Full Question & Answer Text (for Search Engines)
Question 1:
Which of the following statements concerning Ehlers-Danlos syndrome (EDS) is true:
Options:
- EDS type III is the most severe form of the disease.
- EDS is primarily inherited as an autosomal dominant disorder.
- EDS type VII is characterized by dislocated hips and/or knees at birth.
- Demonstrating joint hyperlaxity or voluntary dislocation in EDS patients does not damage the joint.
- Knowing the subtype of the disease does not affect the overall management of the patient.
Correct Answer: EDS type VII is characterized by dislocated hips and/or knees at birth.
Explanation:
Ehlers-Danlos syndrome (EDS) types I, II, III, and VII are commonly seen by orthopedic surgeons. Type VII is characterized by congenital hip and knee dislocations. EDS type III is the mildest form of the disease; the main symptom of this type is hyperlaxity. EDS may be inherited via any of the Mendelian patterns. Children with EDS should be encouraged not to use their hyperlaxity as a â trickâ because of potential long-term joint damage that may occur. Knowing the subtype of the disease is often helpful in management and perioperative planning because than the surgeon may anticipate operative risks and potential complications.
Question 2:
Which subtype of Ehlers-Danlos syndrome (EDS) is caused by lysyl hydroxylase deficiency:
Options:
- EDS type I
- EDS type II
- EDS type III
- EDS type IV
- EDS type VII
Correct Answer: EDS type I
Explanation:
Many of the mutations responsible for the differing subtypes of Ehlers- Danlos syndrome (EDS) have not been identified (EDS types I, II, and III). Lysyl hydroxylase deficiency has been identified as the cause of type IV. A mutation in type I collagen has been identified as the cause of EDS VII.C orrect Answer: EDS type IV
Question 3:
The most common type of chronic inflammatory arthritis in childhood is:
Options:
- Pauciarticular juvenile rheumatoid arthritis
- Polyarticular juvenile rheumatoid arthritis
- Systemic juvenile rheumatoid arthritis
- Seronegative spondyloarthropathy
- Reactive arthropathy
Correct Answer: Pauciarticular juvenile rheumatoid arthritis
Explanation:
Forty percent to 60% of children afflicted with juvenile rheumatoid arthritis (JRA) have the pauciarticular subtype. Polyarticular JRA is the second most common type occurring in 30%-40%. Systemic onset JRA is the least common form and occurs in approximately 20% of children. Seronegative spondyloarthropathy is more rare in patients <20 years old. Polyarticular JRA comprises about 30%-40% of JRA. Systemic onset JRA is the least common form of JRA. Seronegative spondyolarthropathy is uncommon in childhood. Reactive arthropathy is not a chronic inflammation.
Question 4:
A 14-year-old left-handed boy suffers an avulsion of the medial epicondyle of the distal humerus when landing from a fall. The epicondyle is displaced 7 mm. His physical demands include swimming and lifting boxes. The recommended treatment for this injury is:
Options:
- Open reduction and internal fixation
- Manipulation and percutaneous fixation
- Percutaneous fixation in situ
- Splint for 1 week
- Excision of the fragment with reattachment of muscle to bone
Correct Answer: Splint for 1 week
Explanation:
Unless the fragment is entrapped or significant valgus loading is anticipated, nonoperative treatment is indicated. Range of motion should be started within 1 week. Open reduction is only indicated, if the epicondyle was entrapped in the joint, or if significant valgus loading was anticipated. The results of nonoperative treatment are just as good as any invasive treatment. Excision of the fragment is only indicated, if operative treatment is indicated, and the epicondyle is fragmented.
Question 5:
Which of the following statements is true about the medial humeral epicondyle:
Options:
- The medial humeral epicondyle is the first center to ossify in the distal humerus.
- The medial humeral epicondyle usually fuses to the distal humerus at age twelve.
- The medial humeral epicondyle is located anteromedially on the distal humerus.
- The medial humeral epicondyle is the origin of the wrist extensor muscles.
- The medial humeral epicondyle may ossify from several centers.
Correct Answer: The medial humeral epicondyle is the first center to ossify in the distal humerus.
Explanation:
The medial epicondyle may have several ossification centers. The medial epicondyle is the third center to ossify, beginning at age 4 to 6 years old. The medial epicondyle usually fuses near skeletal maturity, at approximately age 15. The medial epicondyle is located posteromedially. The medial epicondyle is the origin of the flexor-pronator muscles.
Question 6:
Which of the following statements is true regarding ankylosing spondylitis:
Options:
- Radiographic changes present early.
- Characteristic features make it easy to diagnose.
- It is a common inflammatory disorder affecting children < 8 years of age.
- It is an inflammation of ligament insertions associated with HLA-B27.
- Long-term prognosis is poor.
Correct Answer: It is an inflammation of ligament insertions associated with HLA-B27.
Explanation:
Ankylosing spondylitis is an inflammatory enthesopathy that rarely affects children. Diagnosis is often difficult because the features may be similar to pauciarticular juvenile rheumatoid arthritis. It typically affects males >8 years of age. It is associated with haplotype HLA-B27. The long-term prognosis in these children is generally good.
Question 7:
A 4-year-old child injures his elbow and presents with swelling and limitation of voluntary movement. The radiographs show no obvious fracture, but it does show a Baumann angle of 71° and an elevation of the posterior fat pad. You tell the parents that this most likely represents:
Options:
- A congenital anomaly with a valgus deformity of the elbow
- A medial epicondyle fracture
- A Salter I physeal separation
- An occult supracondylar fracture
- A variation of normal
Correct Answer: An occult supracondylar fracture
Explanation:
Occult supracondylar fracture was the most common diagnosis assigned after careful study of a clinical series of elevated pediatric posterior fat pads. The value for Baumann angle is normally 81° - 64°. Nothing in this description suggests a congenital anomaly. Medial epicondyle fractures are extremely rare before 9 years of age. Although a Salter I physeal separation is a possibility, it is a rare injury. With an elevation of the posterior fat pad, there is increasing recognition that a fracture exists.
Question 8:
A 6-year-old boy sustains a supracondylar fracture of the humerus. The 2 fragments are not completely displaced, but there is some overlap of the medial column and a gap on the lateral column of the distal humerus. Baumannâ s angle measures 85°-89º.The alignment on the lateral film shows no significant translation, but approximately 15° of increased extension. The recommended treatment is:
Options:
- Accept this and treat in a long arm cast
- Closed reduction with supination of the forearm and application of long arm cast
- Closed reduction with the elbow in extension to better monitor the angulation
- C losed reduction and percutaneous pin fixation
- Open reduction and medial and lateral plate fixation
Correct Answer: Closed reduction with supination of the forearm and application of long arm cast
Explanation:
Closed reduction should allow regain of alignment and percutaneous pin fixation will allow it to be maintained. The elbow is in 10°-15° of varus and this will be an objectionable appearance in the future. Supination will increase the varus. Extension will exacerbate the deformity seen on the lateral and will cause further loss of contact of the fracture fragments. Medial and lateral plate fixation is needed in adolescents and adults with intercondylar fractures to allow early range of movement but is excessive treatment for this fracture in young children.
Question 9:
A 6-year-old girl presents with a fracture of the radial neck that is angulated 25° compared to the other side. No other abnormalities are seen. The recommended treatment is:
Options:
- Sling and early range of motion
- Reduction using an intramedullary K-wire introduced from a retrograde approach (Metaizeau technique)
- Reduction using a percutaneously placed K-wire with intraosseous fixation
- Open reduction without internal fixation
- Open reduction and internal fixation
Correct Answer: Sling and early range of motion
Explanation:
Fractures with angulation <30° have an excellent chance of remodeling, and can be left as they are with early range of motion. Reduction using an intramedullary K-wire introduced from a retrograde approach (Metaizeau technique) is indicated mainly for fractures angulated >30°. Reduction using a percutaneously placed K-wire with intraosseous fixation, while effective, is not needed unless the fracture is angulated >30°. Open reduction and internal fixation are indicated only if the fracture is angulated >50° and does not reduce by one of the manipulative techniques.
Question 10:
A 7-year-old boy falls and suffers a Salter type IV fracture of the proximal radius. The size of the displaced fragment is 40% of the radial head, and it is translated distally by 2 mm. The optimum treatment is:
Options:
- Immobilization for 2 weeks with early range of motion
- Immobilization for 6 weeks with early range of motion
- Percutaneous fixation in situ to prevent further displacement
- Excision of the radial head fragment
- Open reduction, internal fixation
Correct Answer: Open reduction, internal fixation
Explanation:
Because the displacement is likely to be >2 mm, open reduction may lessen the risk of problems with growth and mobility. This is suggested by clinical series. The displacement is likely to be greater than the radiograph shows, and growth disturbance is likely. Range of motion at two weeks is too early. Percutaneous fixation in situ would still carry a risk of growth disturbance, because the displacement is likely to be more than the plain radiographs show due to the largely cartilaginous nature of the radial head. Excision of a fragment this large is likely to produce incongruity of the radio-capitellar joint.
Question 11:
A 12-year-old boy sustains a Salter type II fracture of the proximal humerus during a fall. The fracture has an apex angulation of 40° anteriorly and laterally. The neurovascular examination is normal. The recommended treatment is:
Options:
- Longitudinal traction in abduction followed by slowly bringing the arm into an abduction (airplane) splint
- Closed reduction and percutaneous pin fixation
- Open reduction and plate fixation
- Skeletal traction in abduction with an olecranon pin
- No formal reduction attempt, rather placement of the arm in a sling
Correct Answer: No formal reduction attempt, rather placement of the arm in a sling
Explanation:
Recommended treatment involves no formal reduction attempt, rather placement of the arm in a sling. This simple treatment is adequate for all patients with at least 2 years of growth remaining. This is due to the tendency to self-align, the remodeling potential, and the ability to tolerate some deformity in the region with no functional consequence. The abduction splint is cumbersome. It is not necessary because simpler means are effective due to the young age and remodeling potential. Closed reduction and pin fixation are not needed because adequate remodeling is expected. Any residual deformity is well tolerated in this region. The pins can sometimes cause significant soft tissue irritation in the bulky area of the shoulder. Plate fixation is not feasible because of the open physis. It is also not necessary because simpler means are available. Skeletal traction is not needed because the humerus will align itself better with time in a dependent position.
Question 12:
The most common cause of a pediatric pathologic fracture of the proximal humerus is:
Options:
- Osteochondroma
- Osteogenic sarcoma
- Unicameral bone cyst
- Codman tumor (chondroblastoma)
- Fibrous cortical defect
Correct Answer: Unicameral bone cyst
Explanation:
The most common cause of a pathologic fracture of the proximal humerus is unicameral bone cyst. This fluid-filled cyst expands and weakens the humerus, often causing a fracture as its first evidence of existence. Although the proximal humerus is one of the more common sites of their occurrence, osteochondromas do not significantly weaken the humerus. Osteogenic sarcoma is a relatively rare bone tumor, and it does not weaken the bone until it is at an advanced stage. Codman tumor (chondroblastoma) is classically described in the proximal humerus, it is rare and typically epiphyseal in location, and does not appreciably weaken the bone. Although fibrous cortical defects are common tumors, they rarely present in this way.
Question 13:
A 6-year-old boy has a painful elbow, with swelling over the region of the olecranon. Radiographs reveal a thin sliver of bone that is displaced 4 mm from the proximal border of the olecranon. Treatment should consist of:
Options:
- Closed treatment in a cast in 90° of flexion
- C losed treatment in a cast in extension
- Open excision of the osseous fragment
- Open reduction and tension band fixation
- No immobilization; early range of motion
Correct Answer: Open reduction and tension band fixation
Explanation:
Open reduction and tension band fixation is the best method to hold the proximal ulnar apophysis. The patient has a â sleeveâ fracture that should be reduced because it is attached to the olecranon apophysis. The osseous fragment is attached to the entire olecranon apophysis, which develops a secondary ossification center at age 9. With early range of motion, further displacement and/or nonunion may develop.
Question 14:
Which of the following statements is true about the radiographic development of the proximal ulna:
Options:
- A small sliver of a secondary ossification center is present at birth.
- A secondary ossification center appears at 5 years of age.
- A secondary ossification center appears at 7 years of age.
- A secondary ossification center appears at 9 years of age.
- There is no secondary ossification center for this region.
Correct Answer: A secondary ossification center appears at 5 years of age.
Explanation:
There is a secondary ossification center developing in children approximately 9 years of age. There is no ossification center in the proximal ulna until the child reaches 9 years old.
Question 15:
A 14-year-old boy sustains an intercondylar fracture of the distal humerus. There is a single fracture line into the joint between the capitellum and the trochlea. The medial column of the distal humerus is comminuted, but the lateral column is not. All fragments are highly displaced. Neurovascular status is normal. The recommended treatment is:
Options:
- Olecranon pin traction overhead for 2 weeks and long arm cast
- Closed reduction and long arm cast
- Closed reduction and pin fixation
- Open reduction and dual plate fixation through an anterior incision
- Open reduction and dual plate fixation through a posterior approach
Correct Answer: Open reduction and dual plate fixation through an anterior incision
Explanation:
A posterior approach (Bryan-Morrey or olecranon osteotomy) will facilitate anatomic reduction and rigid fixation sufficient for early range of motion. Prolonged traction and cast will result in an incomplete reduction and excessive stiffness. A cast alone will result in an incomplete reduction and excessive stiffness. Rigid fixation with plates, rather than pins, is required to maintain reduction of these fractures and allow early range of motion. An anterior approach will not allow adequate exposure of the distal humerus for articular fixation.
Question 16:
In treating which of the following elbow fractures is it most important to begin early range of motion:
Options:
- Salter I physeal fracture of distal humerus
- Intercondylar (T-condylar) fracture of distal humerus
- Supracondylar fracture of distal humerus
- Lateral condyle fracture
- Lateral epicondyle fracture
Correct Answer: Intercondylar (T-condylar) fracture of distal humerus
Explanation:
Intercondylar fractures have a significant risk of loss of motion because of the magnitude of injury, intra-articular extension, and older age of patient. Salter I physeal fractures typically occur in young children. They usually pose no difficulty with regaining motion after 4 to 6 weeks of immobilization. Supracondylar fractures usually are followed by regaining motion after healing despite immobilization of up to 6 weeks or more. Patients with this fracture usually regain their motion after healing. Because this is a nonarticular fracture, loss of motion is not a high risk.
Question 17:
A previously healthy 3-year-old girl presents with 3 weeks of painful torticollis and facial asymmetry. A birth history reveals a normal vaginal delivery with no perinatal complications. The girl has no history of esophagitis or gastrointestinal problems. Her mother reports that approximately 1 month ago, the young girl had an upper respiratory tract infection that has since resolved. The most likely diagnosis is:
Options:
- Muscular torticollis
- Os odontoideum
- Grisel syndrome
- Sandifer syndrome
- Pseudosubluxation of C 2 on C 3
Correct Answer: Grisel syndrome
Explanation:
Grisel syndrome is an abnormal rotation of the atlantoaxial joint that produces painful torticollis and often follows an upper respiratory tract infection. Muscular torticollis is unlikely in this patient because this condition is usually attributed to a difficult delivery, breech presentation, or some type of in utero positioning problem. Furthermore, muscular torticollis usually presents itself within the first 4-6 weeks and has no association with respiratory infections. Symptoms associated with os odontoideum consist of neck pain, paresthesia, transient paresis, or myelopathy. Patients with os odontoideum do not have torticollis. Sandifer syndrome is a painful torticollis and the abnormal trunk rotation is associated with gastroesophageal reflux disease. Pseudosubluxation does not produce painful torticollis.
Question 18:
A computerized tomography (C T) scan of the neck reveals an atlantoaxial rotatory displacement with 6 mm of anterior translation. The most likely associated anatomic defect is:
Options:
- Disruption of both the transverse ligament of C 1 and the alar ligaments
- Odontoid fracture
- Disruption of the anterior and posterior longitudinal ligaments
- Disruption of the ligamentum flavum between C 1 and C 2
- Ossiculum terminale
Correct Answer: Disruption of both the transverse ligament of C 1 and the alar ligaments
Explanation:
In order to have anterior displacement of C 1 on C 2 >5 mm, there must be disruption of both the transverse ligament of C 1 and the alar ligaments. Odontoid fracture does not disrupt the articulation between the dens and the atlas, therefore, there would be no abnormal diastasis between the atlas and the dens. The anterior and posterior longitudinal ligaments attach to the anterior and posterior aspects of the vertebral bodies respectively. Insufficiency does not affect the atlantoaxial articulation. Disruption of the ligamentum flavum alone is not thought to result in translation of C 1 on C 2. An ossiculum terminale is a persistent growth center at the tip of the odontoid, but is not indicative of any pathological condition.
Question 19:
A 14-year-old ice hockey player had a jersey pulled over his head in a brawl during a game. He finished the game without incident and denies any other traumatic event. The boy presents the following day with a stiff neck tilted to the right side and an inability to bring his head to a neutral position. On more careful physical examination, the boys head is tilted to the right 20°, rotated to the left 20°, and slightly flexed. Attempts at passive rotation to a neutral position produce pain. The exam is otherwise unremarkable. C omputerized tomography scans show atlantoaxial rotatory displacement with no anterior displacement of C 1 on C 2. Treatment should include:
Options:
- Urgent C 1 to C 2 fusion
- Use of a soft collar, exercises, and nonsteroidal anti-inflammatory drugs (NSAIDs)
- Head halter traction and NSAIDs
- Philadelphia collar, Minerva casting, and NSAIDs
- Occiput to C 2 fusion
Correct Answer: Use of a soft collar, exercises, and nonsteroidal anti-inflammatory drugs (NSAIDs)
Explanation:
A soft collar, exercises, and nonsteroidal anti-inflammatory drugs (NSAIDs) should be tried for 1 week if the diagnosis of atlantoaxial rotatory displacement is made within a week of its onset. The patientâ s progress must be followed closely. If NSAIDs and a collar do not work after 1 week, the patient should be hospitalized and head halter traction should be administered along with muscle relaxants. If head halter traction successfully reduces the deformity, the patient should be placed in a Philadelphia collar with Minerva casting for 6 weeks. If the patient has no neurologic findings and no anterior displacement, the condition is likely to resolve with conservative measures alone. If surgery becomes necessary, the occiput should not be included in surgical treatment of atlantoaxial rotatory displacement.
Question 20:
C ongenital pseudarthrosis of the clavicle occurs most commonly on which side:
Options:
- Bilateral
- Right
- Left
- The side more involved with fibrous dysplasia
- The side with the proximal focal femoral dysplasia
Correct Answer: Right
Explanation:
Ninety percent of cases are noted on the right side. Ten percent of cases are bilateral and have been associated with bilateral cervical ribs. Only a few cases of left-sided pseudarthrosis have been described and have been associated with dextrocardia. Only <5% of cases of congenital pseudarthrosis are on the left. Congenital pseudarthrosis is not related to fibrous dysplasia. Congenital pseudarthrosis is not related to proximal focal femoral dysplasia.
Question 21:
The most common structure to be injured in conjunction with an elbow dislocation is:
Options:
- The ulnar nerve
- The median nerve
- The radial nerve
- The brachial artery
- The biceps tendon
Correct Answer: The ulnar nerve
Explanation:
With an injury rate of approximately 6%, the ulnar nerve is the most common injured structure in an elbow dislocation. Median nerve injuries are rare with elbow dislocation. Such injuries may be due to nerve entrapment. If chronic, this may produce the Matev sign of a groove in the distal humerus. The radial nerve and biceps tendon are not commonly injured with an elbow dislocation. The brachial artery is rarely injured with an elbow dislocation.
Question 22:
A 4-year-old girl is brought in for examination by her mother because of a bump on the lateral side of her elbow. The girl is unable to extend her elbow. She falls as much as any child, but no particular injury to the elbow is recalled. Radiographs show a dislocated, enlarged radial head that is convex proximally. There is a proximal radioulnar synostosis. Recommended treatment includes:
Options:
- Radial head excision
- Open reduction of the radial head and annular ligament reconstruction
- Open reduction of the radial head and ulnar lengthening osteotomy
- Silastic radial head arthroplasty
- No treatment
Correct Answer: No treatment
Explanation:
This child has a congenital dislocation of the radial head, and no treatment is indicated unless the forearm is fixed in a position of extreme malrotation. Radial head excision should only be performed if there is pain and the child is skeletally mature. Silastic radial head arthroplasty has a significant risk of particulate synovitis.
Question 23:
A 6-year-old child falls and suffers a fracture of the elbow. The tenderness is mostly lateral. A fracture line may be seen separating a fragment of the humeral metaphysis and physis 3 mm from the lateral portion of the elbow, but the distal extension of the fracture cannot be visualized because of lack of ossification at this age. Treatment should consist of:
Options:
- No immobilization and early range of motion
- Application of a long arm cast for 4 weeks followed by early motion
- Application of a long arm cast for 8 weeks
- C losed reduction and percutaneous pin fixation
- Open reduction and plate fixation
Correct Answer: C losed reduction and percutaneous pin fixation
Explanation:
Closed reduction and pin fixation should be attempted for all lateral condyle fractures that are displaced more than 2 mm. If closed reduction is not successful, open reduction should be performed. This is a lateral condyle fracture; nonunion may result with no immobilization and early range of motion. With more than 2 mm of displacement, reduction and fixation should be carried out. Plate fixation is not feasible because of the presence of the physis. Rigid fixation beyond the use of pins is not required.
Question 24:
The following is the most common complication of lateral condyle fractures:
Options:
- Radial nerve palsy
- C ompartment syndrome
- Heterotopic ossification
- Nonunion
- Posterior interosseous nerve injury
Correct Answer: Nonunion
Explanation:
Nonunion occurs more commonly after lateral condyle fracture than following most childrenâ s fractures because the fracture line is predominantly intra-articular and not always adequately reduced and immobilized. Radial nerve injury, compartment syndrome, heterotopic ossification, and posterior interosseous nerve injury are uncommon with lateral condyle fractures.
Question 25:
The most common nerve injury in a Monteggia fracture and the type of Monteggia fracture with which it is most commonly found is:
Options:
- Ulnar nerve, type I
- Posterior interosseous nerve, type IV
- Posterior interosseous nerve, type III
- Median nerve, type I
- Median nerve, type III
Correct Answer: Posterior interosseous nerve, type IV
Explanation:
The posterior interosseous branch of the radial nerve is injured in 10%-20% of Monteggia fractures. Most cases occur at the time of fracture, but some occur later. Spontaneous resolution is the usual outcome. The ulnar nerve has only been reported injured in one case. The posterior interosseous nerve is the most commonly injured, at 10-20%, but type I and type III are the most common types affected. The median nerve is the second most commonly injured, after the radial nerve.
Question 26:
A 7-year-old girl is seen because of a persistent anterior dislocation of the radial head that occurred 2 months ago with an ulna fracture. The ulna has healed but has 25° of angulation. Her family would like to have this fixed to remove the prominence in the hope of preventing future joint degeneration. The recommended treatment is:
Options:
- Closed reduction of the radial head
- Open reduction and pin fixation of the radial head
- Open reduction and annular ligament reconstruction
- Open reduction, annular ligament reconstruction, and ulnar osteotomy
- Open reduction, radial shortening, and annular ligament reconstruction
Correct Answer: Open reduction and pin fixation of the radial head
Explanation:
The combination of open reduction, annular ligament reconstruction, and ulnar osteotomy should correct all of the components of the deformity. Closed reduction is not successful beyond 1-2 weeks after injury. Because of the 25° ulnar bow, recurrence is likely, and ulnar osteotomy is indicated. An ulnar osteotomy should be included to prevent recurrence.
Question 27:
A 6-year-old patient has an acute proximal ulnar fracture with an apex posteriorly, as well as a radial head dislocation. Treatment at this stage should consist of:
Options:
- Closed reduction and immobilization in supination and flexion more than 90° in a long arm cast
- Closed reduction and immobilization in extension in a long arm cast
- Closed reduction and intramedullary rod fixation of the ulna
- Open reduction of the radial head and plate fixation of the ulna
- Open reduction of the radial head and annular ligament reconstruction
Correct Answer: Closed reduction and immobilization in supination and flexion more than 90° in a long arm cast
Explanation:
Extension will reduce the dislocation and the fracture. This type II Monteggia proximal fracture is best immobilized in extension. An intramedullary rod is indicated only if closed treatment fails. Open reduction of the radial head and plate fixation of the ulna are indicated only if closed treatment fails. Annular ligament reconstruction is indicated only if the dislocation is unreduced for more than 1 to 2 weeks.
Question 28:
A 5-year-old patient sustains a fracture of the ulna with apex anteriorly, as well as an anterior dislocation of the radial head. The recommended treatment is:
Options:
- Closed reduction with elbow flexed at least 90° and somewhat supinated
- Closed reduction with the elbow in extension
- Closed reduction with the elbow flexed and the forearm in maximal pronation
- Closed reduction of the radial head and intramedullary rod of the ulna
- Open reduction of the radial head, annular ligament repair, and closed reduction of the ulna
Correct Answer: Closed reduction with elbow flexed at least 90° and somewhat supinated
Explanation:
Flexion to at least 90° helps redirect the radial head, as does partial supination. Extension of the elbow will increase the tendency to dislocate. Pronation of the forearm will increase the tendency to dislocate. An intramedullary rod is needed only if closed treatment fails. Open reduction is required only if closed treatment fails.
Question 29:
A 2-year-old boy fell 4 feet from a countertop and landed on his outstretched hand. There is circumferential swelling and tenderness. Radiographs show no fracture, but the posterior fat pad elbow is elevated and the radius and ulna are translated slightly laterally on the anteroposterior view, and posteriorly on the lateral view. The most likely diagnosis is:
Options:
- Undisplaced supracondylar fracture
- Transphyseal fracture of the distal humerus
- Lateral condyle fracture
- Traumatic elbow dislocation
- C ongenital elbow dislocation
Correct Answer: Transphyseal fracture of the distal humerus
Explanation:
The separation occurs through cartilage, so it is not visible as a fracture on plain films. However, the translation indicates a problem and elbow dislocation does not occur with any frequency at this age. An undisplaced supracondylar fracture would not produce translation of the radius and ulna. A lateral condyle fracture would not produce translation of the ulna. Traumatic dislocation is extremely uncommon in this age group. C ongenital elbow subluxation would not account for the swelling and tenderness. This is an extremely rare condition.
Question 30:
A physeal fracture-separation of the distal humerus is seen in an 18-month- old boy. When the parents ask about the prognosis after this injury, you tell them that the most common complication is:
Options:
- C ubitus varus
- Median nerve palsy
- Ulnar nerve injury
- Brachial artery injury
- Undergrowth of the humerus
Correct Answer: C ubitus varus
Explanation:
Cubitus varus occurred in seven out of twelve physeal fracture separations of the distal humerus in one series. This most likely occurred due to malalignment or avascular necrosis of the trochlea. Median nerve injury, ulnar nerve injury, and brachial artery injury are extremely uncommon after this injury because the surfaces of the metaphysis and the physis are relatively smooth in comparison to supracondylar fractures. Also, these injuries are relatively low-energy. Growth plate damage causing undergrowth is rare after this fracture.
Question 31:
Slide 1 A 12-year-old boy presents to the emergency department after being struck by a car (slide 1). His only complaint at the time of presentation is right ankle pain. After obtaining an excellent reduction and casting the leg, the risks of a future growth disturbance through the involved physis must be discussed with the family. What are the chances of a significant growth disturbance of his leg:
Options:
- < 1%
- 2% to 3%
- 10% to 15%
- 45% to 55%
- 80% to 90%
Correct Answer: < 1%
Explanation:
This is a Salter-Harris type II fracture of the distal tibia. The distal tibia is at moderate risk for growth arrest after physeal injury. The average incidence of growth disturbance is 15% for all physeal injuries in this area. The marked displacement and mechanism of injury in this patient increase the risk of permanent physeal damage. The patientâ s age and remaining growth also increase the likelihood of a growth arrest causing a significant deformity or leg length discrepancy.C orrect Answer: 10% to 15%
Question 32:
Three years after a Salter-Harris type I physeal fracture of the right distal femur, a 12-year-old boy presents with complaints of knee pain and a limp. On examination, the boy has a valgus alignment of his right knee and a 2-cm leg length discrepancy with the right leg shorter than the left. Plain radiographs and a scanogram showed 30% growth plate closure with a femoral-tibial angle of 12° of valgus and 2.5 cm of shortening of the right femur. What is the best treatment:
Options:
- Lengthening procedure on the right leg
- Varus osteotomy of the right femur and bilateral distal femur epiphyseodesis
- Physeal bar resection of the right distal femur and opening wedge lateral osteotomy
- Right medial hemiepiphyseal stapling
- C ompletion of distal femoral epiphyseal closure
Correct Answer: Physeal bar resection of the right distal femur and opening wedge lateral osteotomy
Explanation:
The bar resection has a reasonable chance of success. The angulation can be corrected by the osteotomy and the length would be partially corrected. Correction of the length (2 cm) is less important than prevention of future angulation and shortening. At 12 years old, if varus osteotomy of the right femur and bilateral distal femur epiphyseodesis were performed, the patient would be sacrificing 6 cm of leg length which most patients would consider unacceptable. Right medial hemiepiphyseal stapling and completion of distal femoral epiphyseal closure would neither produce significant length equalization nor correct the angulation.
Question 33:
Two years after a Salter-Harris type II fracture of the right distal femur, a 12-year-old girl presents to the clinic with knee pain. On examination, she is found to have a valgus alignment of the right knee and a 3-cm leg length discrepancy with the right leg shorter than the left leg. The scanogram confirms 3 cm of shortening in the right femur. The next step in the management of this patient is:
Options:
- Obtain a magnetic resonance image of the right distal femoral physis
- Obtain a computed tomography scan of the right distal femoral physis
- Obtain a bone scan
- Obtain a single photon emission computed tomography scan
- Patients return in 9 months for a repeat scanogram
Correct Answer: Obtain a magnetic resonance image of the right distal femoral physis
Explanation:
A magnetic resonance image of the right distal femoral physis provides the best detail of the physis if the correct region and sequences are ordered. A computed tomography scan is not the preferred method to allow visualization of the physis. A bone scan or photon emission computed tomography scan will not highlight a bar of the physis. Waiting 9 months would allow for worsening of the deformity.
Question 34:
The mutations underlying Stickler syndrome have been identified in which of the following molecules:
Options:
- Type I collagen
- Type II collagen
- Fibrillin
- Sulfate transport protein
- Fibroblast growth factor receptor protein
Correct Answer: Type II collagen
Explanation:
Type II collagen is abnormal in the classic form of Stickler syndrome, but in a few patients, type XI collagen has been found to be the causative mutation. Type 1 collagen is predominant in bone and is abnormal in osteogenesis imperfecta, for example. Stickler syndrome is characterized by a defect in type II collagen. Fibrillin is abnormal in Marfan syndrome, but in Stickler syndrome, the causative abnormalities have been found in type II collagen. Sulfate transport protein has been found abnormal in diastrophic dysplasia Fibroblast growth factor proteins are abnormal in achondroplasia and hypochondroplasia, but the basic defect in Stickler syndrome is type II collagen.
Question 35:
A 15-month-old child has bowing of the legs. Examination reveals a 3 cm distance between the femoral condyles and a thighfoot angle of 20° internal. Radiographs reveal 10° varus of the mechanical axis, no evidence of skeletal dysplasia, and a metaphyseal-diaphyseal angle of 9° on each side. Recommended treatment is:
Options:
- Full-time bracing with a knee-ankle-foot orthosis
- Bilateral oblique osteotomies of the proximal tibia
- Bilateral hemiepiphyseal stapling of the lateral tibia
- Re-examination in 6 months
- Reassurance to parents that the legs will develop normally; no further follow-up
Correct Answer: Re-examination in 6 months
Explanation:
Although a diagnosis of Blount disease cannot be made at this time, the disease cannot be ruled out. The patient should be rechecked in 6 months by an experienced examiner. However, if the parents are reliable, they can be told that they do not need to return if the childâ s legs develop a normal shape in 6 months. The diagnosis of pathologic varus cannot be made; therefore, no treatment is indicated. The findings described are not outside of normal limits; surgery is not necessary. No pathologic diagnosis has yet been made. In addition, stapling is not an indicated form of treatment for such a young child. Although a pathologic condition has not been diagnosed, one cannot be ruled out either at this stage.
Question 36:
An 11-year-old girl is observed for legs that have been bowed for the past 5 years. She has a mechanical axis that is in 26° of varus, a medial tibial plateau slope of 8°, a tibial joint angle of 15° varus, and a femoral joint angle of 10° varus. Her physis appears open. Recommended treatment is:
Options:
- Tibial valgus osteotomy
- Femoral valgus osteotomy
- Tibial and femoral valgus osteotomy
- Medial tibial plateau elevation
- Brace treatment
Correct Answer: Femoral valgus osteotomy
Explanation:
Both a tibial and a femoral valgus osteotomy are necessary to correct significant deformities in these areas. A tibial valgus osteotomy is necessary but not sufficient. The femoral joint angle is off by 13° from the normal angle. A femoral valgus osteotomy is necessary but not sufficient. The tibial joint angle is off by 15° of varus. A tibial plateau elevation is not necessary for this mild degree of plateau depression. Brace treatment is not recommended for patients older than 3 years of age.
Question 37:
The radiographic feature that is most characteristic of infantile Blount disease is:
Options:
- Widening and irregularity of the entire proximal tibial physis
- Poor bone mineralization
- Focal bowing of the distal medial femur
- Focal bowing of the proximal medial tibia
- External tibial torsion
Correct Answer: Focal bowing of the distal medial femur
Explanation:
Bowing is focally located at the proximal medial tibia in infantile Blount disease. The physis may be widened medially, but it is normal laterally. Bone mineralization is not impaired in Blount disease. Bowing is focally located at the proximal tibia, not the distal femur. Blount disease is associated with internal, not external, tibial torsion.
Question 38:
Marfan syndrome is now recognized as a defect in the following molecule:
Options:
- Fibrillin-1
- Type I collagen
- Type II collagen
- Sulfate transport protein
- Type IX collagen
Correct Answer: Fibrillin-1
Explanation:
Marfan syndrome is due to an abnormality in fibrillin-1, a component of elastic connective tissue. Type I collagen is most commonly abnormal in osteogenesis imperfecta. Type I collagen is normal in Marfan syndrome. Type II collagen is a homotrimer (encoded by a single gene) and is mainly located in cartilaginous tissues. Type II collagen is abnormal in spondyloepiphyseal dysplasia congenita and Stickler syndrome. The sulfate transport protein is important for cartilage formation. The sulfate transport protein is impaired in diastrophic dysplasia. Type IX collagen is also found in cartilage. Type IX collagen is abnormal in some forms of multiple epiphyseal dysplasia.
Question 39:
A 15-year-old basketball player has mild scoliosis, pes planus, pectus carinatum, and long slender fingers. In order to help determine if he has Marfan syndrome and should be allowed to continue playing basketball, it is most useful to order a:
Options:
- C ardiac echo
- Magnetic resonance image of the lumbosacral spine
- Slit lamp examination
- C hest radiograph
- Dermal fibroblast assay
Correct Answer: C ardiac echo
Explanation:
A cardiac echo will give information about enlargement of the ascending aorta, as well as the valves. This is the most important information for activity recommendations and patient prognosis. A magnetic resonance image (MRI) of the lumbosacral spine will either rule in or out dural ectasia, but a MRI has no clinical importance for activity recommendations. A slit lamp examination is not as important as a cardiac echo in making sport recommendations. A chest radiograph may be helpful, if the patient is suspected of having a pneumothorax. A dermal fibroblast assay is useful in assessing collagen, such as in osteogenesis imperfecta, but it is not helpful in diagnosing Marfan syndrome.
Question 40:
The following skeletal feature helps to establish a diagnostic level of major skeletal involvement in Marfan syndrome:
Options:
- Hyperextensible knees
- Atlantoaxial subluxation
- Standing height over 2 m
- Increased thoracic kyphosis
- Pectus carinatum
Correct Answer: Pectus carinatum
Explanation:
Pectus carinatum has a high diagnostic value for Marfan syndrome. Hyperextension of the knees is not common in patients with Marfan syndrome. This skeletal feature is seen in many other conditions; therefore, it has low diagnostic specificity. Atlantoaxial subluxation is rare in Marfan syndrome, but is common in some of the skeletal dysplasias. Although patients with Marfan syndrome are generally tall, height is too nonspecific to be a helpful diagnostic criterion. Kyphosis is not a skeletal diagnostic criterion.
Question 41:
A 12-year-old girl has a scoliosis of 36° from T2-T7 and 15° from T7- L1. She is premenarchal. The following treatment is recommended:
Options:
- C harleston bending brace
- Boston overlap brace
- Milwaukee brace
- Lateral electrical spinal stimulation
- Posterior spinal fusion
Correct Answer: Milwaukee brace
Explanation:
The Milwaukee brace offers the best chance of controlling this curve. Charleston bending braces are not effective for curves larger than 35°. Boston overlap braces are not effective for curves with an apex above T8. Lateral electrical spinal stimulation has been proven ineffective for scoliosis. This curve is not large enough to pose a recommend fusion.
Question 42:
All of these findings are features of patients with Scheuermann kyphosis, except:
Options:
- Vertebral wedging
- Endplate irregularity
- Schmorl nodes
- Truncal obesity
- Back pain
Correct Answer: Truncal obesity
Explanation:
Obesity is not any more common in patients with Scheuermann kyphosis than in the general population. Vertebral wedging is a common feature of Scheuermann kyphosis. Endplate irregularity is a common feature of Scheuermann kyphosis. Schmorl nodes are a manifestation of the disordered behavior of the vertebral endplates under load. Back pain is common in Scheuermann kyphosis.
Question 43:
An 18-year-old man is seen in the office because of back pain in the thoracic region. He has a kyphosis of 65°, a slight wedging in the midthoracic spine, and a Risser sign of 4. Recommended treatment includes:
Options:
- A program of strengthening and stretching exercises
- A Milwaukee brace
- A Boston brace
- A posterior spinal fusion
- An anterior and posterior spinal fusion
Correct Answer: A program of strengthening and stretching exercises
Explanation:
Exercises must be the first treatment for this patient because he is too mature for brace treatment. Brace treatment is not indicated for someone of this skeletal maturity. Surgery is not indicated unless the patient fails conservative treatment.
Question 44:
Prior to treatment, this pathologic finding characterizes clubfoot:
Options:
- The talar head and neck are deviated medially.
- The dome of the talus is flattened.
- The navicular is positioned more laterally than normal.
- The foot has a rocker deformity.
- The tendoachilles inserts in a more lateral position than normal.
Correct Answer: The talar head and neck are deviated medially.
Explanation:
The talar head and neck are deviated medially. This deformity cannot be corrected surgically but may improve with growth. The dome of the talus is not originally flattened, but it may become this way after repeated manipulation. The navicular is positioned more medially than normal and may touch the medial malleolus. The foot has either a normal arch or a cavus deformity (the opposite of a rocker bottom). The rocker bottom foot may develop as a result of over-vigorous manipulation of a clubfoot against a tight heelcord. The tendoachilles inserts are more medially positioned than normal on the calcaneus.
Question 45:
In the surgical correction of a clubfoot, the following clinical or radiographic finding indicates that a child should have a plantar release:
Options:
- Anterior extrusion of the talus
- Inferior subluxation of the calcaneocuboid joint
- Medial subluxation of the calcaneocuboid joint
- Plantarflexion of the first ray
- Lack of ability to dorsiflex the ankle
Correct Answer: Plantarflexion of the first ray
Explanation:
Plantarflexion of the first ray, especially if the first ray is not colinear with the talus on the lateral radiograph, should serve as an indication for a plantar release. Anterior extrusion of the talus is common because of the tightness of the Achilles tendon and the posterior capsule. Inferior subluxation of the calcaneocuboid joint is not a feature of clubfoot. Medial subluxation of the calcaneocuboid joint, in combination with the clinical appearance of a curved lateral border of the foot, should serve as an indication for a lateral release, not a plantar release. Inability to dorsiflex the ankle is an indication for a posterior release.
Question 46:
Hip subluxation is most likely to occur in patients with this type of cerebral palsy:
Options:
- Athetoid
- Diplegic
- Hemiplegic
- Total involvement
- Monoplegic
Correct Answer: Total involvement
Explanation:
Patients with total involvement have the highest degree of axial muscle imbalance; therefore, they have the highest risk of hip subluxation (greater than 50%). Hip dysplasia is uncommon in athetoid cerebral palsy (CP). Diplegic C P has the second highest incidence of neuromuscular hip dysplasia, but total involvement has the highest rate. Hip subluxation is not common in hemiplegic CP. Monoplegia is a rare form of CP with a low rate of subluxation.
Question 47:
A 13-year-old boy sustains a Salter II fracture of the proximal humeral epiphysis. On radiograph, there is a 40° varus angulation and a 30° apex anterior angulation. Recommended treatment includes:
Options:
- Closed reduction and abduction cast
- Closed reduction and sling
- Closed reduction and percutaneous pin fixation
- Open reduction and percutaneous pin fixation
- Application of a sling and swathe
Correct Answer: Application of a sling and swathe
Explanation:
Spontaneous partial reduction will occur when the patient becomes upright, and there is good remodeling potential due to growth. Closed reduction and abduction cast is not necessary because of the patientâ s age, remodeling potential, and range of motion available in the joint. A formal attempt at closed reduction is not necessary because there is no way of holding it without internal fixation. This process will occur naturally to a large degree when the patient becomes upright. Open reduction and percutaneous pin fixation poses a risk of pin tract infection because of the large amount of muscle traversed. This procedure is not necessary because of the good results with conservative treatment.
Question 48:
A 12-year-old girl sustains a closed type III Monteggia fracture. One week after closed reduction, the radial head resubluxates and the ulna bows. The next step of treatment is:
Options:
- Repeat closed reduction and a long arm cast
- Reconstruct the annular ligament using a strip of triceps fascia
- Reduce and internally fix the ulna and close-reduce the radial head
- Reduce and internally fix the ulna and open-reduce the radial head
- Reduce and pin the radial head
Correct Answer: Reduce and internally fix the ulna and close-reduce the radial head
Explanation:
Once the ulna is predictably reduced, the radial head has a good chance of staying reduced. Repeat closed reduction and a long arm cast has a significant chance of redisplacement. If further time passes, radial head reduction will be difficult. Annular ligament reconstruction is only indicated if there is late subluxation (after several weeks) that does not reduce with closed means. Once the ulna is realigned and fixed, closed reduction of the radius must be tried next. Pinning of the radial head should be a last resort because of the risk of breakage and stiffness.
Question 49:
The following parameter is the most useful in predicting the need for surgical correction of developmental coxa vara:
Options:
- The range of active abduction
- The epiphyseal extrusion index
- The acetabular index
- The Hilgenreiner-epiphyseal angle
- Presence of a Trendelenburg gait
Correct Answer: The Hilgenreiner-epiphyseal angle
Explanation:
The Hilgenreiner-epiphyseal angle is a measure of the shear stress on the femoral neck. A value greater than 60° is an indication for surgery. The range of abduction does not directly reflect the mechanical stresses on the femoral neck that may need correction. The epiphyseal extrusion index is a parameter used in Perthes disease. The acetabular index is used in developmental hip dysplasia. It is usually essentially within normal limits, even in severe coxa vara.
Question 50:
A 7-month-old girl is newly seen for a dislocation of the left hip. The newborn exam was unremarkable; there was no history of trauma or evidence of spasticity. Recommended treatment includes:
Options:
- Exam, arthrogram and attempted closed reduction under anesthesia to guide treatment
- Pavlik harness
- Open reduction through a medial approach
- Open reduction through a lateral approach
- A Salter osteotomy
Correct Answer: Exam, arthrogram and attempted closed reduction under anesthesia to guide treatment
Explanation:
An exam under anesthesia and arthrogram should be performed. C losed reduction must be performed if the hip reduces with a medial dye pool less than 4 mm and a safe zone greater than 20°. The Pavlik harness is not strong enough to hold an infant older than 4 to 6 months. Open reduction is reserved for hips that do not reduce by closed means. A Salter osteotomy is only indicated if the hip is still unstable after an open reduction.
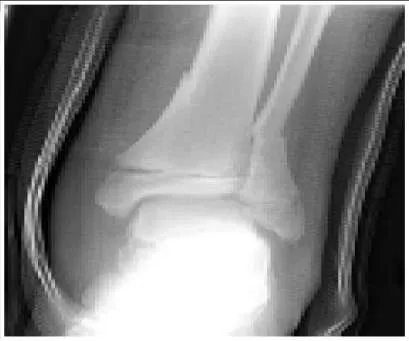
 This is a Salter-Harris type II fracture of the distal tibia. The distal tibia is at moderate risk for growth arrest after physeal injury. The average incidence of growth disturbance is 15% for all physeal injuries in this area. The marked displacement and mechanism of injury in this patient increase the risk of permanent physeal damage. The patientâ s age and remaining growth also increase the likelihood of a growth arrest causing a significant deformity or leg length discrepancy.C orrect Answer: 10% to 15%
This is a Salter-Harris type II fracture of the distal tibia. The distal tibia is at moderate risk for growth arrest after physeal injury. The average incidence of growth disturbance is 15% for all physeal injuries in this area. The marked displacement and mechanism of injury in this patient increase the risk of permanent physeal damage. The patientâ s age and remaining growth also increase the likelihood of a growth arrest causing a significant deformity or leg length discrepancy.C orrect Answer: 10% to 15%