Orthopedic Board Review MCQs: Elbow, Foot, Trauma & Fracture | Part 23
Key Takeaway
This page offers Part 23 of a comprehensive Orthopedic Surgery board review, featuring 50 high-yield MCQs. Designed for orthopedic surgeons and residents preparing for OITE and AAOS certification exams, it covers Elbow, Foot, Fracture, and Trauma topics in interactive Study or Exam Modes.
Orthopedic Board Review MCQs: Elbow, Foot, Trauma & Fracture | Part 23
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 32-year-old woman sustained an injury to her left upper extremity in a motor vehicle accident. Examination reveals a 2-cm wound in the mid portion of the dorsal surface of the upper arm and deformities at the elbow and forearm; there are no other injuries. Her vital signs are stable, and she has a base deficit of minus 1 and a lactate level of less than 2. Radiographs are shown in Figures 9a and 9b. In addition to urgent debridement of the humeral shaft fracture, management should include
Explanation
REFERENCES: Solomon HB, Zadnik M, Eglseder WA: A review of outcomes in 18 patients with floating elbow. J Orthop Trauma 2003;17:563-570.
Pape HC, Hildebrand F, Pertschy S, et al: Changes in the management of femoral shaft fractures in polytrauma patients: From early total care to damage control orthopedic surgery. J Trauma 2002;53:452-461.
Question 2
A patient sustained the injuries shown in the radiographs and clinical photograph seen in Figures 10a through 10c. The neurovascular examination is normal. The first step in emergent management of the extremity injuries should consist of
Explanation
REFERENCES: Sahin V, Karakas ES, Aksu S, et al: Traumatic dislocation and fracture-dislocation of the hip: A long-term follow-up study. J Trauma 2003;54:520-529.
Moed BR, WillsonCarr SE, Watson JT: Results of operative treatment of fractures of the posterior wall of the acetabulum. J Bone Joint Surg Am 2002;84:752-758.
Question 3
Figure 11 shows the radiograph of a 3-year-old girl who sustained a proximal radius injury. Appropriate initial management should include
Explanation
REFERENCES: Leung AG, Peterson HA: Fractures of the proximal radial head and neck in children with emphasis on those that involve the articular cartilage. J Pediatr Orthop
2000;20:7-14.
Radomisli TE, Rosen AL: Controversies regarding radial neck fractures in children. Clin Orthop 1998;353:30-39.
Skaggs DL, Mirzayan R: The posterior fat pad sign in association with occult fracture of the elbow in children. J Bone Joint Surg Am 1999;81:1429-1433.
Gonzalez-Herranz P, Alvarez-Romera A, Burgos J, et al: Displaced radial neck fractures in children treated by closed intramedullary pinning (Metaizeau technique). J Pediatr Orthop 1997;17:325-331.
Question 4
Figures 12a and 12b show the radiographs of a 56-year-old man with diabetes mellitus who has had left foot swelling with no pain for the past several weeks. He denies any history of trauma. Examination reveals warmth, moderate swelling, no tenderness, and mild pes planus with standing. Pulses are palpable, and his sensory examination is grossly intact to light touch. Standing radiographs are shown in Figures 12c and 12d. What is the most likely diagnosis?
Explanation
REFERENCES: Brodsky JW: The diabetic foot, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 7. St Louis, MO, Mosby, 1999, pp 895-969.
Myerson MS: Diabetic neuroarthropathy, in Myerson MS (ed): Foot and Ankle Disorders. Philadelphia, PA, WB Saunders, 2000, pp 439-465.
Question 5
A 25-year-old student sustains the injury shown in Figures 13a through 13c after falling off a curb. Initial management should consist of
Explanation
REFERENCES: Rosenberg GA, Sterra JJ: Treatment strategies for acute fractures and nonunions of the proximal fifth metatarsal. J Am Acad Orthop Surg 2000;8:332-338.
Lawrence SJ, Botte MJ: Jones’ fracture and related fractures of the proximal fifth metatarsal. Foot Ankle 1993;14:358-365.
Question 6
What structure is most often injured in a volar proximal interphalangeal joint dislocation?
Explanation
REFERENCES: Doyle JR: Extensor tendons: Acute injuries, in Green DP, Hotchkiss RN (eds): Operative Hand Surgery, ed 3. New York, NY, Churchill Livingstone, 1993, p 1925.
Newport ML: Extensor tendon injuries in the hand. J Am Acad Orthop Surg 1997;5:59-66.
Question 7
What patient factor is predictive of better outcomes for surgical management of a displaced calcaneal fracture compared to nonsurgical management?
Explanation
REFERENCES: Howard JL, Buckley R, McCormack R, et al: Complications following management of displaced intra-articular calcaneal fractures: A prospective randomized trial comparing open reduction internal fixation with nonoperative management. J Orthop Trauma 2003;17:241-249.
Buckley R, Tough S, McCormack R, et al: Operative compared with nonoperative treatment of displaced intra-articular calcaneal fractures: A prospective, randomized, controlled multicenter trial. J Bone Joint Surg Am 2002;84:1733-1744.
Question 8
Figures 14a and 14b show the initial radiographs of an 18-year-old man who fell while snowboarding. Figures 14c and 14d show the radiographs obtained following closed reduction. Examination reveals that the elbow is stable with range of motion. Management should now consist of
Explanation
REFERENCES: Cohen MS, Hastings H II: Acute elbow dislocations: Evaluation and management. J Am Acad Orthop Surg 1998;6:15-23.
O’Driscoll SW: Elbow dislocations, in Morrey BF (ed): The Elbow and Its Disorders, ed 3. Philadelphia, PA, WB Saunders, 2000, pp 409-420.
Question 9
A 12-year-old boy sustains open comminuted midshaft tibial and fibular fractures while playing indoor soccer. The wound is grossly clean and measures 7 cm with some periosteal stripping. Antibiotics and tetanus toxoid are administered immediately in the emergency department. Following irrigation and debridement of the wound in the operating room, treatment should include
Explanation
REFERENCES: Jones BG, Duncan RD: Open tibial fractures in children under 13 years of age-10 years experience. Injury 2003;34:776-780.
Bartlett CS III, Weiner LS, Yang EC: Treatment of type II and type III open tibia fractures in children. J Orthop Trauma 1997;11:357-362.
Robertson P, Karol LA, Rab GT: Open fractures of the tibia and femur in children. J Pediatr Orthop 1996;16:621-626.
Cullen MC, Roy DR, Crawford AH, et al: Open fracture of the tibia in children. J Bone Joint Surg Am 1996;78:1039-1047.
Question 10
Which of the following is an advantage of unreamed nailing of the tibia compared to reamed nailing?
Explanation
REFERENCES: Larsen LB, Madsen JE, Hoiness PR, et al: Should insertion of intramedullary nails for tibial fractures be with or without reaming? A prospective, randomized study with 3.8 years’ follow-up. J Orthop Trauma 2004;18:144-149.
Blachut PA, O’Brien PJ, Meek RN, et al: Interlocking intramedullary nailing with or without reaming for the treatment of closed fractures of the tibial shaft: A prospective randomized study. J Bone Joint Surg Am 1997;79:640-646.
Question 11
A 12-year-old boy sustained a both bone forearm fracture 10 weeks ago and underwent closed reduction and casting. Examination now reveals that the injury is healed, but he is unable to extend his little and ring fingers of the injured hand with his wrist extended. Full extension is possible with the wrist flexed. A radiograph and clinical photograph are shown in Figures 15a and 15b. The remainder of his hand and wrist examination and neurologic evaluation in the hand are normal. What is the most likely diagnosis?
Explanation
REFERENCES: Watson PA, Blair W: Entrapment of the index flexor digitorum profundus tendon after fracture of both forearm bones in a child. Iowa Orthop J 1999;19:127-128.
Shaw BA, Murphy KM: Flexor tendon entrapment in ulnar shaft fractures. Clin Orthop 1996;330:181-184.
Kolkman KA, van Niekerk JL, Rieu PN, et al: A complicated forearm greenstick fracture: Case report. J Trauma 1992;32:116-117.
Hendel D, Aner A: Entrapment of the flexor digitorum profundus of the ring finger at the site of an ulnar fracture: A case report. Ital J Orthop Traumatol 1992;18:417-419.
Question 12
An otherwise healthy 35-year-old woman reports dorsal wrist pain and has trouble extending her thumb after sustaining a minimally displaced fracture of the distal radius 3 months ago. What is the next most appropriate step in management?
Explanation
REFERENCES: Christophe K: Rupture of the extensor pollicis longus tendon following Colles fracture. J Bone Joint Surg Am 1953;35:1003-1005.
Hove LM: Delayed rupture of the thumb extensor tendon: A 5-year study of 18 consecutive cases. Acta Orthop Scand 1994;65:199-203.
Question 13
Figure 16a shows the radiograph of a 34-year-old woman who sustained a basicervical fracture of the femoral neck. The fracture was treated with a compression screw and side plate. Seven months postoperatively, she continues to have significant hip pain and cannot bear full weight on her hip. A recent radiograph is shown in Figure 16b. Management should now consist of
Explanation
REFERENCES: Marti RK, Schuller HM, Raaymakers EL: Intertrochanteric osteotomy for non-union of the femoral neck. J Bone Joint Surg Br 1989;71:782-787.
Ballmer FT, Ballmer PM, Baumgaertel F, et al: Pauwels osteotomy for nonunions of the femoral neck. Orthop Clin North Am 1990;21:759-767.
Question 14
An 18-year-old man was in a motor vehicle accident and sustained a closed head injury, right displaced scapular body and glenoid fractures, a right proximal humeral fracture, fractures of ribs one through three, facial fractures, and bilateral pubic rami fractures with minimal displacement. He has a systolic blood pressure of 80/40 mm Hg despite fluid resuscitation. A radiograph is shown in Figure 17. Spiral CT does not identify any thoracic or abdominal injuries. What is the next most appropriate step in management?
Explanation
REFERENCES: Althausen PL, Lee MA, Finkemeier CG: Scapulothoracic dissociation: Diagnosis and treatment. Clin Orthop 2003;416:237-244.
Witz M, Korzets Z, Lehmann J: Traumatic scapulothoracic dissociation. J Cardiovasc Surg 2000;41:927-929.
Question 15
What is the major difference in outcome following open reduction and internal fixation (ORIF) of the tibial plafond at 2 to 5 days versus 10 to 20 days?
Explanation
REFERENCES: Sirkin M, Sanders R, DePasquale T, et al: A staged protocol for soft tissue management in the treatment of complex pilon fractures. J Orthop Trauma 1999;13:78-84.
Pollak AN, McCarthy ML, Bess RS, et al: Outcomes after treatment of high-energy tibial plafond fractures. J Bone Joint Surg Am 2003;85:1893-1900.
Question 16
Figure 18a shows the initial lateral radiograph of a 6-year-old girl who sustained a fracture in a motor vehicle accident and was treated in a cast 1 year ago. She now has the valgus deformity seen in Figure 18b. Treatment should consist of
Explanation
REFERENCES: Cozen L: Knock-knee deformity in children: Congenital and acquired. Clin Orthop 1990;258:191-203.
Jackson DW, Cozen L: Genu valgum as a complication of proximal tibial metaphyseal fractures in children. J Bone Joint Surg Am 1971;53:1571-1578.
Brammar TJ, Rooker GD: Remodeling of valgus deformity secondary to proximal metaphyseal fracture of the tibia. Injury 1998;29:558-560.
Ogden JA, Ogden DA, Pugh L, et al: Tibia valga after proximal metaphyseal fractures in childhood: A normal biologic response. J Pediatr Orthop 1995;15:489-494.
Salter RB, Best TN: Pathogenesis of progressive valgus deformity following fractures of the proximal metaphyseal region of the tibia in young children. Instr Course Lect 1992;41:409-411.
Question 17
Figure 19 shows the radiograph of a 45-year-old woman who has a painful nonunion. Treatment should consist of
Explanation
REFERENCES: Haidukewych GJ, Israel TA, Berry DJ: Reverse obliquity fractures of the intertrochanteric region of the femur. J Bone Joint Surg Am 2001;83:643-650.
Koval KJ, Zuckerman JD: Intertrochanteric fractures, in Rockwood & Green’s Fractures in Adults, ed 5. Philadelphia, PA, Lippincott Williams and Wilkins, 2001, pp 1635-1681.
Question 18
A 7-year-old boy has a swollen and deformed right arm after falling off his bicycle. Radiographs reveal a completely displaced posterolateral supracondylar humeral fracture. Examination reveals a warm, pink hand and forearm but absent pulses. What is the next most appropriate step in management?
Explanation
REFERENCES: Shaw BA: The role of angiography in assessing vascular injuries associated with supracondylar humerus fractures remains controversial. J Pediatr Orthop 1998;18:273.
Sabharwal S, Tredwell SJ, Beauchamp RD, et al: Management of pulseless pink hand in pediatric supracondylar fractures of humerus. J Pediatr Orthop 1997;17:303-310.
Schoenecker PL, Delgado E, Rotman M, et al: Pulseless arm in association with totally displaced supracondylar fracture. J Orthop Trauma 1996;10:410-415.
Question 19
What is the treatment of choice for the injury shown in Figures 20a through 20c?
Explanation
REFERENCES: Prokuski LJ, Eglseder WA Jr: Concurrent dorsal dislocations and fracture-dislocations of the index, long, ring, and small (second to fifth) carpometacarpal joints. J Orthop Trauma 2001;15:549-554.
Lawlis JF III, Gunther SF: Carpometacarpal dislocations: Long-term follow-up. J Bone Joint Surg Am 1991;73:52-59.
Question 20
A 32-year-old man has intense right hand and wrist pain, a deformed wrist, and numbness in his fingers after falling off his motorcycle. This is an isolated injury. Examination reveals a swollen wrist, normal capillary refill to all fingers, and limited flexion of all fingers. Radiographs are shown in Figures 21a and 21b. Neurologic examination of the hand will most likely reveal
Explanation
REFERENCES: Ruby LK, Cassidy C: Fractures and dislocations of the carpus, in Browner BD (ed): Skeletal Trauma, ed 3. Philadelphia, PA, WB Saunders, 2003, pp 1297-1300.
Habernek H, Weinstabl R, Kdolsky R, et al: Volar lunate fracture-dislocations of the wrist: Case report for two patients treated with external frame and internal open reduction. J Trauma 1998;45:975-978.
Question 21
A 55-year-old woman fell and sustained an elbow dislocation with a coronoid fracture and a radial head fracture. The elbow is reduced and splinted. What is the most common early complication?
Explanation
REFERENCES: Ring D, Jupiter JB, Zilberfarb J: Posterior dislocation of the elbow with fractures of the radial head and coronoid. J Bone Joint Surg Am 2002;84:547-551.
Ring D, Jupiter JB: Fracture-dislocation of the elbow. J Bone Joint Surg Am 1998;80:566-580.
Question 22
A 25-year-old man sustained the closed injury shown in Figures 22a and 22b. Examination reveals that this is an isolated injury, and he is hemodynamically stable. Treatment should consist of
Explanation
REFERENCES: Brumback RJ, Virkus WW: Intramedullary nailing of the femur: Reamed versus nonreamed. J Am Acad Orthop Surg 2000;8:83-90.
Brumback RJ, Ellison TS, Poka A, et al: Intramedullary nailing of femoral shaft fractures: Part III. Long-term effects of static interlocking fixation. J Bone Joint Surg Am 1992;74:106-112.
Question 23
Figure 23 shows the radiograph of an elderly man who fell on his right arm. What is the most important determinate of a good outcome following this injury?
Explanation
REFERENCES: Koval KJ, Gallagher MA, Marsicano JG, et al: Functional outcome after minimally displaced fractures of the proximal part of the humerus. J Bone Joint Surg Am 1997;79:203-207.
Hodgson SA, Mawson SJ, Stanley D: Rehabilitation after two-part fractures of the neck of the humerus. J Bone Joint Surg Br 2003;85:419-422.
Question 24
A 40 year-old-man was involved in a motor vehicle accident and sustained the pelvic injury seen in Figures 24a and 24b. Definitive management of the injury should consist of reduction by
Explanation
REFERENCES: Tile M: Management of pelvic ring injuries, in Tile M, Helfet DL, Kellam JF (eds): Fractures of the Pelvis and Acetabulum, ed 3. Philadelphia, PA, Lippincott Williams & Wilkins, 2003, pp 168-202.
Kabak S, Halici M, Tuncel M, et al: Functional outcome of open reduction and internal fixation for completely unstable pelvic ring fractures (type C): A report of 40 cases. J Orthop Trauma 2003;17:555-562.
Question 25
A 35-year-old patient sustained a bimalleolar ankle fracture. What is the most reliable method of predicting a tear of the interosseous membrane?
Explanation
REFERENCE: Nielson JH, Sallis JG, Potter HG, et al: Correlation of interosseous membrane tears to the level of the fibular fracture. J Orthop Trauma 2004;18:68-74.
Question 26
When performing a flexor tendon repair of a digit other than the thumb, what structures of the flexor tendon sheath should be preserved?
Explanation
REFERENCES: Doyle JR: Anatomy of the finger flexor tendon sheath and pulley system.
J Hand Surg Am 1988;13:473-484.
Strickland JW: Flexor tendon injuries: I. Foundations of treatment. J Am Acad Orthop Surg 1995;3:44-54.
Question 27
A distal radius fracture in an elderly man is strongly predictive for what subsequent injury?
Explanation
REFERENCE: Haentjens P, Autier P, Collins J, et al: Colles fracture, spine fracture, and subsequent risk of hip fracture in men and women: A meta-analysis. J Bone Joint Surg Am 2003;85:1936-1943.
Question 28
A 13-year-old girl injures her ankle playing soccer. Radiographs reveal a displaced Tillaux fracture. CT scans are shown in Figure 25. What is the most important consideration for appropriate management?
Explanation
REFERENCES: Kay RM, Matthys GA: Pediatric ankle fractures: Evaluation and treatment.
J Am Acad Orthop Surg 2001;9:268-278.
Kling TF Jr: Operative treatment of ankle fractures in children. Orthop Clin North Am 1990;21:381-392.
Duchesneau S, Fallat LM: The Tillaux fracture. J Foot Ankle Surg 1996;35:127-133.
Question 29
What measure of physiologic status best evaluates whether an injured patient is fully resuscitated and best predicts that perioperative complications will be minimized following definitive stabilization of long bone fractures?
Explanation
REFERENCES: Blow O, Magliore L, Claridge JA, et al: The golden hour and silver day: Detection and correction of occult hypoperfusion within 24 hours improves outcomes from major trauma. J Trauma 1999;47:964-977.
Crowl A, Young JS, Kahler DM, et al: Occult hypoperfusion is associated with increased morbidity in patients undergoing early femur fracture fixation. J Trauma 2000;48:260-267.
Shulman AM: Prediction of patients who will develop prolonged occult hypoperfusion following blunt trauma. J Trauma 2004;57:725-800.
Question 30
Based on the findings seen in the radiograph in Figure 26, emergent management should consist of
Explanation
REFERENCES: Isenberg J, Prokop A, Schellhammer F, et al: Palmar lunate dislocation. Unfallchirurg 2002;105:1133-1138.
Ruby LK: Fractures and dislocations of the carpus, in Browner BD, Jupiter JB (eds): Skeletal Trauma, ed 2. Philadelphia, PA, WB Saunders, 1998, pp 1367-1372.
Question 31
A 10-year-old girl has a midshaft both bone forearm fracture. After attempted closed reduction, alignment consists of bayonet apposition, 10° of malrotation, and 8° of volar angulation. Management should now consist of
Explanation
REFERENCES: Do TT, Strub WM, Foad SL, et al: Reduction versus remodeling in pediatric distal forearm fractures: A preliminary cost analysis. J Pediatr Orthop B 2003;12:109-115.
Flynn JM: Pediatric forearm fractures: Decision making, surgical techniques, and complications. Instr Course Lect 2002;51:355-360.
Ring D, Waters PM, Hotchkiss RN, et al: Pediatric floating elbow. J Pediatr Orthop 2001;21:456-459.
Noonan KJ, Price CT: Forearm and distal radius fractures in children. J Am Acad Orthop Surg 1998;6:146-156.
Question 32
In the treatment of ankle fractures, the superficial peroneal nerve is most commonly injured by
Explanation
REFERENCES: Redfern DJ, Sauve PS, Sakellariou A: Investigation of incidence of superficial peroneal nerve injury following ankle fracture. Foot Ankle Int 2003;24:771-774.
Miller SD: Ankle fractures, in Myerson MS (ed): Foot and Ankle Disorders. Philadelphia, PA, WB Saunders, 2000, pp 1341-1366.
Question 33
A 54-year-old man sustained a small superficial abrasion over the left acromioclavicular joint after falling from his bicycle. Examination reveals no other physical findings. Radiographs show a displaced fracture of the lateral end of the clavicle distal to a line drawn vertically to the coracoid process. Management should consist of
Explanation
REFERENCES: Robinson CM, Cairns DA: Primary nonoperative treatment of displaced lateral fractures of the clavicle. J Bone Joint Surg Am 2004;86:778-782.
Deafenbaugh MK, Dugdale TW, Staeheli JW, et al: Nonoperative treatment of Neer type II distal clavicle fractures: A prospective study. Contemp Orthop 1990;20:405-413.
Question 34
A 47-year-old man sustained a degloving injury over the pretibial surface and anterior ankle region in a motor vehicle accident. After debridement and irrigation, there is inadequate tissue for closure of the exposed anterior tibial tendon and tibia. Prior to definitive soft-tissue coverage, management should consist of
Explanation
REFERENCES: Webb LX: New techniques in wound management: Vacuum assisted wound closure. J Am Acad Orthop Surg 2002;10:303-311.
Clare MP, Fitzgibbons TC, McMullen ST, et al: Experience with the vacuum assisted closure negative pressure technique in the treatment of non-healing diabetic and dysvascular wounds. Foot Ankle Int 2002;23:896-901.
Question 35
The humeral nonunion shown in Figure 27 is most likely to unite when using what method of treatment?
Explanation
REFERENCES: Pugh DM, McKee MD: Advances in the management of humeral nonunion.
J Am Acad Orthop Surg 2003;11:48-59.
McKee MD, Miranda MA, Riemer BL, et al: Management of humeral nonunion after the failure of locking intramedullary nails. J Orthop Trauma 1996;10:492-499.
Question 36
An adult with a distal humeral fracture underwent open reduction and internal fixation. What is the most common postoperative complication?
Explanation
REFERENCES: Webb LX: Distal humerus fractures in adults. J Am Acad Orthop Surg 1996;4:336-344.
McKee MD, Wilson TL, Winston L, et al: Functional outcome following surgical treatment of intra-articular distal humeral fractures through a posterior approach. J Bone Joint Surg Am 2000;82:1701-1707.
Question 37
The radiographs and CT scan seen in Figures 28a through 28d reveal what type of acetabular fracture pattern?
Explanation
REFERENCES: Tile M: Describing the injury: Classification of acetabular fractures, in Tile M, Helfet DL, Kellam JF (eds): Fractures of the Pelvis and Acetabulum, ed 3. Philadelphia, PA, Lippincott Williams & Wilkins, 2003, pp 427-475.
Brandser E, Marsh JL: Acetabular fractures: Easier classification with a systematic approach. Am J Roentgenol 1998;171:1217-1228.
Question 38
A 26-year-old man sustained an isolated injury to his left hip joint in a motor vehicle accident. Closed reduction was performed, and the postreduction radiograph is shown in Figure 29. Management should now consist of
Explanation
REFERENCES: Tile M, Olson SA: Decision making: Non operative and operative indications for acetabular fractures, in Tile M, Helfet DL, Kellam JF (eds): Fractures of the Pelvis and Acetabulum. Philadelphia, PA, Lippincott Williams and Wilkins, 2003, pp 496-532.
Letournel E, Judet R: Fractures of the Acetabulum, ed 2. Berlin, Germany, Springer Verlag, 1993, pp 337-339, p 507.
Question 39
A 35-year-old man is brought to the emergency department following a motorcycle accident. He is breathing spontaneously and has a systolic blood pressure of 80 mm Hg, a pulse rate of 120/min, and a temperature of 98.6° F (37° C). Examination suggests an unstable pelvic fracture; AP radiographs confirm an open book injury with vertical displacement on the left side. Ultrasound evaluation of the abdomen is negative. Despite administration of 4 L of normal saline solution, he still has a systolic pressure of 90 mm Hg and a pulse rate of 110. Urine output has been about 20 mL since arrival 35 minutes ago. What is the next best course of action?
Explanation
REFERENCE: Mayo K, Kellam JK: Pelvic ring disruptions, in Browner BD (ed): Skeletal Trauma, ed 3. Philadelphia, PA, WB Saunders, 2003, pp 1052-1108.
Question 40
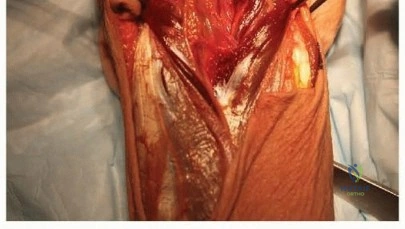
A healthy 25-year-old man sustains a grade IIIB open tibial fracture. Following appropriate debridement, irrigation, and stabilization with an external fixator, the soft-tissue injury is shown in Figure 30. What is the most appropriate definitive soft-tissue coverage procedure?
Explanation
REFERENCES: Mathes SJ, Nahai F: Vascular anatomy of muscle: Classification and applications, in Mathes SJ, Nahai F (eds): Clinical Application for Muscle and Musculocutaneous Flaps. St Louis, MO, CV Mosby, 1982, p 20.
Bos GD, Buehler MJ: Lower-extremity local flaps. J Am Acad Orthop Surg 1994;2:342-351.
Question 41
A 25-year-old woman undergoes surgical treatment of a displaced proximal humeral fracture via a deltopectoral approach. At the first postoperative visit, she reports a tingling numbness along the anterolateral aspect of the forearm. What structure is most likely injured?
Explanation
REFERENCES: McIlveen SJ, Duralde XA, D’Alessandro DF, et al: Isolated nerve injuries about the shoulder. Clin Orthop 1994;306:54-63.
Warner JP: Frozen shoulder: Diagnosis and management. J Am Acad Orthop Surg
1997;5:130-140.
Question 42
A 7-year-old girl has pain and swelling of the right elbow after falling off her bicycle. Radiographs are shown in Figure 31. What is the most appropriate initial step in management?
Explanation
REFERENCES: Finnbogason T, Karlsson G, Lindberg L, et al: Nondisplaced and minimally displaced fractures of the lateral humeral condyle in children: A prospective radiographic investigation of fracture stability. J Pediatr Orthop 1995;15:422-425.
Attarian DE: Lateral condyle fractures: Missed diagnoses in pediatric elbow injuries. Mil Med 1990;155:433-434.
Flynn JC: Nonunion of slightly displaced fractures of the lateral humeral condyle in children: An update. J Pediatr Orthop 1989;9:691-696.
Badelon O, Bensahel H, Mazda K, et al: Lateral humeral condylar fractures in children: A report of 47 cases. J Pediatr Orthop 1988;8:31-34.
Question 43
A 32-year-old man sustained a fracture of his upper arm in a motor vehicle accident. Radiographs are shown in Figure 32. Because of other associated injuries, surgical stabilization is chosen. What technique will result in the least complications and the best outcome?
Explanation
REFERENCES: Schemitsch EH, Bhandari M: Fractures of the humeral shaft, in Browner BD: Skeletal Trauma, ed 3. Philadelphia, PA, WB Saunders, 2003, pp 1481-1511.
Chapman JR, Henley MB, Agel J: Randomized prospective study of humeral shaft fracture fixation: Intramedullary nails versus plates. J Orthop Trauma 2000;14:162-166.
Question 44
A 56-year-old man sustained a nondisplaced extra-articular fracture of the proximal aspect of the third metatarsal after dropping a heavy object on his left foot. Management should consist of
Explanation
REFERENCES: Myerson MS: Foot and Ankle Disorders. Philadelphia, PA, WB Saunders, 2000, pp 1265-1296.
Early JS: Fractures and dislocations of the midfoot and forefoot, in Rockwood and Green’s Fractures in Adults, ed 5. Philadelphia, PA, Lippincott Williams and Wilkins, 2001,
pp 2181-2245.
Question 45
During a posterior approach to the glenoid with retraction as shown in Figure 33, care should be taken during superior retraction to avoid injury to which of the following structures?
Explanation
glenoid fracture, or posterior shoulder pathology, the interval between the teres minor and infraspinatus is split. Excessive superior retraction on the infraspinatus, or excessive dissection superomedially under the infraspinatus muscle and tendon can cause injury to the suprascapular nerve and/or artery. During dissection in this interval, the axillary artery and axillary nerve are well protected. A branch of the circumflex scapular artery ascends between the teres minor
and infraspinatus muscle, but it is at risk during dissection on the scapula in the mid portion of the interval and not during superior retraction. The profunda brachii artery is not present in
this interval.
REFERENCES: Jerosch JJ, Greig M, Peuker ET, et al: The posterior subdeltoid approach: A modified access to the posterior glenohumeral joint. J Shoulder Elbow Surg 2001;10:265-268.
Judet R: Surgical treatment of scapular fractures. Acta Orthop Belg 1964;30:673-678.
Kavanagh BF, Bradway JK, Cofield RH: Open reduction and internal fixation of displaced intra-articular fractures of the glenoid fossa. J Bone Joint Surg Am 1993;75:479-484.
Question 46
A 42-year-old woman sustained a closed, displaced talar neck fracture in a motor vehicle accident. Which of the following is an avoidable complication of surgical treatment?
Explanation
REFERENCES: Rockwood and Green’s Fractures in Adults, ed 5. Philadelphia, PA, Lippincott, Williams and Wilkins, 2001, pp 2091-2132.
Daniels TR, Smith JW, Ross TI: Varus malalignment of the talar neck: Its affects on the position of the foot and on subtalar motion. J Bone Joint Surg Am 1996;78:1559-1567.
Question 47
Figures 34a through 34c show the radiographs of a 51-year-old woman who injured her elbow in a fall from standing height. Examination reveals that elbow range of motion is limited by pain only. Management should consist of
Explanation
function and minimize stiffness. A long arm cast for any length of time will result in severe elbow stiffness.
REFERENCES: Morrey BF: Radial head fracture, in Morrey BF (ed): The Elbow and Its Disorders, ed 3. Philadelphia, PA, WB Saunders, 2000, pp 341-364.
Hotchkiss RN: Displaced fractures of the radial head: Internal fixation or excision? J Am Acad Orthop Surg 1997;5:1-10.
Question 48
Figure 35 shows the radiograph of a 12-year-old boy who fell off a snowmobile and landed on his left shoulder. He has a closed injury. Management should consist of
Explanation
REFERENCES: Kohler R, Trillaud JM: Fracture and fracture separation of the proximal humerus in children: Report of 136 cases. J Pediatr Orthop 1983;3:326-332.
Beaty JH: Fractures of the proximal humerus and shaft in children. Instr Course Lect 1992;41:369-372.
Dobbs MB, Luhmann SL, Gordon JE, et al: Severely displaced proximal humeral epiphyseal fractures. J Pediatr Orthop 2003;23:208-215.
Beringer DC, Weiner DS, Noble JS, et al: Severely displaced proximal humeral epiphyseal fractures: A follow-up study. J Pediatr Orthop 1998;18:31-37.
Wang P Jr, Koval KJ, Lehman W, et al: Salter-Harris type III fracture-dislocation of the proximal humerus. J Pediatr Orthop B 1997;6:219-222.
Question 49
What is the most common complication requiring reoperation after dorsal plating for a distal radius fracture?
Explanation
REFERENCES: Rozental TD, Beredjiklian PK, Bozentka DJ: Functional outcome and complications following two types of dorsal plating for unstable fractures of the distal part of the radius. J Bone Joint Surg Am 2003;85:1956-1960.
Kambouroglou GK, Axelrod TS: Complications of the AO/ASIF titanium distal radius plate system (pi plate) in internal fixation of the distal radius: A brief report. J Hand Surg Am 1998;23:737-741.
Question 50
Figures 36a and 36b show the radiographs of a 48-year-old woman who smokes cigarettes and sustained a segmental femoral shaft fracture in a motor vehicle accident 9 months ago. Initial management consisted of stabilization with a reamed statically locked intramedullary nail. She now reports lower leg pain that increases with activity. In addition to advising the patient to quit smoking, management should include
Explanation
REFERENCES: Webb LX, Winquist RA, Hansen ST: Intramedullary nailing and reaming for delayed union or nonunion of the femoral shaft: A report of 105 consecutive cases. Clin Orthop 1986;212:133-141.
Weresh MJ, Hakanson R, Stover MD, et al: Failure of exchange reamed intramedullary nailing for ununited femoral shaft fractures. J Orthop Trauma 2000;14:335-338.
Hak DG, Lee SS, Goulet JA: Success of exchange reamed intramedullary nailing for femoral shaft nonunion or delayed union. J Orthop Trauma 2000;14:178-182.
Question 51
A 45-year-old man falls on an outstretched hand and sustains a terrible triad injury of the elbow. Intraoperatively, after fixation of the radial head and repair of the lateral ulnar collateral ligament (LUCL), the elbow remains unstable in extension. What is the most appropriate next step?
Explanation
Question 52
A 30-year-old sustained a Hawkins Type III talar neck fracture 8 weeks ago, treated with ORIF. A subchondral radiolucent band is seen on the dome of the talus on an AP ankle radiograph. What does this radiographic finding indicate?
Explanation
Question 53
A 25-year-old motorcyclist sustains a severely comminuted open tibial shaft fracture with a 12-cm soft-tissue defect and exposed bone after extensive debridement. Pulses are symmetric to the contralateral limb. According to the Godina principles, to optimize outcomes, soft-tissue coverage with a free flap should ideally be performed within what timeframe?
Explanation
Question 54
A 68-year-old woman with osteopenia falls and sustains a comminuted, displaced intra-articular distal humerus fracture. Due to severe comminution and poor bone quality, total elbow arthroplasty (TEA) is planned. Which of the following is a strict contraindication to acute TEA in this setting?
Explanation
Question 55
A 22-year-old football player sustains a twisting injury to his midfoot. Weight-bearing radiographs reveal a 3 mm widening between the bases of the first and second metatarsals, with a small avulsion fracture off the base of the second metatarsal. What is the most appropriate management for this athlete?
Explanation
Question 56
A 35-year-old multitrauma patient with bilateral femur fractures arrives at the trauma bay. Which of the following physiologic parameters is the strongest indication to proceed with damage control orthopedics (external fixation) rather than early total care (intramedullary nailing)?
Explanation
Question 57
What is the recommended sequence of surgical reconstruction for a "terrible triad" injury of the elbow?
Explanation
Question 58
A 25-year-old athlete presents with midfoot pain after an axial load to a plantarflexed foot. Weight-bearing radiographs demonstrate a 3 mm diastasis between the base of the first and second metatarsals. The primary ligament injured in this condition connects which two structures?
Explanation
Question 59
According to the Lower Extremity Assessment Project (LEAP) study, which of the following statements regarding severe lower extremity trauma is most accurate?
Explanation
Question 60
A 40-year-old female presents with a displaced fracture of the capitellum that includes the lateral trochlear ridge. According to the Bryan and Morrey classification, what type of fracture is this, and what is the preferred treatment?
Explanation
Question 61
Six weeks following open reduction and internal fixation of a Hawkins Type II talar neck fracture, an anteroposterior radiograph of the ankle reveals subchondral radiolucency in the talar dome. This radiographic finding indicates which of the following?
Explanation
Question 62
A 28-year-old male sustains a vertically oriented, displaced femoral neck fracture (Pauwels type III) after a fall from a height. Which of the following fixation constructs provides the most biomechanical stability for this specific fracture pattern?
Explanation
Question 63
During an olecranon osteotomy approach for open reduction and internal fixation of an intra-articular distal humerus fracture, what is the optimal shape of the osteotomy to maximize stability upon repair?
Explanation
Question 64
A 35-year-old roofer falls and sustains a displaced intra-articular calcaneus fracture. An extensile lateral approach is planned. Which of the following structures is most at risk during the inferior limb of the incision?
Explanation
Question 65
A 42-year-old male arrives in the trauma bay with an APC-III pelvic ring injury and a systolic blood pressure of 75 mm Hg. A pelvic binder is applied. What is the correct anatomical placement for the pelvic binder to effectively reduce pelvic volume?
Explanation
Question 66
A 22-year-old collegiate basketball player sustains a fracture at the metaphyseal-diaphyseal junction of the fifth metatarsal. He is treated with intramedullary screw fixation. This specific fracture location is prone to nonunion primarily due to which of the following vascular anatomical features?
Explanation
Question 67
A 38-year-old female falls on an outstretched hand and sustains a comminuted radial head fracture. On examination, she complains of severe wrist pain and has tenderness over the distal radioulnar joint (DRUJ). Which of the following treatments is contraindicated?
Explanation
Question 68
A 25-year-old male presents with a closed tibial shaft fracture and complains of pain out of proportion to his injury. His blood pressure is 110/70 mm Hg. Compartment pressure measurements reveal an anterior compartment pressure of 35 mm Hg. Which of the following criteria best indicates the need for emergent fasciotomy?
Explanation
Question 69
A 55-year-old patient with long-standing diabetes presents with a swollen, warm, and erythematous foot. Radiographs reveal fragmentation, periarticular debris, and subluxation at the tarsometatarsal joints. According to the Eichenholtz classification of Charcot arthropathy, what stage does this represent?
Explanation
Question 70
A 6-year-old boy falls from monkey bars and sustains a proximal third ulnar shaft fracture with an associated anterior dislocation of the radial head. According to the Bado classification, what type of Monteggia lesion is this?
Explanation
Question 71
A 24-year-old male sustains a low-velocity gunshot wound to the thigh resulting in a comminuted midshaft femur fracture. The bullet passed cleanly through the soft tissues without hitting major neurovascular structures. What is the most appropriate management?
Explanation
Question 72
A professional football player sustains a hyperdorsiflexion injury to his first metatarsophalangeal (MTP) joint, resulting in a tear of the plantar plate, commonly referred to as "turf toe." What is the primary biomechanical role of the sesamoids in the first MTP joint?
Explanation
Question 73
A 45-year-old man falls on an outstretched hand and sustains a 'terrible triad' injury of the elbow. He undergoes operative management. To restore elbow stability, what is the most widely accepted sequence of surgical reconstruction for this specific injury pattern?
Explanation
Question 74
A 25-year-old athlete complains of midfoot pain after a forced plantarflexion injury. A weight-bearing radiograph demonstrates 2 mm of widening between the first and second metatarsal bases and a 'fleck sign'. Which of the following ligaments is primarily disrupted?
Explanation
Question 75
A 30-year-old male sustains a high-energy Pauwels type III femoral neck fracture in a motor vehicle collision. To biomechanically optimize fixation and minimize the high shear forces that typically lead to varus collapse, which construct is most appropriate?
Explanation
Question 76
A 40-year-old roofer falls from a ladder and sustains an intra-articular calcaneus fracture. Preoperative radiographs reveal a Bohler's angle of 5 degrees. What is the primary functional purpose of restoring Bohler's angle during surgical fixation?
Explanation
Question 77
A 35-year-old female presents with a highly comminuted distal humerus fracture after a fall. Imaging identifies a type IV capitellum fracture according to the McKee modification of the Bryan and Morrey classification. What specific finding defines this fracture type?
Explanation
Question 78
A 28-year-old male construction worker is crushed by heavy equipment, sustaining an anteroposterior compression (APC) type III pelvic ring injury. Examination reveals blood at the urethral meatus and a high-riding prostate on digital rectal exam. What is the most appropriate next step in his urologic evaluation?
Explanation
Question 79
A 22-year-old snowboarder sustains a forced dorsiflexion injury of the ankle, resulting in a Hawkins type III talar neck fracture. According to the Hawkins classification, this fracture pattern involves subluxation or dislocation of which specific joints?
Explanation
Question 80
A 5-year-old boy sustains a Gartland type III supracondylar humerus fracture. On initial presentation, the radial pulse is absent, but the hand is pink and warm. Following closed reduction and percutaneous pinning, the hand remains pink and well-perfused, but the pulse is still absent on Doppler. What is the most appropriate next step?
Explanation
Question 81
A 45-year-old agricultural worker sustains a Gustilo-Anderson IIIB open tibial shaft fracture deeply contaminated with soil and manure. In addition to immediate tetanus prophylaxis and aggressive surgical debridement, which antibiotic regimen is most appropriate based on current trauma guidelines?
Explanation
Question 82
A 26-year-old male complains of severe, escalating leg pain 12 hours after an intramedullary nailing of a tibia fracture. He has extreme pain with passive toe stretch. Compartment pressures are measured. Which threshold is currently widely accepted as the absolute indication for four-compartment fasciotomies?
Explanation
None
