Mastering Percutaneous Achilles Tendon Repair: An Intraoperative Masterclass
Key Takeaway
This masterclass details percutaneous Achilles tendon repair, guiding fellows through crucial anatomy, meticulous preoperative planning, and precise intraoperative execution. We explore two techniques: the three transverse and five stab incisions, emphasizing sural nerve protection, suture placement, and tensioning. Learn to manage complications and optimize postoperative rehabilitation for superior patient outcomes in acute ruptures.
Introduction and Epidemiology
Acute rupture of the Achilles tendon is a frequently encountered orthopedic injury, representing the most common tendon rupture in the lower extremity. The incidence of Achilles tendon ruptures has been rising, currently estimated at 18 to 32 per 100,000 person-years in Western populations. This increase is largely attributed to the growing population of older individuals participating in high-demand recreational sports, commonly referred to as "weekend warriors." The demographic distribution is classically bimodal, with a primary peak occurring in males aged 30 to 50 years engaged in intermittent athletic activities, and a secondary peak in older patients associated with degenerative tendinopathy.
Despite its prevalence, more than 20% of acute injuries are misdiagnosed at initial presentation in the emergency department or primary care setting. This high rate of missed diagnosis frequently leads to chronic or neglected ruptures. Misdiagnosis typically occurs because active plantarflexion of the foot is often preserved due to the uninhibited action of the tibialis posterior, peroneals, and long toe flexors. Furthermore, the acute hematoma and subsequent edema can rapidly fill the palpable gap in the tendon, masking the classic physical findings of a complete rupture.
Pathogenesis and Risk Factors
The mechanism of injury is almost exclusively non-contact. The most common mechanism involves a forceful push-off with the weight-bearing forefoot while the knee is extending, which maximizes the eccentric load on the gastrocnemius-soleus complex. Sudden unexpected dorsiflexion of the ankle (such as stepping into a hole) or violent dorsiflexion of a plantarflexed foot (such as falling from a height) are also well-documented mechanisms.
At a cellular level, ruptured Achilles tendons consistently demonstrate pre-existing degenerative changes, including hypoxic degenerative tendinopathy, mucoid degeneration, and lipomatous infiltration. Systemic risk factors significantly alter tendon matrix turnover and collagen synthesis. Fluoroquinolone antibiotics upregulate matrix metalloproteinases, leading to accelerated collagen degradation. Corticosteroid use (both systemic and local injections) inhibits fibroblastic proliferation and collagen synthesis. Other associated systemic conditions include inflammatory arthropathies, gout, hyperparathyroidism, and chronic kidney disease.
Surgical Anatomy and Biomechanics
A profound understanding of the local anatomy is paramount, particularly for percutaneous and minimally invasive interventions where direct visualization is limited. The Achilles tendon is the thickest and strongest tendon in the human body, capable of withstanding loads up to 10 times body weight during running and jumping.
Musculotendinous Architecture
The gastrocnemius muscle comprises two heads arising from the posterior aspects of the medial and lateral femoral condyles. The fleshy, muscular portion extends to approximately the midcalf. As the muscle fibers descend, they insert into a broad aponeurosis that narrows and thickens. Deep to the gastrocnemius lies the soleus muscle, which originates from the posterior tibia and fibula. The soleus aponeurosis merges with the deep surface of the gastrocnemius aponeurosis to form the Achilles tendon proper.
The tendon is approximately 15 cm long, originating in the midcalf and extending distally to insert into the posterior surface of the calcaneal tuberosity. A critical anatomical feature is the 90-degree lateral rotation of the tendon fibers as they descend. Consequently, the gastrocnemius fibers, which begin posteriorly, insert on the lateral aspect of the calcaneus, while the soleus fibers insert medially.

Vascular Supply and The Watershed Area
Unlike tendons with true synovial sheaths, the Achilles tendon is enveloped by a paratenon—a highly vascularized layer of loose connective tissue that allows for tendon gliding and provides the primary extrinsic blood supply. The anterior mesotenon carries the primary segmental vessels.
Microangiographic studies have identified a distinct hypovascular zone, or "watershed area," located 2 to 6 cm proximal to the calcaneal insertion. In this region, the vascular contribution from the paratenon and the osseous insertion is minimal, relying heavily on diffusion. This relative ischemia correlates directly with the most frequent site of spontaneous rupture and plays a significant role in delayed wound healing following open surgical approaches.
Sural Nerve Anatomy
The sural nerve provides sensory innervation to the posterolateral aspect of the distal third of the leg and the lateral border of the foot. It is formed by the union of the medial sural cutaneous nerve (a branch of the tibial nerve) and the sural communicating branch (from the common peroneal nerve).
The nerve pierces the deep fascia at the midcalf and descends adjacent to the small saphenous vein. It crosses the lateral border of the Achilles tendon approximately 9 to 12 cm proximal to the calcaneal insertion. In the distal third of the leg, the nerve lies in close proximity to the lateral border of the tendon, making it highly susceptible to iatrogenic entrapment or transection during percutaneous suture passage.
Indications and Contraindications
The management of acute Achilles tendon ruptures remains a topic of vigorous academic debate. Historically, open surgical repair was favored for young, active patients to minimize re-rupture rates, while conservative management was reserved for older, sedentary patients due to the high risk of soft tissue complications.
Percutaneous repair was developed as a strategic compromise. It aims to provide the optimal functional outcome and lower re-rupture rates associated with open repair while significantly decreasing the incidence of wound healing complications, skin breakdown, and deep infection. Recent literature suggests that minimally invasive and percutaneous techniques are less time-demanding, more cost-effective, and yield functional outcomes comparable to open repair, provided that the sural nerve is meticulously protected.
| Clinical Scenario | Operative Management | Non Operative Management |
|---|---|---|
| Patient Profile | High-demand athletes, young active individuals, delayed presentation (2-4 weeks) | Sedentary lifestyle, elderly patients, significant medical comorbidities |
| Local Tissue Status | Intact skin envelope, minimal to moderate edema | Severe peripheral vascular disease, active local infection, compromised skin envelope |
| Tendon Gap | Palpable gap > 1-2 cm in equinus | Apposition of tendon ends achievable in 20 degrees of plantarflexion (confirmed by ultrasound) |
| Contraindications | Active systemic or local infection, severe vasculopathy, chronic neglected ruptures requiring augmentation | Patient inability to comply with strict rehabilitation, massive gap preventing apposition |
Chronic or neglected ruptures (typically defined as > 4-6 weeks from injury) are generally a contraindication for standard percutaneous repair. The retraction of the proximal stump, combined with the infiltration of fibrous, non-functional scar tissue into the defect, necessitates an open approach for debridement and often requires augmentation with a V-Y advancement, turndown flap, or flexor hallucis longus transfer.
Pre Operative Planning and Patient Positioning
The diagnosis of an acute Achilles tendon rupture is primarily clinical. A thorough history and physical examination are usually sufficient to establish the diagnosis and proceed with surgical planning.
Clinical Examination
Patients typically report a sudden, sharp pain in the posterior calf, often described as feeling like they were struck by a blunt object or kicked. An audible "snap" or "pop" is frequently reported, followed immediately by weakness in push-off and an altered, flat-footed gait.
On physical examination, a palpable defect is usually present 2 to 6 cm proximal to the calcaneal insertion. However, in delayed presentations, organizing hematoma and edema may fill this gap, rendering palpation unreliable.
The Calf Squeeze Test (Simmonds-Thompson test) is the most reliable clinical indicator. With the patient prone and feet hanging clear of the examination table, the examiner squeezes the fleshy, muscular belly of the calf. In a normal limb, this deformation of the soleus mechanically pulls the intact Achilles tendon, resulting in passive plantarflexion of the foot. In a complete rupture, this continuity is lost, and the foot remains stationary.
The Matles Test (Knee Flexion Test) is another highly sensitive maneuver. The prone patient is asked to actively flex both knees to 90 degrees. In a normal limb, resting tension in the intact Achilles tendon keeps the foot in slight plantarflexion. On the affected side, the loss of resting tension causes the foot to fall into neutral or dorsiflexion relative to the contralateral side.

Imaging Studies
While the diagnosis is clinical, imaging can be useful in equivocal cases or to assist in surgical planning.
* Plain Radiographs: Lateral weight-bearing views are obtained to rule out bony avulsions of the calcaneal tuberosity. They may also reveal disruption of Kager's fat pad (the radiolucent triangular space anterior to the Achilles tendon) or a thickened tendon shadow.
* Ultrasonography: A dynamic, cost-effective modality that can confirm the rupture, measure the gap distance in neutral and plantarflexion, and assess the degree of tendon retraction.
* Magnetic Resonance Imaging: MRI is rarely required for acute ruptures but is the gold standard for evaluating chronic ruptures, assessing the quality of the remaining tendon, and planning complex reconstructions.
Patient Positioning and Preparation
General anesthesia, regional anesthesia (spinal block), or local anesthesia with intravenous sedation can be utilized. The patient is placed in the prone position on the operating table. Chest rolls and pelvic bolsters are placed to ensure adequate ventilation and decrease abdominal venous pressure.
The lower extremities should be positioned such that the feet extend just past the edge of the operating table. This allows for unrestricted passive range of motion of the ankle, which is critical for assessing resting tension during knot tying. A thigh tourniquet is applied but may not need to be inflated depending on the specific percutaneous technique and the amount of bleeding encountered. The operative leg is prepped and draped in a standard sterile fashion, ensuring the contralateral leg is accessible for comparison of resting equinus tension.
Detailed Surgical Approach and Technique
The evolution of percutaneous repair has led to the development of various techniques and proprietary jig systems (e.g., PARS, Achillon). The fundamental goal across all percutaneous methods is to pass high-strength sutures through the proximal and distal tendon stumps via small stab incisions, avoiding a large longitudinal incision that disrupts the paratenon and vascular supply.
Incision and Exposure
The palpable defect is carefully marked with a sterile pen. The expected course of the sural nerve is also mapped out along the lateral border of the tendon.
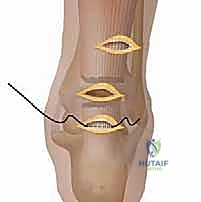
Depending on the specific technique, a series of 4 to 6 transverse or longitudinal stab incisions (approximately 0.5 to 1 cm in length) are made. Typically, two to three incisions are placed along the medial and lateral borders of the proximal stump, and two are placed along the distal stump. Alternatively, a single transverse "mini-open" incision (2-3 cm) can be made directly over the defect, through which a specialized jig is introduced into the paratenon sheath.

Suture Passage and Sural Nerve Protection
Meticulous soft tissue handling is required to prevent sural nerve entrapment. When making the lateral stab incisions, dissection must be carried down bluntly using a hemostat to the level of the paratenon. The sural nerve must be actively swept anteriorly and laterally away from the path of the suture passing instruments.
High-strength, non-absorbable sutures (e.g., #2 or #5 ultra-high molecular weight polyethylene) are utilized.
In a classic percutaneous technique (without a jig):
1. A straight Keith needle or specialized suture passer is introduced through a proximal lateral stab incision, passing transversely through the proximal tendon stump, and exiting the corresponding medial stab incision.
2. The suture is then passed diagonally from the proximal medial incision down to a mid-level lateral incision, creating a locking configuration (similar to a modified Bunnell or Krackow weave) within the substance of the tendon.
3. This process is repeated for the distal stump.
4. Crucially, all sutures must be passed deep to the crural fascia to avoid superficial skin puckering and superficial nerve entrapment.
In jig-assisted techniques:
1. The paratenon is opened transversely at the level of the rupture.
2. The jig is advanced proximally deep to the paratenon but superficial to the tendon.
3. Needles are passed through the guide holes of the jig, traversing the skin, paratenon, and tendon.
4. The jig is then withdrawn, pulling the sutures out through the central incision. This method captures the tendon fibers securely while theoretically pushing the sural nerve outward, minimizing entrapment risk.
Reduction and Fixation
Once the sutures have been securely woven through both the proximal and distal stumps, the free ends are retrieved through the central defect incision (in mini-open techniques) or through one of the distal stab incisions.
The ankle is placed in maximal plantarflexion to approximate the tendon ends. The surgeon must carefully clear the intervening hematoma and any interposed paratenon or fibrinous debris from the gap to ensure true tendon-to-tendon contact.
With the ankle held in plantarflexion, the sutures are tied. The critical step here is establishing the correct resting tension. The tension must be matched to the contralateral, uninjured limb. Undertensioning will result in tendon elongation, leading to a permanent deficit in plantarflexion power and an abnormal gait. Overtensioning can lead to excessive stiffness and difficulty achieving normal dorsiflexion during the stance phase of gait.

Closure
Following secure knot tying, the ankle is passively dorsiflexed to neutral to test the integrity of the repair. The paratenon, if opened, is meticulously closed with fine absorbable sutures (e.g., 3-0 Vicryl) to prevent tendon adhesions to the overlying skin. The skin incisions are closed with non-absorbable monofilament sutures or simple interrupted absorbable sutures. A sterile dressing is applied, and the limb is immobilized in a well-padded short leg cast or a rigid fracture boot locked in 20 to 30 degrees of plantarflexion.
Complications and Management
While percutaneous repair significantly reduces the incidence of major soft tissue complications compared to traditional open repair, it carries a unique complication profile that requires careful preoperative counseling and meticulous surgical technique.
| Complication | Estimated Incidence | Etiology and Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Sural Nerve Injury | 2% - 10% | Blind percutaneous suture passage, lateral stab incisions, anatomical variants | Intraoperative: Blunt dissection to paratenon, sweep nerve laterally. Postoperative: Observation for neuropraxia. If painful neuroma develops, surgical exploration and excision/burying of the nerve stump may be required. |
| Re-rupture | 2% - 5% | Non-compliance with rehab, early aggressive dorsiflexion, inadequate initial fixation | Revision surgery via an open approach. Often requires augmentation (V-Y advancement, FHL transfer) due to tissue retraction and scar formation. |
| Infection (Superficial/Deep) | < 1% - 2% | Poor skin envelope, diabetes, smoking, knot prominence | Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, hardware/suture removal if healing is compromised, targeted IV antibiotics. |
| Tendon Elongation | 5% - 10% | Undertensioning during surgery, aggressive early weight-bearing without heel wedges | Conservative: AFO bracing, focused strengthening. Surgical: Rarely indicated unless functional deficit is profound; requires open shortening osteotomy or plication. |
| DVT / PE | 1% - 5% | Immobilization, hypercoagulable states, delayed weight-bearing | Prophylactic anticoagulation (LMWH or Aspirin) based on patient risk stratification. Therapeutic anticoagulation if diagnosed. |
Sural Nerve Neuropraxia and Entrapment
The most significant specific risk of percutaneous repair is iatrogenic injury to the sural nerve. Older, purely blind percutaneous techniques reported nerve injury rates as high as 10-15%. The advent of mini-open techniques and specialized jigs has reduced this rate to approximately 2-5%. If a patient wakes up with sharp, radiating pain along the lateral foot or profound numbness, an entrapped nerve must be suspected. While transient neuropraxia from traction may resolve with observation, a true suture entrapment often necessitates early return to the operating room to release the offending suture before permanent axonal damage occurs.
Post Operative Rehabilitation Protocols
The paradigm of postoperative management following Achilles tendon repair has shifted dramatically over the past two decades. Prolonged cast immobilization has been largely abandoned in favor of early functional rehabilitation, which has been shown to stimulate collagen synthesis, improve fiber alignment, and decrease the risk of deep vein thrombosis without significantly increasing the re-rupture rate.
Phase 1: Maximum Protection (Weeks 0-2)
- Immobilization: The patient is placed in a short leg cast or a rigid CAM (Controlled Ankle Motion) boot locked in 20 to 30 degrees of equinus.
- Weight-Bearing: Non-weight-bearing (NWB) with crutches or a knee scooter.
- Therapy: Active range of motion of the toes, knee, and hip. Strict elevation to control edema.
Phase 2: Early Mobilization (Weeks 2-6)
- Immobilization: Transition to a CAM boot with stacked heel wedges (typically three 1 cm wedges) to maintain plantarflexion.
- Weight-Bearing: Progressive partial weight-bearing (PWB) to full weight-bearing (FWB) as tolerated in the boot.
- Therapy: The boot is removed for formal physical therapy. Gentle active plantarflexion and active-assisted dorsiflexion to neutral (0 degrees) are initiated. Passive dorsiflexion past neutral is strictly prohibited to protect the healing tendon from excessive tensile loads.
Phase 3: Progression to Neutral (Weeks 6-12)
- Immobilization: Heel wedges are systematically removed (e.g., one wedge every 1-2 weeks) until the foot reaches neutral in the boot. The boot is typically discontinued around week 8-10, transitioning to a normal shoe with a small heel lift.
- Weight-Bearing: FWB in the boot, then in shoes.
- Therapy: Initiation of isometric and isotonic strengthening. Bilateral heel raises progress to unilateral heel raises. Proprioceptive training (e.g., BAPS board, single-leg stance) is emphasized.
Phase 4: Return to Sport (Months 3-6+)
- Therapy: Eccentric strengthening protocols are advanced. Plyometric training, agility drills, and sport-specific activities are introduced.
- Clearance: Return to high-impact sports or competitive athletics is typically permitted between 5 and 9 months postoperatively, contingent upon achieving >90% strength and functional symmetry compared to the uninjured limb.
Summary of Key Literature and Guidelines
The management of acute Achilles tendon ruptures is guided by several landmark studies and meta-analyses that have shaped modern clinical practice guidelines.
The American Academy of Orthopaedic Surgeons (AAOS) Clinical Practice Guidelines provide moderate evidence supporting the use of functional rehabilitation protocols over prolonged immobilization, regardless of whether the patient is managed operatively or non-operatively.
A pivotal randomized controlled trial by Willits et al. (JBJS, 2010) demonstrated that when an accelerated functional rehabilitation protocol is employed, there is no clinically important difference in the re-rupture rate between operatively and non-operatively managed patients. However, operative management (including percutaneous repair) continues to be favored in high-level athletes due to a trend toward improved peak plantarflexion strength and a lower incidence of tendon elongation.
A comprehensive meta-analysis by Soroceanu et al. (JBJS, 2012) evaluated open versus percutaneous repair. The study concluded that percutaneous repair resulted in significantly lower rates of superficial infection and wound complications compared to open repair, with no significant difference in re-rupture rates. The meta-analysis highlighted that while sural nerve injury was historically higher in the percutaneous group, modern mini-open and jig-assisted techniques have largely mitigated this risk, solidifying percutaneous repair as a highly effective, safe, and reliable surgical option for the acute Achilles tendon rupture.
Clinical & Radiographic Imaging




You Might Also Like