Masterclass: Flexor Carpi Ulnaris Transfer for Spastic Wrist Flexion Deformity
Key Takeaway
This masterclass details the Flexor Carpi Ulnaris (FCU) transfer for spastic wrist flexion deformity in cerebral palsy. We meticulously cover patient selection, comprehensive anatomy, step-by-step intraoperative execution including FCU mobilization and ECRB transfer using the Pulvertaft weave, and critical pearls for optimal tensioning. Postoperative rehabilitation and complication management are also thoroughly discussed for maximal functional outcomes.
Introduction and Epidemiology
Cerebral palsy represents a heterogeneous group of primary central nervous system dysfunctions that lead to significant functional impairment due to secondary peripheral manifestations. The upper motor neuron lesion in the developing brain results in a profound loss of normal supraspinal inhibition of tone, manifesting primarily as spasticity. Furthermore, patients exhibit a loss of selective motor control resulting in weakness, and impaired coordination of muscle activity frequently presenting as athetosis or dystonia. Among the various phenotypic presentations, spastic hemiplegia is the most common subtype for which upper extremity surgical intervention is indicated.
In the upper limb of a patient with spastic hemiplegia, the classic peripheral manifestations follow a predictable pattern dictated by the relative strength of spastic muscle groups. These include shoulder internal rotation, elbow flexion, forearm pronation, wrist flexion with ulnar deviation, finger clenching or swan necking, and the thumb-in-palm deformity. Increased muscle spasticity causes a persistent muscle imbalance across the articular surfaces. In the early stages, this imbalance is dynamic; however, over time, the persistent spasticity induces structural changes within the muscle-tendon unit. This includes sarcomere dropout, extracellular matrix proliferation, and ultimately myostatic contracture.
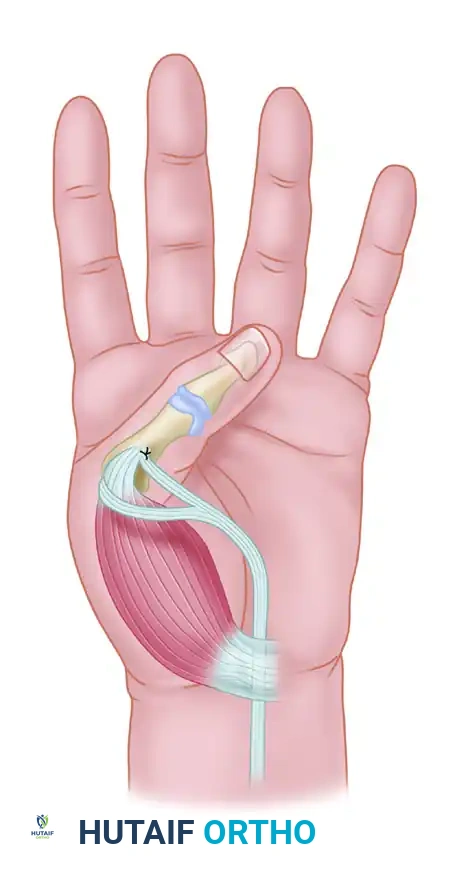
The wrist is the most commonly affected joint in the spastic upper extremity. The resulting wrist flexion and ulnar deviation deformity severely compromises hand function. Grip strength is biomechanically optimized when the wrist is in slight extension (approximately 20 to 30 degrees). When the wrist is forced into severe flexion, the extrinsic digital flexors become actively insufficient, and the extrinsic digital extensors become passively insufficient, rendering the hand functionally useless even if intrinsic selective motor control is preserved. The transfer of the flexor carpi ulnaris to the extensor carpi radialis brevis is a cornerstone procedure designed to rebalance the wrist, augment extension power, and remove the primary deforming flexion force.
Surgical Anatomy and Biomechanics
A thorough understanding of wrist biomechanics and the vector forces of the crossing musculature is requisite for successful tendon transfer surgery. Five primary wrist motors control the spatial position of the radiocarpal and midcarpal joints. The three principal wrist extensors are the extensor carpi radialis brevis, the extensor carpi radialis longus, and the extensor carpi ulnaris. The two primary wrist flexors are the flexor carpi radialis and the flexor carpi ulnaris.
Secondary forces are exerted by the extrinsic digital and thumb musculature. The flexor digitorum profundus, flexor digitorum superficialis, and flexor pollicis longus cross the volar aspect of the wrist and exert a potent flexion moment. Conversely, the extensor pollicis longus, extensor indicis proprius, extensor digitorum communis, and extensor digiti minimi exert a wrist extension moment.

Each muscle crossing the wrist joint possesses a specific physiological cross sectional area and a moment arm, which together define its vector force for flexion, extension, radial deviation, and ulnar deviation. In the setting of cerebral palsy, the flexor carpi ulnaris consistently demonstrates the greatest pathological spasticity and possesses the largest flexion and ulnar deviation vector. The flexor carpi ulnaris inserts onto the pisiform, hook of the hamate, and the base of the fifth metacarpal, providing a massive mechanical advantage for wrist flexion.
When flexor carpi ulnaris spasticity overpowers the weakened and elongated extensor carpi radialis brevis and extensor carpi radialis longus, the wrist is driven into the classic flexion and ulnar deviation posture. The flexor carpi ulnaris is uniquely suited for transfer because of its substantial power and its excursion. The absolute excursion of the flexor carpi ulnaris is approximately 33 millimeters, which closely matches the 30 millimeter excursion requirement of the extensor carpi radialis brevis. By transferring the flexor carpi ulnaris to the extensor carpi radialis brevis, the surgeon accomplishes two biomechanical goals simultaneously. First, the primary deforming force driving wrist flexion and ulnar deviation is eliminated. Second, the transferred muscle unit augments central wrist extension, placing the hand in a functional position to optimize digital flexor mechanics.
Indications and Contraindications
Patient selection is the most critical determinant of success in flexor carpi ulnaris transfer surgery. The surgeon must meticulously differentiate between dynamic spasticity and fixed myostatic contracture. In the early stages of spastic hemiplegia, the joints remain supple with full passive range of motion. Surgical intervention is ideally timed after the child has achieved sufficient neurological maturity to participate in postoperative rehabilitation but before the onset of fixed skeletal deformity or irreversible joint contracture. This window typically occurs between six and twelve years of age.
The primary indication for flexor carpi ulnaris transfer is a dynamic wrist flexion deformity that interferes with the functional use of the hand, specifically when the patient demonstrates preserved selective motor control of the digits but cannot position the wrist in space to utilize that control.
Operative vs Non Operative Indications
| Clinical Scenario | Recommended Management Strategy | Rationale and Biomechanical Considerations |
|---|---|---|
| Dynamic deformity with full passive ROM in child under 5 | Non Operative | Serial casting, orthoses, and targeted botulinum toxin A injections to delay surgical intervention until neurological maturity allows for motor relearning. |
| Zancolli Group 1 or 2A with functional deficits | Operative | Flexor carpi ulnaris transfer to extensor carpi radialis brevis is highly indicated to augment extension and remove the deforming force. |
| Zancolli Group 2B with severe flexor tightness | Operative | Requires concomitant fractional lengthening of the flexor digitorum superficialis and flexor digitorum profundus alongside the tendon transfer. |
| Fixed radiocarpal joint contracture with skeletal deformity | Operative Salvage | Tendon transfer alone will fail. Requires proximal row carpectomy or total wrist arthrodesis to achieve a functional position. |
| Severe athetosis or dystonia as primary movement disorder | Non Operative | Tendon transfers in the setting of severe athetosis yield unpredictable results and frequently lead to reversal of the deformity. |
Contraindications include profound cognitive impairment precluding adherence to postoperative rehabilitation, severe unremitting athetosis, lack of any voluntary finger extension, and fixed bony deformities that cannot be passively corrected to neutral. In cases of fixed joint contracture, soft tissue balancing alone is insufficient, and osseous procedures such as wrist arthrodesis must be considered.
Pre Operative Planning and Patient Positioning
Comprehensive preoperative clinical evaluation dictates the specific surgical blueprint. The cornerstone of this evaluation is the Zancolli classification of the spastic wrist, which categorizes patients based on their capacity for active digital extension relative to wrist position.
Clinical Evaluation and Zancolli Classification
The Zancolli classification is divided into three primary groups.
Group 1 patients can actively extend their fingers with the wrist held in a neutral position. These patients have excellent selective motor control and are ideal candidates for isolated flexor carpi ulnaris transfer.
Group 2 patients can actively extend their fingers, but only when the wrist is allowed to drop into flexion. This group is subdivided into Group 2A, where active finger extension is possible with the wrist flexed less than 20 degrees, and Group 2B, where active finger extension requires wrist flexion greater than 20 degrees. Group 2B patients typically require concomitant fractional lengthening of the extrinsic digital flexors to prevent a reciprocal finger flexion contracture once the wrist is extended.
Group 3 patients possess no active finger extension regardless of wrist position, indicating severe loss of selective motor control or profound fixed contractures. Tendon transfer in Group 3 is generally contraindicated or reserved strictly for hygiene and cosmetic purposes.

Diagnostic modalities such as dynamic electromyography can be utilized to confirm the phase activity of the flexor carpi ulnaris, though the clinical examination remains paramount. Diagnostic blocks using botulinum toxin A injected into the flexor carpi ulnaris can temporarily simulate the postoperative state, allowing the surgeon to unmask underlying weakness in the digital extensors or evaluate the potential functional gains of an extended wrist.
Patient Positioning and Preparation
The patient is placed in the supine position on the operating table. A radiolucent hand table attachment is secured to the operative side. A well padded pneumatic tourniquet is applied to the proximal arm. The entire upper extremity is prepped and draped in a standard sterile fashion, allowing access from the mid humerus to the fingertips. Loupe magnification is highly recommended for the meticulous dissection required to preserve the motor branches of the ulnar nerve during muscle mobilization.
Detailed Surgical Approach and Technique
The surgical execution of the flexor carpi ulnaris to extensor carpi radialis brevis transfer requires precise soft tissue handling, respect for internervous planes, and rigorous biomechanical tensioning. The procedure is divided into harvest, routing, and fixation.
Incision and Flexor Carpi Ulnaris Harvest
A longitudinal incision is made along the volar ulnar aspect of the distal forearm, extending proximally from the proximal wrist crease for approximately 6 to 8 centimeters. The incision is placed directly over the palpable tendon of the flexor carpi ulnaris. Subcutaneous tissues are bluntly dissected, taking care to identify and protect the dorsal sensory branch of the ulnar nerve, which typically emerges from beneath the flexor carpi ulnaris approximately 5 to 8 centimeters proximal to the pisiform.
The fascial sheath of the flexor carpi ulnaris is incised longitudinally. The tendon is traced distally to its insertion on the pisiform. A right angle clamp is passed deep to the tendon, and it is sharply detached directly off the proximal pole of the pisiform to maximize tendon length.

Muscle Mobilization and Nerve Preservation
Once detached, the flexor carpi ulnaris tendon is secured with a locking Krackow suture using a non absorbable braided suture. Traction is applied to the tendon to facilitate proximal dissection. The muscle belly must be mobilized extensively to the proximal third of the forearm to ensure a straight line of pull and adequate excursion.
During proximal mobilization, the surgeon must meticulously separate the flexor carpi ulnaris from the underlying ulnar nerve and ulnar artery. The ulnar nerve lies immediately deep to the muscle belly. As dissection proceeds proximally, the segmental motor branches from the ulnar nerve to the flexor carpi ulnaris will be encountered. The distal most fascial attachments and minor vascular pedicles can be ligated, but the proximal motor branches must be strictly preserved to maintain the viability and contractility of the transferred muscle unit.
Preparation of the Recipient Site
A second longitudinal incision, approximately 4 to 5 centimeters in length, is made over the dorsal radial aspect of the distal forearm, centered over the second and third extensor compartments. The extensor retinaculum is exposed. The extensor carpi radialis brevis and extensor carpi radialis longus tendons are identified. The extensor carpi radialis brevis is selected as the recipient tendon because its central insertion on the base of the third metacarpal provides pure wrist extension without the radial deviation moment associated with the extensor carpi radialis longus. The extensor carpi radialis brevis tendon is isolated and cleared of surrounding tenosynovium to prepare for the tendon weave.
Subcutaneous Routing
A wide subcutaneous tunnel is created between the volar ulnar incision and the dorsal radial incision. The tunnel must be routed around the ulnar border of the forearm. It is imperative that the tunnel is created widely to prevent any fascial tethering or constriction of the transferred muscle belly, which would critically impair excursion. A tendon passer is introduced from the dorsal incision, directed subcutaneously around the ulnar border, and retrieved at the volar incision. The flexor carpi ulnaris tendon is grasped and pulled through the tunnel to the dorsal recipient site. The surgeon must verify that the line of pull is direct and that the muscle belly is not twisted.
Tendon Weaving and Tensioning
The integration of the transferred tendon is achieved using a Pulvertaft weave technique. The extensor carpi radialis brevis tendon is incised longitudinally to create a slit. The flexor carpi ulnaris tendon is passed through this slit.

Tensioning is the most critical and technically demanding aspect of the procedure. The forearm is placed in maximal pronation, as this represents the functional position of the hand. The wrist is extended to approximately 30 to 45 degrees, and the fingers are allowed to rest in a natural cascade. The flexor carpi ulnaris is pulled under maximal physiological tension to eliminate all slack in the muscle tendon unit.
While maintaining this tension, the first pass of the Pulvertaft weave is secured with multiple interrupted non absorbable mattress sutures (e.g., 2-0 or 3-0 braided polyester). A minimum of three, and ideally four, orthogonal passes are made through the recipient tendon, securing each pass with robust suture fixation. The goal is to set the tension such that when the hand is released, the wrist rests dynamically in 20 to 30 degrees of extension. If the wrist drops into flexion upon release, the transfer is under tensioned and must be revised immediately. Following secure fixation, the excess tendon is excised, and the wounds are copiously irrigated and closed in layers.
Complications and Management
Despite meticulous surgical technique, complications can arise following flexor carpi ulnaris transfer. These complications are largely related to errors in tensioning, inadequate patient selection, or failure of postoperative immobilization.
Over tensioning of the transfer is a severe complication that results in an iatrogenic extension contracture of the wrist. This forces the extrinsic digital flexors into increased tension, potentially exacerbating a clenched fist deformity and severely impairing the patient's ability to grasp objects. Conversely, under tensioning fails to correct the primary deformity, leading to recurrent wrist flexion and ulnar deviation.
Complications Incidence and Salvage Strategies
| Complication | Estimated Incidence | Etiology | Salvage Strategy and Management |
|---|---|---|---|
| Under tensioning / Recurrent Flexion | 10 to 15 percent | Inadequate intraoperative tensioning, failure of tendon weave, or progressive spasticity. | Revision tendon transfer with proximal advancement of the weave. May require concomitant wrist arthrodesis if skeletal deformity has developed. |
| Over tensioning / Extension Contracture | 5 to 8 percent | Suturing the transfer with the wrist in excessive extension or failing to account for digital flexor tightness. | Z lengthening of the transferred tendon. Intensive physical therapy. fractional lengthening of digital flexors if secondary clenched fist occurs. |
| Ulnar Nerve Neurapraxia | 2 to 5 percent | Excessive traction during proximal mobilization of the FCU muscle belly. | Observation. Usually resolves spontaneously within 3 to 6 months. Gabapentinoids for neuropathic pain. |
| Tendon Rupture or Pullout | Less than 2 percent | Inadequate Pulvertaft weave technique or premature unprotected mobilization. | Immediate surgical re exploration and revision of the tendon weave. Prolonged postoperative immobilization. |
| Unmasking of Digital Flexor Spasticity | 15 to 20 percent | Preoperative failure to recognize Zancolli Group 2B pathology. Wrist extension increases tension on spastic FDS/FDP. | Secondary surgical intervention for fractional lengthening of the flexor digitorum superficialis and profundus. |
Careful preoperative evaluation utilizing the Zancolli classification is the most effective method for preventing the unmasking of digital flexor spasticity. If a patient requires wrist flexion to achieve active finger extension, isolated wrist extension augmentation will predictably result in a functional decline due to a secondary clenched fist.
Post Operative Rehabilitation Protocols
The success of a tendon transfer is equally dependent on the surgical execution and the postoperative rehabilitation protocol. The transferred muscle must heal securely at the recipient site, and the central nervous system must undergo motor relearning to activate the flexor carpi ulnaris in its new role as a wrist extensor.
Immobilization Phase
Immediately following wound closure, the upper extremity is immobilized in a bulky, well padded long arm cast or rigid splint. The forearm is positioned in neutral rotation to slight pronation, the wrist is immobilized in 30 to 45 degrees of extension, and the metacarpophalangeal joints are left free to allow early active digital motion. This position minimizes tension on the transfer site. Absolute immobilization of the wrist is maintained for a minimum of four to six weeks to allow for robust biological incorporation of the tendon weave.
Activation and Motor Relearning Phase
At the four to six week mark, the cast is removed, and a custom fabricated thermoplastic volar wrist splint is provided. The splint maintains the wrist in 30 degrees of extension and is worn at all times except during directed therapy sessions.
Therapy initiates with active assisted range of motion. Because the flexor carpi ulnaris is a phase dependent muscle (active during flexion), the patient must cognitively retrain the muscle to fire during an extension effort. Biofeedback and neuromuscular electrical stimulation are highly valuable adjuncts during this phase. The therapist instructs the patient to attempt wrist flexion (which fires the FCU) while simultaneously attempting to extend the digits. Over time, cortical plasticity allows the patient to voluntarily activate the transfer for wrist extension.
Strengthening and Long Term Maintenance
By eight to ten weeks postoperatively, progressive resistance exercises are introduced. The daytime splint is gradually weaned as active extension power improves. However, nighttime splinting in extension is strictly maintained for a minimum of six to twelve months, and often until skeletal maturity, to prevent the recurrence of dynamic contractures during sleep. Long term follow up is essential, as the growth of the long bones can alter the tension of the muscle tendon units, potentially leading to recurrent imbalance.
Summary of Key Literature and Guidelines
The academic foundation for the flexor carpi ulnaris transfer in cerebral palsy is robust, built upon decades of clinical observation and biomechanical analysis. The original principles of tendon transfer for spasticity were heavily influenced by the work of Green and Banks in the mid 20th century, who established the flexor carpi ulnaris as the premier donor for wrist extension augmentation.
Subsequent biomechanical studies by Brand delineated the precise vector forces and excursion capacities of the forearm musculature, confirming that the flexor carpi ulnaris possesses the optimal physiological cross sectional area to replace the extensor carpi radialis brevis.
The most critical advancement in patient selection was the development of the clinical classification systems by House and Zancolli. The Zancolli classification remains the gold standard guideline for determining the necessity of concomitant digital flexor lengthening. Contemporary outcomes literature consistently demonstrates that appropriately selected patients (Zancolli Group 1 and 2A) experience statistically significant improvements in grip strength, pinch strength, and validated upper extremity functional scores following flexor carpi ulnaris transfer. Furthermore, even in patients with limited selective motor control, the procedure reliably improves the cosmetic appearance of the hand and facilitates palmar hygiene, significantly reducing the burden of care for caregivers.
Current orthopedic guidelines emphasize that surgical intervention should be viewed as one component of a comprehensive, multidisciplinary spasticity management program. Tendon transfers yield the most predictable and durable results when performed prior to the development of fixed articular deformity, highlighting the importance of early referral and diligent longitudinal assessment by the orthopedic surgeon.
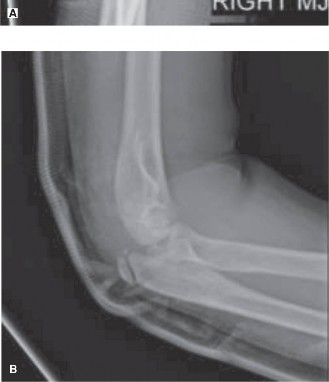
Clinical & Radiographic Imaging




You Might Also Like