Anterior Cervical Approaches: An Intraoperative Masterclass for Spinal Fellows
Key Takeaway
This masterclass guides fellows through anterior cervical approaches, including Smith-Robinson and Whitesides techniques. We cover comprehensive surgical anatomy, meticulous patient positioning, and granular intraoperative steps from incision to hardware application. Critical pearls, potential pitfalls, and strategies for complication management and postoperative rehabilitation are emphasized, ensuring a thorough understanding of these vital spinal procedures.
Introduction and Epidemiology
The anterior approach to the cervical spine remains one of the most fundamental and versatile exposures in orthopedic spine surgery. First popularized by Smith and Robinson, as well as Cloward, in the 1950s, the anterior cervical approach provides direct access to the ventral column of the cervical spine. This trajectory allows for the direct decompression of neural elements, restoration of cervical lordosis, and robust stabilization through interbody fusion or arthroplasty.
Epidemiologically, the demand for anterior cervical procedures has grown exponentially, driven largely by an aging population presenting with cervical spondylotic myelopathy, radiculopathy, and degenerative disc disease. Furthermore, the anterior approach is frequently utilized in the management of cervical trauma, primary and metastatic neoplasms, and infectious processes such as discitis and osteomyelitis. Understanding the nuanced indications, comprehensive surgical anatomy, and precise execution of these approaches is paramount for the operating surgeon to optimize clinical outcomes and minimize perioperative morbidity.




Surgical Anatomy and Biomechanics
A profound understanding of the complex fascial layers and neurovascular structures of the anterior neck is essential for safe navigation to the cervical spine. The dissection proceeds through an avascular internervous plane, making it an elegant and anatomically sound approach.
Fascial Layers and Musculature
The superficial cervical fascia contains the platysma muscle, which is typically divided in line with the skin incision or split longitudinally depending on surgeon preference. Deep to the platysma lies the deep cervical fascia, which is divided into three primary layers:
1. Investing Layer: Envelops the sternocleidomastoid (SCM) and trapezius muscles.
2. Pretracheal Layer: Encloses the visceral structures of the neck, including the thyroid gland, trachea, and esophagus. It blends laterally with the carotid sheath.
3. Prevertebral Layer: Covers the longus colli and longus capitis muscles, as well as the anterior longitudinal ligament of the spine.
The standard Smith-Robinson approach utilizes the internervous plane between the SCM (innervated by the spinal accessory nerve, Cranial Nerve XI) laterally, and the strap muscles (innervated by the ansa cervicalis) medially.
Neurovascular Structures
The carotid sheath, containing the common carotid artery, internal jugular vein, and vagus nerve, is retracted laterally. The visceral axis (trachea and esophagus) is retracted medially.
The recurrent laryngeal nerve (RLN) is a critical structure in this exposure. The right RLN branches from the vagus nerve and loops under the right subclavian artery, ascending obliquely toward the tracheoesophageal groove. Its path is highly variable. The left RLN loops under the aortic arch and ascends vertically within the tracheoesophageal groove, making its location more predictable. The superior laryngeal nerve descends medial to the carotid sheath and can be injured during upper cervical exposures, leading to voice fatigue.
The sympathetic chain lies on the prevertebral fascia, lateral to the medial border of the longus colli. Dissection extending too far laterally over the longus colli risks injury to the sympathetic trunk, resulting in Horner syndrome (ptosis, miosis, anhidrosis).
Biomechanics of the Anterior Column
The anterior column of the cervical spine is the primary load-bearing axis, transmitting approximately 80% of the axial load. Pathologic processes often compromise this load-bearing capacity. Anterior cervical discectomy and fusion (ACDF) or corpectomy addresses this by replacing the diseased disc or bone with a structural graft. The application of an anterior cervical plate acts as a tension band in extension and a buttress in flexion, significantly increasing construct rigidity and promoting high rates of arthrodesis.





Indications and Contraindications
The approach chosen depends on a number of factors, including the spinal segments that must be exposed, the nature of the procedure to be performed, and the patient's body habitus. In general, the standard Smith-Robinson approach allows access from C2 down to T1 in most patients. However, local variations in patient morphology may either limit or increase the extent of available exposure.
Operative Versus Non Operative Management
| Pathology | Operative Indications | Non Operative Management |
|---|---|---|
| Cervical Radiculopathy | Progressive motor deficit, intractable pain failing 6+ weeks of conservative care, severe foraminal stenosis with correlating symptoms. | NSAIDs, physical therapy, oral corticosteroids, selective nerve root blocks (epidural steroid injections). |
| Cervical Spondylotic Myelopathy | Clinical signs of myelopathy (hyperreflexia, clonus, Hoffman sign, gait instability) with correlating MRI cord compression or signal change. | Observation only in very mild, non-progressive cases in high-risk surgical candidates (rarely recommended). |
| Cervical Trauma (Fracture/Dislocation) | Unstable burst fractures, bilateral facet dislocations, progressive neurologic deficit, anterior column compromise. | Rigid cervical collar (Miami J/Aspen) for stable, non-displaced fractures without ligamentous injury. |
| Infection (Discitis/Osteomyelitis) | Epidural abscess with neurologic deficit, severe kyphotic deformity, failure of medical management, sepsis. | Prolonged intravenous antibiotics, rigid immobilization, close serial imaging and inflammatory marker monitoring. |
Approach Specific Indications
The lateral retropharyngeal approach (Whitesides) is often utilized for high cervical bony lesions, including tumors or infections for which a posterior approach is not possible, unstable fractures or dislocations with deficient or incompetent posterior elements, or posterior nonunions (particularly for fusions of C1-C2). It is also useful for access to high cervical ventral or ventrolateral intradural lesions such as neurofibromas or meningiomas.




Pre Operative Planning and Patient Positioning
Thorough preoperative planning is critical for successful execution. Imaging studies should be evaluated for anatomic variations such as medial aberrancy of the vertebral artery. A preoperative MRI is essential for assessing neural compression, while a CT scan provides detailed osseous anatomy, osteophyte morphology, and facet joint orientation.
Airway Management and Intubation
Ease of access to the C2-C3 disc depends on the location of the mandible and can be assessed on the preoperative lateral radiograph. Nasal intubation is preferable when approaching this level as it allows the mandible to be maximally closed, away from the line of sight of the disc. Depending on the location of the mandible with respect to C3-C4, nasal intubation may be preferable in certain instances of C3-C4 access as well. Fiberoptic assistance may be required for patients with severe myelopathy or unstable fractures to allow for awake intubation and continuous neurologic assessment prior to positioning.
Patient Habitus and Exposure Limits
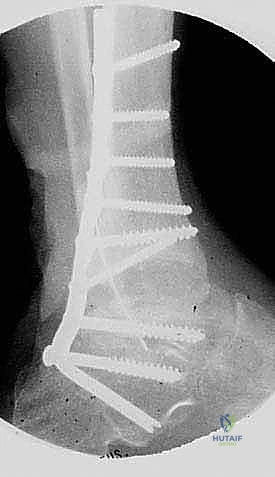
For pathology at C7-T1 or distal, careful scrutiny of the disc space with respect to the sternal notch on lateral radiographs will help to assess whether a sternal-splitting approach may be necessary. In some patients with long necks, access to T2 or even T3 may be possible with a standard Smith-Robinson approach. In those with short or stocky necks, even getting to C7 may be a challenge.


FIG 1 • Long versus short necks. A. In patients with long necks, anterior exposure through a standard Smith-Robinson approach readily provides far distal access (eg, down to T1-T2 disc space [arrow]). B. In those with short necks, however, even getting to C6-C7 may be difficult if the sternum blocks the necessary trajectory to the disc space (arrow), although it can almost always be done.
Vocal Cord Assessment
Considerable debate exists whether the “sidedness” of approach affects the rate of postoperative recurrent laryngeal nerve palsy. The literature is not conclusive but suggests higher rates with right-sided approaches due to the variable path of the right RLN. If a patient has had prior neck surgery and it is desirable to approach the spine from the opposite side to avoid scar, a preoperative indirect laryngoscopy should be performed by ear, nose, and throat (ENT) consultation to rule out an existing, asymptomatic recurrent laryngeal nerve palsy. If one exists, the spine must be approached from the side of the injury to avoid the possibility of bilateral vocal cord palsy, which can result in catastrophic airway compromise. If one does not exist, the spine can be approached from either side.




Detailed Surgical Approach and Technique
Standard Smith Robinson Approach
The patient is positioned supine on a radiolucent table. A gel roll is placed transversely beneath the scapulae to induce cervical extension, thereby opening the anterior disc spaces. The shoulders are taped caudally to maximize radiographic visualization of the lower cervical segments.
A transverse incision is typically made in a natural skin crease for one or two-level procedures. For multi-level corpectomies, an oblique longitudinal incision along the anterior border of the SCM may be preferred. The skin and subcutaneous tissues are incised, and the platysma is divided.
The superficial investing fascia is incised anterior to the SCM. Blunt dissection is utilized to identify the carotid pulse laterally. The dissection proceeds medial to the carotid sheath and lateral to the strap muscles. The omohyoid muscle may be encountered crossing the field obliquely; it can be mobilized or divided if necessary for lower cervical exposure.
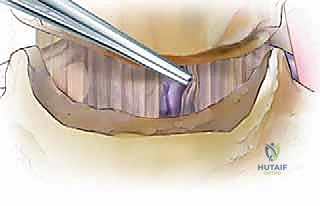
The pretracheal fascia is bluntly swept away, exposing the prevertebral fascia overlying the longus colli muscles. Needle localization with fluoroscopy confirms the correct operative level. The prevertebral fascia is incised longitudinally in the midline. The longus colli muscles are elevated subperiosteally from medial to lateral using a Cobb elevator or Bovie electrocautery. It is critical to stay within the medial borders of the longus colli to avoid injury to the sympathetic chain laterally. Self-retaining retractors are placed beneath the elevated medial edges of the longus colli.
Lateral Retropharyngeal Approach Whitesides
This approach can be used for anterior access to the upper cervical spine but not the basiocciput. It allows unilateral access from C1 to C3. Access to the far contralateral side requires a second approach.
The incision is made along the anterior border of the SCM, extending from the mastoid process to the mid-cervical region. The SCM is mobilized and retracted laterally. The spinal accessory nerve must be meticulously identified and protected as it enters the deep surface of the SCM. The carotid sheath is identified and retracted laterally, while the pharynx and larynx are retracted medially. The superior laryngeal nerve and the hypoglossal nerve must be identified and protected during high exposures.
Potential complications unique to this approach include injury to the spinal accessory nerve and the vertebral artery. The jugular vein also lies within the operative field and can be a site of significant bleeding if inadvertently injured. Significant retropharyngeal swelling has occurred and can result in prolongation of intubation if the patient's airway becomes obstructed.
Anterior Approach to the Cervicothoracic Junction
There are several different approaches for exposing the cervicothoracic junction, including the transmanubrial-transclavicular approach and the median sternotomy.
For the transmanubrial approach, an L-shaped incision is made along the anterior border of the SCM, curving laterally over the clavicle. The medial third of the clavicle and the manubrium are osteotomized to allow inferior retraction of the sternoclavicular complex. This provides direct orthogonal access to the T1-T3 vertebral bodies. Care must be taken to protect the brachiocephalic vein, the pleura, and the thoracic duct (if operating on the left side). Following the spinal reconstruction, the osteotomized bone is rigidly fixed using heavy non-absorbable sutures or orthopedic plating.








Complications and Management
Anterior cervical surgery is generally safe and highly effective, but the dense anatomy of the visceral neck renders it susceptible to specific, potentially devastating complications.
Esophageal Perforation and Dysphagia
Dysphagia is the most common postoperative complaint, occurring in up to 70% of patients transiently, though permanent dysphagia is rare. It is primarily driven by retractor-induced ischemia and localized edema. Strategies to mitigate this include periodic deflation of the endotracheal tube cuff to restore mucosal perfusion and intermittent relaxation of self-retaining retractors.
Esophageal perforation is a rare but life-threatening complication, carrying a high risk of mediastinitis. Intraoperative identification requires immediate primary repair by an otolaryngologist or general surgeon, often augmented with a sternocleidomastoid muscle flap, followed by prolonged nasogastric feeding and broad-spectrum antibiotics.
Vascular and Neurologic Injury
Vertebral artery injury is a catastrophic event, typically occurring due to loss of midline orientation or unrecognized medial aberrancy of the artery within the transverse foramen. If arterial hemorrhage occurs, immediate tamponade must be achieved. Primary repair is rarely feasible; endovascular embolization or direct ligation (if contralateral flow is confirmed adequate) are the primary salvage strategies.
Complications Summary Table
| Complication | Incidence | Avoidance and Salvage Strategy |
|---|---|---|
| Transient Dysphagia | 30% - 70% | Minimize retraction time, deflate ET tube cuff after retractor placement, utilize low-profile plates. Treat with soft diet and speech therapy evaluation. |
| Recurrent Laryngeal Nerve Palsy | 1% - 11% | Avoid excessive medial retraction, use sharp dissection in the tracheoesophageal groove. ENT evaluation for vocal cord injection if persistent >6 months. |
| Horner Syndrome | 0.1% - 1% | Restrict subperiosteal dissection of longus colli strictly to the medial border. Avoid lateral retractor blade migration. Often resolves spontaneously. |
| Vertebral Artery Injury | < 0.5% | Preoperative CT/MRI review for medial aberrancy. Maintain strict midline orientation. Manage with direct tamponade and emergent endovascular intervention. |
| Esophageal Perforation | < 0.3% | Careful placement of sharp retractor blades, avoid over-distraction. Intraoperative primary repair with muscle flap coverage; NPO and broad-spectrum antibiotics. |




Post Operative Rehabilitation Protocols
Postoperative care following anterior cervical approaches is tailored to the extent of the surgical intervention and the quality of the internal fixation.
For standard 1- to 2-level ACDF utilizing modern rigid anterior plating, postoperative immobilization is largely for patient comfort rather than structural necessity. A soft cervical collar may be worn for 1 to 2 weeks. For multi-level corpectomies or patients with poor bone quality (e.g., severe osteoporosis), rigid immobilization with a Miami J or Aspen collar is recommended for 6 to 12 weeks to prevent construct failure and promote arthrodesis.
Dietary advancement should be gradual. Patients are typically started on clear liquids and advanced to a soft mechanical diet as tolerated. If severe dysphagia is present, a formal swallow evaluation by a speech-language pathologist is mandatory prior to advancing the diet to prevent aspiration pneumonia.
Physical therapy is generally initiated at 4 to 6 weeks postoperatively, focusing on isometric neck strengthening, scapular stabilization, and postural re-education. Early aggressive range of motion is discouraged until radiographic evidence of early fusion is observed.



Summary of Key Literature and Guidelines
The academic foundation for anterior cervical approaches is robust. The original description by Smith and Robinson (1958) established the safety and efficacy of the anterior approach utilizing iliac crest bone graft. Bohlman et al. subsequently demonstrated excellent long-term outcomes for radiculopathy and myelopathy utilizing this technique.
Modern literature
Clinical & Radiographic Imaging




































You Might Also Like