Fracture Healing and Bone Regeneration: A Comprehensive Surgical Guide
Key Takeaway
Fracture healing is a highly regulated biological cascade comprising inflammatory, reparative, and remodeling phases. Successful bone regeneration depends on the precise interplay of cellular recruitment, molecular signaling, and mechanobiology. This guide details the physiological pathways of osteogenesis, the management of open fractures, stabilization biomechanics, and advanced bone grafting techniques essential for optimizing clinical and radiographic union in orthopedic trauma.
INTRODUCTION TO FRACTURE HEALING
Fracture healing, or bone regeneration, is a highly complex, postnatal recapitulation of embryonic bone development. It requires the precise spatial and temporal recruitment of specific cellular lineages—including fibroblasts, macrophages, chondroblasts, osteoblasts, and osteoclasts—alongside the expression of genes regulating matrix production, growth factors, and transcription factors.
Unlike other tissues that heal through the formation of fibrotic scar tissue, bone possesses the unique capacity to regenerate completely, restoring its original mechanical and structural properties. The ultimate goal of orthopedic intervention is to facilitate this biological cascade, achieving both clinical and radiographic union.
- Clinical Union: Defined as the point at which progressively increasing stiffness and strength provided by the mineralization process renders the fracture site stable and pain-free upon physiological loading.
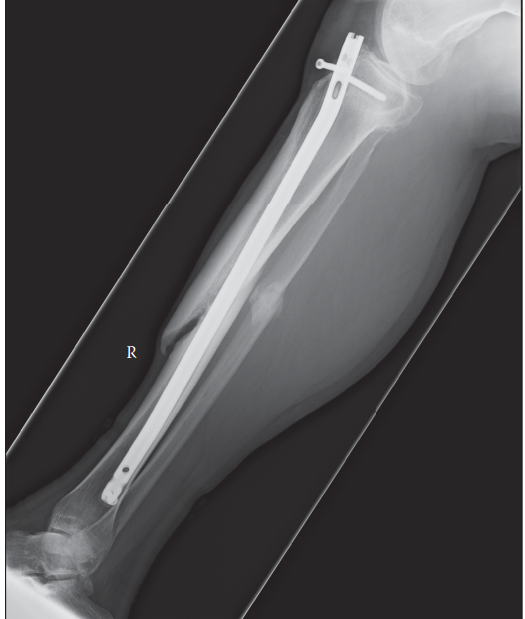
- Radiographic Union: Confirmed when plain radiographs demonstrate continuous bone trabeculae or cortical bone crossing the fracture site on at least three out of four cortices in orthogonal views.
Clinical Pearl: Radioisotope studies demonstrate increased metabolic activity at fracture sites long after painless function has been restored and radiographic union is achieved. This indicates that the microscopic remodeling process continues for months or even years post-injury.
THE BIOLOGICAL CASCADE OF BONE REGENERATION
A fracture initiates an interdependent sequence of inflammation, repair, and remodeling. If this cascade proceeds undisturbed, the injured bone is restored to its pre-injury state.
1. The Inflammatory Phase
Immediately following the mechanical disruption of bone and surrounding soft tissues, blood vessels rupture, leading to the formation of a fracture hematoma. This hematoma is not merely a passive clot; it serves as a critical biological scaffold and a source of potent signaling molecules.
* Inflammatory cells (macrophages, neutrophils) invade the hematoma, initiating the lysosomal degradation of necrotic tissue.
* Degranulating platelets and macrophages release key cytokines, including Transforming Growth Factor-beta (TGF-β) and Platelet-Derived Growth Factor (PDGF).
* These signaling molecules initiate the chemotaxis and proliferation of pluripotential mesenchymal stem cells (MSCs), setting the stage for the reparative phase.
2. The Reparative Phase
Typically beginning 4 to 5 days post-injury, the reparative phase is characterized by the invasion of pluripotential mesenchymal cells.
* Angiogenesis: The proliferation of new blood vessels within the periosteal tissues and marrow space is critical. It routes osteoprogenitor cells to the fracture site and forms a bed of granulation tissue.
* Soft Callus Formation: Under conditions of relative stability (low oxygen tension, micromotion), MSCs differentiate into chondroblasts, producing a cartilaginous soft callus that bridges the fracture gap and provides initial mechanical stability.
* Hard Callus Formation: As angiogenesis progresses and oxygen tension rises, endochondral ossification occurs. The cartilage is calcified, resorbed, and replaced by woven bone through the action of osteoblasts.
3. The Remodeling Phase
The transition of the fracture callus to woven bone and its subsequent mineralization signals the onset of remodeling. This phase is governed by Wolff’s Law, which dictates that bone adapts to the mechanical loads placed upon it.
* Osteoclasts resorb the disorganized woven bone via cutting cones.
* Osteoblasts lay down highly organized lamellar bone along lines of mechanical stress.
* The medullary canal is reconstituted, and the bone's normal morphology and mechanical strength are fully restored.
TISSUE-SPECIFIC RESPONSES AND MECHANOBIOLOGY
Einhorn described four distinct healing responses based on anatomical location: the bone marrow, cortex, periosteum, and external soft tissues.
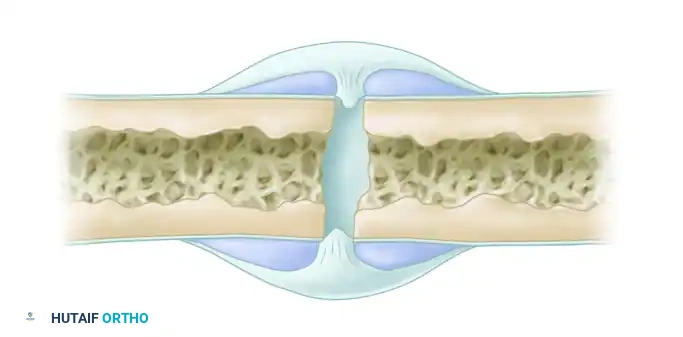
- The Periosteal Response: Perhaps the most critical component of secondary fracture healing. The periosteum contains committed osteoprogenitor cells and uncommitted mesenchymal cells. It is capable of bridging massive gaps (up to half the diameter of the bone) through a combination of intramembranous and endochondral ossification. This response is enhanced by controlled micromotion and inhibited by absolute rigid fixation.
- The External Soft Tissue Response: Heavily dependent on mechanical factors, this response involves rapid cellular activity to develop early bridging callus. Like the periosteal response, it can be suppressed by rigid immobilization.
Mechanobiology of Bone Formation
The type, amount, and location of bone formed are profoundly influenced by the mechanical environment (fixation rigidity, loading, and gap condition). Carter et al. proposed a mechanobiological model demonstrating how stress dictates cellular differentiation:
* Compression and Low Oxygen Tension: Drives differentiation into chondroblasts, resulting in cartilage formation (endochondral ossification).
* Tension and High Oxygen Tension: Drives differentiation into fibroblasts, producing fibrous tissue (intramembranous ossification).
* High Shear Stress: Promotes fibrous tissue formation and heterotopic ossification, often leading to nonunion if excessive.
FACTORS INFLUENCING FRACTURE HEALING
Fracture healing is vulnerable to numerous systemic and local variables. Uthoff classified these factors into those present at the time of injury, those caused by the injury, those dependent on treatment, and those associated with complications.
Systemic Factors
- Endocrine/Metabolic: Diabetes mellitus, thyroid disorders, and hormonal imbalances (growth hormone, corticosteroids) impair microvascular perfusion and cellular proliferation.
- Nutritional: Deficiencies in Vitamins A, C, D, and K, as well as general malnutrition, severely delay mineralization.
- Pharmacological: Nonsteroidal anti-inflammatory drugs (NSAIDs) inhibit prostaglandin synthesis, which is vital for the inflammatory phase. Corticosteroids, anticoagulants, and cytotoxins also suppress osteogenesis.
- Social Habits: Nicotine causes profound peripheral vasoconstriction and cellular toxicity, significantly increasing the risk of nonunion.
Local Factors
- Injury Severity: High-energy trauma causes extensive comminution and severe disruption of the vascular supply to the bone (macrovascular osteonecrosis) and surrounding soft tissues.
- Treatment Variables: The degree of surgical trauma (e.g., periosteal stripping, thermal necrosis from reaming), the rigidity of fixation, and the extent of contact between fragments (gap size, overdistraction) dictate the healing pathway.
Host Classification and Complication Prediction
A patient’s general health, socioeconomic situation, and neuropsychiatric history are powerful predictors of complications, particularly in open fractures.
* Type A Host: Normal, healthy patient.
* Type B Host: Compromised patient (e.g., controlled diabetes, smoker).
* Type C Host: Severely compromised patient (e.g., severe malnutrition, uncontrolled diabetes, immune deficiency).
Surgical Warning: Retrospective data on open tibial fractures reveals that complications develop in 48% of Type C hosts, compared to only 19% of Type A hosts. Infection rates are nearly eight times higher in patients with three or more compromising comorbidities. Host classification should be used alongside the Gustilo-Anderson classification to guide closure and coverage decisions.
SURGICAL MANAGEMENT OF BONE INJURIES AND OPEN FRACTURES
The management of open fractures requires a delicate balance between achieving mechanical stability and preserving the fragile biological environment. Disruption of the periosteum reduces bone vascularity, while severe soft tissue injury exacerbates fracture instability.
Debridement and Fragment Management
Thorough surgical debridement is the cornerstone of open fracture management.
* Small, Avascular Fragments: Bone fragments completely devoid of soft tissue attachment and grossly contaminated must be excised, as adequate cleansing is impossible.
* Large Avascular Segments: The management of large extruded cortical segments remains controversial. Generally, it is safest to remove avascular bone to prevent it from acting as a nidus for bacterial biofilm, planning for delayed autogenous bone grafting.
* Sterilization Techniques: In highly selected cases where large segments of cortical bone are extruded, experimental sterilization using povidone-iodine, chlorhexidine-gluconate, or autoclaving has been attempted, though this carries a high risk of structural failure and infection.
* Retained Fragments: Small pieces of bone with intact periosteum and soft tissue attachments should be meticulously preserved. They act as vascularized autografts and stimulate the healing cascade.
Fracture Stabilization Strategies
The chosen method of stabilization must provide adequate mechanical stability while minimizing further iatrogenic damage to the zone of injury.
- Type I Open Fractures: Generally amenable to standard closed fracture management techniques, including reamed intramedullary (IM) nailing.
- Type II and III Open Fractures: Management is highly debated. Options include external fixation, unreamed IM nailing, and occasionally plate osteosynthesis.
- Metaphyseal-Diaphyseal Fractures: External fixation is often preferred, occasionally supplemented with limited internal screw fixation.
- Diaphyseal Fractures (Lower Extremity): Intramedullary nailing has become the gold standard. Data from the Elvis Presley Regional Trauma Center strongly supports unreamed IM fixation for open femoral and tibial fractures.
- In a series of 125 open femoral fractures, a 100% union rate was achieved with only a 4% infection rate.
- In 50 open tibial fractures (including severe Type IIIB and IIIC), union was achieved in 96%, with an 8% infection rate. Notably, 36% of these required secondary procedures such as dynamization or bone grafting.
- Severe Salvageable Injuries (Type IIIB/IIIC): External fixation remains the primary, safest method of initial stabilization, allowing for aggressive soft tissue management and delayed definitive fixation.
ADVANCED BONE GRAFTING TECHNIQUES
When bone loss is significant or nonunion occurs, bone grafting is required to provide osteoconductive scaffolds, osteoinductive growth factors, and osteogenic cells.
Traditional Autograft Sources
- Iliac Crest Bone Graft (ICBG): The historical gold standard, providing excellent cancellous bone rich in osteoprogenitor cells.
- Fibula and Ribs: Utilized for structural grafts.
- Tibia: Historically used for long corticocancellous structural grafts, though this has declined with the advent of reliable allografts and rigid internal fixation.
The Reamer-Irrigator-Aspirator (RIA) Technique
The harvest of femoral bone marrow using the Reamer-Irrigator-Aspirator (RIA, Synthes) represents a major advancement in orthobiologics.
Indications and Biomechanics:
Originally developed to decrease intramedullary pressure and mitigate the risk of fat embolism during femoral reaming, the RIA system simultaneously captures massive volumes of highly osteogenic material.
Biological Profile of RIA Graft:
* Volume: Depending on the patient's anatomy, 25 to 90 mL of morselized bone and marrow can be harvested from a single femur.
* Cellular Composition: The captured bony fragments are exceptionally rich in mesenchymal stem cells (MSCs).
* Growth Factors: The effluent supernatant is highly concentrated with Fibroblast Growth Factor-2 (FGF-2), Insulin-like Growth Factor-1 (IGF-β1), and latent Transforming Growth Factor-beta 1 (TGF-β1). Interestingly, it does not contain high levels of Bone Morphogenetic Protein-2 (BMP-2).
Surgical Pitfall: While RIA provides massive volumes of high-quality autograft, surgeons must be cautious of over-reaming the donor femur, which can lead to iatrogenic cortical perforation or postoperative pathological fracture. Prophylactic stabilization of the donor femur is rarely required but cortical thickness must be evaluated preoperatively.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The postoperative management of fractures is as critical as the surgical intervention itself. Protocols must be tailored to the method of fixation (absolute vs. relative stability) and the biological status of the patient.
- Weight-Bearing: For diaphyseal fractures treated with intramedullary nails (relative stability), early progressive weight-bearing is encouraged. Axial loading stimulates the mechanotransduction pathways, promoting robust periosteal callus formation. Conversely, fractures treated with rigid plate fixation (absolute stability) require protected weight-bearing to prevent implant fatigue failure before primary bone healing occurs.
- Dynamization: In cases of delayed union following statically locked IM nailing, dynamization (the removal of interlocking screws at the longer end of the nail) may be performed at 10 to 12 weeks. This allows axial compression across the fracture site, stimulating the mechanobiological pathways described by Carter et al.
- Radiographic Monitoring: Serial radiographs should be obtained at 2, 6, 12, and 24 weeks to monitor callus formation, implant integrity, and the progression toward radiographic union.
- Nutritional and Medical Optimization: Postoperative protocols must include strict smoking cessation, optimization of glycemic control (HbA1c < 7.0%), and adequate Vitamin D and calcium supplementation to support the high metabolic demands of the remodeling phase.
You Might Also Like