Orthopedic Prometric Exam Preparation MCQs - Part 11
Prometric Exam Simulator
00:00
Start Quiz
Question 1
In obstetric brachial plexus injury, an indicator of plexus recovery at 3 months is the return of the:
Explanation
Question 2
A 15-year-old boy presented with inability to elevate his right shoulder and flex his elbow. He sustained a fall from an all-terrain vehicle 8 weeks ago. He landed on the right shoulder and twisted his neck. Radiographs of the skull, chest, cervical and thoracic spine, and shoulder were normal. There was no loss of consciousness, chest pain, or breathing difficulties. The patient was observed in the hospital until stable and referred for follow-up in the hand clinic at 4 weeks. An electromyelogram (EMG) was scheduled. Clinical examination revealed weakness of deltoid, supraspinatus, infraspinatus, teres minor, biceps, brachialis, brachioradialis, and extensor carpi radialis longus. The remainder of his forearm musculature was preserved and he could grasp, release, and pinch. Sensations were decreased along the distribution of the axillary nerve. There was 3 cm wasting of his arm and 2 cm of the forearm. Tinelâ s sign is positive around the clavicle. Hornerâ s signs are absent and his arm lies against the body. The EMG report showed fibrillation potentials in the weak muscles. The patient can now flex his elbow. When asked to demonstrate, he flexes his wrist and pronates his forearm to swing his elbow into flexion. Diagnosis of the condition is:
Explanation
Question 3
A 15-year-old boy presented with inability to elevate his right shoulder and flex his elbow. He sustained a fall from an all-terrain vehicle 8 weeks ago. He landed on the right shoulder and twisted his neck. Radiographs of the skull, chest, cervical and thoracic spine, and shoulder were normal. There was no loss of consciousness, chest pain, or breathing difficulties. The patient was observed in the hospital until stable and referred for follow-up in the hand clinic at 4 weeks. An electromyelogram (EMG) was scheduled. C linical examination revealed weakness of deltoid, supraspinatus, infraspinatus, teres minor, biceps, brachialis, brachioradialis, and extensor carpi radialis longus. The remainder of his forearm musculature was preserved and he could grasp, release, and pinch. Sensations were decreased along the distribution of the axillary nerve. There was 3-cm wasting of his arm and 2 cm of the forearm. Tinels sign is positive around the clavicle. Hornerâ s signs are absent and his arm lies against the body. The EMG report showed fibrillation potentials in the weak muscles. The patient can now flex his elbow. When asked to demonstrate, he flexes his wrist and pronates his forearm to swing his elbow into flexion. The level of lesion is:
Explanation
Question 4
A 15-year-old boy presented with inability to elevate his right shoulder and flex his elbow. He sustained a fall from an all-terrain vehicle 8 weeks ago. He landed on the right shoulder and twisted his neck. Radiographs of the skull, chest, cervical and thoracic spine, and shoulder were normal. There was no loss of consciousness, chest pain, or breathing difficulties. The patient was observed in the hospital until stable and referred for follow-up in the hand clinic at 4 weeks. An electromyelogram (EMG) was scheduled. C linical examination revealed weakness of deltoid, supraspinatus, infraspinatus, teres minor, biceps, brachialis, brachioradialis, and extensorcarpi radialis longus. The remainder of his forearm musculature was preserved and he could grasp, release, and pinch. Sensations were decreased along the distribution of the axillary nerve. There was 3 cm wasting of his arm and 2 cm of the forearm. Tinelâ s sign is positive around the clavicle. Hornerâ s signs are absent and his arm lies against the body. The EMG report showed fibrillation potentials in the weak muscles. The patient can now flex his elbow. When asked to demonstrate, he flexes his wrist and pronates his forearm to swing his elbow into flexion. The least helpful test in further management of this patient is:
Explanation
Question 5
A 15-year-old boy presented with inability to elevate his right shoulder and flex his elbow. He sustained a fall from an all-terrain vehicle 8 weeks ago. He landed on the right shoulder and twisted his neck. Radiographs of the skull, chest, cervical and thoracic spine, and shoulder were normal. There was no loss of consciousness, chest pain, or breathing difficulties. The patient was observed in the hospital until stable and referred for follow-up in the hand clinic at 4 weeks. An electromyelogram (EMG) was scheduled. C linical examination revealed weakness of deltoid, supraspinatus, infraspinatus, teres minor, biceps, brachialis, brachioradialis, and extensor carpi radialis longus. The remainder of his forearm musculature was preserved and he could grasp, release, and pinch. Sensations were decreased along the distribution of the axillary nerve. There was 3 cm wasting of his arm and 2 cm of the forearm. Tinelâ s sign is positive around the clavicle. Hornerâ s signs are absent and his arm lies against the body. The EMG report showed fibrillation potentials in the weak muscles. The patient can now flex his elbow. When asked to demonstrate, he flexes his wrist and pronates his forearm to swing his elbow into flexion. The plan of management in this patient 5 months postinjury with no clinical improvement should be:
Explanation
Question 6
A 15-year-old boy presented with inability to elevate his right shoulder and flex his elbow. He sustained a fall from an all-terrain vehicle 8 weeks ago. He landed on the right shoulder and twisted his neck. Radiographs of the skull, chest, cervical and thoracic spine, and shoulder were normal. There was no loss of consciousness, chest pain, or breathing difficulties. The patient was observed in the hospital until stable and referred for follow-up in the hand clinic at 4 weeks. An electromyelogram (EMG) was scheduled. C linical examination revealed weakness of deltoid, supraspinatus, infraspinatus, teres minor, biceps, brachialis, brachioradialis, and extensor carpi radialis longus. The remainder of his forearm musculature was preserved and he could grasp, release, and pinch. Sensations were decreased along the distribution of the axillary nerve. There was 3 cm wasting of his arm and 2 cm of the forearm. Tinelâ s sign is positive around the clavicle. Horners signs are absent and his arm lies against the body. The EMG report showed fibrillation potentials in the weak muscles. The patient can now flex his elbow. When asked to demonstrate, he flexes his wrist and pronates his forearm to swing his elbow into flexion. The most important indication for early exploration in this patient is:
Explanation
Question 7
A 15-year-old boy presented with inability to elevate his right shoulder and flex his elbow. He sustained a fall from an all-terrain vehicle eight weeks prior. He landed on the right shoulder and twisted his neck. Radiographs of the skull, chest, cervical and thoracic spine, and shoulder were normal. There was no loss of consciousness, chest pain, or breathing difficulties. The patient was observed in the hospital until stable and referred for follow-up in the hand clinic at 4 weeks. An electromyelogram (EMG) was scheduled. C linical examination revealed weakness of deltoid, supraspinatus, infraspinatus, teres minor, biceps, brachialis, brachioradialis, and extensor carpi radialis longus. The remainder of his forearm musculature was preserved and he could grasp, release, and pinch. Sensations were decreased along the distribution of the axillary nerve. There was 3-cm wasting of his arm and 2 cm of the forearm. Tinelâ s sign is positive around the clavicle. Hornerâ s signs are absent and his arm lies against the body. The EMG report showed fibrillation potentials in the weak muscles. The patient can now flex his elbow. When asked to demonstrate, he flexes his wrist and pronates his forearm to swing his elbow into flexion. The most important function that needs to be restored in this patient is:
Explanation
Question 8
An 18-month-old boy presents with a clawing deformity of the right hand. He was born full term after a difficult delivery complicated by shoulder dystocia. He weighed 9.5 lbs at birth. The patient had a brief episode of apnea with an APGAR score of 5 at birth and needed resuscitation and admission to the neonatal intensive care unit. A tender bump was noted on the patients right clavicle, which was diagnosed as clavicle fracture. A week later, the patient could not flex the fingers of his right hand. The neonatologist informed the parents that the fracture was managed conservatively and the absence of finger flexion was due to fracture and would recover. However, recovery can be prolonged and may take up to two years. The patient has grown and his immunization is complete. His right hand has extension at all the metacarpal joints of the fingers while the proximal interphalangeal and distal interphalangeal joints are flexed. The thumb is in an adducted position, and it is difficult to passively bring the thumb to full abduction. There is obvious wasting of the hand and forearm. The patient moves the arm well with no abnormalities noticed at the shoulder, elbow, and wrist. Radiograph of the chest shows a healed clavicle fracture with no evidence of diaphragmatic paralysis. There is no evidence of Hornerâ s syndrome and the grasp reflex is absent. Diagnosis of this condition is:
Explanation
Question 9
An 18-month-old boy presents with a clawing deformity of the right hand. He was born full term after a difficult delivery complicated by shoulder dystocia. He weighed 9.5 lbs at birth. The patient had a brief episode of apnea with an APGAR score of 5 at birth and needed resuscitation and admission to the neonatal intensive care unit. A tender bump was noted on the patients right clavicle, which was diagnosed as clavicle fracture. A week later, the patient could not flex the fingers of his right hand. The neonatologist informed the parents that the fracture was managed conservatively and the absence of finger flexion was due to fracture and would recover. However, recovery can be prolonged and may take up to two years. The patient has grown and his immunization is complete. His right hand has extension at all the metacarpal joints of the fingers while the proximal interphalangeal and distal interphalangeal joints are flexed. The thumb is in an adducted position, and it is difficult to passively bring the thumb to full abduction. There is obvious wasting of the hand and forearm. The patient moves the arm well with no abnormalities noticed at the shoulder, elbow, and wrist. Radiograph of the chest shows a healed clavicle fracture with no evidence of diaphragmatic paralysis. There is no evidence of Horners syndrome and the grasp reflex is absent. The level of the lesion in this patient is:
Explanation
Question 10
An 18-month-old boy presents with a clawing deformity of the right hand. He was born full term after a difficult delivery complicated by shoulder dystocia. He weighed 9.5 lbs at birth. The patient had a brief episode of apnea with an APGAR score of 5 at birth and needed resuscitation and admission to the neonatal intensive care unit. A tender bump was noted on the patients right clavicle, which was diagnosed as clavicle fracture. A week later, the patient could not flex the fingers of his right hand. The neonatologist informed the parents that the fracture was managed conservatively and the absence of finger flexion was due to fracture and would recover. However, recovery can be prolonged and may take up to two years. The patient has grown and his immunization is complete. His right hand has extension at all the metacarpal joints of the fingers while the proximal interphalangeal and distal interphalangeal joints are flexed. The thumb is in an adducted position, and it is difficult to passively bring the thumb to full abduction. There is obvious wasting of the hand and forearm. The patient moves the arm well with no abnormalities noticed at the shoulder, elbow, and wrist. Radiograph of the chest shows a healed clavicle fracture with no evidence of diaphragmatic paralysis. There is no evidence of Horners syndrome and the grasp reflex is absent. Appropriate surgical management in this case is:
Explanation
Question 11
An 18-month-old boy presents with a clawing deformity of the right hand. He was born full term after a difficult delivery complicated by shoulder dystocia. He weighed 9.5 lbs at birth. The patient had a brief episode of apnea with an APGAR score of 5 at birth and needed resuscitation and admission to the neonatal intensive care unit. A tender bump was noted on the patients right clavicle, which was diagnosed as clavicle fracture. A week later, the patient could not flex the fingers of his right hand. The neonatologist informed the parents that the fracture was managed conservatively and the absence of finger flexion was due to fracture and would recover. However, recovery can be prolonged and may take up to two years. The patient has grown and his immunization is complete. His right hand has extension at all the metacarpal joints of the fingers while the proximal interphalangeal and distal interphalangeal joints are flexed. The thumb is in an adducted position, and it is difficult to passively bring the thumb to full abduction. There is obvious wasting of the hand and forearm. The patient moves the arm well with no abnormalities noticed at the shoulder, elbow, and wrist. Radiograph of the chest shows a healed clavicle fracture with no evidence of diaphragmatic paralysis. There is no evidence of Hornerâ s syndrome and the grasp reflex is absent. Reconstructive surgery includes all of the following except:
Explanation
Question 12
Which mechanism and long-term deformity is most often associated with a dorsal avulsion fracture at the base of the middle phalanx:
Explanation
Question 13
At what degree of flexion is ulnar collateral ligament injury tested:
Explanation
Question 14
Which of the following structures are found within the first dorsal compartment:
Explanation
Question 15
A 28-year-old man fell off his bike and sustained a fall onto his outstretched hand. He experiences thumb and index finger numbness. Attempts at reduction of his grade I open extra-articular distal radius fracture are unsuccessful. The next appropriate step of management is:
Explanation
Question 16
Which of the following is not usually associated with radial deficiency:
Explanation
Question 17
Which of the following is the most common carpal coalition in the hand:
Explanation
Question 18
A 6-year-old boy presents with a Salter-Harris II distal radius fracture 3 weeks after injury. He is nontender and neurologically intact. On radiographs, he has a 35º dorsal angulation. The appropriate course of treatment is:
Explanation
Question 19
The oblique retinacular ligament connects with what two structures:
Explanation
Question 20
A patient presents with hand weakness. On examination, she has no sensory deficient, decreased strength with pronation, and her elbow is at 90º of flexion and pulp-to-pulp contact on key pinch. The most likely diagnosis is:
Explanation
Question 21
Indications for operative treatment in an acute elbow dislocation include:
Explanation
Question 22
When performing open reduction and internal fixation of radial neck fractures, the plate should be placed:
Explanation
Question 23
Heterotopic ossification after elbow dislocations is not associated with which of the following:
Explanation
Question 24
What is the order of joint destruction in a patient with scapholunate disassociation:
Explanation
Question 25
Which of the following is not characteristic of Dupuytrenâ s disease:
Explanation
Question 26
Operative indications for Dupuytrenâ s contracture include:
Explanation
Question 27
Favorable indications for attempted replantation include:
Explanation
Question 28
Injuries to the central articular disk portion of the triangular fibrocartilage complex are related to all of the following except:
Explanation
Question 29
All of the following transfers may be used to improve function in a patient who has had radial nerve paralysis longer than 6 months, except:
Explanation
Question 30
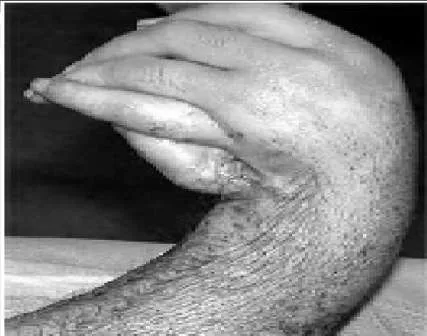
A 24-year-old man presents with a short forearm and a hand deformity. The patient is otherwise healthy with no other congenital defects. The clinical appearance of his forearm is shown (Slide). Your diagnosis is:
Explanation
Question 31
A 24-year-old man presents with a short forearm and a hand deformity. The patient is otherwise healthy with no other congenital defects. The clinical appearance of his forearm is shown (Slide). The patient has an elbow flexion contracture of 70° and desires lengthening. Which of the following statements is not true regarding lengthening:
Explanation
Question 32
A 24-year-old man presents with a short forearm and a hand deformity. The patient is otherwise healthy with no other congenital defects. The clinical appearance of his forearm is shown (Slide). The potential complications of lengthening are discussed, and the patient is advised against it. However, the elbow flexion contracture is corrected by gradual distraction. One year postoperatively, the patient has attained a 30° correction of the flexion deformity, which remains mobile. Now, he desires that his wrist deformity be corrected. The procedure of choice is:
Explanation
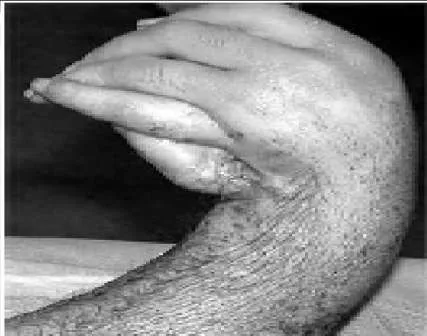 Wrist arthrodesis is the best solution for this patient and his recurrent deformity because it provides a stable platform for grasp.C orrect Answer: Arthrodesis
Wrist arthrodesis is the best solution for this patient and his recurrent deformity because it provides a stable platform for grasp.C orrect Answer: Arthrodesis
Question 33
A 24-year-old man presents with a short forearm and a hand deformity. The patient is otherwise healthy with no other congenital defects. The clinical appearance of his forearm is shown (Slide). Although the patient has a thumb, it is in an abnormal position. Any attempt to make his thumb more functional will be influenced by:
Explanation
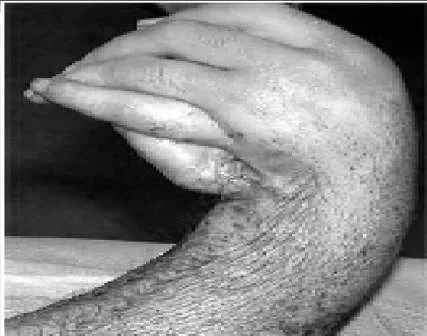 The pattern of usage of the hand is established in the brain by 2 to 3 years of age. Although pollicization has been performed in adolescents, patients continue to prefer a scissor pinch. At 24 years of age, this pattern will be well established. The patient can be coaxed to use his thumb, but it will not be involuntary and automatic.C orrect Answer: Presence of a side-to-side finger grip
The pattern of usage of the hand is established in the brain by 2 to 3 years of age. Although pollicization has been performed in adolescents, patients continue to prefer a scissor pinch. At 24 years of age, this pattern will be well established. The patient can be coaxed to use his thumb, but it will not be involuntary and automatic.C orrect Answer: Presence of a side-to-side finger grip
Question 34
A radial club hand is the result of an insult during which phase of the gestation period:
Explanation
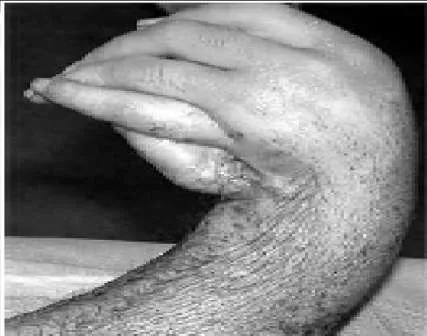 A radial club hand is the result of an insult during weeks 4 to 7 of gestation.
A radial club hand is the result of an insult during weeks 4 to 7 of gestation.
Question 35
A 15-day-old boy presents with deformity of the right hand. The boy was delivered prematurely and underwent an urgent arterial switch for transposition of great vessels. The patient is in stable condition. He has a radial club hand, and because the radial head cannot be palpated, total absence of radius is suspected. The thumb is absent and the index finger has camptodactyly. The forearm is short compared to the left side, and the patient flexes his elbow upon stimulation. Spontaneous finger motion is also present. A thorough physical examination is performed and a set of investigations is ordered. The results are as follows: complete blood count 10,000 mcu/L; platelet 254 254×103 mcu/L; neutophils 50%; Hb 14.2 mg/dL; lymphocytes 40%; Hct 45; and monocytes 10%. No renal abnormalities were noted on ultrasonogram of the abdomen. A radiograph of the spine is normal. Diagnosis is:
Explanation
Question 36
The principal abnormality associated with Holt-Oram syndrome is:
Explanation
Question 37
The hereditary pattern for Holt-Oram syndrome is:
Explanation
Question 38
A 15-day-old boy presents with deformity of the right hand. The boy was delivered prematurely and underwent an urgent arterial switch for transposition of great vessels. The patient is in stable condition. He has a radial club hand, and because the radial head cannot be palpated, total absence of radius is suspected. The thumb is absent and the index finger has camptodactyly. The forearm is short compared to the left side, and the patient flexes his elbow upon stimulation. Spontaneous finger motion is also present. A thorough physical examination is performed and a set of investigations is ordered. The results are as follows: complete blood count 10,000 mcu/L; 254×103 mcu/L; neutophils 50%; Hb 14.2 mg/dL; lymphocytes 40%; Hct 45; and monocytes 10%. No renal abnormalities were noted on ultrasonogram of the abdomen. A radiograph of the spine is normal. The next step in the management of the radial club hand is:
Explanation
Question 39
A 15-day-old boy presents with deformity of the right hand. The boy was delivered prematurely and underwent an urgent arterial switch for transposition of great vessels. The patient is in stable condition. He has a radial club hand, and because the radial head cannot be palpated, total absence of radius is suspected. The thumb is absent and the index finger has camptodactyly. The forearm is short compared to the left side, and the patient flexes his elbow upon stimulation. Spontaneous finger motion is also present. A thorough physical examination is performed and a set of investigations is ordered. The results are as follows: complete blood count 10,000 mcu/L; platelet 254×103 mcu/L; neutophils 50%; Hb 14.2 mg/dL; lymphocytes 40%; Hct 45; and monocytes 10%. No renal abnormalities were noted on ultrasonogram of the abdomen. A radiograph of the spine is normal. Centralization will be performed on the patient. All of the following statements are true about centralization except:
Explanation
Question 40
A 15-day-old boy presents with deformity of the right hand. The boy was delivered prematurely and underwent an urgent arterial switch for transposition of great vessels. The patient is in stable condition. He has a radial club hand, and because the radial head cannot be palpated, total absence of radius is suspected. The thumb is absent and the index finger has camptodactyly. The forearm is short compared to the left side, and the patient flexes his elbow upon stimulation. Spontaneous finger motion is also present. A thorough physical examination is performed and a set of investigations is ordered. The results are as follows: complete blood count 10,000 mcu/L; 254 103 mcu/L; neutophils 50%; Hb 14.2 mg/dL; lymphocytes 40%; Hct 45; and monocytes 10%. No renal abnormalities were noted on ultrasonogram of the abdomen. A radiograph of the spine is normal. When the patient is 10 years old, he is not satisfied with the length of his forearm and wishes to lengthen it. Which of the following is not a satisfactory recommendation:
Explanation
Question 41
Which of the following conditions is present in patients with radial club hand but not in patients with ulnar club hand:
Explanation
Question 42
All of the following developmental anomalies are associated with ulnar club hand except:
Explanation
Question 43
Which of the following syndromes is associated with ulnar club hand:
Explanation
Question 44
Which of the following areas is not involved in ulnar club hand:
Explanation
Question 45
All of the following are true statements regarding elbow involvement in ulnar club hand except:
Explanation
Question 46
All of the following statements are true regarding the carpal bones in patients with ulnar club hand except:
Explanation
Question 47
All of the following anomalies are present in patients with ulnar club hand except:
Explanation
Question 48
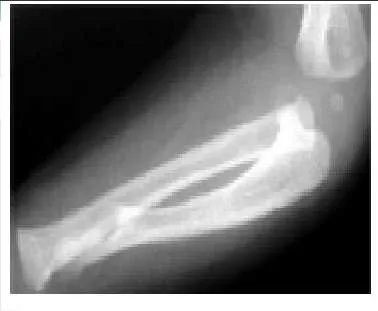
A 1-year-old boy was born full-term and pregnancy was uneventful. However, the parents noticed deformity of the patientâ s forearm, which progressed with growth. The parents consulted a pediatric orthopaedic surgeon 4 months prior and were advised to observe the growth. Multiple investigations in the form of two-dimensional echogram, abdomen ultrasonography, radiographs of the spine, and complete blood work did not reveal any abnormalities. No genetic or syndromic abnormality was reported. A radiograph taken 4 months prior is shown.
Explanation
 The ulnar deficiency is longitudinal and the ulna is considered a postaxial bone. Ulnar agenesis means absence while radial club hand is a pre-axial longitudinal deficiency and cleft hand is a central deficiency.
The ulnar deficiency is longitudinal and the ulna is considered a postaxial bone. Ulnar agenesis means absence while radial club hand is a pre-axial longitudinal deficiency and cleft hand is a central deficiency.
Question 49
A 45-year-old man presents with marked lateral elbow pain. He says that the pain has been present for 3 weeks. He has no history of recent trauma. He is an avid tennis player, and he feels increased pain after playing tennis and when doing wrist extension exercises in the gym. His pain is maximally reproduced with resisted middle finger extension and with forearm supination with the elbow extended. Electromyography would confirm the diagnosis as:
Explanation
Question 50
A 45-year-old man presents with marked lateral elbow pain. He says that the pain has been present for 3 weeks. He has no history of recent trauma. He is an avid tennis player, and he feels increased pain after playing tennis and when doing wrist extension exercises in the gym. His pain is maximally reproduced with resisted middle finger extension and with forearm supination with the elbow extended. Which of the following is the appropriate initial treatment:
Explanation
You Might Also Like