Masterclass: Surgical Repair of Dislocating Peroneal Tendons with Indirect Fibular Groove Deepening
Key Takeaway
This masterclass provides an exhaustive, real-time guide to surgical repair of dislocating peroneal tendons. We cover essential anatomy, meticulous preoperative planning, precise intraoperative steps for indirect fibular groove deepening, and critical pearls to navigate potential pitfalls. Fellows will gain a deep understanding of technique, rationale, and comprehensive postoperative management, ensuring successful outcomes for chronic peroneal instability.
Introduction and Epidemiology
Peroneal tendon subluxation or dislocation from the retrofibular groove is a relatively rare but highly debilitating cause of lateral ankle pain and functional disability. The acute injury often remains unrecognized in the emergency or primary care setting, frequently misdiagnosed as a standard lateral ankle sprain involving the anterior talofibular ligament or calcaneofibular ligament. Untreated or misdiagnosed acute injuries invariably predispose the patient to recurrent peroneal dislocation, potentially devastating peroneal tendon tears, and chronic lateral ankle instability.

The epidemiological profile of peroneal tendon instability demonstrates a strong predilection for specific athletic populations. It is most commonly observed in sports requiring rapid, forceful dorsiflexion of the ankle combined with sudden inversion, such as Alpine skiing, springboard diving, gymnastics, and American football. In the general population, the incidence is low, but among high-level athletes presenting with lateral ankle pain, the index of suspicion must remain high. Chronic subluxation leads to a mechanical attrition of the tendons, particularly the peroneus brevis, which becomes compressed between the subluxating peroneus longus and the sharp posterior ridge of the fibula.
Pathogenesis and Classification Mechanisms
Acute subluxation or dislocation of the peroneal tendons classically occurs when the foot is forcefully dorsiflexed while the peroneal muscles are in a state of strong, eccentric contraction. A classic example is the forward fall in Alpine skiing, where the rigid ski boot forces the ankle into extreme dorsiflexion while the skier attempts to correct the fall via violent peroneal contraction. Alternatively, resisted plantarflexion and inversion while the peroneals contract may also precipitate subluxation, frequently associating this injury with concomitant lateral ligamentous instability. Furthermore, peroneal dislocation may manifest as a sequela to severe intra-articular calcaneal fractures that result in lateral wall blowout and subsequent displacement of the calcaneus, which mechanically alters the retrofibular space.

The pathoanatomy of peroneal tendon dislocations is best understood through the Eckert and Davis classification system, which was later modified by Oden to include a fourth grade. This classification dictates the surgical approach and the specific structures requiring repair:
* Grade I: The superior peroneal retinaculum is stripped off the lateral malleolus, creating a periosteal pouch into which the tendons dislocate anteriorly. This is the most common variant.
* Grade II: The distal fibrous ridge of the fibula is avulsed along with the superior peroneal retinaculum.
* Grade III: A thin cortical bone fragment is avulsed from the posterolateral aspect of the fibula along with the superior peroneal retinaculum.
* Grade IV: The superior peroneal retinaculum is torn from its posterior insertion on the calcaneus or deep fascia, leaving the fibular attachment intact.
Surgical Anatomy and Biomechanics
A profound understanding of the lateral ankle compartment and the retrofibular anatomy is paramount for the successful surgical management of recurrent peroneal instability. The peroneus longus and brevis muscles constitute the two major dynamic stabilizers within the lateral compartment of the leg. Both muscles originate from the proximal and middle thirds of the fibula.

As these structures descend, they become tendinous before crossing the ankle joint, sharing a common synovial sheath. The spatial relationship between the two tendons is highly consistent and clinically relevant: as they course distally, the tendon of the peroneus brevis lies directly against the posterior surface of the distal fibula, positioned anterior and medial to the tendon of the peroneus longus. Distal to the tip of the fibula, each tendon enters a distinct tendon sheath, anatomically separated by the peroneal tubercle of the calcaneus.
Osteology and Retinacular Structures
Posterior to the distal fibula, both tendons are stabilized within the retrofibular groove by the superior peroneal retinaculum. The posterior surface of the distal fibula is covered by a specialized layer of fibrocartilage designed to facilitate the smooth, frictionless gliding of the peroneal tendons during ankle range of motion.

The morphological characteristics of the retrofibular groove are highly variable among individuals and play a critical role in the pathogenesis of instability. Cadaveric and advanced imaging studies demonstrate that a definite, concave groove is present in approximately 80 percent of the population. In the remaining 20 percent, the posterior surface of the fibula is either completely flat or distinctly convex, creating a biomechanical environment highly susceptible to tendon subluxation. Furthermore, a fibrocartilaginous rim located on the posterolateral border of the fibula typically adds an additional 2 to 4 millimeters to the functional depth of the sulcus.

The superior peroneal retinaculum serves as the primary static restraint to peroneal tendon subluxation. It is composed of a thickened band of deep crural fascia that is continuous with the periosteum of the distal fibula. Importantly, it does not attach directly to the fibrocartilage rim or the absolute posterolateral edge of the bone, but rather slightly anterior to it. The superior peroneal retinaculum exhibits extreme variability in both width and thickness. Anatomical studies have described five distinct insertional patterns, with the most common configuration involving bifurcated bands inserting into both the Achilles tendon sheath and the lateral calcaneus.

The fiber orientation of the superior peroneal retinaculum runs parallel to the calcaneofibular ligament. This shared vector means that severe inversion injuries resulting in calcaneofibular ligament rupture frequently impart significant sheer stress to the superior peroneal retinaculum, leading to simultaneous injury and combined lateral ankle and peroneal instability.
Indications and Contraindications
The decision to proceed with operative intervention for peroneal tendon instability depends heavily on the chronicity of the injury, the patient's functional demands, and the presence of concomitant intra-articular or tendinous pathology. While a first-time acute dislocation in a low-demand patient may occasionally be managed with strict immobilization in a short-leg cast with the ankle in slight plantarflexion and inversion, the recurrence rate in athletic populations approaches 50 to 70 percent. Therefore, acute dislocations in high-level athletes are increasingly considered an indication for early surgical repair to restore the anatomical constraints and prevent secondary tendon tears.

Chronic, recurrent lateral ankle instability involving the peroneal tendons is an absolute indication for surgical reconstruction. Patients typically present with a snapping sensation behind the lateral malleolus, chronic posterolateral swelling, and pain exacerbated by uneven terrain. Advanced imaging, specifically Magnetic Resonance Imaging or Computed Tomography, is mandatory to evaluate the morphology of the retrofibular groove, assess the integrity of the superior peroneal retinaculum, and identify longitudinal split tears of the peroneus brevis, which are present in over 60 percent of chronic cases.

| Clinical Scenario | Operative Indications | Non Operative Indications | Contraindications to Surgery |
|---|---|---|---|
| Acute Dislocation | High-demand athlete, concomitant lateral ligament rupture, displaced bony avulsion (Grade III) | Sedentary patient, non-displaced Grade I injury willing to undergo 6 weeks of rigid casting | Active local soft tissue infection, severe peripheral vascular disease |
| Chronic Subluxation | Recurrent symptomatic snapping, MRI evidence of peroneus brevis split tear, flat or convex fibular groove | Asymptomatic snapping, patient unfit for anesthesia | Charcot neuroarthropathy, uncorrectable hindfoot varus driving the instability |
| Combined Instability | Concomitant ATFL/CFL insufficiency requiring modified Broström-Gould alongside peroneal repair | Mild subjective instability responding well to peroneal strengthening and proprioceptive physical therapy | Inadequate soft tissue envelope for primary closure |
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning begins with a comprehensive review of the advanced imaging modalities. Axial CT scans are particularly useful for quantifying the depth of the retrofibular groove and identifying the presence of a convex fibular morphology, which dictates the necessity of a groove deepening procedure. MRI is scrutinized for fluid within the peroneal sheath, tenosynovitis, and the classic "boomerang" shape of the peroneus brevis, which indicates a longitudinal split tear requiring tubularization.

If the patient exhibits a significant cavovarus foot posture, the surgeon must plan for a concomitant lateralizing calcaneal osteotomy or dorsiflexion first metatarsal osteotomy. Failure to correct a rigid hindfoot varus will subject the repaired superior peroneal retinaculum to excessive tension, inevitably leading to surgical failure and recurrent dislocation.

For the isolated peroneal tendon repair and groove deepening, the patient is typically placed in the lateral decubitus position. This affords excellent, unobstructed access to the posterolateral ankle. Alternatively, a supine position with a large bump placed under the ipsilateral hip can be utilized, internally rotating the leg to expose the lateral malleolus. A thigh tourniquet is applied and inflated to provide a bloodless surgical field. Prophylactic intravenous antibiotics are administered prior to inflation. The operative leg is prepped and draped in a standard sterile fashion, ensuring the foot is entirely free to allow for intraoperative dynamic testing of the tendons.
Detailed Surgical Approach and Technique
The surgical management of recurrent peroneal instability typically involves a triad of procedures performed through a single approach: exploration and repair of the peroneal tendons, deepening of the retrofibular groove, and imbrication or reconstruction of the superior peroneal retinaculum.

Soft Tissue Dissection and Tendon Inspection
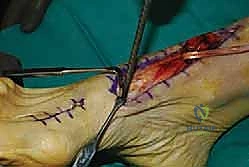
A longitudinal incision is made approximately 1 centimeter posterior to the posterior border of the distal fibula, extending from 4 centimeters proximal to the tip of the lateral malleolus down to the level of the peroneal tubercle. The subcutaneous tissues are carefully dissected. The surgeon must remain highly vigilant for the sural nerve and the lesser saphenous vein, which course superficially in the distal aspect of the incision. These structures are identified, mobilized, and gently retracted posteriorly using vessel loops.

The deep fascia is incised, revealing the superior peroneal retinaculum. The retinaculum is often found to be attenuated, redundant, or stripped from its fibular insertion, forming a false pouch. The retinaculum is sharply incised longitudinally, leaving a 2 to 3-millimeter cuff of tissue attached to the fibula to facilitate subsequent repair.

Both the peroneus longus and brevis tendons are luxated from the groove and meticulously inspected. The peroneus brevis is highly susceptible to longitudinal split tears due to the mechanical shear against the fibula. If a tear is identified, the degenerative margins are sharply debrided. If less than 50 percent of the tendon cross-sectional area is involved, the tendon is tubularized using a running locked absorbable suture (e.g., 3-0 Vicryl or PDS). If the degeneration is severe, tenodesis of the proximal and distal stumps of the brevis to the intact peroneus longus may be required.

Fibular Groove Deepening
Historically, various bone block procedures (such as the Kelly or DuVries techniques) were utilized to physically block anterior translation of the tendons. However, these have largely been abandoned due to high rates of hardware prominence, fracture of the bone block, and tendon attrition. The current gold standard is the direct fibular groove deepening procedure.

A rectangular cortical trapdoor is marked out on the posterior surface of the distal fibula. Using a sharp, thin osteotome or an oscillating microsaw, the cortical bone containing the smooth fibrocartilaginous gliding surface is carefully elevated, hinging it medially. Once the trapdoor is reflected, a high-speed burr or curette is utilized to excavate the underlying cancellous bone of the lateral malleolus, creating a deep concavity.

The cortical trapdoor is then tamped back down into the newly created cancellous void. Because the underlying bone has been removed, the cortical surface now forms a deep, concave, anatomical groove. The trapdoor is typically stable via impaction, but if necessary, it can be secured with a small bioabsorbable pin or bone wax. The integrity of the smooth fibrocartilaginous surface is maintained, preventing postoperative tendon adhesions.
Retinacular Repair and Augmentation
Once the groove is deepened, the tendons are reduced back into their anatomical position. The ankle is taken through a full range of motion, specifically forced dorsiflexion and eversion, to confirm that the tendons remain stable within the deepened sulcus.
The final, critical step is the robust repair of the superior peroneal retinaculum. If the native tissue is of good quality, it is advanced and repaired directly to the posterolateral ridge of the fibula. To achieve a secure osseous fixation, two or three small suture anchors (typically 2.5 mm or 3.0 mm) are placed along the posterolateral border of the fibula. The sutures are passed through the superior peroneal retinaculum using a pants-over-vest imbrication technique to eliminate any redundancy and obliterate the false pouch.
If the native retinaculum is severely deficient or absent, local tissue transfer is required. A slip of the Achilles tendon or a periosteal flap from the fibula can be rotated and sutured over the tendons to serve as a reconstructed retinaculum. After tying the sutures, dynamic stability is tested one final time. The subcutaneous tissue is closed with interrupted absorbable sutures, and the skin is reapproximated with a subcuticular closure or nylon sutures.
Complications and Management
While surgical outcomes for peroneal tendon repair and groove deepening are generally excellent, the procedure is not without risk. Complications can compromise functional recovery and necessitate revision surgery. A thorough understanding of these potential pitfalls is essential for the operating surgeon.

The most frequent complication is transient or permanent injury to the sural nerve. The nerve is highly variable in its course and can be easily stretched by retractors or entrapped in the retinacular repair sutures. Meticulous dissection and the use of blunt retractors are mandatory. Postoperative stiffness and tendon tethering can occur if the retinaculum is repaired too tightly or if the patient is immobilized for an extended period, leading to fibroplasia within the tendon sheath.
| Surgical Complication | Estimated Incidence | Prevention Strategy | Salvage and Management Strategy |
|---|---|---|---|
| Sural Neuritis / Neuroma | 5% to 10% | Direct visualization, gentle vessel loop retraction, careful suture placement | Gabapentinoids, targeted nerve blocks. Surgical exploration, neurolysis, or proximal neurectomy and burying into muscle if a true neuroma forms. |
| Recurrent Subluxation | 2% to 5% | Adequate groove deepening, robust anchor fixation, correction of hindfoot varus | Revision surgery with allograft reconstruction of the SPR, calcaneal osteotomy to correct underlying mechanical axis. |
| Tendon Adhesions / Tethering | 5% to 8% | Maintain cortical trapdoor integrity, avoid over-tightening SPR, early ROM protocols | Aggressive physical therapy. If refractory, surgical tenolysis and sheath reconstruction. |
| Suture Anchor Prominence | 1% to 3% | Use knotless anchors or bury knots deep to the fascial layer, avoid lateral placement | Hardware removal once biological healing of the retinaculum is confirmed (typically after 6 months). |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol must balance the need for rigid immobilization to allow the retinacular repair to heal with the necessity of early mobilization to prevent tendon adhesions and joint stiffness.

Phase 1: Tissue Healing (Weeks 0 to 2)
Immediately following surgery, the patient is placed in a well-padded, short-leg plaster or fiberglass splint with the ankle immobilized in slight plantarflexion and neutral inversion/eversion. This position removes all tension from the repaired superior peroneal retinaculum. The patient is strictly non-weight-bearing on the operative extremity using crutches or a knee scooter. Elevation and cryotherapy are emphasized to control edema.
Phase 2: Early Mobilization (Weeks 2 to 6)
At the two-week postoperative mark, the sutures are removed. The patient is transitioned into a controlled ankle motion (CAM) boot. Weight-bearing is gradually progressed, starting with partial weight-bearing and advancing to full weight-
Clinical & Radiographic Imaging



















You Might Also Like