Osteochondral Allograft Transplantation: A Masterclass in Cartilage Restoration
Key Takeaway
This masterclass details osteochondral allograft transplantation for focal cartilage defects. Fellows will learn patient selection, comprehensive knee anatomy, and meticulous intraoperative techniques from incision to graft delivery. We cover preoperative planning, precise sizing, recipient site preparation, and donor graft handling, emphasizing critical pearls for optimal outcomes. Postoperative care and complication management are also discussed.
Introduction and Epidemiology
Articular cartilage lesions are focal, usually isolated, cartilage defects that may be either highly symptomatic or incidentally discovered during arthroscopy or advanced imaging. The management of these lesions remains one of the most challenging domains in orthopedic surgery due to the inherently poor healing capacity of hyaline cartilage. Small, full-thickness chondral defects may heal adequately with mechanically inferior fibrocartilage (composed primarily of type I collagen) following marrow stimulation techniques such as microfracture. However, larger defects, particularly those exceeding 2 to 3 square centimeters or those involving significant subchondral bone loss, often require advanced cartilage transplant surgery to restore the damaged chondral surface and underlying osseous architecture.

Osteochondritis dissecans (OCD) represents a distinct subset of osteochondral lesions occurring primarily in adolescents and young adults. The natural history and management ramifications for juvenile OCD differ significantly from those of adult presentations. While juvenile OCD often responds to conservative management or simple fixation due to open physes and robust healing potential, adult OCD or unhealed juvenile lesions frequently progress to structural failure, necessitating restorative procedures.

The utilization of fresh osteochondral allograft (OCA) transplantation has emerged as a premier surgical solution for massive, symptomatic osteochondral defects. By transplanting mature, viable hyaline cartilage attached to a structurally intact subchondral bone base, OCA directly addresses both the chondral and osseous pathology. This procedure circumvents the donor-site morbidity associated with osteochondral autograft transfer (OATS) and provides a biomechanically superior articular surface compared to cell-based therapies or marrow stimulation.

Surgical Anatomy and Biomechanics
Composition of Articular Cartilage
Normal articular cartilage is an avascular, aneural, and alymphatic tissue composed predominantly of water (65% to 80% by weight) and a highly organized extracellular matrix. The structural framework is heavily reliant on type II collagen, which provides tensile strength, and proteoglycans (primarily aggrecan), which provide compressive resistance through osmotic swelling pressure. Chondrocytes, the resident cells responsible for producing and maintaining this extracellular matrix, are of mesenchymal stem cell origin and constitute only 1% to 2% of the tissue volume.

Zonal Architecture
The complex biomechanical properties of hyaline cartilage are dictated by its distinct zonal architecture:
1. Superficial Zone: Characterized by densely packed collagen fibers aligned parallel to the articular surface, providing high tensile strength and resistance to shear forces.
2. Transitional Zone: Contains thicker collagen fibers oriented obliquely, serving as a biomechanical bridge.
3. Deep Zone: Features thick collagen fibers oriented perpendicular to the joint surface, anchoring the cartilage to the underlying bone and providing maximum resistance to compressive loads.
4. Calcified Cartilage Zone: Separated from the deep zone by the tidemark, this layer transitions into the subchondral bone plate.

Topographic Pathology and Mechanism of Injury
Osteochondral lesions may occur in all three compartments of the knee, but specific etiologies dictate classic anatomic locations. Traumatic lesions are frequently caused by compaction or shearing mechanisms. For instance, an anterior cruciate ligament (ACL) tear often results in a lateral-based osteochondral injury due to the classic pivot-shift compaction mechanism (lateral femoral condyle impacting the posterolateral tibial plateau). Conversely, chondral defects resulting from a lateral patellar dislocation are typically found on the medial patellar facet or the lateral aspect of the femoral trochlea due to shearing forces during dislocation or spontaneous reduction.

Atraumatic lesions, such as those seen in osteonecrosis or OCD, present differently. Classically, osteochondritis dissecans occurs at the lateral aspect of the medial femoral condyle. The precise etiology of OCD remains uncertain; traumatic, inflammatory, developmental, and ischemic causes have all been proposed but definitively unproven. Degenerative lesions, typically seen in older populations, represent a diffuse breakdown of the matrix rather than a focal osteochondral defect amenable to isolated allografting.

Indications and Contraindications
Patient selection is paramount for the success of fresh osteochondral allograft transplantation. Candidates are typically active, young to middle-aged adults presenting with focal, symptomatic, full-thickness osteochondral defects. Many of these patients have a history of previous knee surgery and failed attempts at cartilage regeneration by other methods (e.g., microfracture, autologous chondrocyte implantation, or osteochondral autograft transplant).

Primary Indications
Fresh OCA is indicated for large (>2 cm²) full-thickness chondral or osteochondral defects. It is particularly valuable in cases with underlying bony changes, deficient subchondral bone, or significant cystic formation, as cell-based therapies (like ACI) cannot adequately address structural osseous voids. Adult OCD, post-traumatic osteochondral defects, and localized osteonecrosis (e.g., secondary to corticosteroid use or spontaneous osteonecrosis of the knee) are classic indications.

Contraindications
Absolute contraindications include diffuse, advanced osteoarthritis (e.g., tricompartmental disease), inflammatory arthropathies, active intra-articular infection, and uncorrected mechanical malalignment or ligamentous instability. Failure to identify and address ligamentous deficiency or mechanical malalignment will lead to rapid structural failure of restorative cartilage procedures due to pathologic loading. "Kissing lesions" (bipolar defects on opposing articular surfaces) are generally considered a strong relative contraindication, as outcomes in these scenarios are significantly inferior.

Operative vs Non Operative Management Parameters
| Clinical Parameter | Non-Operative Management | Operative Management (Fresh OCA) |
|---|---|---|
| Patient Age/Status | Juvenile (open physes), low demand | Adult (closed physes), high functional demand |
| Lesion Size | Small (<1-2 cm²), asymptomatic | Large (>2 cm²), failed previous interventions |
| Lesion Depth | Partial thickness, intact subchondral bone | Full thickness, subchondral bone loss/cysts |
| Etiology | Incidental finding, stable juvenile OCD | Symptomatic adult OCD, post-traumatic shear/compaction |
| Mechanical Alignment | Normal or uncorrectable malalignment | Normal, or malalignment correctable via concurrent osteotomy |
| Ligamentous Status | Normal or unstable (unwilling to undergo reconstruction) | Stable, or concurrent ligamentous reconstruction planned |

Pre Operative Planning and Patient Positioning
Clinical Evaluation
Patients with focal osteochondral lesions typically range in age from adolescence to middle age. The clinical presentation is highly variable. Often, the history does not include a specific traumatic episode, and physical findings can be subtle, frequently mimicking meniscal pathology with intermittent pain, catching, and effusion.

Condylar defects typically present with high-impact loading complaints (e.g., pain with running or jumping). Conversely, patellofemoral defects produce anterior knee pain-type complaints, exacerbated by stair climbing, descending, and prolonged sitting (the "theater sign"). Physical examination should note chronic or recurrent effusions, pain at extremes of range of motion, and focal tenderness at the defect site (condyle, patellar facets, or trochlea). In patellofemoral defects, patellar mobility, tracking, and apprehension must be meticulously assessed.

Advanced Imaging and Graft Matching
Appropriate imaging studies are critical. Weight-bearing radiographs (including Rosenberg, Merchant, and long-leg alignment views) assess joint space narrowing and mechanical axis. Mechanical alignment must be quantified; varus or valgus malalignment exceeding 2 to 3 degrees relative to the affected compartment typically necessitates a concomitant unloading osteotomy (High Tibial Osteotomy or Distal Femoral Osteotomy).

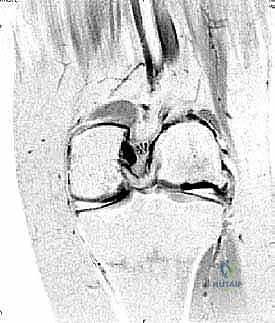
Magnetic Resonance Imaging (MRI) is the gold standard for defining lesion size, depth, and the status of the subchondral bone plate. MRI sequences such as T2 mapping or delayed gadolinium-enhanced MRI of cartilage (dGEMRIC) can evaluate the biochemical integrity of the surrounding cartilage.
Once surgical intervention is elected, pre-operative templating is required to order a size-matched, side-specific fresh osteochondral allograft. The graft must be matched for anterior-posterior dimensions and medial-lateral condylar width. Fresh allografts are typically stored at 4°C and must be utilized within 14 to 28 days of procurement to maximize chondrocyte viability, which is essential for long-term matrix maintenance.

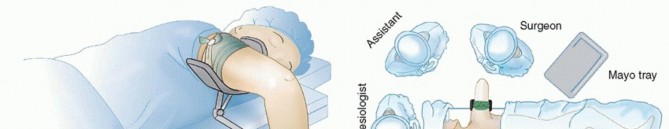
Patient Positioning and Setup
The patient is positioned supine on the operating table. A well-padded tourniquet is applied to the proximal thigh. The operative leg is typically placed in a leg holder or against a lateral post to allow for full range of motion and valgus/varus stress during the procedure. Prophylactic intravenous antibiotics are administered prior to tourniquet inflation.

Detailed Surgical Approach and Technique
Diagnostic Arthroscopy
The procedure begins with a systematic diagnostic arthroscopy to confirm the size and location of the lesion, assess the integrity of the surrounding cartilage, evaluate the opposing articular surface (to rule out bipolar kissing lesions), and address any concomitant intra-articular pathology, such as meniscal tears or loose bodies.

Surgical Exposure
Following arthroscopy, a mini-arthrotomy is performed. A medial parapatellar arthrotomy is utilized for medial femoral condyle and medial trochlear lesions, while a lateral parapatellar arthrotomy is preferred for lateral condyle and lateral trochlear defects. The incision must provide adequate orthogonal access to the lesion, as precise perpendicular instrumentation is critical for the success of the dowel technique.

Recipient Site Preparation
- Sizing the Defect: A cylindrical sizing guide is placed over the defect. The goal is to encompass the entire diseased area while minimizing the removal of healthy surrounding cartilage. Common dowel sizes range from 15 mm to 35 mm in diameter.
- Guide Pin Placement: Once the appropriate size is determined, a central guide pin is drilled strictly perpendicular to the articular surface. Malalignment of this pin will result in a proud or sunken graft, leading to abnormal contact pressures and early failure.
- Reaming: A cannulated reamer is advanced over the guide pin to excavate the diseased cartilage and sclerotic subchondral bone. The depth of reaming is typically between 6 mm and 8 mm—deep enough to reach healthy, bleeding cancellous bone, but shallow enough to avoid excessive structural weakening of the condyle.
- Measurement: The depth of the recipient socket is meticulously measured at four distinct quadrants (12, 3, 6, and 9 o'clock) using a depth gauge. These precise measurements are recorded for graft preparation.

Allograft Preparation
Attention is then turned to the back table, where the fresh osteochondral allograft is prepared under strict aseptic conditions.
1. Securing the Donor Condyle: The donor hemicondyle is secured in a specialized allograft workstation.
2. Topographic Matching: The surgeon identifies a region on the donor condyle that anatomically matches the contour and radius of curvature of the recipient site.
3. Harvesting the Dowel: A coring reamer, matching the exact diameter of the recipient socket, is advanced perpendicular to the donor articular surface. The resulting osteochondral dowel is extracted.
4. Trimming to Depth: The dowel is marked according to the four-quadrant measurements obtained from the recipient socket. The osseous portion of the graft is carefully trimmed using an oscillating saw to match these exact depths.
5. Pulsatile Lavage: This is a critical step. The osseous portion of the graft is subjected to high-pressure pulsatile lavage with normal saline. This removes donor marrow elements, fat, and cellular debris, significantly reducing the immunogenic load and the risk of graft rejection or disease transmission.

Graft Implantation and Fixation
The prepared allograft dowel is introduced into the recipient socket. Due to the exact size matching, insertion is typically achieved via a press-fit mechanism. The graft is gently advanced using an oversized tamp and a mallet. It is imperative to avoid striking the cartilage surface directly with narrow instruments, as this can cause iatrogenic chondrocyte necrosis.

The final position is assessed by palpation. The allograft articular surface must be perfectly flush with the surrounding native cartilage. A graft that is proud by even 1 mm will experience massive shear stresses and fail, while a sunken graft will fail to participate in load-bearing, leading to adjacent cartilage overload. In most cases, the press-fit stability is excellent, and supplemental fixation is unnecessary. If stability is questionable, bioabsorbable pins or headless compression screws may be utilized.

Complications and Management
While fresh osteochondral allografting yields excellent clinical outcomes in properly selected patients, complications can occur and must be managed aggressively to salvage the joint.
Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology / Risk Factors | Management / Salvage Strategy |
|---|---|---|---|
| Graft Subsidence / Non-union | 5% - 10% | Poor initial press-fit, thermal necrosis during reaming, premature weight-bearing | Prolonged NWB, bone grafting, revision OCA, or conversion to Arthroplasty |
| Immunologic Rejection | < 1% | Inadequate pulsatile lavage of donor marrow elements | Debridement, removal of graft, conversion to Unicompartmental or Total Knee Arthroplasty |
| Disease Transmission | Extremely Rare | Contaminated donor tissue (bacterial, viral) | Aggressive I&D, graft removal, targeted intravenous antibiotic/antiviral therapy |
| Arthrofibrosis | 3% - 8% | Prolonged immobilization, poor pain control, inadequate early CPM use | Aggressive physical therapy, manipulation under anesthesia (MUA), arthroscopic lysis of adhesions |
| Subchondral Edema / Pain | 10% - 15% | Altered biomechanics, delayed osseous integration | Protected weight-bearing, NSAIDs, bisphosphonates (off-label), observation (often resolves by 12-18 months) |

Post Operative Rehabilitation Protocols
The post-operative rehabilitation protocol is designed to protect the osseous integration of the graft while providing mechanical stimulation to maintain chondrocyte viability and prevent arthrofibrosis.
Phase 1: Tissue Protection and Early Motion (Weeks 0-6)
- Weight-Bearing: Strict non-weight-bearing (NWB) or toe-touch weight-bearing (TTWB) with crutches.
- Range of Motion: Continuous Passive Motion (CPM) is initiated immediately post-operatively, typically for 6 to 8 hours per day. This cyclic loading is essential for cartilage nutrition via synovial fluid diffusion. The goal is to achieve 90 degrees of flexion by week 2 and full ROM by week 6.
- Bracing: A hinged knee brace locked in extension during ambulation to protect
Clinical & Radiographic Imaging























You Might Also Like