Full Question & Answer Text (for Search Engines)
Question 1:
Which digit is most commonly affected by macrodactyly:
Options:
- Thumb
- Index
- MIddle
- Ring
- Small
Correct Answer: Index
Explanation:
The index finger is most frequently affected, although multiple digital enlargement is actually more commonly seen.
Question 2:
Syndactyly is present in what percentage of patients with macrodactyly:
Options:
Correct Answer: 10%
Explanation:
The majority of patients (90%) present with unilateral macrodactyly, and men are more often affected than women. Macrodactyly is most frequently found in the index finger, followed by the long finger, thumb, ring, and little fingers. Typically, two digits are affected â most commonly the thumb and index or the index and long. Syndactyly may be present in 10% of patients with macrodactyly.
Question 3:
Macrodactyly that is present at birth is termed:
Options:
- Birth advancing macrodactyly (BAM)
- Static macrodactyly
- Progressive macrodactyly
- Simple macrodactyly
- C omplex macrodactyly
Correct Answer: Static macrodactyly
Explanation:
Barsky described macrodactyly as either static or progressive. Static macrodactyly is present at birth, and the affected digit grows larger as the child develops. In the progressive type of macrodactyly, growth begins soon after birth. This form of the disorder is more common than static macrodactyly.
Question 4:
The most accepted theory for the cause of macrodactyly is:
Options:
- Idiopathic
- Neural
- Vascular
- Humoral
- C ongenital
Correct Answer: Neural
Explanation:
Some surgeons believe that macrodactyly is a variant of neurofibromatosis. Although macrodactyly is not an inherited anomaly, there are syndromes that may be associated with enlarged digits such as Proteus syndrome. Although numerous causes have been suggested, the most accepted theory was described by Inglis in 1950. He theorized that the abnormal nerves exert influence on the local tissues to stimulate growth.
Question 5:
Syndromes that may be associated with macrodactyly include:
Options:
- Proteus syndrome
- Freeman-Sheldon syndrome
- Madelungâ s deformity
- Holt-Oram syndrome
- Poland syndrome
Correct Answer: Proteus syndrome
Explanation:
Some surgeons believe that macrodactyly is a variant of neurofibromatosis. Although macrodactyly is not an inherited anomaly, there are syndromes that may be associated with enlarged digits such as Proteus syndrome. Theoretical causes for macrodactyly include a neural cause, a vascular cause, as well as a humoral mechanism. The most accepted theory is that abnormal nerves exert some influence on the local tissues to stimulate growth.7
Question 6:
Macrodactyly affects:
Options:
- Only bones
- Bones and fat
- Bones, fat, and nerves
- Bones, fat, nerves, and blood vessels
- Bones, fat, nerves, blood vessels, and tendons
Correct Answer: Bones, fat, and nerves
Explanation:
Although this is controversial, the majority of surgeons believe that macrodactyly affects bones, fat, and nerves.
Question 7:
A 2-year-old child is brought to your office for evaluation of a "big hand." Upon examination, you notice that the child has mildly enlarged ring and small fingers. There is full range of motion without instability. After examination of the patient, you recommend:
Options:
- Scheduling the patient for immediate surgery
- Telling the parents to return when the child develops functional abnormalities
- Performing surgery within 1 week of diagnosis
- Scheduling surgery to coincide with the patient beginning school
- Performing additional testing
Correct Answer: Performing surgery within 1 week of diagnosis
Explanation:
The child is not ready for surgery. Although surgery may coincide with the patient beginning school, this does not always occur. At this time, additional examination and testing are recommended.
Question 8:
A 2-year-old child is brought to your office for evaluation of a "big hand." Upon examination, you notice that the child has mildly enlarged ring and small fingers. There is full range of motion without instability. The childâ s parents inform you that they would like you to amputate the affected digits as soon as possible. You should:
Options:
- Begin radiation therapy to arrest the growth of the affected digits
- Proceed with amputation because you have the parentsâ consent
- Send the patient to another hand surgeon
- Explain the typical course of macrodactyly and order additional testing
- Schedule the patient for a debulking procedure
Correct Answer: Explain the typical course of macrodactyly and order additional testing
Explanation:
Although amputation may be necessary in some patients with macrodactyly, it is too early in the course of this case to begin entertaining such a drastic measure. A debulking procedure is not recommended for a 2-year-old child. Radiation therapy is not an option in uncomplicated cases of macrodactyly. The surgeon must educate the parents about the disease process and order additional testing.
Question 9:
You discover that a patient who you have been treating for macrodactyly has been followed by the Proteus Syndrome Foundation. Exhaustive work-up has been completed and radiographs of the hand reveal:
Options:
- Multiple enchondromas in the affected fingers
- Enlarged bones in length only
- Enlarged bones in length and width
- Enlarged bones in width only
- Normal appearing bones
Correct Answer: Enlarged bones in length only
Explanation:
In patients with macrodactyly, surgeons do not typically find enchondromas, especially not multiple enchondromas in the affected fingers. Enlargement of the bones is found in all dimensions â not only in the length and width. If the bones appear normal on radiograph, then they are not affected by macrodactyly.
Question 10:
A 2-year-old child is brought to your office for evaluation of a "big hand." Upon examination, you notice that the child has mildly enlarged ring and small fingers. There is full range of motion without instability. After examination of the patient, you discuss the diagnosis of macrodactyly with the parents. The parents feel assured after your discussion of the disease process and your review of the radiographs. You should next see the patient:
Options:
- Never
- In 1 year
- When functional abnormalities develop
- When the enlargement of the digits has ceased
- When the patient is old enough to consent for surgery
Correct Answer: In 1 year
Explanation:
Patients with macrodactyly should be followed up yearly. Although the parents may be difficult, this is not a reason to stop seeing a patient. The other answers choices are incorrect because treatment would be too late.
Question 11:
Which of the following is not a complication of macrodactyly surgery:
Options:
- Nerve injury
- Bony malunion
- Decreased sensation
- Joint laxity
- Infection
Correct Answer: Joint laxity
Explanation:
Complications of macrodactyly surgery include poor healing of flaps secondary to devascularization or undue tension, nerve injury or decreased sensation, infection, stiffness, bony nonunion or malunion, and failure of the epiphysiodesis.
Question 12:
Epiphysiodesis for macrodactyly should be performed at the following location:
Options:
- Proximal phalanx only
- Proximal phalanx and middle phalanx
- Proximal phalanx, middle phalanx, and distal phalanx
- Middle phalanx only
- Proximal phalanx and distal phalanx
Correct Answer: Proximal phalanx only
Explanation:
Treatment by epiphysiodesis for macrodactyly is ineffective if only single phalanges are treated. Therefore, treatment of the proximal phalanx, distal phalanx, or the middle phalanx alone is incorrect. The author prefers to perform epiphysiodesis only on the proximal and distal phalanges. The middle phalanx is not treated to preserve motion at the proximal interphalangeal joint.
Question 13:
When ruptured, which portion of the scapholunate ligament leads to scaphoid-lunate diastasis:
Options:
- Distal
- Proximal
- Intermediate
- Dorsal
- Volar
Correct Answer: Dorsal
Explanation:
The dorsal section of the scapholunate ligament is the strongest portion, requiring 300 N of load for failure. The volar (150 N) and intermediate portions (25 N to 50 N) contribute less to overall stability.
Question 14:
Which of the following radiographic views is not routinely used to diagnose scapholunate injury:
Options:
- Semisupination oblique view
- C lenched fist view
- Lateral view
- Anteroposterior (AP) view
- Oblique view
Correct Answer: Semisupination oblique view
Explanation:
The semisupination oblique view is used to visualize the pisiform and pisotriquetral joint. The PA oblique and lateral views are the primary films used to diagnose scapholunate instability. The clenched fist view is used as a provocative view to bring out dynamic instability.
Question 15:
Which of the following treatments is not used for acute scapholunate ligament ruptures:
Options:
- Open repair with bone sutures
- Proximal row carpectomy
- C losed reduction and long arm cast
- Arthroscopically assisted reduction and pinning
- Open repair with suture anchors
Correct Answer: Proximal row carpectomy
Explanation:
Proximal row carpectomy is a salvage procedure for chronic instability with focal radioscaphoid arthritis. Open repair with sutures through bone tunnels, open repair with suture anchors, and arthroscopically assisted reduction and pinning have been used successfully in acute cases.
Question 16:
Which of the following is considered indicative of a scaphoid-lunate ligament tear on posteroanterior radiograph:
Options:
- Terry Thomas sign
- Volar intercalated segmental instability (VISI) pattern
- Spilled tea cup sign
- Watson-Jones scaphoid shift
- Dorsal intercalated segment instability (DISI) pattern
Correct Answer: Terry Thomas sign
Explanation:
The VISI, DISI, and spilled tea cup signs are seen on lateral radiographs, whereas the Watson-Jones scaphoid shift test is a clinical sign. The classic pattern after scaphoid-lunate ligament injury is a DISI pattern as the lunate extends and the scaphoid flexes. The spilled tea cup sign is present in perilunate dislocations.
Question 17:
The Terry Thomas sign, which is considered indicative of scaphoid-lunate ligament rupture, is best described as:
Options:
- Scapholunate diastases larger than 3 mm
- Scapholunate angle more than 30º to 60º on lateral radiographs
- Reduction and exaggeration of scapholunate diastases on radial and ulnar deviation motion studies
- Exaggeration and reduction of scaphoid-lunate diastases on radial and ulnar deviation radiographs, respectively
- Scaphoid flexion with lunate extension
Correct Answer: Scapholunate diastases larger than 3 mm
Explanation:
The Terry Thomas sign refers to scapholunate diastases that may be apparent on posteroanterior radiographs of the wrist and is indicative of rupture if the diastases are larger than 3 mm. It is named after the famous comedian who had a gap between his front teeth.
Question 18:
The most important requirement for a diagnostic magnetic resonance image (MRI) study in cases of scaphoid-lunate ligament injury is:
Options:
- 2 mm thin slices
- Tangential cuts
- Gallium-enhanced scan
- Dedicated wrist coil
- MRI in neutral, radial, and ulnar deviation
Correct Answer: Dedicated wrist coil
Explanation:
MRI is not considered the technique of choice for the evaluation of the scaphoid-lunate ligament. Standard MRI coils are not adequate for the evaluation of the ligaments of the wrist. To maximize the yield from a wrist MRI, high-field strength and highresolution images must be obtained using dedicated wrist coils. Only with such dedicated coils can detailed information be derived regarding the continuity of the scapoid-lunate ligament. Physical examination and wrist arthroscopy remain the gold standards for the evaluation of a torn scaphoid-lunate ligament.
Question 19:
In cases of subacute scaphoid-lunate ligament injury with no arthrosis, all of the following are acceptable options except:
Options:
- Herbert screw (reduction association of the scapholunate)
- Scaphotrapeziotrapezoid (STT) fusion
- Scaphoid-lunate ligament reconstruction using bone-ligament-bone autograft
- Allograft ligament
- Repair with capsulodesis
Correct Answer: Scaphotrapeziotrapezoid (STT) fusion
Explanation:
In cases of subacute scaphoid-lunate ligament injury without arthrosis, it is acceptable to attempt reconstruction with bone anchors, allograft ligament repair, capsulodesis, bone-ligament-bone autograft, and the RASL procedure with a Herbert screw. In the presence of localized arthritis, one might consider one of the limited wrist fusions such as scaphotrapeziotrapezoid fusion.
Question 20:
Mallet finger injuries refer to:
Options:
- Fractures of the bony tuft
- Flexor tendon injuries
- Lack of conjoined tendon continuity at the distal interphalangeal (DIP) joint
- Fractures of the middle phalanx
- Intrinsic tightness
Correct Answer: Lack of conjoined tendon continuity at the distal interphalangeal (DIP) joint
Explanation:
Mallet finger injuries may be associated with fractures of the bony tuft, fractures of the middle phalanx, flexor tendon injuries, and intrinsic tightness. However, mallet injuries refer to lack of continuity at the DIP joint.
Question 21:
In mallet finger injuries, the distal phalanx posture is:
Options:
- Hyperextended
- Flexed
- Neutral
- Radially deviated
- Ulnarly deviated
Correct Answer: Flexed
Explanation:
The characteristic deformity is â droopingâ at the distal interphalangeal (DIP) joint. The DIP is flexed. It is not hyperextended, neutral, or deviated.
Question 22:
Mallet finger injuries are typically:
Options:
- Secondary to hyperextension injuries
- Secondary to forced flexion injuries
- Secondary to torsion injuries
- Secondary to fingertip amputations
- Asymptomatic
Correct Answer: Secondary to hyperextension injuries
Explanation:
Mallet finger usually results from a blow to the tip of the extended finger. This forces distal phalanx flexion and disruption of the extensor mechanism at the distal interphalangeal joint. Open injuries to the extensor mechanism can also cause mallet finger.
Question 23:
Treatment of a type I mallet finger is typically closed. This involves:
Options:
- C ast immobilization of the affected digit in extension
- Dorsal block splint of the affected digit
- Early active motion of the affected joint
- Splinting of the affected distal interphalangeal joint (DIP) joint in flexion
- Splinting of the affected DIP joint in extension
Correct Answer: Splinting of the affected distal interphalangeal joint (DIP) joint in flexion
Explanation:
Cast immobilization is excessive and will cause undue stiffness in the affected finger. Dorsal blocking splints, splinting in flexion, and early active motion are contraindicated in these injuries. Only the affected joint should be splinted in extension.
Question 24:
Type I mallet finger injuries must be immobilized constantly for a minimum of:
Options:
- 4 weeks
- 5 weeks
- 6 weeks
- 7 weeks
- 8 weeks
Correct Answer: 8 weeks
Explanation:
Eight weeks of immobilization is preferred. If the finger is immobilized for a shorter period of time, the clock is reset and immobilization is started again.
Question 25:
The most common mallet finger injuries are:
Options:
- Type I
- Type II
- Type III
- Type IV
- Type V
Correct Answer: Type I
Explanation:
Type I mallet injuries are by far the most common mallet injuries. There is no such classification as a type V injury.
Question 26:
On physical examination, a mallet finger assumes a:
Options:
- Resting flexed posture with active and passive extension
- Resting flexed posture without passive extension
- Resting flexed posture without active extension
- Resting flexed posture without active or passive extension
- Resting flexed posture with active extension
Correct Answer: Resting flexed posture with active and passive extension
Explanation:
The distal phalanx assumes a resting flexed posture. The patient is not able to actively extend the fingertip, but it can be passively extended.
Question 27:
The following mallet finger injuries always require tendon repair:
Options:
- Type I and type II
- Type II and type III
- Type III and type IV
- Type IV and type V
- Type I and type IV
Correct Answer: Type II and type III
Explanation:
Type II and III injuries have absolute requirements for tendon repair as there is a laceration or loss of tendon substance.
Question 28:
After placing a type I mallet finger in a splint at the initial visit, next follow- up should be:
Options:
- The following day
- In 1 week
- In 2 weeks
- In 1 month
- At the end of the 8-week regimen
Correct Answer: In 1 week
Explanation:
After placement of the splint, the patient should follow-up in the next week to make sure the finger is still maintained in full extension. Loosening of the splint will occur as swelling decreases.
Question 29:
The most common bone tumor of the upper extremity is:
Options:
- Enchondroma
- Osteoblastoma
- Osteochondroma
- Giant cell tumor
- C hondromyxoid tumor
Correct Answer: Osteochondroma
Explanation:
Osteochondromas are the most common primary benign bony tumors.
Question 30:
The most common benign bone tumor of the hand is:
Options:
- Enchondroma
- Osteoblastoma
- Osteochondroma
- Giant cell tumor
- C hondromyxoid tumor
Correct Answer: Enchondroma
Explanation:
Unlike the entire upper extremity, enchondromas are the most common tumors of the hand.
Question 31:
Osteochondromas are benign but can have a malignant transformation in which of the following cases:
Options:
- Diaphyseal achalasia
- Ollierâ s disease
- Osteochondromatosis malignant transformans
- Osteochondroma larger than 5 cm
- Mafucci's syndrome
Correct Answer: Diaphyseal achalasia
Explanation:
Diaphyseal achalasia, also known as multiple hereditary exostoses, has a risk of malignant degeneration in up to 25% patients. Olliers disease and Mafucciâ s syndrome are associated with enchondromas. There is no lesion called an osteochondromatosis malignant transformans.
Question 32:
The risk of malignant transformation in patients with multiple hereditary exostoses is:
Options:
- 0%
- Less than 1%
- 1% to 2%
- Greater than 5%
- 0.5% to 25%
Correct Answer: 0%
Explanation:
The rate of malignant transformation in patients with multiple hereditary exostoses is variable and is generally reported between 0.5% to 25%.
Question 33:
Recurrence of osteochondroma is likely if:
Options:
- The cartilage cap is incompletely excised
- The overlying bursa is incompletely excised
- The bony stalk is incompletely excised
- The tumor is incompletely excised
- Its connection with the medullary canal is not obliterated
Correct Answer: The cartilage cap is incompletely excised
Explanation:
The cartilaginous portion of an osteochondroma is the neoplastic part; its complete excision is essential to avoid recurrences.
Question 34:
Malignant transformation of osteochondroma commonly occurs to:
Options:
- High-grade osteosarcoma
- High-grade chondrosarcoma
- Low-grade chondrosarcoma
- Low-grade osteosarcoma
- Parosteal osteosarcoma
Correct Answer: Low-grade chondrosarcoma
Explanation:
Osteochondroma is a cartilaginous tumor and malignant transformation is to a low-grade chondrosarcoma.
Question 35:
All of the following suggest a possibility of malignant transformation in multiple hereditary exostoses except:
Options:
- Recent onset of pain
- Growth after skeletal maturity
- C artilaginous cap thickness greater than 3 cm
- Soft tissue extension
- C alcific stippling in the cap on radiograph
Correct Answer: C alcific stippling in the cap on radiograph
Explanation:
Stippling on radiographs in the cap is due to calcification and is a common characteristic of cartilaginous tumors.
Question 36:
Enchondromas are commonly involved in which of the following sites:
Options:
- Metacarpals
- C arpus
- Radius
- Ulna
- C lavicle
Correct Answer: Metacarpals
Explanation:
Metacarpals and phalanges are the most common areas of hand involvement, and the hand is involved in 40% to 65% of cases. Enchondromas are also the most common primary benign bone tumor of the hand (90% cases).
Question 37:
The most common forearm deformity in patients with hereditary multiple osteochondromatosis is:
Options:
- Ulnar shortening
- Radial shortening
- Radial head dislocation
- Madelungâ s deformity
- Translocation of carpus
Correct Answer: Ulnar shortening
Explanation:
Ulnar involvement and shortening frequently occurs in patients with hereditary multiples osteochondromatosis because the distal ulnar growth plate is smaller than that of the radius, consequently its length is affected more. The ulnar shortening causes radial bowing or radial head dislocation.
Question 38:
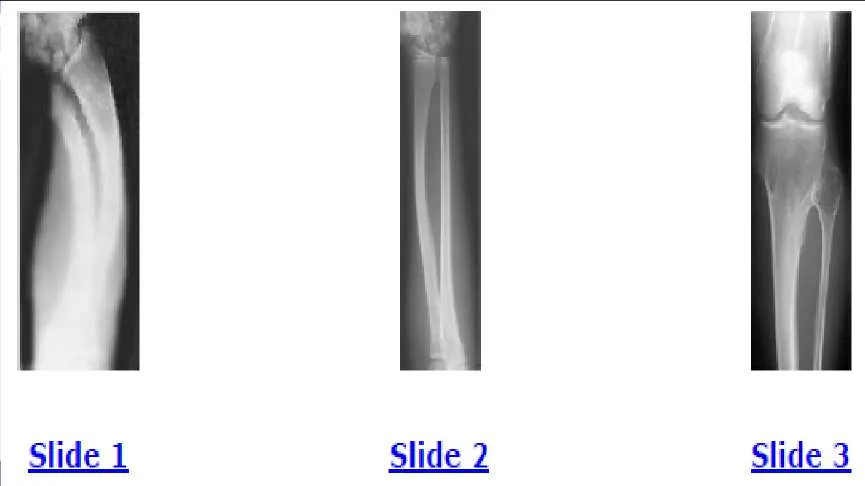
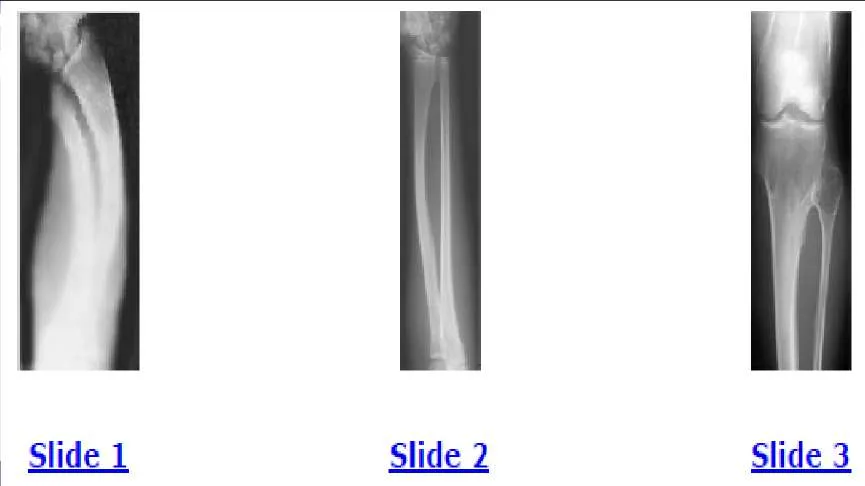
A 12-year-old boy is brought to the clinic by his concerned parents. The boyâ s forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well. The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungâ s deformity and are concerned that the disease is now involving other areas of his body. You order a radiograph of the patientâ s forearm. The anteroposterior radiograph is shown (Slide). The next step is to order a:
Options:
- Skeletal radiograph survey
- Magnetic resonance imaging (MRI)
- Magnetic resonance imaging (MRI) with wrist arthrogram
- Genetic evaluation
- C omputed tomography (C T) scan
Correct Answer: Skeletal radiograph survey
Explanation:
The next step is to order a skeletal survey to rule out involvement of other areas.
Question 39:
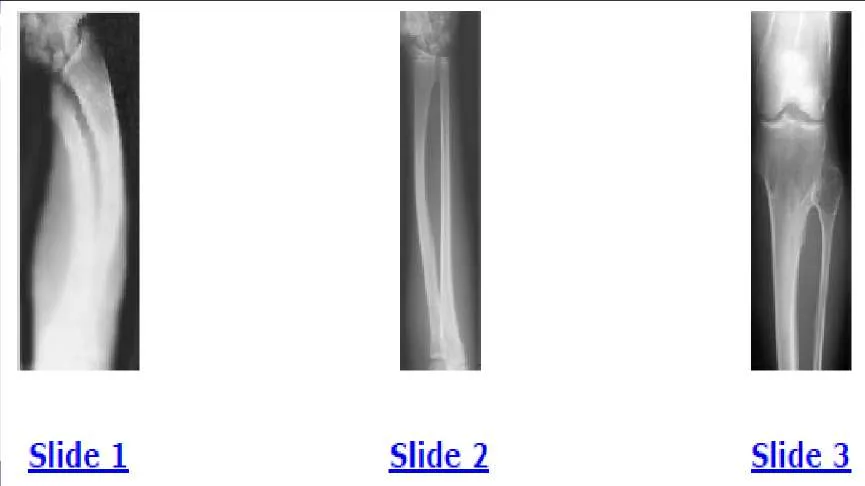
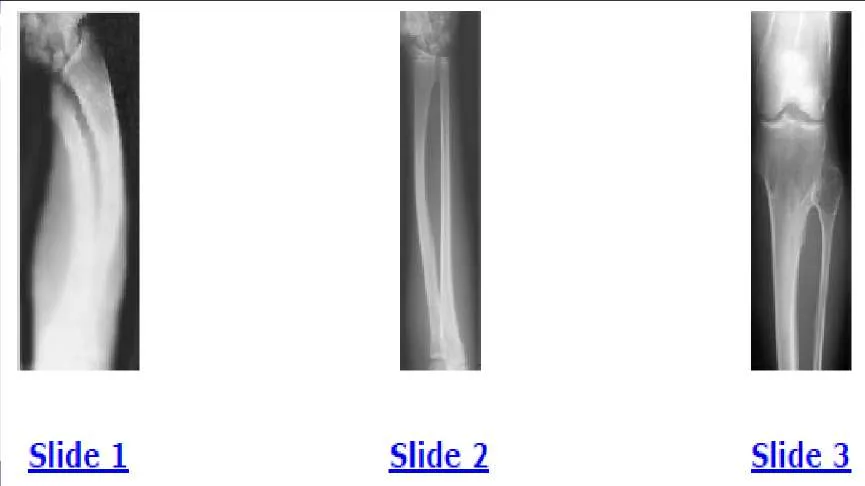
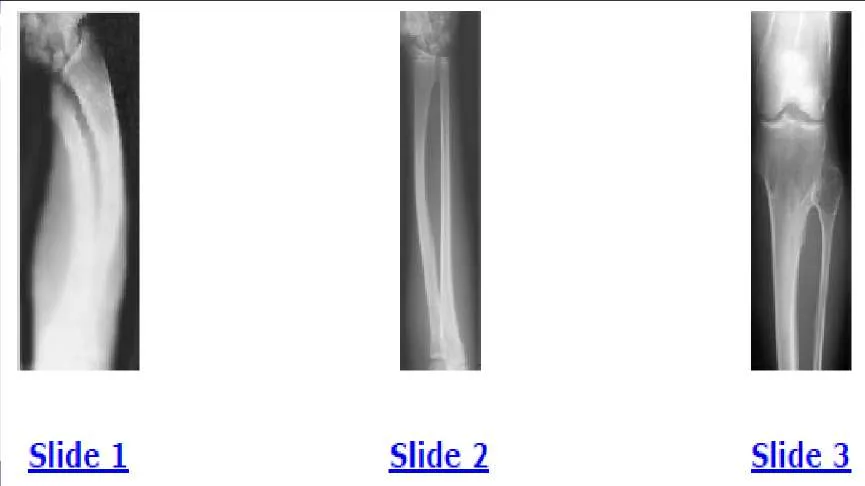
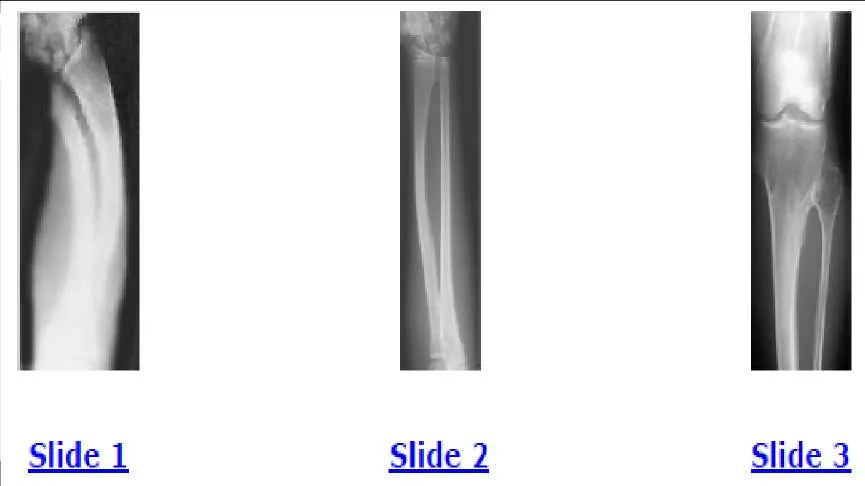
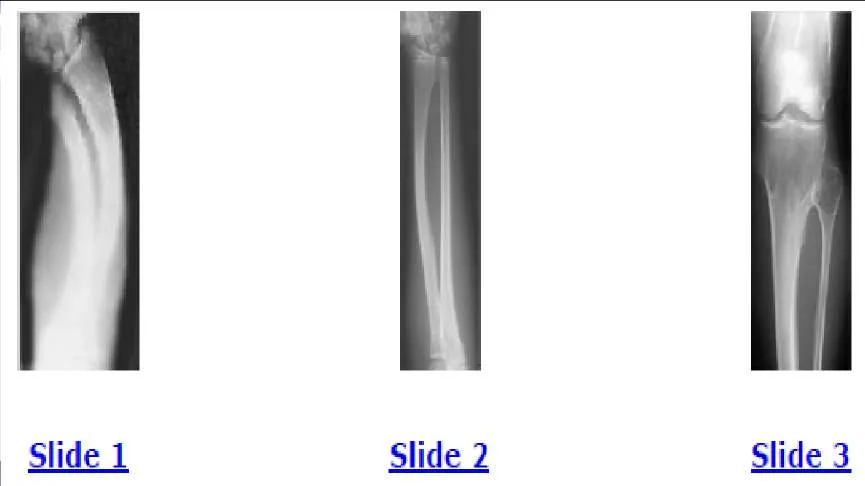
A 12-year-old boy is brought to the clinic by his concerned parents. The boyâ s forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well. The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungs deformity and are concerned that the disease is now involving other areas of his body. An immediate appointment for magnetic resonance imagine (MRI) and computed tomography (C T) scan are not available, and a genetic evaluation has been carried out previously. As you await the report from the geneticist office, you decide to get a skeletal radiograph series on the patient. The radiograph of the opposite forearm (Slide 1) and right leg are shown (Slide 2). You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 3). Your suspected diagnosis is:
Options:
- Diaphyseal achalasia
- Madelungâ s deformity
- Multiple enchondromatosis
- Multiple epiphyseal dysplasia
- Infection
Correct Answer: Diaphyseal achalasia
Explanation:
Diaphyseal achalasia, also called multiple hereditary exostoses, classically presents in a young individual with multiple sites of involvement. The more involved the disease, the more likely hand involvement becomes. Forearm involvement is also common. The radius is bowed due to the shortened ulna. The risk of radial head dislocation is higher if the radius does not bow. While infection or traumatic injury could have produced early physeal arrest as seen in the first radiograph, presence of lesions elsewhere indicates multiple hereditary exostoses and should be investigated with skeletal surveys. Multiple epiphyseal dysplasia is not a possible diagnosis as only the ulna is involved in the first radiograph and radius alone in the left forearm. No enchondromas are present.
Question 40:
A 12-year-old boy is brought to the clinic by his concerned parents. The boys forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well. The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungs deformity and are concerned that the disease is now involving other areas of his body. You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 1). The childâ s skeletal radiograph survey is also presented (Slide 2 and Slide 3). The genetic pattern seen in patients with this type of presentation is:
Options:
- Autosomal recessive
- Autosomal dominant
- Sex-linked recessive
- Sex-linked dominant
- Sporadic
Correct Answer: Autosomal dominant
Explanation:
Multiple hereditary exostoses is inherited in an autosomal-dominant manner with 90% penetrance.
Question 41:
A 12-year-old boy is brought to the clinic by his concerned parents. The boy s forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well. The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungs deformity and are concerned that the disease is now involving other areas of his body. You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 1). The childâ s skeletal radiograph survey is also presented (Slide 2 and Slide 3). Which of the following areas is unlikely to be involved:
Options:
- Phalanges
- Pelvis
- C lavicle
- Femur
- Talus
Correct Answer: C lavicle
Explanation:
The clavicle is a membranous bone, and osteochondromas do not arise in membranous bones.
Question 42:
A 12-year-old boy is brought to the clinic by his concerned parents. The boyâ s forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well. The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungâ s deformity and are concerned that the disease is now involving other areas of his body. You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 1). The childâ s skeletal radiograph survey is also presented (Slide 2 and Slide 3). The chance of hand involvement in this child is:
Options:
- 0%
- 10%
- 25%
- Greater than 25%
- Undetermined
Correct Answer: 25%
Explanation:
The hand is involved in 30% to 80% of cases.
Question 43:
A 12-year-old boy is brought to the clinic by his concerned parents. The boyâ s forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well. The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungs deformity and are concerned that the disease is now involving other areas of his body. You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 1). The childâ s skeletal radiograph survey is also presented (Slide 2 and Slide 3). The most likely complication in this child is:
Options:
- Malignant degeneration
- C arpal translocation
- Posterior interosseous neuropathy (PIN) palsy
- Peroneal nerve palsy
- Elbow dislocation
Correct Answer: C arpal translocation
Explanation:
Ulnar carpal translocation occurs due to the steep radial articular angulation that occurs due to the tethering effect of a shortened ulna and is already apparent in early stages in the first radiograph. While peroneal palsy is possible due to a proximal fibula lesion, it is less common. Malignant transformation occurs, risk varies with families.
Question 44:
A 12-year-old boy is brought to the clinic by his concerned parents. The boys forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well. The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungs deformity and are concerned that the disease is now involving other areas of his body. You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 1). The childâ s skeletal radiograph survey is also presented (Slide 2 and Slide 3). The difference between Madelungâ s deformity and this boyâ s condition is:
Options:
- The ulna is shorter
- The radius is shorter
- There is radial head dislocation
- There is bilateral involvement
- It is not congenital
Correct Answer: The ulna is shorter
Explanation:
The ulna is elongated or dorsally subluxed in Madelung's deformity.
Question 45:
A 12-year-old boy is brought to the clinic by his concerned parents. The boys forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well. The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungs deformity and are concerned that the disease is now involving other areas of his body. You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 1). The childâ s skeletal radiograph survey is also presented (Slide 2 and Slide 3). All of the following are acceptable options, either alone or in combination, for management of this childâ s condition, except:
Options:
- Excision of osteochondromas
- Ulnar lengthening
- Hemiphyseal stapling
- Radial osteotomy
- Observation
Correct Answer: Hemiphyseal stapling
Explanation:
Although hemiphyseal stapling is an acceptable option to correct radial articular angulation, in this boy the distal radial physis is already fused as is seen in the first radiograph.
Question 46:
A 12-year-old boy is brought to the clinic by his concerned parents. The boys forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well. The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungs deformity and are concerned that the disease is now involving other areas of his body. You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 1). The childâ s skeletal radiograph survey is also presented (Slide 2 and Slide 3). Which of the following is not true regarding the possibility of malignant degeneration in this child:
Options:
- There is a risk of up to 25%
- Bone scan can differentiate
- Most common secondary malignancy is chondrosarcoma
- Risk of malignancy varies between families
- Malignant change occurs in adulthood
Correct Answer: Bone scan can differentiate
Explanation:
Bone scan cannot differentiate between an active lesion and a malignant transformation.
Question 47:
Horners syndrome includes all of the following except:
Options:
- Miosis
- Anhidrosis
- Enophthalmosis
- Exophthalmosis
- Diplopia
Correct Answer: Exophthalmosis
Explanation:
Horners syndrome is caused by disruption of sympathetic innervation and is characterized by enophthalmosis, not exophthalmosis. Other symptoms include anhidrosis, miosis, and ptosis.
Question 48:
Axonotmesis involves injury to the:
Options:
- Epineurium
- Endoneurium
- Perineurium
- Axon
- Vasonervorum
Correct Answer: Axon
Explanation:
Axontmesis, as described in Seddonâ s classification, implies injury to the axon and myelin sheath. Neurontmesis involves injury to all three layers.
Question 49:
All of the following may be seen with preganglionic lesion except:
Options:
- Horners syndrome
- Hemidiaphragmatic palsy
- Positive histamine test
- Tinelâ s sign
- Root avulsion sleeve on myelogram
Correct Answer: Tinelâ s sign
Explanation:
Tinels sign is seen with postganglionic lesions.
Question 50:
Weakness is not seen with root avulsion in the:
Options:
- Rhomboids
- Serratus anterior
- Supraspinatus
- Trapezius
- Infraspinatus
Correct Answer: Trapezius
Explanation:
The trapezius is innervated by spinal accessory nerve and thus will not be involved in a brachial plexus lesion. In the case of a preganglionic lesion, all muscles innervated by the nerve roots will be affected.