Orthopedic Surgery Board Review MCQs: Ankle & Trauma Fractures - Part 95
Key Takeaway
This interactive quiz offers 50 high-yield Orthopedic Surgery MCQs for surgeons and residents. Modeled on OITE/AAOS exams, it provides detailed explanations and flexible study modes. Essential for comprehensive preparation and successful AAOS/ABOS board certification.
Orthopedic Surgery Board Review MCQs: Ankle & Trauma Fractures - Part 95
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 45-year-old female presents with a closed trimalleolar ankle fracture. A preoperative CT scan demonstrates a posterior malleolus fracture with a large posteromedial fragment extending to the medial malleolus, consistent with a Haraguchi Type II fracture.
Which of the following surgical approaches provides the most optimal visualization and access for rigid internal fixation of this specific posterior malleolar fracture pattern?
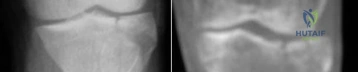
Explanation
Question 2
A 65-year-old male with poorly controlled type 2 diabetes mellitus and peripheral neuropathy sustains a displaced bimalleolar equivalent ankle fracture. He undergoes open reduction and internal fixation (ORIF). Which of the following postoperative regimens or fixation strategies is considered the standard of care to minimize complications in this specific patient population?
Explanation
Question 3
During surgical exploration of an unstable ankle fracture, the surgeon identifies an avulsion fracture of the anterior inferior tibiofibular ligament (AITFL) from its fibular attachment. This specific osseous fragment is known as:
Explanation
Question 4
A 38-year-old construction worker falls from scaffolding, sustaining a high-energy closed pilon fracture (AO/OTA 43-C3) with massive soft tissue swelling, hemorrhagic fracture blisters, and shortening of the limb. What is the most appropriate initial management?
Explanation
Question 5
A 30-year-old male sustains a twisting injury to his right ankle. In the emergency department, plain radiographs show a severely displaced fracture-dislocation. Attempts at closed reduction under conscious sedation are repeatedly unsuccessful due to a mechanical block. A Bosworth fracture-dislocation is suspected. What is the anatomic block to reduction in this injury?
Explanation
Question 6
A 22-year-old female presents with an ankle injury after a fall during a soccer match. Radiographs demonstrate a short oblique fracture of the lateral malleolus starting at the level of the syndesmosis and extending proximally and posteriorly. Additionally, the medial clear space is widened to 6 mm on the gravity stress view. According to the Lauge-Hansen classification, what stage of injury does this represent?
Explanation
Question 7
A 25-year-old male is involved in a high-speed motor vehicle collision and sustains a talar neck fracture. Radiographs and a subsequent CT scan confirm a completely displaced talar neck fracture with dislocation of both the subtalar and tibiotalar joints. The talonavicular joint remains reduced. According to the Hawkins classification, what type of fracture is this, and what is the approximate historical rate of avascular necrosis (AVN) associated with it?
Explanation
Question 8
An orthopedic surgeon is utilizing an extensile lateral approach for open reduction and internal fixation of a displaced intra-articular calcaneus fracture.
To minimize the risk of apex wound necrosis, the full-thickness flap must be elevated in a 'no-touch' subperiosteal plane. Which of the following vascular structures provides the primary blood supply to the apex of this flap?
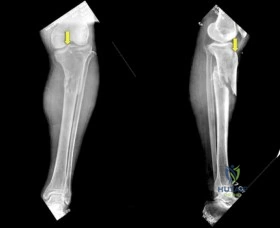
Explanation
Question 9
A 24-year-old athlete reports midfoot pain after an axial load on a plantarflexed foot. Weight-bearing radiographs of the foot appear largely normal, but a close inspection reveals a small bony fragment in the first intermetatarsal space, known as the 'fleck sign.' This sign represents an avulsion from which of the following structures?
Explanation
Question 10
A 28-year-old male presents with isolated medial ankle pain and swelling after an inversion and rotational injury. Radiographs show a transverse fracture of the medial malleolus and widening of the tibiofibular clear space. A full-length tibia-fibula radiograph reveals a fracture of the proximal third of the fibula. What is the most likely Lauge-Hansen mechanism for this specific injury pattern (Maisonneuve fracture)?
Explanation
Question 11
An 82-year-old female with severe osteoporosis, dementia, and compromised soft tissues presents with a highly unstable bimalleolar ankle fracture. Given her inability to comply with non-weight-bearing restrictions, the surgeon elects to perform a primary tibiotalocalcaneal (TTC) nailing. Which of the following is the most significant advantage of this approach in this specific patient compared to traditional ORIF?
Explanation
Question 12
During open reduction and internal fixation of a Weber B ankle fracture, the surgeon must intraoperatively assess the integrity of the syndesmosis. Under live fluoroscopy, which of the following stress tests is the most reliable and sensitive for demonstrating latent syndesmotic instability?
Explanation
Question 13
A 21-year-old snowboarder presents with chronic lateral ankle pain 6 weeks after a hard landing. He was initially diagnosed with an 'ankle sprain' at an urgent care. He has localized tenderness just inferior to the tip of the lateral malleolus. An occult fracture is suspected. What specific anatomical structure is most likely fractured in this 'snowboarder's fracture'?
Explanation
Question 14
A 35-year-old male falls from a height of 10 feet, landing on a plantarflexed foot. Radiographs reveal a comminuted compression fracture of the cuboid with notable shortening of the lateral column of the foot (the 'nutcracker' fracture). What is the primary surgical objective when treating this injury?
Explanation
Question 15
A surgeon is performing an anterolateral approach to the distal tibia for fixation of a complex pilon fracture. During the superficial dissection, the surgeon creates an internervous interval. Which nerve is at greatest risk of iatrogenic injury as it crosses the operative field from medial to lateral over the distal fibula/ankle joint?
Explanation
Question 16
A 20-year-old collegiate basketball player complains of acute lateral foot pain after cutting during a game. Radiographs demonstrate a non-displaced transverse fracture at the metaphyseal-diaphyseal junction of the fifth metatarsal, extending into the fourth-fifth intermetatarsal facet. What is the most appropriate management for this elite athlete to ensure the fastest reliable return to play?
Explanation
Question 17
A 35-year-old male sustains a severe ankle injury following an axial load on a neutral foot. Radiographs show vertical migration of the talus driving apart the tibia and fibula, severely disrupting the syndesmosis without significant medial or lateral malleolar fractures. This specific high-energy injury pattern is colloquially known as:
Explanation
Question 18
A 14-year-old male complains of right ankle pain after a skateboarding fall. Radiographs reveal a Salter-Harris III fracture of the anterolateral aspect of the distal tibia.
This specific fracture (juvenile Tillaux) is possible due to the asymmetric closure pattern of the distal tibial physis. What is the predictable chronological sequence of this physeal closure?

Explanation
Question 19
According to the Lauge-Hansen classification, an ankle fracture characterized by a transverse fracture of the medial malleolus, rupture of the syndesmosis, and a comminuted or short oblique 'bending' fracture of the fibula above the level of the joint line is produced by which mechanism?
Explanation
Question 20
A 28-year-old male presents with a highly comminuted, displaced coronal shear fracture of the talar body. Open reduction and internal fixation are required. To achieve perpendicular visualization and adequate access for hardware placement on the medial aspect of the talar dome and body, which of the following approaches or osteotomies is most frequently utilized?
Explanation
Question 21
A 35-year-old male presents after an ankle injury. Radiographs show a fracture-dislocation of the ankle. Closed reduction in the ED is unsuccessful. The lateral radiograph demonstrates the proximal fibular fragment trapped posterior to the posterior tubercle of the distal tibia.
Which of the following is the most appropriate next step in management?
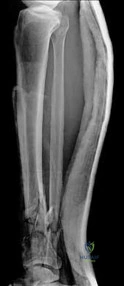
Explanation
Question 22
A 42-year-old male sustains a high-energy closed pilon fracture (AO/OTA 43-C3). An ankle-spanning external fixator is applied on the day of injury.
What is the most reliable clinical indicator that the soft tissue envelope is ready for definitive open reduction and internal fixation (ORIF)?

Explanation
Question 23
A 28-year-old female is 8 weeks status post ORIF of a Hawkins Type II talar neck fracture. A radiograph reveals a subchondral radiolucent band in the talar dome.
What is the prognostic significance of this radiographic finding?

Explanation
Question 24
A 14-year-old male presents with lateral ankle pain after a twisting injury playing soccer. Radiographs and a subsequent CT scan demonstrate a displaced Salter-Harris III fracture of the anterolateral aspect of the distal tibial epiphysis. What is the primary deforming force responsible for this specific fracture pattern?
Explanation
Question 25
A 13-year-old female sustains a triplane ankle fracture.
Which of the following best describes the classical anatomical planes of injury in the three parts of this fracture?

Explanation
Question 26
A 24-year-old male presents with persistent lateral ankle pain 3 weeks after a snowboarding accident. Initial plain radiographs were reported as negative for fracture. Clinical examination reveals tenderness inferior and anterior to the lateral malleolus. Which of the following injuries is most likely present and best diagnosed with a CT scan?
Explanation
Question 27
A 38-year-old male undergoes ORIF of a displaced intra-articular calcaneus fracture via an extensile lateral approach.
Postoperatively, the patient reports numbness over the lateral aspect of the foot and lateral heel. Which nerve is most likely at risk during the distal extension of this surgical approach?

Explanation
Question 28
A 45-year-old manual laborer sustains a purely ligamentous Lisfranc injury involving the 1st, 2nd, and 3rd tarsometatarsal joints. Which of the following statements regarding the definitive surgical management is most supported by current orthopedic literature?
Explanation
Question 29
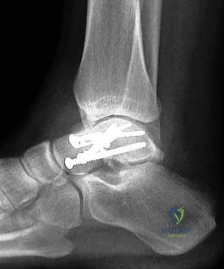
A 50-year-old female presents with chronic ankle pain following a conservatively managed bimalleolar ankle fracture 1 year ago. Radiographs demonstrate a malunion.
Which radiographic parameter is most sensitive for detecting fibular shortening in a malunited ankle fracture?
Explanation
Question 30
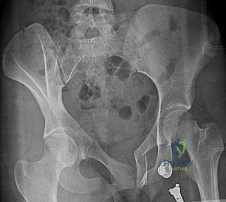
A 22-year-old elite collegiate basketball player sustains a fracture at the base of the fifth metatarsal. Radiographs show a transverse fracture extending into the intermetatarsal articulation (between the 4th and 5th metatarsals).
What is the recommended treatment to minimize the risk of nonunion and expedite return to play in this athlete?
Explanation
Question 31
A 30-year-old male is brought to the emergency department after a motor vehicle collision. He has severe midfoot swelling and deformity. Radiographs confirm a dorsal dislocation of the navicular from the talus and the cuboid from the calcaneus, without fracture. What is this specific injury pattern known as?
Explanation
Question 32
A horseback rider sustains a crush injury to the foot when her horse falls on her. She presents with lateral column foot pain. Radiographs reveal a comminuted fracture of the cuboid with shortening of the lateral column of the foot.
What is the classic mechanism of injury for this "nutcracker" fracture?

Explanation
Question 33
A 27-year-old female presents with ankle pain after an external rotation injury. Ankle radiographs show a widened medial clear space and disruption of the distal tibiofibular syndesmosis, but no lateral malleolus fracture is visible. What is the most critical next step in radiographic evaluation?
Explanation
Question 34
When placing a syndesmotic screw for a confirmed distal tibiofibular syndesmosis injury, which of the following describes the most widely accepted mechanical principles for fixation?
Explanation
Question 35
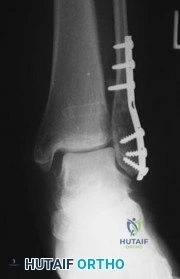
A 40-year-old male falls from a height and sustains a severely displaced comminuted fracture of the talar body. Surgical planning dictates that extensive exposure of the medial and central aspects of the talar dome is required for anatomical reduction.
Which surgical approach provides the most optimal visualization for this injury?
Explanation
Question 36
In the setting of a trimalleolar ankle fracture, recent literature emphasizes the importance of fixing the posterior malleolus. Which of the following is considered the primary biomechanical rationale for anatomical open reduction and internal fixation of the posterior malleolus, even for smaller fragments?
Explanation
Question 37
A 45-year-old male sustains an acute, closed, midsubstance Achilles tendon rupture. He is active but not a professional athlete. He is considering non-operative management with an early functional rehabilitation protocol versus surgical repair. Based on recent high-quality randomized controlled trials, what is the most accurate information regarding re-rupture rates?
Explanation
Question 38
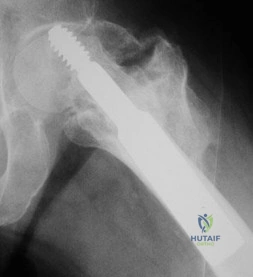
A 20-year-old track and field athlete presents with an insidious onset of vague midfoot pain. Radiographs are unremarkable, but a subsequent MRI reveals a stress fracture through the central third of the tarsal navicular.
Why is this specific anatomical location at a high risk for delayed union or nonunion?
Explanation
Question 39
A 55-year-old female presents to the emergency department after a slip and fall on ice. Her ankle is visibly deformed with the foot displaced laterally. The skin over the medial malleolus is severely blanched and tightly tented, but intact. What is the most urgent and appropriate next step?
Explanation
Question 40
In the management of severe (AO/OTA 43-C3) pilon fractures, the evolution from immediate internal fixation to a staged protocol (initial external fixation followed by delayed ORIF) was primarily driven by the unacceptably high rate of which specific complication?
Explanation
Question 41
A 45-year-old female sustains a rotational ankle fracture. Computed tomography demonstrates a posterior malleolus fragment. Based on recent biomechanical and clinical literature, what is considered the most critical indication for surgical fixation of the posterior malleolus?
Explanation
Question 42
A 38-year-old male presents with a comminuted distal tibia pilon fracture. The surgeon plans an anterolateral approach to the distal tibia. During this approach, which of the following nerves is at greatest risk of iatrogenic injury as it crosses the surgical field?
Explanation
Question 43
A 28-year-old male sustains a high-energy motor vehicle collision, resulting in a Hawkins Type III fracture of the talar neck. What is the approximate rate of avascular necrosis (AVN) of the talar body associated with this specific injury pattern?
Explanation
Question 44
A 24-year-old snowboarder presents with lateral ankle pain after a hard landing. Initial plain radiographs are unremarkable, but a subsequent CT scan reveals a displaced fracture of the lateral process of the talus.
Which of the following physical examination findings is most specific for this injury compared to a standard ankle sprain?

Explanation
Question 45
In the Sanders classification system for intra-articular calcaneus fractures, which specific imaging modality and view is primarily utilized to determine the classification?
Explanation
Question 46
A 42-year-old male sustains a severe ankle injury. Radiographs show a fracture-dislocation with the fibula resting posterior to the tibia. Closed reduction in the emergency department is unsuccessful. In this classic Bosworth fracture-dislocation, which anatomical structure typically entraps the proximal fibular fragment?
Explanation
Question 47
A 14-year-old boy falls while skateboarding and sustains a Salter-Harris III fracture of the anterolateral aspect of the distal tibia. Which specific ligament is responsible for the avulsion force creating this fracture fragment?
Explanation
Question 48
A 30-year-old male presents with severe midfoot swelling and pain following a motorcycle accident. Radiographs reveal a dislocation involving the talonavicular and calcaneocuboid articulations. What is the standard eponym used to describe this specific joint complex?
Explanation
Question 49
Following a severe crush injury to the foot from heavy machinery, a patient develops excruciating pain out of proportion to the injury, pain with passive toe stretch, and tense swelling. You suspect compartment syndrome. How many anatomically distinct fascial compartments are recognized in the foot for the purposes of surgical fasciotomy?
Explanation
Question 50
A 55-year-old female sustains an isolated medial malleolus fracture. In deciding between tension band wiring and lag screw fixation, which of the following scenarios represents the clearest advantage for utilizing a tension band construct?
Explanation
Question 51
A 33-year-old equestrian falls, and her foot is forcefully abducted while caught in the stirrup. She sustains a highly comminuted 'nutcracker' fracture of the cuboid. This specific fracture pattern occurs secondary to severe compression between which two bones?
Explanation
Question 52
A 62-year-old male with long-standing, poorly controlled diabetes and profound peripheral neuropathy sustains a bimalleolar ankle fracture. Which of the following modifications to standard surgical fixation and postoperative care is recommended to minimize the risk of hardware failure and Charcot arthropathy?
Explanation
Question 53
When performing an extensile lateral approach for the open reduction and internal fixation of a displaced intra-articular calcaneus fracture, the incision is made in an 'L' shape. Which nerve is at greatest risk of transection if the horizontal limb of the incision is carried too far anteriorly or placed too dorsally?
Explanation
Question 54
A 29-year-old male sustains a supination-external rotation ankle injury. Non-weight-bearing radiographs demonstrate an isolated, minimally displaced trans-syndesmotic fracture of the distal fibula (Weber B). The medial clear space measures 3 mm.
What is the most appropriate next step to assess the integrity of the deep deltoid ligament and rule out a bimalleolar equivalent injury?

Explanation
Question 55
A 35-year-old construction worker sustains a Gustilo-Anderson Type II open ankle fracture. Based on current literature and major trauma guidelines, what is the single most critical factor in reducing the risk of subsequent deep infection?
Explanation
Question 56
A 21-year-old elite collegiate basketball player sustains an acute fracture at the metaphyseal-diaphyseal junction of the fifth metatarsal during practice. He wishes to return to competitive play as quickly and safely as possible. What is the evidence-based recommended treatment?
Explanation
Question 57
A 25-year-old marathon runner presents with a 4-week history of vague, progressively worsening dorsal midfoot pain. Initial radiographs are negative, but an MRI demonstrates a stress fracture strictly localized to the central third of the navicular body. The characteristically high risk of delayed union or nonunion in this specific region is anatomically due to:
Explanation
Question 58
A 68-year-old female with osteoporosis misjudges a curb step and feels a sudden 'pop' in her posterior heel. Radiographs reveal a large 'beak' type avulsion fracture of the superior calcaneal tuberosity, displaced proximally by 4 cm.
On examination, the skin overlying the posterior heel is visibly blanched and tense. What is the most appropriate management?

Explanation
Question 59
A 40-year-old male underwent open reduction and internal fixation of a severe rotational ankle fracture. The syndesmosis was stabilized utilizing a single 3.5 mm cortical screw placed across four cortices. At 3 months post-operatively, he is asymptomatic, but radiographs show the syndesmotic screw has fractured within the clear space. What is the current consensus regarding the management of this finding?
Explanation
Question 60
The posterior process of the talus is anatomically divided into a medial tubercle and a lateral tubercle, separated by a distinct fibro-osseous groove. Which of the following tendons traverses this groove and may become symptomatic in cases of a lateral tubercle fracture (Shepherd's fracture) or a symptomatic os trigonum?
Explanation
Question 61
A 42-year-old female undergoes fixation of a posterior malleolus fracture via a posterolateral approach.
Which of the following describes the correct internervous/intermuscular interval for this approach?

Explanation
Question 62
Following reduction and screw fixation of a syndesmotic injury in a pronation-external rotation (PER) ankle fracture, the surgeon is concerned about malreduction. Which of the following modalities is the most sensitive and specific for detecting syndesmotic malreduction postoperatively?
Explanation
Question 63
A 30-year-old male presents with a severely deformed ankle following a fall. Radiographs demonstrate a fracture of the fibula with the proximal fibular fragment displaced posterior to the posterior tubercle of the distal tibia. Closed reduction in the emergency department is unsuccessful. What is the most likely anatomic block to reduction?
Explanation
Question 64
Recent biomechanical and clinical studies regarding the fixation of the posterior malleolus in trimalleolar ankle fractures have shifted the paradigm away from solely using fragment size (>25%) as the primary indication for fixation. What is the primary biomechanical advantage of directly fixing the posterior malleolus?
Explanation
Question 65
A 45-year-old female sustains a Supination-External Rotation (SER) stage IV ankle injury. Radiographs show a trans-syndesmotic fibula fracture. A gravity stress view shows a medial clear space of 6 mm. Which specific component of the medial ligamentous complex must be disrupted to allow this lateral talar shift?
Explanation
Question 66
A 72-year-old female with severe, poorly controlled diabetes mellitus, profound peripheral neuropathy, and a BMI of 38 presents with a closed, highly comminuted unstable ankle fracture. The soft tissues are significantly compromised. Which of the following surgical options offers the most rigid construct and lowest risk of soft tissue failure in this specific high-risk patient?
Explanation
Question 67
A 14-year-old boy presents with an ankle injury after a skateboarding accident. Radiographs reveal a Salter-Harris type III fracture of the anterolateral aspect of the distal tibia epiphysis. Which of the following ligaments is responsible for this avulsion injury?
Explanation
Question 68
According to the Lauge-Hansen classification, what is the correct sequential order of structural failure in a Supination-External Rotation (SER) ankle fracture?
Explanation
Question 69
A 32-year-old male sustains a severe ankle injury. Closed reduction in the emergency department is unsuccessful. Radiographs demonstrate a fracture-dislocation where the proximal fibular fragment is displaced posterior to the posterior tubercle of the distal tibia. Which of the following is the most appropriate management?
Explanation
Question 70
When utilizing the posterolateral approach to the ankle for fixation of a posterior malleolus fracture, the surgical interval is developed between which of the following muscle bellies?
Explanation
Question 71
A 28-year-old female presents with an ankle fracture following an inversion injury. Radiographs reveal a transverse fracture of the distal fibula below the level of the syndesmosis and a vertical fracture of the medial malleolus. What is the most biomechanically sound fixation strategy for the medial malleolus in this injury pattern?
Explanation
Question 72
Following open reduction and internal fixation of a severe pronation-external rotation (PER) ankle fracture with syndesmotic instability, which imaging modality is considered the gold standard for evaluating the accuracy of syndesmotic reduction?
Explanation
Question 73
A surgeon chooses to use a posterolateral anti-glide plate for a Danis-Weber type B lateral malleolus fracture. While biomechanically superior to lateral plating, this technique is most commonly associated with which of the following complications?
Explanation
Question 74
A 72-year-old male with severe peripheral neuropathy and a history of Charcot arthropathy presents with an acute, closed, highly unstable bimalleolar ankle fracture. The soft tissues are significantly compromised. To minimize catastrophic failure and soft tissue complications, what is the most appropriate definitive surgical intervention?
Explanation
Question 75
During pre-operative planning for an ankle fracture, a CT scan reveals a large avulsion fracture of the posterolateral aspect of the distal tibia. This specific fragment, which serves as the attachment site for the posterior inferior tibiofibular ligament (PITFL), is eponymously referred to as:
Explanation
None
