Full Question & Answer Text (for Search Engines)
Question 1:
Immobilization as a postoperative therapy for flexor tendon repair is recommended for:
Options:
- Lacerations that involve both the flexor digitorum superficialis tendon and the flexor digitorum profundus tendon
- 2-strand tendon repairs
- C hildren
- Associated pulley rupture
- Flexor tendon laceration in the thumb
Correct Answer: C hildren
Explanation:
As children have difficulties in following the detailed flexor tendon rehabilitation program that is recommended for adults after flexor tendon repair, it is advisable to completely immobilize them to protect the repair and avoid inadvertent rupture.
Question 2:
Optimization of early active motion protocols for flexor tendon rehabilitation includes:
Options:
- Multi-strand repair
- Splinting the digit in extension
- Using passive flexion of the finger to gain flexibility
- Therapist hyperextension of the finger
- Ultrasound as an adjunct
Correct Answer: Multi-strand repair
Explanation:
The use of 6- and 8-strand repair techniques allow the flexor tendon repair to withstand the force applied by early active motion protocols. The addition of epitendinous tendon repair also strengthens the repair.
Question 3:
The splint for early active motion flexor tendon rehabilitation protocols includes:
Options:
- A wrist flexion piece
- A dynamic extension outrigger
- A yoke over the affected finger
- A hinge at the wrist to allow a tenodesis effect
- None of the above
Correct Answer: A hinge at the wrist to allow a tenodesis effect
Explanation:
A hinge at the wrist, which provides a tenodesis effect, allows the patient to passively extend the wrist and flex the fingers in preparation for gentle muscle contraction of the fingers.
Question 4:
A 13-year-old boy tears his anterior cruciate ligament (ACL) while playing flag football. What is the preferred graft material for his ACL reconstruction:
Options:
- Bone-patellar tendon-bone autograft
- Quadriceps tendon autograft
- Four-strand hamstring tendon autograft
- Four-strand hamstring tendon allograft
- Achilles tendon allograft
Correct Answer: Four-strand hamstring tendon autograft
Explanation:
Due to the patients age, autograft is the preferred option. Also, due to the patientâ s age, his growth plates are open and the surgeon is prohibited from using a graft with a bone construct due to the possible damage to the growth plate.
Question 5:
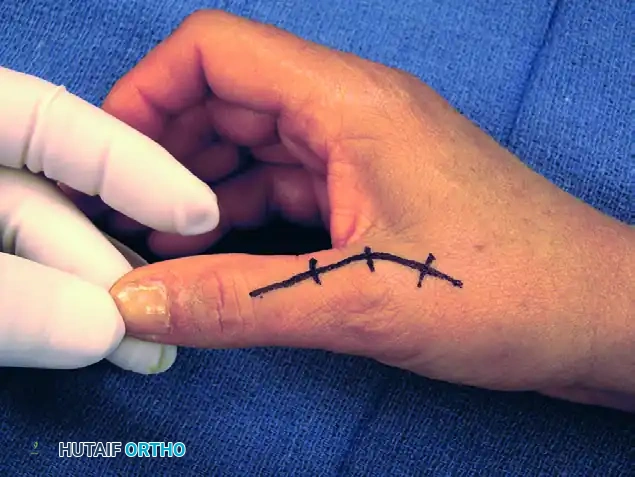
What deformity can develop in a mistreated volar PIP joint dislocation?
Options:
- Swan neck deformity
- Extensor lag
- Boutonniere deformity
- Flexion contracture
- Hyperextension deformity
Correct Answer: Boutonniere deformity
Explanation:
With volar PIP joint dislocations, there is almost always a disruption of the central slip of the extensor tendon. Because the central slip is involved, the PIP joint will hold a flexed position, and the lateral bands will fall volar to the axis of rotation of the PIP joint. The lateral bands will then exacerbate the flexion at the PIP joint, and due to their pull on the terminal tendon at the insertion on the distal phalanx, the DIP joint will hyperextend. This results in a boutonniere deformity.
Question 6:
What percentage of the articular surface must be involved in a dorsal PIP joint fracture dislocation for disruption of the collateral ligaments to occur?
Options:
Correct Answer: 40%
Explanation:
The percentage of articular surface involved differentiates a stable dorsal PIP joint fracture dislocation from an unstable one. It is believed that when the involved fracture fragment is less than 40% of the articular surface, the insertion site of the collateral ligaments is not disrupted and the joint is stable. If more than 40% of the articular surface is fractured, then the insertion of the collateral ligaments is involved and the joint will subsequently be unstable.
Question 7:
Which structures are disrupted in a lateral PIP joint dislocation?
Options:
- Volar plate by itself
- Volar plate and both collateral ligaments
- Volar plate, both collateral ligaments and central slip
- Volar plate and one collateral ligament
- Volar plate and lateral bands
Correct Answer: Volar plate by itself
Explanation:
When a lateral PIP joint dislocation occurs, failure probably begins with disruption of the collateral ligament either from its origin on the head of the proximal phalanx or its insertion on the base of the middle phalanx. The injury then proceeds through the accessory collateral ligaments and terminates with disruption of the insertion of the volar plate on the middle phalangeal base.
Question 8:
A 22-year old right-hand dominant male college student consumes a large amount of alcohol and falls asleep for eleven hours with his right arm over a chair. When he awakens, he is unable to feel the dorsum of his hand and cannot extend his elbow, wrist, or the metacarpalphalangeal joints of his affected arm. Initial management should consist of
Options:
- Upper Extremity Angiography
- Observation
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
- Electromyography
- Emergent Nerve Exploration, with repair if necessary
Correct Answer: Observation
Explanation:
Saturday night palsy is the term used for external compression of the radial nerve, and commonly occurs following the clinical scenario described above. The accepted treatment is observation, as Sunderland et al, described complete relief in all seven patients with Saturday night palsy after a period of observation without any adjunctive treatments. Although NSAIDs can be used if pain is a symptom or there is significant edema, these are not necessarily needed. Electromyography may be indicated if there is no improvement in symptoms after a three to six month period of observation. Emergent nerve exploration is indicated only for open fractures with a known radial nerve injury. There is no role for angiography in treatment of Saturday night palsy.
Question 9:
Flumazenil can be administered to reverse the effects of which of the following drugs:
Options:
- Propofol
- Fentanyl
- Midazolam
- Ketamine
- Methohexital
Correct Answer: Midazolam
Explanation:
Midazolam is a benzodiazepine. Flumazenil is the only commercially available benzodiazepine antagonist. The recommended dose is 0.01 mg/kg every minute until reversed to a maximum dose of 1 mg. Fentanyl is an opioid and is reversible with naloxone. Flumazenil is a benzodiazepine antagonist and has no effects on the effects of opioids. Propofol, ketamine, and methohexital have no known antagonists.
Question 10:
A 7-year-old boy fell off the jungle gym and landed on his outstretched right arm sustaining a forearm fracture in both bones. The fracture requires reduction. He was given a combination of fentanyl and midazolam for sedation. At his current level of sedation, he is protecting his own airway. His oxygen saturation has dropped slightly to 92% but is stable. He does not display any awareness or discomfort when the fracture is being manipulated. How would you define his current level of sedation:
Options:
- Analgesia
- C onscious sedation
- Deep sedation
- General anesthesia
- Dissociative amnesia
Correct Answer: Deep sedation
Explanation:
Deep sedation is the level where most fracture reductions are performed. Patients who are deeply sedated do not respond to verbal or noxious stimuli; they may display both a decreased ability to protect their airway and decreased respiratory drive. Analgesia is defined as affecting the sensation of pain, however, there is no change in overall awareness. Conscious sedation is defined as a lessening of awareness, with maintenance of protective reflexes. Patients will respond appropriately to commands and awaken to verbal stimuli. Patients do not respond to commands or noxious stimuli. With general anesthesia, patients will not respond to verbal or noxious stimuli. Additionally, they lose all of their respiratory drive and ability to protect their airway.
Question 11:
A 14-year-old girl with a history of multiple food allergies and severe asthma was involved in a motor vehicle accident and sustained an isolated right femur fracture. Which of the following medications is the best choice to control her pain:
Options:
- Ketamine
- Morphine
- Methohexital
- Meperidine
- Midazolam
Correct Answer: Meperidine
Explanation:
The goal in this patient is to provide safe, effective, and long-acting analgesia. Meperidine is recommended in this circumstance. It is an opioid that provides intermediate and long-term analgesia. Additionally, it does not cause the associated histamine release and bronchospasm that can occur in patients with asthma and atopia. Ketamine would provide short-term analgesia, but would also alter the level of consciousness. Morphine is well known for precipitating bronchospasm in patients with atopia and asthma. Therefore, it would not be the best choice in the scenario presented. Methohexital (a barbiturate) and midazolam (a benzodiazepine) both cause decreased awareness and have no analgesic properties.
Question 12:
Which of the following choices is the best for sedating an otherwise healthy child for a fracture reduction:
Options:
- Morphine, diazepam
- Meperidine, midazolam
- Fentanyl, diazepam
- Demerol, phenergan, and thorazine
- Fentanyl, midazolam
Correct Answer: Fentanyl, midazolam
Explanation:
The combination of fentanyl and midazolam is the closest we have to an ideal drug combination for conscious sedation. Both drugs have commercially available antagonists. Fentanyl and midazolam are both quick- onset and short-duration drugs. When using these two drugs together, there is a significant risk of respiratory depression. It is important to monitor patients closely.
Question 13:
A 3-year-old child presents with an obvious right lower extremity abnormality. The left lower extremity has normal alignment and joint function. The right lower extremity displays a severely short thigh with a flexed hip. The right foot and leg are also abnormal. Radiographs reveal a right proximal femur with no femoral head or neck, as well as acetabular dysplasia. There is also fibular hemimelia and two missing lateral rays of the foot. The parents want treatment to preserve the function of the normal leg. The most appropriate treatment is:
Options:
- Observation
- Right Syme's amputation with knee fusion and prosthetic fitting
- Van Nes rotation-plasty
- Femoral lengthening
- Equinus prosthesis
Correct Answer: Right Syme's amputation with knee fusion and prosthetic fitting
Explanation:
According to the Aitken classification, the patient has a type C proximal femoral focal deficiency (PFFD). In addition to a severe leg length discrepancy, a dysfunctional foot and ankle are also present. The patient would be best suited with an operative procedure to allow the development of ambulatory skills. The Syme's amputation with knee fusion is the standard procedure for severe PFFD and allows the patient to become proficient in the use of a prosthesis at an early age. In a child this young, a rotation-plasty may not be the best option due to a propensity to de-rotate and the weakness of the underdeveloped right ankle. For severe PFFD with unstable or dysplastic joints, lengthening is not the best option. If the leg length discrepancy were predicted to be <20 cm and a hip joint were present, then lengthening would be a better choice. If the child had a mild leg length discrepancy and was a candidate for lengthening, then an equinus prosthesis would be a reasonable choice until appropriate age for lengthening.
Question 14:
The most common associated abnormality with proximal femoral focal deficiency (PFFD) is:
Options:
- Tibial hemimelia
- Fibular hemimelia
- Absent radius
- Congenital scoliosis
- Cardiac defects
Correct Answer: Fibular hemimelia
Explanation:
Up to 45% of proximal femoral focal deficiency (PFFD) cases have coexisting fibular hemimelia. Tibial hemimelia may also have associated abnormalities of the distal femoral physis leading to a varus knee, but PFFD is more common. Absent radius is typically associated with thrombocytopenia agenesis radius (TAR) syndrome. Congenital scoliosis and cardiac defects are not commonly reported with PFFD.
Question 15:
Osteogenesis imperfecta (OI) is caused by defects in:
Options:
- Calcitonin
- Type I collagen
- Type II collagen
- Type X collagen
- Osteoclasts
Correct Answer: Type I collagen
Explanation:
Both quantitative and qualitative defects in type I collagen lead to the various types of osteogenesis imperfecta (OI). Several hundred different collagen I mutations have been found in patients with OI. The less severe forms of OI are caused by mutations in which the defective gene product is not incorporated into collagen, so that formation of cells using the unimpaired strands can continue.
Question 16:
Genetic transmission of osteogenesis imperfecta (OI) is best described as:
Options:
- Autosomal dominant
- Autosomal recessive
- Sex-linked dominant
- Autosomal dominant and autosomal recessive
- Not genetically transmitted
Correct Answer: Autosomal dominant
Explanation:
Depending on the particular mutation involved, osteogenesis imperfecta can be either autosomal dominant or autosomal recessive. Osteogenesis imperfecta occurs because of a defect in type I collagen. The genes for type I collagen are found on chromosomes 7 and 17, and are therefore not sex- linked.
Question 17:
The most common neurologic complications of osteogenesis imperfecta (OI) is:
Options:
- Intracranial hemorrhage
- Subdural hematoma
- Brainstem compression
- Mental retardation
- Herniated nucleus pulposes
Correct Answer: Brainstem compression
Explanation:
Basilar impression with brainstem compression is a neurologic sequela of the deforming types of osteogenesis imperfecta (OI). It can be identified by noting that the tip of the dens projects 7 mm or more above McGregor's line on plain film.
Question 18:
Criteria for diagnosis of neurofibromatosis 1 (NF1) include all the signs below except:
Options:
- Cafa-au-lait spots
- Lisch nodules
- Axillary or inguinal freckling
- Neurologic deficit
- A distinctive osseous lesion
Correct Answer: Neurologic deficit
Explanation:
While neurologic deficit may be associated with some of the spinal deformities in neurofibromatosis 1 (NF1), it does not constitute one of the diagnostic criteria. The diagnostic criteria for NF1 were established by The C onsensus Development Conference on Neurofibromatosis at the National Institutes of Health in 1987: Six or more cafa-au-lait spots, at least 15 mm in diameter in adults and 5 mm in children. Two or more neurofibromas of any type or one plexiform neurofibroma. Freckling in the axillae or inguinal regions (Crowe sign). Two or more iris hamartomas (Lisch nodules). A distinctive osseous lesion, such as sphenoid dysplasia or thinning of long bone cortex, with or without pseudarthrosis. A first-degree relative with NF1 by the above criteria.
Question 19:
The most common osseous abnormality in neurofibromatosis 1 (NF1) is:
Options:
- Congenital tibial dysplasia
- Scoliosis
- Valgus deformity of the ankle
- Macrodactyly
- Dysplasia of posterior cranial fossa
Correct Answer: Scoliosis
Explanation:
Of the many orthopedic manifestations of neurofibromatosis 1 (NF1), including kyphoscoliosis, lordoscoliosis, spondylolisthesis, congenital tibial dysplasia, segmental hypertrophy, cystic bone lesions, and subperiostial bone proliferation, scoliosis is the most common.
Question 20:
The origin of "dumbbell lesions" found in radiographs of patients with neurofibromatosis 1 (NF1) is:
Options:
- Flattening of the intervertebral disk with enlargement on the lateral borders
- Thinning of the midshaft of the tibia giving this bone the appearance of a dumbbell
- Neurofibromas or meningoceles that protrude through spinal foramina
- Subperiostial bone proliferation
- Two closely spaced cysts within a bone
Correct Answer: Neurofibromas or meningoceles that protrude through spinal foramina
Explanation:
Intraspinal lesions, such as neurofibromas and meningoceles, that protrude through the neural foramina give the radiologic appearance of a "dumbbell lesion." Flattening of the intervertebral disk with enlargement of the lateral borders is not a feature of neurofibromatosis 1 (NF1). Tibial dysplasia seen in patients with NF1 lead to anterolateral bowing and does not give the appearance of a dumbbell. While subperiostial bone proliferation is seen in NF1, it does not give the appearance of a dumbbell. Bone cysts are a recognized complication of NF1, but are not the origin of the dumbbell lesions seen on radiographs.
Question 21:
Which of the following treatments is contraindicated as treatment for kyphoscoliosis in neurofibromatosis 1 (NF1):
Options:
- Laminectomy over the apex of the kyphosis
- Halo traction
- Bracing
- Anterior spinal fusion
- Posterior spinal fusion
Correct Answer: Laminectomy over the apex of the kyphosis
Explanation:
Laminectomy is contraindicated because the cord is usually compressed anteriorly and resection removes bone necessary for fusion.
Question 22:
A 1-year-old girl presents with a right lower extremity abnormality. Her parents report that she has been attempting to stand, but she has not yet walked. C linically, she has a stiff, flexed, varus right knee with an obvious leg length discrepancy. Her ankle is also in a varus position. She does not spontaneously flex or extend the knee from its flexed position. Radiographs show that she has complete tibial hemimelia. The best choice of treatment at this time for the condition is:
Options:
- Observation
- Syme amputation
- Limb lengthening
- Knee disarticulation
- Brown procedure
Correct Answer: Knee disarticulation
Explanation:
Knee disarticulation eliminates the malformed knee and ankle, allows the use of a prosthesis at an early age to promote ambulation development, and has good long-term results. Observation is a poor option due to the severity of the deformity and the need for treatment to develop ambulation. Syme's amputation does not address the deformity of the knee. In general, joint malformation or instability precludes lengthening procedures. The Brown procedure centralizes the fibula at the knee and includes a Syme's amputation for the abnormal ankle. However, a functioning quadriceps is a prerequisite and there is a high likelihood of flexion contracture postoperatively.
Question 23:
All of the following are consistent with tibial hemimelia (TH) except:
Options:
- Hypoplastic distal femur
- Absent extensor mechanism
- Ankle varus
- Knee valgus
- Knee flexion contracture
Correct Answer: Knee valgus
Explanation:
All of the answers are consistent with tibial hemimelia (TH) except for knee valgus. The knee is typically in varus due to a present fibula in TH. The foot is typically also in equinovarus, and the leg segment is shortened. Knee disarticulation is the best treatment for a complete TH.
Question 24:
Fibular hemimelia (FH) can be associated with which of the following abnormalities:
Options:
- Femoral shortening
- Anterior cruciate ligament (AC L) deficiency
- Equinovalgus foot
- Tarsal coalition
- All of the above
Correct Answer: All of the above
Explanation:
All of the stated abnormalities can be found with femoral hemimelia. It is estimated that 15% of cases have femoral deficiency. Commonly seen in the condition are tarsal coalition, anterior cruciate ligament deficiency, and an equinovalgus foot.
Question 25:
A 7-year-old boy presents with bilateral high arches. His parents report that they are having difficulty finding shoes that comfortably fit him. The patient denies any foot pain. The father had similar problems with his feet and was diagnosed with a "mild" neurologic condition. On exam, the child has bilateral pes cavus with a supple hindfoot. Treatment of the feet at this time should consist of:
Options:
- Soft tissue procedures alone
- Soft tissue procedures and calcaneal osteotomy
- Triple arthrodesis
- Bracing
- Observation
Correct Answer: Soft tissue procedures alone
Explanation:
The child has a supple deformity secondary to C harcot-Marie-Tooth disease that will progress if untreated. Soft tissue procedures, which may consist of claw toe correction, plantar release, and possibly tendon transfer, are recommended for children younger than 8 years old who have a supple hindfoot. The calcaneal osteotomy is reserved for patients with a rigid hindfoot. Triple arthrodesis is a salvage procedure reserved for a fixed, painful foot in older children. Bracing and observation are not preferred options due to the progressive nature of the disease, and the lack of ability to apply corrective forces to the foot in cavus.
Question 26:
A 17-year-old man with C harcot-Marie-Tooth disease (C MT) presents with pain in his right foot. He has had no treatment for the foot in the past. On exam, he is noted to have a rigid pes cavus with hindfoot varus, as well as some weakness in the anterior tibialis and peroneal muscles. Radiographs display the above deformity with degenerative changes in the subtalar joint. Treatment of the foot should consist of:
Options:
- Observation
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Triple arthrodesis
- Soft tissue release and tendon transfers
- Soft tissue release and calcaneal osteotomy
Correct Answer: Triple arthrodesis
Explanation:
The patient has a rigid, painful deformity with radiographic signs of arthritis. A triple arthrodesis is his best chance at a pain-free, plantigrade foot. Observation will not solve his pain due to the deformity and degenerative changes in the foot. Nonsteroidal anti-inflammatory drugs (NSAIDs) may help with his pain, however, the degeneration in the foot will continue to progress. Because the patient has a rigid deformity, soft tissue procedures will not alleviate the pain.
Question 27:
Which ancillary test is not helpful in the diagnosis of C harcot-Marie-Tooth disease (C MT):
Options:
- Electromyography (EMG)
- Nerve conduction velocity (NC V)
- Nerve biopsy
- Muscle biopsy
- Muscle enzymes
Correct Answer: Muscle enzymes
Explanation:
Charcot-Marie-Tooth disease (C MT) is a neuropathic process resulting in muscle atrophy, therefore, muscle enzyme studies will not be helpful. Electromyography (EMG) will confirm the diagnosis by displaying increased amplitude and duration of signals, both of which are indicative of a neuropathic process. Nerve conduction velocity (NC V) will also confirm the diagnosis by displaying decreased motor and sensory conduction velocities. Nerve biopsy can be helpful by showing loss of myelinated fibers and fibrosis. Muscle biopsy will show diffuse atrophy, fibrosis, and adipose tissue within muscle.
Question 28:
Which of the following is not a feature of the foot deformity in C harcot- Marie-Tooth disease (C MT):
Options:
- Hindfoot valgus
- Forefoot pronation
- Plantarflexed 1st metatarsal
- Metatarsophalangeal (MTP) joint hyperextension
- Interphalangeal (IP) joint flexion
Correct Answer: Hindfoot valgus
Explanation:
Hindfoot varus develops to counter forefoot pronation due to weakness of evertors with preservation of inverter muscle strength. The first metatarsal plantarflexes relative to the other metatarsals, leading to pronation of the forefoot. Plantarflexion of the first metatarsal occurs as part of the windlass mechanism as the intrinsics and plantar fascia contract. As the intrinsics weaken, the toe extensors pull the metatarsophalangeal (MTP) joint into hyperextension as part of the claw toe deformity. When the MTP joint hyperextends, the strength of the long toe flexors pulls the interphalangeal joint into flexion contributing to the claw toe deformity.
Question 29:
Which of the following etiologies is not thought to be associated with pseudarthrosis of the clavicle:
Options:
- Prominent cervical ribs
- Failure of fusion of the medial and lateral clavicular ossification centers
- C leidocranial dysplasia
- Pressure from the higher position of the right subclavian artery
- Stress lesion from dominant arm
Correct Answer: Stress lesion from dominant arm
Explanation:
Several theories have been proposed to explain the rare phenomenon of isolated pseudarthrosis of the clavicle. The most accepted theory is pressure from the higher riding right subclavian artery. Pseudarthrosis has also been described in patients with prominent cervical ribs. Finally, some believe that this condition is caused by failure of fusion of the medial and lateral ossification centers of the clavicle. C leidocranial dysplasia may be associated with pseudarthrosis of the clavicle. There is no evidence that they are related to stress.
Question 30:
The most common presenting symptoms of congenital pseudarthrosis of the clavicle are:
Options:
- Enlarging mass and history of pseudoparalysis at birth
- Refusal to use arm, palpable defect, and pain
- Minimally painful or painless prominence with no history of trauma
- Limitation of abduction to less than or equal to 90°
- Weakness in the distribution of the upper trunk of the brachial plexus
Correct Answer: Minimally painful or painless prominence with no history of trauma
Explanation:
The most common presentation of pseudarthrosis of the clavicle is a painless mass in right the clavicle. There is no history of trauma, and the child uses the extremity normally, with minimal pain, and with no signs of instability. There is no history of pseudoparalysis involved with congenital pseudarthrosis. Arm use is nearly normal, except for aching with activity. There is minimal restriction of motion with the pseudarthrosis, which is one reason it is sometimes not diagnosed until later in childhood. There has not been neurologic impairment with this condition.
Question 31:
Which of the following statements regarding congenital pseudarthrosis of the clavicle is not true:
Options:
- C ongenital pseudarthrosis of the clavicle occurs primarily on the right, rarely bilaterally, and when occurring on the left, congenital pseudarthrosis of the clavicle is usually associated with dextrocardia.
- Congenital pseudarthrosis of the clavicle is strongly associated with neurofibromatosis and patients often have other pseudarthroses, with the tibia being the most commonly affected site.
- Congenital pseudarthrosis of the clavicle is thought to occur due to pressure on the clavicle from the subclavian artery or prominent cervical ribs.
- Treatment for congenital pseudarthrosis of the clavicle involves intercalary bone grafting, plate, and screws.
- Impairment of the upper trunk of the brachial plexus rarely develops over time.
Correct Answer: Impairment of the upper trunk of the brachial plexus rarely develops over time.
Explanation:
Pseudarthrosis of the clavicle occurs primarily on the right side. The right predominance has been attributed to pressure on the right clavicle from the subclavian artery and occasionally cervical ribs. Treatment is straightforward with intercalary bone grafting with plate and screws fixation. There is no association with neurofibromatosis and/or pseudarthrosis of the tibia. Unlike pseudarthrosis of the tibia, congenital pseudarthrosis of the clavicle is rarely, if ever, associated with neurofibromatosis Pressure from the subclavian artery or prominent cervical ribs have been used to explain the observation that the pseudarthrosis is almost always located on the right, and if bilateral, it is associated with bilateral cervical ribs Bone graft with plate fixation is the usual treatment for these cases, although there have been reports of success in younger children from simply suturing the periosteum of the two ends together Brachial plexus impairment rarely develops in the untreated pseudarthrosis.
Question 32:
Which of the following laboratory findings are consistent with ankylosing spondylitis:
Options:
- Elevated erythrocyte sedimentation rate (ESR), positive antinuclear antibody (ANA), negative rheumatoid factor (RF), and HLADR4
- Normal ESR, negative ANA, negative RF, and HLA-B27
- Elevated ESR, negative ANA, positive RF, and HLA-B27
- Elevated ESR, negative ANA, negative RF, and positive HLA-B27
- Normal ESR, positive ANA, positive RF, and HLA-B27
Correct Answer: Elevated ESR, negative ANA, positive RF, and HLA-B27
Explanation:
Diagnostic work-up for an inflammatory autoimmune condition should include an erythrocyte sedimentation rate (ESR), antinuclear antibody (ANA), rheumatoid factor (RF), haplotype, and Lyme titer. The laboratory results most consistent with ankylosing spondylitis are an elevated ESR at the time of an acute exacerbation, negative ANA and RF, and a haplotype of HLAB27.
Question 33:
Which of the following clinical features distinguishes homocystinuria from Marfan syndrome:
Options:
- Lens dislocation
- Scoliosis
- Chest wall abnormalities
- Tall stature
- Delayed intellectual development
Correct Answer: Delayed intellectual development
Explanation:
Patients with Marfan syndrome do not typically have defects in intellectual functioning, while patients with homocystinuria typically do show signs of delayed intellectual development. Patients with Marfan syndrome and homocystinuria both develop lens dislocations, scoliosis, chest wall abnormalities, and tall stature.
Question 34:
Patients with homocystinuria undergoing lower extremity and spinal surgery must be warned of an increased risk of which complication:
Options:
- Aortic root dissection
- High output heart failure
- Venous thromboembolic disease
- Prolonged ventilator dependence
- Spontaneous pneumothorax
Correct Answer: Venous thromboembolic disease
Explanation:
Arterial and venous thromboembolic disease is common in patients with homocystinuria. Patients are at increased risk for this major complication when undergoing any surgical procedure. Unlike patients with Marfan syndrome, patients with homocystinuria do not develop aortic root dilation, aneurysms, mitral valve prolapse with high output heart failure, or spontaneous pneumothoraces. Underlying lung pathology is not a feature of homocystinuria, therefore, these patients are not at an increased risk for prolonged ventilatory support.
Question 35:
What is the molecular disturbance responsible for the development of homocystinuria:
Options:
- Translocation of chromosome 11 and 22
- Accumulation of cerebrosides in the reticuloendothelial system
- Methionine deficiency
- Deficiency of cystathionine b-synthase
- Pyridoxine deficiency
Correct Answer: Deficiency of cystathionine b-synthase
Explanation:
The metabolic disturbance responsible for homocystinuria is a deficiency of cystathionine ß-synthase. A translocation of chromosome 11 and 22 is a feature of some patients with Ewingâ s tumor. Accumulation of cerebrosides in the reticuloendothelial system is found in Gaucherâ s disease. Methionine is present in excessive quantities in homocystinuria because it cannot be converted to cysteine due to the deficiency of cystathionine ß- synthase. Pyridoxine deficiency is a secondary feature of the disorder, but it is not the primary cause.
Question 36:
Which form of chronic inflammatory arthritis is more common in boys than in girls?
Options:
- Polyarticular
- Pauciarticular
- Systemic onset
- Seronegative spondyloarthropaty
- Monoarticular
Correct Answer: Seronegative spondyloarthropaty
Explanation:
Overall, juvenile rheumatoid arthritis (JRA) is much more common in girls. In pauciarticular JRA, the ratio is 4:1 female. In polyarticular JTA, it is 3:1 female, and in systemic JRA the ratio is 1:1. Seronegative spondylarthropathy is more common in males. The incidence of polyarticular JRA is 3 times higher in girls than in boys. The incidence of pauciarticular JRA occurs 4 times more often in girls than in boys. Girls and boys are equally affected by systemic onset JRA.
Question 37:
Which of the following subtypes of juvenile rheumatoid arthritis (JRA) results in the highest risk of developing iritis:
Options:
- Systemic JRA
- Pauciarticular JRA
- Polyarticular JRA
- All are at approximately equal risk
- Eye involvement is not a problem in JRA
Correct Answer: Pauciarticular JRA
Explanation:
Patients with pauciarticular juvenile rheumatoid arthritis (JRA) have the highest risk of developing iritis, cataracts, and blindness. Polyarticular JRA has the second highest risk. Patients with systemic JRA rarely develop iritis. All newly diagnosed JRA patients should be acutely evaluated and closely followed by an ophthalmologist. Systemic-onset JRA has the lowest risk of uveitis There is a distinct difference among the types of JRA in terms of risk of eye involvement. Eye involvement is one of the problems physicians should be alert for in order to make an early diagnosis and prevent cataracts and blindness.
Question 38:
In the evaluation of a child with possible inflammatory arthritis, which tests should be ordered for possible juvenile rheumatoid arthritis:
Options:
- C BC , ANA, RF, ESR, C RP, ophthalmology consult
- RF, C RP, ANA, ESR, and C BC
- C BC , echocardiogram, ANA, RF, and C RP
- HLA-typing, ophthalmology consult, ANA, RF, and C BC
- RF and synovial fluid analysis
Correct Answer: C BC , ANA, RF, ESR, C RP, ophthalmology consult
Explanation:
Juvenile rheumatoid arthritis (JRA) is primarily a clinical diagnosis; however, routine screening tests should be ordered as part of a routine work- up. All patients should have a C BC , RF, ANA, ESR, C RP, and ophthalmology consult to look for eye involvement. An echocardiogram is not necessary unless a pericardial rub or other cardiac symptoms are present. HLA associations have been made with the different sub-types of the disease; however, this test is not necessary or diagnostic. The CBC helps to rule out hematologic malignancy and assess the patientâ s general health. The ANA looks at the possibility of systemic lupus erythematosus and, if positive at low titer, heralds an increased risk of uveitis. A positive RF helps rule in JRA and makes the risk of later erosive disease more likely. ESR and C RP are helpful for monitoring disease activity. Ophthalmology consultation will help to rule out or detect uveitis at an early stage. HLA typing is not indicated in the typical patient with JRA; it may be useful in the older male with axial symptoms. Synovial fluid analysis yields inflammatory fluid in this condition, but no information specific for the diagnosis.
Question 39:
A 7-year-old child sustained a type 3 closed supracondylar fracture of the humerus 2 hours ago. Neurologic function is intact, but a pulse cannot be found by palpation or doppler. The hand is slightly cool. Your next step is to perform:
Options:
- Arteriogram of the extremity.
- Injection of lidocaine into the antecubital region
- An attempt at closed reduction of the fracture
- Open reduction of the fracture
- Vascular repair
Correct Answer: An attempt at closed reduction of the fracture
Explanation:
Closed reduction should be carefully attempted at first, and often a tethered artery will be freed. If no pulse returns, open exploration is indicated if the hand remains cool. An arteriogram is rarely indicated because it is unlikely to yield additional information. Lidocaine may be instilled if there is spasm at the time of open reduction. Open reduction of the fracture is indicated only if closed reduction fails, or if the fracture is open. Vascular repair is not the first step; exploration and repair should be carried out only if the pulse does not return after an attempt at closed reduction.
Question 40:
The nerve most commonly injured at the time of a supracondylar fracture is:
Options:
- Radial nerve
- Median nerve
- Ulnar nerve
- Anterior interosseous nerve
- Posterior interosseous nerve
Correct Answer: Anterior interosseous nerve
Explanation:
The anterior interosseous nerve is the most commonly injured nerve. The anterior interosseous nerve can be tested by asking the patient to make an "O" with the thumb and index fingers, and watching for active flexion of the distal interphalangeal joints. The radial nerve is the second most commonly injured, after the anterior interosseous nerve. The ulnar nerve is not the most commonly injured at time of fracture but is the most commonly injured at time of treatment. The posterior interosseous nerve is rarely injured.
Question 41:
A 9-year-old child presents one year after a supracondylar humerus fracture is healed. The elbow is in 15° more varus than the other side. Which of the following statements to the family is true:
Options:
- This is likely to be due to growth plate damage in the distal humerus.
- This is likely to correct fully before the end of growth.
- The deformity is probably due to hyperemia and overgrowth of the capitellum.
- The deformity is likely due to malposition of the fracture during healing.
- The varus will likely lead to an increased likelihood of degenerative joint disease.
Correct Answer: The deformity is probably due to hyperemia and overgrowth of the capitellum.
Explanation:
Fracture malalignment is the most common cause of cubitus varus. Physeal damage is rare after supracondylar fractures. Angular malalignment corrects slowly and incompletely in the distal humerus, especially in the coronal plane. There is no reason for selective hyperemia of the capitellum in this fracture. There is no evidence of predisposition to degenerative joint disease in cubitus varus.
Question 42:
Positioning of the humeral stem at the time of total shoulder arthroplasty should allow congruent articulation with the glenoid component. C ongruent articulation occurs in most shoulders with a humeral stem positioned in:
Options:
- Neutral version
- 10° to 20° of retroversion
- 20° to 30° of retroversion
- 10° to 20° of anteversion
- 20° to 30° of anteversion
Correct Answer: 20° to 30° of retroversion
Explanation:
It is important to place the humeral stem in appropriate version to "mate" with the glenoid component. This is most often represented by 20° to 30° of humeral retroversion.
Question 43:
Which of the following tests is most specific for the diagnosis of Lyme disease:
Options:
- Elevated erythrocyte sedimentation rate (ESR)
- Elevated C -reactive protein (C RP)
- Negative antinuclear antibody (ANA)
- Negative rheumatoid factor
- Elevated antibody titer to Borrelia burgdorferi
Correct Answer: Elevated antibody titer to Borrelia burgdorferi
Explanation:
The most specific laboratory finding is an elevated antibody titer to Borrelia burgdorferi. This test is commonly referred to as a Lyme titer. All of the mentioned tests are generally seen in Lyme disease, however, elevated erythrocyte sedimentation rate, elevated C - reactive protein, negative antinuclear antibody, and negative rheumatoid factor are all nonspecific.
Question 44:
Which of the following statements is true regarding Lyme disease:
Options:
- C ardiac and neurologic symptoms are the most common manifestations of the disease.
- Arthritic symptoms primarily affect large joints and a majority of patients are cured with antibiotic therapy.
- The characteristic skin rash occurs late in the disease and can be permanently disfiguring.
- Arthritic symptoms often do not fully resolve with antibiotic treatment, with a majority of patients progressing on to a rheumatoid-like destructive arthritis.
- Lyme disease is easy to diagnose and a majority of cases are picked up after a few weeks.
Correct Answer: Arthritic symptoms primarily affect large joints and a majority of patients are cured with antibiotic therapy.
Explanation:
Approximately 60% of patients develop arthritic symptoms that primarily affect large joints. The prognosis for most patients is good after treatment with antibiotics. Cardiac and neurologic symptoms occur in a minority of patients, however, they can be the most serious symptoms. Erythema chronicum migrans is the characteristic skin rash. The rash tends to remit with antibiotic treatment and permanent disfigurement is not typically a problem. Only 1%-2% of pediatric patients develop chronic arthritis. Lyme disease may be difficult to diagnose because of the numerous possible presentations.
Question 45:
Lyme disease is caused by which of the following organisms or mechanisms:
Options:
- Group A Streptococcus
- Borrelia burgdorferi
- Vibrio vulnificus
- Group B Streptococcus
- Autoimmune disorder of unknown etiology
Correct Answer: Borrelia burgdorferi
Explanation:
Lyme disease was initially thought to be an idiopathic autoimmune disorder; however, in the 1970s, researchers at Yale University identified Borrelia burgdorferi as the cause of the disease. The disease is transmitted by a deer tick known as Ixodes ricinusi. Group A streptococcal pharyngitis may be followed by rheumatic fever, but not Lyme disease. Vibrio vulnificus is the organism responsible for severe soft tissue infections in patients who are exposed to fresh-water shellfish. Group B Streptococcus is a common etiologic agent for necrotizing fasciitis.
Question 46:
The most serious long-term sequela of rheumatic fever is:
Options:
- Skin disfiguration from migratory rash
- Disabling arthritis in affected joints
- Rheumatic valvular heart disease
- Need for long-term prophylaxis for the prevention of relapses
- Decreased lung capacity secondary to fibrosis
Correct Answer: Rheumatic valvular heart disease
Explanation:
The most serious potential long-term sequela of rheumatic fever is rheumatic valvular heart disease. Patients do not develop any permanent skin lesions or joint disability from the disease. Some patients require long-term prophylaxis to prevent recurrences, however, this is an inconvenience and not a sequela. The lungs are not affected in the acute fever or subsequent relapses.
Question 47:
Joint pain in rheumatic fever:
Options:
- Affects 2 to 4 large joints over several months
- Responds to aspirin therapy
- Results in long-term disability with joint destruction
- Is best treated with penicillin G
- Is a major criterion for diagnosis
Correct Answer: Responds to aspirin therapy
Explanation:
Joint pain is common in rheumatic fever. It is an intensely painful arthralgia that migrates from joint to joint within hours. The pain responds to aspirin therapy, as well as rest. Although oral penicillin G is used for treatment of the disease, it will not produce rapid resolution of the joint pain. In untreated cases, it can affect up to 16 joints. Most patients are left with no long-term sequelae or disability of the musculoskeletal system from rheumatic fever. Joint arthralgias are minor criteria for diagnosis.
Question 48:
Patients with homocystinuria phenotypically resemble patients with:
Options:
- Achondroplasia
- Larsen's syndrome
- Marfan syndrome
- Gaucher's disease
- Noonan's syndrome
Correct Answer: Marfan syndrome
Explanation:
Patients with homocystinuria may phenotypically resemble patients with Marfan syndrome. Patients with homocystinuria and Marfan syndrome are tall with long limbs, arachnodactyly, scoliosis, chest wall deformities, and lens dislocations. Achondroplasia is characterized by short stature, frontal bossing, and rhizomelic shortening of the limbs. Larsen's syndrome is a disorder characterized by short stature and multiple joint dislocations. Gaucher's disease is a lysosomal storage disease characterized by accumulation of cerebroside in cells of the reticuloendothelial system. As in patients with homocystinuria, patients with Gaucher's disease have osteoporosis, however, they do not develop any of the other phenotypic features seen in homocystinuria. Noonan's syndrome effects boys and clinical features include short stature, a webbed neck, and cubitus valgus deformities.
Question 49:
A genetic defect found in some types of Ehlers-Danlos syndrome (EDS) is:
Options:
- Fibrillin
- Type I collagen
- Fibroblast growth factor (FGF) receptor 3
- Dystrophin
- Hypoxanthine-guanine phosphoribosyl transferase
Correct Answer: Type I collagen
Explanation:
Ehlers-Danlos syndrome (EDS) was once described as a single gene disorder affecting type I collagen, but it has since been discovered that EDS is a family of heterogeneous disorders with many described mutations. Type I collagen is defective in EDS type VII and collagen type III is defective in EDS type IV and VIII. Fibrillin and fibroblast growth factor (FGF) receptor 3 are defective in Marfan syndrome and achondroplasia, respectively. Dystrophin is deficient in muscular dystrophy. Hypoxanthine-guanine phosphoribosyl transferase is defective in Lesch- Nyhan syndrome.
Question 50:
Which of the following features differentiates Marfan syndrome from Ehlers-Danlos syndrome (EDS):
Options:
- Joint hypermobility
- Scoliosis
- Lens dislocation
- Vascular problems
- Joint dislocations
Correct Answer: Lens dislocation
Explanation:
Patients with Ehlers-Danlos syndrome (EDS) and Marfan syndrome may have joint hypermobility, scoliosis, vascular problems, and recurrent joint instability. Patients with Marfan syndrome also develop lens dislocations, and while some patients with EDS exhibit eye problems, it is related to ocular globe fragility. Lens dislocation is not a feature of EDS.