Full Question & Answer Text (for Search Engines)
Question 1:
Following two previous shoulder stabilization procedures for recurrent dislocations, a 45-year-old man complains of pain and limited motion. Examination reveals increased passive external rotation and an inability to lift the back of the hand away from his back. Which of the following muscles is injured:
Options:
- Subscapularis
- Supraspinatus
- Infraspinatus
- Deltoid
- Teres minor
Correct Answer: Subscapularis
Explanation:
The patient has an incompetent subscapularis muscle. An inability to lift the back of the hand away from the back (a positive Liftoff test) has been described by Gerber and colleagues and is a reliable method of evaluating subscapularis integrity. Patients with subscapularis tears often demonstrate an increase in passive external rotation and weakness in internal rotation.
Question 2:
Which of the following is not a cause of failure following arthroscopic subacromial decompression:
Options:
- Error in diagnosis
- Detachment of the deltoid
- Reconstitution of bursal tissue
- Inadequate bone resection
- Retained coracoacromial (C A) ligament
Correct Answer: Reconstitution of bursal tissue
Explanation:
Causes of failure following arthroscopic decompression are similar to the causes of failure following open acromioplasty. Numerous studies have documented errors in diagnosis as the most common cause of failure. Inadequate bone resection can also cause continued pain and dysfunction. A retained coracoacromial ligament attachment can decrease the volume in the subacromial space and lead to recurrent impingement. Although bursal tissue can reconstitute following partial excision, this has not been shown as a common cause of failure following decompression. Deltoid detachment may cause weakness and pain.
Question 3:
Which of the following structures is involved in the â essential lesionâ of a stiff shoulder:
Options:
- Biceps tendon
- Coracohumeral ligament
- Posterior capsule
- Labrum
- Axillary pouch
Correct Answer: Coracohumeral ligament
Explanation:
The long head of the biceps tendon defines the region of the rotator interval, which is the area between the anterior edge of the supraspinatus tendon and the superior edge of the subscapularis tendon. This region usually is contracted in individuals who lack external rotation of the adducted shoulder. Coracohumeral ligament contracture is an important component of adhesive capsulitis.
Question 4:
A 35-year-old businessman sustains a type III acromioclavicular (AC ) separation of his dominant shoulder. Preferred treatment should be:
Options:
- Open subacromial decompression with distal clavicle resection
- Arthroscopic subacromial decompression
- Repair of coracoacromial ligament and fixation with a Bosworth screw
- Symptomatic treatment followed by return to activities as tolerated
- Reduction of the AC joint and stabilization with pins
Correct Answer: Symptomatic treatment followed by return to activities as tolerated
Explanation:
Long-term outcome studies have demonstrated good and excellent results following symptomatic, nonsurgical treatment of grade I-III acromioclavicular separations. Surgical treatment may lead to complications (especially with the use of transfixing smooth pins), loss of reduction, and chronic pain due to joint instability.
Question 5:
Which of the following muscles is most responsible for deceleration of the arm during pitching:
Options:
- Deltoid
- Coracobrachilis
- Teres minor
- Long head of the biceps
- Short head of the biceps
Correct Answer: Teres minor
Explanation:
During the deceleration phase, the excess kinetic energy that was not transferred to the ball is dissipated by controlled deceleration of the upper extremity. The rotator cuff (primarily teres minor) is the principle decelerator and is susceptible to tensile failure from eccentric loading.
Question 6:
Which of the following conditions most often accompanies a dislocation of the longhead of the biceps tendon?
Options:
- Anterior instability
- Presence of a Buford complex
- Subscapilars tendon pathology or tear
- Hill-Sachs lesions
- Excessive glenoid anteversion
Correct Answer: Subscapilars tendon pathology or tear
Explanation:
Although isolated ruptures of the biceps tendon have been described, most cases involving biceps tendon pathology are accompanied by rotator cuff injury. When computerized tomography arthrograms are performed on patients who have clinical criteria for isolated ruptures of the long head of the biceps, the incidence of isolated lesions decreases to 6%. Although primary bicipital tendinitis was recognized as a frequent cause of anterior shoulder pain in the 1950s, it is currently a diagnosis of exculsion that is made far less frequently.
Question 7:
Which of the following combinations correctly describes the contributions of the acromioclavicular ligaments and coracoclavicular ligaments in stabilizing the acromioclavicular joint:
Options:
- Horizontal stability is controlled by the coracoacromial ligament.
- Vertical stability is controlled by the acromioclavicular ligament.
- Horizontal stability is controlled by the coracoclavicular ligament and vertical stability is controlled by the acromioclavicular ligament.
- Horizontal stability is controlled by the coracoacromial ligament and vertical stability is controlled by the acromioclavicular ligament.
- Horizontal stability is controlled by the acromioclavicular ligament and vertical stability is controlled by the coracoclavicular ligament.
Correct Answer: Horizontal stability is controlled by the coracoacromial ligament.
Explanation:
Fuduka and colleagues have studied the individual ligamentous contributions to acromioclavicular stability by performing load displacement tests on sectioned cadaveric models. These experiments led to the conclusion that the horizontal stability of the acromioclavicular joint is controlled by the acromioclavicular ligament and vertical stability is controlled by the coracoclavicular ligament.
Question 8:
Which of the following statements is true concerning the bands of the anterior cruciate ligament:
Options:
- The anterolateral band is tightest in flexion.
- The posterolateral band is tightest in flexion.
- The posteromedial band is tightest in extension.
- The anteromedial band is tightest in flexion.
- The anteromedial band is tightest in extension.
Correct Answer: The anteromedial band is tightest in flexion.
Explanation:
The anterior cruciate ligament is composed of at least two functional bands. The larger anteromedial band is tightest in flexion and loosest in extension. The smaller posterolateral band is tightest in extension and loosest in flexion. Conventional anterior cruciate ligament reconstruction replaces only the anteromedial band.
Question 9:
Which of the following statements is true concerning the bands of the posterior cruciate ligament:
Options:
- The anterolateral band is tightest in flexion.
- The posterolateral band is tightest in flexion.
- The posteromedial band is tightest in flexion.
- The anteromedial band is tightest in flexion.
- The anteromedial band is tightest in extension.
Correct Answer: The anterolateral band is tightest in flexion.
Explanation:
The posterior cruciate ligament is composed of two functional bands. The larger anterolateral band is tightest in flexion and loosest in extension. The smaller posteromedial band is tightest in extension and loosest in flexion. Conventional posterior cruciate ligament reconstruction replaces only the anterolateral band.
Question 10:
The most sensitive test for posterior cruciate ligament injury is the:
Options:
- Posterior drawer test
- Quadriceps active drawer test
- Posterior sag sign
- Posterior Lachman test
- Dynamic posterior shift test
Correct Answer: Posterior drawer test
Explanation:
All of the above tests have been described for evaluating posterior cruciate ligament injury. Of these tests, the posterior drawer test is the most sensitive(95%).
Question 11:
A 30-year-old male avid runner presents with a 2-week history of right lateral knee pain. He denies any history of trauma, swelling, or mechanical symptoms. The pain only occurs with running and is relieved by cessation of activity. Physical examination does not demonstrate any effusion, and there is no pathologic laxity of the collateral or cruciate ligaments. There is tenderness to palpation along the lateral aspect of the knee that is most severe over the lateral epicondyle, particularly with the knee flexed to 30°. The next most appropriate course of action is:
Options:
- Obtain an magnetic resonance image
- Steroid injection to the right knee
- Arthroscopic debridement of the right lateral meniscus
- Arthroscopic repair of the right lateral meniscus
- Stretching of the right iliotibial band, temporary decrease in mileage, and anti-inflammatory medication
Correct Answer: Stretching of the right iliotibial band, temporary decrease in mileage, and anti-inflammatory medication
Explanation:
The patient has iliotibial band friction syndrome, which is common in runners. Physical therapy is successful in the majority of patients. Rarely, debridement of an ellipse of the iliotibial band will be required to provide relief.
Question 12:
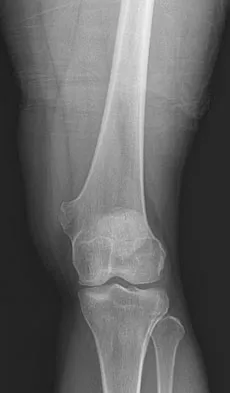
This radiograph shows a diaphysis of a 21-year-old female collegiate soccer player. She reports pain in the midshaft of her tibia for 7 months. She has been previously treated with cessation of soccer, 8 weeks in a short leg cast, and 3 months of treatment with an ultrasonic bone stimulator. Recommended treatment at this time should include:
Options:
- Observation
- Application of a long leg cast
- Application of a short leg case
- C ontinued treatment with an ultrasonic bone stimulator
- Insertion of a reamed intramedullary nail
Correct Answer: Insertion of a reamed intramedullary nail
Explanation:
The tibia is the bone most prone to stress fractures in athletes. The appearance of the "dreaded black line" is a poor prognostic indicator for
healing. Since this patient has failed nonoperative treatment, insertion of a reamed intramedullary nail would offer her the best chance of healing and earlier return to activity.
Question 13:
A "stinger" (transient weakness of the upper extremity commonly seen after a blow to the head and shoulder in football) most commonly affects the:
Options:
- Spinal cord
- C -5/C -6 nerve roots
- C -7/C -8 nerve roots
- Axillary nerve
- Musculocutaneous nerve
Correct Answer: C -5/C -6 nerve roots
Explanation:
"Stingers" are common in football. They generally result from a transient stretch to the C -5/C -6 nerve roots resulting in temporary loss of strength of the biceps, deltoid, and spinatus muscles. It is generally safe to allow the athlete to return to participation, provided the cervical spine examination is normal and any neurological deficits have completely resolved.
Question 14:
A 16-year-old male high school football player was making a tackle when he felt sudden pain in his right long finger. He has swelling and tenderness along the volar aspect of the injured digit. He is unable to actively flex the distal interphalangeal joint of the injured digit. Radiographs are negative for fracture. Recommended treatment should include:
Options:
- Observation
- Splinting of the distal interphalangeal joint in extension
- Splinting of the distal interphalangeal joint in flexion
- Immediate active range of motion exercises
- Surgical repair
Correct Answer: Surgical repair
Explanation:
Avulsion of the flexor digitorum profundus, or "jersey finger," is a common injury in football. Appropriate treatment includes surgical repair.
Question 15:
C atastrophic cervical spine injuries occurring during contact sports are most commonly a result of:
Options:
- Hyperflexion
- Hyperextension
- Flexion/compression
- Rotation
- Distraction
Correct Answer: Flexion/compression
Explanation:
Catastrophic injury of the cervical spine resulting in paralysis or death usually occurs from an axial loading mechanism, such as "spear" tackling in football. C ontroversy exists as to whether cervical spinal stenosis is a predisposing factor for catastrophic cervical spine injuries.
Question 16:
A collegiate level sprinter sustains an acute nondisplaced fracture at the proximal metaphyseal-diaphyseal junction of the fifth metatarsal. Appropriate treatment for early return to play includes:
Options:
- Observation
- Short leg walking cast
- Short leg non-weightbearing cast
- Application of an ultrasonic bone stimulator
- C ompression screw fixation
Correct Answer: C ompression screw fixation
Explanation:
Fractures of the metaphyseal-diaphyseal junction of the fifth metatarsal base, the Jones fracture, is treated more aggressively than its avulsed counterpart. In the acute situation, these fractures are treated in a non-weightbearing cast until union is obtained. Occasionally, an elite athlete will sustain a Jones fracture. It is important to determine whether this represents an acute injury or a stress fracture. Stress fractures are treated initially with non-weightbearing until union occurs and symptoms resolve. Acute Jones fractures in the athlete are best treated with compression screw fixation with bone graft to insure healing in a timely manner.
Question 17:
This is the radiograph of a right hand dominant 15-year-old baseball player who felt a pop when swinging a bat. There is pain in the upper portion of the first rib. Recommended treatment should consist of:
Options:
- Immobilization in a shoulder spica cast
- Immobilization in a sling
- Open reduction internal fixation with bone graft
- Open biopsy
- Observation
Correct Answer: Observation
Explanation:
First rib fractures in athletes are rare. These fractures are thought to be stress fractures, usually occurring in pitchers. Treatment is observation until the fracture is healed.
Question 18:
A 10-year-old female gymnast twists her knee on her dismount from the balance beam. She hears a pop and has immediate swelling. She is unable to continue with activity. Physical examination reveals a positive Lachman test and positive pivot shift. She has no joint line tenderness. Radiographs are normal. After an initial period of ice and range of motion exercises, recommended treatment should include:
Options:
- Direct repair of the anterior cruciate ligament
- Reconstruction of the anterior cruciate ligament using patellar tendon
- Reconstruction of the anterior cruciate ligament using hamstrings
- Extra-articular reconstruction
- Rehabilitation emphasizing hamstring strengthening
Correct Answer: Rehabilitation emphasizing hamstring strengthening
Explanation:
Anterior cruciate ligament injuries in children represent a vexing clinical problem. Standard anterior cruciate ligament reconstructions would involve drilling across an open physis, which may cause a growth disturbance. Results of direct repair or extra-articular reconstruction have been no better in children than in adults. The most reasonable initial treatment is rehabilitation. If despite adequate rehabilitation, the child continues to have instability, it is recommended that the child discontinues the activities that result in instability until skeletal maturity when a standard reconstruction can be performed, or when the child undergoes a physeal sparing reconstruction (i.e., Bergfeld's "tomato stake" reconstruction).
Question 19:
The most common location of osteochondritis dissecans in the knee is the:
Options:
- Lateral aspect of the medial femoral condyle
- Medial aspect of the lateral femoral condyle
- Medial aspect of the medial femoral condyle
- Lateral facet of the patella
- Lateral aspect of the femoral trochlea
Correct Answer: Lateral aspect of the medial femoral condyle
Explanation:
Osteochondritis dissecans affects adolescents, and the knee joint is the most commonly affected joint. The most common location in the knee is the lateral aspect of the medial femoral condyle at the intercondylar notch. Treatment varies with the stability of the lesion from observation to operative reduction and fixation.
Question 20:
A 15-year-old female volleyball player twisted her knee while planting her foot. She states she felt her knee give out. She had immediate swelling and was unable to continue participation. She denies hearing a pop. Physical examination reveals a large effusion with a range of motion from full extension to 80° flexion. She has marked tenderness along the medial retinaculum of her knee. She has no joint line tenderness. There is no pathologic laxity involving the collateral or cruciate ligaments. The most likely diagnosis is:
Options:
- Partial anterior cruciate ligament tear
- Posterior cruciate ligament tear
- Medial collateral ligament sprain
- Patellar subluxation
- Peripheral medial meniscal tear
Correct Answer: Patellar subluxation
Explanation:
Patellar subluxation is a common injury in athletes. It generally presents with a large effusion. Patients usually have a limited arc of motion but can usually obtain full extension. In addition to medial retinacular tenderness, patients will have apprehension to attempts at lateral displacement of the patella. Treatment is initially nonoperative, emphasizing quadriceps strengthening. Operative treatment is reserved for patients with continued instability despite appropriate rehabilitation.

 healing. Since this patient has failed nonoperative treatment, insertion of a reamed intramedullary nail would offer her the best chance of healing and earlier return to activity.
healing. Since this patient has failed nonoperative treatment, insertion of a reamed intramedullary nail would offer her the best chance of healing and earlier return to activity.