Chevron-Type Medial Malleolar Osteotomy: An Intraoperative Masterclass for Talar Dome Lesion Exposure
Key Takeaway
Join us in the OR for a detailed masterclass on the chevron-type medial malleolar osteotomy. This technique provides unparalleled exposure for posteromedial talar dome lesions. We'll meticulously cover preoperative planning, patient positioning, intricate surgical anatomy, step-by-step execution, critical pearls to avoid pitfalls, and comprehensive postoperative care, ensuring optimal outcomes for complex ankle pathologies.
Introduction: Mastering Talar Dome Exposure
Welcome, fellows, to the operating theater. Today, we're tackling a challenging but immensely rewarding procedure: the chevron-type medial malleolar osteotomy. This isn't a procedure we undertake lightly; it's reserved for those elusive, often central or posteromedial lesions of the talar dome that defy conventional arthroscopic or standard arthrotomy approaches. Think of comminuted talar body fractures, complex osteochondral lesions of the talus (OCLTs), or other intra-articular pathologies that demand direct, uncompromised visualization.
The goal here is simple yet profound: to achieve excellent visualization and wide exposure of the tibiotalar joint, particularly the medial talar dome, which is often obscured by the medial malleolus itself. While various techniques exist, including arthroscopy, standard arthrotomy, or even tibial grooving, the medial malleolar osteotomy, especially the chevron variant, offers a stable, reproducible solution. It allows us to perform precise interventions, such as osteochondral allograft insertion or other advanced cartilage replacement techniques, with the confidence that comes from direct access.
However, like any powerful tool, it comes with considerations. Possible disadvantages include the need for prolonged postoperative immobilization, the potential for degenerative ankle arthrosis or nonunion, and the occasional issue of prominent hardware requiring removal. Our aim today is to meticulously execute this procedure, minimizing these risks and maximizing patient outcomes.
Preoperative Planning: The Blueprint for Success
Before we even consider making an incision, thorough preoperative planning is paramount. This isn't just about the osteotomy; it's about the underlying talar lesion or fracture we're addressing.
Imaging and Diagnostic Studies
- Standard Ankle Radiographs: Always our first line. We need AP, lateral, and mortise views to get a baseline assessment of the ankle joint and any gross pathology.
- Magnetic Resonance Imaging (MRI): This is crucial for evaluating osteochondral lesions. An MRI will give us detailed information on the size, location, and extent of articular cartilage involvement. It helps us assess the integrity of the subchondral bone, detect any associated edema, and screen for other articular abnormalities that might influence our approach. For OCLTs, understanding the lesion's depth and surrounding tissue quality is critical for determining suitability for cartilage repair or restoration.
- Computed Tomography (CT) Scans: For comminuted talar body fractures, CT scans are indispensable. They provide a three-dimensional roadmap, allowing us to precisely plan potential fixation strategies, evaluate the extent of articular injury, and identify any cystic lesions. For osteochondral lesions, a CT scan is particularly helpful in determining if the lesion is "contained" within the talar dome, making it an ideal candidate for osteochondral transplantation. We'll use these images for templating our osteotomy and hardware placement.
Patient Counseling
It's vital to have a frank discussion with the patient about the necessity of this approach, the expected recovery, the potential complications (nonunion, nerve injury, hardware prominence), and the prolonged immobilization. Informed consent is not just a formality; it's a critical component of our patient care.
Patient Positioning and Surgical Setup
Let's get our patient ready.
Positioning
The patient will be positioned supine on the operating table. We'll slightly abduct and externally rotate the hip, and gently flex the knee, to allow optimal access to the medial aspect of the ankle. This positioning ensures that the medial malleolus is easily accessible and that fluoroscopy can be brought in without obstruction. A bump under the ipsilateral hip can further facilitate this external rotation and maintain the position.
Tourniquet and Prep
A thigh tourniquet will be applied to ensure a bloodless field, crucial for precise dissection and osteotomy. The limb will then be prepped and draped in the standard sterile fashion, ensuring a wide operative field extending from the mid-calf to the toes.
Fluoroscopy Setup
We'll need our C-arm ready to obtain AP, lateral, and mortise views of the ankle. This is non-negotiable. Fluoroscopy will be used extensively throughout the procedure to confirm osteotomy trajectory, ensure accurate malleolar reduction, and verify hardware placement. Position the C-arm so it can be brought in and out easily without compromising sterility or the surgical field.
Comprehensive Surgical Anatomy: Navigating the Medial Ankle
Fellows, understanding the pertinent anatomy is key to executing this osteotomy safely and effectively. Let's review the critical structures we'll encounter.
The Medial Malleolus
The medial malleolus is the distal-most projection of the tibia. It's subcutaneous on its medial aspect, making it readily palpable. Its medial border is convex, while its lateral surface, which forms part of the ankle mortise, is slightly concave. This is our primary target.
Tendons of the Malleolar Sulcus
Posterior to the medial malleolus, we find the malleolar sulcus. This groove houses two important tendons:
* Posterior Tibialis Tendon: This is the most anterior of the tendons in the sulcus. It's a powerful invertor and plantarflexor of the foot. We must identify and protect it.
* Flexor Digitorum Longus (FDL) Tendon: Lies just posterior to the posterior tibialis tendon.
The Deltoid Ligament
The deltoid ligament is a strong, fan-shaped ligament on the medial side of the ankle. It has both superficial and deep components, originating from the medial malleolus and inserting onto the talus, calcaneus, and navicular. It provides significant medial ankle stability. A crucial aspect of our osteotomy technique is to maintain the superficial and deep attachments of the deltoid ligament to the osteotomized fragment. This preserves its blood supply and facilitates stable re-fixation, contributing to the stability of the malleolar fragment.
Neurovascular Structures
Several critical neurovascular structures are in proximity and demand our utmost respect:
* Saphenous Vein and Nerve: These structures typically run anteromedial to the medial malleolus. The saphenous nerve is a sensory branch of the femoral nerve, providing sensation to the medial aspect of the leg and foot. Injury here can lead to painful neuromas or persistent numbness, a significant patient morbidity. The great saphenous vein is often superficial to the nerve. We must meticulously identify and protect both during our initial incision and superficial dissection.
* Posterior Tibial Neurovascular Bundle: Located more posteriorly, deep to the flexor retinaculum, this bundle contains the posterior tibial artery, posterior tibial nerve, and accompanying veins. While our primary approach is anterior to this bundle, aggressive posterior retraction or an overly posterior osteotomy cut can put these structures at risk. The flexor hallucis longus (FHL) tendon lies most posterior in the deep posterior compartment.
Intraoperative Execution: The Masterclass in Detail
Alright, fellows, let's scrub in. We'll proceed systematically, step by step, ensuring precision and safety at every turn.
1. Incision and Initial Dissection
"Scalpel, please. We're making a standard medial approach, fellows. The incision will be centered directly over the medial malleolus, curving slightly distally towards the navicular. This curvilinear path allows for good exposure and typically heals well."
- Skin Incision: "Make a clean, precise incision through the skin. Now, as we deepen this, remember our anatomy. We need to take extreme care to avoid injury to the saphenous vein and nerve. These structures are often quite superficial, lying just beneath the subcutaneous fat, anteromedial to the malleolus. Use gentle blunt dissection with Metzenbaum scissors or a small hemostat to identify them."
- Subcutaneous Dissection: "Alright, identify the saphenous vein and nerve. We'll gently retract them anteriorly and posteriorly using vessel loops or blunt retractors. This isolation is crucial. Next, incise the deep fascia overlying the medial malleolus. This exposes the periosteum."
- Periosteal Exposure: "Now, elevate the periosteum from the medial malleolus, exposing the bone surface where we plan our osteotomy. Use a periosteal elevator, staying subperiosteal to minimize soft tissue trauma and bleeding. Ensure you have a clear view of the entire medial malleolus, from its proximal base to its distal tip, and extending slightly posteriorly into the malleolar sulcus."
2. Posterior Tibialis Tendon Exposure and Protection
"Next, we need to address the posterior tibialis tendon. This tendon lies directly posterior to the medial malleolus and will be in our path for posterior retraction."
- Tendon Sheath Incision: "Carefully open the posterior tibialis tendon sheath at the level of the ankle mortise. Use a small scalpel or fine scissors. Be precise; we don't want to damage the tendon itself."
- Tendon Retraction: "Once the sheath is open, we can gently retract the posterior tibialis tendon posteriorly. A small, blunt Hohmann retractor or a flexible tendon retractor works well here. The goal is to protect it throughout the osteotomy and subsequent exposure. Ensure the FDL tendon, lying just posterior, is also protected."
3. Osteotomy Planning and Predrilling
"This is a critical phase, fellows. Predrilling for our fixation screws before the osteotomy is a non-negotiable pearl. This ensures accurate reduction and prevents the challenges of trying to drill through an unstable fragment post-osteotomy."
- Fluoroscopic Guidance: "Let's bring in the C-arm. We need perfect AP and lateral views. We're going to plan our chevron osteotomy. The apex will be directed proximally, towards the tibial plafond, and the limbs of the chevron will extend distally from the level of the ankle mortise."
- Osteotomy Trajectory: "In the AP plane, the osteotomy should be angled towards the junction of the medial malleolus and the tibial plafond articular surface. This ensures we maximize the bone-to-bone contact for healing and stability. Mark your osteotomy lines precisely on the bone with a sterile marking pen."
- Predrilling: "Now, using a 2.5-mm drill bit, we're going to predrill the screw holes for our two 4.0-mm partially threaded cancellous screws. Drill these holes across the planned osteotomy line, from the medial malleolus into the tibia. Ensure your drill trajectory is perpendicular to the osteotomy plane for optimal compression. Measure the depth with a depth gauge, and then tap the near cortex if using fully threaded screws, though we'll be using partially threaded today for lag effect. This predrilling step is crucial for achieving a perfect reduction later."
💡 Pearls and Pitfalls
Surgical Warning: Predrilling for Accuracy
"Failing to predrill before the osteotomy is a common pitfall leading to inaccurate reduction and difficulty with screw placement. Always predrill for your fixation screws while the malleolus is still a stable, contiguous part of the tibia. This provides a stable platform for drilling and ensures your screw trajectories are perfectly aligned for re-fixation."
4. Performing the Chevron Osteotomy
"Now for the osteotomy itself. Precision is key here. We'll use a microsagittal saw for the main cuts, then a fine osteotome to complete it cleanly."
- Saw Cuts: "Take the microsagittal saw. Carefully make the two limbs of your chevron osteotomy. Guide the saw blade along your pre-marked lines. The saw should be angled appropriately to create the chevron shape with the apex pointing proximally. Control the depth of your cut meticulously. We want to cut through the cortical bone and most of the cancellous bone, but we must avoid plunging the saw blade into the articular cartilage of the tibiotalar joint."
- Completing the Osteotomy: "Once the saw cuts are almost complete, switch to a fine hand osteotome. Gently tap the osteotome along the remaining bone bridge to complete the osteotomy. This helps to create a clean fracture line and, critically, avoids a 'Kerf' effect within the joint. The 'Kerf' effect refers to the bone loss caused by the saw blade's thickness. If the saw cuts directly into the joint, this gap can lead to articular incongruity and future arthrosis. A controlled osteotome fracture minimizes this."
- Controlled Fracture: "You should feel a distinct give as the osteotomy completes. The medial malleolar fragment is now mobile."

Figure: Intraoperative view of the chevron osteotomy, showing the precise saw cuts and the resulting bone fragment.
5. Malleolar Retraction and Lesion Exposure
"With the osteotomy complete, we can now retract the malleolar fragment to gain our desired exposure."
- Retraction: "Gently grasp the osteotomized medial malleolus fragment with a small bone clamp or a suture passed through its distal tip. Carefully retract it. As you retract, you may need to release any remaining anterior and posterior soft tissues that tether the fragment. Use a small scalpel or electrocautery for this, being mindful of the deltoid ligament attachments."
- Deltoid Ligament Preservation: "This is a critical step: as we retract, we must maintain the superficial and deep attachments of the deltoid ligament to the osteotomized fragment. This preserves the blood supply to the fragment and provides a robust hinge, facilitating stable re-fixation later. Aggressive stripping or detachment of the deltoid ligament can compromise the vascularity of the fragment and contribute to nonunion."
- Achieving Exposure: "Retract the fragment sufficiently to achieve excellent and wide exposure of the talar dome lesion. You should now have an unobstructed view of the central or posteromedial aspect of the talus, allowing for precise intervention."
💡 Pearls and Pitfalls
Surgical Warning: Maintaining Deltoid Integrity
"Compromising the deltoid ligament attachments to the malleolar fragment during retraction is a significant pitfall. This can lead to avascular necrosis or nonunion of the osteotomy. Always aim to preserve these attachments, using them as a hinge for retraction."Surgical Warning: Avoiding Distal Osteotomy Arms
"When planning your chevron, avoid making the exiting areas of the arms of the osteotomy too distal. This can compromise the deltoid ligament insertion and reduce the stability of your osteotomy fragment, making retraction and subsequent fixation more challenging and potentially leading to instability."
6. Addressing the Talar Lesion
"Now that we have this superb exposure, we can proceed with addressing the primary pathology, whether it's a talar body fracture fixation, osteochondral allograft insertion, microfracture, or other cartilage repair technique. This part of the procedure is dictated by the specific lesion and its treatment protocol."
- (At this point, we would perform the necessary intervention on the talar dome.)
7. Osteotomy Reduction and Fixation
"Once the talar lesion has been addressed, it's time to reduce and fix our medial malleolar osteotomy. This must be anatomical and stable."
- Anatomical Reduction: "Gently bring the osteotomized fragment back into its anatomical position. Ensure perfect alignment of the bone edges. You should feel it 'seat' back into place. Confirm this anatomical reduction with fluoroscopy in AP, lateral, and mortise views. Any malreduction, even subtle, can lead to articular incongruity and future arthrosis."
- Screw Insertion: "Now, using our predrilled holes, we'll insert the two 4.0-mm partially threaded cancellous screws (Synthes, USA). The partially threaded design allows for a lag effect, providing compression across the osteotomy site, which is crucial for healing. Carefully advance the screws, ensuring they engage the far cortex firmly. We want good compression without overtightening, which could strip the threads or cause a fracture."
- Final Fluoroscopic Check: "Once both screws are in, let's get a final set of fluoroscopic images – AP, lateral, and mortise views. We need to confirm that the osteotomy is perfectly reduced, the screws are in good position, and there's no intra-articular penetration."
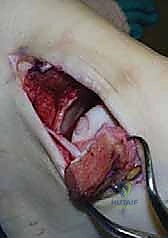
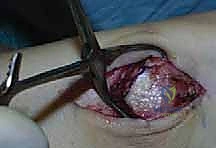
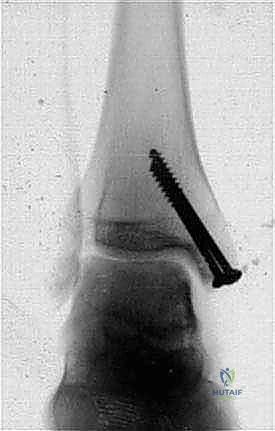
Figure: Postoperative radiographs (AP view) demonstrating stable fixation of the chevron-type medial malleolar osteotomy with two cancellous screws, confirming anatomical reduction.
8. Wound Closure
"With the osteotomy securely fixed, we can now proceed with a layered wound closure."
- Deep Fascia: "Close the deep fascia with absorbable sutures."
- Subcutaneous Tissue: "Reapproximate the subcutaneous tissues."
- Skin Closure: "Close the skin with staples or non-absorbable sutures. Apply a sterile dressing."
Postoperative Care and Complication Management
Our work isn't done when the patient leaves the OR. Postoperative care is critical for successful outcomes.
Postoperative Care Protocol
- Initial Immobilization (0-14 days): The patient will be placed in a plaster splint immediately postoperatively. This provides rigid immobilization to protect the osteotomy and allow initial soft tissue healing.
- Early Range of Motion (10-14 days): Once the wound has sealed and is stable (typically around 10 to 14 days post-op), we'll transition the patient. The splint is removed, sutures/staples are removed, and active range of motion (ROM) exercises are initiated.
- Removable Cast Brace: The patient will be placed in a removable short-leg cast brace. This allows for protected ROM while still providing support.
- Non-Weight Bearing (NWB): Non-weight bearing ambulation is maintained until radiographic evidence confirms maintenance of reduction and early signs of osteotomy union. This typically occurs around 6 weeks postoperatively, at which point repeat radiographs will be obtained to assess healing. Progression to partial and then full weight-bearing will be guided by clinical and radiographic assessment of osteotomy consolidation.
Potential Complications and Management
Despite our best efforts, complications can occur. It's crucial to recognize and manage them effectively.
- Nonunion:
- Incidence: Nonunion rates for medial malleolar osteotomy are reported to be as high as 12%. The chevron-type osteotomy, theoretically, provides excellent stability for fixation, which should reduce this risk.
- Management: If a nonunion is diagnosed (persistent pain, lack of radiographic healing), options include prolonged protected weight-bearing, bone stimulators, or surgical revision with debridement, bone grafting, and more rigid fixation.
- Saphenous Nerve Injury:
- Presentation: This can manifest as medial ankle numbness, paresthesias, or a painful subcutaneous neuroma.
- Management: Initial management is conservative, including observation, nerve blocks, and neuropathic pain medications. If a painful neuroma develops and is refractory to conservative measures, surgical excision or neurolysis may be considered. Prevention through meticulous identification and protection during dissection is key.
- Posterior Tibial Tendon Laceration:
- Presentation: Laceration of the posterior tibial tendon can lead to displacement of the osteotomy, progressive flatfoot deformity, and potentially progressive arthrosis due to altered biomechanics.
- Management: If recognized intraoperatively, immediate primary repair of the tendon is indicated. Postoperatively, if diagnosed, surgical repair may be necessary, often requiring tendon grafting or transfer depending on the extent of the injury and chronicity.
- Degenerative Ankle Arthrosis:
- Presentation: Long-term risk, especially if there was pre-existing articular damage, malreduction of the osteotomy, or significant cartilage damage during the primary procedure.
- Management: Symptomatic management with NSAIDs, activity modification, bracing, injections. If severe, further surgical interventions like ankle arthrodesis or arthroplasty may be considered.
- Hardware Prominence:
- Presentation: The subcutaneous nature of the medial malleolus makes hardware prominence a common issue, causing irritation or pain.
- Management: If symptomatic after osteotomy union, hardware removal can be performed as a secondary procedure.
- Wound Dehiscence or Infection:
- Presentation: Standard surgical wound complications.
- Management: Debridement, antibiotics, wound care, and potentially negative pressure wound therapy.
Outcomes
While specific studies focusing solely on the morbidity of medial malleolar osteotomy are limited, the advantages of excellent visualization and wide exposure for complex talar dome lesions are well-established. When performed meticulously, with careful attention to anatomy, surgical technique, and postoperative care, this procedure allows us to effectively treat challenging intra-articular pathologies, improving patient function and potentially preventing long-term disability.
That concludes our masterclass on the chevron-type medial malleolar osteotomy. Remember, fellows, precision, patience, and a deep understanding of anatomy are your most valuable instruments in the OR.
REFERENCES
-
A retrospective review was performed on 19 patients who underwent medial malleolar osteotomy for the treatment of pathology of the talar dome. 6 Chart review, radiographic examination, and clinical examination were performed in all patients. Fifteen patients had osteochondral lesions of the medial talar dome. All patients failed conservative treatment of these lesions, including a period of immobilization and anti-inflammatory medication. The location of the lesion was in the posterior or central portion of the talar dome in all patients.
-
Alexander AH, Lichtman DM. Surgical treatment of transchondral talar-dome fractures (osteochondritis dissecans). J Bone Joint Surg Am 1980;62A:646–652.
-
Alexander IJ, Watson JT. Step-cut osteotomy of the medial malleolus for exposure of the medial ankle joint space. Foot Ankle Int 1991;11:242–243.
-
Berndt AL, Harty M. Transchondral fractures (osteochondritis dissecans) of the talus. J Bone Joint Surg Am 1959;41A:988–1020.
-
Bryant DD, Siegel MG. OCD of the talus: a new technique for arthroscopic drilling. Arthroscopy 1993;9:238–241.
-
Canale ST, Belding RH. Osteochondral lesions of the talus. J Bone Joint Surg Am 1980;62A:97–102.
-
Cohen BE, Anderson RB. Chevron-type transmalleolar osteotomy: an approach to medial talar lesions. Tech Foot Ankle Surg 2002;1: 158–162.
-
Ferkel RD, Fasulo GJ. Arthroscopic treatment of ankle injuries. Orthop Clin North Am 1994;25:17–32.
-
Flick AB, Gould N. Osteochondritis dissecans of the talus (transchondral fractures of the talus): review of the literature and new surgical approach of medial dome lesions. Foot Ankle 1985;5:165–185.
-
Gepstein R, Conforty B, Weiss RE, et al. Closed percutaneous drilling for osteochondritis dissecans of the talus. Clin Orthop Relat Res 1986;213:197–199.
-
Kristensen G, Lind T, Lavard P, et al. Fracture stage 4 of the lateral talar dome treated arthroscopically using Biofix for fixation. Arthroscopy 1990;6:242–244.
-
McCullough CJ, Venegopal V. OCD of the talus: the natural history. Clin Orthop Relat Res 1979;144:264–268.
-
O’Farrell TA, Costello BG. OCD of the talus: the late results of surgical treatment. J Bone Joint Surg Br 1982;64B:494–497.
-
Ove N, Bosse MJ, Reinert CM. Excision of posterolateral talar dome lesions through a medial transmalleolar approach. Foot Ankle 1989; 9:171–175.
-
Parisien JS. Arthroscopic treatment of osteochondral lesions of the talus. Am J Sports Med 1986;14:211–217.
-
Ray RB, Coughlin EJ. Osteochondritis dissecans of the talus. J Bone Joint Surg Am 1947;29A:697–706.
-
Roden S, Tillegard P, Unanderscharin L. Osteochondritis dissecans and similar lesions of the talus. Acta Orthop Scand 1953;23: 51–52.
-
Scharling M. Osteochondritis dissecans of the talus. Acta Orthop Scand 1978;49:89–94.
-
Thompson JP, Looner RL. Osteochondral lesion of the talus in a sports medicine clinic: a new radiographic technique and surgical approach. Am J Sports Med 1984;12:460–463.
-
Yvars MF. Osteochondral fracture of the dome of the talus. Clin Orthop Relat Res 1976;114:185–191.
-
Three patients had medial malleolar osteotomy performed for exposure during internal fixation of displaced talar dome fractures. One additional patient had curettage and bone grafting of a large medial talar cyst.
-
About 50% of the patients had undergone prior surgery on the affected ankle. Six patients had a total of nine prior arthroscopic procedures. The average age of the patients was 32 years (range 14 to 51). The length of follow-up was 12 months (range 6 to 43).
-
All patients achieved union of the osteotomy both clinically and radiographically. The average time to radiographic union was 7 weeks (range 5 to 12). No failures of fixation were noted.
-
Preoperative and postoperative tibiotalar range of motion was measured. At the last follow-up, only 2 of 19 patients had any loss of motion compared to their preoperative evaluation. This decreased range of motion was about 10 degrees of total arc of motion.
-
Four patients had slight (less than 2 mm) displacement at the osteotomy site. This displacement was noted immediately postoperatively and was felt to be due to technical errors during the bone cuts for the osteotomy. No progressive displacement was noted in these patients. All four patients were asymptomatic at the osteotomy site and no progressive ankle arthrosis was noted. Three patients had symptomatic prominent screws that resulted in hardware removal. All the screws were removed as an outpatient procedure under a local anesthetic without complications. No postoperative complications, including infection, nonunion, or delayed wound healing, were noted in the study population.
You Might Also Like