Orthopedic Board Review MCQs: Fracture, Dislocation & Nerve | Part 93
Key Takeaway
This page offers Part 93 of a comprehensive orthopedic surgery board review. Featuring 50 high-yield MCQs, it's designed for orthopedic residents and surgeons preparing for OITE and AAOS certification exams. Enhance your knowledge across key topics like fracture, hip, and elbow with detailed explanations and literature references in both study and exam modes.
Orthopedic Board Review MCQs: Fracture, Dislocation & Nerve | Part 93
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
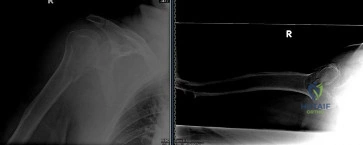
A 35-year-old man sustains a closed spiral fracture of the distal third of the humeral shaft (Holstein-Lewis type). On examination in the emergency department, he is unable to extend his wrist or fingers, but triceps function is completely intact.
What is the most appropriate initial management of this nerve injury?
Explanation
Question 2
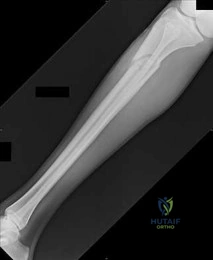
A 24-year-old athlete sustains an anterior shoulder dislocation during a rugby tackle.
After successful closed reduction, he is noted to have decreased sensation over the lateral aspect of his deltoid. Which of the following physical examination findings is most specifically associated with this nerve injury?
Explanation
Question 3
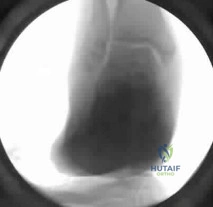
A 6-year-old boy presents with a completely displaced extension-type supracondylar fracture of the humerus.
Which of the following clinical deficits represents the most common nerve injury associated with this specific fracture pattern?
Explanation
Question 4
A 7-year-old girl falls on an outstretched hand and sustains a Bado Type I Monteggia fracture-dislocation.
She is noted to have a nerve palsy on presentation. What is the expected clinical presentation of her neurological deficit?
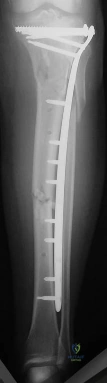
Explanation
Question 5
A 28-year-old male is involved in a high-speed motor vehicle collision and sustains a severe traumatic knee dislocation resulting in a complete foot drop.
Given the mechanism and neurological deficit, which adjacent vascular structure is most critically at risk and requires emergent evaluation?
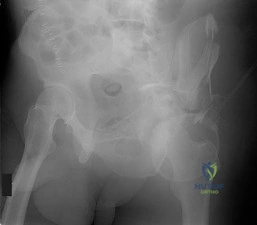
Explanation
Question 6
A 45-year-old man falls from a roof, sustaining a Zone 3 sacral fracture according to the Denis classification.
Which of the following neurological deficits is most commonly associated with this specific fracture zone?
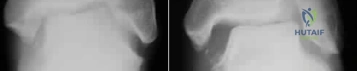
Explanation
Question 7
A 33-year-old unrestrained driver sustains a posterior wall acetabular fracture with a posterior hip dislocation.
On initial evaluation, the patient has weakness in ankle dorsiflexion and great toe extension, with completely intact ankle plantar flexion. Which nerve division is most likely injured?
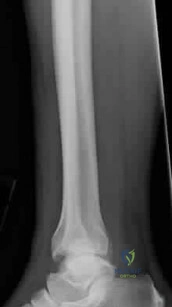
Explanation
Question 8
A 65-year-old female sustains a closed, displaced intra-articular distal humerus fracture (AO type 13-C3).
Preoperatively, she reports numbness and tingling in her ring and small fingers. What is the most appropriate intraoperative management of the ulnar nerve during open reduction and internal fixation (ORIF)?
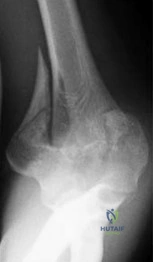
Explanation
Question 9
A 25-year-old male sustains an anteroposterior compression (APC) type III pelvic ring injury. He undergoes anterior plating of the symphysis pubis and percutaneous posterior sacroiliac (SI) joint screw fixation. Postoperatively, he is noted to have a foot drop and weakness in great toe extension, but sensation to the plantar aspect of the foot is intact. Which of the following nerve roots is most likely injured due to its precise anatomical relationship to the sacral ala?
Explanation
Question 10
A 19-year-old cyclist sustains a closed, highly displaced midshaft clavicle fracture that is treated nonoperatively. Several weeks later, he presents with new-onset progressive paresthesias in his medial forearm and hand, alongside weakness of intrinsic hand muscles.
Which of the following is the most likely cause of his neurological symptoms?

Explanation
Question 11
A 30-year-old soccer player sustains a twisting injury to the knee. Radiographs reveal an isolated, slightly displaced fracture of the fibular head. He exhibits a complete inability to dorsiflex his foot and has numbness over the entire dorsum of the foot, involving both the superficial and deep peroneal nerve territories. What is the typical mechanism of injury for the nerve in this specific scenario?
Explanation
Question 12
A 45-year-old man sustains a comminuted fracture of the scapular body that extends into the spinoglenoid notch.
If the nerve passing through this specific notch is entrapped by fracture callus, which of the following physical examination findings would be exclusively expected?
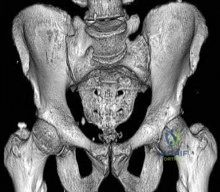
Explanation
Question 13
A 55-year-old female sustains a completely displaced, volarly angulated fracture of the distal radius (Smith fracture). In the emergency department, she complains of severe, progressively worsening burning pain in her hand and numbness in her thumb, index, and middle fingers. The pain is exacerbated by passive extension of her digits. What is the most appropriate immediate next step in management?
Explanation
Question 14
A 22-year-old man undergoes intramedullary nailing of a midshaft femur fracture on a fracture table.
The procedure takes 4 hours due to significant difficulty achieving a closed reduction. Postoperatively, he complains of numbness in his perineal region and presents with erectile dysfunction. What is the most likely cause of this complication?
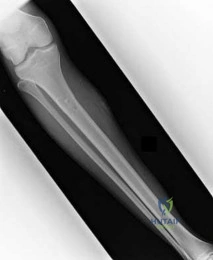
Explanation
Question 15
A 30-year-old construction worker drops a heavy steel beam on his midfoot, sustaining a severe Lisfranc fracture-dislocation.
In the emergency department, he complains of significant numbness over the dorsal aspect of the first web space of his foot. Which nerve is most likely compromised, and what is its anatomic course relative to the injury?
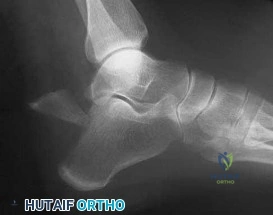
Explanation
Question 16
A 40-year-old male presents with a chronic anterior shoulder dislocation missed for 6 weeks. During open reduction and stabilization using a Latarjet procedure, the conjoint tendon is aggressively retracted medially to gain exposure to the glenoid. Postoperatively, the patient is unable to flex his elbow against resistance when the forearm is supinated and has sensory loss over the lateral forearm. Which nerve was most likely injured?
Explanation
Question 17
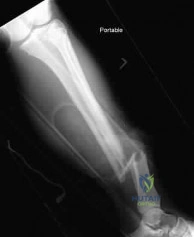
A 35-year-old man is struck by a car and sustains a Schatzker VI tibial plateau fracture.
He undergoes temporary spanning external fixation. Twelve hours later, he develops intractable leg pain out of proportion to his injury, severe pain with passive toe flexion, and decreased sensation in the first web space. His dorsalis pedis pulse remains palpable. Which of the following is the most accurate statement regarding his condition?
Explanation
Question 18
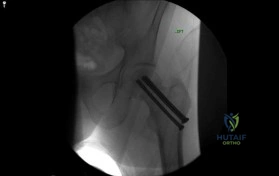
In a Holstein-Lewis fracture (a spiral fracture of the distal third of the humerus), the radial nerve is particularly vulnerable to entrapment or laceration.
At what specific anatomical location does the nerve typically become entrapped by the fracture fragments?
Explanation
Question 19
A 32-year-old male sustains a posterior hip dislocation. He presents with a foot drop but retains full strength in ankle plantar flexion and toe flexion. Why is the peroneal division of the sciatic nerve more frequently and severely injured than the tibial division in this clinical scenario?
Explanation
Question 20
A 45-year-old roofer falls from a ladder, sustaining a severely comminuted, depressed intra-articular calcaneus fracture. It is treated non-operatively due to severe patient comorbidities. Six months later, he complains of a burning, neuropathic pain in the plantar aspect of his foot and toes that worsens with weight-bearing. Tinel's sign is strongly positive just posterior to the medial malleolus. What anatomical structure forms the roof of the fibro-osseous tunnel causing the compression of the involved nerve?
Explanation
Question 21
An 18-year-old male sustains a closed distal third spiral humeral shaft fracture.
On physical examination, he is unable to actively extend his wrist or digits. What is the most appropriate initial management of this nerve palsy?

Explanation
Question 22
A 25-year-old male presents with an anterior shoulder dislocation following a rugby tackle. Post-reduction, he reports numbness over the lateral aspect of his shoulder. If this nerve injury persists, which muscle's function will most likely demonstrate profound weakness on subsequent examination?
Explanation
Question 23
A 6-year-old boy falls on an outstretched hand and sustains a Bado Type I Monteggia fracture-dislocation. On examination, he is unable to extend his thumb and digits at the metacarpophalangeal joints, but active wrist extension is preserved, accompanied by radial deviation. Which nerve is most likely injured?
Explanation
Question 24
A 5-year-old boy presents with a Gartland type III extension-type supracondylar humerus fracture. Which specific physical examination finding is the hallmark of the most common nerve injury associated with this fracture pattern?
Explanation
Question 25
A 30-year-old male sustains a high-energy traumatic knee dislocation.
Following reduction, he presents with a foot drop and numbness over the dorsum of the foot. Which specific ligamentous injury pattern is most highly associated with this neurologic deficit?

Explanation
Question 26
A 40-year-old female sustains a comminuted Denis Zone III sacral fracture after a fall from a height. Based on the anatomic location of this fracture, which of the following neurologic deficits is most frequently encountered?
Explanation
Question 27
A 28-year-old male is involved in a motor vehicle collision, sustaining a posterior wall acetabular fracture and a posterior hip dislocation.
Following a successful closed reduction, he demonstrates profound weakness in ankle dorsiflexion but preserved plantarflexion. Which division of the sciatic nerve is most commonly injured in this clinical scenario?

Explanation
Question 28
A 62-year-old female undergoes open reduction and internal fixation of a distal radius fracture using a standard Henry (volar) approach. Post-operatively, she is unable to actively flex the interphalangeal joint of her thumb. Which structure was most likely subjected to excessive retraction during the procedure?
Explanation
Question 29
A 35-year-old male sustains a severely displaced scapular fracture with a fracture line extending deep into the spinoglenoid notch. He complains of persistent shoulder weakness. Which specific physical examination finding is most characteristic of nerve entrapment at this anatomic location?
Explanation
Question 30
A 25-year-old male undergoes intramedullary nailing of a femoral shaft fracture on a fracture table utilizing a perineal post. Post-operatively, he complains of numbness in his perineum and erectile dysfunction. What is the most appropriate initial management?
Explanation
Question 31
A 68-year-old female sustains a 3-part proximal humerus fracture. Due to severe pain, comprehensive motor testing is difficult. What is the most sensitive and reliable physical examination maneuver to assess the integrity of the nerve most commonly injured in this setting?
Explanation
Question 32
A 45-year-old male sustains a pronation-external rotation (PER) ankle fracture with lateral dislocation. Post-reduction, he notes numbness on the dorsal aspect of the foot (sparing the first web space) and weakness in active foot eversion. Which nerve is involved?
Explanation
Question 33
A 10-year-old boy sustains a 'floating elbow' injury consisting of an ipsilateral displaced supracondylar humerus fracture and a both-bone forearm fracture. He is splinted in the emergency department. Two hours later, he develops severe, unrelenting pain in his forearm, and severe pain with passive extension of his fingers. What is the most appropriate NEXT step?
Explanation
Question 34
A 55-year-old female presents with a non-displaced distal radius fracture treated with a well-molded short arm cast. Two days later, she reports severe, progressively worsening numbness and tingling in her thumb, index, and middle fingers, as well as worsening pain. What is the most appropriate next step in management?
Explanation
Question 35
A 30-year-old man sustains a severe grade IIIA open midshaft humerus fracture resulting from a motorcycle crash. On initial presentation, he has an isolated radial nerve palsy. He is scheduled for urgent surgical debridement. What is the recommended management for the radial nerve during this procedure?
Explanation
Question 36
A 70-year-old female sustains a primary anterior shoulder dislocation. After a successful and atraumatic closed reduction, she demonstrates persistent, profound weakness in active external rotation and active shoulder abduction. However, sensation over the lateral deltoid remains completely intact. What is the most likely etiology of her weakness?
Explanation
Question 37
A 15-year-old gymnast sustains a medial epicondyle fracture that is displaced 15 mm into the joint, necessitating open reduction and internal fixation. During the surgical approach, the ulnar nerve is identified. According to current orthopedic literature, what is the most appropriate management of the ulnar nerve?
Explanation
Question 38
A 32-year-old male sustains a severe Hawkins type III talar neck fracture following a fall from height. Given the typical direction of displacement of the talar body in this specific fracture pattern, which neurovascular structure is at greatest risk of impingement or injury?
Explanation
Question 39
A collegiate football player sustains a direct blow to the lateral aspect of his knee, resulting in a fibular neck fracture and a subsequent complete foot drop due to common peroneal nerve injury. During his rehabilitation phase, return of function in which of the following muscles would serve as the earliest clinical indicator of nerve recovery?
Explanation
Question 40
A 45-year-old male patient with a historically malunited, highly displaced midshaft clavicle fracture presents with progressive upper extremity weakness, numbness, and tingling. Examination reveals intrinsic hand muscle wasting and sensory deficits along the medial aspect of the forearm and hand. Hypertrophic fracture callus is identified on imaging. Which nerve roots are most likely compressed in this form of Thoracic Outlet Syndrome?
Explanation
Question 41
A 26-year-old unrestrained driver is involved in a motor vehicle collision. He presents with his right hip flexed, adducted, and internally rotated. Following closed reduction of the hip, he is unable to dorsiflex his right foot or extend his toes, but plantar flexion is symmetric to the contralateral side. Which of the following best explains the specific pattern of this neurological deficit?
Explanation
Question 42
A 7-year-old girl falls from monkey bars and sustains a Bado Type III Monteggia fracture-dislocation. She exhibits a nerve palsy characterized by weakness in thumb and finger extension, but normal wrist extension with radial deviation. Which nerve is most likely injured?
Explanation
Question 43
A 34-year-old man sustains a Grade II open midshaft humerus fracture. On initial evaluation, he is unable to actively extend his wrist or fingers, and he has decreased sensation over the dorsal first web space. What is the most appropriate management of his nerve injury?
Explanation
Question 44
A 5-year-old boy presents with a displaced flexion-type supracondylar humerus fracture after falling directly onto a flexed elbow. Which of the following nerve injuries is most frequently associated with this specific fracture pattern?
Explanation
Question 45
A 45-year-old man is undergoing open reduction and internal fixation of a posterior wall acetabular fracture via a Kocher-Langenbeck approach. What intraoperative leg position is most critical to minimize iatrogenic tension on the sciatic nerve?
Explanation
Question 46
A 22-year-old football player sustains a high-energy Lisfranc injury with lateral displacement of the second through fifth metatarsals. If he develops a neurological deficit secondary to this injury, what physical examination finding is most likely?
Explanation
Question 47
A 48-year-old man presents with progressive numbness in his small and ring fingers, accompanied by intrinsic muscle wasting in his dominant hand. He reports having 'broken his elbow' as a young child. Radiographs reveal a severe cubitus valgus deformity. Nonunion of which of the following pediatric fractures is the most likely underlying cause?
Explanation
Question 48
A 29-year-old man falls on an outstretched hand. Lateral radiographs of his wrist show the lunate displaced volarly and 'spilled' from the radius, while the capitate remains aligned with the radius. He reports severe pain and numbness in his index and middle fingers. What is the most appropriate management?
Explanation
Question 49
A 31-year-old female sustains an anterior knee dislocation (KD-III) following a trampoline injury. Vascular exam is normal, but she has a complete foot drop and cannot actively extend her toes. Where is the most likely anatomic site of nerve tethering causing this injury?
Explanation
Question 50
A 28-year-old male sustains a posterior hip dislocation. Following successful closed reduction, he is noted to have a dense foot drop and absent sensation over the dorsal aspect of his foot. Which anatomic characteristic makes the primarily involved nerve division most susceptible to this specific injury?
Explanation
Question 51
A 7-year-old girl presents with a flexion-type supracondylar humerus fracture. Her hand is well-perfused, but she exhibits a specific neurologic deficit. Which nerve is most commonly injured in this specific fracture pattern?

Explanation
Question 52
A 22-year-old male sustains a traumatic knee dislocation (KD-III). Vascular examination is normal, but he exhibits a complete common peroneal nerve palsy. Assuming a closed injury with a grossly stable reduction, what is the most appropriate initial management of the nerve injury?
Explanation
Question 53
A 6-year-old child presents with a Bado Type III Monteggia fracture-dislocation. Following closed reduction, the patient cannot extend the fingers at the metacarpophalangeal joints but demonstrates normal wrist extension with radial deviation. What is the expected natural history of this neurologic deficit?
Explanation
Question 54
A 29-year-old male falls from a roof and sustains a dorsal perilunate dislocation. He presents with severe wrist pain, absent 2-point discrimination in the thumb and index finger, and weakness in thumb opposition. What is the most appropriate initial surgical management?
Explanation
Question 55
A 40-year-old male undergoes intramedullary nailing of a comminuted femoral shaft fracture utilizing a fracture table. Postoperatively, he complains of perineal numbness and erectile dysfunction. What is the most likely etiology of this complication?
Explanation
Question 56
A 35-year-old female sustains a U-type sacral fracture extending through the central sacral canal (Denis Zone III). Based on this specific fracture classification, she is most at risk for which of the following neurologic deficits?
Explanation
Question 57
A 45-year-old man is involved in a motor vehicle collision, sustaining a posterior hip dislocation and a posterior wall acetabular fracture. Following closed reduction, he is unable to dorsiflex his ankle or extend his great toe, though plantar flexion remains intact. Which division of the affected nerve is most likely injured, and what is its typical relative prognosis?
Explanation
Question 58
A 22-year-old male sustains a KD-III knee dislocation. Post-reduction, he exhibits completely absent ankle dorsiflexion and eversion. At 3 months follow-up, there is zero return of clinical function, and an EMG shows absent motor unit action potentials in the anterior compartment musculature. What is the most appropriate next step in management?
Explanation
Question 59
A 7-year-old girl falls and sustains a Bado Type III Monteggia fracture-dislocation. On examination, she is unable to actively extend the MCP joints of her fingers, but wrist extension is preserved with radial deviation. Which nerve structure is injured?
Explanation
Question 60
A 55-year-old female presents with a completely displaced fracture of the distal radius. After a closed reduction and splinting, she complains of rapidly escalating pain and progressive loss of two-point discrimination in her thumb, index, and long fingers within 2 hours. What is the definitive management?
Explanation
Question 61
A 30-year-old man sustains a closed mid-distal humeral shaft fracture. His initial neurologic examination in the trauma bay is entirely normal. Following an attempt at closed reduction and application of a coaptation splint, he is noted to have a complete loss of wrist and finger extension. What is the most appropriate management?
Explanation
Question 62
An 8-year-old boy presents to the emergency department with a flexion-type supracondylar humerus fracture. Which of the following nerve injuries is most frequently associated with this specific fracture configuration?
Explanation
Question 63
A 25-year-old male is involved in a severe crush injury resulting in a Denis Zone III sacral fracture. Which of the following neurologic deficits is most specifically characteristic of this injury pattern?
Explanation
Question 64
A 40-year-old motorcyclist presents after a high-speed crash with massive soft tissue swelling over the left shoulder. Radiographs demonstrate lateral displacement of the scapula, an intact but widened acromioclavicular joint, and a severely displaced clavicle fracture. Radial pulses are diminished. Which nerve injury is most common in this scenario?
Explanation
Question 65
A 35-year-old man sustains a lateral compression (LC-1) pelvic ring injury involving a significantly displaced fracture through the sacral ala. On physical examination, he demonstrates weakness in ankle dorsiflexion and great toe extension. Which nerve root is most likely compromised by this specific fracture?
Explanation
Question 66
A 65-year-old woman sustains a 3-part proximal humerus fracture. Her pain prevents any active shoulder movement. To accurately assess the function of the axillary nerve in this acute setting, which examination finding is most reliable?
Explanation
Question 67
A 28-year-old man falls on his outstretched hand. His wrist is diffusely swollen, and he holds his fingers in slight flexion. A lateral radiograph demonstrates the 'spilled teacup' sign. He reports severe, continuous numbness in his thumb, index, and middle fingers. What is the most appropriate initial management?
Explanation
Question 68
A 12-year-old boy sustains a traumatic elbow dislocation that is reduced in the emergency department. Post-reduction radiographs show widening of the medial joint space, and the medial epicondyle ossification center is completely absent from its normal anatomic position. He has new-onset numbness in his small finger. What is the most likely pathomechanism?
Explanation
Question 69
A 25-year-old man sustains a Grade II open fracture of the middle third of the humerus. On initial evaluation, he has an absent brachioradialis reflex and is entirely unable to extend his wrist or fingers. What is the standard of care for the nerve injury in this specific scenario?
Explanation
Question 70
A 45-year-old man is 6 months status post ORIF of a severe intra-articular calcaneus fracture. He complains of burning pain on the plantar aspect of his foot that worsens at night. He has a strongly positive Tinel's sign posterior to the medial malleolus. What is the most likely diagnosis?
Explanation
Question 71
A 22-year-old man sustains a low-velocity gunshot wound to the arm, resulting in a comminuted midshaft humerus fracture and a complete radial nerve palsy. Distal pulses are strong, and the limb is well-perfused. What is the most appropriate initial treatment strategy?
Explanation
Question 72
A 30-year-old man suffers a "floating knee" injury (ipsilateral femur and tibia fractures) in a rollover collision. Postoperatively, he exhibits a complete foot drop and absent two-point discrimination in the first dorsal web space. Which nerve was injured, and where is its most common site of traumatic tethering?
Explanation
Question 73
A 40-year-old man sustains a Pipkin IV fracture-dislocation of the hip with an immediate, profound sciatic nerve palsy. He is reduced and placed in skeletal traction. A post-reduction CT scan clearly demonstrates a large posterior wall fragment directly impinging upon the sciatic nerve. What is the next best step in management?
Explanation
None
