OITE & AAOS Board Exam MCQs: Spinal Deformity & Scoliosis | Part 211

Key Takeaway
This page presents Part 211 of our expert-authored Orthopedic Surgery Board Review. It features 100 verified, high-yield MCQs focusing on Deformity and Scoliosis, precisely mirroring OITE/AAOS exam formats. Tailored for orthopedic residents and practicing surgeons, this interactive quiz is crucial for comprehensive board certification preparation and success.
About This Board Review Set
This is Part 211 of the comprehensive OITE and AAOS Orthopedic Surgery Board Review series authored by Dr. Mohammed Hutaif, Consultant Orthopedic & Spine Surgeon.
This set has been strictly audited and contains 100 100% verified, high-yield multiple-choice questions (MCQs) modelled on the exact format of the Orthopaedic In-Training Examination (OITE) and the American Academy of Orthopaedic Surgeons (AAOS) board examinations.
How to Use the Interactive Quiz
Two distinct learning modes are available:
- Study Mode — After selecting an answer, you immediately see whether you are correct or incorrect, together with a full clinical explanation and literature references.
- Exam Mode — All feedback is hidden until you click Submit & See Results. A live timer tracks elapsed time. A percentage score and detailed breakdown are displayed upon submission.
Pro Tip: Use keyboard shortcuts A–E to select options, F to flag a question for review, and Enter to jump to the next unanswered question.
Topics Covered in Part 211
This module focuses heavily on: Deformity, Scoliosis.
Sample Questions from This Set
Sample Question 1: Etanercept modifies the natural history of inflammatory arthropathies through what mechanism?...
Sample Question 2: What region of the thoracic curve is most dangerous for pedicle screw insertion while performing a posterior fusion for adolescent idiopathic scoliosis?...
Sample Question 3: -A 14-year-old girl has a painless deformity of the right tibia. A radiograph from 2 years ago is seen in Figure a; nothing was done at that time. Her current radiograph is seen in Figure b. She has no pain, fever, or drainage. What is the ...
Sample Question 4: Which of the following clinical scenarios represents an appropriate indication for convex hemiepiphysiodesis/hemiarthrodesis in the treatment of a child with a congenital spinal deformity?...
Sample Question 5: A 4-month-old infant is referred for evaluation of congenital scoliosis. The child has no congenital heart anomalies, and a renal ultrasound shows that he has one kidney. Examination reveals mild scoliosis and a large hairy patch on the chi...
Why Active MCQ Practice Works
Evidence consistently demonstrates that active recall through spaced MCQ practice yields substantially greater long-term retention than passive reading alone (Roediger & Karpicke, 2006). All questions in this specific module have been algorithmically verified for clinical integrity and complete explanations.
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
Etanercept modifies the natural history of inflammatory arthropathies through what mechanism?
Explanation
Question 2
What region of the thoracic curve is most dangerous for pedicle screw insertion while performing a posterior fusion for adolescent idiopathic scoliosis?
Explanation
REFERENCES: Liljenqvist U, Allkemper T, Hackenberg L, et al: Analysis of vertebral morphology in idiopathic scoliosis with use of magnetic resonance imaging and multiplanar reconstruction. J Bone Joint Surg Am 2002;84:359-368.
Parent S, Labelle H, Skalli W, et al: Thoracic pedicle morphometry in vertebrae from scoliotic spines. Spine 2004;29:239-248.
Question 3
-A 14-year-old girl has a painless deformity of the right tibia. A radiograph from 2 years ago is seen in Figure a; nothing was done at that time. Her current radiograph is seen in Figure b. She has no pain, fever, or drainage. What is the most likely diagnosis?
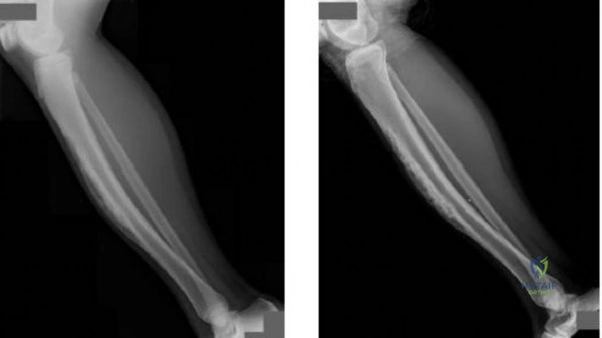
Explanation

Question 4
Which of the following clinical scenarios represents an appropriate indication for convex hemiepiphysiodesis/hemiarthrodesis in the treatment of a child with a congenital spinal deformity?
Explanation
REFERENCE: Winter RB, Lonstein JE, Denis F, Sta-Ana de la Rosa H: Convex growth arrest for progressive congenital scoliosis due to hemivertebrae. J Pediatr Orthop 1988;8:633-638.
Question 5
A 4-month-old infant is referred for evaluation of congenital scoliosis. The child has no congenital heart anomalies, and a renal ultrasound shows that he has one kidney. Examination reveals mild scoliosis and a large hairy patch on the child’s back. Neurologic evaluation is normal for his age. A clinical photograph and radiograph are shown in Figures 19a and 19b. Initial management should consist of Review Topic
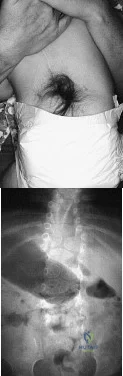
Explanation
Question 6
A 19-year-old woman sustained a displaced talar neck fracture while cliff jumping. The fracture is managed with open reduction and internal fixation. Which of the following best describes the findings in the 2-months postoperative radiographs shown in Figures 67a and 67b, and subsequent treatment plan? Review Topic
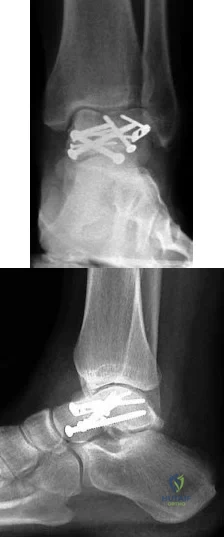
Explanation
Osteonecrosis is best diagnosed with radiographs. Although MRI can be helpful in assessing the extent of osteonecrosis, it is unnecessary for purely diagnostic purposes. A Hawkins sign typically will appear at 6 to 8 weeks after fracture; however, the absence of a Hawkins sign at that time does not necessarily indicate osteonecrosis. Most authors agree that even in the absence of a Hawkins sign, weight bearing can commence at 10 to 12 weeks after surgery.
Question 7
A 32-year-old man presents to the emergency department with a humeral shaft fracture. He has wrist drop as well as impaired finger and thumb extension. Which motor function would be expected to recover last?

Explanation
Abrams et al detailed the order of innervation of the radial nerve and found the following order (proximal to distal): brachioradialis, extensor carpi radialis longus, supinator, extensor carpi radialis brevis, extensor digitorum communis, extensor carpi ulnaris, extensor digiti quinti, abductor policis longus, extensor policis longus, extensor policis brevis, and extensor indicis proprius.
Branovacki et al found a slightly different pattern: brachioradialis, extensor carpi radialis longus, superficial sensory, extensor carpi radialis brevis, supinator, extensor digitorum/extensor carpi ulnaris, extensor digiti minimi, abductor pollicis longus, extensor pollicis brevis, extensor pollicis longus and extensor indicis proprius.
While both extensor digitorum and extensor indicis proprius extend the index finger MCP joint, only extensor indicis proprius hyperextends the index finger past neutral
Question 8
Figure 13a shows the radiograph of a 9-year-old girl who sustained complete transverse fractures of the radial and ulnar shafts while in-line skating. A manipulative closed reduction is performed, and the result is seen in Figure 13b. What is the next most appropriate step in management?
Explanation
REFERENCES: Price CT, Scott DS, Kurzner ME, Flynn JC: Malunited forearm fractures in children. J Pediatr Orthop 1990;10:705-712.
Vittas D, Larsen E, Torp-Pedersen S: Angular remodeling of midshaft forearm fractures in children. Clin Orthop 1991;265:261-264.
Question 9
What is the main mechanism for nutrition of the adult disk?
Explanation
REFERENCES: Biyani A, Andersson GB: Low back pain: Pathophysiology and management. J Am Acad Orthop Surg 2004;12:106-115.
Urban JG, Holm S, Maroudas A, et al: Nutrition of the intervertebral disc: Effect of fluid flow on solute transport. Clin Orthop 1982;170:296-302.
Park AE, Boden SD: Intervertebral disk: Form and function, in Einhorn TA, O’Keefe RJ, Buckwalter JA (eds): Orthopaedic Basic Science: Foundations of Clinical Practice, ed 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, in press.
Question 10
An year-old obese woman has left knee pain. She had surgery 5 years ago for a patellar nonunion after total knee arthroplasty that was complicated by infection, which was treated with implant removal and patellectomy. She has not been ambulatory since then. She states she is no longer on antibiotics. She has moderate pain, but her primary problem is instability of the knee. She has a 40° extensor lag. Darkening of the skin is present distal to the incision consistent with venous stasis changes. The erythrocyte sedimentation rate is 12 mm/h (reference range 0 to 20 mm/h) and her C-reactive protein level is 0 mg/L (reference range 08 to 1 mg/L). Left knee aspiration shows a white blood cell count of 800 and 20% neutrophils. What is the best next step?
Explanation
This patient is elderly, obese, and nonambulatory and has a chronic quadriceps tendon rupture after infected total knee arthroplasty. Her potential for ambulation after revision total knee arthroplasty is very low. Primary repair of the tendon is unlikely to be successful, even with augmentation, so revision total knee arthroplasty with primary quadriceps tendon repair and two-stage revision knee arthroplasty and quadricep repair with Achilles allograft are not the best management techniques. Extensor mechanism allograft could be done but would have a high failure rate in a patient of this size. No sign of infection is seen, based on laboratory studies, so a two-stage procedure is not necessary. The best management although not optimal, would be treatment in a drop-lock brace. Arthrodesis is also an option, but would have a high complication rate, and in a patient that is nonambulatory, a fused knee would be increasingly
difficult with activities of daily living and mobility.
Question 11
A 42-year-old patient has had a fever and low back pain for several days. Laboratory studies show an elevated erythrocyte sedimentation rate and a WBC count of 9,500 mm3 with 75% neutrophils. A CT scan is shown in Figure 15. Examination will most likely reveal what other findings?
Explanation
REFERENCES: Cellier C, Gendre JP, Cosnes J, et al: Psoas abscess complication Crohn’s disease. Gastroenterol Clin Biol 1992;16:235-238.
Netter FH: Atlas of Human Anatomy. Summit, NJ, Ciba-Geigy, 1989, pp 470-471, 506.
Question 12
A 67-year-old man with right shoulder osteoarthritis (OA) remains symptomatic despite a course of nonsurgical treatment. A CT scan of the shoulder shows eccentric posterior glenoid wear with 10° of retroversion. What is the appropriate management of this glenoid bone loss during surgery for an anatomic total shoulder arthroplasty?
Explanation
glenoid bone grafting may be considered for glenoid retroversion >15°.
Question 13
A 20-year-old man is brought to the emergency department after a high-speed motor vehicle accident. His initial blood pressure is 70/40 mm Hg. He is currently receiving intravenous fluids as well as blood. His Focused Assessment with Sonography for Trauma examination did not show any free fluid in his abdomen and his chest radiograph is unremarkable. An AP pelvis radiograph is shown in Figure 15. What is the next most appropriate step in the management of his pelvic injury? Review Topic
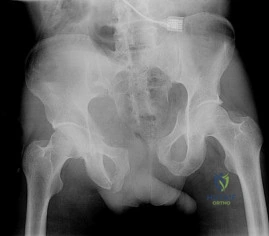
Explanation
Question 14
A 20-year-old male military recruit reports a 5-day history of progressive deep groin pain that is made worse with weight-bearing activities and running. His initial coronal T2-weighted MRI scan is shown in Figure 75. His initial treatment should consist of which of the following? Review Topic
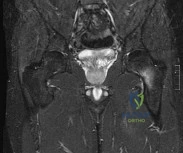
Explanation
Question 15
Figures 42a and 42b show the radiographs of a 52-year-old man who sustained a fall from a motorcycle 6 months ago and now reports pain and stiffness in his left shoulder. What is the most reliable treatment to improve function and comfort of the shoulder? Review Topic
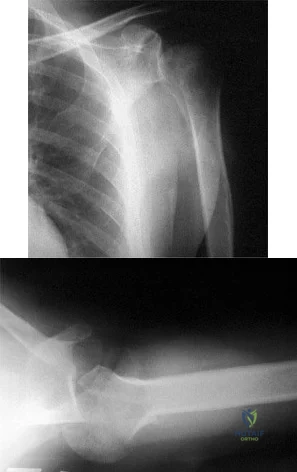
Explanation
Question 16
Figure 1 is the radiograph of an otherwise healthy 68-year-old man with a 4-year history of increasing global left knee pain. He has noticed stiffness, and despite physical therapy, bracing and nonsteroidal anti-inflammatory drugs, he has continued to develop worsening symptoms and progression in his deformity. Physical examination demonstrates 80°of flexion and a 10° flexion contracture. What is the best next step?
Explanation
Question 17
A patient with refractory long head biceps pain in the shoulder undergoes biceps tenotomy. The patient is concerned about possible postoperative deformity and loss of supination strength. Which of the following techniques provides the strongest initial fixation to prevent distal migration?
Explanation
REFERENCES: Ozalay M, Akpinar S, Karaeminogullari O, et al: Mechanical strength of four different biceps tenodesis techniques. Arthroscopy 2005;21:992-998.
Richards DP, Burkhart SS: A biomechanical analysis of two biceps tenodesis fixation techniques. Arthroscopy 2005;21:861-866.
Question 18
An otherwise healthy 76-year-old woman has pain 2 years after total hip arthroplasty. The clinical photograph in Figures below demonstrates her skin envelope, and associated radiograph. Her C-reactive protein level is normal, and her erythrocyte sedimentation rate is mildly elevated. The white blood cell count is normal. Hip aspiration attempted under fluoroscopy generates no fluid. What is the best definitive treatment?
Explanation
This patient clearly has a chronically infected total hip arthroplasty, indicated by the open, draining sinus, as well as trochanteric bone resorption on radiographs, and two years of pain. Recently, specific guidelines have been published to better help the clinician define infection. Repeating the hip aspiration is unnecessary, because infection is already evident. Initiating a wound care consult would not address the underlying infection. The determination whether to retain the components or perform a two-stage exchange is based more on the acuity of infection. In this particular case, the patient is chronically infected. Irrigation and debridement with a liner exchange and retention of the components are reserved for the acute setting.
Question 19
A B C Figures 91a through 91c are CT images of a 76-year-old man who was involved in a motor vehicle collision. Which of the following scenarios would pose a contraindication to closed reduction of this injury prior to MR imaging?
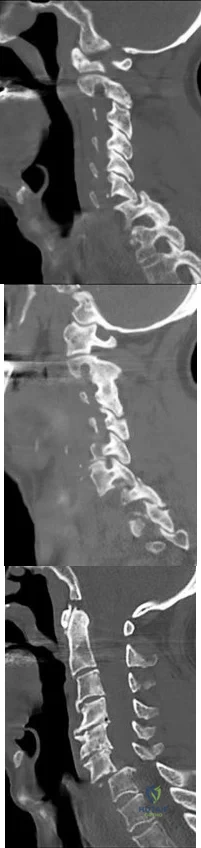
Explanation
This patient has bilateral jumped facet joints at C6-7. Although MR imaging is useful for revealing disk herniations, cord injuries, and bony fragments, early closed reduction to restore anatomic alignment may be attempted prior to MR imaging because reduction will decrease pressure on the cord. There have been reports of catastrophic outcomes with closed reduction in patients who are intubated when disk fragments are pushed into the spinal cord. Consequently, closed reduction should be attempted only in awake and cooperative patients for whom neurologic status monitoring is possible. MR imaging is generally performed after reduction is attempted (successful or not).
RECOMMENDED READINGS
Initial closed reduction of cervical spine fracture-dislocation injuries. Neurosurgery. 2002 Mar;50(3 Suppl):S44-50. Review. PubMed PMID: 12431286. View Abstract at PubMed Radcliff K, Sonagli MA, Delasotta L, Singh N, Morrison E, Levine AM, Vaccaro AR. Cervical facet fractures and dislocations. In: Zigler JE, Eismont FJ, Garfin SR, Vaccaro AR, eds. Spine Trauma. 2nd ed. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2011:441-464.
Vaccaro AR, Falatyn SP, Flanders AE, Balderston RA, Northrup BE, Cotler JM. Magnetic resonance evaluation of the intervertebral disc, spinal ligaments, and spinal cord before and after closed traction reduction of cervical spine dislocations. Spine (Phila Pa 1976). 1999 Jun 15;24(12):1210-7. PubMed PMID: 10382247. View Abstract at PubMed
Wimberley DW, Vaccaro AR, Goyal N, Harrop JS, Anderson DG, Albert TJ, Hilibrand AS. Acute quadriplegia following closed traction reduction of a cervical facet dislocation in the setting of ossification of the posterior longitudinal ligament: case report. Spine (Phila Pa 1976). 2005 Aug 1;30(15):E433-8. PubMed PMID: 16094262. View Abstract at PubMed
Question 20
Staphylococcus aureus develops methicillin resistance through production of which of the following agents?
Explanation
REFERENCES: Fuda C, Suvorov M, Vakulenko SB, et al: The basis for resistance to beta-lactam antibiotics by penicillin-binding protein 2a (PBP2a) of methicillin-resistant staphylococcus aureus. J Biol Chem 2004;279:40802-40806.
Lim D, Strynadka NC: Structural basis for the beta lactam resistance of PBP2a from methicillin-resistant Staphylococcus aureus. Nat Struct Biol 2002;9:870-876.
Schwarz EM: Infections in orthopaedics, in Einhorn TA, O’Keefe RJ, Buckwalter JA (eds): Orthopaedic Basic Science: Foundations of Clinical Practice, ed 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, in press.
Question 21
Figures A and B are post-operative radiographs of a 54-year-old female. In the first 6 months after this procedure, what is the most likely factor for functional impairment in this patient?
Explanation
Anterior knee pain is reported to be a common symptom following treatment of patellar fractures. A likely contributing factor to the anterior knee pain is scarring and tightness of the structures surrounding the knee, as well as patella maltracking due to quadricep/hamstring weakness and/or poor muscle synchrony. Other factors for anterior knee pain may include symptomatic hardware, which may be treated with removal of fixation after union has been achieved.
Lazaro et al. looked at the outcome data on thirty patients with isolated unilateral patellar fractures. Anterior knee pain during activities of daily living was experienced by twenty-four (80%) of the patients. The knee extensor mechanism on the injured side had deficits in strength (-41%), power (-47%), and endurance (-34%) as compared with the uninjured side.
Lebrun et al. reviewed a series of 40 operatively treated patella fractures and found that at over 6 years postoperatively, significant symptomatic complaints and functional deficits persisted based on validated outcome measures as well as objective physical evaluations. Removal of symptomatic fixation was required in 52% of the patients treated with osteosynthesis, whereas 38% of those with retained fixation self-reported implant-related pain at least some of the time.
Figure A and B show AP and lateral radiographs of a comminuted patella fracture treated with a tension band repair construct. The articular surface looks well reduced.
Incorrect Answers:
Question 22
A 70-year-old woman with a body mass index (BMI) of 34 and a history of hypercholesterolemia has elected to undergo total hip arthroplasty. Her son recently learned he has factor V Leiden following an episode of pulmonary embolism. What are this patient's risk factors for thromboembolic disease?
Explanation
Risk stratification is one of the most critical clinical evaluations to undertake before performing total joint arthroplasty. Many factors have been identified that increase the risk for venous thromboembolism (VTE) The major factors include previous VTE, obesity, type of surgery (such as total joint arthroplasty), hypercoagulable states, myocardial infarction, congestive heart failure, family history of VTE, and hormone replacement therapy. Hypercholesterolemia is not a risk factor for thromboembolic disease.
Question 23
A 70-year-old woman has a 3-year history of gradually increasing diffuse and global right knee pain. Her main issues are difficulty with stairs, stiffness with prolonged sitting, and swelling. She has taken NSAIDs and has received intra-articular steroid injections, all with decreasing efficacy. Her right knee examination reveals a range of motion of 15° to 80° with a fixed deformity to varus and valgus stress. Her symptoms are no longer manageable nonsurgically. Radiographs reveal a 30-degree mechanical axis deformity. When using the measured resection technique during total knee arthroplasty (TKA), the best way to avoid femoral malrotation is to reference the
Explanation
In the setting of valgus deformities, TKA poses different challenges than those encountered when varus deformities are present. Most valgus alignment is attributable to a deformity of the distal femur rather than of the proximal tibia, as seen in varus knees. One of the major anatomical differences is a hypoplastic lateral femoral condyle which, when not recognized and used as a rotational reference point, can lead to internal rotation of the femoral component. This malrotation in turn leads to patellofemoral maltracking
or instability, which is a common complication associated with primary TKA.
Question 24
A 24-year-old dancer reports posterior ankle pain when in the “en pointe” position. Examination reveals posteromedial tenderness, no pain reproduction with passive forced planter flexion, and pain with motion of the hallux. What is the most likely diagnosis?
Explanation
REFERENCES: Garrick JG (ed): Orthopaedic Knowledge Update: Sports Medicine 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 249-261.
Hamilton WG, Geppert MJ, Thompson FM: Pain in the posterior aspect of the ankle in dancers: Differential diagnosis and operative treatment. J Bone Joint Surg Am 1996;78:1491-1500.
Question 25
A 30-year-old man requires surgical stabilization of a hypermobile spondylolisthesis of L5 on S1. History reveals that he has smoked one pack of cigarettes a day for 15 years. During preoperative counseling, the patient should be advised to
Explanation
REFERENCES: Silcox DH III, Daftari T, Boden SD, Schimandle JH, Hutton WC, Whitesides TE Jr: The effect of nicotine on spinal fusion. Spine 1995;20:1549-1553.
Deguchi M, Rapoff AJ, Zdeblick TA: Posterolateral fusion for isthmic spondylolisthesis in adults: Analysis of fusion rate and clinical results. J Spinal Disord 1998;11:459-464.
Glassman SD, Anagnost SC, Parker A, Burke D, Johnson JR, Dimar JR: The effect of cigarette smoking and smoking cessation on spinal fusion. Spine 2000;25:2608-2615.
Question 26
A 25-year-old man sustained a head injury after being ejected from his car. Examination reveals a Glasgow Coma Scale score of 7 and a swollen right knee. Clinical examination shows that the knee is very unstable, suggesting tears of the medial collateral and anterior and posterior cruciate ligaments, as well as the posterior lateral corner. What is the most appropriate first step to rule out a vascular injury?
Explanation
REFERENCES: Miranda FE, Dennis JW, Veldenz HC, et al: Confirmation of the safety and accuracy of physical examination in the evaluation of knee dislocation for injury of the popliteal artery: A prospective study. J Trauma 2002;52:247-252.
Mills WJ, Barei DP, McNair P: The value of the ankle-brachial index for diagnosing arterial injury afterknee dislocation: A prospective study. J Trauma 2004;56:1261-1265.
Question 27
Which of the following is considered the most important factor in eliminating infection in chronic osteomyelitis?
Explanation
REFERENCES: Cierny G III, Cook WG, Mader JT: Ankle arthrodesis in the presence of ongoing sepsis: Indications, methods, and results. Orthop Clin North Am 1989;20:709-721.
Cierny G, Zorn EZ: Arthrodesis of the tibiotalar joint for sepsis. Foot Ankle Clin 1996;1:177-197.
Richter D, Hahn MP, Laun RA, Ekkernkamp A, Muhr G, Osterman PA: Arthrodesis of the infected ankle and subtalar joint: Technique, indications and results of 45 consecutive cases. J Trauma 1999;47:1072-1078.
Question 28
An active 66-year-old man who underwent total shoulder arthroplasty 3 years ago now reports pain. Laboratory studies reveal an elevated erythrocyte sedimentation rate and C-reactive protein. Intraoperative frozen section reveals greater than 10 white blood cells per high power field on two slides and the Gram stain reveals gram-positive cocci in clusters. What is the most appropriate surgical treatment to eradicate the infection and maintain function? Review Topic
Explanation
Question 29
Exostoses in which of the following anatomic locations is the most likely to undergo malignant transformation in a patient with multiple hereditary exostosis (MHE)?
Explanation
REFERENCES: Peterson HA: Multiple hereditary osteochondromata. Clin Orthop 1989;239:222.
McCornack EB: The surgical management of hereditary multiple exostosis. Orthop Rev 1981;10:57.
Question 30
A 62-year-old woman has back pain and right L2 radicular pain. MRI scans suggest a neoplastic lesion at L2, and a bone scan is negative except at L2. History reveals that she was treated for breast cancer without known metastatic disease 12 years ago and is thought to be free of disease. What is the next most appropriate step in management?
Explanation
REFERENCE: Fardin DF, Garfin SR, Abitbol J, et al (eds): Orthopaedic Knowledge Update: Spine 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 411-430.
Question 31
What portion of the pitching phase creates forces approaching the tensile limit of the medial ulnar collateral ligament of the elbow? Review Topic
Explanation
Fleisig et al. were among the first to elucidate the elbow and shoulder kinetics in healthy adult pitchers using high-speed motion capture analysis. Inability to generate sufficient elbow varus torque may result in medial tension, lateral compression, or posteromedial impingement injury.
According to Lynch et al. the late cocking phase of the overhand throw places a marked valgus moment across the medial elbow. This repetitive force reaches the tensile limits of the medial collateral ligament, subjecting it to microtraumatic injury and attenuation. The anterior bundle of the medial collateral ligament has been identified as the primary restraint to valgus load and is the focus of reconstruction.
Incorrect Responses:
1,4,5: The medial elbow forces are less during these phases. 4: Ball release is not one of the 5 phases of throwing and marks the end of the acceleration and beginning of deceleration phase.
Question 32
- A skeletal survey is more accurate than a bone scan for detecting skeletal involvement in which of the following neoplastic diseases?
Explanation
Question 33
-Figure is the radiograph of a 55-year-old veteran who developed avascular necrosis after a traumatic hip dislocation. He was treated with hemiarthroplasty 10 years ago and also has posttraumatic stress disorder and chronic pain. He has had multiple spinal surgeries and takes 30 mg of methadone daily. He now has severe groin pain and is unable to ambulate. Laboratory studies showed a C-reactive protein level of 0.2 mg/L (reference range, 0-3 mg/L), erythrocyte sedimentation rate of 50 mm/h (reference range, 0-20 mm/h), hip aspiration of 500/mm3 white blood cell count, 50% polynucleated cells, 30%monocytes, and 20% lymphocytes What is the most likely cause of his hip pain?
Explanation

Question 34
A 32-year-old man sustained an injury to the right thumb metacarpophalangeal (MP) joint ulnar collateral ligament (UCL) and is undergoing surgical repair (Figure 1). What structure in the clinical photograph is blocking reduction of the ulnar collateral ligament?
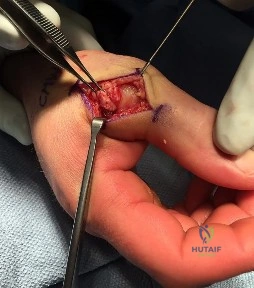
Explanation
When the thumb MP UCL is torn from the proximal phalanx, the distal stump can be displaced superficial to the adductor aponeurosis, known as a Stener lesion. The adductor aponeurosis effectively blocks reduction of the ligament to the normal attachment site. The EPB and EPL tendons are dorsal to the UCL, and the ulnar sesamoid bone/volar plate are in a volar position in relation to the UCL. The dorsal capsule would also not block reduction of the UCL due to it's anatomic location. The other responses do not block the UCL with this type of injury.
Question 35
Figures 1 through 3 show the clinical photographs obtained from a 45-year-old woman who is right-hand dominant. She has pain in the left ring proximal interphalangeal (PIP) joint that gets worse during lifting or gripping activities. On examination, she has PIP range of motion of 15° to 50° with laxity of the radial collateral ligament and tenderness around the joint. The flexor and extensor tendons are intact. She has rotational malalignment when making a composite fist. Radiographs reveal end-stage arthritis at the PIP joint. She elects to move forward with surgery and undergoes arthroplasty. What component of the examination is essential to determine which implant arthroplasty—silicone or surface replacement—is best?
Explanation
This patient has end-stage arthritis in conjunction with ligament insufficiency. The treatment for arthritis is arthroplasty or fusion. Given that her ring finger is affected, arthroplasty is recommended to preserve motion and grip. Two types of arthroplasties are available: silicone and surface replacement. The prerequisites are the same for both and include good bone stock, good sensibility of the joint, adequate soft-tissue coverage, and normally functioning tendons. Adequate collateral ligaments are required for surface replacement arthroplasty. This patient has a deficiency of the radial collateral ligament, evidenced by her clinical examination. Thus, silicone arthroplasty is the recommended option for joint replacement in this patient.
Question 36
Which of the following factors is most associated with malrotation during antegrade or retrograde femoral nailing?

Explanation
According to a review by Hufner et al, malrotation (internal or external >15 degrees) was seen in 22% of their patients via CT scan after intramedullary nailing. There was a significant difference depending on the time of surgery, with significantly more malrotation during the night shift. Increased fracture comminution also significantly increased malrotation rates. No significant increases were seen with the other answers listed above.
Question 37
A 25-year-old professional baseball pitcher reports a 4-month history of gradually increasing medial elbow pain that occurs during the late cocking and acceleration phases of throwing. The pain occasionally refers distally along the ulnar aspect of the forearm. He denies any weakness; however, he notes occasional paresthesias. A nerve conduction velocity study demonstrates increased latency across the cubital tunnel. Management consisting of 6 weeks of rest and rehabilitation fails to provide relief as the symptoms returned when he resumed throwing. What is the best course of action?
Explanation
REFERENCES: Schickendantz MS: Diagnosis and treatment of elbow disorders in the overhead athlete. Hand Clin 2002;18:65-75.
Eaton RG, Crowe JF, Parkes JC III: Anterior transposition of the ulnar nerve using a non-compressing fasciodermal sling. J Bone Joint Surg Am 1980;62:820-825.
Question 38
A 17-year-old high school football player reports wrist pain 5 months after the conclusion of the football season. A radiograph and MRI scan are shown in Figures 29a and 29b. What is the recommended intervention?
Explanation
REFERENCES: Waters PM, Stewart SL: Surgical treatment of nonunion and avascular necrosis of the proximal part of the scaphoid in adolescents. J Bone Joint Surg Am 2002;84:915-920.
Steinmann SP, Bishop AT, Berger RA: Use of the 1,2 intercompartmental supraretinacular artery as a vascularized pedicle bone graft for difficult scaphoid nonunion. J Hand Surg Am 2002;27:391-401.
Question 39
Physiologic bowing of the lower extremities should spontaneously correct by what age?
Explanation
REFERENCES: Abel MF (ed): Orthopaedic Knowledge Update: Pediatrics 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, p 7.
Salenius P, Vankka E: The development of the tibiofemoral angle in children. J Bone Joint Surg Am
J V :
Question 40
The parents of a 10-year-old boy with Down syndrome are seeking sports clearance for participation in the high jump at the Special Olympics. He is asymptomatic, and the neurologic examination is normal. The hips and patellae are clinically stable. Radiographs of the cervical spine in flexion and extension show a maximum atlanto-dens interval (ADI) of 6 mm. Based on these findings, what recommendation should be made?
Explanation
REFERENCES: Atlantoaxial instability in Down syndrome: Subject review. American Academy of Pediatrics Committee on Sports Medicine and Fitness. Pediatrics 1995;96:151-154.
Tredwell SJ, Newman DE, Lockitch G: Instability of the upper cervical spine in Down syndrome. J Pediatr Orthop 1990;10:602-606.
Segal LS, Drummond DS, Zanotti RM, et al: Complications of posterior arthrodesis of the cervical spine in patients who have Down syndrome. J Bone Joint Surg Am 1991;73:1547-1554.
Question 41
A 4-year-old girl who is undergoing chemotherapy for acute lymphocytic leukemia sustains a displaced fracture through an osteolytic lesion in the metaphysis of the distal femur as a result of a fall. Treatment should include
Explanation
Question 42
Figure 11 shows the radiograph of a 3-year-old girl who sustained a proximal radius injury. Appropriate initial management should include
Explanation
REFERENCES: Leung AG, Peterson HA: Fractures of the proximal radial head and neck in children with emphasis on those that involve the articular cartilage. J Pediatr Orthop
2000;20:7-14.
Radomisli TE, Rosen AL: Controversies regarding radial neck fractures in children. Clin Orthop 1998;353:30-39.
Skaggs DL, Mirzayan R: The posterior fat pad sign in association with occult fracture of the elbow in children. J Bone Joint Surg Am 1999;81:1429-1433.
Gonzalez-Herranz P, Alvarez-Romera A, Burgos J, et al: Displaced radial neck fractures in children treated by closed intramedullary pinning (Metaizeau technique). J Pediatr Orthop 1997;17:325-331.
Question 43
Compared to postoperative radiation therapy, preoperative radiation therapy has a higher rate of what complication?
Explanation
REFERENCES: Vaccaro AR (ed): Orthopaedic Knowledge Update 8. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2005, pp 197-215.
Davis AM, O’Sullivan B, Turcotte R, et al: Late radiation morbidity following randomization to preoperative versus postoperative radiotherapy in extremity soft tissue sarcoma. Radiother Oncol 2005;75:48-53.
Question 44
A 14-year-old gymnast misses her dismount off of the uneven bars, hits the mat face first, and loses consciousness for about 15 seconds. She is dazed and confused for several minutes. She does not complain of pain; numbness; or weakness, and she is moving all extremities without deficit. The athlete and coach want to go back to competition that day. How should they be advised?
Explanation
symptoms with cognitive effort. They must be off of medications that could mask or alter concussion symptoms. Neurocognitive testing can be a helpful tool in determining brain function even after all symptoms of concussion have resolved. With a comparison baseline test, this evaluation, in conjunction with a physician's examination, may reduce risk for second impact syndrome. The athlete's clinical neurologic examination findings (cognitive, cranial nerve, balance testing) must return to baseline before resuming exercise. Research has shown that among youth athletes, it may take longer for tested functions to return to baseline (compared with the recovery rate in adult athletes). Brain MRI scan has no role in evaluating athletes for return to play in this situation.
Question 45
A 14-year-old male soccer player was seen initially in the emergency room 1 week ago after an acute right hip injury during a soccer tournament. The patient reports that the hip pain has improved, but still requires crutches for long distance ambulation. His radiograph is seen in Figure A. What would be the next most appropriate step in management? Review Topic
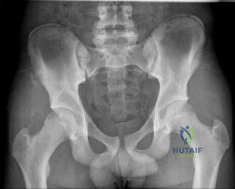
Explanation
The diagnosis of an avulsion fracture of the anterior superior iliac spine is made on the basis of: 1. History (sudden contraction of the sartorial and tensor fasciae latae muscle), 2. Physical findings (tenderness over the anterior superior iliac spine [ASIS] and pain with straight-leg raise), 3. Patient's age (most commonly in adolescents or young adults), and 4. Radiographs (confirmed fracture on standard views of the pelvis). Treatment of these injuries is almost always conservative with crutches and progressive weight-bearing activities as tolerated. The relative indications for operative treatment include displacement of the fracture fragment > 3 cm or painful non-union.
White et al. defined two types of anterior superior iliac spine avulsion fractures. A sartorius avulsion fracture (Type 1) usually occurs when sprinting. The fracture fragment is usually small and displaced anteriorly. The tensor avulsion fracture (Type 2) usually occurs when twisting the trunk (e.g. swinging a bat). This fragment is usually larger than Type 1 fractures and more likely to be displaced laterally.
Holden et al. reviewed pediatric pelvic fractures. They state that avulsion fractures of the anterior superior iliac spine are usually low-energy injures, and are not associated with other life-threatening injuries. They do not require an extensive workup (e.g. CT scanning)
Figure A is an antero-posterior view of the pelvis with a small right-sided avulsion fracture of the anterior superior iliac spine.
Incorrect Answers:
Question 46
A 15-year-old diver has had persistent, activity-related low back pain for the past 2 months. He denies any history of trauma. Examination reveals that the pain is localized to the lumbosacral junction, and there are no radicular symptoms. The pain is worse with back extension. Neurologic examination is normal, as are AP, lateral, and oblique radiographs of the lumbosacral spine. Further evaluation should include
Explanation
REFERENCES: Congeni J, McCulloch J, Swanson K: Lumbar spondylolysis: A study of natural progression in athletes. Am J Sports Med 1997;25:248-253.
Harvey CJ, Richenberg JL, Saifuddin A, Wolman RL: The radiological investigation of lumbar spondylolysis. Clin Radiol 1998;53:723-728.
Question 47
A 55-year-old woman develops posttraumatic arthritis in the elbow following a distal humerus fracture. What is the most likely mid-term (5- 10 years after surgery) complication following semiconstrained total elbow arthroplasty (TEA)?
Explanation
60°, and passive forward shoulder flexion of 160°. He has 2/5 forward flexion and external rotation strength. Initial plain radiographs are unremarkable. A coronal MRI scan of his shoulder is shown in Figure 1. After a thorough discussion, the patient elects to proceed with surgical intervention. During intraoperative assessment, the surgeon contemplates performing a single versus a dual row repair. Currently, what is the consistent difference between the two repair techniques?
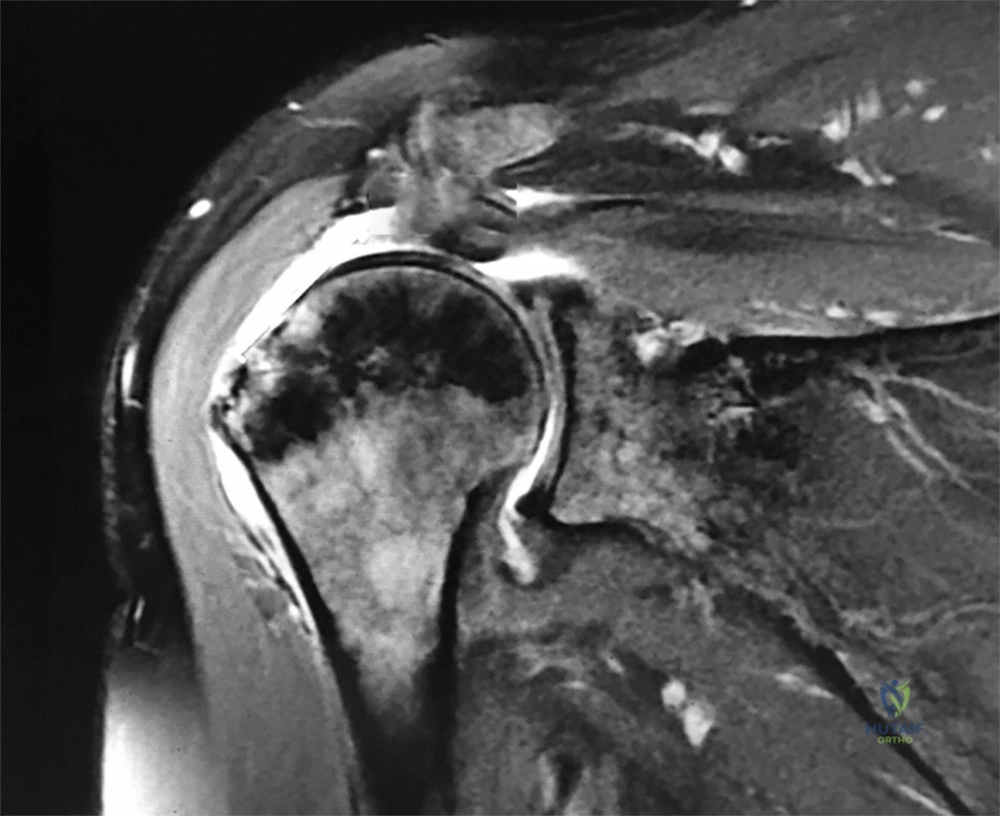
A. Dual row repairs result in superior objective clinical outcomes
B. Dual row repairs provide a larger footprint coverage.
C. Single row repairs have a reported higher complete retear rate.
D. Single row repairs have fewer points of tendon fixation.
Question 48
Delayed-onset muscle soreness (DOMS) is initially evident at the muscle tendon junction and can spread throughout the entire muscle. It is primarily associated with what type of exercise? Review Topic
Explanation
Question 49
A 75-year-old man has persistent radial sided hand and wrist pain. Radiographs demonstrate severe scaphotrapezial trapezoidal arthritis. His basal joint is unaffected. His pain has failed to improve with bracing, activity modification, and image-guided corticosteroid injection. He has elected surgical treatment. What longterm complication can arise from a distal scaphoid resection?
Explanation
Resection of the distal pole of the scaphoid eliminates the arthritic contact at the scaphotrapeziotrapezoid joint; however, it functionally shortens the scaphoid. Theoretically, the lunate is at equilibrium between the extension moment of the capitate and the triquetrum and the flexion moment of the scaphoid. Shortening the scaphoid allows the extension moment of the triquetrum to predominate, pulling the lunate into extension and creating a DISI deformity. Concomitant capsulodesis or interposition is recommended by some authors to prevent this complication.
Question 50
Figure 21 is the radiograph of a 45-year-old woman who was severely injured in a motorcycle crash. Her injuries include a traumatic subarachnoid hemorrhage, bilateral pneumothoraces with pulmonary contusions and flail chest, fracture-dislocation of the left hip, and open fractures of the right distal femur and proximal tibia. Antibiotics and tetanus are administered in the emergency department. The patient is intubated and bilateral chest tubes are placed. A closed reduction is performed on the left hip. After appropriate resuscitation, what is the most appropriate initial management of the right knee injury?
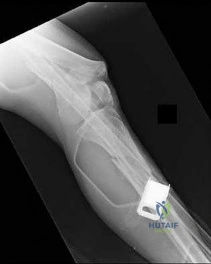
Explanation
Question 51
A 58-year-old woman has had a painless periscapular mass for the past year. An MRI scan and biopsy specimen are shown in Figures 4a and 4b. What is the most likely diagnosis?
Explanation
REFERENCES: Briccoli A, Casadei R, Di Renzo M, Favale L, Bacchini P, Bertoni F: Elastofibroma dorsi. Surg Today 2000;30:147-152.
Enzinger FM, Weiss SW: Soft Tissue Tumors, ed 3. St Louis, MO, Mosby Year Book, 1995, pp 165-201.
Question 52
A full-term newborn has webbing at the knees, rigid clubfeet, a Buddha-like posture of the lower extremities, and no voluntary or involuntary muscle action at and below the knees. Radiographs of the spine and pelvis reveal an absence of the lumbar spine and sacrum. What maternal condition is associated with this diagnosis?
Explanation
REFERENCES: Chan BW, Chan KS, Koide T, et al: Maternal diabetes increases the risk of caudal regression caused by retinoic acid. Diabetes 2002;51:2811-2816.
Zaw W, Stone DG: Caudal regression syndrome in twin pregnancy with type II diabetes.
J Perinatol 2002;22:171-174.
Question 53
A 14-year-old boy sustained a 100% displaced distal radius Salter-Harris type II fracture. Neurologic examination demonstrates normal motor examination and two-point discrimination. He undergoes fracture reduction to the anatomic position with the application of a long arm cast. Postreduction he reports increasing hand and wrist pain with diminution of two-point discrimination to 10 mm over the index and middle fingers over the next several hours after surgery. The cast is bivalved and the padding released relieving all external pressure over the arm. Reevaluation reveals increasing sensory deficit over the affected area. What is the next most appropriate management intervention?
Explanation
Question 54
Figure 109 is the radiograph of an 11-year-old boy who felt a snap in his right hip while jumping hurdles during track practice yesterday. He complains of pain to his right groin region and is walking with a limp. What physical examination test will cause the patient to experience the most discomfort?
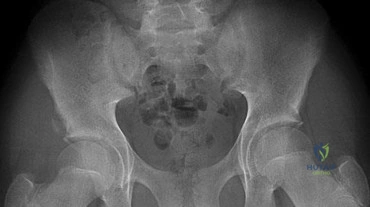
Explanation
Question 55
Which of the following is the only nonreversible effect of anabolic steroids? Review Topic
Explanation
Question 56
Figure 4a shows the radiograph of a 20-year-old man who has an injury to the right shoulder. Figure 4b shows an arthroscopic view (posterior portal). The arrow points to a Review Topic
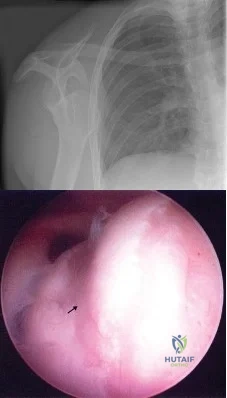
Explanation
Question 57
The patient in Figure 99 has pain at the first MTP joint.
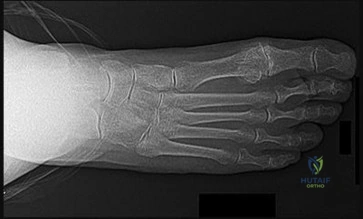
Explanation
General principles can be used as bunion surgery guidelines even though there is extensive debate on the topic. A distal metatarsal osteotomy is most appropriate for patients with mild deformity and no transfer metatarsalgia. A proximal osteotomy potentially can correct more severe
deformities. A lapidus procedure, or tarsometatarsal fusion, provides the highest potential to correct deformity plus the advantage of stabilizing the first tarsometatarsal joint and limiting or eliminating transfer metatarsalgia. A first MTP fusion is most appropriate for patients with severe first MTP arthrosis.
RECOMMENDED READINGS
Easley ME, Trnka HJ. Current concepts review: hallux valgus part II: operative treatment. Foot Ankle Int. 2007 Jun;28(6):748-58. Review. PubMed PMID: 17592710.View Abstract at PubMed
Coughlin MJ, Shurnas PS. Hallux rigidus. Grading and long-term results of operative treatment. J Bone Joint Surg Am. 2003 Nov;85-A(11):2072-88. PubMed PMID: 14630834. View Abstract at PubMed
Question 58
Which of the following best describes the relative content of the components of articular cartilage in decreasing order?
Explanation
REFERENCE: Schiller AL: Pathology of osteoarthritis, in Kuettner KE, Goldberg VM: Osteoarthritic Disorders. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1995,
pp 95-101.
Question 59
Figure 31 shows the radiograph of a 64-year-old woman who is seen in the emergency department following a motor vehicle accident. She has no voluntary motor function in her distal upper extremities or lower extremities. She does not have a bulbocavernosus reflex. She has a blood pressure of 80/50 mm Hg with a pulse of 50/min. Her hypotension does not improve with initial fluid resuscitation. Further treatment of her hypotension should consist of
Explanation
REFERENCES: Spivak JM, Connolly PJ (eds): Orthopaedic Knowledge Update: Spine 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 179-187.
Nockels RP: Nonoperative management of acute spinal cord injury. Spine 2001;26:S31-S37.
Question 60
A 20-year-old woman sustained the closed injury shown in Figures 49a and 49b in a motor vehicle accident. Examination reveals that this is an isolated injury; however, she has a complete radial nerve palsy. Management should consist of
Explanation
REFERENCES: Ring D, Chin K, Jupiter JB: Radial nerve palsy associated with high-energy humeral shaft fractures. J Hand Surg Am 2004;29:144-147.
Foster RJ, Swiontkowski MF, Bach AW, et al: Radial nerve palsy caused by open humeral shaft fractures. J Hand Surg Am 1993;18:121-124.
Question 61
A 74-year-old woman has had acute medial right knee pain for the past 3 months. She denies any history of trauma or previous problems. Coronal and sagittal MRI scans are shown in Figures 11a and 11b. What is the most likely diagnosis? Review Topic
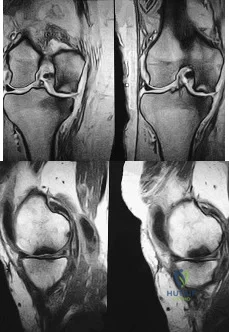
Explanation
Question 62
The transverse diameter of the pedicle is most narrow at which of the following levels?
Explanation
REFERENCES: O’Brien MF, Lenke LG, Mardjetko S, et al: Pedicle morphology in thoracic adolescent idiopathic scoliosis: Is pedicle fixation an anatomically viable technique? Spine 2000;25:2285-2293.
Vaccaro AR, Rizzolo SJ, Allardyce TJ, et al: Placement of pedicle screws in the thoracic spine: Part I. Morphometric analysis of the thoracic vertebrae. J Bone Joint Surg Am
1995;77:1193-1199.
Question 63
Figures below show the radiographs, and the CT obtained from a 58-year-old woman who underwent cementless left total hip arthroplasty. Nine months after surgery, she continued to have groin pain when actively flexing her hip. She has trouble walking up stairs and getting out of her car. What is the most likely diagnosis?
Explanation
Groin pain after total hip replacement has a number of possible causes, and an exact diagnosis may remain elusive in some patients. Infection should be ruled out with laboratory studies and, if indicated, diagnostic aspiration of the hip joint. Implant loosening should be evaluated by plain radiograph and bone scan, if indicated. Synovitis resulting from wear debris should be considered in patients with polyethylene liners who experience late-onset symptoms or in any patient with a metal-on-metal bearing. This patient's symptoms are classic for iliopsoas tendonitis. Physical examination usually reveals pain and weakness with resisted hip flexion. A cross-table lateral radiograph and CT show that the anterior edge of the acetabulum protrudes beyond the anterior wall, thereby acting as a source of iliopsoas tendon irritation. In such cases, acetabular component revision and repositioning are indicated. Fluoroscope-guided iliopsoas cortisone injection can help to establish the diagnosis and relieve groin pain. If the acetabular component is well positioned, then iliopsoas tenotomy should be considered.
Question 64
Benign Ethnic Neutropenia is more common in males.
Explanation
Access to pediatric orthopaedic management has been well investigated. Numerous Level 4 studies have shown that orthopaedic offices in urban and rural areas prefer treating patients with private insurance over patients with Medicaid.
Iobst et al. telephoned 100 urban and rural orthopaedic outpatient offices to schedule an appointment for a 10-year-old patient with a forearm fracture. They showed that 8/100 offices would schedule an appointment within 1 week to the child with Medicaid insurance, as compared to 36/100 that gave an appointment to a child with private insurance.
Pierce et al. contacted 42 orthopaedic practices to schedule an appointment for a 14- year-old patient with an ACL injury. They showed that 38/42 offices scheduled an appointment for the child within 2 weeks with private insurance. This compared to 6/42 that scheduled an appointment for a similar child with Medicaid.
Incorrect Answers:
The perioperative use of which medication has been shown to increase the risk of post-operative infection following orthopaedic procedures in patients with rheumatoid arthritis (RA)?
Naproxen
Leflunomide
Sulfasalazine
Etanercept
Aspirin
Of the medications listed, only etanercept has been shown to increase the risk of post- operative infection following orthopaedic procedures in patients with RA.
Etanercept is a TNF-alpha antagonist with a short half-life that is administered once or twice weekly in patients with RA. Since TNF-alpha plays a central role in the pathogenesis of RA and is instrumental in causing joint destruction, the inhibition of this molecule has shown excellent results in controlling disease. The most powered study on TNF-alpha inhibitor use in the perioperative period following an orthopaedic procedures demonstrated a significant increase in
post-operative infection.
Howe et al. review the medical management of patients with RA who underwent orthopaedic procedures. They state that while there is conflicting information regarding TNF-alpha antagonists, they recommend holding them prior to major orthopaedic interventions.
Giles et al. review 91 patients with rheumatoid arthritis who underwent an orthopaedic procedure. They found TNF-alpha inhibitor therapy to be significantly associated with the development of a serious postoperative infection (p=.041)
Perhala et al. review 61 patients with RA who were treated with methotrexate during the perioperative period surrounding a total joint arthroplasty. They
failed to find a significant increase in complications in this patient group, stating the perioperative use of methotrexate does not affect wound healing or increase the likelihood of periprosthetic infection.
Illustration A shows the site of action of TNA-alpha inhibitors in the RA pathway.
Incorrect Answers:
Communication breakdown is the leading cause of which of the following?
Delayed diagnoses
Medication errors
Surgical site infections
1 and 2
All of the above
Communication failures are the leading cause of wrong side surgeries, medication errors and diagnostic delays.
Poor communication sets up environments in which medical errors can take place. Per the Joint Commission, medical errors may be the among the top 10 causes of death in the United States. Establishing open lines of communication is critical to reduce the risk of error and enhance patient safety.
Gandhi et al. designed a framework to study missed or delayed diagnoses and their causes. The most significant factors contributing to errors were poor handoffs, failures in judgment, failures in memory and failures in knowledge.
O’Daniel et al. review the importance of professional communication and collaborative team efforts. They note that patient safety is at risk when poor communication is in place. The leading cause for medication errors, treatment delays and wrong-site surgeries is communication failure.
Illustration A shows the leading causes of death in the United States. This includes “preventable errors” as a cause.
Incorrect Answers:
treatment, medication errors and wrong side surgery
Which of the following is true regarding osteoprotegerin (OPG)?
It is secreted by osteoclasts
It increases bone resorption
Binds to prostoglandin E2 before stimulating osteoclasts
Osteoprotegerin knock-out mice develop osteopetrosis
Binds to and sequesters RANKL
Osteoprotegerin is a decoy receptor for RANKL. Binding to RANKL causes decreased production of osteoclasts by inhibiting the differentiation of osteoclast precursors.
Bone resporption/remodeling is a complex process regulated by a large variety of molecules. Molecules that have shown to inhibit osteoclasts include OPG, calcitonin, estrogen, TGF-B, and IL-10. Corticosteroids have been shown to decrease production of OPG, thereby enhancing osteoclast formation and longevity. Prolia, or denosumab, is a newly approved drug used to treat osteoporosis and has a mechanism of action similar to osteoprotegerin
(inhibits binding of RANKL to RANK).
Boyle et al. review osteoclast differentiation and activation. The authors state that targeted disruption of OPG causes increased osteoclastogenesis and/or activation resulting in osteopenia.
Illustration A shows how OPG binds to RANKL inhibiting the stimulation of osteoclasts.
Incorrect Answers:
A 55-year-old woman has T-score -2.0 at the femoral neck. According to the World Health Organization Fracture Risk Assessment Tool (FRAX), she has a ten- year probability of sustaining a hip fracture of 1.5% and a ten-year probability of sustaining a major osteoporotic fracture of 8.9%. Which of the following statements is true regarding her antiresorptive therapy management?
Antiresorptive therapy should be started based on her T-score
Antiresorptive therapy should be started based on her risk of hip fracture alone
Antiresorptive therapy should be started based on her risk of major osteoporotic fracture alone
Antiresorptive therapy should not be started
Antiresorptive therapy should be started based on her risks of both hip fracture and major osteoporotic fracture
This patient has osteopenia. Assessment by FRAX shows that ten-year risk of hip fracture is less than 3% and her ten-year risk of major osteoporosis- related fracture is less than 20%. Therefore, antiresorptive therapy is not indicated at this time.
According to the 2008 National Osteoporosis Foundation guidelines, pharmacologic treatment for osteoporosis should be considered if patients are
postmenopausal women or men greater than 50 years old AND meet one of the following criteria: (1) they have a prior hip or vertebral fracture, (2) they have a T score -2.5 or less at the femoral neck or spine, (3) they have a T score between -1.0 and -2.5 at the femoral neck or spine AND a 10-year risk of hip fracture greater than 3% or 10-year risk of major osteoporosis-related fracture greater than 20%.
FRAX (World Health Organization Fracture Risk Assessment Tool) calculates
year risk of fracture based on the following variables: age, sex, race, height, weight, BMI, history of fragility fracture, parental history of hip fracture, use of oral glucocorticoids, secondary osteoporosis and alcohol use to calculate 10-year risk of fracture.
Unnanuntana et al. reviewed the assessment of fracture risk. Besides FRAX score and T-score, they discussed biochemical markers of bone formation and resorption, which are useful for monitoring the efficacy of antiresorptive / anabolic therapy, and may help identify patients at high risk for fracture.
Ekman et al. reviewed the role of the orthopaedic surgeon in minimizing mortality and morbidity associated with fragility fractures. The surgeon should consider prescribing appropriate medications, physical therapy, assessing fall risk and preventing falls and changing lifestyle factors (exercise, smoking and alcohol).
Illustration A shows the FRAX online tool (http://www.shef.ac.uk/FRAX/tool.aspx?country= =9).Illustration B shows the clinical risk factors considered in FRAX calculation.
Incorrect Answers:
A 32-year-old runner sustains a trimalleolar left ankle fracture. She undergoes open reduction and internal fixation and is kept non- weightbearing after surgery. At 2 months, what changes will occur in the articular cartilage of both her knees as a result of her current weightbearing regimen?
Cartilage thickening in the left (ipsilateral) knee and no change in cartilage thickness in the right (contralateral) knee
Cartilage thinning in both knees
Cartilage thinning in the left (ipsilateral) knee and no change in cartilage thickness in the right (contralateral) knee
Cartilage thinning in the left (ipsilateral) knee and increased cartilage thickness in the right (contralateral) knee
Increased cartilage thickness in both knees
After a period of off-loading, the off-loaded limb will experience cartilage thinning. The contralateral limb will not demonstrate any cartilage changes.
Physiologic loading of cartilage increases proteoglycan synthesis and cell proliferation and is chondroprotective. Joint immobilization leads to cartilage thinning, tissue softening, and reduced proteoglycan content, leading to cartilage erosion. Joint overuse leads to cartilage damage (in vitro only).
Hinterwimmer et al. examined cartilage atrophy after partial load bearing
using quantitative MRI. They found cartilage thinning in all knee compartments (greatest thinning, medial tibia; least thinning, patella). There was no change in cartilage morphology in the contralateral knee.
Sun reviewed the relationship between mechanical loading and cartilage degeneration. In OA, cartilage breakdown occurs at the articular surface, and is then fueled by synovial proteases and cytokines. In RA, synovial cells and macrophages are the source of degradative enzymes and incite cartilage destruction.
Milward-Sadler et al. examined mRNA levels following mechanical stimulation in normal and osteoarthritic chondrocytes. Normal chondrocytes showed increased aggrecan mRNA and decreased matrix metalloproteinase 3 (MMP-3) mRNA after stimulation. This
chondroprotective response was absent in osteoarthritic chondrocytes.
Illustration A shows pro- and anti-inflammatory mechanisms of mechanical loading on chondrocytes. Underloading and overloading induce cartilage damage through pathways involving the upregulation of MMPs and ADAMTSs (ADAMTS, a disintegrin and metalloproteinase with thrombospondin motifs, or aggrecanase). Physiological loading blocks these increases.
Incorrect Answers:
A morbidly obese 40-year-old man is scheduled to undergo hemilaminectomy for resection of an painful osteoid osteoma of the T6 lamina. He is positioned prone on a Jackson table and localization is performed with intraoperative fluoroscopy prior to the start of the case. At close to the end of the case, intraoperative frozen section reveals only normal bone fragment from the resected lamina. A probe is placed and a cross-table lateral radiograph reveals that the T7 lamina was resected instead of T6. At this point, the surgeon should
do all of the following EXCEPT
Complete the surgery
Abort the case and obtain further imaging
Apologize to the patient and family
Formally document the error in the operative report
Inform the patient and family immediately after the operation
Fluoroscopic localization of the correct thoracic vertebra can be difficult in the obese
patient. Upon detection of wrong level surgery, he should not abort the case. Rather, he should perform the desired procedure at the correct site, and advise the patient and family upon completion.
Adverse events are inevitable. The correct action following wrong-site surgery is to perform the desired procedure at the correct site followed by frank and honest communication with the patient/family. Open, honest communication favorably affects patient behavior, health outcomes, patient satisfaction, and often reduces the incidence of medical professional liability actions. The
discussion should include a disclosure of known facts and an explanation as to the likely cause, as well as ongoing treatment, follow up care, and prognosis.
The AAOS Information Statement about Wrong Site Surgery identifies 3 treatment steps following discovery of an error during surgery under general anesthesia: Return the patient to his preoperative condition, perform the correct procedure at the correct site, and advise the patient and family of what occurred and the likely consequences, if any, of the wrong- site surgery.
The AAOS Information Statement on Communicating Adverse Events states that the surgeon has an ethical and professional obligation to disclose the error to the patient and/or family. Disclosure should include what happened, why it happened, health implications, and what measures are being instituted to prevent recurrences.
Incorrect Answers:
All of the following are Standards of Professionalism relating to interactions with industry for practicing orthopaedic surgeons EXCEPT:
Decline gifts from industry with a market value over $100 (unless they are medical textbooks or patient educational materials)
Disclose to the patient any financial arrangements with industry that relates to the patient's treatment
Accept no direct financial inducements from industry for utilizing a particular implant
Disclose any relationship with industry to colleagues who may be influenced by your work
Decline to participate in industry sponsored non-CME courses or
conferences
The AAOS has adopted the Standards of Professionalism (SOP). These SOP’s establish mandatory, minimum levels of acceptable conduct for fellows and members of the AAOS to engage in relationships with industry. There are 17 standards with relation to industry. Answer choice 5 is not a SOP as surgeons are allowed to participate in or consult in meetings that are conducive to the effective exchange of information. The SOP also stipulate that tuition, travel, and modest hospitality (including meals and receptions) are allowed to attend an industry-sponsored non-CME course.
A prospective randomized trial is conducted to test the efficacy of Vitamin C versus placebo in treating patients who develop chronic regional pain syndrome (CRPS) after distal radius fractures. At first follow-up, the rates of CRPS are 1% and 9% in the study and placebo group, respectively. Which statistical test is most appropriate to determine significance?
Single factor analysis of variance
Chi-square test
Student t-test
Mann-Whitney rank sum test
Wilcoxon rank sum test
In the study provided, we need to determine whether distributions of categorical variables differ from one another. The appropriate study is the chi- square test.
Data can be classified as numerical (continuous) or categorical (proportional). Responses to such questions as "What is your major?" or Do you own a car?" are categorical because they yield data such as "biology" or "no." In contrast, responses to such questions as "How tall are you?" or "What is your G.P.A.?" are numerical. When comparing two independent means from numeric data, a t-test is performed. However, if categorical data is being compared, the chi- square test will determine if the proportions are really different.
Kocher et al. review basic clinical epidemiology and biostatistics relevant to orthopaedic surgery. Amongst other things, they describe that data can be summarized in terms of measures of central tendency, such as mean, median, and mode, and in terms of measures of dispersion, such as range, standard deviation, and percentiles.
Illustration A shows an algorithm for determining which test to use for varying data. Incorrect Answers:
distributed.
A 35-year-old patient is involved in a motor vehicle accident and sustains multiple fractures including a closed comminuted proximal meta-diaphyseal tibia fracture. The surgeon is considering bridge plating the fracture using a minimally invasive approach. Which of the following is true regarding bridge plating?
A locked plate construct (locked screws) or hybrid construct (locked and non- locked screws) is necessary.
Periosteal stripping is performed through two incisions proximal and distal to the fracture.
Bridge plating is performed following direct reduction of the fracture.
AO Type A diaphyseal fractures are best treated with this technique.
Bridge plating with a long working length creates a flexible, axially stable construct.
In bridged plating, only the most proximal and distal screw holes are filled. This creates a flexible, axially stable construct.
Bridge plating is applicable to all long-bone fractures with complex fragmentation and where intramedullary nailing or conventional plate fixation is not suitable. The construct preserves the blood supply to the fracture fragments as the fracture site is undisturbed during the operative procedure. It provides RELATIVE stability, allowing for some motion at the fracture site, leading to callus formation and secondary bone healing. The construct is FLEXIBLE because of increased distance between the 2 screws closest to the fracture (long working length), allowing for stress distribution and permitting more motion at the fracture site. The construct is also AXIALLY STABLE because the plate acts as an extramedullary splint and resists axial compression.
Livani et al. advocate using an anterior or antero-lateral approach for minimally invasive plating of the humerus. They recommend that distal access is obtained first, allowing identification of the lateral antebrachial cutaneous nerve. For distal fractures, they recommend extending the plate down to the lateral column.
Apivatthakakul et al. defined minimally-invasive plate osteosynthesis (MIPO) danger zones from the lateral epicondyle. They found the musculocutaneous nerve averaged 18- 43% of the humeral length, the danger zone for the radial nerve averaged 36-59% of the humeral length, and the most dangerous screws that penetrated or touched the radial nerve lay 47-53% of the humeral length.
Illustration A shows a distal tibia fracture. Illustration B shows radiographs 5 months after bridge plating of this fracture. There is callus formation, characteristic of indirect bone healing.
periosteal blood supply is critical.
Which of the following components of bone is most responsible for compressive strength?
Type I collagen
Osteocalcin
Proteoglycans
Osteonectin
Osteopontin
Proteoglycans, in addition to calcium hydroxyapatite [Ca10(PO4)6(OH)2], are most responsible for providing compressive strength.
Bone is composed of both organic and inorganic components. Inorganic components include calcium hydroxyapatite and osteocalcium phosphate. Organic components include collagen, proteoglycans, matrix proteins, cytokines and growth factors. While Type I collagen is responsible for providing the tensile strength of bone, proteoglycans and calcium hydroxyapatite [Ca10(PO4)6(OH)2] are most responsible for providing compressive strength. Proteoglycans contain a core protein with various
numbers of covalently attached side chains of glycosaminoglycans. In addition to providing compressive strength, they are also responsible for binding growth factors and inhibiting mineralization.
Knothe et al. review the osteocyte. They discuss that osteocytes are the most abundant
cells in bone, are actively involved in maintaining the bony matrix, and may act as mechanosensors.
Illustration A shows a proteoglycan aggregate, which can form when individual molecules link onto a chain of hyaluronic acid.
Incorrect Answers:
A prospective, randomized controlled trial of 150 patients undergoing total hip arthroplasty is performed to test whether repair of the capsule during a posterior approach reduces post-operative dislocations in the first three months. The study found no difference in dislocation rate if the capsule was repaired versus not repaired (p =
.34). Subsequently, a multicenter follow-up study of 2000 patients showed that repairing the capsule led to a decreased dislocation rate
in the first three months (p = .03). Assuming the second study reflects reality, which of the following errors occurred in the first study?
Observer bias
Type-II error
Alpha error
Type-I error
Confounding error
In this situation, the null hypothesis was accepted when it should have been rejected.
This is a type-II error.
A study can have two types of errors. Type-I errors, or alpha errors, occur when the null hypothesis is rejected when it should have been accepted. The alpha level refers to the probability of a type-I error. By convention, the alpha level of significance is set at 0.05, which means that we accept the finding of a significant association if there is less than a one in twenty chance that the observed association was due to chance alone. Type-II errors, or beta errors, occur when the null hypothesis is accepted when it should be rejected. This
often occurs when studies are underpowered. In the example above, the null hypothesis is that repair of the capsule does not reduce dislocations within the first three months. Since the first study did not show a statistically significant difference, the null hypothesis was accepted. Since a more powered study showed that repair of the capsule does reduce dislocations, the null hypothesis should have been rejected in the initial study (if it was adequately powered).
Fosgate et al. review the importance of sample size calculations when performing research. They state that sample size ensures statistical significance if the subsequent data collection is perfectly consistent with the assumptions made for the sample size calculation (assuming power was set as
50% or greater).
Illustration A shows the difference between type-I and type-II errors. Video V is a lecture discussing statistical definition review of PPV, NPV, sensitivity and specificity.
Incorrect Answers:
that properly constructed studies attempt to avoid.
Which of the following is a potential cause of fretting corrosion?
The micromotion at the femoral head-neck junction in a modular total hip replacement
A stainless-steel cerclage wire is in contact with a titanium-alloy femoral stem
Friction between polyethylene liner and femoral head leading to osteolysis
The formation of pits within a stainless-steel plate and the subsequent release of metal ions
The formation of an adherent oxide coating on titanium implants
Micromotion at the femoral head-neck junction can lead to fretting corrosion, one of the most common causes of failure of a modular implant.
Modular components give surgeons excellent intraoperative flexibility, but are susceptible to various types of corrosion. While titanium and cobalt-chrome contain a protective surface oxide layer, continued micromotion at the modular junction may disrupt the protective layer leading to fretting corrosion, defined as micromotion at contact sites under load. This may eventually lead to a painful synovitis that necessitates a revision procedure.
Srinivasan et al. review modularity in total hip arthroplasty. Amongst other things, they discuss the modularity of the femoral head/neck junction, describing the morse taper interlocking system that provides both axial and rotational stability.
Illustration A shows an example of corrosion at the head/neck junction of a total hip arthroplasty.
Incorrect Answers:
Which of the following situations is most likely to decrease sentinel event errors?
Physician and nurse training is lengthened by 20%
Resident hours are decreased to 55 hours per week
An environment is created where all members of the healthcare team feel empowered to express their concerns and beliefs
Holding individuals responsible for errors in clinical judgement
Physicians and nurses are assigned to a smaller number of patients
Creating an environment where all members of the healthcare team feel empowered to express their beliefs increases communication, the key element in decreasing sentinel events.
Research has shown that 70% of sentinel event errors are caused by improper communication. Specific ways to improve communication include effective clinical handover between shifts and breaking down the "hierarchy" so that all members of the team can discuss their expectations and concerns. Barriers to effective communication include distractions, cultural differences, power distance relationships, time pressures, and lack of organization.
Leonard et al. describe specific clinical experiences in the application of surgical briefings, properties of high reliability perinatal care, the value of critical event training and simulation, and benefits of a standardised communication process in the care of patients transferred from hospitals to skilled nursing facilities. They recommend embedding standardized tools and behaviors to bridge differences in communications styles between clinicians.
Incorrect Answers:
Which of the following side effects is most strongly associated with the use of NSAIDs?
Hepatic dysfunction
Renal impairment
Prolonged QTc
Seizures
Hematuria
All NSAIDs have the potential to cause serious renal impairment.
NSAIDs work by inhibiting the cyclooxygenase pathway (COX), which is comprised of the COX-1 and COX-2 pathways. The COX-1 pathway is involved in prostaglandin E2– mediated gastric mucosal protection and thromboxane effects on coagulation, while the COX-2 pathway is mainly involved with the modulation of pain and fever without effect on platelet function. While selective COX-2 inhibitors have a decreased side effect profile, all NSAIDS
have the potential to cause renal impairment and their use should be limited in patients with underlying renal disease.
Horlocker et al. review multimodal pain management in the perioperative setting of a total joint arthroplasty. Specifically, they note that NSAIDs should be used cautiously in patients with underlying renal dysfunction who are to undergo a procedure with major blood loss.
Griffin et al. reviewed 1,799 patients hospitalized for acute renal failure. They found that NSAIDs increased the risk of renal failure by 58% and that NSAID use resulted in 25 excess hospital admissions per 10,000 years of use.
Illustration A shows the COX pathways and their inhibition by NSAIDs. Incorrect Answers:
It is recommended that invasive dental work be completed prior to the initiation of which of the following medications?
Glucosamine
Cholecalciferol
Levothyroxine
Teriparatide
Bisphosphonates
Bisphosphonate therapy combined with invasive dental work increases the risk for development osteonecrosis of the jaw.
Bisphosphonates are a class of drugs that prevent bone mass loss by inhibiting osteoclast resorption. They are used in the treatment of vertebral compression fractures, non- vertebral fragility fractures, osteogenesis imperfecta, multiple myeloma, and avascular necrosis. Because bisphosphonates have been associated with osteonecrosis of the jaw, it is suggested that all invasive
dental work be completed prior to initiation of treatment.
Pazianas et al. (2011) review the safety profile of bisphosphonates. Specifically, they cite gastrointestinal discomfort, atypical femur fractures, osteonecrosis of the jaw, ocular inflammation, and musculoskeletal pain as common side effects. They state there is limited evidence surrounding
bisphosphonate's association with esophageal cancer and atrial fibrillation.
Pazianas et al. (2007) reviewed 11 publications that reported 26 cases of osteonecrosis of the jaw following initiation of bisphosphonate treatment. Age
>60 years, female sex, and previous invasive dental treatment were the most common characteristics of those who developed ONJ.
Illustration A shows the various bisphosphonates and their mechanisms of action. Illustration B shows an example of osteonecrosis of the jaw, a side effect that has been linked to bisphonphonate treatment.
Incorrect Answers:
Figures A and B show radiographs of a 24-year-old female with a soccer injury. A physical examination reveals an isolated, closed injury with no clinical features of neurovascular injury or compartment syndrome. She has been consented to be treated with intramedullary nail fixation. A pre-operative note by the anaesthesiology team makes reference to the patients fair skin and natural red-hair color. How will this information affect the post-operative management of this patient?
Longer duration of anticoagulation due to increased risk of DVT
Avoiding anticoagulation medications due to increased risk of bleeding
Require higher dosages of post-operative analgesia
Longer period of non-weight bearing on surgical limb
Avoiding opioids due to higher risk of unrecognized allergies
Female patients with natural red-hair may require higher dosages of post- operative analgesia compared to other hair types.
Melanocortin-1-receptor (MC1R) is one of the key proteins involved in hair color and skin tone. Mutations of the MC1R alleles can render this protein non- functional, which results in a phenotype of red-hair and fair skin. Mutations of the MC1R have shown to modulate the pain response and opioid efficacy in these patients. Women are more commonly affected and often require more anaesthetic and higher dosages of opioid to achieve comparable MAC level and pain-relief, respectively, as women with other hair types.
Liem et al. showed that a greater concentration of induction and maintenance agents (sevoflurane and desflurane, respectively) were required to sustain comparable MAC levels in red-haired patients as dark haired patients.
Fillingim et al. reviewed the affect of gender, sex and pain. They concluded there is a biopsychosocial element of pain that is perceived differently by men and women. In terms of postoperative and procedural pain, the outcome might be more severe in women than men.
Delaney et al. looked at the involvement of the melanocortin-1 receptor in acute pain in mice. They found that while the MC1R is better known as a gene involved in mammalian hair colour, it was shown to be involved in the pain pathway of inflammatory but not neuropathic origin. Mutations of MC1R showed increased tolerance to noxious pain stimulus in mice.
Figures A and B are AP and lateral radiographs of a left tibia. There is a low energy, distal third shaft fracture with no cortical apposition on the AP view.
Incorrect Answers:
Which of the following medications used for thromboprophylaxis following orthoapedic surgery is a direct inhibitor of factor Xa?
Dextran
Rivaroxaban (Xarelto)
Coumadin
Fondaparinux (Arixtra)
Aspirin
Rivaroxaban (Xarelto), an oral anticoagulant, is a direct inhibitor of factor Xa.
Rivaroxaban (Xarelto) is a member of a new class of oral, direct (antithrombin- independent) factor Xa inhibitors, which restrict thrombin generation both in vitro and in vivo. Inhibition of Factor Xa interrupts the intrinsic and extrinsic pathway of the blood coagulation cascade, inhibiting both thrombin formation and development of thrombi.
Eriksson et al. compare rivaroxaban to enoxaparin for the prevention of symptomatic venous embolism following total hip arthroplasty. Major venous thromboembolism occurred in 4 of 1686 patients (0.2%) in the rivaroxaban group and in 33 of 1678 patients (2.0%) in the enoxaparin group. Additionally, major bleeding events were similar between the two groups.
Illustration A shows the mechanisms of action of various agents used for thromboprophylaxis.
Incorrect Answers:
as Protein C and Protein S.
The origin of bovine derived grafts is particularly important to which of the following religious groups?
Christianity
Islam
Hinduism
Buddhism
Judaism
The origin of bovine-derived surgical implants should be discussed in further detail with patients ascribing to Hinduism.
Patients come from a variety of religious backgrounds. Depending on a patient’s religion, the origin of surgical implants may have implications for their use. In Hinduism, bovine animals are considered sacred. Use of cow by- products is considered purifying in nature. Subsequently, the origin of bovine derived implants should be discussed with patients ascribing to Hinduism.
Easterbrook et al. evaluated the utility of porcine and bovine surgical implants amongst those of Jewish, Muslim and Hindu faiths. Hindu religious leaders, who were surveyed, did not approve of the use of bovine surgical implants.
Enoch et al. evaluated the acceptability of biological products amongst various religious groups. The Hindu religious leaders were found to not have an objection to the use of biological implants derived from cows.
Illustration A shows a clinical photo of a fetal bovine derived dermal substitute. Incorrect Answers:
Immunological testing of anti-cyclic citrullinated peptide antibodies (anti- CCP) is most commonly used for the diagnosis and prognosis of which immunological condition?
Ankylosis spondylitis
Rheumatoid arthritis
Psoriatic arthritis
Systemic lupus erythematosus
Reiter's syndrome
Anti-cyclic citrullinated peptide antibodies (anti-CCP) are commonly used as a marker for the diagnosis and prognosis of rheumatoid arthritis (RA).
Immunological studies are commonly performed to investigate cases of suspected rheumatoid arthritis. Rheumatoid factor has historically been used as a primary marker for RA. However, in more recent years, the use of anti- CCP antibodies has shown to be as sensitive as, and more specific than, rheumatoid factor (RF) in early and fully established disease. In general, anti-
CCP assays equate to a sensitivity of 50-75% and a specificity of 90-95%. High levels of anti-CCP have been shown to be indicative of a more erosive disease process and may be detected before the onset of arthritis.
Gardner and Kadel reviewed the laboratory studies most commonly used in rhuematologic diseases. Standard ordering for clinically suspected RA include Rf, anti- CCP, ESR/CRP as well as other markers of autoimmune diseases such as antinuclear antibodies, anticardiolipin antibodies and lupus anticoagulant, HLA-B27, and uric acid levels.
Illustration A shows the sensitivity and specificity of anti-CCP vs. RF in a variety of autoimmune diseases.
Incorrect Answers:
Vitamin C has been shown to decrease the likelihood of which of the following complications following surgery on the foot and ankle in non-diabetic patients?
Nonunion
Complex Regional Pain Syndrome, type II
Malunion
Complex Regional Pain Syndrome, type I
Wound infection
Vitamin C has been shown to decrease the likelihood of developing complex regional pain syndrome (CRPS), type 1, when given post-operatively to patients undergoing foot and ankle and wrist surgery.
CRPS is a frequent post-operative complication, with rates varying from 10-
37%. Type I CRPS does not have an identifiable nerve lesion, while type II has an identifiable nerve lesion. Multiple studies have shown that vitamin C decreases rates of CRPS following distal radius fractures, and more recently, the same has been shown following foot and ankle surgery. While the exact mechanism of CRPS is unknown, vitamin C has been shown to reduce lipid peroxidation, scavenge hydroxyl radicals, protect the capillary endothelium, and inhibit vascular permeability. All of these characteristics of vitamin C may play a role in modulating the pain pathway.
Zollinger et al. perform a double-blind, prospective, multicenter trial where
416 patients with 427 wrist fractures were randomly allocated to treatment with placebo or treatment with 200, 500, or 1500 mg of vitamin C daily for fifty days. The prevalence of complex regional pain syndrome was 2.4% in the vitamin C group and 10.1% in the placebo group.
Besse et al. compare two groups of patients undergoing surgery on the foot and ankle to determine the effect of vitamin C on the development of CRPS, type I. CRPS type I occurred in 18 cases (9.6%) in the group not given vitamin C, and 4 cases (1.7%) in the group given vitamin C.
Illustration A shows an example of a limb affected by CRPS. Note the increased swelling, a common physical exam finding in patients afflicted with the disease.
Incorrect Answers:
A 25-year-old Spanish speaking male presents to the emergency department 6 hours after sustaining the injury seen in Figure A. He is grossly intoxicated and screaming in pain. Physical examination reveals a closed injury with overlying muscular compartments that are extremely firm to palpation. After sedating the patient, measurements of the intracompartmental pressures were all found to be
>75mmHg. His wife is Spanish speaking and expected to arrive to the hospital in 2-3 hours with a relative to help with translation. No medical translator is
available. You attempt to outline the risk and benefits of surgery to the patient, but the he repeatedly interrupts you and yells out ,"No surgery!". An English-Spanish speaking friend is with the patient and says that he has known the patient for over 2 years and will help with any decision making. What would be the next most appropriate step in the management of this patient?
Delay surgery to monitor the patient for impending compartment syndrome
Proceed with surgery with urgent fasciotomy after documenting the necessity of treatment without consent
Delay the surgery until the wife arrives and able to give informed consent with the aid of a translator
Proceed with surgery for urgent fasciotomy after obtaining informed consent from the patients friend
Respect the patients autonomy and reassess the patient in the morning when he demonstrates capacity to accurately comprehend the proposed treatment
This patient is presenting with compartment syndrome of the right tibia. In a situation of required surgery for limb threatening injury without available legal consent the surgeon should confirm and document the necessity of care with a fellow colleague.
Physicians are responsible for whether a patient is able to reasonably understand their medical condition and the nature of any proposed medical procedure, including the risks, benefits, and available alternatives. If the patient lacks this capacity, disclosure imposed by the doctrine of informed
consent are excused because irreparable harm that may result from the physician’s hesitation to provide treatment. Detailed documentation is also important. In addition, the attending physician should contact the Risk Management Dept at the hospital for support prior to surgical intervention or have a medical translator involved to ensure information is being translated properly.
Katz et al. reviewed the medical decision making process of Hispanic people. They showed that Hispanic people are more likely to permit their physician to take the predominant role in making health decisions compared to Non- Hispanic people.
Figure A shows a comminuted tibia and fibula fracture. Incorrect Answers
A Spanish speaking child sustained the injury seen in Figure A after a fall at school. He was casted in the emergency department without the assistance of an interpreter and advised to return to see an orthopaedic surgeon in 1 week. However, the family returns to the emergency department with the child 3 months later, still in the cast. What is the most likely reason the child did not attend the recommended orthopaedic follow-up visit.?
The child is a victim of neglect
The child had no symptoms of pain
He was allowed to return to school wearing the cast
Concerns of cost
Follow-up instructions were not effectively communicated
The most likely reason the child did not attend the recommended orthopaedic follow-up visit was a language barrier preventing effective communication of the intended follow-up instructions.
Communication skills and cultural competence is a key element in good orthopaedic care. Poor communication can often lead to devastating outcomes. In this example, poor communication resulted in this patient being lost to
follow-up. Language barriers must be accommodated and alternative methods of communication must be utilized.
Levinson et al. examined how patients present their medical issues in clinical encounters and how physicians respond to these clues in routine primary care and surgical settings. They showed that good communication relies mostly on the physicians ability to identify patient clues within the clinical encounter.
Poor communication between the physician tended to delay clinical visits, poor follow-up and unsatisfactory outcomes.
Figure A is an AP radiograph of the elbow in a skeletally immature patient. Figure B is a lateral radiograph of the elbow with a posterior fat pad sign, suggestive of an occult fracture.
Incorrect Answers:
A 25-year-old female presents to the emergency room within increasing left shoulder pain after walking into a door 5 months ago. She previously sustained a femoral fracture 2 years ago after tripping on a rug. Relevant skeletal survey radiographs and tissue biopsy results are shown in Figures A through D. Laboratory investigations show normal glomerular filtration rate and creatinine clearance. Dual energy x-ray absorptiometry (DEXA) scan shows T-score of -1.4 and
-1.2 at the hip and lumbar spine, respectively. Which of the following laboratory values in Figure E most likely reflects this patient's condition?
A
B
C
D
E
This patient has primary hyperparathyroidism. Laboratory investigations are likely to show elevated serum intact parathyroid hormone (PTH), alkaline phosphatase (ALP) and ionized serum calcium, and low serum phosphate.
Primary hyperparathyroidism is most commonly caused by a single adenoma (80-90%). Besides the signs and symptoms of hypercalcemia, patients present
with calcification of menisci and articular cartilage, erosions in hand bones, "salt and pepper skull", and brown tumors (osteoclastomas), which appear as lytic regions expanding the cortex and causing pathological fractures, so named because of hemosiderin deposition.
Singhal et al. reviewed primary hyperparathyroidism. They advocate routine serum calcium levels for patients with pathologic fractures. If this is elevated, total and ionized calcium and intact PTH levels should be obtained. They feel that surgery for orthopaedic stabilization and parathyroidectomy should be performed simultaneously for better outcome.
Mankin et al. reviewed metabolic bone disease. They suggest that patients with mild disease with normal calcium levels do not require treatment. For patients with high calcium levels, treatment should include maintenance of fluid balance, localization and removal of the adenoma, bony stabilization, and medications (calcitonin, estrogen, bisphosphonates, and calcimimetics such as cinacalcet).
Figure A is an AP radiograph showing a lytic expansile lesion with pathological fracture in metadiaphyseal region of left humerus with similar lesion in the
fifth posterior rib. Figure B is an AP radiograph showing a lytic expansile lesion in the third metacarpal of the right hand and the fifth metacarpal of the left hand. Figure C is a low power micrograph of a brown tumor demonstrating a central zone of bone resorption, and filling with fibroblastic tissue, with a peripheral rim of osteoid production. Figure D is a high power micrograph of a brown tumor. In areas of bone resorption, there are numerous osteoclast-like giant cells amidst a fibrous stroma. This is unlike a true giant cell tumor, which lacks a fibrogenic stroma.
Incorrect Answers:
and impaired 1,25-dihydroxyvitamin D production by the diseased kidneys. This patient has normal renal function. Answer 3: Elevated PTH, ALP, serum calcium and phosphate occur in tertiary hyperparathyroidism. This again occurs in chronic renal disease after prolonged chronic secondary hyperparathyroidism or after renal transplantation, where the parathyroid glands become autonomous and PTH levels do not normalize. This patient has normal renal function.
elevated.
FOR ALL MCQS CLICK THE LINK ORTHO MCQ BANK
Question 65
A 38-year-old left hand-dominant bodybuilder reports ecchymosis in the left axilla and anterior brachium after sustaining an injury while bench pressing 3 weeks ago. Coronal and axial MRI scans are shown in Figures 16a and 16b. What treatment method yields the best long-term results? Review Topic
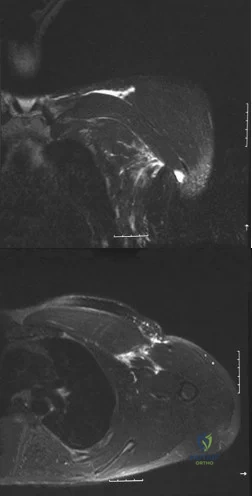
Explanation
Question 66
A 23-year-old woman has had a 3-year history of snapping and pain in her left hip. She notes that the snapping started while marathon training and is only problematic about 15 minutes into a run. Examination is consistent with a negative Stinchfield, negative logroll, negative flexion abduction/external rotation test (FABER) of the hip; however, she has a positive Ober test as she has difficulty adducting her hip across the midline in the lateral decubitus position. Management consisting of nonsteroidal anti-inflammatory drugs and stretching has failed to improve her snapping. What is the most reliable surgical treatment? Review Topic
Explanation
Question 67
- The pharmacologic action of botulinum-A toxin can be best described as
Explanation
Question 68
A 46-year-old patient with cervical myelopathy undergoes a multilevel posterior cervical laminectomy from C3 to C7. The risk of postlaminectomy kyphosis is greatest with removal of which of the following structures?
Explanation
REFERENCE: Zdeblick TA, Abitol JJ, Kunz DN, et al: Cervical stabilization after sequential capsule resection. Spine 1993;18:2005-2008.
Question 69
In the evaluation of somatosensory-evoked potential waveforms for intraoperative neuromonitoring for spinal surgery, the minimum criteria for determining potentially significant changes include Review Topic
Explanation
Question 70
- An infected total knee replacement with symptoms occurring within 4 weeks of surgery and no radiographic signs of osteomyelitis would be best managed with
Explanation
Arthroscopic debridement not recommended secondary to missing cutaneous tracks and soft tissue/muscle involvement.
Question 71
03 A 23 year old sustains an isolated right knee dislocation in an MVA. A closed reduction is performed and confirmed with radiographs. What is the next appropriate study?
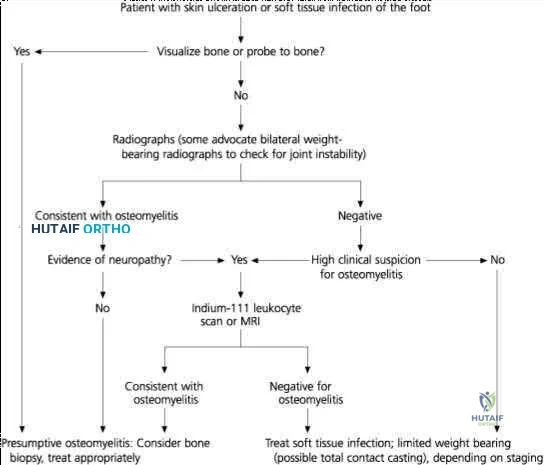
Explanation
OKU Truama 2 says “the use of ABI with the blood pressure cuff and Doppler evaluation of the distal circulation has been proposed as effective in determining any occult vascular injury. A ratio > 0.9indicates a normal study.”[1] The referenced article confirms this. “Confirmation of the safety and accuracy of physical exam in the evaluation of knee dislocation for injury of the popliteal artery.” J. Trauma2002; 52: 247-252
back to this question next question
[1] OKU Trauma 2 pg 151-153
Question 72
A 55-year-old man who works as a carpenter reports chronic right anterior shoulder pain and weakness. Examination reveals 90 degrees of external rotation (with the arm at the side) compared to 45 degrees on the left side. His lift-off examination is positive, along with a positive belly press finding. An MRI scan reveals a chronic, retracted atrophied subscapularis tendon. What is the most appropriate management of his shoulder pain and weakness?
Explanation
REFERENCES: Jost B, Puskas GJ, Lustenberger A, et al: Outcome of pectoralis major transfer for the treatment of irreparable subscapularis tears. J Bone Joint Surg Am 2003;85:1944-1951.
Resch H, Povacz P, Ritter E, et al: Transfer of the pectoralis major muscle for the treatment of irreparable rupture of the subscapularis tendon. J Bone Joint Surg Am 2000;82:372-382.
Question 73
03 A rotational periacetabular osteotomy offers what advantage over a medial displacement pelvic osteotomy for treating adolescent hip dysplasia?

Explanation

The acetabulum remodels until age 8 y/o and it is preferable to treat hip dysplasia (whether it is from DDH or CP) as a child with open growth plates. If hip dysplasia presents as an adolescent, there are two main types of pelvic osteotomies: medial displacement and rotational periacetabular.

Medial displacement osteotomies are Salter, Triple and Shelf / Chiari. The acetabulum itself remains unchanged. These osteotomies can be used for an incruent hip. They provide only lateral acetabular coverage and can be preformed with or without
internal fixation. They often involve multiple incisions. A triple osteotomy involves a Salter cut with cuts of both the superior and inferior rami. The Shelf / Chiari osteotomy is a salvage procedure and is only used as a last resort for femoral containment.

A rotational periacetabular osteotomy is called a Ganz or Bernese. It allows acetabular reorientation and either medial or lateral displacement. The advantages of this procedure is that it provides hyaline cartilage coverage (ans. 4)over the adolescent hip, can be performed with a single surgical approach and preserves the normal shape of the pelvis—permitting normal vaginal delivery. An additional advantage is preservation of blood supply to the acetabular fragments. No complete cut is made, so it is very stable. The disadvantage is that it is technically demanding and often additional training is needed for the surgeon to become comfortable.

Reshaping (incomplete) osteotomies include the Pemberton and Degas require an open triradiate cartilage and can achieve posterior or posterolateral femoral head coverage. This question asked about the adolescent hip.

There is a good review in JAAOS Sept / Oct 1999 pp.325-336.

For the Atlanta crew, remember: God loves a Pemberton.
Question 74
A 4-year-old boy with arthrogryposis has little active motion of his knees or elbows. Both elbows are in full extension with good triceps strength, but he is unable to bring his hand to his face or feed himself. Management should consist of
Explanation
REFERENCES: Van Heest A, Waters PM, Simmons BP: Surgical treatment of arthrogrypsosis of the elbow. J Hand Surg Am 1998;23:1063-1070.
Caroll RE, Hill NA: Triceps transfer to restore elbow flexion: A study of fifteen patients with paralytic lesions and arthrogryposis. J Bone Joint Surg Am 1970;52:239-244.
Question 75
When do most symptomatic thromboembolic events occur after total joint arthroplasty?
Explanation
Most clinical venous thromboembolism events occur between the second and sixth weeks after surgery. It is estimated that 10% of patients are readmitted to the hospital within the first 3 months after total hip or knee arthroplasties. Most pulmonary events on the day of surgery are related to fat embolism or cardiac events.
Question 76
A 17-year-old high school football player is seen for follow-up after sustaining an injury 3 days ago. He reports that he tackled a player, felt numbness throughout his body, and could not move for approximately 15 seconds. A spinal cord injury protocol was initiated on the field. Evaluation in the emergency department revealed a normal neurologic examination and full painless neck motion. He states that he has no history of a similar injury. An MRI scan of the cervical spine is normal. During counseling, the patient and his family should be informed that he has sustained
Explanation
REFERENCES: Morganti C, Sweeney CA, Albanese SA, et al: Return to play after cervical spine injury. Spine 2001;26:1131-1136.
Odor JM, Watkins RG, Dillin WH, et al: Incidence of cervical spinal stenosis in professional and rookie football players. Am J Sports Med 1990;18:507-509.
Torg JS, Naranja RJ Jr, Palov H, et al: The relationship of developmental narrowing of the cervical spinal canal to reversible and irreversible injury of the cervical spinal cord in football players. J Bone Joint Surg Am 1996;78:1308-1314.
Vaccaro AR, Watkins B, Albert TJ, et al: Cervical spine injuries in athletes: Current return-to-play criteria. Orthopedics 2001;24:699-703.
Question 77
A 6-year-old boy presents to the emergency room after falling off a trampoline and landing on his elbow. Examination reveals good radial and ulnar pulses, and a warm, pink, sensate extremity. Radiographs are shown in Figures A and
Explanation
Pulselessness occurs 10-20% of the time following extension type supracondylar fractures. Most authors recommend observation of the pink, pulseless limb as in the majority of cases, vascular spasm will resolve in 12-24 hours and/or the collateral circulation will be adequate. Isolated nerve injuries are usually neuropraxia and can be observed. Pulseless hands with AIN or median nerve palsy warrant early exploration because of the high probability of arterial entrapment at the fracture site, or tethering.
Choi et al. performed a review of 1255 pediatric supracondylar fractures treated at a single institution. There were 33 pulseless fractures (2.6%). All 24 well perfused patients did well postoperatively without vascular repair, although 10 remained pulseless. Of the 9 poorly perfused patients, 4 underwent vascular repair and 2 developed compartment syndrome. They concluded that patients with poor perfusion were at increased risk of vascular repair and compartment syndrome.
Franklin et al. reviewed pediatric supracondylar fractures with neurovascular compromise. They recommend: (1) observation for 48h for the pulseless, well-perfused hand, (2) exploration if the pulse disappears after reduction, (3) exploration for pulseless hands with AIN/median nerve palsy, (4) delay of 8-21 hours did not increase the risk of complications.
Figures A and B are AP and lateral radiographs showing a Gartland type III supracondylar fracture of the humerus.
Incorrect Answers:
Question 78
A 25-year-old man injures his shoulder while skiing. Examination reveals increased passive external rotation, pain in the cocked position, and a positive lift-off test. What is the most likely diagnosis?
Explanation
REFERENCES: Gerber C, Krushell RJ: Isolated rupture of the tendon of the subscapularis muscle: Clinical features in 16 cases. J Bone Joint Surg Br 1991;73:389-394.
Hawkins RJ, Bokor DJ: Clinical evaluation of the shoulder, in Rockwood CA, Matsen FA III (eds): The Shoulder. Philadelphia, PA, WB Saunders, 1990, pp 149-177.
Question 79
A 72-year-old woman who is right hand-dominant has severe pain in the right shoulder that has failed to respond to nonsurgical management. She reports night pain and significant disability. Examination reveals 30 degrees of active forward elevation. An AP radiograph is shown in Figure 27. Which of the following treatment options will provide the best functional improvement?
Explanation
REFERENCES: Frankle M, Siegal S, Pupello D, et al: The reverse shoulder prosthesis for glenohumeral arthritis associated with severe rotator cuff deficiency: A minimum two-year follow-up study of sixty patients. J Bone Joint Surg Am 2005;87:1697-1705.
Werner CM, Steinmann PA, Gilbart M, et al: Treatment of painful pseudoparesis due to irreparable rotator cuff dysfunction with the Delta III reverse-ball-and-socket total shoulder prosthesis. J Bone Joint Surg Am 2005;87:1476-1486.
Question 80
A 56-year-old man sustained a nondisplaced extra-articular fracture of the proximal aspect of the third metatarsal after dropping a heavy object on his left foot. Management should consist of
Explanation
REFERENCES: Myerson MS: Foot and Ankle Disorders. Philadelphia, PA, WB Saunders, 2000, pp 1265-1296.
Early JS: Fractures and dislocations of the midfoot and forefoot, in Rockwood and Green’s Fractures in Adults, ed 5. Philadelphia, PA, Lippincott Williams and Wilkins, 2001,
pp 2181-2245.
Question 81
Reverse total shoulder arthroplasty improves kinematics in the rotator cuff deficient joint by what directional change to the center of rotation? Review Topic
Explanation
Question 82
Figures below depict the radiographs obtained from a 53-year-old man who has had swelling in his right knee for 2 years, with minimal pain. He did not note an injury to the knee but has been unable to ambulate without crutches during this period. His past history is unremarkable, and he denies a history of diabetes or back problems. The social history reveals that he emigrated from China, and he works at a desk job. Physical examination shows a healthy man in no acute distress. Range of motion of the right knee is 5° to 120° actively and 0° to 120° passively, without pain. Sensation is decreased on the bottom of both feet, but otherwise the neurologic examination is unremarkable. Laboratory testing reveals a positive rapid plasma reagin (RPR) test. What is the best next step?
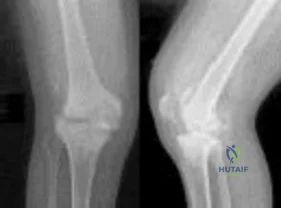
Explanation
This patient has a neuropathic knee caused by neurosyphilis, as shown by the joint destruction on the radiographs, with a lack of pain and a positive RPR test. He has a low-demand job and would be best treated with a hinged knee arthroplasty to provide stability for his knee.
Question 83
A 22-year-old volleyball player has atrophy of the infraspinatus muscle. This deficit is the result of entrapment of what nerve?
Explanation
REFERENCES: Ferretti A, Cerullo G, Russo G: Suprascapular neuropathy in volleyball players. J Bone Joint Surg Am 1987;69:260-263.
Bigliani LU, Dalsey RM, McCann PD, April EW: An anatomical study of the suprascapular nerve. Arthroscopy 1990;6:301-305.
Question 84
A 33-year-old man reports an enlarging painful soft-tissue mass in his right forearm. A radiograph and MRI scans are shown in Figures 45a through 45c. Treatment should consist of
Explanation
REFERENCES: Damron TA: What to do with deep lipomatous tumors. Instr Course Lect 2004;53:651-655.
Gaskin CM, Helms CA: Lipomas, lipoma variants, and well-differentiated liposarcomas (atypical lipomas): Results of MRI evaluations of 126 consecutive fatty masses. Am J Roentgenol 2004;182:733-739.
Rozental TD, Khoury LD, Donthineni-Rao R, et al: Atypical lipomatous masses of the extremities: Outcome of surgical treatment. Clin Orthop Relat Res 2002;398:203-211.
Question 85
The patient undergoes further testing and it is discovered that the lesion encompasses 70% of the joint. What is the best next treatment option?
Explanation
A tarsal coalition is an abnormal connection of 2 or more bones in the foot. Although tarsal coalitions are present at birth, children and adults typically do not show signs of the disorder until early adolescence or later. The exact incidence of the disorder is hard to determine; however, it is caused by a gene mutation that affects cells that produce the tarsal bones. The 2 most common locations for tarsal coalitions are between the calcaneus and the navicular or between the talus and the calcaneus. It is estimated that 1 out of every 100 people may have a tarsal coalition. In 50% of cases, both feet are affected. Tarsal coalitions are rarely discovered until symptoms arise. Symptoms may include stiff and painful feet, a rigid flatfoot, or increased pain or a limp with high-level activities. Upon examination, symptoms may include tenderness in the area of the coalition, loss of motion, rigid flat feet, and arthritic changes of the joint. Imaging studies begin with radiographs. A CT scan can provide bony detail for imaging tarsal coalitions and determining the extent of the coalition and any accompanying degenerative change. MRI can provide details of the soft tissues. Treatment includes nonsurgical care including rest, orthotics, a temporary boot or cast, and injections. Surgical options include resection with interposition of muscle or fatty tissue from another area of the body or fusions when large (exceeding 50% of the joint), more severe coalitions are encountered.
RECOMMENDED READINGS
Lemley F, Berlet G, Hill K, Philbin T, Isaac B, Lee T. Current concepts review: Tarsal coalition. Foot Ankle Int. 2006 Dec;27(12):1163-9. Review. PubMed PMID: 17207452. View Abstract at PubMed
Badgley CE. Coalition of the calcaneus and the navicular. Arch Surg. 1927;15:75-88. Conway JJ, Cowell HR. Tarsal coalition: clinical significance and roentgenographic demonstration. Radiology. 1969 Mar;92(4):799-811. PubMed PMID: 5767760. View Abstract at PubMed
Herzenberg JE, Goldner JL, Martinez S, Silverman PM. Computerized tomography of talocalcaneal tarsal coalition: a clinical and anatomic study. Foot Ankle. 1986 Jun;6(6):273-
Question 86
During fracture healing, granulation tissue tolerates the greatest strain before failure so that mature bone can eventually bridge the fracture gap during healing. What is the definition of strain?
Explanation
The mechanical environment at the fracture site has a major influence on fracture healing. Granulation tissue can withstand higher strain, which stabilizes the mechanical environment and forms a scaffold on which cartilage and bone eventually form; this occurs after strain decreases incrementally. Optimal healing, however, depends on duration, rate, timing and type of mechanical influence. Bone is formed by osteoblasts that are adapted to the very low strains of over 1% change in length. Osteoblast synthesis and proliferation is stimulated at uniaxial strain of between 0.3% and 2.8%. It is known that limited inter-fragmentary movement of 0.2 mm to 1 mm is optimal for fracture healing, resulting in promotion of callus and increase in rigidity. Excessive movement, on the other hand, prolongs fracture healing. Researchers have identified that tissue strain of 2% is suitable for primary bone healing and secondary bone healing takes place at tissue strain of 2-10%. Strain of 10-100% results in fibrous tissue formation and 100% strain to non-union. This is known as Perren's theory.
Stokes published a review article on the effects of stress on bone healing and growth, and notes the importance of the 'Hueter-Volkmann Law' (growth is retarded by increased mechanical compression, and accelerated by reduced loading in comparison with normal values) in bone growth. Stokes also notes that sustained compression of physiological magnitude inhibits growth by 40% or more, while distraction increases growth rate by a much smaller amount.
Illustration A shows an example of a stress-strain curve, with several key definitions labeled on the diagram.
Incorrect Answers:
Question 87
A 25-year-old athlete presents with symptoms attributed to injury to ligament D in Figure A. Which of the following symptoms and signs is characteristic of this injury? Review Topic
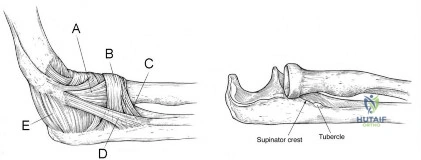
Explanation
PLRI can be diagnosed using the lateral pivot shift or posterolateral drawer. According to O’Driscoll, the elbow dislocates in 3 stages from lateral to medial (circle of Horii). Stage 1 involves disruption of the LUCL and partial/total disruption of the LCL complex (creating PLRI). Patients have pain with varus stress. Stage 2 includes disruption of the anterior capsule from incomplete elbow posterolateral dislocation. Stage 3 is divided into:
(a) Disruption of all soft tissues surrounding/ including the posterior MCL except for the anterior bundle. This bundle forms the pivot around which the elbow dislocates in a posterior direction by way of a posterolateral rotatory mechanism; and (b) complete disruption of the MCL.
O'Driscoll et al. describe PLRI diagnosed in 5 patients who had elbow dislocation using the posterolateral rotatory instability test, which they describe as being analogous to the test for lateral rotatory instability of the knee after ACL rupture. They believed the condition was laxity of the LUCL, which allowed transient rotatory subluxation of the ulnohumeral joint and secondary dislocation of the radiohumeral joint, without radio-ulnar joint dislocation. They recommended repair of the LUCL to eliminate PLRI.
Sanchez-Sotelo et al. retrospectively described 12 cases of direct repair and 33 ligamentous reconstructions for PLRI. 86% were satisfied with the procedure. Better results were obtained with patients with post-traumatic etiology, instability at presentation, and those with augmented reconstruction with tendon graft (compared with ligament repair alone).
Figure A shows structures on the lateral side of the elbow. The corresponding labels are seen in Illustration A. Illustration B shows the lateral pivot shift (also known as the posterolateral rotatory instability test).
Incorrect Answers:
Question 88
A year-old woman experiences pain 1 year after total knee arthroplasty (TKA). She reports sharp anterior pain and a painful catching sensation that is aggravated by rising from a chair or climbing stairs. Physical examination reveals a mild effusion and a range of motion of 2° to 130°, with patellar crepitus. The symptoms are reproduced by resisted knee extension. Radiographs show a well-aligned posterior- stabilized TKA without evidence of component loosening. What is the most likely cause of this patient's pain?
Explanation
Patellar clunk syndrome is caused by the development of a fibrous nodule on the posterior aspect of the quadriceps tendon at its insertion into the patella. It causes a painful catching sensation when the extensor mechanism traverses over the trochlear notch as the knee extends from 45° of flexion to 30° from full extension. It characteristically occurs in posterior stabilized total knee arthroplasties and appears to be related to femoral component design. The syndrome can usually be prevented by excising the residual synovial fold just proximal to the patella. Flexion gap instability can also cause a painful total knee arthroplasty but is less common in posterior stabilized implants. Femoral component malrotation can cause pain attributable to a flexion gap imbalance or patellar tracking problems. Polyethylene wear would be unlikely after just 1 year. Patellar clunk syndrome can usually be addressed successfully with arthroscopic synovectomy. Recurrence is uncommon. Physical therapy may help to strengthen the quadriceps following synovectomy but would not resolve the clunk syndrome symptoms. Femoral or tibial insert revision is not indicated if patellar clunk syndrome is the only problem resulting in a painful
total knee arthroplasty.
Question 89
A 45-year-old man reports that he awoke 2 weeks ago with severe pain in his right arm. Examination reveals weakness in the biceps, brachialis, and wrist extensors. There is decreased sensation in the thumb and index finger and a diminished brachioradialis reflex. Assuming this patient has a posterolateral herniated nucleus pulposus, what level is involved?
Explanation
REFERENCES: Standaert CJ: The patient history and physical examination: Cervical, thoracic and lumbar, in Herkowitz HN, Garfin SR, Eismont FJ, et al (eds): Rothman-Simeone The Spine, ed 5. Philadelphia, PA, Saunders Elsevier, 2006, vol 1, pp 171-186.
Bates B: A Guide to Physical Examination and History Taking, ed 5. Philadelphia, PA,
JB Lippincott, 1991.
Question 90
What molecules have been shown to promote fibrosis during muscle injury?
Explanation
Question 91
A 17-year-old pitcher reports pain over the medial aspect of the elbow that occurs during the acceleration phase of throwing, and it prevents him from throwing at the velocity needed to be competitive. What structure is most likely injured in this patient?
Explanation
REFERENCES: Azar FM, Andrews JR, Wilk KE, et al: Operative treatment of ulnar collateral ligament injuries of the elbow in athletes. Am J Sports Med 2000;28:16-23.
Cain EL, Dugas JR, Wolf RS, et al: Elbow injuries in throwing athletes: A current concepts review. Am J Sports Med 2003;31:621-635.
Rettig AC, Sherrill C, Snead DS, et al: Nonoperative treatment of ulnar collateral ligament injuries in
throwing athletes. Am J Sports Med 2001 ;29:15-17.
/
Figure 55a Question 55
A 22-year-old male basketball player has had knee pain for the past 3 months. He denies any history of trauma. He has symptoms of catching but no locking. He has rested for 2 weeks but symptoms returned when he resumed sporting activities. Tr and T2-weighted MRI scans are shown in Figures 55a and 55b. What is the most likely diagnosis?
Locked lateral meniscus tear
Anterior cruciate ligament tear
Ganglion cyst of the anterior cruciate ligament
Synovial osteochondromatosis
Pigmented villonodular synovitis PREFERRED RESPONSE: 3
DISCUSSION: The MRI scans show a cystic structure within the anterior cruciate ligament. It is fluid filled as seen on the T2 sequence. Ganglion cysts of the cruciate ligaments are rare. The most common presentation is pain with occasional loss of motion. Instability is not a chief complaint and often there is no evidence of laxity on examination. If nonsurgical management fails, arthroscopic debridement of the cyst is the accepted method of treatment.
REFERENCES: Liu SH, Osti L, Mirzayan R: Ganglion cysts of the anterior cruciate ligament: A case report and review of the literature. Arthroscopy 1994; 10:110-112.
Parish EN, Dixon P, Cross MJ: Ganglion cysts of the anterior cruciate ligament: A series of 15 cases. Arthroscopy 2005;21:445-447.
Question 92
Where is the underlying defect in a rhizomelic dwarf with the findings shown in Figure 5?
Explanation
REFERENCES: Johnson TR, Steinbach LS: Essentials of Musculoskeletal Imaging. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 809-812.
Caffey J: Achondroplasia of the pelvis and lumbosacral spine: Some roentgenographic features. Am J Roentgenol 1958;80:449.
Question 93
They found statistically significant decreases in need for secondary intervention, hardware failure, and infection as well as faster wound healing and faster time to fracture union.
Explanation
A 76-year old patient underwent partial foot amputation through the talonavicular and calcaneocuboid joints. Besides Achilles tendon lengthening, what additional procedure(s) may be required to prevent the most common post-operative deformity?
Posterior capsule release
Anterior tibialis transfer to the talar neck
Anterior tibialis transfer to cuboid
Flexor hallucis longus transfer to calcaneus
Peroneus brevis transfer to calcaneus Corrent answer: 2
Achilles tendon lengthening AND anterior tibialis transfer to the talar neck would be required to prevent equinovarus deformity.
Partial foot amputation through the talonavicular and calcaneocuboid joints is also known as the Chopart amputation. Chopart amputation alone is known to result in significant equinovarus deformity. This deformity results in excessive pressure on the anterior wound during gait, causing pain and wound complications. Transfer of the tibialis anterior tendon to talar neck will provide force, and muscle tone, that promotes ankle dorsiflexion. Lengthening of the Achilles tendon will also reduce the equinus moment force across the ankle joint.
Dillion et al. examined the gait patterns of partial foot amputees. They found that amputations proximal to the metatarsal heads compromised the normal propulsive function of the foot and ankle. The ideal level of amputation to maintain normal propulsive function was distal to the metatarsal heads (i.e., disarticulating the metatarsophalangeal (MTP) joint).
Illustration A is a lateral radiograph showing a Chopart amputation. Incorrect Answers:
prevent the equinovarus deformity.
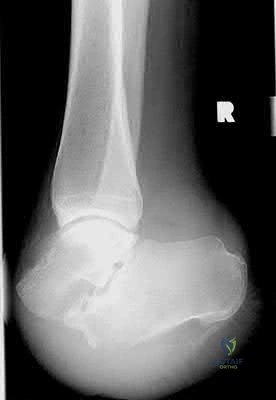
OrthoCash 2020
A 32-year-old male is involved in a motor vehicle collision and sustains the injury seen in Figure A. What is the most common urological injury associated with this injury pattern?
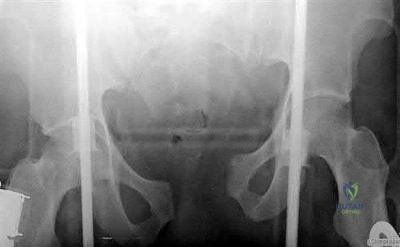
Testicular torsion
Posterior urethral tear
Bladder denervation
Testicular rupture
Renal hematoma
The figure shows an anteroposterior pelvic ring injury. The most common urological injury with pelvic ring injuries remains the posterior urethral tear, followed by bladder rupture.
Watnik et al notes lower urinary tract (bladder to end of urethra) injuries in up to 25% of patients with this injury. He reports that when contaminated urine communicates with the anterior arch, the possibility of infection exists, and early repair of bladder disruptions with simultaneous anterior arch plating minimizes this risk.
Routt et al notes that even with simultaneous treatment of these injuries, complications are common (late stricture in 44%, impotence in 16%, delayed incontinence in 20% of females, anterior deep pelvic infection in 4%). Despite this, they report that early urological repairs are easily performed at the time of anterior pelvic open reduction and internal fixation.
OrthoCash 2020
A 26-year-old women, 31-weeks pregnant, presents to the emergency department with the injury shown in Figure A. She states the injury occurred while lifting a heavy vacuum five days ago. She suffers from chronic headaches and sleep disturbances. On inspection, there are multiple dorsal and volar bruising over her wrist and upper arm. She is neurologically intact. After closed reduction and immobilizing the arm, what would be the next best step in management of this patient?
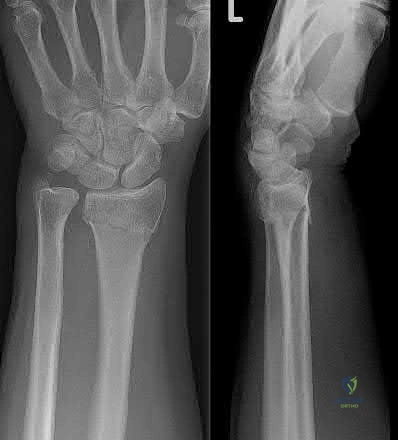
Diagnostic wrist arthroscopy
Urgent MRI wrist
Skeletal survey radiographs
Request a consultation with social worker in the hospital
Urgent open reduction internal fixation Corrent answer: 4
This patient presents with classic features of domestic violence. The most appropriate next step would be consultation with a social worker at the hospital, assess for child and patient safety, and encouraging the patient to seek self-protection.
Factors suggestive of domestic violence in the patient include pregnancy, delayed presentation after injury, inconsistent history, multiple bruises and complaints of chronic headache/sleep disturbances. Victims frequently miss days of work and as a result are at risk for losing their jobs. Victims are also more likely to engage in high-risk behavior with sex, drugs, alcohol, smoking, and eating.
The AAOS published a document outlining the Orthopaedic Surgeon’s responsibilities in domestic and family violence. Musculoskeletal injuries that should raise a suspicion of a problem include (1) Multiple injuries/fractures; (2) Unusual patterns of injury/fracture; (3) Injuries/fractures of varying ages; (4)
Injuries/fractures inconsistent with or disproportional to the history; (5) Multiple injuries treated in different hospital emergency departments or by different providers.
Incorrect Answers:
OrthoCash 2020
A 45-year-old man undergoes open reduction and internal fixation for a comminuted intra-articular humerus fracture . An olecranon osteotomy is performed and subsequently fixed with an intramedullary cancellous screw. Which of the following options in the table shown in Figure A best describes the characteristics of this osteotomy?
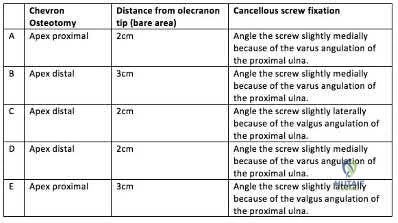
Question 94
Radiographs of the femur are unremarkable. A radionuclide bone scan demonstrates abnormal uptake in the mid-femur. A radionuclide bone marrow scan demonstrates decreased uptake within the marrow. Which of the following is the best step in management?
Explanation
Skaggs et al reviewed 79 cases of acute extremity pain in sickle cell patients. Radionuclide bone marrow and bone scan was used to differentiate osteomyelitis from bone infarct. Four cases of infection were diagnosed by normal uptake on the bone marrow scan and abnormal uptake on the bone scan. These cases were confirmed osteomyelitis by positive culture. Seventy cases were diagnosed as bone infarct by decreased uptake on the bone marrow scan and abnormal uptake bone scan.
Chambers et al reviewed the charts of 2000 known sickle cell patients. Fourteen patients had an episode of osteomyelitis or septic arthritis. Radiographs and bone scans were not helpful in differentiating infection from an acute bone infarct. Salmonella was the most frequent organism cultured from the osteomyelitis cases. The authors recommend bone aspiration or biopsy in an sickle cell patient with extremity pain, swelling, and a fever greater than 38.2 degrees C.
An otherwise healthy, 65-year-old male undergoes a right total knee arthroplasty without complications. Which of the following statements is recommended by the American Academy of Orthopaedic Surgeons Clinical Practice Guidelines for preventing venous thromboembolic disease in patients undergoing elective hip and knee arthroplasty?
Administer aspirin one week pre-operatively
Use elastic compressive stockings for 10 days pre-operatively
Obtain a post-operative duplex ultrasound of the patient for screening purposes
Administer Coumadin to maintain the patient’s INR between 1.5 and 2.5 during the post-perative period
Use mechanical compressive devices in the postoperative period
Use of mechanical compressive devices and aspirin during the postoperative period is
recommended by the American Academy of Orthopaedic Surgeons Clinical Practice Guidelines.
In 2011, the American Academy of Orthopaedic Surgeons published their Clinical Practice Guidelines for preventing venous thromboembolic disease in patients undergoing elective hip and knee arthroplasty. A summary of those guidelines provide general recommendations for venous thromboembolic disease in patients with and without bleeding disorders. These recommendations range from strong (recommending against the use of routine post-operative duplex ultrasonography), to moderate (using mechanical compressive devices or a pharmacologic agent for prophylaxis in the post- operative period), to inconclusive (they are unable to recommend for or against specific pharmacologic prophylaxis agents). Additionally, there are recommendations based on consensus agreement of the authors (the recommendation of early mobilization in the post-operative period).
These guidelines are now much closer to in agreement with the American College of Chest Surgeons (ACCS) 2012 guidelines for VTE prophylaxis. One of the differences between the guidelines is that the AAOS guidelines do not state a specific amount of time that a pharmacologic agent should be given post- operatively while the ACCS recommends such agents for a minimum of 10-14 days.
Incorrect answers:
The definition of effect size is best described as which of the following?
Likelihood that a statistically significant difference would be found between 2 groups given that a difference truly did exist
Estimated magnitude of the difference in the means between two groups
Average of the squares of each value's deviation from the mean
Range within which it is probable that the true value lies for the whole population of patients
Probability of obtaining a result equal to or more extreme than what was actually observed assuming the null hypothesis is true
The effect size is best defined as the magnitude of the difference in the means of the control and experimental groups in a study with respect to the pooled standard deviation. Effect sizes are normally used for continuous variables in contrast to relative risk reduction which is used for dichotomous variables. Power (1), variance (3), confidence interval (4), and P value (5) are the other options provided.
Which of the following patients are at greatest risk of having a future vertebral fragility fracture?
Elderly female with prior hip fragility fracture
Elderly female with prior distal radius fragility fracture
Elderly female with prior T6 compression fragility fracture
Elderly female with a T-score of -3.0
Elderly female currently on hormone replacement therapy
History of a prior vertebral fragility fracture is the strongest predictor of a future fragility fracture. A meta-analysis by Klotzbuecher et al examined risk factors for fragility fractures and found an association between prior and subsequent fragility fractures. The strongest associations were observed between prior and subsequent vertebral fractures. They found women with preexisting vertebral fractures had an approximately 4 times greater risk of subsequent vertebral fractures than those without prior fractures. They also found this risk increases with the number of prior vertebral fractures. Other combinations of prior and future fracture sites, such as the hip or wrist, were also strongly associated, but none so high as vertebral fractures.
A 79-year-old female falls onto her right hip at home and sustains the injury shown in Figure A. She undergoes an uncemented unipolar hemiarthroplasty. During insertion of the stem into the femoral canal, the patient becomes hypotensive and hypoxic. Which of the following has most likely occurred?
Femoral shaft fracture
Inadequate fluid resuscitation during surgery
Acute myocardial infarction
Pulmonary embolism caused by dislodging of deep venous thrombosis during hip exposure
Intramedullary fat and marrow embolization
During insertion of the femoral stem, the intramedullary pressures are increased. Fat and marrow elements can become embolized into the bloodstream at this point resulting in ventilation perfusion mismatch in the lungs.
Kim et al prospectively followed 156 total hip arthroplasties including bilateral and unilateral procedures as well as cemented and uncemented procedures. They found no difference in fat embolization amongst any of the groups. However, they did find that if patients had evidence of bone marrow cells in the right atrium on the first postoperative day, they developed diffuse encephalopathy with confusion and agitation that lasted for about twenty-four hours.
Which of the following investigative studies is most useful in the definitive diagnosis of Amyotrophic Lateral Sclerosis (ALS)?
Genetic testing
MRI brain and spinal cord
Muscle biopsy
Serum protein electrophoresis and immunoelectrophoresis
Electrodiagnostic studies
The diagnosis of ALS requires a period of clinical observation to document the progressive loss of upper and lower motor function. Electrodiagnositic studies are required to make a definitive diagnosis.
Amyotrophic lateral sclerosis (ALS) is the most common degenerative disease of the motor neuron system. Nerve conduction studies and needle electromyography (EMG) are useful for confirming the diagnosis of ALS and for excluding peripheral conditions that resemble ALS. Hallmark findings in the electrodiagnosis of ALS are abnormal motor nerve conduction studies, with normal sensory nerve conduction studies. UMN signs are mild weakness, spasticity, and abnormally brisk reflexes; LMN signs are progressive weakness, wasting, and loss of reflexes and muscle tone.
Brooks et al. developed a diagnostic algorithm for the diagnosis of ALS. The algorithm is based on the degree of certainty of diagnosis, which is increased by the number of body segments that demonstrate upper motor neuron (UMN) and lower motor neuron (LMN) abnormalities. Clinical and electrophysiologic findings in 3 or more body segments is definitive of the diagnosis.
Incorrect Answers:
Radiographic changes suggestive of osteopetrosis in children are a known complication of which of the following types of medications?
TNF-alpha inhibitors
Bone morphogenic proteins
Bisphosphonates
Fluoroquinolones
RANKL antibiodies
Radiographic changes suggestive of osteopetrosis (marble bone disease) are a known complication of bisphosphonate usage. The common cellular pathway in this process is the osteoclast. Bisphosphonates target and inhibit the osteoclast, and these cells are not functioning in patients with osteopetrosis.
Whyte et al describe a case report of a 12-year-old child with idiopathic hyperphosphatasia treated with bisphosphonates who developed osteopetrosis.
Falk et al report on their small case series which showed the beneficial effects and known complications in the treatment of osteogenesis imperfecta with bisphosphonate therapy.
Marini presents a perspective article describing the off-label use of bisphosphonates in children.
What function does computerized physician order entry have on medication monitoring?
Reduces the rate of medication errors
Improves physician satisfaction
Decreases narcotic requirements by patients
Increases rates of allergy related medication errors
Improves physician knowledge about the drugs they are prescribing
Computerized physician order entry has greatest impact on reducing medication errors.
Bobb et al. studied medication errors averted by pharmacists at a 700-bed academic center and concluded that 65% of them would likely have been prevented with computerized physician order entry.
Upperman et al. reviewed medication errors at a pediatric hospital before and after implementation of a computerized physician order entry system. They found a significant decrease in adverse drug events following establishment of the computerized system.
Incorrect Answers:
2: Physician satisfaction has not been correlated with computer entry for medications.
3: Narcotic requirements are related to injury or patient characteristics, not computerized entry.
4: Allergy-related errors are decreased with use of computerized entry.
5: Physician knowledge is not necessarily increased with computerized entry.
What is the cellular mechanism of action for non-nitrogen containing bisphosphonates (such as clodronate and etidronate) to induce osteoclast apoptosis?
Inhibiting caspase
Inhibiting matrix metalloprotease
Inhibiting reverse transcriptase
Targeting of farnesyl diphosphate synthase
Creating toxic analog of adenosine triphosphate that targets mitochondria
Bisphosphonates work by one of two mechanisms. Non-nitrogren containing bisphosphonates (such as etidronate and clodronate) work by creating a toxic analog of ATP which inhibits ATP and leads to osteoclast apoptosis. Nitrogen containing bisphosphonates (such as alendronate, risedronate, and zoledronate) inhibit the enzyme farnesyl diphosphate synthase which prevents protein geranylgeranylation and prevents osteoclastic bone resorption.
Reska et. al. specifically discuss the difference between the two pathways. Non-nitrogen containing compounds inhibit ATP production and cause osteoclast apoptosis. Nitrogen containing bisphophonates inhibit protein synthesis by interrupting the cholesterol biosynthetic pathway, which prevents osteoclastic resorption.
Which class of antibiotics inhibit early fracture healing through toxic effects on chondrocytes?
cephalosporins
quinolones
penicillins
macrolides
sulfonamides
Animal models have shown that quinolones inhibit early fracture healing through a toxic effect on chondrocytes. The study by Perry et al demonstrated that fracture calluses in the animals treated with quinolones showed a lower histologic grade as compared with control animals representing a less mature callus with the presence of more cartilage and less woven bone. The study by Huddleston et al demonstrated fracture calluses in the animals treated with ciprofloxacin showed abnormalities in cartilage morphology and endochondral bone formation and a significant decrease in the number of chondrocytes compared with the controls. None of the other antibiotics listed are known to have toxic effects on chondrocytes.
A mutation of the retinoblastoma gene RB-1 leads to the development of malignancies such as retinoblastoma and osteosarcoma. Which term best characterizes the RB-1 gene?
growth factor
retro-oncogene
proto-oncogene
oncogene
tumor suppressor
A tumor suppressor is a gene whose presence normally prevents neoplasia and whose absence leads to unregulated cell growth. Two well-studied tumor suppressor genes include p53 and RB-1. P53 normally suppresses cell division by blocking the cell cycle if genetic damage is present. If it is absent or mutated, the p53 suppressing effect no longer regulates cell growth and neoplasm results. In a similar fashion, a mutation in RB-1, or the retinoblastoma gene, may leads to retinoblastoma and osteosarcoma.
Youarecounseling ayoungfemalepatientabout herfuturerisk of osteoporosis. Which of the following regarding peak bone mass (PBM) is true?
PBM is consistently attained by the end of the second decade of life in both men and women.
PBM is independent from environmental factors.
PBM correlates strongly with post-menopausal bone mineral density
Timing of PBM varies based on anatomic site.
Women attain PBM prior to men, regardless of anatomic site. Corrent answer: 4
The timing and magnitude of PBM varies based on anatomic site. PBM is often reached in the appendicular skeleton earlier than in the axial skeleton.
PBM is defined as the greatest amount of bone an individual will attain in his or her lifetime. Controversy has surrounded the timing of PBM due to significant anatomical variations as well as strong gender-based, genetic, geographic, environmental, and mechanical influences. While women may reach PBM
earlier than men in the hip, the converse has been found to be true of the spine. Furthermore, the age at which each is obtained varies widely. Though the PBM of the hip is most often achieved by the end of the second decade of life, PBM of the spine may not occur until the third or fourth decade of life. Interestingly, PBM has been found to correlate poorly with post-menopausal bone mineral density, likely a result of these strong confounding influences.
Bonjour et al. reviewed the controversy behind peak bone mass. The authors note that the gender-based difference in bone mass becomes expressed during puberty and that there is a large variability in normal values of bone mineral density between anatomic sites.
They conclude that bone mass accumulation can be completed by the end of the second decade at both the lumbar spine and femoral neck, but that this may be significantly influenced by a number of variables during growth such as genetics, diet, endocrine and mechanical factors.
Berger et al. more recently evaluated trends in peak bone mass from longitudinal data in the Canadian Multicentre Osteoporosis Study (CaMos). The authors found that peak bone mass was highly variable between the axial and appendicular skeleton. Specifically, lumbar spine PBM was reached in women
at 33-40 years, but much earlier in men at 19-33 years. Conversely, hip PBM was reached earlier in women at 16-19 years and later in men at 19-21 years. Furthermore, there was a lack of concordance between PBM and BMD over age
Question 95
Which of the following best describes the use of epidural morphine and steroid paste after laminectomy?
Explanation
REFERENCES: Kramer MH, Mangram AJ, Pearson ML, et al: Surgical-site complications associated with a morphine nerve paste used for postoperative pain control after laminectomy. Infect Control Hosp Epidemiol 1999;20:183-186.
Lowell TD, Errico TJ, Eskenazi MS: Use of steroids after discectomy may predispose to infection. Spine 2000;25:516-519.
Question 96
..Figures 78a and 78b are the radiographs of a 47-year-old right-hand-dominant woman who has a 3-month history of gradually progressive right shoulder pain. She reports no previous trauma, but does report pain at night and with activity such as weight training. Examination demonstrates active and passive range of motion to be 110 degrees forward elevation, external rotation to 20 degrees, and internal rotation to the sacrum. The next treatment step should include
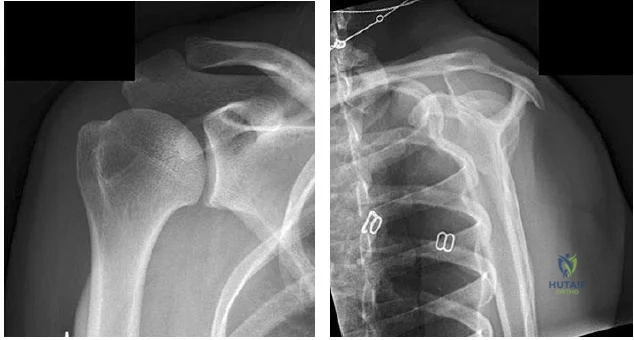
Explanation
Rotator cuff and scapular stabilizer strengthening exercises
Diagnostic and therapeutic corticosteroid injection
Arthroscopic debridement
Completion of rotator cuff tear, repair, and biceps tenotomy
Acromioplasty
Repair of rotator cuff and superior labrum anterior to posterior (SLAP) repair
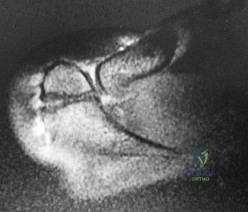
Repair of subscapularis tendon and biceps tenodesis
Question 97
A 14-year-old gymnast presents after a fall from the balance beam with a hyperextension injury to her left knee. She could ambulate with pain but was unable to continue exercise due to pain. On examination she has a swollen knee with painful
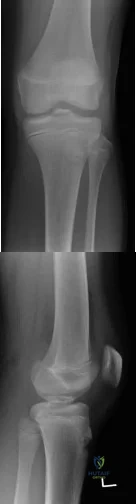
Explanation
Tibial eminence fractures are rare but occur more often in pediatric populations, often in the setting of sports-related injuries. Debate continues over operative vs nonoperative treatment, as well as fixation type (screw vs suture) for openly treated fractures. Past evidence suggested closed treatment was adequate but there has been an increase in operative management. Closed treatment is suggested for minimally displaced fractures (Type I and reducible Type II) and open treatment for completely displaced fractures (non-reducible Type II and Type III).
Wilfinger et al provide the results of a closed reduction protocol at their institution including 38 patients with long term followup. All patients underwent aspiration and closed reduction in the OR under fluoroscopic guidance followed by long leg casting in hyperextension and graduated weight bearing over weeks. No patients complained of persistent pain, swelling, giving way, or disability at follow up.
However, Edmonds et al in a retrospective review compare open reduction internal fixation (ORIF), arthroscopic-assisted internal fixation (AAIF), and closed reduction with casting (CRC) for pediatric patients with displaced tibial spine fractures. They report improved reduction but also increased arthrofibrosis in ORIF and AAIF groups
compared to CRC, but of the 24% of patients with long term followup results, there was no difference in functional outcomes across all 3 groups. There was a 17% rate of later operation for the CRC group patients. They suggest closed treatment for fractures with <5mm displacement, otherwise ORIF or AAIF.
Gans et al conducted a systematic review focused on the questions of open vs closed reduction, and screw vs suture fixation. The 26-article review found insufficient evidence to have any clear recommendations. They did find reduced laxity and improved range of motion for minimally displaced fractures that had an open reduction, and that completely displaced fractures treated nonoperative had higher rates of nonunion.
Figures A and B are AP and lateral knee radiographs demonstrating a moderately displaced (Meyers and McKeever Type II) tibial spine fracture in a skeletally immature patient.
Incorrect Responses
Question 98
Which of the following characteristics is seen in patients with osteochondritis dissecans of the elbow? Review Topic
Explanation
Question 99
A 23-year-old man has had right posterolateral knee pain and occasional lateral calf dysesthesias for the past 8 months. A radiograph, CT scan, MRI scans, and a biopsy specimen are shown in Figures 62a through 62e. What is the most likely diagnosis?
Explanation
REFERENCES: Rosenthal DI: Radiofrequency treatment. Orthop Clin North Am 2006;37:475-484.
Ghanem I: The management of osteoid osteoma: Updates and controversies. Curr Opin Pediatr 2006;18:36-41.
Question 100
A 12-year-old boy reports limping and chronic knee pain that is now inhibiting his ability to participate in sports. Clinical examination and radiographs of the knee are normal. Additional evaluation should include Review Topic
Explanation
