Orthopedic Board Review MCQs: Spine & Scoliosis | Part 106

Key Takeaway
This page presents Part 106 of an orthopedic board review, offering 50 high-yield, OITE/AAOS-style MCQs focusing on Scoliosis and Spine. Designed for orthopedic surgeons and residents, it facilitates ABOS/AAOS certification exam preparation through interactive study and exam modes.
Orthopedic Board Review MCQs: Spine & Scoliosis | Part 106
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 14-year-old girl with adolescent idiopathic scoliosis presents for evaluation. Standing radiographs show a right thoracic curve of 55°, a left lumbar curve of 35°, and a proximal thoracic curve of 20°. On side-bending films, the thoracic curve reduces to 30°, the lumbar curve to 15°, and the proximal thoracic to 10°. The apical lumbar vertebra is L2, and the center sacral vertical line (CSVL) touches the medial border of the left L2 pedicle. Sagittal T5-T12 kyphosis is +25°. Based on the Lenke classification, what is the correct curve type and modifier?
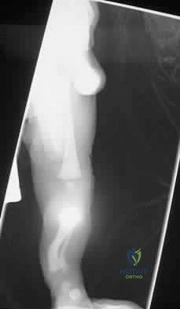
Explanation
Question 2
A 65-year-old man presents with progressive gait unsteadiness and loss of fine motor skills in his hands over the past 8 months. Examination reveals a positive Hoffmann's sign and hyperreflexia in the lower extremities. MRI of the cervical spine demonstrates severe multi-level spondylotic myelopathy. Which of the following MRI findings is the most reliable predictor of poor neurologic recovery following surgical decompression?
Explanation
Question 3
A 52-year-old man with a history of intravenous drug use presents with severe back pain, fevers, and new-onset profound right foot drop. His ESR is 95 mm/hr and CRP is 120 mg/L. MRI confirms a large dorsal epidural abscess at L4-L5 with severe thecal sac compression. What is the most appropriate next step in management?
Explanation
Question 4
A newborn is evaluated for a spinal deformity noted at birth. Radiographs reveal a congenital spinal anomaly. Which of the following specific congenital vertebral anomalies carries the highest risk of rapid curve progression and often requires early in situ fusion?
Explanation
Question 5
A 68-year-old woman presents with severe mechanical low back pain, forward stooping posture, and early satiety. Radiographs demonstrate degenerative adult spinal deformity. Her measured pelvic incidence (PI) is 60°. To restore optimal spinopelvic sagittal balance postoperatively, what is the surgical target for her lumbar lordosis (LL)?
Explanation
Question 6
A 16-year-old male gymnast presents with chronic low back pain and radicular symptoms radiating down his left leg. Lateral radiographs demonstrate a L5-S1 isthmic spondylolisthesis with a 65% slip (Meyerding Grade III). Which nerve root is most commonly compressed in this specific condition?
Explanation
Question 7
A 35-year-old man falls from a 10-foot ladder and sustains a thoracolumbar injury. He is neurologically intact. CT demonstrates an L1 burst fracture with 40% loss of anterior body height and 20% canal compromise. MRI confirms that the posterior ligamentous complex (PLC) is fully intact. Based on the Thoracolumbar Injury Classification and Severity Score (TLICS), what is his total score and the recommended management?
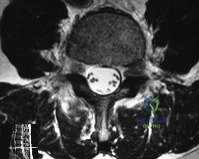
Explanation
Question 8
A 55-year-old woman with a 20-year history of rheumatoid arthritis complains of severe occipital headaches and upper extremity paresthesias. Lateral cervical spine radiographs show anterior atlantoaxial subluxation. Which of the following measurements is the most critical and direct predictor of impending neurologic deficit, indicating the need for surgical stabilization?
Explanation
Question 9
A 15-year-old boy presents with progressive mid-back pain and a rounded posture. Standing lateral radiographs reveal a thoracic kyphosis of 65°. Which of the following defines the strict Sorensen radiographic criteria for the diagnosis of Scheuermann's kyphosis?
Explanation
Question 10
A 14-year-old female soccer player presents with acute right-sided low back pain that is exacerbated by spinal extension. Anteroposterior, lateral, and oblique radiographs of the lumbar spine are completely normal. What is the most appropriate next imaging modality to definitively evaluate for an acute pars interarticularis stress reaction or fracture?
Explanation
Question 11
A 13-year-old boy with Duchenne muscular dystrophy is non-ambulatory and has developed a progressive scoliotic curve of 35°. His forced vital capacity (FVC) is 45% of predicted. What is the most appropriate management for his spinal deformity?
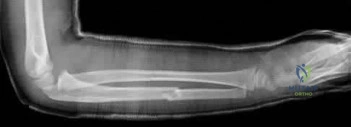
Explanation
Question 12
A 6-year-old girl is diagnosed with Klippel-Feil syndrome. Physical examination demonstrates a short neck, low posterior hairline, and severely limited cervical range of motion. Given the known associations of this syndrome, which of the following screening tests is mandatory?
Explanation
Question 13
A 45-year-old man with a known history of ankylosing spondylitis presents to the emergency department after a minor trip and fall. He complains of moderate neck pain. He is neurologically intact. Cross-table lateral radiographs of the cervical spine are difficult to interpret due to extensive syndesmophytes and overlapping shoulder anatomy, but the resident interprets them as 'negative for acute fracture'. What is the most appropriate next step in management?
Explanation
Question 14
A 28-year-old woman is involved in a motor vehicle collision and sustains a traumatic spondylolisthesis of C2 (Hangman's fracture). Imaging demonstrates severe angulation of C2 on C3 and 2 mm of anterior translation. The mechanism is determined to be flexion-distraction, classifying this as a Levine-Edwards Type IIA fracture. What is a critical principle regarding the initial non-operative management of this specific injury pattern?
Explanation
Question 15
A 68-year-old man with known cervical spondylosis slips on ice, striking his forehead and forcing his neck into sudden hyperextension. He presents to the ED with burning pain in his upper extremities and severe weakness in his hands and arms. His leg strength is 4/5 bilaterally, and he is able to ambulate with assistance. Perianal sensation is intact. What is the most likely diagnosis?
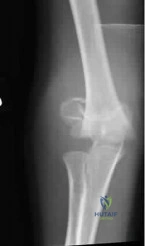
Explanation
Question 16
A 15-year-old boy presents with an acute onset of severe lower back pain radiating down his posterior right leg, accompanied by a noticeable left-sided trunk shift. He reports the pain worsens with sitting and coughing. Standing radiographs reveal a right-sided lumbar scoliosis of 20° without pedicle rotation. What is the most likely underlying etiology of this deformity?
Explanation
Question 17
When evaluating a patient with a metastatic spinal lesion, the Spinal Instability Neoplastic Score (SINS) is utilized to assess the need for surgical stabilization. Which of the following individual findings contributes the highest number of points (greatest instability) to the SINS score?
Explanation
Question 18
A 42-year-old man presents to the emergency department complaining of severe 10/10 low back pain and bilateral sciatica for the past 24 hours. He is anxious and reports 'saddle' numbness. Which of the following clinical findings is widely considered the most sensitive and earliest indicator of cauda equina syndrome?
Explanation
Question 19
A 75-year-old woman with a T-score of -3.2 undergoes balloon kyphoplasty for a painful osteoporotic compression fracture of L1. Postoperatively, she experiences immediate pain relief. Over the next year, she remains at the highest risk for developing which of the following specific complications related to the treated level?
Explanation
Question 20
A 35-year-old man is brought to the trauma bay after a high-speed rollover motor vehicle collision. He complains of severe neck pain and numbness in his right thumb. Lateral cervical spine radiographs show C5 is translated anteriorly over C6 by approximately 25% of the vertebral body width. The facet joints at C5-C6 demonstrate a 'bowtie' or 'batwing' sign. What is the most likely diagnosis?
Explanation
Question 21
A 14-year-old girl is undergoing posterior spinal fusion for adolescent idiopathic scoliosis. During the curve correction maneuver, the anesthesiologist reports a 60% decrease in motor evoked potentials (MEP) amplitude in the bilateral lower extremities. Somatosensory evoked potentials (SSEP) are unchanged. Blood pressure is 110/70 mmHg, and temperature is 36.8°C. The surgeon pauses the procedure and asks the anesthesiologist to review the medication regimen. Which of the following anesthetic agents is most likely contributing to the loss of MEP signals while sparing SSEPs?
Explanation
Question 22
A 60-year-old man presents with progressive lower extremity weakness and hyperreflexia over the past 2 weeks. He has a history of renal cell carcinoma. MRI demonstrates a metastatic lesion in the T8 vertebral body causing high-grade epidural spinal cord compression (ESCC). He is ambulatory but requires assistance. According to the NOMS framework, what is the most appropriate management strategy?

Explanation
Question 23
In the evaluation of adult spinal deformity, achieving optimal sagittal balance is critical for long-term patient outcomes. A 65-year-old woman is being planned for a long posterior spinal fusion from T10 to the pelvis. Her pelvic incidence (PI) is 58 degrees. To minimize the risk of proximal junctional kyphosis (PJK) and mechanical failure, her post-operative lumbar lordosis (LL) should ideally be targeted within what range?
Explanation
Question 24
A 24-year-old man is brought to the trauma bay intubated and sedated (GCS 3T) following a high-speed motorcycle crash. CT scan of the cervical spine reveals a unilateral C5-C6 facet dislocation. What is the most appropriate next step in management to address the cervical spine injury?
Explanation
Question 25
A 5-year-old boy is placed in a halo vest for a rigid atlantoaxial rotatory subluxation (AARS) that failed soft collar treatment and halter traction. Three days after halo application, the mother notices the child is keeping his right eye turned inward and complains of seeing double when looking to the right. Which of the following cranial nerves is most likely injured?
Explanation
Question 26
A 58-year-old male undergoes a complex 10-level posterior spinal fusion for adult degenerative scoliosis. The surgery lasts 11 hours, with an estimated blood loss of 3.5 liters. He is positioned on a Jackson table. On postoperative day 1, the patient complains of painless, bilateral vision loss. Pupillary light reflexes are sluggish. What is the most common cause of this complication in this clinical scenario?
Explanation
Question 27
Recombinant human bone morphogenetic protein-2 (rhBMP-2) is frequently used off-label in spine surgery to enhance fusion rates. When used in anterior cervical discectomy and fusion (ACDF), which of the following is the most widely recognized and significant complication associated with its use?

Explanation
Question 28
A 45-year-old intravenous drug user presents with 2 weeks of worsening back pain, fevers, and new-onset bilateral lower extremity weakness with urinary retention. MRI reveals a large epidural fluid collection with peripheral enhancement from L1 to L4 compressing the cauda equina. He is hemodynamically stable. Blood cultures are drawn. What is the most appropriate next step in management?
Explanation
Question 29
A 16-year-old boy presents with back pain that is worse at night and relieved by NSAIDs. Physical exam reveals a painful left-sided thoracic scoliosis. CT scan shows a 9 mm sclerotic lesion with a central lucent nidus in the left T8 pedicle. Which of the following is true regarding this condition?
Explanation
Question 30
A 14-year-old gymnast presents with progressive lower back pain and a noticeable 'step-off' on her lower spine. Imaging confirms a Grade III L5-S1 isthmic spondylolisthesis. During surgical intervention involving reduction of the slip and L5-S1 instrumented fusion, the patient is at highest risk for injury to which of the following nerve roots?

Explanation
Question 31
A 50-year-old woman presents with progressive myelopathy, hyperreflexia, and a sensory level at the umbilicus. MRI demonstrates a large, calcified central thoracic disc herniation at T9-T10 causing severe spinal cord compression. Which of the following surgical approaches is CONTRAINDICATED in the management of this pathology?
Explanation
Question 32
A 12-year-old boy with Duchenne Muscular Dystrophy (DMD) presents for evaluation of a progressive 45-degree thoracolumbar scoliosis. He recently became wheelchair-dependent. His forced vital capacity (FVC) is 45% of predicted. What is the most appropriate recommendation regarding his spinal deformity?
Explanation
Question 33
In the evaluation of a patient with cervical ossification of the posterior longitudinal ligament (OPLL), the 'K-line' is determined on a lateral cervical radiograph. The K-line connects the midpoints of the spinal canal at C2 and C7. A patient is considered 'K-line negative' if the OPLL mass crosses anterior to this line. What is the clinical significance of a K-line negative finding?

Explanation
Question 34
During an anterior thoracoabdominal approach for a T10-L2 fusion, the surgeon ligates multiple segmental vessels. Postoperatively, the patient is noted to have loss of bilateral lower extremity motor function and pain/temperature sensation, but preservation of proprioception and light touch. This syndrome is most likely caused by ischemia in the territory of which of the following vessels?
Explanation
Question 35
A 4-year-old girl with early-onset idiopathic scoliosis and a 65-degree curve undergoes implantation of magnetically controlled growing rods (MCGR). What is the primary advantage of this technology compared to traditional growing rods (TGR)?

Explanation
Question 36
A 22-year-old man falls 30 feet from a roof, landing on his buttocks. He complains of severe sacral pain, perineal numbness, and inability to void. Radiographs and CT demonstrate a transverse sacral fracture at the S2 level connecting bilateral longitudinal sacral fractures. Which of the following terms best describes this fracture pattern, and what is the primary neurovascular concern?
Explanation
Question 37
A 68-year-old male with a long-standing history of ankylosing spondylitis presents with localized, progressive lower back pain over the past 6 months without recent acute trauma. Inflammatory markers (CRP, ESR) are normal. Radiographs reveal a radiolucent defect and localized kyphosis at the L3-L4 intervertebral disc space with adjacent endplate sclerosis. There is no large paraspinal mass. What is the most likely diagnosis?
Explanation
Question 38
A 19-year-old male presents with slowly progressive, unilateral weakness and atrophy of his right hand and forearm intrinsic muscles over the past 2 years. He denies pain, sensory loss, or lower extremity symptoms. MRI of the cervical spine in neutral is unremarkable, but a flexion MRI demonstrates anterior displacement of the posterior dura compressing the lower cervical cord. What is the most likely diagnosis?
Explanation
Question 39
A newborn is diagnosed with multiple hemivertebrae and a unilateral unsegmented bar in the thoracic spine on screening radiographs. Given the high association of VACTERL and other congenital anomalies, which of the following screening tests is mandatory in the initial workup of this patient?
Explanation
Question 40
A 35-year-old man dives into a shallow pool and sustains an isolated C1 (atlas) burst fracture. An open-mouth odontoid view demonstrates a combined lateral mass overhang of 8 mm. According to the Rule of Spence, what structure is presumed to be incompetent, dictating the need for more rigid stabilization?
Explanation
Question 41
In the Bracing in Adolescent Idiopathic Scoliosis Trial (BRAIST), what factor was most strongly correlated with the prevention of curve progression to a surgical magnitude (>=50 degrees)?
Explanation
Question 42
A 3-year-old child presents with a congenital scoliosis. Radiographs demonstrate a unilateral unsegmented bar with fully segmented contralateral hemivertebrae at the same levels. What is the most appropriate management?
Explanation
Question 43
A 65-year-old woman undergoes corrective surgery for severe adult spinal deformity. To minimize the risk of adjacent segment disease, proximal junctional kyphosis, and mechanical failure, the pelvic incidence minus lumbar lordosis (PI-LL) should ideally be corrected to within what range?
Explanation
Question 44
A 55-year-old man presents with cervical myelopathy due to severe ossification of the posterior longitudinal ligament (OPLL) from C3-C6. Sagittal MRI and CT show the OPLL mass anteriorly exceeds the K-line (K-line negative). What is the most appropriate surgical approach?
Explanation
Question 45
A 15-year-old girl undergoes posterior spinal fusion for a 65-degree thoracic scoliosis. On post-operative day 5, she develops bilious vomiting, significant abdominal distension, and rapid weight loss. What is the most likely anatomic cause of her symptoms?
Explanation
Question 46
A 25-year-old man presents after a high-speed motor vehicle collision with quadriparesis. Imaging shows a C5-C6 bilateral facet dislocation. He is fully alert, cooperative, and medically stable.
What is the most appropriate next step in management?

Explanation
Question 47
A 45-year-old man falls from a height. CT shows an L1 burst fracture with 40% loss of height and 30% canal compromise. He is neurologically intact. MRI confirms the posterior ligamentous complex (PLC) is intact. What is his Thoracolumbar Injury Classification and Severity (TLICS) score, and what is the recommended treatment?
Explanation
Question 48
A 60-year-old man with known renal cell carcinoma presents with intractable mechanical back pain. Imaging reveals an L3 lytic metastasis with vertebral collapse, bilateral pedicle involvement, and no epidural spinal cord compression. The Spinal Instability Neoplastic Score (SINS) is 14. What is the most appropriate management?
Explanation
Question 49
According to the Spine Patient Outcomes Research Trial (SPORT) for degenerative spondylolisthesis, which of the following statements is true regarding outcomes of surgical versus non-operative treatment?
Explanation
Question 50
A 42-year-old man complains of radiating right arm pain. Examination shows weakness in wrist flexion and triceps extension, decreased sensation over the middle finger, and an absent triceps reflex. Which cervical nerve root is most likely compressed?
Explanation
Question 51
A 55-year-old man presents with severe lower back pain and low-grade fevers. MRI shows L4-L5 discitis and osteomyelitis without a significant epidural abscess. He is neurologically intact, and three sets of blood cultures are negative. What is the most appropriate next step?
Explanation
Question 52
A 14-year-old girl is undergoing a posterior spinal fusion for adolescent idiopathic scoliosis. During deformity correction, the neuromonitoring technician reports a sudden, sustained 80% decrease in motor evoked potentials (MEPs) in the bilateral lower extremities, while somatosensory evoked potentials (SSEPs) remain at baseline. A wake-up test confirms the patient cannot move her lower extremities. Which of the following anatomic structures is most likely compromised?
Explanation
Question 53
A 10-month-old infant presents with a left-sided thoracic curve measuring 35 degrees. Supine radiographs demonstrate a rib-vertebra angle difference (RVAD) of 25 degrees at the apical vertebra. Furthermore, the rib head on the concave side overlaps the apical vertebral body. What is the most appropriate management for this patient?
Explanation
Question 54
A 68-year-old woman presents with severe flatback deformity and sagittal imbalance following a prior lumbar fusion from L3 to S1. Her pelvic incidence (PI) is 55 degrees. Standing full-length radiographs reveal a current lumbar lordosis (LL) of 15 degrees and a sagittal vertical axis (SVA) of +12 cm. To achieve optimal sagittal balance, what should be the target postoperative lumbar lordosis?
Explanation
Question 55
A 22-year-old restrained driver is involved in a high-speed motor vehicle collision. Radiographs and CT of the thoracolumbar spine demonstrate a flexion-distraction injury (Chance fracture) through the L2 vertebral body and posterior elements. Which of the following associated injuries must be highly suspected?
Explanation
Question 56
A 15-year-old male with a history of back pain presents with bilateral lower extremity radicular pain. Radiographs reveal a Grade IV isthmic spondylolisthesis at L5-S1. During surgical reduction and fusion, the patient is at highest risk for iatrogenic injury to which of the following nerve roots?
Explanation
Question 57
A 60-year-old woman with a 20-year history of severe rheumatoid arthritis presents with neck pain and progressive clumsiness in her hands. Which of the following radiographic parameters is the most reliable predictor of impending neurologic compromise and paralysis?
Explanation
Question 58
A 55-year-old man undergoes a complex 10-level posterior spinal fusion for adult spinal deformity. The surgery lasts 11 hours with an estimated blood loss of 3.5 liters. On postoperative day 1, he complains of painless, profound bilateral vision loss. Pupillary reflexes are sluggish. What is the most likely etiology of this complication?
Explanation
Question 59
A 16-year-old boy presents with severe, progressive right-sided back pain that is worse at night and dramatically relieved by ibuprofen. Examination reveals a left-sided thoracic scoliosis. CT scan shows a 1 cm sclerotic lesion with a central lucent nidus in the right T8 pedicle. Which of the following best describes the relationship between the lesion and the scoliotic curve?
Explanation
Question 60
A 62-year-old man presents with dull, aching sacral pain and recent onset of bowel/bladder dysfunction. MRI demonstrates a large, destructive midline sacral mass. Biopsy reveals physaliferous cells with abundant vacuolated cytoplasm. What is the most appropriate definitive management?
Explanation
Question 61
A 28-year-old man falls from a height and sustains a Type II odontoid fracture. The fracture line slopes from anterior-inferior to posterior-superior. Intact transverse ligament is noted on MRI. Which of the following makes this patient a poor candidate for an anterior odontoid screw?
Explanation
Question 62
A 45-year-old man with acute severe low back pain and bilateral sciatica presents to the emergency department. He reports difficulty urinating. Which of the following post-void residual (PVR) bladder volumes is most indicative of cauda equina syndrome?
Explanation
Question 63
A 15-year-old boy presents with progressive mid-back pain and a rounded posture. Lateral radiographs of the thoracic spine demonstrate anterior wedging of T7, T8, and T9. According to Sorensen's criteria for classic Scheuermann's kyphosis, what is the minimum degree of anterior wedging required in these consecutive vertebrae?
Explanation
Question 64
A surgeon is planning a corrective osteotomy for a 60-year-old man with severe fixed sagittal imbalance. The surgeon decides to perform a pedicle subtraction osteotomy (PSO) at L3. Approximately how many degrees of sagittal correction can realistically be expected from a single-level lumbar PSO?
Explanation
Question 65
A 16-year-old girl undergoes a posterior spinal fusion from T4 to L3 for adolescent idiopathic scoliosis (Lenke 1A). On postoperative day 4, she develops severe bilious emesis, abdominal distension, and weight loss. Upright abdominal films show a dilated stomach and proximal duodenum with abrupt cutoff. What is the anatomic mechanism of this complication?
Explanation
Question 66
A 4-year-old girl is diagnosed with Klippel-Feil syndrome. She exhibits a low posterior hairline, short neck, and limited cervical range of motion. Because of known systemic associations with this syndrome, which of the following screening tests is most highly recommended?
Explanation
Question 67
A 50-year-old man presents with left arm pain radiating to his thumb and index finger. Examination demonstrates weakness in wrist extension and a diminished brachioradialis reflex. Which cervical nerve root is most likely compressed?
Explanation
Question 68
A 75-year-old woman presents with severe back pain 3 months after a mechanical fall. Radiographs reveal a T12 vertebral compression fracture with a distinct radiolucent shadow within the vertebral body (intravertebral vacuum cleft). What is the underlying pathophysiology of this specific radiographic sign?
Explanation
Question 69
A 3-year-old boy is evaluated for congenital scoliosis. Radiographs demonstrate a unilateral unsegmented bar on the left spanning T5 to T8, with a contralateral fully segmented hemivertebra at T6. What is the natural history of this specific spinal anomaly if left untreated?
Explanation
Question 70
A 16-year-old male gymnast complains of insidious onset, mechanical lower back pain. Radiographs are normal. A T2-weighted STIR MRI of the lumbar spine reveals bilateral high signal intensity in the L5 pars interarticularis. There is no spondylolisthesis. What is the most appropriate initial management?
Explanation
Question 71
A 40-year-old woman undergoes an anterior cervical discectomy and fusion (ACDF) for C5-C6 spondylosis. Postoperatively, she is noted to have a new-onset unilateral vocal cord paralysis and a hoarse voice. Injury to the recurrent laryngeal nerve is suspected. Which surgical approach and anatomical relationship most likely contributed to this injury?
Explanation
Question 72
A 65-year-old woman with adult spinal deformity is planning for surgery. Her pelvic incidence (PI) is 60 degrees. To minimize the risk of adjacent segment disease and mechanical failure, her postoperative lumbar lordosis (LL) should be targeted closest to what value?
Explanation
Question 73
A 58-year-old man undergoes a C3-C6 cervical laminectomy and posterior spinal fusion for cervical spondylotic myelopathy. On postoperative day 2, he develops profound weakness in bilateral shoulder abduction and elbow flexion, with no sensory changes. What is the most likely etiology of this new deficit?
Explanation
Question 74
A newborn is noted to have a congenital hemivertebra at T8 causing early scoliotic deformity. Which of the following screening tests is most critical in the initial workup of this patient to rule out associated anomalies?
Explanation
Question 75
A 6-year-old boy undergoes a posterior spinal fusion without anterior fusion for a severe progressing thoracic scoliosis. Over the next four years, he develops progressive rotational deformity and lordosis despite a solid posterior fusion mass. What is the primary cause of this phenomenon?
Explanation
Question 76
A 35-year-old woman falls from a height and sustains a T12 burst fracture. She is neurologically intact. MRI demonstrates an intact posterior ligamentous complex (PLC). According to the Thoracolumbar Injury Classification and Severity (TLICS) score, what is her total score and the recommended management?
Explanation
Question 77
A 15-year-old boy presents with progressive back pain and a prominent thoracic kyphosis. Standing lateral radiographs reveal anterior wedging of multiple consecutive thoracic vertebrae. According to Sorensen's criteria, what is the strict radiographic definition of classic Scheuermann's disease?
Explanation
Question 78
An 82-year-old man sustains a Type II odontoid fracture after a ground-level fall. He is neurologically intact. Radiographs show a 3 mm posterior displacement. He has severe medical comorbidities (ASA IV). What is the most appropriate management?
Explanation
Question 79
A 60-year-old man with a 20-year history of ankylosing spondylitis presents to the ED after a minor rear-end motor vehicle collision. He complains of severe lower cervical pain. Plain radiographs show marked osteopenia and bridging syndesmophytes, but no obvious fracture. What is the most appropriate next step?
Explanation
Question 80
A 14-year-old non-ambulatory boy with spastic quadriplegic cerebral palsy presents with progressive scoliosis. His Cobb angle is 85 degrees and he has 30 degrees of pelvic obliquity causing severe seating difficulties and ischial skin breakdown. When planning posterior spinal fusion, what is the most appropriate distal extent of fixation?
Explanation
Question 81
A 16-year-old female gymnast complains of mechanical low back pain for 6 months. Imaging reveals a bilateral L5 pars defect with a Grade I anterior slip of L5 on S1. Conservative treatment has failed. Which of the following pelvic parameters is the strongest predictor for progression of the spondylolisthesis?
Explanation
Question 82
When applying a halo vest orthosis, placing the anterior pins 1 cm superior to the orbital rim and lateral to the supraorbital notch specifically avoids injury to which of the following structures?
Explanation
Question 83
A 45-year-old man presents with acute onset of severe low back pain, bilateral sciatica, saddle anesthesia, and urinary retention with overflow incontinence. MRI reveals a massive L4-L5 herniated disc. To maximize the chance of full neurologic recovery, surgical decompression should ideally be performed within what timeframe from the onset of autonomic symptoms?
Explanation
Question 84
A 55-year-old man with a history of renal cell carcinoma presents with progressive paraparesis. MRI shows a destructive lesion in the T8 vertebral body causing severe spinal cord compression. The tumor is highly vascular and radioresistant. Which of the following is the most appropriate surgical approach?
Explanation
Question 85
A 40-year-old intravenous drug user presents with T10-T11 discitis and a small ventral epidural abscess. He is neurologically completely intact. Blood cultures are positive for Methicillin-sensitive Staphylococcus aureus (MSSA). What is the standard initial management?
Explanation
Question 86
A 12-year-old girl with adolescent idiopathic scoliosis has a 35-degree right thoracic curve. Her Risser stage is 1. Her menarche occurred 2 months ago. What is the most appropriate management?
Explanation
Question 87
A 50-year-old woman requires surgical decompression for a large, central, calcified T8-T9 disc herniation causing severe myelopathy. Which of the following surgical approaches is CONTRAINDICATED due to an unacceptably high risk of iatrogenic spinal cord injury?
Explanation
None
