Orthopedic Board Review MCQs: Elbow, Shoulder & Trauma | Part 85
Key Takeaway
This page offers Part 85 of an interactive orthopedic surgery board review quiz. Featuring 50 high-yield MCQs in OITE/AAOS format, it targets orthopedic residents and surgeons preparing for their AAOS and ABOS board exams. Covering Elbow, Shoulder, Trauma, it ensures robust certification exam preparation.
Orthopedic Board Review MCQs: Elbow, Shoulder & Trauma | Part 85
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
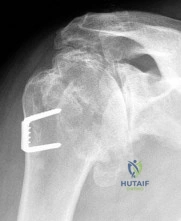
A 45-year-old female presents after a fall on an outstretched hand. Imaging reveals a terrible triad injury of the elbow.
During surgical intervention, what is the most widely accepted sequence of repair to restore elbow stability?
Explanation
Question 2
A 72-year-old male with severe rotator cuff tear arthropathy undergoes a reverse total shoulder arthroplasty (rTSA). How does the rTSA implant alter the biomechanics of the shoulder joint compared to the native anatomy?
Explanation
Question 3
A 35-year-old male suffers a distal biceps tendon rupture and undergoes surgical repair via a two-incision technique. Compared to the single anterior incision technique, the two-incision approach is associated with a higher risk of which of the following complications?
Explanation
Question 4
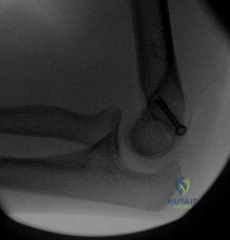
According to the criteria described by Hertel et al. for proximal humerus fractures, which of the following combinations of radiographic findings is most predictive of humeral head ischemia?
Explanation
Question 5
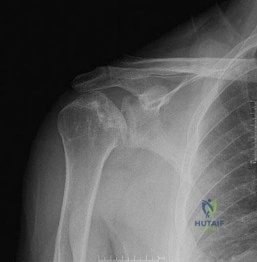
A 28-year-old polytrauma patient sustains an isolated, closed body and neck fracture of the scapula. According to current consensus guidelines, which of the following radiographic parameters is considered an absolute indication for Open Reduction and Internal Fixation (ORIF)?
Explanation
Question 6
A 19-year-old male sustains a midshaft clavicle fracture during a cycling accident. Which of the following factors most significantly increases the risk of nonunion if this injury is treated nonoperatively?
Explanation
Question 7
A 45-year-old male presents with a closed, spiral fracture of the distal third of the humerus (Holstein-Lewis fracture). On initial examination, the patient has normal radial nerve function. A coaptation splint is applied in the emergency department. Upon re-evaluation post-reduction, the patient is unable to extend his wrist or fingers and has numbness in the first dorsal web space. What is the most appropriate next step in management?
Explanation
Question 8
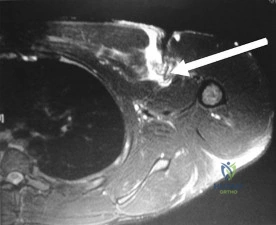
A 22-year-old collegiate rugby player presents with recurrent anterior shoulder instability. A 3D CT scan reveals 26% anterior glenoid bone loss.
What is the most appropriate surgical intervention to prevent further dislocations in this athlete?
Explanation
Question 9
During a physical examination of the shoulder, a patient is asked to place the palm of their hand on their opposite shoulder, with the elbow kept elevated. The examiner then applies a downward force to the patient's forearm while the patient resists. This test is highly specific for evaluating a tear of which structure?
Explanation
Question 10
A 6-year-old girl is brought to the emergency department after falling from monkey bars. Radiographs demonstrate an isolated fracture of the ulnar shaft with dorsal angulation and an associated posterior dislocation of the radial head. According to the Bado classification, what type of Monteggia lesion is this?
Explanation
Question 11
During the surgical repair of a chronic, complete rupture of the pectoralis major muscle, the surgeon must mobilize and anatomically repair the sternal and clavicular heads to their footprint on the humerus. What is the correct anatomical relationship of the clavicular head relative to the sternal head at their humeral insertion?
Explanation
Question 12
Historically, it was taught that the anterior circumflex humeral artery provides the primary blood supply to the humeral head via its arcuate branch. However, modern quantitative studies (e.g., Hettrich et al.) have demonstrated that the principal blood supply to the humeral head is actually provided by which vessel?
Explanation
Question 13
A 24-year-old male is evaluated for compartment syndrome following a high-energy tibia fracture.
Intracompartmental pressures are measured. According to standard trauma protocols, a four-compartment fasciotomy is indicated if the "Delta P" falls below what threshold?
Explanation
Question 14
A 68-year-old female with rheumatoid arthritis undergoes a primary total elbow arthroplasty (TEA) for severe joint destruction. She is educated post-operatively regarding lifelong activity modifications. Which of the following is the most commonly cited long-term mechanical complication of TEA?
Explanation
Question 15
A 27-year-old elite baseball pitcher presents with medial elbow pain during the late cocking and early acceleration phases of throwing. Clinical examination and MRI confirm an isolated tear of the anterior bundle of the ulnar collateral ligament (UCL). Which band of the anterior bundle is the primary restraint to valgus stress at 30 to 120 degrees of elbow flexion?
Explanation
Question 16
A 21-year-old male arrives at the trauma bay following an assault. He sustained a low-velocity gunshot wound to the right thigh. Radiographs reveal a closed, simple transverse midshaft femur fracture with the bullet retained in the posterolateral thigh musculature. The patient is hemodynamically stable with normal distal pulses. What is the standard of care for this injury?
Explanation
Question 17
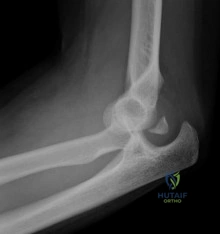
A 32-year-old male falls directly onto the point of his shoulder while snowboarding. Clinical exam reveals a prominent clavicle, and radiographs show the distal clavicle displaced posteriorly into the trapezius muscle.
According to the Rockwood classification of acromioclavicular (AC) joint injuries, what type of injury is this?
Explanation
Question 18
A 25-year-old professional volleyball player presents with insidious onset, painless weakness of the right shoulder. Physical examination reveals isolated atrophy of the infraspinatus fossa, with normal bulk of the supraspinatus. At which anatomic location is the nerve compression most likely occurring?
Explanation
Question 19
During a deltopectoral approach for an open reduction internal fixation (ORIF) of a proximal humerus fracture, the surgeon must be mindful of the axillary nerve. On average, at what distance distal to the lateral border of the acromion does the axillary nerve cross the deep surface of the deltoid?
Explanation
Question 20
A trauma patient presents with a pelvic ring injury after a motor vehicle collision. Radiographs and CT demonstrate a vertically oriented fracture through the sacrum and rami fractures on the same side. According to the Young-Burgess classification, which of the following injury mechanisms is most strongly associated with the highest volume of retroperitoneal hemorrhage requiring angioembolization?
Explanation
Question 21
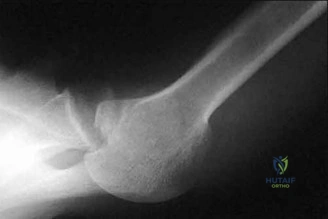
A 45-year-old male falls on an outstretched hand and sustains the injury shown in the radiograph.
During surgical reconstruction of this "terrible triad" of the elbow, the surgeon systematically addresses the structures. Following fixation of the coronoid process, management of the radial head, and repair of the lateral collateral ligament (LCL) complex, the elbow remains unstable in extension. What is the most appropriate next step in management?
Explanation
Question 22
A 60-year-old osteoporotic female sustains a highly comminuted, intra-articular distal humerus fracture.
You are planning open reduction and internal fixation (ORIF) with dual plating. Based on biomechanical studies comparing parallel versus orthogonal plate configurations for distal humerus fractures, which of the following statements is most accurate?

Explanation
Question 23
A 32-year-old male sustains a closed, oblique fracture of the distal third of the humeral shaft (Holstein-Lewis fracture). Upon examination in the emergency department, he is unable to extend his wrist or fingers, though his triceps function is intact. There is no open wound. What is the most appropriate initial management?
Explanation
Question 24
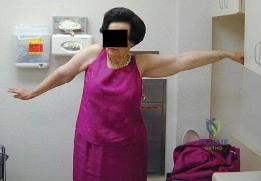
A 28-year-old professional weightlifter presents with a dull, aching pain in his right posterior shoulder and neck. On examination, there is pronounced lateral winging of the scapula, which is exacerbated during resisted external rotation and shoulder abduction. He recently had a minor lymph node biopsy in the posterior triangle of his neck. Injury to which of the following nerves is the most likely cause of his scapular winging?
Explanation
Question 25
A 40-year-old male undergoes a single-incision anterior approach for repair of a distal biceps tendon rupture. Postoperatively, he complains of numbness and tingling along the radial border of his forearm. Which of the following is the most likely etiology of this complication?
Explanation
Question 26
A 68-year-old female sustains a complex proximal humerus fracture.
According to Hertel's radiographic criteria, which combination of findings is the most reliable predictor of subsequent avascular necrosis (AVN) of the humeral head?

Explanation
Question 27
A 25-year-old mountain biker falls directly onto the point of his shoulder, sustaining an acute high-grade (Type V) acromioclavicular (AC) joint separation.
Surgical reconstruction of the coracoclavicular (CC) ligaments is planned. Biomechanically, which native structure acts as the primary restraint to superior translation of the distal clavicle?

Explanation
Question 28
A 35-year-old mechanic sustains an Essex-Lopresti injury after falling from a ladder. This injury pattern is characterized by a radial head fracture, disruption of the distal radioulnar joint (DRUJ), and tearing of the interosseous membrane (IOM). If the radial head is completely excised without replacement in this patient, what is the expected biomechanical consequence?
Explanation
Question 29
A 45-year-old male sustains a transverse fracture of the olecranon. The surgeon plans to use a tension band wiring technique. To maximize the biomechanical strength of the construct and minimize wire pullout, where should the K-wires be directed and seated?
Explanation
Question 30
A 22-year-old elite rugby player with recurrent anterior shoulder instability undergoes a Latarjet procedure due to 25% anterior glenoid bone loss. The procedure relies on a "triple blocking" effect. Which of the following provides the most significant contribution to the dynamic stability (the "sling effect") conferred by the Latarjet procedure when the arm is abducted and externally rotated?
Explanation
Question 31
A 50-year-old male is involved in a high-speed motor vehicle accident and sustains a closed fracture of the scapular neck.
According to the criteria described by Goss and Ada, what threshold of medial displacement (medialization) of the glenoid fragment relative to the lateral border of the scapula is widely considered an absolute indication for operative fixation?

Explanation
Question 32
A 38-year-old female falls onto an extended arm and presents with severe elbow pain. Radiographs and CT scan reveal a coronal shear fracture of the distal humerus. The fracture fragment includes the capitellum and the lateral half of the trochlea. According to the Bryan and Morrey classification with McKee's modification, what type of fracture is this?
Explanation
Question 33
A 65-year-old male with chronic kidney disease presents with posterior elbow pain and an inability to actively extend his elbow against gravity following a sudden eccentric load. Radiographs show a small "Fleck sign" avulsed from the proximal ulna. You diagnose a complete triceps tendon rupture and plan for surgical repair. What is the anatomic characteristic of the triceps insertion on the olecranon?
Explanation
Question 34
Which of the following variables is considered the STRONGEST independent predictor for the development of nonunion in a midshaft clavicle fracture treated non-operatively?
Explanation
Question 35
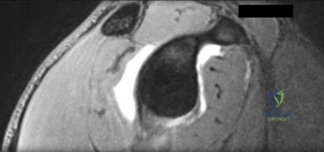
A 6-year-old boy presents to the emergency department after falling from monkey bars. Radiographs reveal a plastic deformation of the ulnar shaft and an anterior dislocation of the radial head. This corresponds to a Bado Type I Monteggia equivalent lesion.
What is the most appropriate initial management for this injury?
Explanation
Question 36
A 75-year-old female sustains a displaced 4-part proximal humerus fracture. Given her poor bone quality and fracture complexity, she undergoes a Reverse Total Shoulder Arthroplasty (RTSA). During the procedure, the tuberosities are repaired to the shaft and the prosthesis. Healing of which of the following structures is most strongly associated with improved external rotation and higher overall patient-reported functional outcome scores?
Explanation
Question 37
A 30-year-old male bodybuilder feels a sudden "pop" and tearing sensation in his anterior chest and axilla while performing a heavy bench press. MRI confirms a complete rupture of the sternal head of the pectoralis major muscle from its humeral insertion. The clavicular head is intact. Anatomically, how does the sternal head of the pectoralis major insert onto the humerus relative to the clavicular head?
Explanation
Question 38
An 18-year-old football player presents after a direct blow to the medial clavicle. He is complaining of severe pain, shortness of breath, mild stridor, and difficulty swallowing. Clinical examination and plain radiographs are suggestive of a posterior sternoclavicular (SC) joint dislocation.
What is the most appropriate next step in management?

Explanation
Question 39
A 35-year-old male complains of a painful "clunk" and giving way of his right elbow when he pushes himself out of a chair with his arms. A lateral pivot-shift test of the elbow reproduces his symptoms. This condition is primarily caused by insufficiency of a specific ligamentous structure. What is the normal anatomic origin and insertion of the deficient ligament?
Explanation
Question 40
A 42-year-old male is brought to the trauma bay following a motorcycle crash. He is diagnosed with a "floating shoulder," defined as a double disruption of the superior shoulder suspensory complex (SSSC). According to Goss, the SSSC is a bone-and-soft-tissue ring. Which of the following components is NOT considered part of the SSSC?
Explanation
Question 41
A 28-year-old elite volleyball player presents with insidious onset of posterior shoulder pain and weakness. On examination, there is isolated weakness in external rotation with the arm at the side, but abduction is normal. MRI shows a paralabral cyst. Which of the following is true regarding this condition?
Explanation
Question 42
A 19-year-old rugby player presents to the emergency department after a direct blow to the medial clavicle. He is complaining of chest pain, dyspnea, and dysphagia. Physical examination reveals a palpable defect over the medial clavicle. An AP radiograph and CT scan confirm a posterior sternoclavicular dislocation. What is the most appropriate next step in management?
Explanation
Question 43
A 45-year-old man falls from a height and sustains a comminuted radial head fracture. During surgery, the radial head is deemed unsalvageable and excised. Postoperatively, the patient develops progressive wrist pain and ulnar-sided prominence.
What is the primary pathomechanical cause of this complication?

Explanation
Question 44
When performing an olecranon osteotomy for the surgical management of an intra-articular distal humerus fracture (AO/OTA type 13C), what is the optimal shape of the osteotomy to maximize stability and surface area for healing?
Explanation
Question 45
A 35-year-old weightlifter undergoes a single-incision anterior approach for a distal biceps tendon rupture repair using suture anchors. Postoperatively, he complains of numbness and tingling over the lateral aspect of his forearm. Which nerve was most likely injured, and what structure does it pierce to become superficial?
Explanation
Question 46
A 40-year-old woman falls on an outstretched hand and sustains a 'terrible triad' injury of the elbow.
Which of the following describes the most universally accepted sequence of intraoperative repair for this injury?

Explanation
Question 47
What is the strongest predictor of nonunion in nonoperatively managed midshaft clavicle fractures?
Explanation
Question 48
A 22-year-old competitive rugby player undergoes evaluation for recurrent anterior shoulder instability. A 3D CT scan reveals a 20% anterior glenoid bone loss and a Hill-Sachs lesion. According to the 'glenoid track' concept, an 'off-track' Hill-Sachs lesion is defined by which of the following?
Explanation
Question 49
A 6-year-old boy presents with an elbow injury after falling from monkey bars. Radiographs demonstrate a fracture of the proximal third of the ulna with apex posterior angulation and a posterior dislocation of the radial head. According to the Bado classification, what type of Monteggia lesion is this?
Explanation

Question 50
A 28-year-old man sustains a closed, displaced transverse fracture of the middle third of the humeral shaft. On initial evaluation, he is unable to extend his wrist or fingers, and has numbness in the first dorsal web space. What is the most appropriate management regarding the nerve palsy?
Explanation
Question 51
A 42-year-old woman falls on her outstretched hand and sustains a shear fracture of the distal humerus articular surface. Radiographs reveal a fracture involving the capitellum and the lateral half of the trochlea, with a large piece of subchondral bone attached. According to the Bryan and Morrey classification, what type of fracture is this?
Explanation
Question 52
Which of the following biomechanical changes is most directly responsible for restoring active elevation in a patient with rotator cuff arthropathy undergoing a reverse total shoulder arthroplasty?
Explanation
Question 53
A 32-year-old carpenter presents with right shoulder weakness and a dull ache in the shoulder blade. On physical examination, when the patient pushes against a wall with arms extended forward, the medial border of the right scapula becomes prominent. Injury to which nerve is the most likely cause of this finding?
Explanation
Question 54
A 25-year-old cyclist falls directly onto his right shoulder. He complains of severe pain at the top of the shoulder. Radiographs show a 200% superior displacement of the distal clavicle relative to the acromion.
Which ligaments are disrupted in this Rockwood Type V injury?

Explanation
Question 55
When performing a shoulder hemiarthroplasty for a severe 4-part proximal humerus fracture, what is the most critical factor for a successful functional outcome?
Explanation
Question 56
A 'floating shoulder' typically involves ipsilateral fractures of the clavicular shaft and which other structure?
Explanation
Question 57
A 30-year-old motorcyclist is involved in a high-speed collision and presents with severe swelling of the left shoulder and complete loss of motor and sensory function in the left upper extremity. An AP chest radiograph shows lateral displacement of the left scapula compared to the right, and an intact clavicle. Which associated injury has the highest immediate mortality risk in this condition?
Explanation
Question 58
A 35-year-old man undergoes surgical release for post-traumatic elbow stiffness following a terrible triad injury 1 year ago. To prevent recurrence due to heterotopic ossification (HO), which of the following is the most standard prophylactic regimen?
Explanation
Question 59
A 26-year-old baseball pitcher presents with pain deep in his throwing shoulder and a 'dead arm' sensation. MR arthrogram reveals a SLAP lesion.
During diagnostic arthroscopy, the superior labrum and biceps anchor are found to be detached from the superior glenoid. What type of SLAP tear is this according to the Snyder classification?

Explanation
Question 60
A 22-year-old gymnast sustains an anterior sternoclavicular (SC) joint dislocation. She complains of an unsightly bump on her chest but has no respiratory or swallowing difficulties. After a trial of conservative management, she continues to have pain and instability. If surgery is considered, which of the following is the most appropriate procedure?
Explanation
Question 61
Which combination of radiographic findings in a proximal humerus fracture is most highly predictive of humeral head ischemia according to Hertel's criteria?
Explanation
Question 62
In reverse total shoulder arthroplasty (rTSA), which of the following glenosphere configurations is most effective at minimizing the risk of inferior scapular notching?
Explanation
Question 63
A 65-year-old male with an irreparable posterosuperior rotator cuff tear and a positive Hornblower's sign undergoes a latissimus dorsi tendon transfer. During the harvest of the tendon, which neurovascular bundle is at greatest risk and must be carefully protected?
Explanation
Question 64
A 42-year-old female presents with persistent shoulder pain and weakness 4 weeks after undergoing a lymph node biopsy in the posterior cervical triangle. On physical exam, she demonstrates lateral winging of the scapula and an inability to actively abduct the shoulder past 90 degrees. Injury to which of the following nerves is the most likely cause?
Explanation
Question 65
A 38-year-old male undergoes surgical repair of a complete distal biceps tendon rupture using a single-incision anterior approach. Postoperatively, he complains of numbness over the radial aspect of his volar forearm. Which structure was most likely injured during the procedure?
Explanation
Question 66
A 28-year-old female complains of recurrent clicking and a sense of instability in her elbow when pushing up from a chair. Physical examination reveals apprehension during a pivot-shift test. This condition is primarily due to insufficiency of which of the following structures?
Explanation
Question 67
A 45-year-old male falls from a height and sustains a comminuted radial head fracture, along with significant wrist pain. Radiographs show proximal migration of the radius. If the radial head is resected without replacement in this setting, what is the most likely biomechanical consequence?
Explanation
Question 68
A 78-year-old female with severe rheumatoid arthritis sustains a highly comminuted, osteopenic distal humerus fracture (AO/OTA 13-C3). She is treated with a total elbow arthroplasty (TEA). What is the most critical postoperative restriction she must strictly adhere to?
Explanation
Question 69
A 30-year-old male sustains a closed, spiral fracture of the distal third of the humeral shaft. Initial examination reveals an intact neurologic profile. Following a closed reduction and application of a coaptation splint, the patient demonstrates an inability to extend his wrist and fingers. What is the most appropriate next step in management?
Explanation
Question 70
A 19-year-old male rugby player presents to the emergency department with severe anterior chest wall pain, dysphagia, and a sensation of choking following a direct blow to the medial clavicle. Suspecting a posterior sternoclavicular dislocation, what is the most appropriate initial imaging modality to confirm the diagnosis and assess associated risks?
Explanation
Question 71
A 25-year-old male sustains a severe crush injury to the forearm. Several hours later, he develops excruciating pain out of proportion to the injury. Which of the following clinical findings is generally considered the most reliable early indicator of evolving forearm compartment syndrome?
Explanation
Question 72
According to current literature, which of the following is a widely accepted absolute indication for Open Reduction and Internal Fixation (ORIF) of a scapular fracture?
Explanation
Question 73
A 22-year-old male collegiate wrestler presents with recurrent anterior shoulder instability. Advanced imaging reveals an anterior glenoid bone defect measuring 28% of the glenoid width, along with an engaging Hill-Sachs lesion. Which of the following surgical procedures is most appropriate?
Explanation
Question 74
Following an unsalvageable radial head fracture, a metallic radial head arthroplasty is planned. To prevent overstuffing the radiocapitellar joint, the proximal articular surface of the radial head implant should ideally be placed at which anatomic landmark relative to the proximal radioulnar joint (PRUJ)?
Explanation
Question 75
A 35-year-old cyclist sustains a midshaft clavicle fracture. Which of the following radiographic parameters is most strongly associated with an increased risk of symptomatic nonunion if treated nonoperatively?
Explanation
Question 76
A 45-year-old male presents with a closed, isolated scapula fracture following a high-energy fall. Which of the following radiographic parameters is a widely accepted indication for operative fixation?
Explanation
Question 77
A 6-year-old boy presents with an anterior dislocation of the radial head and a fracture of the ulnar diaphysis. What is the most commonly injured nerve associated with this specific injury pattern?
Explanation
Question 78
Recent quantitative perfusion studies have redefined the vascularity of the proximal humerus. According to these studies, which artery provides the predominant blood supply to the humeral head?
Explanation
Question 79
A 32-year-old female sustains a coronal shear fracture of the distal humerus that involves the capitellum and the lateral half of the trochlea. Which classification accurately describes this fracture pattern?
Explanation
Question 80
A 50-year-old female with poorly controlled type 2 diabetes presents with progressive, painful restriction of active and passive shoulder motion. What is the predominant histological finding in the joint capsule of a patient with this condition?
Explanation
Question 81
A 28-year-old cyclist sustains a closed midshaft clavicle fracture. If managed nonoperatively, which of the following fracture characteristics is most strongly associated with an increased risk of nonunion?
Explanation
Question 82
A 40-year-old male undergoes radial head arthroplasty for a severely comminuted radial head fracture. Overstuffing the radiocapitellar joint during this procedure will most likely lead to which of the following complications?
Explanation
Question 83
During arthroscopic evaluation of a 22-year-old baseball pitcher, a superior labral anterior-posterior (SLAP) tear is identified with detachment of the biceps anchor. Which of the following physical examination findings was most likely positive preoperatively?
Explanation
Question 84
When utilizing an olecranon osteotomy for open reduction and internal fixation of a multi-fragmentary distal humerus fracture (AO/OTA 13C3), which osteotomy type is biomechanically superior for minimizing nonunion?
Explanation
Question 85
A 30-year-old competitive weightlifter ruptures his pectoralis major tendon during a bench press. When performing an anatomic primary repair, where should the sternal head insert on the humerus relative to the clavicular head?
Explanation
Question 86
Which tendon is most commonly and primarily involved in the underlying pathoanatomy of lateral epicondylitis (tennis elbow)?
Explanation
Question 87
A 19-year-old male presents to the trauma bay with a posterior sternoclavicular joint dislocation following a rugby tackle. He has mild dysphagia but stable vitals. What is the most appropriate initial management?
Explanation
Question 88
A 26-year-old female presents with lateral scapular winging and an inability to actively abduct her arm past 90 degrees. She recently underwent a lymph node biopsy in the posterior cervical triangle. Which nerve was most likely injured?
Explanation
Question 89
A 42-year-old male sustains an Essex-Lopresti injury characterized by a comminuted radial head fracture, rupture of the interosseous membrane, and disruption of the distal radioulnar joint (DRUJ). In the acute setting, what is the most appropriate management of the radial head?
Explanation
None
