Orthopedic Surgery Board Review MCQs: Lower Extremity Arthroplasty & Ankle | Part 171
Key Takeaway
This page offers Part 171 of a comprehensive Orthopedic Surgery board review quiz. It features 100 high-yield MCQs, meticulously verified and formatted for OITE and AAOS exams. Designed for orthopedic residents and surgeons, it covers Ankle, Arthroplasty, Hip, and Knee, crucial for certification preparation.
Orthopedic Surgery Board Review MCQs: Lower Extremity Arthroplasty & Ankle | Part 171
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 65-year-old male presents with severe groin pain and swelling 8 years after a metal-on-metal total hip arthroplasty. Imaging demonstrates a large cystic mass compressing the femoral vein. Blood cobalt and chromium levels are markedly elevated. Aspiration yields fluid negative for infection. What is the most appropriate definitive management for this patient?
Explanation
Question 2
A 70-year-old female complains of knee swelling and a sense of instability when rising from a chair or descending stairs 1 year after a primary posterior-stabilized total knee arthroplasty. On physical examination, she lacks varus or valgus laxity in full extension, but demonstrates a positive anterior and posterior drawer test when the knee is flexed to 90 degrees. Radiographs show well-fixed components with no evidence of loosening. What is the most likely technical error leading to this complication?
Explanation
Question 3
A 60-year-old male with end-stage post-traumatic ankle osteoarthritis is being evaluated for surgical options. Which of the following conditions is considered an absolute contraindication to a total ankle arthroplasty (TAA)?
Explanation
Question 4
During a direct anterior approach for a total hip arthroplasty, the surgeon dissects through the superficial internervous plane. Which two nerves supply the muscles that define this specific interval?
Explanation
Question 5
A 68-year-old female presents with recurrent posterior dislocations of her primary total hip arthroplasty. CT evaluation demonstrates the acetabular component is positioned in 10 degrees of anteversion and 35 degrees of abduction. The uncemented femoral component is fixed in 5 degrees of retroversion. What is the most appropriate surgical strategy to restore stability?
Explanation
Question 6
A 55-year-old female undergoes a total ankle arthroplasty via a standard anterior approach. Three months postoperatively, she reports numbness over the dorsum of her foot. During the surgical exposure, the extensor digitorum longus (EDL) was retracted laterally. Which cutaneous nerve was most likely injured or stretched during this dissection?
Explanation
Question 7
A 65-year-old male who underwent a posterior-stabilized total knee arthroplasty 8 months ago complains of a catching sensation and an audible 'clunk' at the superior pole of the patella as his knee extends from 40 degrees to 30 degrees of flexion. Which specific implant design characteristic is most strongly associated with the development of this condition?
Explanation
Question 8
During preparation of the proximal femur for an uncemented, tapered-wedge total hip arthroplasty stem, the surgeon notes a non-displaced longitudinal fracture of the calcar propagating 2 cm distal to the lesser trochanter. The broach remains axially and rotationally stable within the canal. What is the most appropriate next step in management?
Explanation
Question 9
When counseling a patient on the expected outcomes of total ankle arthroplasty (TAA) compared to ankle arthrodesis for end-stage ankle osteoarthritis, which of the following statements is most supported by current literature?
Explanation
Question 10
A 72-year-old female presents with an inability to perform a straight leg raise 3 years after a primary total knee arthroplasty. Imaging demonstrates patella alta and a palpable defect at the tibial tubercle. An extensor mechanism allograft reconstruction is planned. To maximize the likelihood of a successful outcome, at what degree of knee flexion should the allograft be tensioned and fixed?
Explanation
Question 11
According to the 2018 International Consensus Meeting (ICM) criteria, which of the following is considered a definitive major criterion for diagnosing a periprosthetic joint infection?
Explanation
Question 12
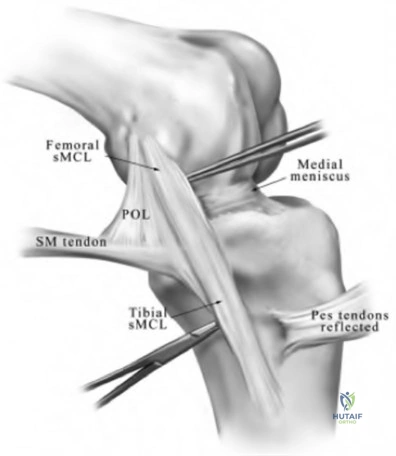
During the medial release of a primary total knee arthroplasty for a varus deformity, the surgeon inadvertently transects the mid-substance of the medial collateral ligament (MCL). The bone cuts have been made, but the components have not yet been implanted. What is the most appropriate intraoperative management strategy?
Explanation
Question 13
A 60-year-old male with a metal-on-polyethylene total hip arthroplasty presents with new-onset groin pain and swelling 7 years postoperatively.
Radiographs show a well-fixed stem and cup. Serum cobalt is 8.5 ppb and chromium is 1.2 ppb. MRI with metal artifact reduction shows a solid pseudotumor. What is the most likely source of the elevated metal ions?
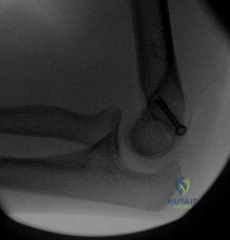
Explanation
Question 14
A 58-year-old patient with end-stage post-traumatic ankle arthritis and a rigid 20-degree coronal plane varus deformity is scheduled for a total ankle arthroplasty (TAA). To minimize the risk of premature implant failure and edge loading, which adjunctive procedure should most likely be performed?
Explanation
Question 15
During a primary total knee arthroplasty, the trial reduction reveals that the knee is symmetric and stable in full extension, but excessively tight in 90 degrees of flexion, preventing full range of motion. Which of the following surgical adjustments will most effectively correct this specific imbalance?
Explanation
Question 16
Following a primary total hip arthroplasty performed via a standard posterolateral approach, patients are commonly instructed on 'hip precautions.' Which specific combination of hip movements places the joint at the greatest risk for a posterior dislocation?
Explanation
Question 17
The concept of kinematic alignment in total knee arthroplasty has gained popularity in recent years. How does the fundamental goal of kinematic alignment differ from that of traditional mechanical alignment?
Explanation
Question 18
A 55-year-old patient presents with end-stage ankle osteoarthritis and is scheduled for a Total Ankle Arthroplasty (TAA).
Preoperative evaluation includes a weight-bearing CT scan. Which of the following findings on weight-bearing CT would most strongly indicate the need for a concomitant subtalar arthrodesis at the time of the TAA?
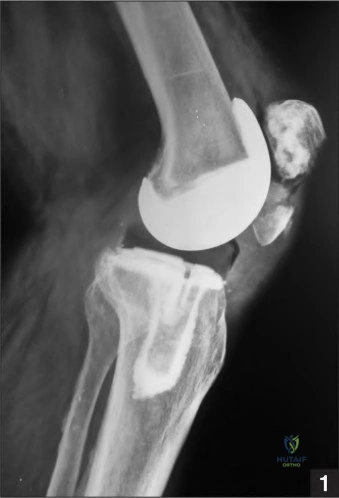
Explanation
Question 19
A 72-year-old female is undergoing preoperative planning for a total hip arthroplasty. She has a history of a multisegmental lumbar spinal fusion from L2 to the sacrum, resulting in a 'flatback' deformity and a stiff spine. How should the surgeon adjust the positioning of the acetabular component to minimize the risk of dislocation?
Explanation
Question 20
A 68-year-old male with a BMI of 40 presents with severe, start-up knee pain 5 years after a primary cemented total knee arthroplasty. Radiographs demonstrate continuous, progressive radiolucent lines measuring 3 mm in all zones surrounding the tibial component. The femoral and patellar components appear well-fixed. ESR, CRP, and a joint aspiration are entirely normal, ruling out infection. What is the most appropriate surgical management?
Explanation
Question 21
A 62-year-old male undergoes a primary total ankle arthroplasty (TAA). Postoperatively, he develops severe medial gutter pain. Radiographs demonstrate impingement between the talar component and the medial malleolus. Which technical error during the index procedure is the most likely cause of this complication?
Explanation
Question 22
A 68-year-old woman presents with persistent, loud squeaking from her hip 3 years after a ceramic-on-ceramic total hip arthroplasty (THA). Radiographs show well-fixed components with no evidence of osteolysis. Which of the following component positionings is most strongly associated with this complication?
Explanation
Question 23
During a primary posterior-stabilized total knee arthroplasty (TKA), the surgeon evaluates the gaps and notes the knee is unacceptably tight in flexion but symmetric and perfectly balanced in extension. Which of the following is the most appropriate next step to balance the knee?
Explanation
Question 24
A 75-year-old male with a history of TKA 2 years ago presents with acute onset knee pain and swelling that began 3 days ago following a dental procedure. Aspiration yields a WBC count of 35,000 cells/uL with 92% PMNs. Radiographs show well-fixed components. Which of the following is the most appropriate surgical treatment?
Explanation
Question 25
A 68-year-old female presents with an unstable THA. She has dislocated posteriorly 3 times in the past month. Radiographs demonstrate well-fixed implants with the acetabular component at 40 degrees of inclination and 15 degrees of anteversion. The femoral stem is well-fixed in 15 degrees of anteversion. What is the most appropriate surgical intervention?
Explanation
Question 26
A 55-year-old female presents with severe lateral ankle pain and a rigid hindfoot 5 years after an ORIF of a pilon fracture. She is diagnosed with end-stage post-traumatic ankle arthritis. She has a BMI of 42 and absent protective sensation in a stocking-glove distribution due to diabetes. Which of the following is the most appropriate definitive management?
Explanation
Question 27
A 72-year-old female sustains a periprosthetic femur fracture around a cemented, polished taper-slip stem 6 years after a THA. Radiographs show a spiral fracture at the tip of the stem with subsidence of the stem by 3 cm within the cement mantle. The femoral bone stock is adequate. What is the most appropriate treatment?
Explanation
Question 28
A 60-year-old man undergoes an uncemented THA via a direct anterior approach. Postoperatively, he complains of localized numbness and burning pain over the anterolateral aspect of his thigh. This complication is most likely due to injury to a nerve that courses between which of the following intervals?
Explanation
Question 29
During a primary TKA, the surgeon utilizes kinematic alignment principles. Which of the following statements best describes the fundamental goal of kinematic alignment compared to traditional mechanical alignment?
Explanation
Question 30
A 58-year-old male with a history of a metal-on-polyethylene THA 7 years ago presents with spontaneous groin pain. Radiographs show massive osteolysis of the proximal femur. Aspiration reveals fluid with macrophages containing particulate debris. What is the primary biologic mechanism for this osteolysis?
Explanation
Question 31
Which of the following is the most critical anatomical landmark for establishing the proper rotational alignment of the femoral component in a total knee arthroplasty to optimize patellofemoral tracking?
Explanation
Question 32
A 68-year-old male presents with a Vancouver B1 periprosthetic femur fracture. The surgeon elects to perform an open reduction and internal fixation with a lateral locking plate. To minimize the risk of mechanical failure at the proximal plate construct, what is the recommended minimum plate length extending proximal to the fracture site?
Explanation
Question 33
A patient is evaluated for an isolated ankle arthrodesis versus total ankle arthroplasty (TAA). Which of the following long-term kinematic changes is most typically observed following an isolated ankle arthrodesis compared to a successful TAA?
Explanation
Question 34
A 62-year-old woman reports anterior knee pain and a painful \"catching\" sensation when extending her knee from a flexed position, 18 months after a posterior-stabilized TKA. On examination, a palpable clunk is felt at 30 degrees of flexion as the knee extends. What is the most likely etiology?
Explanation
Question 35
A 70-year-old male undergoes a primary TKA. In the recovery room, he is noted to have a dense foot drop and numbness over the dorsum of the foot. Which of the following preoperative deformities places the patient at the highest risk for this specific complication?
Explanation
Question 36
A 50-year-old male presents with severe groin pain 4 years after a THA utilizing a 36-mm metal head on a titanium stem. MRI shows a large fluid collection in the abductor musculature. Serum cobalt levels are markedly elevated, while chromium is normal. What is the most likely diagnosis?
Explanation
Question 37
A 65-year-old male with end-stage medial compartment knee osteoarthritis and a reducible 10-degree varus deformity is scheduled for a unicompartmental knee arthroplasty (UKA). Which of the following represents an absolute contraindication for a traditional fixed-bearing UKA?
Explanation
Question 38
Which of the following intraoperative surgical techniques most significantly decreases the risk of postoperative dislocation following a primary THA performed via a posterior approach?
Explanation
Question 39
A 78-year-old female presents with thigh pain and inability to bear weight after a mechanical fall. She underwent a right total hip arthroplasty (THA) 10 years ago. Radiographs demonstrate a displaced spiral fracture around the femoral stem, which extends just distal to the tip of the prosthesis. The stem has subsided by 1.5 cm compared to prior radiographs, but the distal femoral bone stock remains robust. What is the most appropriate surgical management?
Explanation
Question 40
A 68-year-old male complains of knee instability and swelling 18 months following a posterior-stabilized total knee arthroplasty. On examination, the knee is stable in full extension and at 90 degrees of flexion, but exhibits marked laxity to varus and valgus stress at 30 to 45 degrees of flexion. Which of the following technical errors most likely caused this specific pattern of instability?
Explanation
Question 41
A 62-year-old male with end-stage post-traumatic ankle osteoarthritis and a rigid 15-degree varus deformity is undergoing total ankle arthroplasty (TAA). Intraoperatively, after making the bony cuts and placing trial components, the ankle remains tight medially and fails to correct to a neutral coronal alignment. Which of the following is the most appropriate next step in management?
Explanation
Question 42
A 72-year-old male with ankylosing spondylitis and a completely fused lumbopelvic spine is planned for a total hip arthroplasty. His spine is fused in a flattened position, resulting in fixed pelvic retroversion. How does this rigid spinopelvic state alter the risk of dislocation, and what intraoperative adjustment should be considered?
Explanation
Question 43
A 45-year-old male patient who underwent a ceramic-on-ceramic total hip arthroplasty 5 years ago presents complaining of an audible, high-pitched squeaking noise coming from his hip with every step. He denies pain or instability. What is the most widely recognized biomechanical cause for this phenomenon?
Explanation
Question 44
A 55-year-old heavy manual laborer with severe end-stage ankle osteoarthritis opts for a tibiotalar arthrodesis over arthroplasty. To optimize his postoperative gait mechanics and minimize adjacent joint arthritis, what is the ideal position for the ankle fusion?
Explanation
Question 45
A 60-year-old female presents with persistent lateral-sided knee pain and a palpable, painful snapping sensation during active flexion 6 months after a primary posterior-stabilized TKA. Radiographs reveal well-fixed, appropriately sized components. Dynamic ultrasound confirms the popliteus tendon snapping over the edge of the femoral component. What is the most appropriate management?
Explanation
Question 46
A 55-year-old active male is undergoing a primary total hip arthroplasty. The surgeon is deciding on the optimal bearing surface. Compared to other bearing combinations, which of the following is the most distinct clinical profile of a ceramic-on-ceramic articulation?
Explanation
Question 47
During a primary posterior-stabilized total knee arthroplasty, the surgeon performs the initial bone cuts and inserts spacer blocks. The knee is perfectly balanced and stable in full extension, but it is extremely tight and unable to flex past 80 degrees in flexion. Which of the following technical adjustments is the most appropriate next step to balance the knee?
Explanation
Question 48
A 62-year-old female with end-stage ankle osteoarthritis is being evaluated for a total ankle arthroplasty (TAA). Which of the following preoperative findings represents an absolute contraindication to performing a TAA?
Explanation
Question 49
A 68-year-old male undergoes a right total hip arthroplasty. Six months postoperatively, he has experienced three episodes of posterior dislocation while rising from a low chair. Radiographs and CT imaging demonstrate the acetabular cup is positioned in 20 degrees of anteversion and 40 degrees of inclination. The femoral stem is fixed in 10 degrees of retroversion. What is the most appropriate surgical management?
Explanation
Question 50
A 71-year-old male presents with a 4-day history of acute, severe right knee pain and swelling. He underwent an uncomplicated primary total knee arthroplasty 3 years ago. He recently had a dental extraction 2 weeks prior without prophylactic antibiotics. Joint aspiration yields a synovial fluid WBC count of 85,000 cells/uL with 92% neutrophils. Radiographs show well-fixed components. What is the most appropriate surgical intervention?
Explanation
Question 51
A surgeon is performing a primary total knee arthroplasty (TKA). During trialing, the extension gap is excessively tight, preventing full extension, but the flexion gap is perfectly balanced. Which of the following is the most appropriate next step to correct this kinematic mismatch?
Explanation
Question 52
A 45-year-old active female undergoes THA with a ceramic-on-ceramic bearing. At 2 years postoperatively, she complains of a loud, reproducible squeaking noise from her hip during normal gait. Which of the following is the most established biomechanical cause for this phenomenon?
Explanation
Question 53
Total ankle arthroplasty (TAA) provides excellent outcomes in appropriately selected patients but relies on specific structural and neurologic prerequisites. Which of the following represents an absolute contraindication for TAA?
Explanation
Question 54
A 72-year-old woman falls and sustains a periprosthetic femur fracture around a cemented polished taper slip stem. Radiographs show a fracture traversing the mid-stem. The stem has subsided by 2 cm, and there is an osteolytic lesion in the proximal femur, but distal diaphyseal bone stock is adequate. How is this classified and best treated?
Explanation
Question 55
A 68-year-old male presents with the inability to perform a straight leg raise 6 weeks after a primary TKA. Ultrasound confirms a complete mid-substance patellar tendon rupture. What is the most reliable surgical management for this complication?
Explanation
Question 56
A 55-year-old female presents with anterior groin pain 1 year after an uncemented THA. The pain is exacerbated by active hip flexion. Radiographs demonstrate that the acetabular component is placed with 10 degrees of anteversion and overhangs the anterior acetabular rim by 12 mm. Image-guided injection of the psoas bursa temporarily resolves her pain. What is the most appropriate definitive management?
Explanation
Question 57
A 62-year-old patient with rheumatoid arthritis has severe end-stage ankle osteoarthritis alongside symptomatic, radiographically advanced subtalar arthritis. The patient is undergoing preoperative planning for a total ankle arthroplasty (TAA). What is the recommended management approach for the subtalar joint?
Explanation
Question 58
A 65-year-old male presents with a painful, audible "clunk" in his knee when extending from 45 degrees of flexion, 1 year after a posterior-stabilized (PS) TKA. Radiographs show well-fixed components. Which of the following is the primary pathophysiologic cause of this condition?
Explanation
Question 59
A 60-year-old male with a metal-on-polyethylene THA presents with a large anterior thigh mass and significantly elevated serum cobalt levels, while chromium levels remain normal. Radiographs demonstrate well-fixed components with a modular femoral head. Aspiration reveals sterile, opaque fluid. What is the most likely etiology?
Explanation
Question 60
A 68-year-old female is 8 weeks post-operative from an uncomplicated primary TKA. Her current range of motion is 10 degrees to 75 degrees despite aggressive, compliant physical therapy. She is medically stable and radiographs show well-aligned components. What is the most appropriate next step in management?
Explanation
Question 61
During a standard posterior approach to the hip for a THA, the short external rotators are tagged and reflected over the posterior capsule. Which of the following structures is most at risk of iatrogenic injury if a retractor is placed too aggressively deep and posterior to the acetabulum?
Explanation
Question 62
A patient complains of anterior knee pain and a sensation of patellar subluxation 1 year after a primary TKA. A computed tomography (CT) scan evaluates component rotation and demonstrates excessive internal rotation of the tibial component. What is the expected biomechanical consequence of a severely internally rotated tibial component on patellar tracking?
Explanation
None
