First Metatarsal Lengthening for Revision Hallux Valgus: An Intraoperative Masterclass
Key Takeaway
Join us in the OR for a masterclass on first metatarsal lengthening. We'll meticulously cover the surgical anatomy, preoperative planning, and step-by-step intraoperative execution, focusing on external fixator application and corticotomy. Learn critical pearls and pitfalls to manage revision hallux valgus with debilitating transfer metatarsalgia, ensuring optimal outcomes and patient recovery.
Introduction and Epidemiology
Shortening of the first metatarsal is a well-documented and frequently unavoidable consequence of first metatarsal osteotomies performed for hallux valgus correction. While minor shortening is often clinically insignificant, substantial iatrogenic shortening disrupts the highly calibrated biomechanics of the forefoot. When the first metatarsal is considerably shortened, the structural deficit precipitates a pathologic shift in weight-bearing forces, leading to the development of painful transfer metatarsalgia of the lesser toes.

The epidemiology of transfer metatarsalgia secondary to first ray shortening correlates directly with the type and geometry of the primary corrective osteotomy. Distal chevron osteotomies, proximal crescentic osteotomies, and Scarf osteotomies all inherently result in some degree of longitudinal bone loss due to the width of the saw blade (kerf) and the geometric translation of the capital fragment. Furthermore, procedures such as the Lapidus arthrodesis (first tarsometatarsal fusion) require joint preparation that routinely shortens the medial column. While radiographic shortening is present in the vast majority of hallux valgus corrections, symptomatic transfer metatarsalgia occurs in approximately 5% to 15% of patients, dictating the need for advanced reconstructive procedures such as first metatarsal lengthening to restore normal forefoot kinematics.

Surgical Anatomy and Biomechanics
Normal Metatarsal Parabola and Length Relationships
The physiologically normal first metatarsal is generally of similar length to, or slightly shorter than, the neighboring second metatarsal. This specific length relationship between the first metatarsal and the lesser metatarsals is critical for maintaining the metatarsal parabola—a geometric arch that allows for a smooth, progressive weight transfer across the forefoot during the stance phase of gait.

The Windlass Mechanism
The relative length and plantar position of the first metatarsal head, along with its articulation with the sesamoid complex, optimizes the windlass mechanism described by Hicks. During terminal stance and toe-off, dorsiflexion of the hallux tightens the plantar fascia around the first metatarsal head. This action elevates the medial longitudinal arch, supinates the hindfoot, and creates a rigid lever for propulsion. The relative plantar position of the first metatarsal head makes the windlass mechanism more effective in transferring weight to the lesser toes and may, in some cases, compensate for a physiologically shorter first metatarsal.

Pathogenesis of Biomechanical Failure
An iatrogenically shortened first metatarsal fundamentally disrupts the normal forefoot weight transfer mechanism. When the first ray fails to bear its proportional load (typically supporting twice the load of any lesser metatarsal), a pathologic overload of the adjacent second and third metatarsals occurs.
Relative dorsiflexion (elevation) of the first metatarsal head frequently accompanies shortening after hallux valgus correction. This biplanar deformity exacerbates the mechanical disadvantage of the shortened metatarsal, completely unweighting the first ray during stance and severely compounding the transfer metatarsalgia. Over time, the excessive ground reaction forces on the lesser metatarsal heads lead to plantar plate attenuation, metatarsophalangeal (MTP) joint instability, and eventually, cross-over toe deformities.
Clinical Evaluation and Patient History
Natural History of Transfer Lesions
Transfer metatarsalgia generally does not resolve spontaneously, particularly if coupled with concomitant forefoot fat pad atrophy. Mild transfer metatarsalgia may initially be well tolerated as the patient intuitively modifies their gait, stance, and activity levels to compensate for the altered biomechanics. However, the problem typically progresses. Painful hyperkeratotic callus formation develops under the lesser metatarsal heads due to chronic shear and compressive forces. Severe, recalcitrant transfer metatarsalgia causes debilitating forefoot pain that persists until normal forefoot biomechanics are surgically restored or highly specialized footwear accommodation is utilized.
Physical Examination Findings
During physical examination, the great toe usually, but not always, appears visibly shorter than the adjacent second toe, especially when compared to the contralateral foot. The plantar surface of the forefoot reliably presents with intractable plantar keratoses (IPK) or calluses under the second and sometimes third metatarsal heads.


Palpation of the lesser metatarsal heads elicits marked tenderness, and the clinician must assess for associated plantar plate tears using the Lachman test of the MTP joints. When examined simultaneously, the first metatarsal head (and sesamoids) may appear elevated and more proximal relative to the second metatarsal head.
Medial forefoot incisions from prior forefoot surgery must be meticulously documented in anticipation of potential revision surgery, as prior scars dictate the surgical approach to minimize soft tissue necrosis. Furthermore, hallux MTP joint alignment must be examined. A recurrence of hallux valgus deformity after prior surgery will need to be corrected in conjunction with the metatarsal lengthening procedure.
Assessment of Metatarsophalangeal Joint Motion
Hallux MTP joint motion is a critical determinant of surgical candidacy. First metatarsal lengthening significantly increases tension on the soft tissue envelope, particularly the extensor hallucis longus (EHL) and the dorsal capsule. Pre-existing stiffness and crepitance strongly suggest underlying arthrosis. In the presence of degenerative joint disease or severe stiffness, restoring length via an interposition graft may exacerbate joint pain and severely limit range of motion, favoring a first MTP joint arthrodesis over an isolated metatarsal lengthening.



Indications and Contraindications
The decision to proceed with structural lengthening of the first metatarsal requires careful patient selection. The primary indication is debilitating, recalcitrant transfer metatarsalgia secondary to documented iatrogenic shortening of the first ray that has failed exhaustive non-operative management (e.g., custom orthotics with metatarsal offloading pads, rocker-bottom shoe modifications, and corticosteroid injections).

Contraindications primarily revolve around the quality of the surrounding soft tissues, the viability of the bone, and the status of the first MTP joint. Lengthening a metatarsal with an arthritic MTP joint will predictably result in a stiff, painful joint due to the increased capsular tension. In such cases, converting the prior osteotomy to a first MTP arthrodesis utilizing a structural bone block is the preferred reconstructive option.

| Management Strategy | Indications | Contraindications |
|---|---|---|
| Non-Operative Management | Mild to moderate transfer metatarsalgia, flexible lesser digit deformities, medically unfit for surgery, non-compliant patient. | Severe, debilitating pain failing conservative care, progressive rigid cross-over toe deformities. |
| First Metatarsal Lengthening | Symptomatic iatrogenic shortening (>5mm), preserved MTP joint cartilage, supple MTP range of motion, failed conservative care. | First MTP arthrosis, severe soft tissue contracture, active infection, compromised vascular status, Charcot neuroarthropathy. |
| First MTP Arthrodesis with Bone Block | Iatrogenic shortening combined with first MTP arthrosis, severe rigid hallux valgus recurrence, avascular necrosis of the metatarsal head. | Active infection, viable and supple MTP joint in a young, active patient. |
Pre Operative Planning and Patient Positioning
Radiographic Evaluation
Standard weight-bearing radiographs of the foot (anteroposterior, lateral, and sesamoid axial views) are mandatory. The AP radiograph is utilized to assess the metatarsal parabola. The relative length of the first metatarsal can be quantified using the Hardy and Clapham method or by assessing the Maestro criteria, which evaluates the relative lengths of all five metatarsals to determine the ideal functional curve.

The lateral radiograph is critical for evaluating the sagittal plane alignment. Iatrogenic elevation (dorsiflexion) of the first metatarsal must be identified, as the reconstructive osteotomy must simultaneously plantarflex and lengthen the ray to restore the weight-bearing tripod. The sesamoid axial view assesses the integrity of the sesamoid articulation and the presence of degenerative changes that might preclude joint-sparing surgery.

Templating and Graft Selection
Preoperative templating determines the exact size of the structural bone graft required. Lengthening defects of 5mm to 12mm are typically managed with a single-stage structural interposition bone graft (autologous iliac crest or tricortical allograft). Defects greater than 12mm to 15mm significantly increase the risk of soft tissue tension-related complications and may require gradual distraction osteogenesis utilizing an external fixator.

Patient Positioning
The patient is placed in the supine position on the operating table. A bump is placed under the ipsilateral hip to internally rotate the leg to a neutral position, allowing direct visualization of the dorsal and medial aspects of the foot. A thigh tourniquet is applied to ensure a bloodless surgical field. If autologous iliac crest bone graft (ICBG) is planned, the ipsilateral iliac crest is prepped and draped simultaneously.

Detailed Surgical Approach and Technique
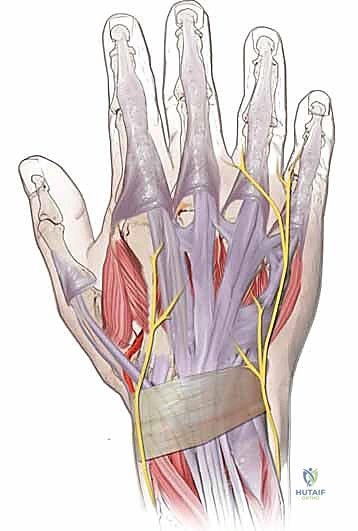
Incision and Soft Tissue Dissection
A dorsomedial longitudinal incision is typically utilized, centered over the first metatarsal diaphysis. It is imperative to incorporate or carefully bypass previous surgical scars to prevent narrow skin bridges that could lead to full-thickness necrosis.

Dissection is carried down through the subcutaneous tissues. The medial dorsal cutaneous nerve and the deep peroneal nerve branches must be identified and protected. The extensor hallucis longus (EHL) tendon is mobilized and retracted laterally. The periosteum is incised longitudinally, and full-thickness flaps are elevated dorsally and plantarward to expose the metatarsal diaphysis. Care is taken to preserve the plantar blood supply to the metatarsal head.

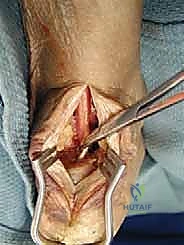
Osteotomy Preparation
A transverse or slightly oblique osteotomy is planned in the proximal or middle third of the metatarsal diaphysis, avoiding the previous osteotomy site if possible to ensure healthy, vascularized bone at the host-graft interface. Under fluoroscopic guidance, a sagittal saw is used to create the osteotomy.

Once the osteotomy is complete, a lamina spreader or specialized distraction forceps are inserted into the osteotomy site. The metatarsal is gradually distracted to the preoperatively templated length.

During distraction, the surgeon must carefully monitor the tension on the EHL tendon and the neurovascular bundle. Concomitant plantarflexion of the distal fragment is performed at this stage to correct any pre-existing dorsal elevation.

Graft Harvesting and Preparation
If autograft is selected, a structural tricortical block is harvested from the anterior iliac crest. Alternatively, a structural allograft (e.g., femoral head or iliac crest wedge) can be utilized to avoid donor site morbidity, though this carries a theoretically higher risk of delayed incorporation. The graft is meticulously contoured using a rongeur and burr to match the geometric defect created by the distraction, ensuring maximum cortical contact between the host bone and the graft.

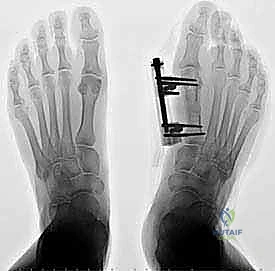
Graft Insertion and Fixation
The contoured structural graft is impacted into the osteotomy gap while maintaining distraction. Once the distractor is removed, the inherent soft tissue tension often provides excellent provisional compression across the graft.

Rigid internal fixation is paramount for the incorporation of a structural interposition graft. A low-profile dorsal or dorsomedial locking plate is applied. The plate must span the entire length of the osteotomy and graft, with a minimum of three bicortical locking screws securing the proximal and distal host bone segments.

An independent interfragmentary lag screw may be placed through the plate or outside the plate to compress the graft, provided the graft geometry allows for it without fracturing.

Soft Tissue Balancing
Following rigid fixation, the tension on the hallux MTP joint must be assessed. Significant lengthening inevitably tightens the EHL and the dorsal capsule, potentially leading to a rigid extension contracture of the hallux. If the MTP joint cannot be passively plantarflexed to neutral, a Z-lengthening of the EHL tendon and a dorsal MTP capsulotomy are required.
Complications and Management
First metatarsal lengthening is a technically demanding procedure associated with a distinct complication profile, primarily related to bone healing and soft tissue tension.

The utilization of structural interposition grafts inherently creates two osteotomy interfaces that must heal, doubling the risk of delayed union or nonunion compared to a primary osteotomy. Furthermore, the soft tissue envelope of the foot is unforgiving; excessive lengthening can lead to ischemic changes in the distal flap or severe joint stiffness.

| Complication | Incidence | Prevention and Management Strategies |
|---|---|---|
| Delayed Union / Nonunion | 5% - 15% | Prevention: Meticulous preparation of host bone, use of viable autograft, rigid locking plate fixation. Management: Prolonged immobilization, bone stimulator. If hardware fails, revision with rigid fixation and autologous bone grafting. |
| MTP Joint Stiffness | 20% - 40% | Prevention: Limit lengthening to <10mm in a single stage, perform prophylactic EHL lengthening and capsulotomy. Management: Aggressive physical therapy. If debilitating and arthritic, conversion to MTP arthrodesis. |
| Hardware Prominence / Failure | 5% - 10% | Prevention: Use low-profile plates, ensure adequate soft tissue coverage. Management: Hardware removal following complete radiographic union. |
| Recurrent Transfer Metatarsalgia | 5% - 10% | Prevention: Accurate preoperative templating to restore the Maestro curve, ensuring plantar |
Clinical & Radiographic Imaging





























You Might Also Like