur fracture with a standard sliding hip screw (dynamic hip screw). Six weeks later, radiographs show catastrophic cut-out of the lag screw and medialization of the femoral shaft. What is the primary biomechanical reason a sliding hip screw is relatively contraindicated for this specific fracture pattern?
Explanation
Question 17
A 70-year-old male presents with severe anterior knee pain and a complete inability to actively extend his knee, occurring 3 years after a primary total knee arthroplasty. Imaging confirms a chronic, complete, and retracted patellar tendon rupture.
What is the most reliable reconstructive option given the chronic nature and poor tissue quality?

Explanation
Question 18
A 68-year-old female with long-standing ankylosing spondylitis and a fully fused thoracolumbar spine is planned for a primary total hip arthroplasty. How does her stiff spinopelvic complex influence the preoperative planning for acetabular component positioning?
Explanation
Question 19
A 30-year-old male sustains a vertically oriented, highly displaced femoral neck fracture (Pauwels type III). Which of the following internal fixation constructs provides the most biomechanical stability against the extreme shear forces present in this specific fracture pattern?
Explanation
Question 20
During the femoral preparation of a primary total knee arthroplasty, the surgeon is utilizing a posterior referencing sizing guide.
The patient's anatomy falls exactly between sizes on the guide. If the surgeon elects to downsize the femoral component, what is the most likely geometric consequence?

Explanation
Question 21
During a primary total knee arthroplasty, trial components are placed. The knee is symmetric and balanced in extension, but it is symmetrically tight in 90 degrees of flexion. Which of the following is the most appropriate intraoperative step to balance the knee?
Explanation
Question 22
A 78-year-old female presents with thigh pain and inability to bear weight after a mechanical fall. Radiographs demonstrate a periprosthetic femur fracture around the tip of her cemented total hip arthroplasty stem. The stem is grossly loose on imaging, and the proximal femoral bone stock is severely deficient with diaphyseal thinning.
What is the most appropriate surgical management?

Explanation
Question 23
A 45-year-old male who underwent a ceramic-on-ceramic total hip arthroplasty 4 years ago complains of a loud squeaking noise from his hip with every step. He denies pain or instability. Which of the following is the most significant risk factor for this phenomenon?
Explanation
Question 24
Postoperatively, a patient who underwent a primary total knee arthroplasty complains of anterior knee pain and a feeling of instability. Radiographs demonstrate lateral patellar tilt and subluxation. Which of the following errors during component positioning most likely contributed to this finding?
Explanation
Question 25
A 55-year-old female with a metal-on-metal total hip arthroplasty presents with new-onset groin pain and a palpable anterior mass. Laboratory evaluation shows normal CRP and ESR. An MRI with MARS sequencing reveals a large cystic pseudotumor. What is the primary pathophysiology underlying this complication?
Explanation
Question 26
A 70-year-old female sustains a supracondylar femur fracture 2 cm above the flange of her primary total knee arthroplasty. The femoral component is a posterior-stabilized, closed-box design and appears well-fixed. Which of the following is the most appropriate fixation strategy?
Explanation
Question 27
During a direct anterior (Smith-Petersen) approach for total hip arthroplasty, the surgeon performs deep dissection between the sartorius and tensor fasciae latae. Which nerve is at greatest risk of iatrogenic injury if dissection is carelessly carried too superficially in this interval?
Explanation
Question 28
A 65-year-old male presents with persistent pain 3 years after a primary total knee arthroplasty. Serum ESR is 45 mm/hr and CRP is 25 mg/L. Synovial fluid aspiration yields a WBC count of 4,500 cells/μL with 85% PMNs. What is the most appropriate next step in management?
Explanation
Question 29
A patient undergoes a primary total hip arthroplasty. Postoperative templating reveals that the femoral offset was decreased by 15 mm compared to the contralateral native hip. What is the most likely clinical consequence of this biomechanical alteration?
Explanation
Question 30
Revision of a 20-year-old total knee arthroplasty reveals severe destruction of the polyethylene insert. The implant records indicate the polyethylene was sterilized by gamma irradiation in air. Which of the following wear mechanisms is predominantly responsible for this failure?
Explanation
Question 31
Six months after a posterior-stabilized total knee arthroplasty, a patient complains of a painful catching sensation in the knee when extending from a flexed position, specifically between 30 and 40 degrees of flexion. What is the most likely etiology?
Explanation
Question 32
A patient sustains a fall 3 weeks after an uncomplicated primary total hip arthroplasty. Radiographs show a minimally displaced (<1 cm) fracture of the greater trochanter. The femoral stem remains perfectly aligned and well-fixed without evidence of subsidence. What is the most appropriate management?
Explanation
Question 33
A 60-year-old patient presents for a 10-year follow-up after receiving a fully porous-coated, extensively fixed cylindrical stem total hip arthroplasty. Radiographs demonstrate excellent distal diaphyseal fixation but severe localized proximal medial bone resorption. The patient is entirely asymptomatic. What is the primary cause of this radiographic finding?
Explanation
Question 34
Fourteen days after an elective total hip arthroplasty, a patient returns with a fever of 101.5°F, escalating hip pain, and a draining, erythematous surgical wound. Radiographs show perfectly positioned, well-fixed components. What is the most appropriate initial surgical intervention?
Explanation
Question 35
A 68-year-old male undergoes a primary total hip arthroplasty via a posterior approach. Postoperatively, he experiences recurrent posterior dislocations. Radiographs show the acetabular component at 40 degrees of abduction and 20 degrees of anteversion, and the femoral stem is well-fixed in 15 degrees of anteversion. Which of the following pre-existing conditions is the most significant risk factor for this patient's recurrent instability despite appropriate component positioning?
Explanation
Question 36
A 68-year-old male is undergoing a total hip arthroplasty. The surgeon plans to use highly cross-linked polyethylene (HXLPE) to reduce wear. Which of the following manufacturing processes is critical to eliminate free radicals generated during the cross-linking process and prevent in vivo oxidative degradation?
Explanation
Question 37
During a primary posterior-stabilized total knee arthroplasty, the knee is balanced in extension but is found to be excessively tight in flexion, preventing full range of motion. The extension gap is symmetric and perfectly tensioned. Which of the following is the most appropriate step to correct this kinematic mismatch?
Explanation
Question 38
A 78-year-old female sustains a periprosthetic femur fracture around her cementless total hip arthroplasty after a fall. Radiographs demonstrate a fracture around the tip of the stem. The stem is radiographically loose, and there is significant proximal osteolysis with poor bone stock in the proximal metaphysis. Which of the following is the most appropriate management (Vancouver Type B3)?
Explanation
Question 39
Which of the following biomechanical changes most effectively decreases the joint reactive force across the hip during a single-leg stance following a total hip arthroplasty?
Explanation
Question 40
A 65-year-old female presents with a painful clunking sensation in her knee when extending from a flexed position. She underwent a posterior-stabilized total knee arthroplasty 18 months ago. Examination reveals a palpable catch at approximately 40 degrees of flexion. Which of the following is the underlying pathophysiology of this condition?
Explanation
Question 41
In a patient undergoing revision total hip arthroplasty, the surgeon encounters severe pelvic discontinuity. Radiographs and intraoperative findings show complete separation of the superior and inferior hemipelvis. Which of the following surgical constructs is generally considered the most reliable for achieving stability and long-term fixation in this scenario?
Explanation
Question 42
When balancing a severe varus deformity during a primary total knee arthroplasty, the surgeon performs a sequential medial release. After releasing the deep medial collateral ligament (MCL) and removing osteophytes, the knee remains tight medially in extension but balanced in flexion. Which structure should be released next to correct the medial tightness in extension?
Explanation
Question 43
A 55-year-old male presents with acute onset of severe left knee pain 14 days after a primary total knee arthroplasty. The knee is swollen, erythematous, and warm. Aspiration yields purulent synovial fluid with a white blood cell count of 65,000 cells/uL (95% neutrophils). What is the most appropriate surgical management?
Explanation
Question 44
A patient with a metal-on-metal total hip arthroplasty presents 5 years postoperatively with groin pain and a palpable mass. MRI with metal artifact reduction sequence (MARS) reveals a large cystic lesion adjacent to the joint. Histology from a subsequent revision surgery shows a perivascular lymphocytic infiltrate. This reaction is best classified as which type of hypersensitivity?
Explanation
Question 45
An 82-year-old male sustains a closed supracondylar femur fracture just proximal to his total knee arthroplasty (Lewis-Rorabeck Type II). The femoral component is well-fixed, and there is no evidence of osteolysis. Which of the following is the most appropriate surgical treatment?
Explanation
Question 46
During a total knee arthroplasty, optimizing patellofemoral tracking is crucial. Which of the following technical errors most strongly predisposes the patella to track laterally and potentially subluxate or dislocate?
Explanation
Question 47
A 70-year-old active female undergoes a total hip arthroplasty via a posterior approach for a displaced femoral neck fracture. Compared to a bipolar hemiarthroplasty for the same indication, which of the following outcomes is most associated with total hip arthroplasty?
Explanation
Question 48
Which of the following is considered an absolute contraindication for a medial unicompartmental knee arthroplasty (UKA)?
Explanation
Question 49
A surgeon encounters a well-fixed, proximally porous-coated femoral stem that must be removed for a recurrent periprosthetic joint infection. To facilitate extraction while minimizing catastrophic bone loss, the surgeon plans an extended trochanteric osteotomy (ETO). What is the optimal location and length for the osteotomy?
Explanation
Question 50
A patient with a large-diameter metal-on-polyethylene total hip arthroplasty presents with unexplained hip pain 4 years postoperatively. Radiographs show a well-fixed implant with a short, thin femoral trunnion. Serum cobalt levels are highly elevated, while chromium is normal. What is the most likely diagnosis?
Explanation
Question 51
Regarding the kinematics of the native knee and its replication in total knee arthroplasty (TKA), what is the primary biomechanical function of femoral rollback during deep flexion?
Explanation
Question 52
A 45-year-old male with end-stage avascular necrosis undergoes a primary total hip arthroplasty. The surgeon uses the direct anterior (Smith-Petersen) approach. Which of the following nerve injuries is most specifically associated with the superficial dissection of this approach?
Explanation
Question 53
A 79-year-old male is scheduled for a total hip arthroplasty. He has a history of severe heterotopic ossification (HO) following a contralateral THA. Which of the following prophylactic regimens is most appropriate to prevent HO in this patient?
Explanation
Question 54
When setting femoral rotation during a primary total knee arthroplasty, the surgeon aligns the epicondylar axis. If the surgeon mistakenly references the posterior condylar axis in a severely valgus knee with lateral femoral condyle hypoplasia without compensating for it, what is the most likely error?
Explanation
Question 55
A 72-year-old woman presents with persistent, disabling knee stiffness 8 weeks after a primary total knee arthroplasty. Her active range of motion is 15 to 65 degrees. Physical therapy has failed to improve her motion. Radiographs show well-positioned components without loosening. What is the most appropriate next step in management?
Explanation
Question 56
A patient presents with a recurrent knee effusion and a feeling of "giving way" when descending stairs 1 year after a posterior-stabilized TKA. Radiographs show well-fixed components. Physical exam reveals increased anteroposterior laxity at 90 degrees of flexion but stability in full extension. What intraoperative error most likely caused this isolated flexion instability?
Explanation
Question 57
A 45-year-old male complains of a high-pitched, audible squeaking from his hip during walking 3 years after a primary total hip arthroplasty. Radiographs show well-fixed components with a cup abduction angle of 55 degrees. Which combination of bearing surfaces is most associated with this clinical phenomenon?
Explanation
Question 58
When evaluating a painful total knee arthroplasty for potential periprosthetic joint infection, which of the following synovial fluid biomarkers acts by binding to microbial cell membranes, forming pore-like defects, and offers exceptionally high sensitivity and specificity?
Explanation
Question 59
A 78-year-old female presents with a periprosthetic femur fracture 12 years after a primary THA. Radiographs reveal a fracture around a loose femoral stem with severe comminution and nearly completely deficient proximal bone stock extending to the diaphysis. According to the Vancouver classification, what is the most appropriate surgical treatment?
Explanation
Question 60
During a primary total knee arthroplasty, the surgeon accidentally internally rotates the femoral component 5 degrees relative to the surgical epicondylar axis. What is the most likely biomechanical consequence of this positioning error?
Explanation
Question 61
A surgeon is performing a primary THA via the direct anterior (Smith-Petersen) approach. During the deep dissection between the tensor fasciae latae and sartorius, a vascular bundle is routinely encountered crossing the field that must be ligated to prevent excessive bleeding. This bundle represents branches of which of the following arteries?
Explanation
Question 62
A 68-year-old male sustains a supracondylar femur fracture just above a posterior-stabilized total knee arthroplasty. Radiographs confirm the fracture is displaced but the femoral component remains rigidly fixed with no osteolysis. What is the preferred surgical treatment?
Explanation
Question 63
What anatomic or mechanical feature primarily drives posterior femoral rollback during deep flexion in a cruciate-retaining (CR) total knee arthroplasty?
Explanation
Question 64
A 65-year-old female presents with recurrent anterior dislocations of her total hip arthroplasty. Intraoperative evaluation during revision reveals that the well-fixed acetabular component is in 35 degrees of anteversion, and the well-fixed femoral stem is in 20 degrees of anteversion. What is the most appropriate management?
Explanation
Question 65
A patient develops a diffuse, eczematous dermatitis over the surgical knee and progressive joint stiffness 6 months following a primary TKA. Infection is definitively ruled out. Patch testing confirms a severe nickel allergy. The pathogenesis of this reaction is best described as:
Explanation
Question 66
Which of the following design factors has been most strongly associated with an increased risk of mechanically assisted crevice corrosion (trunnionosis) at the head-neck junction in total hip arthroplasty?
Explanation
Question 67
A 70-year-old male presents with a complete, chronic rupture of the patellar tendon 3 months after a primary TKA. He cannot actively extend his knee against gravity. Primary repair is impossible due to tissue retraction. What is the most reliable surgical reconstruction technique?
Explanation
Question 68
Which of the following is classically considered an absolute contraindication to performing a medial unicompartmental knee arthroplasty (UKA)?
Explanation
Question 69
A patient complains that their operative leg feels longer after a primary THA. Clinical examination reveals the distance from the umbilicus to the medial malleolus is equal bilaterally, but the distance from the anterior superior iliac spine (ASIS) to the medial malleolus is 2 cm longer on the operative side. Which of the following best explains these findings?
Explanation
Question 70
Which of the following preoperative patient characteristics is statistically the most significant independent risk factor for deep wound infection and poor wound healing following total knee arthroplasty?
Explanation
Question 71
Tranexamic acid (TXA) is routinely utilized in total joint arthroplasty to minimize perioperative blood loss. Which of the following describes its precise pharmacological mechanism of action?
Explanation
None
