Orthopedic Surgery Board Review MCQs: Trauma, Upper Extremity & Foot | Part 3
Key Takeaway
This page presents Part 3 of a comprehensive orthopedic board review quiz. Crafted for residents and surgeons preparing for AAOS/OITE certification, it features 100 high-yield, verified MCQs covering clinical scenarios, with detailed explanations and versatile learning modes for effective exam prep.
About This Board Review Set
This is Part 3 of the comprehensive OITE and AAOS Orthopedic Surgery Board Review series authored by Dr. Mohammed Hutaif, Consultant Orthopedic & Spine Surgeon.
This set has been strictly audited and contains 100 100% verified, high-yield multiple-choice questions (MCQs) modelled on the exact format of the Orthopaedic In-Training Examination (OITE) and the American Academy of Orthopaedic Surgeons (AAOS) board examinations.
How to Use the Interactive Quiz
Two distinct learning modes are available:
- Study Mode — After selecting an answer, you immediately see whether you are correct or incorrect, together with a full clinical explanation and literature references.
- Exam Mode — All feedback is hidden until you click Submit & See Results. A live timer tracks elapsed time. A percentage score and detailed breakdown are displayed upon submission.
Pro Tip: Use keyboard shortcuts A–E to select options, F to flag a question for review, and Enter to jump to the next unanswered question.
Topics Covered in Part 3
This module focuses heavily on: Deformity, Elbow, Foot, Shoulder, Trauma.
Sample Questions from This Set
Sample Question 1: A 20-year-old collegiate football player who sustained blunt head trauma during the first half of a game is emotional and confused. During the halftime intermission, his affect, memory, and disorientation are totally resolved and have retur...
Sample Question 2: A 9-year-old girl has pain over the fifth toe that is aggravated by shoe wear. Clinical photographs are shown in Figures 28a and 28b. Treatment of this deformity should consist of...
Sample Question 3: A 24-year-old collegiate pitcher has had increasing pain over his medial elbow for 3 months. He has point tenderness over his medial epicondyle and reproduction of his symptoms with a valgus stress test. What phase of the throwing cycle mos...
Sample Question 4: A 5-year-old girl sustains an isolated injury to the right shoulder area after falling off the monkey bars. Examination reveals intact neurovascular function in the extremity distally, but she is quite uncomfortable. An AP radiograph of the...
Sample Question 5: Percutaneous placement of a lateral proximal tibial locking plate that extends down to the distal third of the leg is associated with postoperative decreased sensation of which of the following distributions?...
Why Active MCQ Practice Works
Evidence consistently demonstrates that active recall through spaced MCQ practice yields substantially greater long-term retention than passive reading alone (Roediger & Karpicke, 2006). All questions in this specific module have been algorithmically verified for clinical integrity and complete explanations.
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 20-year-old collegiate football player who sustained blunt head trauma during the first half of a game is emotional and confused. During the halftime intermission, his affect, memory, and disorientation are totally resolved and have returned to preinjury baseline. The only residual finding is a very mild headache. He wants to play the second half. What is the most appropriate course of action?
Explanation
REFERENCES: Garrick J (ed): Orthopaedic Knowledge Update: Sports Medicine 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 29-48.
Guskiewicz KM, McCrea, Marshall SW, et al: Cumulative effects associated with recurrent concussion in collegiate football players: The NCAA Concussion Study. JAMA
2003;290:2549-2555.
Question 2
A 9-year-old girl has pain over the fifth toe that is aggravated by shoe wear. Clinical photographs are shown in Figures 28a and 28b. Treatment of this deformity should consist of
Explanation
REFERENCES: Black GB, Grogan DP, Bobechko WP: Butler arthroplasty for correction of adducted fifth toe: A retrospective study of 36 operations between 1968 and 1982. J Pediatr Orthop 1985;5:439-441.
Paton RW: V-Y plasty for correction of varus fifth toe. J Pediatr Orthop 1990;10:248-249.
Coughlin MJ, Mann RA: Lesser toe deformities, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 5. St Louis, MO, Mosby, 1986, pp 132-157.
Question 3
A 24-year-old collegiate pitcher has had increasing pain over his medial elbow for 3 months. He has point tenderness over his medial epicondyle and reproduction of his symptoms with a valgus stress test. What phase of the throwing cycle most likely will reproduce his symptoms? Review Topic
Explanation
Question 4
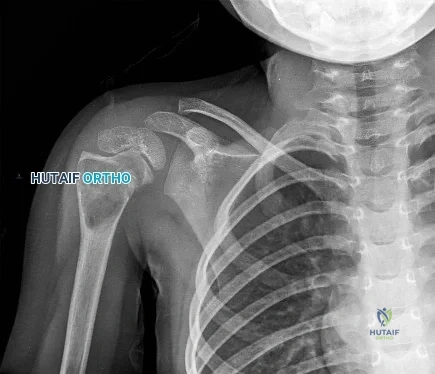
A 5-year-old girl sustains an isolated injury to the right shoulder area after falling off the monkey bars. Examination reveals intact neurovascular function in the extremity distally, but she is quite uncomfortable. An AP radiograph of the proximal humerus is shown in Figure 24. Her parents state that she is a very talented gymnast. Considering her age and potential athletic career, management should consist of
Explanation
REFERENCES: Martin RF: Fractures of the proximal humerus and humeral shaft, in Letts RM (ed): Management of Pediatric Fractures. New York, NY, Churchill Livingstone, 1994,
pp 144-148.
Sanders JO, Rockwood CA Jr, Curtis RJ: Fractures and dislocation of the humeral shaft and shoulder, in Rockwood CA Jr, Wilkins KE, Beaty JH (eds): Fractures in Children, ed 4. Philadelphia, PA, Lippincott-Raven, 1996, vol 3, pp 937-939.
Question 5
Percutaneous placement of a lateral proximal tibial locking plate that extends down to the distal third of the leg is associated with postoperative decreased sensation of which of the following distributions?

Explanation
Question 6
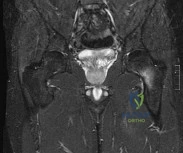
A 47-year-old landscaper presents with worsening left shoulder pain and weakness. Three years ago, he injured the left shoulder in a fall and elected for nonoperative management to minimize time off from work. Physical therapy was effective until 6 months ago when his shoulder function worsened to the point that he is now unable to work. Examination of his active range of motion reveals forward elevation 120° with pain, abduction 100°, IR at neutral to T8 and ER at neutral 5°. He has a positive ER lag sign and Hornblower's sign. Belly press and lift-off tests are normal. A recent radiograph is shown in Figures A. MRI images are shown in Figures B and C. Which of the following is the best treatment option? Review Topic
Explanation
Irreparable rotator cuff tears are marked by: (1) Superior displacement of the humeral head (AHI < 5-7mm), (2) Fatty infiltration of the rotator cuff muscles (Goutallier stage 3-4), (3) Increased duration of the tendon tear and (4) Profound external rotation weakness. These findings are predictive of poor-quality tissue and stiffness of the muscle-tendon unit, not amenable to primary repair. In this setting, a latissimus dorsi
transfer can be utilized to restore shoulder strength, function and improve pain. Relative contraindications include subscapularis deficiency, deltoid deficiency, pseudoparalysis of the shoulder and advanced glenohumeral arthritis.
Gerber et al. performed a case series analysis of 67 patients with irreparable rotator cuff tears managed with latissimus dorsi transfer. Patients with an intact subscapularis demonstrated improvement in pain, range of motion and strength postoperatively, while no improvement was noted in patients with subscapularis deficiency. The authors conclude that latissimus dorsi transfer should not be performed in the setting of poor subscapularis function.
Iannotti et al. found that better clinical results following latissimus dorsi transfer were associated with: preserved active shoulder range of motion and strength (specifically forward elevation > 90° and external rotation > 20°), synchronous firing of the transferred latissimus dorsi muscle and male gender.
Figure A is an AP radiograph of the left shoulder with superior migration of the humeral head (AHI < 5mm) and no evidence of glenohumeral arthritis. Figures B and C show a retracted posterosuperior rotator cuff tear and Goutallier stage 4 atrophy (more fat than muscle) of the supraspinatus, infraspinatus and teres minor, rendering this tear irreparable. Illustration A shows a latissimus dorsi transfer. The latissimus dorsi tendon is positioned over the top of the humeral head, covering most of the rotator cuff defect. The tendon is then secured to the subscapularis tendon edge and lesser tuberosity anteriorly, the remnant supraspinatus and infraspinatus tendons medially, and the greater tuberosity laterally.
Incorrect Answers:
Question 7
A 22-year-old woman underwent closed reduction and percutaneous pinning with casting of a displaced extra-articular distal radius fracture. The surgery was completed with a supraclavicular regional anesthesia. After the block wears off, she reports new onset dense numbness in the palmar aspect of the thumb, index, and middle fingers as well as severe pain in the hand. What is the next step in management?
Explanation
Question 8
A 12-year-old girl has the painful foot deformity seen in Figure 79. You advise her that she has juvenile bunions. How do they differ from adult bunions?
Explanation
angle is less than the adult bunion. Bursal thickenings and prominence of the medial eminence are less in a juvenile bunion.
Question 9
A 20-year-old man is brought to the emergency department after a high-speed motor vehicle accident. His initial blood pressure is 70/40 mm Hg. He is currently receiving intravenous fluids as well as blood. His Focused Assessment with Sonography for Trauma examination did not show any free fluid in his abdomen and his chest radiograph is unremarkable. An AP pelvis radiograph is shown in Figure 15. What is the next most appropriate step in the management of his pelvic injury? Review Topic
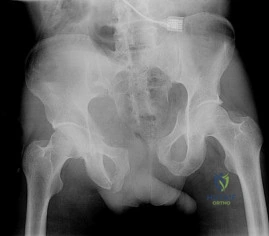
Explanation
Question 10
A 58-year-old man has had increasing midback pain for 8 weeks. Radiographs reveal mild osteopenia and mild disk degeneration but no fractures or lesions. An MRI of the spine reveals diskitis with a small-intensity signal within the spinal canal that is consistent with an epidural abscess at T11-12. The patient is neurologically intact but in significant pain. CT-guided biopsy of the disk space is positive for methicillin-sensitive Staphylococcus aureus. What is the most appropriate treatment?
Explanation
The treatment of spinal infections is variable. A diskitis in a patient with a mechanically stable spine without neurologic compromise is typically treated with needle biopsy/culture and appropriate IV antibiotics. Epidural abscess often is considered one of the true orthopaedic emergencies that necessitates surgical intervention. However, there is growing evidence that medical management can be appropriate to treat epidural abscesses in certain cases. In cases involving neurologic deterioration, surgical decompression, drainage, and systemic IV antibiotics is the treatment of choice. Medical management of spinal abscesses can be considered when a patient refuses surgical decompression; surgery is contraindicated because of high risk, pain, or
infection; or paralysis lasting longer than 24 to 36 hours results in a likely inability to reverse the paralysis. Patients who are neurologically intact may also be treated with medical management alone if they are stable and have an identifiable microorganism that can be observed closely to assess for neurologic deterioration. If neurologic changes are noted, surgical decompression and debridement and continued IV antibiotic therapy are appropriate.
RECOMMENDED READINGS
Darouiche RO. Spinal epidural abscess. N Engl J Med. 2006 Nov 9;355(19):2012-20. Review. PubMed PMID: 17093252.View Abstract at PubMed
Kim SD, Melikian R, Ju KL, Zurakowski D, Wood KB, Bono CM, Harris MB. Independent predictors of failure of nonoperative management of spinal epidural abscesses. Spine J. 2014 Aug 1;14(8):1673-9. doi: 10.1016/j.spinee.2013.10.011. Epub 2013 Oct 30. PubMed PMID:
Question 11
Figures 25a and 25b show the radiograph and MRI scan of a 7 1/2-year-old boy who has been limping for 1 year. His pain has worsened over the past 2 weeks, and his parents note swelling over the dorsum of the foot for the past 4 days. Examination reveals no fever, and laboratory studies show a WBC of 6,700/mm 3 , an erythrocyte sedimentation rate of 26 mm/h, and a normal C-reactive protein level. What is the most likely diagnosis?
Explanation
REFERENCES: Wang MN, Chen WM, Lee KS, Chin LS, Lo WH: Tuberculous osteomyelitis in young children. J Pediatr Orthop 1999;19:151-155.
Watts HG, Lifeso RM: Tuberculosis of the bones and joints. J Bone Joint Surg Am 1996;78:288-298.
Question 12
intermittent PTH injections increase bone mass, 2) continous infusion lead to bone resorption, and 3) dosing should not continue past 2 yrs. Thus, intermittent parathyroid hormone is anabolic to bone and is used as a treatment of osteoporosis (forteo).
Explanation
a transmembrane protein that acts intracellularly to activate the G protein pathways. Myc is a proto-oncogene that encodes for a transcription factor involved in numerous cell- activation pathways, but is not directly phosphorylated by BMP receptor.
ß-catenin is an intracellular molecule that plays a key role in the Wnt signaling pathway. This pathway is also involved in osteoblastic differentiation, but differs in target proteins within the cell.
A 45-year-old previously healthy woman has experienced weakness and fatigability for 2 months. She states she feels best in the morning, but tires easily with exertion. If she sits and rests her strength improves, but she easily tires with each activity. When her fatigue is most severe, she has double vision. Physical examination is
positive for ptosis with upward gaze after 20 seconds. When she holds her arms out straight she shows good initial strength, but rapidly decreasing strength with time. What is the pathologic cause of her muscle weakness?
Ig antibodies at the neuromuscular (NM) junction
Decreased release of acetylcholine at the NM junction
Decrease in myelin sheath of axonal nerves with loss of NM junction
Absence of dystrophin with excess calcium at sarcolemma
The patient has myasthenia gravis, which has its onset in middle age and causes progressive weakness because of the loss of acetylcholine receptors secondary to autoimmune antibodies at the NM junction. Rest periods allow uptake of acetylcholine and initial strength, but easy fatigability. Treatment is aimed at immunomodulation; acetyl cholinesterase inhibitors often coupled with thymectomy can control symptoms.
Decreased release of acetylcholine at the NM junction is the effect of a nondepolarizing drug or toxin botulinum. Patients with muscular dystrophy lack dystrophin that acts at the sarcolemma to regulate calcium channels, and onset of this condition occurs at a younger age. The decrease in myelin indicates Charcot-Marie-Tooth disease and is
often seen with long axon degeneration, such as in the feet and lower legs.
You are studying a single continuous variable after administration of a defined treatment intervention. Your statistician informs you the data are not normally distributed. What is the best test to analyze the data?
Analysis of variance (ANOVA)
Regression analysis
Student t test
Mann-Whitney U test
The Mann-Whitney U test is used when data are nonparametric, meaning either not normally distributed or variances are not equal among groups. Both the Student t test and ANOVA are used with parametric, normally distributed data. A regression analysis is a
statistical model that allows for control of potentially confounding variables. It is used to assess the relationship between a dependent variable and (usually) multiple independent variables.
Which of the following is the mechanism of action of aspirin?
Inhibition of vitamin K-dependent carboxylation
Inhibition of factor Xa through antithrombin binding
Binding of cyclooxygenase (COX)-1 and COX-2
Direct thrombin inhibition
Glycoprotein IIIb agonist binding
Aspirin works by the irreversible binding of cycloxygenase (COX). This effect inhibits platelet generation of thromboxane A2, resulting in an antithrombotic effect. In addition, there is a decrease in the level of prostaglandin production due to the COX-1 binding.
Aspirin's effects and respective mechanisms of action vary with dose:
Low doses (typically 75 to 81 mg/day) are sufficient to irreversibly acetylate serine 530 of cyclooxygenase (COX)-1. This effect inhibits platelet generation of thromboxane A2, resulting in an antithrombotic effect.
FOR ALL MCQS CLICK THE LINK ORTHO MCQ BANK
Intermediate doses (650 mg to 4 g/day) inhibit COX-1 and COX-2, blocking prostaglandin (PG) production, and have analgesic and antipyretic effects. Illustration A shows the mechanism of action of aspirin.
InCORRECT Answers: 1,2,4,5: Aspirin does not have any of these mechanisms of action.
A study is proposed in which 2 groups of patients are randomized to treatment with bisphosphonates or placebo. This is an example of what study type?
Crossover design trial
Parallel design trial
Cohort study
Case series
In a parallel design trial, participants are randomized to 2 or more groups, each of which receives a different treatment or intervention. For example, Group A receives the drug and Group B receives the placebo. This type of
design allows for comparison between groups. In a crossover design clinical trial, both groups receive both interventions over a defined time period. For example, Groups A and B both receive the drug as well as the placebo. This allows for within-participant comparisons. In a cohort study, patient groups are followed over time on the basis of having or not having received an exposure. Cohort studies are not randomized. In a case series, patients often receive a particular treatment and the outcomes are then examined.
An otherwise healthy 50-year-old man who is a smoker undergoes a posterior spine fusion with instrumentation for spondylolisthesis. What can the patient do to minimize his risk for pseudarthrosis?
Increase calcium and vitamin D intake
Avoid all nonsteroidal anti-inflammatory drugs (NSAIDs)
Maintain smoking cessation
Engage in early physical therapy to strengthen the trunk musculature
Smoking is the biggest risk factor for nonunion and should be strictly avoided. NSAIDs interfere with bone healing, but not as strongly as smoking. Early mobilization would potentially stress the construct, inducing movement that leads to nonunion. Without history of calcium and vitamin D deficiency, increasing intake would not decrease the risk of nonunion.
When making a comparison to autograft incorporation, the inflammatory process in allograft tissue anterior cruciate ligament (ACL) reconstruction
occurs earlier.
occurs later.
is prolonged.
is shortened.
Compared to similar autograft, allograft tissue demonstrates a prolonged inflammatory response, slower rate of biological incorporation and remodeling, and a higher proportion of large-diameter collagen fibrils. Native ACL inserts
into bone through a transition of 4 distinct zones: tendon, unmineralized fibrocartilage, mineralized fibrocartilage, and bone. This transition is not reproduced with tendon grafts, which instead heal with interposed fibrovascular scar at the graft-tunnel interface. The scar rapidly remodels to form perpendicular fibers resembling Sharpey fibers and, eventually, mature bone growth into the outer portion of the graft. The intra- articular portion of allograft undergoes an initial phase of necrosis followed by repopulation by host synovial cells into the acellular collagen scaffold.
Revascularization and maturation complete the ligamentization of graft tissue.
A researcher decides she wants to look at the current total number of patients who have methicillin-resistant Staphylococcus aureus (MRSA) infections in a hospital on 1 particular day. What is the researcher measuring?
Correlation coefficient of MRSA
Prevalence of MRSA
Incidence of MRSA
Relative risk of MRSA
The prevalence of a disease is a measure of the number of cases of a disease at or during a specific time point or time period. In this case, the researcher wants to know the prevalence of disease on a given day. Incidence measures new cases of a disease or event per unit of time. Correlation coefficient is a measure of how 2 things correlate with one another, while relative risk is a statistical outcome that is often used in case-control or cohort studies to provide a measure of the risk of a particular disease occurring when a certain exposure has already occurred.
A 48-year-old man who is scheduled to undergo total knee replacement has an X-linked clotting disorder that leads to abnormal bleeding and recurrent, spontaneous hemarthrosis. Before undergoing surgery, he should have replacement therapy of
protein C and S.
vitamin K.
von Willebrand factor.
factor VIII.
Hemophilia A is an X-linked recessive deficiency of factor VIII that can lead to significant bleeding problems including recurrent spontaneous hemarthroses that can lead to synovitis and joint destruction. von Willebrand disease is a lack of von Willebrand factor that leads to decreased platelet aggregation; more commonly patients have mucosal bleeding and not hemarthroses. Vitamin K deficiency is not hereditary; it is typically attributable to inadequate dietary intake, malabsorption, and loss of storage sites from hepatocellular disease. Protein C and S deficiencies are autosomal-dominant diseases that lead to thrombosis, not bleeding, as protein C and S shut off thrombin formation.
What is the recommended optimal timing of presurgical antibiotic administration to prevent infection in patients undergoing total joint replacement surgery?
Within 1 hour before incision
Within 2 hours before incision
Immediately after incision
Within 1 hour after incision
The current recommendation for antibiotic prophylaxis for major orthopaedic surgical procedures is to administer intravenous antibiotics within 1 hour of surgical incision. Redosing of antibiotics should occur 3 to 4 hours after the initial dose for procedures that extend beyond 3 to 4 hours. Little evidence supports postsurgical antibiotic use beyond 24 hours. As you move beyond 1 hour from time of administration of antibiotics, risk for infection increases and rates of bacterial cell death decline. It is not acceptable to
administer presurgical antibiotics after incision.
Bacterial resistance to antibiotics in biofilm is an example of
avoidance.
decreased susceptibility.
inactivation.
mutation. CORRECT answer: 1
Three basic mechanisms of antibiotic resistance have been identified: avoidance, decreased susceptibility, and inactivation. Biofilm formation is a classic example of avoidance, whereby the biofilm creates a physical barrier to the antibiotic. Bacteria can decrease their susceptibility to antibiotics by mutating the antibiotic target or generating a mechanism to inactivate the antibiotic. Biofilm formation develops when a sufficient mass of bacteria forms on a surface. The cell-to-cell signaling becomes sufficient to activate transcription of genes needed for biofilm formation in a process known as quorum sensing. Once the bacteria produce a mature biofilm, they enter a greatly reduced or stationary phase of growth. Lastly, high-shear
environments seem to stimulate biofilm production.
A patient with Paget disease who is intolerant of bisphosphonates is given calcitonin. What is the mechanism of action of calcitonin?
Promotes reabsorption of phosphate in the renal tubules
Interferes with osteoclast maturation
Interferes with intestinal absorption of calcium
Upregulates osteoblast formation
Calcitonin is a hormone that reduces serum calcium concentration by directly interfering with osteoclast maturation via receptors. Calcitonin inhibits phosphate reabsorption and decreases calcium reabsorption in the kidneys. By attenuating cartilage breakdown and stimulating cartilage formation via inhibitory pathways of matrix metalloproteinases, calcitonin also has a
chondro-protective effect on articular cartilage. Calcitonin has no major effects on intestinal absorption of calcium, but may aid in small-bowel secretion of sodium, potassium, chloride, and water. Calcitonin also has no receptor effect on osteoblasts.
A cartilage water content increase is the hallmark of which
osteoarthritis stage?
Prearthritis
Early
Late
Terminal
The first stage of osteoarthritis is marked by an increase in water content secondary to disruption of the matrix framework. This is followed by an increase in chondrocyte anabolic and catabolic activity in response to tissue damage. Wnt-induced signal protein 1 increases chondrocyte protease expression. Failure to restore tissue balance ultimately leads to continued destruction and osteoarthritis. One hallmark of osteoarthritic cartilage is a reduced repair mechanism attributable to decreased chondrocyte response to growth factor stimulation (transforming growth factor-alpha and insulin-like growth factor-1).
Mitochondrial dysfunction and increased production of reactive oxygen species may promote cell senescence, a progressive slowing of cellular activity. Microscopic evidence of cartilage degeneration begins with fibrillation of the superficial and transition zones, followed by disruption of the tidemark by subchondral blood vessels and eventual subchondral bone remodeling. This process ultimately leads to cartilage degradation with decreased water content in the late and terminal phases of osteoarthritis.
What is the plasma half-life of warfarin?
1 to 2 hours
4 to 6 hours
12 to 18 hours
36 to 42 hours
Warfarin, which is dosed daily, can take 72 to 96 hours to reach therapeutic levels. It has a plasma half-life of 36 to 42 hours. Low-molecular heparins have a plasma half-life of 4 to 5 hours, and fondaparinux has a half-life of 17 to 21 hours. Warfarin will not affect the International Normalized Ratio (INR) until 2 to 3 days after it is given. Patients on chronic warfarin therapy should
have treatment stopped 3 to 5 days before elective surgery to allow the INR to normalize.
A 70-year-old woman with a body mass index (BMI) of 34 and a history of hypercholesterolemia has elected to undergo total hip arthroplasty. Her son recently learned he has Factor V Leiden following an episode of pulmonary embolism. What are this patient's risk factors for thromboembolic disease?
Type of surgery, age, and BMI
Type of surgery, hypercholesterolemia, and age
Age, BMI, and hypercholesterolemia
BMI, type of surgery, and hypercholesterolemia
Risk stratification is one of the most critical clinical evaluations before undergoing total joint arthroplasty. Many factors have been identified to increase risk for venous thromboembolism (VTE). The major factors include previous VTE, obesity, type of surgery (such as total joint arthroplasty), hypercoagulable states, myocardial infarction, congestive heart failure, family history of VTE, and hormonal replacement therapy.
Hypercholesterolemia is not a risk factor for thromboembolic disease.
DNA replication occurs during which phase of the cell cycle?
M
S
R
G1
G2
The cell cycle consists of four distinct phases: initial growth (G1), DNA replication/synthesis (S), a gap (G2), and mitosis (M) (see illustration).
The G1 and G2 phases of the cell cycle represent the “gaps” or growth phases in the cell cycle that occur between DNA synthesis and mitosis. G0 cells are in a stable state and have not entered the cell cycle. During the S phase, the DNA is synthesized and replicated. During the M phase or mitosis, all genetic material divides into two daughter cells.
The cells are diploid (2N) in the G0 and G1 phases. The cells become tetraploid (4N) at the end of S and for the entire G2 phases. There is no R phase in the cell cycle.
What antithrombotic agent is a selective factor I0a inhibitor?
Warfarin
Low-molecular-weight heparin
Rivaroxaban
Aspirin
Rivaroxaban is a selective factor I0a inhibitor. Aspirin is a cyclooxygenase inhibitor. Low-molecular-weight heparin is a nonspecific anticoagulant. Warfarin is a vitamin K antagonist and reduces production of clotting factors II, VII, IX, and X.
A 68-year-old woman had advanced right knee arthritis and total knee replacement was planned. She learned she had primary biliary cirrhosis at age 41 and now has advancing liver failure. Preoperative coagulation tests show a baseline International Normalized Ratio (INR) of 1.36. Appropriate methods to prevent thromboembolic
disease as recommended by the 2011 AAOS Clinical Practice Guideline, Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee
Arthroplasty, include
use of mechanical prophylaxis (eg, pneumatic calf compressors) while in the hospital.
oral warfarin with a goal INR between 2.0 and 3.0.
low-dose warfarin for 3 weeks postsurgically beginning 48 hours after surgery.
no prophylaxis because this patient already is partially anticoagulated secondary to her liver disease.
The 2011 AAOS Clinical Practice Guideline, Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee Arthroplasty, recommends the use of mechanical prophylaxis for patients at increased risk
for bleeding (including those with liver disease or hemophilia). This recommendation is the consensus of the workgroup that established these guidelines because there was insufficient evidence to justify a stronger recommendation in this clinical scenario. The other responses use no prophylaxis or pharmacological prophylaxis. Pharmacological prophylaxis is not recommended in patients who are at increased risk for bleeding.
The pharmacokinetics of which deep venous thrombosis (DVT) prophylactic agent are affected by liver function and dietary intake?
Dalteparin
Warfarin
Fondaparinux
Enoxaparin
Warfarin is an oral vitamin K antagonist that is rapidly absorbed from the gastrointestinal tract. It accumulates in the liver, where it is metabolized and excreted. The pharmacokinetics of warfarin can be affected by certain drugs or disease states that influence liver function. Fondaparinux is a synthetic factor Xa inhibitor that is eliminated through the kidneys. Both Dalteparin and Enoxaparin are low-molecular-weight heparins that activate antithrombin and inhibit factors Xa and IIa. Like Fondaparinux, they are eliminated through the kidneys and should be used with caution in patients with kidney disease.
What infection-control measure has been shown to have the most notable impact in reducing surgical-site infections?
Intravenous antibiotic administration within 1 hour of surgical incision
Screening and decolonization of patients colonized with methicillin-resistant
<em>Staphylococcus aureus</em>
Horizontal laminar flow
Use of enclosed body exhaust suits
Timely administration of prophylactic antibiotics is the most important factor shown to decrease surgical-site infections. The use of horizontal laminar flow and body exhaust suits has not been shown to significantly affect infection rates.
The resistance to pullout of a screw in osteoporotic bone is increased by all of the following EXCEPT?
Placement parallel to the trabecular pattern
Purchase in cortical bone
Use of a fixed angle (locking screw construct)
Tapping prior to screw placement
Augmentation with polymethylmethacrylate
Of the options listed, tapping prior to screw placement is the only variable that does not increase the pullout strength of a screw in osteoporotic bone.
Cornell reviews internal fixation in osteoporotic bone. According to this article, the quality of the bone is the primary determinant of the holding power of an individual screw. Other factors that increase the pullout strength include fixation in cortical bone (cortical bone has greater mineral density and, therefore, greater resistance to screw pullout than trabecular bone), screws placed parallel to the trabecular pattern, and screw fixation augmented with PMMA. The addition of a locking plate will also increase the resistance to failure by creating a fixed angle construct. Tapping prior to placement of the screw has not been shown to increase resistance to pullout, on the contrary studies have shown
this decreases resistance to pullout.
Turner et al examined the holding strength of small and large diameter screws in healthy bovine and diseased human bone. They found the screw diameter, trabecular orientation of the bone, and mineral content of the bone all affect the holding strength. A larger diameter screw, parallel placement to the trabecular pattern, and purchase in bone with a higher density all increase the holding strength.
Gigantism affects which region of the growth plate labeled in Figure A?
A
B
C
D
E
Gigantism, like achondroplasia, affects the proliferative zone (Region C of Figure A) of the growth plate. In Figure A, Region A is the epiphysis, Region B is the resting zone, Region D is the hypertrophic zone, and Region E is the metaphysis. Illustration A is another depiction of the physis which is labeled. Gigantism is typically caused by a pituitary adenoma which over secretes growth hormone. Its effect on the proliferative zone results in bone overgrowth and excessive height and limb length. Acromegaly may also be
caused by a pituitary adenoma that over secretes growth hormone, but has its effect once the physis has closed.
Plain radiographs do not provide an accurate assessment of bone mineral density (BMD) until what percentage of mineral has been lost?
Question 13
During the cocking and acceleration phases of the overhand throw (pitch), there are several static and dynamic restraints to provide medial elbow support and prevent valgus instability. The dynamic structures found to be most important during these phases of the overhand throw are the flexor digitorum Review Topic
Explanation
Question 14
A 14-year-old boy sustained a 100% displaced distal radius Salter-Harris type II fracture. Neurologic examination demonstrates normal motor examination and two-point discrimination. He undergoes fracture reduction to the anatomic position with the application of a long arm cast. Postreduction he reports increasing hand and wrist pain with diminution of two-point discrimination to 10 mm over the index and middle fingers over the next several hours after surgery. The cast is bivalved and the padding released relieving all external pressure over the arm. Reevaluation reveals increasing sensory deficit over the affected area. What is the next most appropriate management intervention?
Explanation
Question 15
Which of the following statements regarding the use of thermal shrinkage during arthroscopic shoulder surgery is most accurate? Review Topic
Explanation
Question 16
Chronic traumatic encephalopathy (CTE) is a neurodegenerative disease that is characterized by
Explanation
Question 17
A 12-year-old boy sustained a grade III open tibial fracture 1 week ago and underwent multiple debridements and fracture fixation. He now has a soft-tissue defect that measures 6 cm × 6 cm, with an area of exposed bone and muscle on the distal medial leg that is a few centimeters proximal to the ankle. Management of the soft-tissue defect should now consist of
Explanation
A free flap and skin graft would be required for closure. VAC is very effective in soft-tissue defects such as this one. Healthy granulation tissues form quickly. VAC can be the definitive treatment, or it can be used before skin grafting. Wet-to-dry dressings could promote granulation, but the process is hastened substantially by VAC. Amputation is not a consideration because there are no signs of infection or fracture healing problems at this time.
REFERENCES: Mooney JF III, Argenta LC, Marks MW, et al: Treatment of soft tissue defects in pediatric patients using the V.A.C. system. Clin Orthop 2000;376:26-31.
Caniano DA, Ruth B, Teich S: Wound management with vacuum-assisted closure: Experience in 51 pediatric patients. J Pediatr Surg 2005;40:128-132.
Question 18
A 20-year-old college baseball pitcher reports the insidious onset of medial elbow pain. Examination reveals medial elbow tenderness, a normal neurologic examination, and no obvious valgus laxity. Plain radiographs are normal. MRI scans are shown in Figures 39a and 39b. Management should consist of
Explanation
REFERENCES: Norris TR (ed): Athletic Injuries of the Elbow. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, pp 311-323.
Hyman J, Breazeale NM, Altchek DW: Valgus instability of the elbow in athletes. Clin Sports Med 2001;20:11-24.
Question 19
Steroids are thought to prevent neurologic deterioration after traumatic spinal cord injury by which of the following mechanisms? Review Topic
Explanation
Question 20
A 65-year-old woman fell onto her outstretched right arm and immediately had pain. She has a history of osteoporosis. Examination of the right arm reveals lateral arm swelling, ecchymosis, and she is unable to move the elbow due to pain. Her neurovascular status is intact. Radiographs are shown in Figures 14a and 14b. Appropriate treatment should include
Explanation
REFERENCES: Hotchkiss RN: Displaced fractures of the radial head: Internal fixation or excision? J Am Acad Orthop Surg 1997;5:1-10.
Beredjiklian PK, Nalbantoglu U, Potter HG, et al: Prosthetic radial head components and proximal radial morphology: A mismatch. J Shoulder Elbow Surg 1999;8:471-475.
Question 21
Following resection of malignant tumors, complications related to endoprosthetic reconstruction are most common in what anatomic location?
Explanation
REFERENCE: Horowitz SM, Glasser DB, Lane JM, Healey JH: Prosthetic and extremity survivorship after limb salvage for sarcoma: How long do the reconstructions last? Clin Orthop 1993;293:280-286.
Question 22
A 65-year-old man has had “catching” in front of his knee since he had a total knee arthroplasty 9 months ago. Examination reveals a palpable and audible snap in the anterior aspect of the knee at about 40 degrees of flexion as the knee is being actively extended. A radiograph of the prosthetic knee will most likely show
Explanation
Pathologically, the clunk is produced by a suprapatellar fibrous nodule seen superior to the patellar component at re-operation. This nodule has been seen to catch in the intercondylar notch in primarily first generation TKAs. Current component designs have decreased this phenomenon through better engineering of femoral components. Treatment is by arthroscopic debridement or open arthroplasty resection. The nodule may be recurrent.
Question 23
A well-developed college football player reports swelling and a heaviness in the arm after lifting weights. Examination reveals that distal pulses are normal and equal in both arms. A venogram is shown in Figure 13. What is the most likely cause of this condition?
Explanation
REFERENCES: Angle N, Gelabert HA, Farooq MM, et al: Safety and efficacy of early surgical decompression of the thoracic outlet for Paget-Schroetter syndrome. Ann Vasc Surg 2001;15:37-42.
Azakie A, McElhinney DB, Thompson RW, et al: Surgical management of subclavian-vein effort thrombosis as a result of thoracic outlet compression. J Vasc Surg 1998;28:777-786.
Question 24
In infantile idiopathic scoliosis, which of the following factors suggests progression? Review Topic
Explanation
Question 25
Figures below show the radiographs, MRI, and MR arthrogram obtained from a 25-year-old collegiate soccer player who has new-onset left groin pain. He played competitive soccer from a young age and has competed or practiced 5 to 6 times per week since the age of 10. He denies any specific hip injury that necessitated treatment, but his trainer contends that he had a groin pull. He reports groin pain with passive flexion and internal rotation of the left hip, and his hip has less internal rotation than his asymptomatic right hip. He is otherwise healthy. What is the primary cause of a cam deformity?
Explanation
Question 26
Figures 38a and 38b
Explanation
Inversion of the ankle can cause various injuries about the foot and ankle, all via the same mechanism. Fifth metatarsal base avulsion (Figure 35) fractures can be treated with use of a walking boot until pain subsides. Jones fractures (Figure 36) can be treated with surgical or nonsurgical treatment, although young, active patients are perhaps better treated with ORIF, which can decrease disability time. Treatment of an anterior process calcaneus fracture (Figure 37) is similar to that for a fifth metatarsal base avulsion fracture. Figures 38a and 38b show a calcaneal fracture-dislocation, which necessitates ORIF.
RECOMMENDED READINGS
Schepers T, Backes M, Schep NW, Carel Goslings J, Luitse JS. Functional outcome following a locked fracture-dislocation of the calcaneus. Int Orthop. 2013 Sep;37(9):1833-8. PubMed PMID: 23959223. View Abstract at PubMed
Polzer H, Polzer S, Mutschler W, Prall WC. Acute fractures to the proximal fifth metatarsal bone: development of classification and treatment recommendations based on the current evidence. Injury. 2012 Oct;43(10):1626-32. doi: 10.1016/j.injury.2012.03.010. Epub 2012 Mar 30. Review. PubMed PMID: 22465516. View Abstract at PubMed
Roche AJ, Calder JD. Treatment and return to sport following a Jones fracture of the fifth metatarsal: a systematic review. Knee Surg Sports Traumatol Arthrosc. 2013 Jun;21(6):1307-15. doi: 10.1007/s00167-012-2138-8. Epub 2012 Sep 6. Review. PubMed PMID: 22956165. View Abstract at PubMed
Berkowitz MJ, Kim DH. Process and tubercle fractures of the hindfoot. J Am Acad Orthop Surg. 2005 Dec;13(8):492-502. Review. PubMed PMID: 16330511. View Abstract at PubMed
Question 27
Figures 16a and 16b are the radiograph and MR image of a 15-year-old dance athlete with 2 weeks of pain at the left distal femur, a limp, and an inability to dance. Knee motion is 0 to 135 degrees with minimal pain and there is no effusion. Her temperature is 37.0°C, WBC is 12000 /µL (rr, 4500-11000 /µL), CRP is 0.8 mg/L (rr, 0.08-3.1 mg/L), and ESR is 21 mm/h (rr, 0-20 mm/h).
Explanation
Figures 14a through 14e show a 13-year-old boy with osteomyelitis of the distal tibia and a large subperiosteal abscess. The patient has failed treatment with IV ceftriaxone, and methicillin-resistant Staphylococcus aureus infection is likely. Aspiration, cultures, irrigation and debridement, IV vancomycin, an infectious disease consult, and an evaluation for possible deep vein thrombosis is prudent initial treatment. Figure 15a through 15c show a 7-year-old girl who sustained a deer tick bite while vacationing in Connecticut. She has Lyme arthritis and a Lyme “bulls-eye” rash on the same leg. Aspiration, cultures, Lyme serology, and oral amoxicillin for 30 days is prudent initial treatment. Figures 16a and 16b are the radiograph and MR image of a 15-year-old dance athlete with a probable minor fracture via a benign cyst of the distal femur. The geographic cyst may be a nonossifying fibroma, eosinophilic granuloma, Brodie abscess, or simple bone cyst. Biopsy, culture, curettage and bone graft, and possible internal fixation is reasonable initial treatment.
Question 28
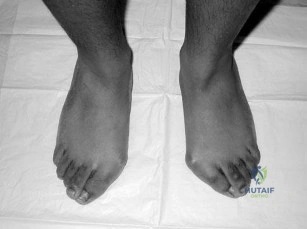
Figures 14a and 14b show the clinical photographs of a patient who was stranded in a subzero region for several days. The photographs were taken the morning after arrival in the hospital. The patient is otherwise healthy and fit, and takes no medication. He has no clinical signs of sepsis. He reports burning pain and tingling in both feet. What is the best treatment?
Explanation
REFERENCES: McAdams TR, Swenson DR, Miller RA: Frostbite: An orthopedic perspective.
Am J Orthop 1999;28:21-26.
Taylor MS: Cold weather injuries during peacetime military training. Milit Med 1992;157:602-604.
Question 29
A 20-year-old woman with a history of subtotal meniscectomy has a painful knee. What associated condition is a contraindication to proceeding with a meniscal allograft?
Explanation
REFERENCE: Koval KJ (ed): Orthopaedic Knowledge Update 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, p 499.
Question 30
The use of elevated rim acetabular liners and long femoral necks may result in
Explanation
REFERENCES: Cobb TK, Morrey BF, Ilstrup DM: The elevated rim acetabular liner in total hip arthroplasty: Relationship to postoperative dislocation. J Bone Joint Surg Am 1996;78:80-86.
Urquhart AG, D’Lima DD, Venn-Watson E, Colwell CW Jr, Walker RH: Polyethylene wear after total hip arthroplasty: The effect of a modular femoral head with an extended flange-reinforced neck. J Bone Joint Surg Am 1998;80:1641-1647.
Question 31
A patient sustains a comminuted calcaneus fracture. Three months after the injury the patient complains of shoewear problems secondary to clawing of the lesser toes. What is the most likely explanation for this deformity?

Explanation
Myerson reported 3/43 patients in his series below had chronic foot compartment syndrome. There are 9 compartments in the foot: (1) medial, (2) superficial, (3) lateral, (4) adductor, (5-8) four interossei, and (9) calcaneal. The plantar fascia limits the space available for hematoma and swelling, causing damage to the intrinsic flexors of the foot (particularly the lumbricals and interossei), resulting in clawtoes.
Question 32
A 32-year-old patient reports progressively increasing pain and stiffness after undergoing arthroscopic shoulder stabilization 1 year ago. The stabilization procedure was a Bankart repair with anchor fixation and supplemented with the heat probe. Radiographs are shown in Figures 45a and 45b. What is the most likely diagnosis?
Explanation
REFERENCES: Levine WN, Clark AM Jr, D’Alessandro DF, et al: Chondrolysis following arthroscopic thermal capsulorrhaphy to treat shoulder instability: A report of two cases. J Bone Joint Surg Am 2005;87:616-621.
Petty DH, Jazrawi LM, Estrada LS, et al: Glenohumeral chondrolysis after shoulder arthroscopy: Case reports and review of the literature. Am J Sports Med 2004;32:509-515.
Question 33
A 78-year-old man with ankylosing spondylitis sustains a minor fall. Shortly afterward he experiences sudden worsening of his chronic back pain and is brought to the emergency department by his caregiver. Radiographs and a CT scan of the spine do not show a clear fracture. What is the most appropriate next step?
Explanation
Patients with ankylosing spondylitis are at high risk for occult fractures after low-energy injuries. Although radiographs and a CT scan do not demonstrate a spinal fracture in this patient, high risk for an unstable occult fracture necessitates further imaging with MRI to ensure that no fractures are missed. Although a CT scan is typically the primary imaging modality for workup of spine injuries in similar patients, CT and MRI complement each other and each detects fractures that are missed using the other modality. A CT myelogram might detect cord or root compression but would not aid in the diagnosis of an occult fracture. Nonsteroidal anti-inflammatory drugs are first-line treatment for idiopathic low-back pain. In a patient with ankylosing spondylitis at high risk for fracture, further workup is needed to rule out an occult fracture. Flexion and extension radiographs of the spine are inferior to MRI for evaluating occult fractures and ligamentous injuries. The primary concern for this patient remains an unstable spinal fracture, which necessitates an MRI of the spine before initiating a workup for other possible causes of his back pain.
RECOMMENDED READINGS
Duane TM, Cross J, Scarcella N, Wolfe LG, Mayglothling J, Aboutanos MB, Whelan JF, Malhotra AK, Ivatury RR. Flexion-extension cervical spine plain films compared with MRI in the diagnosis of ligamentous injury. Am Surg. 2010 Jun;76(6):595-8. PubMed PMID: 20583514. View Abstract at PubMed
Hitchon PW, From AM, Brenton MD, Glaser JA, Torner JC. Fractures of the thoracolumbar spine complicating ankylosing spondylitis. J Neurosurg. 2002 Sep;97(2 Suppl):218-22. PubMed PMID: 12296682. View Abstract at PubMed
Koivikko MP, Koskinen SK. MRI of cervical spine injuries complicating ankylosing spondylitis. Skeletal Radiol. 2008 Sep;37(9):813-9. doi: 10.1007/s00256-008-0484-x. Epub 2008 Apr
Question 34
A 10-year-old boy has a painful, swollen knee after falling off his bicycle. Examination reveals no other injuries. Radiographs are shown in Figures 35a and 35b. Initial management of this fracture should consist of
Explanation
REFERENCES: Meyers MH, McKeever FM: Fractures of the intercondylar eminence of the tibia. J Bone Joint Surg Am 1970;52:1677-1684.
Wiley JJ, Baxter MP: Tibial spine fractures in children. Clin Orthop 1990;255:54-60
Janarv PM, Westblad P, Johansson C, Hirsch G: Long-term follow-up of anterior tibial spine fractures in children. J Pediatr Orthop 1995;15:63-68.
Kuhn JE, Sailer MJ, Sterett WI, Hawkins RJ: Arthroscopic technique for the treatment of tibial spine fractures in the skeletally immature patient. J Ortho Tech 1995;3:7-12.
Question 35
Six months later, the patient’s fracture has healed and a CT scan to further evaluate the physis is performed (Video 85). Based on these findings, how should you advise the family?
Explanation
The hypertrophic zone is the weakest biomechanical zone of the physis and is most likely to fracture. The deep peroneal nerve supplies motor innervation to the ankle and toe
dorsiflexors (anterior compartment) and the first web space, which, in this history, have deficits. The superficial peroneal nerve supplies sensation to the dorsum of the foot and motor to the lateral compartment peroneal musculature (ankle evertors), which also has deficits. The injury must involve both peroneal branches (the common peroneal nerve). Because sensation to the sole of the foot and toe/ankle plantar flexion is intact, the tibial nerve is intact.
Because the nerve was visualized intact, a neuropraxia is the most likely type of nerve injury. This should recover in time and does not necessitate urgent exploration. In pediatric patients, an advancing Tinel sign and partial nerve recovery by 3 months is expected and can be followed clinically. If there is no sign of nerve recovery, an electromyogram should be ordered with consideration for nerve exploration if there is no sign of reinnervation. There is no sign of compartment syndrome because the patient has an unchanged neurologic deficit, is comfortable, and has no pain with passive range of motion.
These injuries are associated with a very high rate of growth arrest (up to 80% in some studies). The CT scan shows an asymmetric growth arrest, which suggests angulation through the distal femur.
Question 36
Figures 191a and 191b are the radiographs of an 18-year-old man who had an ankle fracture requiring open reduction and internal fixation 2 years ago. He has a progressive symptomatic ankle deformity.Surgical intervention should consist of
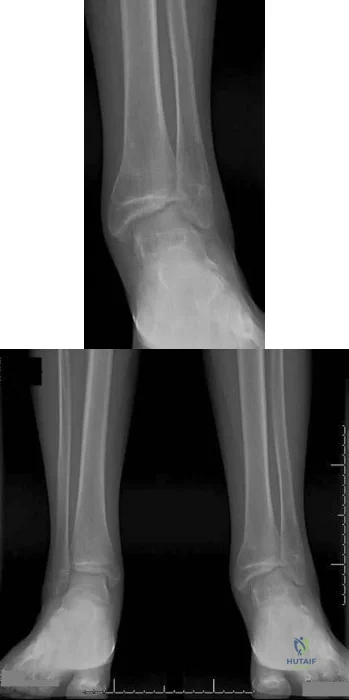
Explanation
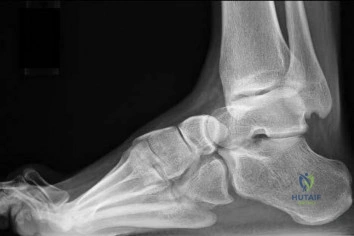
Question 37
Figure below shows the radiograph obtained from a 76-year-old woman who has sharp pain in her groin, thigh, and buttocks that worsens with activity. She has been dealing with this pain for more than a year but is otherwise healthy. Recently, she has begun to notice night pain. The pain no longer responds to NSAIDs. She would like to be able to dance at her daughter's wedding in 4 months and wonders how best to proceed. What is the best next step?
Explanation
The next best course of action is total hip arthroplasty. The patient is an otherwise healthy woman requesting pain relief and expresses a desire to be dancing in 4 months. She has had more than 6 months of symptoms that are classic hip osteoarthritis symptoms, with pain in the groin and thigh. Severe osteoarthritis is seen in the radiograph as well. NSAIDs are no longer working. Given the objective findings, the subjective reports, and the duration of symptoms, this patient merits surgery. Consideration for steroid injection is reasonable, but given her desire to be dancing in 4 months, an injection would increase her risk of infection if total hip arthroplasty were to be performed within 3 months of the
injection.
Question 38
A 10-year-old boy who plays baseball reports acute pain after throwing a softball from the outfield to second base. A radiograph is shown in Figure 26. Management should consist of
Explanation
REFERENCE: Yandow SM, Lundeen GA, Scott SM, Coffin C: Autogenic bone marrow injections as a treatment for simple bone cyst. J Pediatr Orthop 1998;18:616-620.
Question 39
A 20-year-old male military recruit reports a 5-day history of progressive deep groin pain that is made worse with weight-bearing activities and running. His initial coronal T2-weighted MRI scan is shown in Figure 75. His initial treatment should consist of which of the following? Review Topic

Explanation
Question 40
Which of the following long bone fracture patterns occurs after a pure bending force is exerted to the bone?
Explanation
REFERENCES: Tencer AF, Johnson KD: Biomechanics in Orthopaedic Trauma: Bone Fracture and Fixation. Philadelphia, PA, JB Lippincott, 1994.
Gonza ER: Biomechanical long bone injuries, in Gonza ER, Harrington IJ (eds): Biomechanics of Musculoskeletal Injury. Baltimore, MD, Williams & Wilkins, 1982, pp 1-30.
Simon SR (ed): Orthopaedic Basic Science. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1994, p 297.
Question 41
A 19-year-old man sustains a low-velocity gunshot wound to the forearm. What factor most strongly correlates with the development of compartment syndrome after this injury?
Explanation
REFERENCES: Moed BR, Fakhouri AJ: Compartment syndrome after low-velocity gunshot wounds to the forearm. J Orthop Trauma 1991;5:134-137.
Hahn M, Strauss E, Yang EC: Gunshot wounds to the forearm. Orthop Clin North Am 1995;26:85-93.
Question 42
A 35-year-old man is brought to the emergency department following a motorcycle accident. He is breathing spontaneously and has a systolic blood pressure of 80 mm Hg, a pulse rate of 120/min, and a temperature of 98.6° F (37° C). Examination suggests an unstable pelvic fracture; AP radiographs confirm an open book injury with vertical displacement on the left side. Ultrasound evaluation of the abdomen is negative. Despite administration of 4 L of normal saline solution, he still has a systolic pressure of 90 mm Hg and a pulse rate of 110. Urine output has been about 20 mL since arrival 35 minutes ago. What is the next best course of action?
Explanation
REFERENCE: Mayo K, Kellam JK: Pelvic ring disruptions, in Browner BD (ed): Skeletal Trauma, ed 3. Philadelphia, PA, WB Saunders, 2003, pp 1052-1108.
Question 43
A 40-year-old man who is a manual laborer has had 3 years of worsening medial-sided left knee pain that has inhibited his ability to work. He reports undergoing a left subtotal medial meniscectomy 10 years ago. He has been treated with nonsteroidal anti-inflammatory drugs and two different corticosteroids, with the most recent injection given 1 month ago. Each injection provided him with a few weeks of pain control. His medical history is unremarkable, and he has smoked 20 cigarettes per day for the last 15 years. His BMI is 22. On examination, he has varus alignment of the involved leg and medial joint line tenderness and no lateral or patellofemoral pain. His knee range of motion is 3° shy of full extension to 130° of flexion. He has negative Lachman and posterior drawer test results. He demonstrates no lateral thrust with ambulation. What is the most appropriate next step in treatment?
Explanation
Question 44
After sustaining a muscle contusion injury, prolonged immobilization leads to Review Topic
Explanation
Question 45
In Charcot-Marie-Tooth disease a progressive deformity develops in the foot. Which functional muscles predominate in deformity formation?
Explanation
REFERENCE: Herring JA (ed): Tachjians Pediatric Orthopedics, ed 3. Philadelphia, PA,
WB Saunders, 2002, vol 2, p 984.
Question 46
A 56-year-old man with poorly controlled diabetes mellitus has rapidly developing and advancing erythema, warmth and swelling with bullae formation on the left lower extremity. These findings appear to be advancing proximally several millimeters per hour. Culture results are most likely to reveal
Explanation
the diagnosis is confirmed and an extensive debridement should be performed. The Laboratory Risk Indicator for Necrotizing Fasciitis (LRINEC) score can be utilized to risk stratify people who have signs of cellulitis and determine the likelihood of necrotizing fasciitis being present. It uses six serologic measures, including C-reactive protein, total white blood cell count, hemoglobin, sodium, creatinine and glucose.
Polymicrobial synergistic infection was the most common cause of necrotizing fasciitis (48 patients; 53.9%) with streptococci and enterobacteriaceae being the most common isolates. Group-A streptococcus was the most common cause of monomicrobial necrotizing fasciitis. The most common associated comorbidity was diabetes mellitus (63 patients; 70.8%).
Question 47
What is the primary role of superficial zone protein (SZP) in articular cartilage?
Explanation
REFERENCES: Hlavacek M: The influence of the acetabular labrum seal, intact articular superficial zone and synovial fluid thixotropy on squeeze-film lubrication of a spherical synovial joint. J Biomech 2002;35:1325-1335.
Jay GD, Tantravahi U, Britt DE, et al: Homology of lubricin and superficial zone protein (SZP): Products of megakaryocyte stimulating factor (MSF) gene expression by human synovial fibroblasts and articular chondrocytes localized to chromosome 1q25. J Orthop Res 2001;19:677-687.
Question 48
Which of the following prophylactic regimens for the prevention of deep venous thrombosis after knee arthroplasty has received a grade 1A recommendation in favor of its use from the American College of Chest Physicians (ACCP) in the 2004 guidelines?
Explanation
REFERENCE: Geerts WH, Pineo GF, Heit JA, et al: Prevention of venous thromboembolism: The seventh ACCP Conference on antithrombotic and thrombolytic therapy. Chest 2004;126:338S-400S.
Question 49
Figure 36 shows the radiograph of a patient who has hip pain and is unable to ambulate. What is the most appropriate management for this patient?
Explanation
REFERENCES: Duncan CP, Masri BA: Fractures of the femur after hip replacement. Instr Course Lect 1995;44:293-304.
Parvizi J, Rapuri VR, Purtill JJ, et al: Treatment protocol proximal femoral periprosthetic fractures. J Bone Joint Surg Am 2004;86:8-16.
Question 50
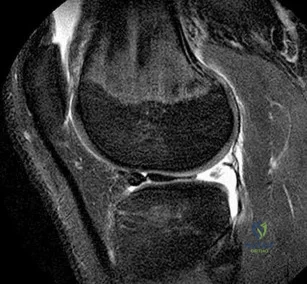
A 34-year-old woman who is a professional skier (Figure 42)
Explanation
Question 51
Figures 54a and 54b are the radiographs of a 23-year-old man who fell from a height and sustained an isolated injury to his right leg. Which of the following is a useful surgical technique to optimize alignment during intramedullary nailing?
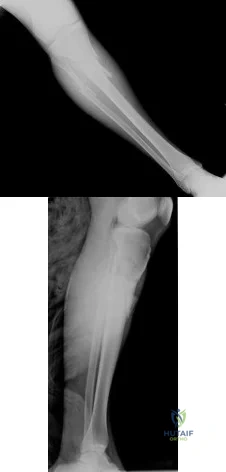
Explanation
(SBQ12TR.65) A patient falls and sustains the isolated injury seen in Figures A and
B. The surgical plan includes open reduction and internal fixation with a small mini-fragment plate using a direct lateral approach. During the approach, the forearm was placed in a fully pronated position. What would be the correct position of the forearm during plate application?
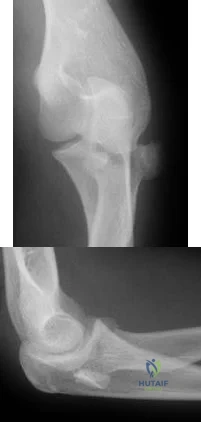
Full pronation
25 degrees pronation
Neutral
25 degrees supination
Full supination
Using the lateral approach (Kocher or Kaplan), the correct placement of the arm should be in a neutral position so that the plate can be placed on the bare area of the proximal radius.
Displaced radial head fractures with less than 3 fragments can be amendable to open reduction internal fixation. The methods of fixation include buried or headless screws, if placed at the articular surface, or posterolateral plating, if placed in the bare area. The safe zone for plating is located at a 90-110 arc from the radial styloid to Lister's tubercle with the arm in neutral rotation. This position helps to avoid impingement of ulna against the plate with forearm rotation. It should be noted that during the approach, that the forearm should be fully pronated to avoid injury to the posterior interosseous nerve.
Mathew et al. reviewed the concepts of terrible triad injuries of the elbow. Radial
head fractures are treated conservatively when there is an isolated minimally displaced (less than 2mm) fracture with no mechanical block to motion. Open reduction internal fixation is used for Mason II or III fractures with < 3 fragments. Radial head replacement is considered for comminuted fractures (Mason Type III) with 3 or more fragments.
Cheung et al. reviewed the surgical approaches to the elbow. The lateral approach (Kocher or Kaplan) is most commonly used with these injuries. The Kocher approach utilizes the intramuscular plane between anconeus and extensor carpi ulnaris. Kaplan utilizes the plane between extensor digitorum commons and extensor carpi radialis brevis.
Figure A and B show AP and lateral radiographs of the left elbow. There is a displaced radial head fracture. Illustration A shows a schematic diagram of the radial head "safe zone" between the radial styloid to Lister's tubercle.
Incorrect Answers:
Question 52
Figure 46 shows the AP radiograph of an active 80-year-old patient with an acetabular fracture. The fracture was initially managed nonsurgically; however, the patient is now scheduled to undergo total hip arthroplasty. What is the treatment of choice for the contained acetabular bone defect?
Explanation
REFERENCES: Mears DC: Surgical treatment of acetabular fractures in elderly patients with osteoporotic bone. J Am Acad Orthop Surg 1999;7:128-141.
Bellabarba C, Berger RA, Bentley CD, et al: Cementless acetabular reconstruction after acetabular fracture. J Bone Joint Surg Am 2001;83:868-876.
Question 53
A 20-year-old man has a large soft-tissue mass behind his knee. MRI scans are shown in Figures 10a through 10c. Figure 10d shows a clinical photograph of his chest. The patient’s condition is most likely a result of a defect in what gene?
Explanation
REFERENCES: Theos A, Korf BR, American College of Physicians, et al: Pathophysiology of neurofibromatosis Type 1. Ann Intern Med 2006;144:842-849.
Menendez LR: Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002.
Question 54
A previously healthy 29-year-old man reports a 2-day history of severe atraumatic lower back pain. He denies any bowel or bladder difficulties and no constitutional signs. Examination is consistent with mechanical back pain. No focal neurologic deficits or pathologic reflexes are noted. What is the most appropriate management?
Explanation
REFERENCES: Miller P, Kendrick D, Bentley E, et al: Cost effectiveness of lumbar spine radiographs in primary care patients with low back pain. Spine 2002;27:2291-2297.
Wong DA, Transfeldt E: Macnab’s Backache, ed 4. Philadelphia, PA, Lippincott Williams and Wilkins 2007, pp 298-338.
Question 55
Figure 3 shows the AP radiograph of a patient with diabetes mellitus who has knee pain. A semiconstrained knee prosthesis was used in this patient to prevent which of the following complications?
Explanation
REFERENCES: Parvizi J, Marrs J, Morrey BF: Total knee arthroplasty for neuropathic (Charcot) joints. Clin Orthop 2003;416:145-150.
Kim YH, Kim JS, Oh SW: Total knee arthroplasty in neuropathic arthropathy. J Bone Joint
Surg Br 2002;84:216-219.
Question 56
Figures below demonstrate the radiographs obtained from a 35-year-old woman with end-stage debilitating osteoarthritis of the right hip. She is contemplating total hip arthroplasty (THA). She has a history of right hip dysplasia and underwent hip osteotomy as an adolescent. Over the years, nonsurgical treatment, including weight loss, activity modifications, and intra-articular injections, has failed. Her infection work-up reveals laboratory findings within defined limits. A further work-up reveals elevations in serum cobalt and chromium levels and fluid collections surrounding the hip on MRI with MARS. Revision THA is recommended. The most common complication following revision of a failed metal-on-metal hip arthroplasty is
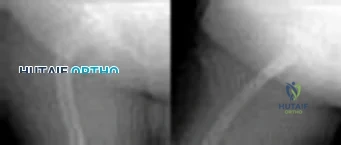
Explanation
Question 57
A 16-year-old boy has abdominal and back pain after being involved in a high-velocity head-on motor vehicle accident. He was restrained in the rear of the automobile by a lap belt only. A radiograph and CT scan are shown in Figure 47. The patient has no other injuries. Optimal management should include
Explanation
REFERENCES: Greenwald TA, Mann DC: Pediatric seatbelt injuries: Diagnosis and treatment of lumbar flexion-distraction injuries. Paraplegia 1994;32:743-751.
Glassman SD, Johnson JR, Holt RT: Seatbelt injuries in children. J Trauma 1992;33:882-886.
Raney EM, Bennett JT: Pediatric Chance fracture. Spine 1992;17:1522-1524.
Question 58
During total hip arthroplasty, what characteristic of irradiated (10 Mrad) and subsequently melted highly cross-linked polyethylene should provide a more wear-resistant construct than traditional gamma- irradiated (2.5-4 Mrad)-in-air polyethylene mated with the same head?
Explanation
Highly cross-linked polyethylene makes material resistant to adhesive wear. Abrasive wear from third bodies does not decrease wear. The fatigue strength of such material is inferior to that of traditional polyethylene, and its resistance to creep is the same, if not lower, than that of traditional polyethylene.
Question 59
Factors contributing to an increased risk of hip fracture include reduced bone mineral density of the femoral neck, cognitive status of the individual, and
Explanation
Hayes and Myers noted that striking the ground in a stiff state with the trunk muscles contracted actually increased the peak impact force, whereas falling in a relaxed state actually reduced peak impact force. Flexion of the trunk at impact had no bearing on the impact force. Direction of the fall was important; falls to the side, not forward, were associated with an increased risk of hip fracture. Increased muscle activity about the hip is thought to be associated with spontaneous fractures of the hip and may actually account for up to 25% of hip fractures; however, it is not related to fractures resulting from a fall.
REFERENCE: Hayes WC, Myers ER: Biomechanical considerations of hip and spine fractures in osteoporotic bone, in Springfield D (ed): Instructional Course Lectures 46. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, pp 431-438.
Question 60
Which of the following best characterizes the injury shown in Figure 53? Review Topic
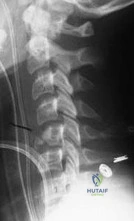
Explanation
Question 61
A patient who underwent primary total hip arthroplasty 7 years ago that resulted in excellent pain relief and a normal gait now reports pain and a limp. Postoperative and current AP radiographs are shown in Figures 2a and 2b. What is the most likely cause of the pathology seen?
Explanation
REFERENCES: Claus MC, Hopper RH, Engh CA: Fractures of the greater trochanter induced by osteolysis with the anatomic medullary locking prosthesis. J Arthroplasty 2002;17:706-712.
Heekin RD, Engh CA, Herzwurm MF: Fractures through cystic lesions of the greater trochanter: A cause of late pain after cementless total hip arthroplasty. J Arthroplasty 1996;11:757-760.
Question 62
The cavovarus deformity associated with Charcot-Marie-Tooth (CMT) disease is caused by which of the following?
Explanation
REFERENCES: Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 135-143.
Charcot-Marie-Tooth Disease (CMT) Penn State Hershey Medical Center.
www.hmc.psu.edu/healthinfo/c/cmt.htm
Question 63
What is the typical axial plane transverse angulation of the thoracic pedicles?
Explanation
starting point is more lateral. T2 angles about 15 degrees, and then the pedicles average about
5 to 7 degrees down to T10. At T11 and 12, the angulation is minimal.
REFERENCES: Weinstein L: Pediatric Spine Principles and Practice. New York, NY, Raven Press, 1994, pp 1659-1681.
Lenke LG, Orchowski J: Segmental posterior spinal instrumentation: Thoracic spine to sacrum, in Frymoyer JW, Wiesel SW (eds): The Adult and Pediatric Spine, ed 3. Philadelphia, PA, Lippincott Williams and Wilkins, 2004, pp 537-552.
Question 64
A 46-year-old man reports occasional squeaking of his hip 2 years after undergoing an uneventful total hip arthroplasty. History reveals no pain, physical examination cannot reproduce audible squeaking, and radiographs show appropriate implant position. What is the most appropriate management?
Explanation
Hopefully, with a better understanding of acoustic phenomena following ceramic total hip arthroplasty, this complication can be minimized.
REFERENCES: Yang CC, Kim RH, Dennis DA: The squeaking hip: A cause for concem-disagrees. Orthopedics
2007;30:739-742.
Walter WL, O’Toole GC, Walter WK, et al: Squeaking in ceramic-on-ceramic hips: The importance of acetabular component orientation. J Arthroplasty 2007;22:496-503.
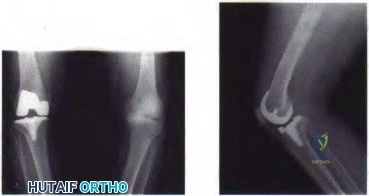
Figure 80a Figure 80b
Question 65
An active 47-year-old woman with rheumatoid arthritis reports forefoot pain and deformity and has difficulty with shoe wear. Examination reveals hallux valgus and claw toes. A radiograph is shown in Figure 10. What is the most appropriate surgical treatment?
Explanation
REFERENCES: Coughlin MJ: Arthritides, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 7. St Louis, MO, Mosby, 1999, p 572.
Abdo RV, Iorio LJ: Rheumatoid arthritis of the foot and ankle. J Am Acad Orthop Surg 1994;2:326-332.
Question 66
A 47-year-old woman with no history of trauma has had a painful, stiff shoulder for the past 3 months. Treatment consisting of subacromial injection and nonsteroidal anti-inflammatory drugs has been ineffective. Her active range of motion is painful and is limited to 90 degrees of abduction, 60 degrees of elevation, 30 degrees of external rotation, and internal rotation to the posterior superior iliac spine. Plain radiographs of the cervical spine and shoulder are normal. Management at this time should consist of
Explanation
Question 67
In rotator cuff tear arthropathy with pseudoparalysis, forward elevation of the humerus away from the body is prohibited because of
Explanation
Question 68
Which of the following methods most reliably detects mechanical loosening of the hip?
Explanation
REFERENCES: Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 455-492.
Miniaci A, Bailey WH, Bourne RB, McLaren AC, Rorabeck CH: Analysis of radionuclide arthrograms, radiographic arthrograms, and sequential plain radiographs in the assessment of painful hip arthroplasty. J Arthroplasty 1990;5:143-149.
Question 69
A 51-year-old woman with no preoperative neurologic deficit is undergoing elective anterior cervical diskectomy and fusion (ACDF) with plating and fusion for a C5-6 disk herniation with right-sided neck pain. Thirty minutes into the surgery the neurophysiologic monitoring shows a rapid drop and then loss of amplitude in the right cortical somatosensory-evoked potential waveform. All other waveforms remained normal and unchanged, including right-sided cervical (subcortical) and peripheral (Erb’s point), and those from the left-sided upper extremity and both lower extremities. What is the most likely cause of the change? Review Topic
Explanation
Question 70
A 50-year-old man with metastatic renal cell carcinoma has right hip pain. A radiograph and CT scan are shown in Figures 48a and 48b. The first step in management should consist of
Explanation
REFERENCES: Layalle I, Flandroy P, Trotteur G, Dondelinger RF: Arterial embolization of bone metastases: Is it worthwhile? J Belge Radiol 1998;81:223-225.
Chatziioannou AN, Johnson ME, Pneumaticos SG, Lawrence DD, Carrasco CH: Preoperative embolization of bone metastases from renal cell carcinoma. Eur Radiol 2000;10:593-596.
Question 71
A 20-year-old college athlete is seen for follow-up after sustaining an injury at football practice 2 days ago. He reports that he tackled a player and felt neck pain and numbness in both arms. The numbness resolved within seconds, but his neck remains painful and stiff. He denies any history of neck pain or injury. Examination reveals limited neck motion. The neurologic examination and radiographs are normal. MRI scans of the cervical spine are shown in Figure 34. During counseling, the patient, his family, and his coach should be informed that he has an acute cervical disk herniation and cannot play
Explanation
REFERENCES: Morganti C, Sweeney CA, Albanese SA, Burak C, Hosea T, Connolly PJ: Return to play after cervical spine injury. Spine 2001;26:1131-1136.
Vaccaro AR, Watkins B, Albert TJ, Pfaff WL, Klein GR, Silber JS: Cervical spine injuries in athletes: Current return-to-play criteria. Orthopedics 2001;24:699-705.
Question 72
Which of the following is most commonly associated with an open clavicular fracture?
Explanation
REFERENCE: Taitsman LA, Nork SE, Coles CP, et al: Open clavicle fractures and associated injuries. J Orthop Trauma 2006;20:396-399.
Question 73
The MRI scan of the shoulder shown in Figure 2 was performed with the arm in abduction and external rotation. The image reveals what condition?
Explanation
REFERENCES: Schickendantz MS, Ho CP, Keppler L, Shaw BD: MR imaging of the thrower’s shoulder: Internal impingement, latissimus dorsi/subscapularis strains, and related injuries. Magn Reson Imaging Clin N Am 1999;7:39-49.
Walch G, Boileau P, Noel E, et al: Impingement of the deep surface of the supraspinatus tendon on the posterosuperior glenoid rim: An arthroscopic study. J Shoulder Elbow Surg 1992;1:238-245.
McFarland EG, Hsu CY, Neira C, O’Neil O: Internal impingement of the shoulder: A clinical and arthroscopic analysis. J Shoulder Elbow Surg 1999;8:458-460.
Question 74
A 27-year-old man has neck pain after being involved in a motor vehicle accident. A lateral cervical radiograph is shown in Figure 21. What would be the most common neurologic finding?
Explanation
REFERENCES: Levine AM: Traumatic spondylolisthesis of the axis (Hangman’s fracture), in Levine AM, Eismont FJ, Garfin S, Zigler JE (eds): Spine Trauma. Philadelphia, PA, WB Saunders, 1998, pp 287-288.
Francis WR, Fielding JW, Hawkins RJ, Pepin J, Hensinger R: Traumatic spondylolisthesis of the axis. J Bone Joint Surg Br 1981;63:313-318.
Question 75
A healthy, active, independent 74-year-old woman fell and sustained the elbow injury shown in Figures 41a and 41b. Management should consist of
Explanation
REFERENCES: Frankle MA, Herscovici D Jr, DiPasquale TG, et al: A comparison of open reduction and internal fixation and primary total elbow arthroplasty in the treatment of intra-articular distal humerus fractures in women older than 65. J Orthop Trauma 2003;17:473-480.
Cobb TK, Morrey BF: Total elbow arthroplasty as primary treatment for distal humerus fractures in elderly patients. J Bone Joint Surg Am 1997;79:826-832.
Obremskey WT, Bhandari M, Dirschl DR, et al: Internal fixation versus arthroplasty of comminuted fractures of the distal humerus. J Orthop Trauma 2003;17:463-465.
Question 76
The standard Bankart lesion involves detachment of the labrum along with which of the following capsular ligaments? Review Topic
Explanation
Question 77
A 23-year-old male is involved in a motor vehicle accident and sustains a left open femur fracture, right open humeral shaft fracture, and an LC-II pelvic ring injury. Which of the following best describes the radiographic findings associated with this pelvic injury pattern using the Young-Burgess Classification system?

Explanation
Burgess et al discuss the effectiveness of a treatment protocol as determined by their pelvic injury classification and hemodynamic status. The injury classification system was based on lateral compression, anteroposterior compression, vertical shear, and combined mechanical injury types. They found that their classification-based treatment protocols reduce the morbidity and mortality related to pelvic ring disruption.
Tile discusses acute pelvic trauma and his classification system for pelvic injuries (ie. Types A, B, and C). He states that any classification system must be seen only as a general guide to treatment, and that the management of each patient requires careful, individualized decision making.
Incorrect
2:
This
describes
an
APC-II
injury
3:
This
describes
an
APC-III
injury
4:
This
describes
and
LC-I
injury
Question 78
A 72-year-old woman with rheumatoid arthritis who underwent primary total knee arthroplasty 2 years ago has had diffuse knee pain that developed shortly after the surgery. The patient has difficulty with stair descent and arising from chairs. Evaluation for infection is negative. AP and lateral radiographs are shown in Figure 26. Management should now consist of
Explanation
REFERENCES: Pagnano MW, Hanssen AD, Lewallen DG, Stuart MJ: Flexion instability after primary posterior cruciate retaining total knee arthroplasty. Clin Orthop 1998;356:39-46.
Fehring TK, Valadie AL: Knee instability after total knee arthroplasty. Clin Orthop 1994;299:157-162.
Fehring TK, Odum S, Griffin WL, Mason B, Nadaud M: Early failures of total knee arthroplasty. Clin Orthop 2001;392:315-318.
Question 79
Which of the following statements best describes the instantaneous axis of rotation (IAR) for the functional spinal unit? Review Topic
Explanation
Question 80
Which of the following ligaments are the primary static restraints to inferior translation of the arm when the shoulder is in 0 degrees of abduction and neutral rotation?
Explanation
REFERENCES: Warner JJ, Deng XH, Warren RF, et al: Static capsuloligamentous restraints to superior-inferior translation of the glenohumeral joint. Am J Sports Med 1992;20:675-685.
Jost B, Koch PP, Gerber C: Anatomy and function of the rotator interval. J Shoulder Elbow Surg 2000;9:336-341.
Question 81
When performing knee arthroplasty, which of the following procedures provides the most consistent fixation for the tibial component?
Explanation
REFERENCE: Vaccaro AR (ed): Orthopaedic Knowledge Update 8. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2005, pp 457-468.
Question 82
Figure 23 shows the postoperative radiograph of a patient who underwent an anterior cruciate ligament (ACL) reconstruction (with bone-patella tendon-bone autograft) that failed. He initially had loss of flexion postoperatively. What is the most likely cause of this failure?
Explanation
REFERENCES: Fu FH, Bennett CH, Latterman C, et al: Current trends in anterior cruciate ligament reconstruction: Part 1. Biology and biomechanics of reconstruction. Am J Sports Med 1999;27:821-830.
Fu FH, Bennett CH, Ma CB, et al: Current trends in anterior cruciate ligament reconstruction: Part II. Operative procedures and clinical correlations. Am J Sports Med 2000;28:124-130.
Question 83
A 57-year-old man involved in a motor vehicle accident sustains an injury to his right shoulder. A spot AP radiograph is shown in Figure 34. What is the next most appropriate step in the orthopaedic management of this patient? Review Topic
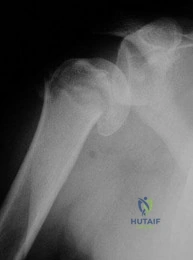
Explanation
Question 84
Which of the following lumbar disk components has the highest tensile modulus to resist torsional, axial, and tensile loads?
Explanation
REFERENCE: Rhee JM, Schaufele M, Abdu WA: Radiculopathy and the herniated lumbar disc: Controversies regarding pathophysiology and management. J Bone Joint Surg Am 2006;88:2070-2080.
Question 85
- A patient is in respiratory distress as a result of a high-speed motor vehicle accident. After emergent intubation, the arterial blood is poorly oxygenated, and examination shows left-sided tracheal deviation, absence of breath sounds on the right side and tympany on percussion over the right side of the chest. Management should include
Explanation
Question 86
What complication is frequently associated with the Weil lesser metatarsal osteotomy (distal, oblique) in the treatment of claw toe deformities?
Explanation
REFERENCES: Trnka HJ, Nyska M, Parks BG, et al: Dorsiflexion contracture after the Weil osteotomy: Results of cadaver study and three-dimensional analysis. Foot Ankle Int
2001;22:47-50.
Trnka HJ, Muhlbauer M, Zettl R, et al: Comparison of the results of the Weil and Helal osteotomies for the treatment of metatarsalgia secondary to dislocation of the lesser metatarsophalangeal joints. Foot Ankle Int 1999;20:72-79.
Question 87
An active 49-year-old woman who sustained a diaphyseal fracture of the clavicle 8 months ago now reports persistent shoulder pain with daily activities. An AP radiograph is shown in Figure 8. Management should consist of
Explanation
shown some healing response with callus formation, but these techniques are not successful
in an atrophic nonunion. The preferred technique for achieving union is open reduction and internal fixation with bone graft. Percutaneous fixation has no role in treatment of nonunions
of the clavicle.
REFERENCES: Boyer MI, Axelrod TS: Atrophic nonunion of the clavicle: Treatment by compression plating, lag-screw fixation and bone graft. J Bone Joint Surg Br 1997;79:301-303.
Simpson NS, Jupiter JB: Clavicular nonunion and malunion: Evaluation and surgical management. J Am Acad Orthop Surg 1996;4:1-8.
Question 88
A healthy, active 72-year-old man trips and falls, landing on his left hip 10 weeks after an uncomplicated left primary uncemented total hip replacement. A radiograph taken 6 weeks after surgery and before the fall is shown in Figure 1. A radiograph taken after the fall is shown in Figure 2. He is unable to bear weight and is brought to the emergency department. Examination reveals a slightly shortened left lower extremity and some mild ecchymosis just distal to the left greater trochanteric region, but his skin is intact, without abrasions or lacerations. What is the most appropriate treatment?
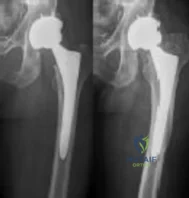
Explanation
This patient has a periprosthetic femoral fracture with a loose femoral stem and normal femoral bone stock, representing a Vancouver type B2 fracture. The most appropriate treatment is fixation of the fracture, along with revision of the stem. Considering his age, bone quality, and activity level, a longer uncemented stem is most predictable. Although a cylindrical stem may also be used, the fluted stem option is the only uncemented choice listed and is the most appropriate option. A cemented stem is a poorer choice because it is difficult to keep the cement out of the fracture site, which would pose a risk for nonunion at the fracture. Also, overall poorer results have been associated with long cemented stems in healthy, active people. Surgery does not need to be delayed to allow the ecchymosis to resolve, and simple open reduction and fixation does not address the loose stem.
Question 89
Figures 30a through 30c show the CT scans and standing lateral radiograph of a 30-year-old woman who was injured in a fall while snowboarding. She is neurologically intact in the lower extremities and has normal rectal tone and sensation. She has tenderness at the thoracolumbar junction but no ecchymosis or palpable defect. Mobilization in a thoracolumbosacral orthosis for this patient has been proven to result in which of the following clinical outcomes? Review Topic
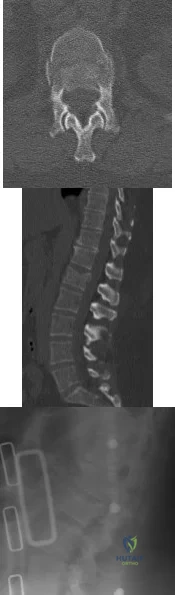
Explanation
Question 90
Which of the following findings is the best radiographic indicator of segmental instability at L4-L5?
Explanation
11° of angulation is considered instability criteria for the cervical spine. Internal disk disruption does not denote instability.
REFERENCES: Boden SD, Wiesel SW: Lumbosacral segmental motion in normal individuals. Have we been measuring instability properly? Spine 1990;15:571-576.
Garfin SR, Rauschning W: Spinal stenosis. Instr Course Lect 2001;50:145-152.
Question 91
-What is the most likely diagnosis for her condition?
Explanation
Streeter dysplasia or amniotic band syndrome is a congenital disorder caused by entrapment of fetal parts (usually a limb or digits) in fibrous amniotic bands in utero. It is associated with cleft lip or palate, terminal amputations, constriction bands, encephalocele, renal abnormalities, cardiac defects, hemihypertrophy, anterolateral bowing, tibial pseudarthrosis, and limb-length discrepancy. Clubfoot is seen in up to 25% of cases. Tight bands around the peroneal nerve that occur in 50% of children with
clubfeet can lead to nerve damage. This patient has chronic osteomyelitis resulting from pressure on the fifth metacarpal head in the presence of an insensate lateral foot. Traditional pinning in open clubfoot surgery does not breach the distal metatarsal. In an open procedure, releasing the abductor hallucis addresses forefoot abduction and is performed medially. The lateral release impacts the midfoot and hindfoot, but not lateral ray plantar flexion.
Question 92
A patient has a C6 spinal cord injury. Following stabilization of the spine, the patient should be advised that their expected maximum level of function
Explanation
Question 93
Figures 50a and 50b show the standing clinical photographs of a 12-year-old boy who has had increasing pain in the left foot for the past 9 months. He reports that the pain is activity related, aching in nature, and localized to the medial aspect of the midfoot and hindfoot. History reveals that he sustained a puncture wound located superior and posterior to the medial malleolus from a plate glass window 18 months ago. Examination reveals no restriction of ankle or subtalar motion, normal neurovascular status, no masses, and a well-healed 1.5-cm laceration posterior to the superior aspect of the medial malleolus. Inversion strength of the foot is decreased to grade 3/5. Radiographs of the foot show no bony abnormalities. Treatment should consist of
Explanation
REFERENCES: Mosca VS: Flexible flatfoot and skewfoot, in Drennan JC (ed): The Child’s Foot and Ankle. New York, NY, Raven Press, 1992, pp 355-376.
Myerson MS: Adult acquired flatfoot deformity: Treatment of dysfunction of the posterior tibial tendon, in Springfield DS (ed): Instructional Course Lectures 46. Rosemont, Ill, American Academy of Orthopaedic Surgeons, 1997, pp 393-405.
Question 94
A 25-year-old man is unresponsive at the scene of a high-speed motor vehicle accident and remains obtunded. Initial evaluation in the emergency department reveals a left-sided femoral shaft fracture and a right-sided humeral shaft fracture. The cervical spine remains immobilized in a semi-rigid cervical collar, and the initial AP and lateral radiographs obtained in the emergency department are unremarkable. What is the most appropriate management at this time?
Explanation
REFERENCES: Chiu WC, Haan JM, Cushing BM, et al: Ligamentous injuries of the cervical spine in unreliable blunt trauma patients: Incidence, evaluation, and outcome. J Trauma 2001;50:457-463.
Sanchez B, Waxman K, Jones T, et al: Cervical spine clearance in blunt trauma: Evaluation of a computed tomography-based protocol. J Trauma 2005;59:179-183.
Nunez D Jr: Value of complete cervical helical computed tomographic scanning in identifying cervical spine injury in the unevaluable blunt trauma patient with multiple injuries:
A prospective study. J Trauma 2000;48:988-989.
Question 95
A 25-year-old man reports wrist pain following a motorcycle accident. Examination reveals minimal swelling, slightly limited active range of motion, and point tenderness in the snuff box region. AP and oblique radiographs are shown in Figures 40a and 40b. Management should consist of
Explanation
REFERENCES: Amadio PC, Taleisnik J: Fractures of the carpal bone, in Green DP, Hotchkiss RN, Pederson WC (eds): Green’s Operative Hand Surgery, ed 4. Philadelphia, PA, 1999,
pp 809-823.
Rettig ME, Kozin SH, Cooney WP: Open reduction and internal fixation of acute displaced scaphoid waist fractures. J Hand Surg Am 2001;26:271-276.
Cooney WP, Dobyns JH, Linscheid RL: Fractures of the scaphoid: A rational approach to management. Clin Orthop 1980;149:90-97.
Szabo RM, Manske D: Displaced fractures of the scaphoid. Clin Orthop 1988;230:30-38.
Question 96
The anterolateral (Watson-Jones) approach to the hip exploits the intermuscular interval between the
Explanation
REFERENCES: Hoppenfeld S, deBoer P: Surgical Exposures in Orthopaedics: The Anatomic Approach. Philadelphia, PA, JB Lippincott, 1984, pp 316-332.
Crenshaw AH (ed): Campbell’s Operative Orthopedics, ed 7. St Louis, MO, CV Mosby, 1987,
p 63.
Question 97
A 25-year-old male polytrauma patient undergoes initial temporary external fixation for a femoral shaft fracture. He is converted to a femoral nail at 7 days. This management can be expected to result in
Explanation
REFERENCES: Harwood PJ, Giannoudis PV, Probst C, et al: The risk of local infective complications after damage control procedures for femoral shaft fracture. J Orthop Trauma 2006;20:181-189.
Roberts CS, Pape HC, Jones AL, et al: Damage control orthopaedics: Evolving concepts in the treatment of patients who have sustained orthopaedic trauma. Instr Course Lect
2005;54:447-462.
Question 98
A 17-year-old boy has had a mass in his right thigh for the past 6 months. He denies any history of trauma. Examination reveals that the mass is painless and firm. A radiograph and axial MRI scan are shown in Figures 49a and 49b. What is the most likely diagnosis?
Explanation
REFERENCE: Wold LA, et al: Osteochondroma: Atlas of Orthopaedic Pathology. Philadelphia, PA, WB Saunders, 1990, p 50.
Question 99
During head-on motor vehicle collisions occurring at highway speeds, airbag-protected individuals have a decreased rate (as compared to non-airbag protected individuals) of all of the following EXCEPT:

Explanation
Question 100
A 30-year-old man reports pain and weakness in his right arm. Examination reveals grade 4 strength in wrist flexion and elbow extension, decreased sensation over the middle finger, and decreased triceps reflex. These symptoms are most compatible with impingement on what spinal nerve root?
Explanation
REFERENCES: Hoppenfeld S: Physical Examination of the Spine and Extremities. Upper Saddle River, NJ, Prentice Hall, 1976, p 125.
Lauerman WC, Goldsmith ME: Spine, in Miller MD (ed): Review of Orthopaedics, ed 3. Philadelphia, PA, WB Saunders, 2000, pp 353-378.
