FHL Tendon Augmentation for Insertional Achilles Tendinosis: An Intraoperative Masterclass
Key Takeaway
Join us in the OR for an immersive masterclass on Flexor Hallucis Longus (FHL) tendon augmentation for insertional Achilles tendinosis. We'll meticulously cover preoperative planning, precise patient positioning, and a granular, real-time breakdown of surgical execution, from initial incision to graft fixation and wound closure. Learn critical anatomical considerations, pearls, pitfalls, and comprehensive postoperative rehabilitation strategies to ensure optimal patient outcomes.
Introduction and Epidemiology
The term insertional Achilles tendinitis is widely recognized in historic orthopedic literature; however, it is fundamentally a misnomer. Histologic analyses demonstrate that the condition is more accurately characterized as a degenerative process rather than a primary acute inflammatory event. Consequently, the nomenclature should reflect this underlying pathophysiology, more appropriately designating the condition as insertional Achilles tendinosis or tendinopathy.

Insertional Achilles tendinopathy is identified by a recalcitrant, painful condition at the tendinous enthesis of the tendo Achilles on the posterior calcaneus. Epidemiological data indicate that insertional pathology represents approximately 10% to 20% of all Achilles tendon disorders. It is most frequently encountered as an overuse injury in athletic populations, particularly in runners and "push-off" athletes such as basketball or volleyball players. However, it is also highly prevalent in older, more sedentary patients, where it manifests as a progressive degenerative process linked to age-related tissue senescence and metabolic factors.

The pathogenesis of insertional Achilles tendinosis is multifactorial. Repetitive mechanical stress leads to a combination of degenerative and reactive changes. Degeneration occurs as the already compromised vascularity of the tendon insertion is further diminished by microtrauma and chronological aging. At the microscopic level, tenocytes are reduced in both number and metabolic quality, which severely blunts the intrinsic repair potential of the tendon. Macroscopically, this manifests as disorganized collagen architecture, mucoid degeneration, and angiofibroblastic hyperplasia.
While the tendon substance itself undergoes degeneration, inflammatory changes are often isolated to the paratenon, presenting as paratenonitis. This leads to thickening, fibrosis, and adherence of the paratenon to the underlying Achilles tendon. Furthermore, the continuum of chronic injury and inadequate biological repair capacity creates a pathological cycle of ectopic bone formation. Fibrocartilaginous metaplasia leads to collagen and calcium deposition at the tendinous enthesis in a biomechanical effort to stabilize the insertion site. This results in the generation of abundant, poor-quality tissue, enlargement of the insertion site (calcific spurring), and severe mechanical irritation of the surrounding bursal tissues.
Untreated insertional Achilles tendinosis typically follows a progressive natural history. Persistent pathology leads to continued pain and swelling of the retrocalcaneal heel, creating a vicious cycle in which further mechanical loading induces more disorganized attempts at repair. Range of motion is progressively reduced, leading to increased susceptibility to acute injury with any activity that places the tendo Achilles under eccentric strain. Intratendinous calcific debris compromises the viscoelasticity of the tendon, rendering the tissue less pliable and significantly increasing the risk of partial or complete insertional avulsion or rupture.
Surgical Anatomy and Biomechanics
The tendo Achilles is the largest and strongest tendon in the human body, formed by the confluence of the gastrocnemius and soleus muscle aponeuroses. Its chief biomechanical function is plantarflexion of the foot and ankle, providing the primary propulsive force during the gait cycle.

Biomechanically, the normal Achilles tendon is highly viscoelastic. It is capable of elongating up to 15% under physiological loads and routinely bears up to 10 times total body weight in single-legged stance during running and jumping activities. The Achilles insertion is not a single focal point but rather a broad, crescentic expanse that envelops the entire posterior tuberosity of the os calcis. It sends robust Sharpey fibers to the medial, lateral, and plantar borders of the bone, effectively dissipating stress across a wide osseous footprint.

Immediately anterior to the distal Achilles tendon lies the retrocalcaneal bursa, a synovial-lined sac that facilitates smooth gliding of the tendon over the posterosuperior calcaneal tuberosity. Deep to this bursa is a variably sized posterolateral bony prominence of the calcaneus, clinically recognized as a Haglund deformity. In the setting of insertional tendinosis, this prominence acts as a mechanical fulcrum, causing abrasive wear on the anterior fibers of the Achilles tendon during ankle dorsiflexion.

More anteriorly lies the deep posterior compartment musculature, which includes the flexor hallucis longus muscle and the primary neurovascular bundle of the posterior leg, containing the tibial nerve and posterior tibial vessels.
The flexor hallucis longus is of paramount surgical importance when considering augmentation for Achilles tendinosis. The flexor hallucis longus originates from the posterior surface of the distal two-thirds of the fibula and the adjacent interosseous membrane. The muscle belly extends remarkably distal, often reaching the level of the tibiotalar joint. The tendon travels obliquely and distally to pass posterior to the medial malleolus, coursing under the sustentaculum tali through a distinct fibro-osseous tunnel. It then traverses the plantar aspect of the foot, crossing dorsal to the flexor digitorum longus at the master knot of Henry, before finally inserting onto the base of the distal phalanx of the hallux.

The flexor hallucis longus is the ideal candidate for Achilles augmentation for several anatomical and biomechanical reasons. First, it is an in-phase plantarflexor, firing synergistically with the gastrocsoleus complex during the push-off phase of gait. Second, its axis of contractility is closely aligned with the Achilles tendon. Third, the low-lying muscle belly of the flexor hallucis longus provides a rich, local vascular supply to the relatively avascular Achilles insertion site when transferred, promoting biological healing of the compromised soft tissue envelope.
Indications and Contraindications
Patients typically present with a highly accurate description of their symptoms, complaining of insidious onset, progressive pain directly at the bone-tendon interface on the retrocalcaneal heel. The pain is characteristically worse following periods of inactivity or immediately after strenuous physical exertion. Upon physical examination, pathognomonic findings include localized tenderness at the central insertion, palpable thickening of the tendon, and a prominent retrocalcaneal exostosis.

Surgical intervention, specifically Achilles tendon debridement with flexor hallucis longus augmentation, is indicated when patients have failed exhaustive non-operative management and exhibit significant structural compromise of the tendon.

| Clinical Scenario | Operative Indications | Non Operative Indications |
|---|---|---|
| Duration of Symptoms | Refractory to treatment > 6 months | Acute or subacute onset (< 6 months) |
| Tendon Integrity | > 50% tendon detachment/debridement required | Intact tendon, minimal intrasubstance tearing |
| Patient Profile | Older, sedentary, or immunocompromised patients with poor tissue quality | Young athletes with isolated paratenonitis |
| Imaging Findings | Large intratendinous calcifications, massive Haglund deformity, severe tendinosis on MRI | Mild retrocalcaneal bursitis, minimal calcification |
| Functional Status | Severe limitation in activities of daily living, antalgic gait | Pain primarily after high-impact sports only |
Contraindications to flexor hallucis longus augmentation include active local or systemic infection, severe peripheral vascular disease that precludes safe wound healing, and profound medical comorbidities making anesthesia unsafe. Additionally, patients with pre-existing severe hallux rigidus or those who rely heavily on hallux push-off (such as elite ballet dancers) require careful preoperative counseling, as flexor hallucis longus harvest may result in subjective weakness of the great toe.
Pre Operative Planning and Patient Positioning
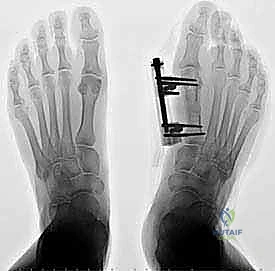
Thorough preoperative planning relies on a combination of clinical evaluation and advanced imaging modalities. Weight-bearing lateral radiographs of the foot and ankle are mandatory to assess the morphology of the calcaneus, specifically the presence of a Haglund deformity, the pitch of the calcaneus, and the extent of insertional calcific spurring.

Magnetic Resonance Imaging is the gold standard for evaluating the soft tissue architecture. Sagittal and axial T1 and T2-weighted sequences allow the surgeon to quantify the percentage of tendinosis, the presence of intrasubstance tears, and the quality of the flexor hallucis longus muscle belly. If MRI indicates that more than 50% of the tendon insertion is diseased and will require resection, flexor hallucis longus augmentation should be planned.

Surgical positioning is critical for optimal exposure. The patient is placed in the prone position on a standard operating table. Chest rolls and pelvic supports are utilized to ensure adequate pulmonary excursion and prevent abdominal compression. All bony prominences are meticulously padded.

A well-padded thigh tourniquet is applied to the operative limb to provide a bloodless surgical field. The operative extremity is prepped and draped in a standard sterile fashion. A bump is often placed beneath the distal tibia to allow the foot to hang freely over the edge of the bed, facilitating full, unobstructed intraoperative manipulation of the ankle joint through its entire range of motion.
Detailed Surgical Approach and Technique
Surgical Incision and Exposure
The surgical approach begins with a longitudinal incision. While some surgeons prefer a medial or lateral paratendinous approach, a central tendon-splitting approach is highly effective for direct access to the central degenerative pathology and the retrocalcaneal exostosis. The incision is centered over the distal Achilles tendon, extending from approximately 5 cm proximal to the insertion down to the distal aspect of the calcaneal tuberosity.

Careful dissection is carried through the subcutaneous tissues. It is imperative to maintain full-thickness fasciocutaneous flaps to preserve the fragile vascular supply to the posterior skin, thereby mitigating the high risk of postoperative wound necrosis. The paratenon is incised longitudinally and carefully reflected.

Achilles Tendon Debridement and Calcaneal Exostectomy
The Achilles tendon is incised longitudinally in its midline, following the direction of its fibers. The tendon is split and retracted medially and laterally, exposing the diseased central core, the retrocalcaneal bursa, and the posterosuperior calcaneal prominence.

All frankly necrotic, mucoid, and calcified tendon tissue is sharply excised until healthy, bleeding tendon margins are encountered. The retrocalcaneal bursa is completely excised to prevent postoperative bursitis.

Attention is then directed to the bony pathology. Using an osteotome or a sagittal saw, the Haglund deformity (posterosuperior exostosis) is resected. The osteotomy is directed from posterosuperior to anteroinferior, ensuring that a sufficient amount of bone is removed to prevent any residual impingement on the anterior aspect of the Achilles tendon during maximal ankle dorsiflexion. The resected bone edges are smoothed with a rasp or burr.

Flexor Hallucis Longus Harvest
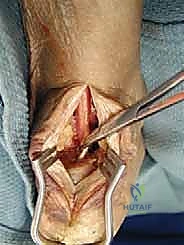
Once it is determined that the Achilles debridement has compromised more than 50% of the tendon insertion, flexor hallucis longus harvest is initiated. The harvest can be performed via a single-incision or double-incision technique. In the single-incision technique, dissection is carried deep through the deep crural fascia, medial to the Achilles tendon.

The flexor hallucis longus muscle belly is identified by its low-lying nature. The neurovascular bundle (posterior tibial artery and tibial nerve) lies immediately medial to the flexor hallucis longus and must be rigorously protected. The flexor hallucis longus tendon is identified and traced as far distally as possible into the fibro-osseous tunnel beneath the sustentaculum tali.

Maximal plantarflexion of the hallux allows the surgeon to pull the tendon proximally into the wound. The tendon is transected as distally as possible using a tendon stripper or direct sharp dissection, yielding an adequate length of tendon for transfer. A Krackow whipstitch using high-tensile non-absorbable suture is placed into the distal end of the harvested tendon.

Tendon Transfer and Fixation
A bone tunnel is prepared in the calcaneus to receive the flexor hallucis longus tendon. A guide pin is placed centrally within the decorticated Achilles footprint, directed from dorsal-posterior to plantar-anterior. The tunnel is reamed to match the measured diameter of the harvested flexor hallucis longus tendon (typically 7 to 8 mm).

The prepared flexor hallucis longus tendon is passed into the calcaneal tunnel. Fixation is most commonly achieved using a bioabsorbable or PEEK interference screw.

Tensioning of the transfer is a critical step. The ankle is held in neutral dorsiflexion (0 degrees) or slight plantarflexion (10-15 degrees), and maximum physiological tension is applied to the flexor hallucis longus tendon before advancing the interference screw. This ensures that the transferred muscle functions effectively as an active plantarflexor rather than a passive tenodesis.
Achilles Reconstruction and Wound Closure
Following rigid fixation of the flexor hallucis longus, the remaining native Achilles tendon is repaired. If the insertion was detached, it is reapproximated to the calcaneus using suture anchors. The longitudinal split in the Achilles is closed with absorbable sutures. The low-lying muscle belly of the flexor hallucis longus is draped over the repair site, providing a robust vascular bed to aid in the healing of the dysvascular Achilles tendon.
Meticulous hemostasis is achieved following tourniquet deflation. The wound is closed in multiple layers, ensuring the paratenon (if viable) and subcutaneous tissues are meticulously approximated to eliminate dead space. The skin is closed with non-absorbable vertical mattress sutures or staples, avoiding excessive tension on the skin edges.
Complications and Management
Surgical management of insertional Achilles tendinosis with flexor hallucis longus augmentation is a highly successful procedure, but it carries a distinct complication profile due to the tenuous vascularity of the posterior heel and the complex biomechanics of the region.

Wound healing complications are the most frequently encountered adverse events. The watershed vascular supply to the posterior skin makes it highly susceptible to ischemia, particularly if tissue handling is rough or if the skin flaps are elevated too superficially.

Deep infection is a catastrophic complication that may require serial debridements, removal of hardware (interference screws or suture anchors), and prolonged intravenous antibiotic therapy.

| Complication | Estimated Incidence | Prevention and Salvage Strategies |
|---|---|---|
| Wound Dehiscence / Necrosis | 5% - 10% | Prevention: Full-thickness flaps, meticulous hemostasis, avoid tight skin closure. Salvage: Local wound care, negative pressure wound therapy, reverse sural artery flap for massive defects. |
| Deep Infection | 1% - 3% | Prevention: Preoperative antibiotics, strict sterile technique. Salvage: Aggressive surgical debridement, hardware removal, infectious disease consultation. |
| Sural Nerve Injury | 2% - 5% | Prevention: Careful lateral dissection, avoid placing retractors too deeply on the lateral aspect. Salvage: Neuroma excision, burying the nerve stump into local muscle. |
| Hallux Weakness | 10% - 15% (Subjective) | Prevention: Distal harvest to preserve maximum length, tenodesis of FHL stump to FDL (optional). Salvage: Physical therapy focusing on intrinsic foot musculature. |
| Tendon Transfer Failure | < 2% | Prevention: Adequate interference screw sizing, proper tensioning in neutral ankle position. Salvage: Revision surgery, allograft reconstruction, or V-Y advancement flap. |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol is designed to protect the tendon transfer and the tenuous soft tissue envelope while progressively restoring range of motion and functional strength.

Phase 1: Maximum Protection (Weeks 0-2)
Immediately postoperatively, the patient is placed in a well-padded, short-leg plaster splint with the ankle immobilized in 15 to 20 degrees of plantarflexion. The patient is strictly non-weight-bearing on the operative extremity. Elevation is heavily emphasized to minimize edema and protect the surgical incision. At the 2-week mark, sutures are removed provided the wound is completely healed.
Phase 2: Controlled Mobilization (Weeks 2-6)
The patient is transitioned to a controlled ankle motion (CAM) boot equipped with heel wedges. The ankle remains in slight plantarflexion initially. Over the course of 4 weeks, the heel wedges are sequentially removed to gradually bring the ankle to a neutral position. Weight-bearing is progressively advanced from touch-down to full weight-bearing as tolerated within the boot. Active plantarflexion and active-assisted dorsiflexion to neutral are initiated.

Phase 3: Strengthening and Proprioception (Weeks 6-12)
The CAM boot is discontinued, and the patient transitions to a supportive athletic shoe, occasionally utilizing a small silicone heel lift for comfort. Formal physical therapy is intensified. The focus shifts to eccentric strengthening of the gastrocsoleus complex and the transferred flexor hallucis longus. Proprioceptive training on unstable surfaces (e.g., BAPS board) is incorporated to restore neuromuscular control.
**Phase 4:
Clinical & Radiographic Imaging



























You Might Also Like