Orthopedic Board Review MCQs: High-Yield Case Analysis
Orthopedic Board Review MCQs: High-Yield Case Analysis
This module contains 50 advanced orthopedic multiple-choice questions meticulously developed to mirror the American Board of Orthopaedic Surgery (ABOS) Part I and AAOS OITE examinations. These questions are comprehensively derived from the clinical teaching case: Orthopedic Board Review MCQs (2026 Edition) - Part 5.
Comprehensive Exam
00:00
Start Quiz
Question 1
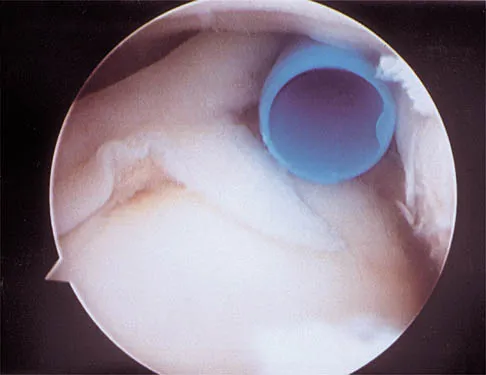
A 21-year-old collegiate pitcher undergoes shoulder arthroscopy for chronic pain. The image shows a Type I SLAP lesion. Which of the following best describes the pathologic anatomy of a Type I SLAP lesion?
Explanation
Correct Answer: A
A Type I SLAP lesion is characterized by fraying and degeneration of the superior labrum, but the biceps anchor remains firmly attached to the glenoid. Treatment typically involves simple debridement. Type II involves detachment of the superior labrum and biceps anchor. Type III is a bucket-handle tear of the labrum with an intact biceps anchor. Type IV is a bucket-handle tear extending into the biceps tendon.
Question 2
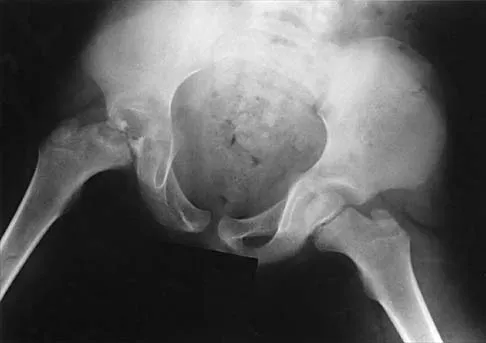
A 7-year-old boy with Legg-Calvé-Perthes disease presents with a painful limp and limited abduction. Radiographs demonstrate hinge abduction. What is the primary pathomechanical consequence of persistent hinge abduction if left untreated?
Explanation
Correct Answer: B
Hinge abduction occurs when the extruded, enlarged anterolateral portion of the femoral head impinges on the lateral margin of the acetabulum during abduction. Persistent hinge abduction prevents the acetabulum from effectively remodeling the femoral head, leading to a permanently deformed, aspherical femoral head (coxa magna) and early osteoarthritis. It does not cause premature closure of the triradiate cartilage or avascular necrosis of the acetabulum.
Question 3
The MRI scans shown demonstrate a lipohemarthrosis in the knee. Which of the following is the most common underlying etiology for this specific MRI finding?

Explanation
Correct Answer: C
Lipohemarthrosis is characterized by the layering of fat and blood within a joint cavity. The most common cause is an intra-articular fracture, which allows marrow fat to escape into the joint space. On MRI, it typically shows a superior layer of fat, a central layer of serum, and an inferior layer of red blood cells. While an ACL tear causes a hemarthrosis, it does not typically cause a lipohemarthrosis unless accompanied by an osteochondral fracture.
Question 4
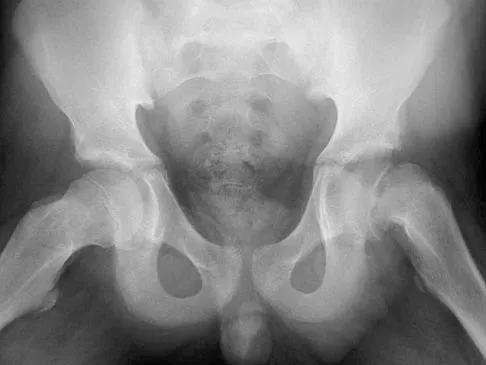
An obese 12-year-old boy presents with left hip pain and the radiograph shown. He is diagnosed with a slipped capital femoral epiphysis (SCFE). Which of the following treatments is contraindicated due to its association with a high risk of osteonecrosis?
Explanation
Correct Answer: B
Forceful closed reduction of a slipped capital femoral epiphysis is contraindicated because it significantly increases the risk of osteonecrosis (avascular necrosis) of the femoral head by disrupting the already tenuous retinacular blood supply. The standard of care is in situ fixation. Spica casting is generally not used as primary treatment due to poor control and stiffness, but closed reduction is the most dangerous intervention listed.
Question 5
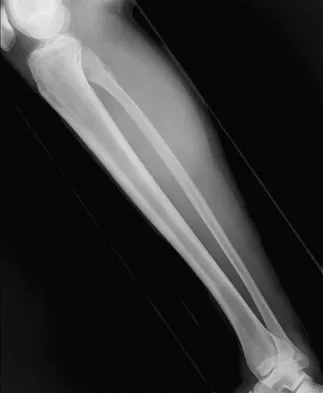
A 23-year-old man presents with right posterolateral knee pain, worse at night and relieved by NSAIDs. Imaging and histology are shown. The histologic specimen demonstrates a cellular, vascular stroma with plump osteoblasts producing immature woven bone. What is the currently preferred minimally invasive treatment for this lesion?
Explanation
Correct Answer: B
The clinical presentation, imaging (cortically based lytic lesion with surrounding sclerosis/edema), and histology (vascular stroma with osteoblasts and woven bone) are classic for an osteoid osteoma. Percutaneous radiofrequency ablation (RFA), typically under CT guidance, has become the preferred treatment method, offering high success rates with minimal morbidity compared to open surgical excision.
Question 6
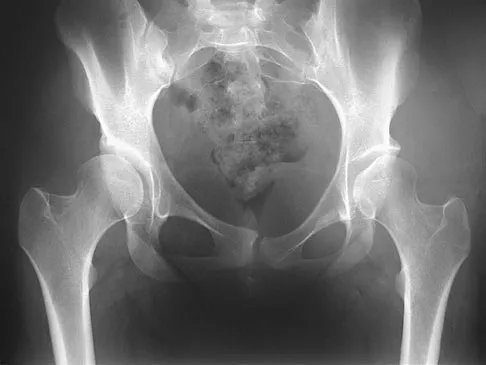
A 32-year-old woman presents with right hip pain and the radiograph shown, demonstrating developmental dysplasia of the hip (DDH) with a high acetabular index. A Bernese (Ganz) periacetabular osteotomy is planned. Which of the following is a primary biomechanical goal of this procedure?
Explanation
Correct Answer: A
The Bernese periacetabular osteotomy (PAO) is designed to reorient the acetabulum to improve femoral head coverage. A key biomechanical goal and advantage of the PAO is the ability to medialize the hip joint center, which decreases the joint reactive forces by reducing the lever arm of the body weight, thereby improving the mechanical environment of the dysplastic hip.
Question 7
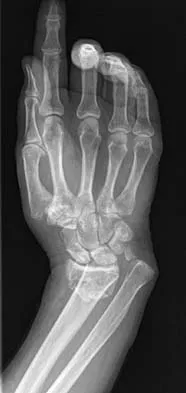
A 64-year-old woman sustains the wrist injury shown in the radiographs. The injury is a volar displaced intra-articular distal radius fracture. When utilizing a volar buttress plate for this specific fracture pattern, what is the primary biomechanical function of the plate?
Explanation
Correct Answer: C
The radiographs show a volar Barton's fracture (volar displaced intra-articular fracture of the distal radius). The primary deforming forces are axial loading and volar shear, which cause the carpus to subluxate volarly with the fracture fragment. A volar buttress plate is applied to physically block (buttress) this volar displacement, neutralizing the axial and shearing forces.
Question 8
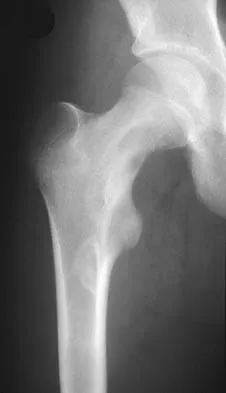
A 13-year-old girl presents with right groin pain and the imaging and histology shown. The histology reveals irregular, woven bone trabeculae in a fibrous stroma without osteoblastic rimming ('Chinese letter' pattern). This condition is associated with a somatic activating mutation in which of the following genes?
Explanation
Correct Answer: B
The clinical, radiographic (ground-glass appearance, Shepherd's crook deformity), and histologic ('Chinese letter' woven bone lacking osteoblastic rimming in a fibrous stroma) findings are diagnostic of fibrous dysplasia. Fibrous dysplasia is caused by a somatic, post-zygotic activating mutation in the GNAS1 gene, which encodes the alpha subunit of the stimulatory G protein (Gs-alpha), leading to increased intracellular cAMP and abnormal osteoblast differentiation.
Question 9
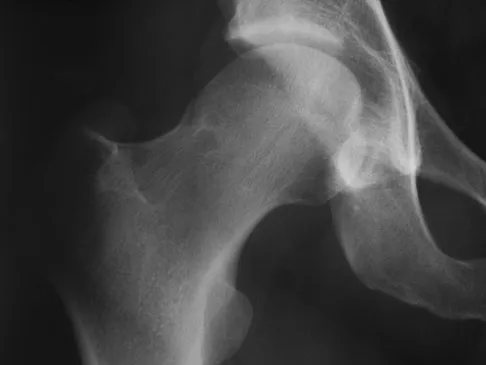
A 38-year-old runner presents with right hip pain. Imaging reveals a well-circumscribed, radiolucent lesion with a sclerotic margin in the anterosuperior aspect of the femoral neck. This lesion, known as a synovial herniation pit, is most frequently associated with which of the following underlying conditions?
Explanation
Correct Answer: C
Synovial herniation pits (Pitt's pits) are benign, often incidental, radiolucent lesions with sclerotic margins typically located in the anterosuperior femoral neck. They are thought to result from mechanical abrasion and herniation of synovium into the bone. They are highly associated with cam-type femoroacetabular impingement (FAI), where the abnormal femoral head-neck junction abuts the acetabular rim.
Question 10
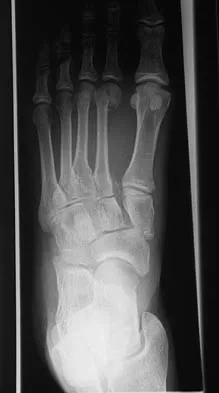
A 22-year-old man sustains the midfoot injury shown in the radiograph. The injury involves disruption of the Lisfranc ligament complex. Which of the following best describes the anatomic attachments of the primary, strongest band of the Lisfranc ligament?
Explanation
Correct Answer: B
The radiograph demonstrates a Lisfranc injury (tarsometatarsal fracture-dislocation). The Lisfranc ligament is a critical stabilizing structure of the midfoot. Its primary, strongest, and most important band (the interosseous Lisfranc ligament) attaches from the lateral aspect of the medial cuneiform to the medial aspect of the base of the second metatarsal. There is no direct ligamentous connection between the first and second metatarsal bases.
Question 11
A 21-year-old collegiate pitcher presents with chronic shoulder pain that has failed to improve with rest and physical therapy. An arthroscopic view from the posterior portal is shown. Probing reveals fraying of the superior labrum, but the biceps anchor is firmly attached to the superior glenoid tubercle. Which of the following best describes the Snyder classification and the most appropriate management for this lesion?

Explanation
Correct Answer: Type I; arthroscopic debridement
The arthroscopic image demonstrates a Type I SLAP (Superior Labrum Anterior and Posterior) lesion, which is characterized by fraying and degeneration of the superior labrum with an intact biceps anchor. The appropriate treatment for a Type I SLAP lesion is simple arthroscopic debridement. Biceps tenodesis or tenotomy is not indicated because the biceps anchor is stable. Type II lesions involve detachment of the superior labrum and biceps anchor and are typically treated with repair. Type III lesions are bucket-handle tears of the labrum with an intact biceps anchor, and Type IV lesions are bucket-handle tears that extend into the biceps tendon.
Question 12
A 7-year-old boy with a history of a painless limp is diagnosed with Legg-Calvé-Perthes disease. An arthrogram is performed to evaluate joint congruency. The maximum abduction/internal rotation view is shown in Figure A, and the abduction view is shown in Figure B. The failure of the lateral epiphysis to slide under the acetabular edge with abduction, accompanied by medial dye pooling, is pathognomonic for which of the following conditions?
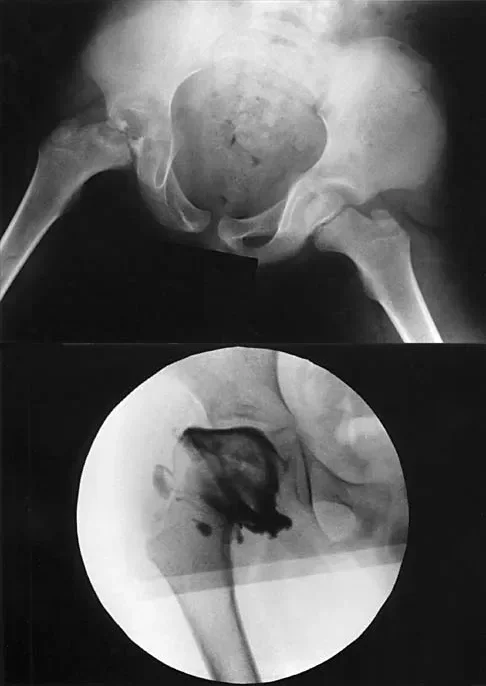
Explanation
Correct Answer: Hinge abduction
The arthrogram images demonstrate classic hinge abduction, a critical finding in severe Legg-Calvé-Perthes disease. Hinge abduction occurs when the enlarged, deformed lateral portion of the femoral head extrudes and impinges against the lateral margin of the acetabulum during abduction. Instead of gliding smoothly into the acetabulum, the femoral head hinges on the acetabular rim, causing the medial joint space to widen (distract), which is visualized as medial dye pooling on the arthrogram. Persistent hinge abduction prevents normal spherical remodeling of the femoral head and is an indication for surgical intervention to restore congruency.
Question 13
A patient presents to the emergency department with acute knee swelling following a high-energy trauma. T1-weighted MRI is obtained and shown. The distinct layering effect seen in the suprapatellar pouch is most strongly associated with which of the following underlying injuries?

Explanation
Correct Answer: Intra-articular fracture
The MRI scan demonstrates a lipohemarthrosis, characterized by the layering of fat, serum, and red blood cells in the joint space. The superior layer contains fat (high signal intensity on T1), the middle layer contains serum, and the dependent layer contains red blood cells. The presence of a lipohemarthrosis is highly indicative of an intra-articular fracture, which allows marrow fat to escape into the joint cavity. While ligamentous and meniscal injuries can cause a hemarthrosis, they do not typically introduce marrow fat into the joint unless accompanied by an osteochondral defect or fracture.
Question 14
A 25-year-old man presents with right shoulder pain. An arthroscopic view from the posterior portal viewing the articular surface of the supraspinatus is shown. The lesion is identified as a partial articular-sided supraspinatus tendon avulsion (PASTA). If this lesion involves greater than 50% of the tendon thickness, which of the following is an accepted surgical management strategy?
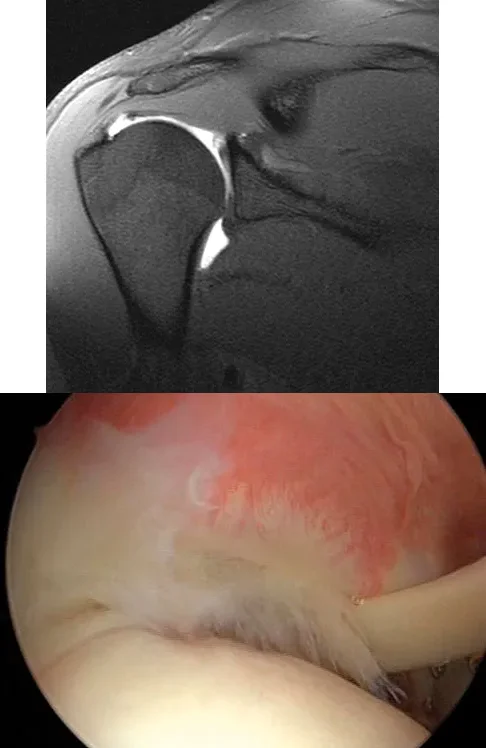
Explanation
Correct Answer: Transtendon arthroscopic repair
The images demonstrate a PASTA lesion (Partial Articular-Sided Tendon Avulsion). When a PASTA lesion involves greater than 50% of the tendon footprint thickness, surgical repair is generally indicated. An accepted and common technique is a transtendon arthroscopic repair, which allows the surgeon to secure the articular-sided tear down to the footprint without taking down the intact bursal-sided tissue. This preserves the intact lateral fibers of the rotator cuff while restoring the medial footprint anatomy.
Question 15
A 23-year-old man presents with right posterolateral knee pain that is worse at night and dramatically relieved by NSAIDs. Imaging reveals a well-circumscribed, cortically based lytic lesion in the proximal fibula with surrounding edema. Histology demonstrates a cellular stroma with plump osteoblasts producing immature woven bone. What is the preferred definitive treatment for this condition?

Explanation
Correct Answer: Percutaneous radiofrequency ablation
The clinical presentation (night pain relieved by NSAIDs), radiographic appearance (cortically based lytic lesion with surrounding sclerosis/edema), and histology (plump osteoblasts producing woven bone in a vascular stroma) are classic for an osteoid osteoma. Percutaneous radiofrequency ablation (RFA), typically performed under CT guidance, has become the preferred, minimally invasive treatment of choice for most osteoid osteomas, offering high success rates and low morbidity compared to open surgical resection or curettage.
Question 16
A 32-year-old woman presents with chronic right hip pain. The AP pelvis radiograph demonstrates developmental dysplasia of the hip with a high acetabular index (27 degrees) and anterior undercoverage. Assuming the joint space is well-preserved and there is no advanced osteoarthritis, which of the following is the most appropriate surgical intervention?

Explanation
Correct Answer: Bernese (Ganz) periacetabular osteotomy
The radiograph shows symptomatic developmental dysplasia of the hip (DDH) with significant anterolateral undercoverage. In a young, active patient with preserved joint space and symptomatic dysplasia, a redirectional pelvic osteotomy is indicated to improve femoral head coverage and biomechanics, thereby delaying or preventing the onset of osteoarthritis. The Bernese (Ganz) periacetabular osteotomy is the most widely accepted procedure for this indication in adults, as it allows for multiplanar correction while maintaining the integrity of the posterior column.
Question 17
A 64-year-old woman sustains the wrist injury shown in the radiographs after a fall on an outstretched hand. The fracture pattern involves a volar displaced intra-articular fragment. What is the primary biomechanical rationale for utilizing a volar buttress plate in the surgical management of this specific injury?
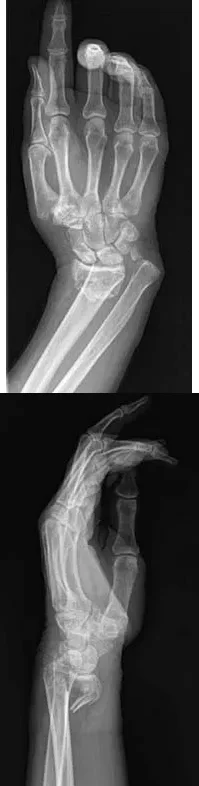
Explanation
Correct Answer: It neutralizes axial loading forces on the fractured volar fragment.
The radiographs demonstrate a volar Barton's fracture, which is a volar displaced intra-articular fracture-dislocation of the distal radius. The volar carpal ligaments remain attached to the volar fragment, pulling the carpus volarly. A volar buttress plate is biomechanically ideal for this injury because it acts as an anti-glide plate, neutralizing the axial loading and shear forces that drive the fragment proximally and volarly. A dorsal plate would not provide this buttress effect and would make maintaining the reduction difficult.
Question 18
A 58-year-old woman who underwent a right total knee arthroplasty 2 years ago sustains a fall. Radiographs demonstrate an oblique periprosthetic distal femur fracture above a well-fixed, posterior-stabilized closed-box femoral component. Which of the following is the most appropriate surgical management?
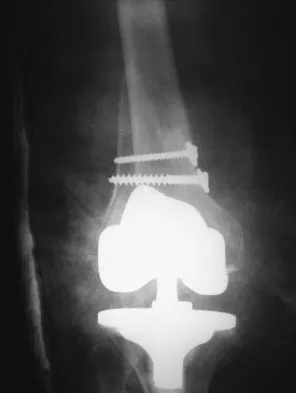
Explanation
Correct Answer: Open reduction and internal fixation with a locked plate
The patient has a displaced periprosthetic distal femur fracture above a well-fixed femoral component. Because the component is a posterior-stabilized closed-box design, retrograde intramedullary nailing is contraindicated (the box prevents nail passage). Since the component is well-fixed, revision arthroplasty is unnecessary and would sacrifice bone stock. Therefore, open reduction and internal fixation (ORIF) with a locked laterally based plate is the most appropriate treatment to provide stable fixation while preserving the prosthesis.
Question 19
A 13-year-old girl presents with right groin pain. Radiographs reveal a ground-glass lesion in the proximal femur with a mild 'Shepherd's crook' deformity. Histologic examination demonstrates proliferating fibroblasts in a loose spindle cell background with dysplastic metaplastic trabeculae arranged in a 'Chinese letter' pattern. Which of the following is the most likely diagnosis?
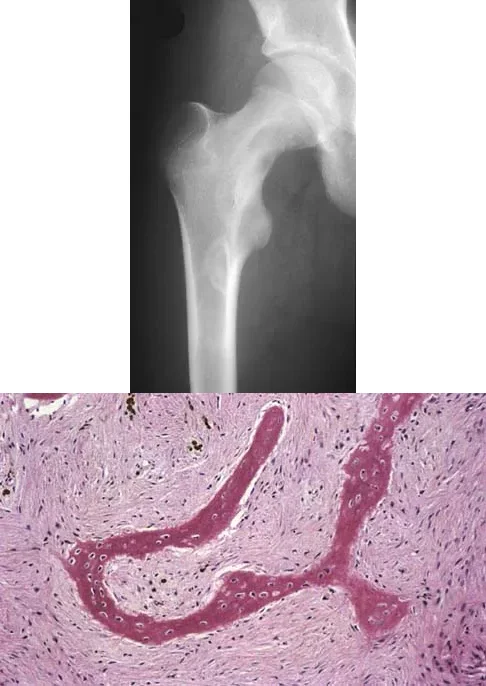
Explanation
Correct Answer: Fibrous dysplasia
The clinical, radiographic, and histologic findings are classic for fibrous dysplasia. Radiographically, it presents as a lytic, expansile lesion with a 'ground-glass' matrix, often leading to bowing deformities in the proximal femur known as a 'Shepherd's crook' deformity. Histologically, it is characterized by a fibrous stroma containing irregular, woven bone trabeculae that lack osteoblastic rimming, often described as having a 'Chinese letter' or 'alphabet soup' appearance.
Question 20
A 7-year-old girl presents with a painful volar forearm mass. Radiographs demonstrate multiple small, rounded calcifications within the soft tissues. MRI reveals a heterogeneous intramuscular mass with increased signal intensity on T1-weighted images, suggesting interspersed fat. What do the calcifications seen on the radiographs most likely represent?
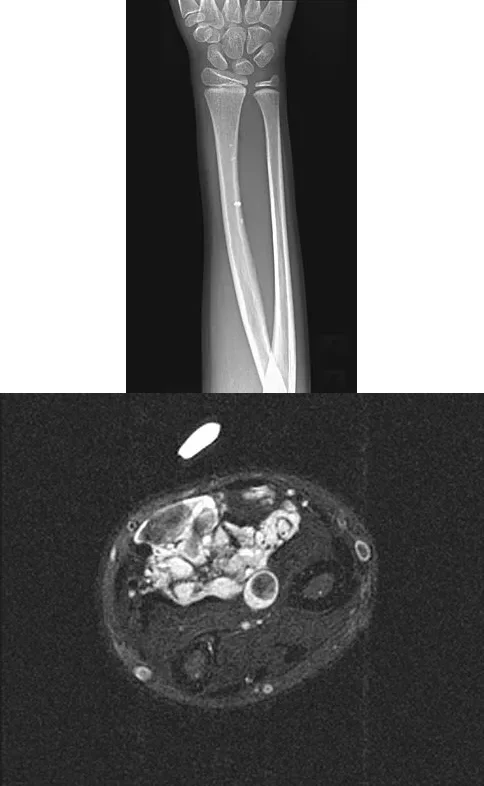
Explanation
Correct Answer: Phleboliths associated with a hemangioma
The presence of small, rounded calcifications in a soft-tissue mass on radiographs is highly suggestive of phleboliths, which are calcified thrombi within the venous channels of a hemangioma. The MRI findings of a heterogeneous mass with high T1 signal (due to interspersed fat) further support the diagnosis of an intramuscular hemangioma. Myositis ossificans typically shows peripheral ossification, while chondroid matrix usually appears as stippled or rings-and-arcs calcifications.
Question 21
A 21-year-old collegiate pitcher presents with shoulder pain. Arthroscopy reveals fraying of the superior labrum with an intact biceps anchor, as shown in the provided image. Which of the following is the most appropriate management for this specific lesion?

Explanation
Correct Answer: Arthroscopic debridement
The image and description correspond to a Type I SLAP lesion (fraying of the superior labrum with an intact biceps anchor). The appropriate treatment is simple debridement. Biceps tenodesis or release is not indicated because the biceps tendon and anchor are intact. There is no indication for labral repair or capsulorrhaphy.
Question 22
A 23-year-old competitive overhead athlete undergoes shoulder arthroscopy. The intraoperative finding is shown in the provided image. Which of the following treatments is most appropriate to allow return to competitive overhead sports?
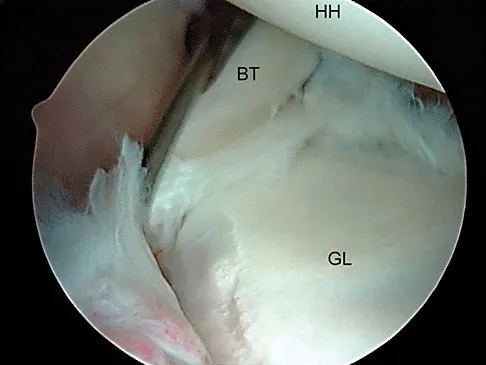
Explanation
Correct Answer: Arthroscopic labral repair
The image shows a Type II SLAP tear (detachment of the superior labrum and biceps anchor). In a young, competitive overhead athlete, arthroscopic labral repair is the treatment of choice to restore anatomy and function. Labral debridement leads to predictably poor results in this demographic, while biceps tenodesis or tenotomy is generally reserved for older patients or those who are not competitive overhead athletes.
Question 23
A 7-year-old boy with a history of a painless limp undergoes an arthrogram of the hip, as shown in the provided images. The failure of the lateral epiphysis to slide under the acetabular edge during abduction is diagnostic of which of the following?
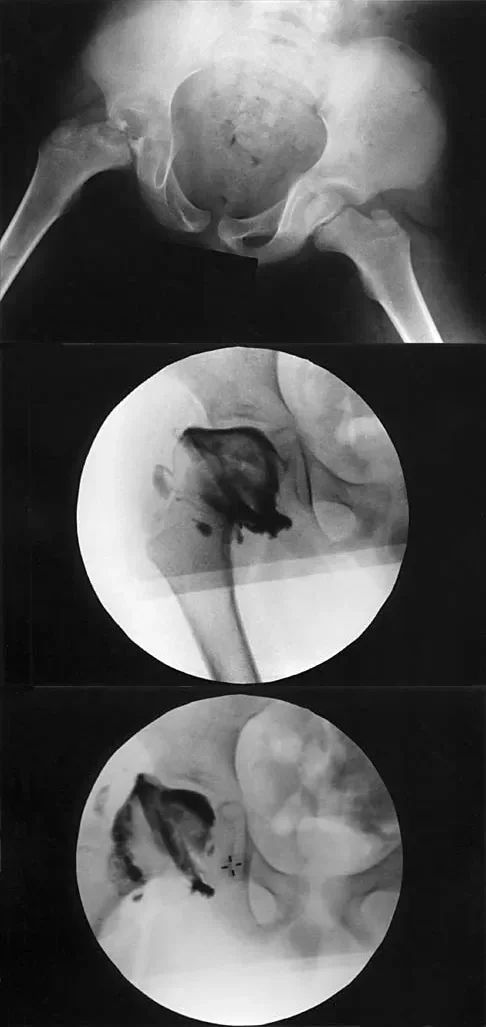
Explanation
Correct Answer: Hinge abduction
The arthrogram demonstrates hinge abduction, a severe complication of Legg-Calvé-Perthes disease where the deformed, extruded lateral portion of the femoral head hinges against the lateral acetabular margin during abduction, preventing concentric reduction. This persistent hinge abduction prevents femoral head remodeling by the acetabulum.
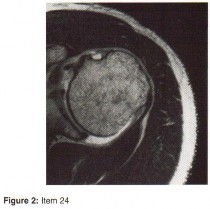
Question 24
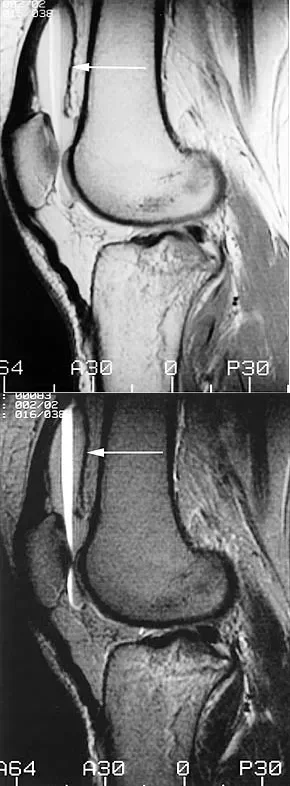
A patient presents with acute knee swelling following trauma. MRI scans (T1 and T2-weighted) are shown. The layering effect seen within the joint space is most strongly associated with which of the following underlying injuries?
Explanation
Correct Answer: Intra-articular fracture
The MRI shows lipohemarthrosis, characterized by layering of fat (superior, high signal on T1), serum (central, low signal), and red blood cells (inferior, low signal). This finding is highly indicative of an intra-articular fracture, which allows marrow fat to escape into the joint space.
Question 25
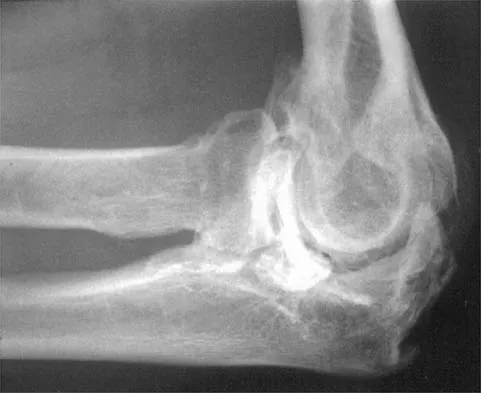
A 52-year-old former baseball pitcher presents with pain at the extremes of elbow flexion and extension. A radiograph is provided. Which of the following is the most appropriate surgical intervention if nonoperative management fails?
Explanation
Correct Answer: Excision of osteophytes and loose bodies with capsular release
The radiograph and history are classic for primary degenerative arthritis of the elbow, characterized by osteophytes on the coronoid and olecranon, and loose bodies. Treatment consists of removal of loose bodies and impinging osteophytes along with capsular release. Total elbow arthroplasty is generally contraindicated in younger, active patients who wish to maintain heavy use of the extremity.
Question 26
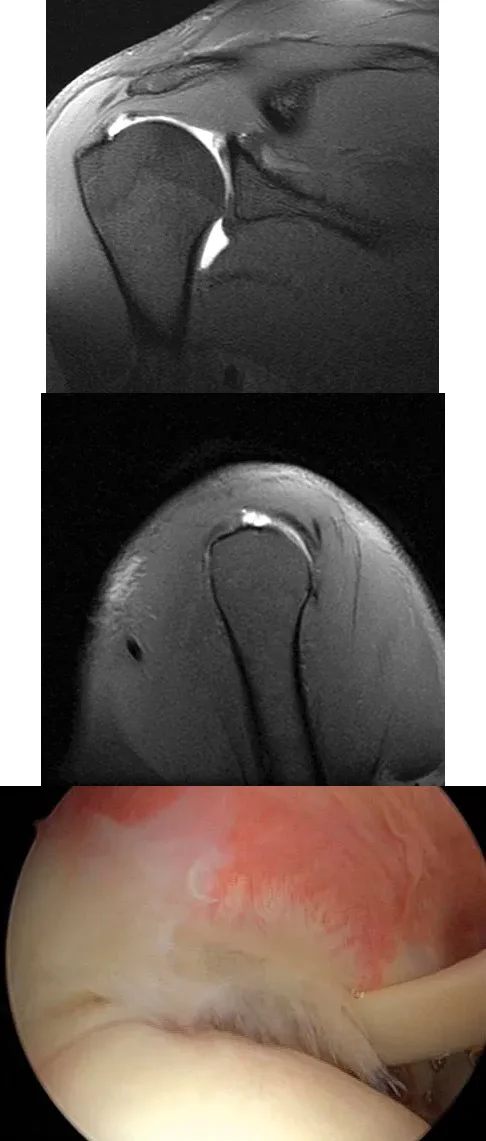
A 25-year-old man presents with right shoulder pain. MRI and arthroscopic images are provided. The pathology shown is best described as:
Explanation
Correct Answer: A partial articular-sided supraspinatus tendon avulsion
The images demonstrate a partial articular surface supraspinatus tear (PASTA lesion). The arthroscopic view from the posterior portal shows the articular surface of the supraspinatus with partial tearing. These tears are a common source of shoulder pain and are often amenable to transtendon arthroscopic repair without detachment of the intact bursal surface.
Question 27
An obese 12-year-old boy presents with left hip pain and an antalgic gait. A radiograph is provided. Which of the following complications is most strongly associated with attempts at closed reduction of this condition?

Explanation
Correct Answer: Osteonecrosis of the femoral head
The radiograph shows a slipped capital femoral epiphysis (SCFE). Closed reduction of a SCFE is contraindicated because it significantly increases the risk of osteonecrosis (avascular necrosis) of the femoral head. The recommended treatment is percutaneous pinning in situ.
Question 28
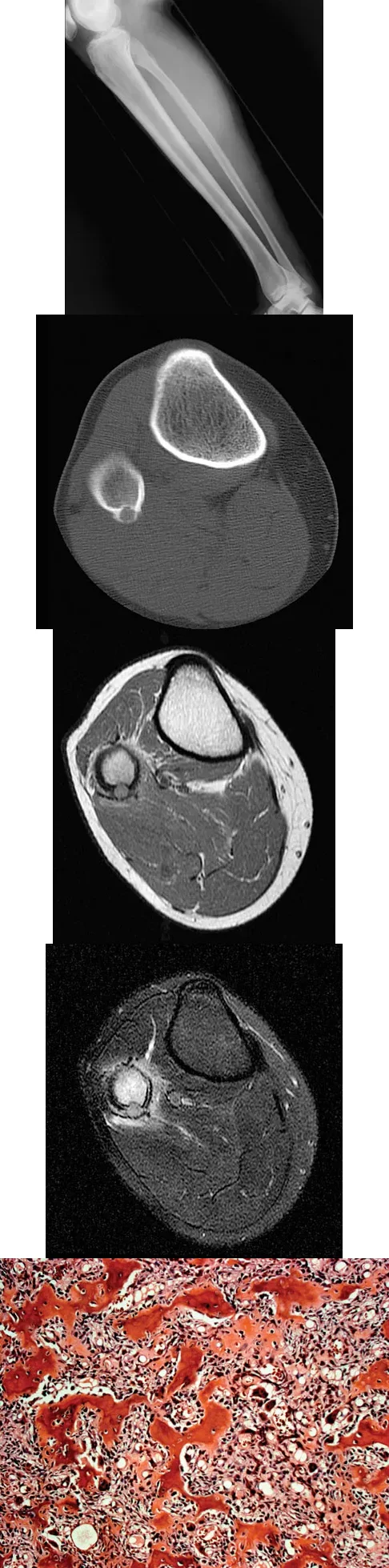
A 23-year-old man presents with right posterolateral knee pain that is worse at night and relieved by NSAIDs. Imaging and histology are provided. The histologic specimen is most likely to demonstrate which of the following?
Explanation
Correct Answer: A cellular stroma with plump osteoblasts producing immature woven bone
The clinical presentation, imaging (cortically based lytic lesion with surrounding edema), and histology are diagnostic of an osteoid osteoma. Histologically, it consists of a highly vascularized nidus of interlacing trabeculae of osteoid and woven bone lined by plump, benign osteoblasts.
Question 29
A 32-year-old woman presents with chronic right hip pain. A radiograph is provided, demonstrating developmental dysplasia of the hip with a high acetabular index. Which of the following is the primary biomechanical goal of the most appropriate joint-preserving surgery for this patient?

Explanation
Correct Answer: Medialization of the hip center of rotation and improvement of anterior and lateral femoral head coverage
The radiograph shows developmental dysplasia of the hip (DDH). The Bernese (Ganz) periacetabular osteotomy is the treatment of choice for symptomatic dysplasia with preserved joint space. Its biomechanical goals include improving anterior and lateral coverage of the femoral head and medializing the hip center of rotation to decrease joint contact forces.
Question 30
A 14-year-old girl presents with a painful mass in her proximal humerus. Imaging is provided, demonstrating an expansile, eccentric, lytic lesion with fluid-fluid levels on MRI. Following curettage and bone grafting, which of the following factors is most strongly associated with an increased risk of local recurrence?
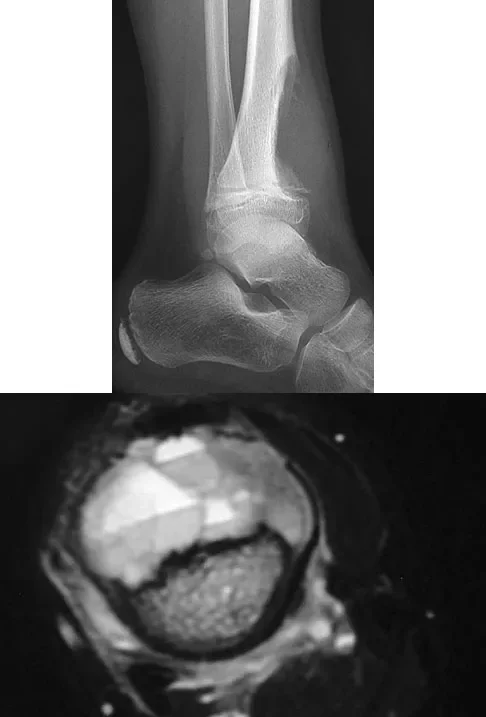
Explanation
Correct Answer: Young age and open physes
The imaging is classic for an aneurysmal bone cyst (ABC), showing fluid-fluid levels on MRI. Factors associated with a higher rate of local recurrence include young age, open physes, and inadequate surgical margins. The use of a high-speed burr and local adjuvants (like phenol or argon beam) decreases the recurrence rate.
Question 31
A 21-year-old overhead athlete presents with chronic shoulder pain that has not improved with rest and physical therapy. Arthroscopy reveals fraying of the superior labrum without detachment of the biceps anchor, as seen in the provided image. Which of the following is the most appropriate management for this specific lesion?

Explanation
Correct Answer: B
The image demonstrates a Type I superior labrum anterior and posterior (SLAP) lesion, characterized by fraying and degeneration of the superior labrum with an intact biceps anchor. The appropriate treatment for a Type I SLAP lesion is simple arthroscopic debridement. Biceps tenodesis or tenotomy is not indicated because the biceps anchor is stable. Suture anchor repair is reserved for Type II or Type IV SLAP lesions where the biceps anchor is detached.
Question 32
A 23-year-old competitive baseball pitcher undergoes shoulder arthroscopy for refractory pain. The intraoperative finding is shown in the image. Which of the following treatments provides the most predictable return to competitive throwing for this patient?

Explanation
Correct Answer: C
The image shows a classic Type II SLAP tear, where the superior labrum and biceps anchor are detached from the superior glenoid. In a young, competitive overhead athlete, arthroscopic labral repair yields the highest satisfaction and best chance for return to overhead sports. Labral debridement alone leads to predictably poor results in this demographic. Biceps tenodesis or tenotomy may be considered in older patients or non-overhead athletes with Type II SLAP tears.
Question 33
A 7-year-old boy with a history of a painless limp presents with limited abduction and spasm on internal rotation. Radiographs obtained during an arthrogram are shown. The failure of the lateral epiphysis to slide under the acetabular edge during abduction is diagnostic of which of the following?
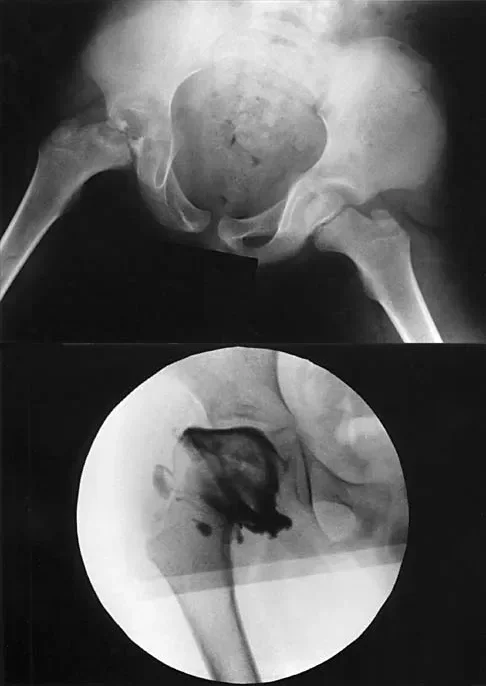
Explanation
Correct Answer: B
The radiographs demonstrate classic hinge abduction in a patient with Legg-Calve-Perthes disease. Hinge abduction occurs when the enlarged, deformed lateral portion of the femoral head impinges on the lateral acetabular margin during abduction, preventing the head from sliding concentrically into the acetabulum. The arthrogram shows medial dye pooling due to distraction of the joint. Persistent hinge abduction prevents proper femoral head remodeling and is an indication for surgical intervention.
Question 34
A patient presents with acute knee swelling following trauma. T1- and T2-weighted MRI scans are shown, demonstrating a characteristic layering effect within the joint effusion. This finding is most strongly associated with which of the following underlying injuries?
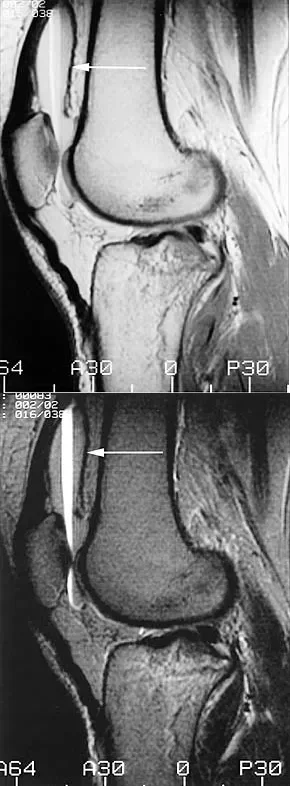
Explanation
Correct Answer: C
The MRI scans demonstrate a lipohemarthrosis, characterized by the layering of fat (superiorly, high signal on T1), serum (centrally), and red blood cells (inferiorly, low signal). The most common cause of a lipohemarthrosis is an intra-articular fracture, which allows marrow fat to escape into the joint space. While an ACL tear can cause a hemarthrosis, it typically does not produce a lipohemarthrosis unless accompanied by an osteochondral fracture.
Question 35
A 25-year-old man presents with right shoulder pain. MRI and arthroscopic images are provided. The arthroscopic view from the posterior portal demonstrates a partial articular-sided supraspinatus tendon avulsion (PASTA). Which of the following is an accepted surgical management strategy for this lesion if it involves greater than 50% of the tendon thickness?
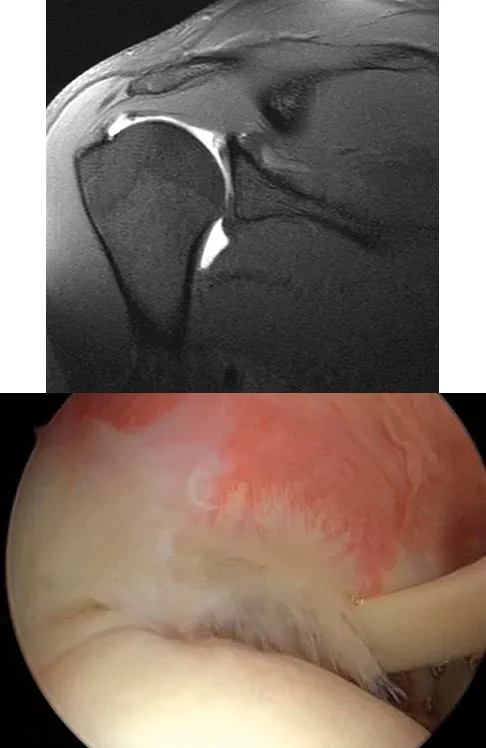
Explanation
Correct Answer: A
The images show a partial articular surface supraspinatus tear (PASTA lesion). When these tears involve greater than 50% of the tendon thickness, surgical repair is often indicated. A common and effective technique is a transtendon arthroscopic repair, which secures the articular-sided avulsion while preserving the intact bursal surface of the tendon. Acromioplasty alone does not address the structural tendon defect.
Question 36
An obese 12-year-old boy presents with left hip pain and an obligatory external rotation during hip flexion. An AP pelvis radiograph is shown. Which of the following is the most appropriate definitive management for the left hip?

Explanation
Correct Answer: C
The radiograph demonstrates a slipped capital femoral epiphysis (SCFE) of the left hip. The standard of care for a stable SCFE is percutaneous pinning in situ with a single cannulated screw to prevent further slippage and promote physeal closure. Closed reduction is contraindicated as it significantly increases the risk of osteonecrosis. Spica casting and observation are not appropriate definitive treatments.
Question 37
A 23-year-old man complains of right posterolateral knee pain that is worse at night and relieved by NSAIDs. Imaging and histology are shown. The histology demonstrates a cellular, vascular stroma with plump osteoblasts producing immature woven bone. What is the preferred modern treatment modality for this lesion?
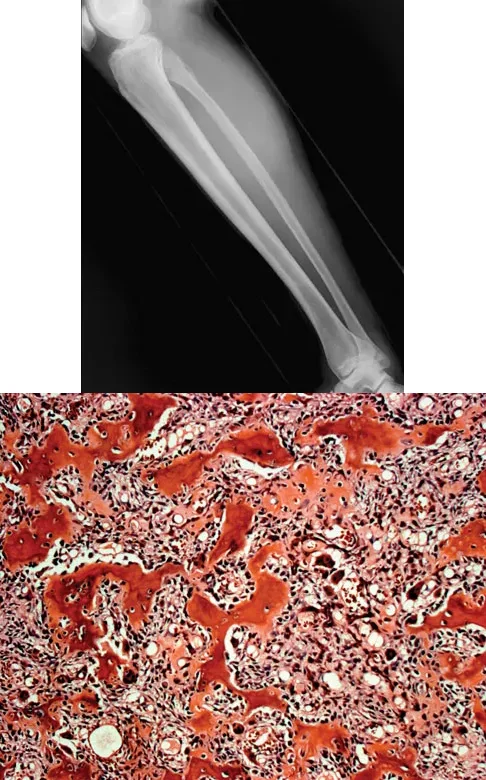
Explanation
Correct Answer: B
The clinical presentation (night pain relieved by NSAIDs), radiographic appearance (cortically based lytic lesion with surrounding sclerosis), and histology (vascular stroma with osteoblasts and woven bone) are diagnostic of an osteoid osteoma. The preferred modern treatment for most osteoid osteomas is CT-guided percutaneous radiofrequency ablation, which is minimally invasive and highly effective. En bloc resection is rarely required today.
Question 38
A 32-year-old woman presents with right hip pain that has failed conservative management. An AP pelvis radiograph is shown, demonstrating a high acetabular index and anterolateral undercoverage of the femoral head with preserved joint space. Which of the following surgical interventions is most appropriate?

Explanation
Correct Answer: C
The radiograph reveals developmental dysplasia of the hip (DDH) with significant anterolateral undercoverage but preserved joint space. In a young, active patient with symptomatic DDH and minimal osteoarthritis, a Bernese (Ganz) periacetabular osteotomy is the procedure of choice. It reorients the acetabulum to improve femoral head coverage and biomechanics, delaying or preventing the need for total hip arthroplasty.
Question 39
A 65-year-old woman presents with chronic aching in her elbow. Radiographs and a biopsy specimen are shown. The histology reveals round to oval cells with an eccentric nucleus, prominent nucleolus, and a clear perinuclear area representing the Golgi apparatus. Which of the following is the most likely diagnosis?
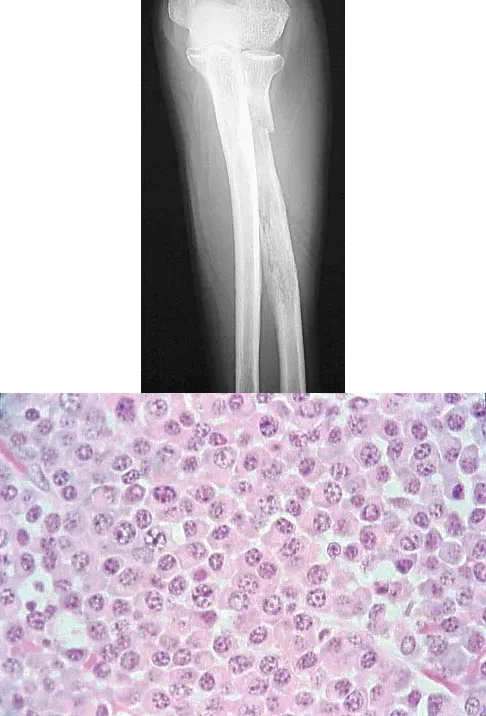
Explanation
Correct Answer: C
The histologic description and image are pathognomonic for plasma cells, which characterize multiple myeloma. The cells are round/oval with an eccentric nucleus, prominent nucleolus, and a perinuclear clearing (halo) that represents the prominent Golgi apparatus. Multiple myeloma frequently presents as lytic bone lesions in older adults.
Question 40
A 64-year-old woman sustains a wrist injury after a fall. Radiographs demonstrate a volar displaced, intra-articular distal radius fracture-dislocation. Which of the following surgical approaches and fixation methods is most appropriate to neutralize the axial loading forces on the fractured fragment?
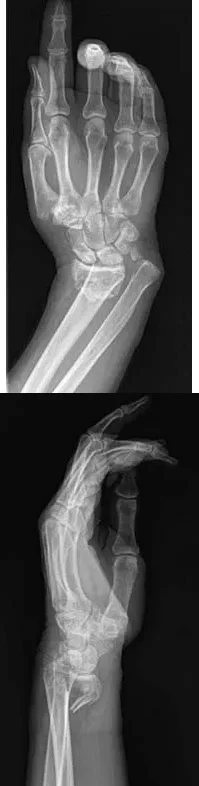
Explanation
Correct Answer: B
The radiographs show a volar Barton's fracture (volar displaced intra-articular distal radius fracture-dislocation). The most biomechanically sound treatment is an open reduction through a volar approach and stabilization with a volar buttress plate. The buttress plate effectively neutralizes the axial loading and shear forces that drive the volar fragment proximally. A dorsal plate cannot provide this buttress effect for a volar shear fracture.
Question 41
A 24-year-old recreational weightlifter presents with vague anterior shoulder pain. An arthroscopic image from the posterior portal is shown. Probing reveals fraying of the superior labrum, but the biceps anchor is firmly attached to the superior glenoid tubercle. Which of the following is the most appropriate management?

Explanation
Correct Answer: B
The image and clinical description are consistent with a Type I SLAP lesion, which is characterized by degenerative fraying of the superior labrum with an intact biceps anchor. The appropriate treatment for a Type I SLAP lesion is simple arthroscopic debridement of the frayed tissue. Repair or tenodesis is not indicated because the biceps anchor remains stable and intact.
Question 42
A 35-year-old skier sustains a twisting injury to the knee. An MRI is obtained, and a T1-weighted sagittal image is shown. The layering effect seen in the suprapatellar pouch is most strongly associated with which of the following underlying injuries?

Explanation
Correct Answer: C
The MRI demonstrates lipohemarthrosis, characterized by a distinct layering effect in the suprapatellar pouch. Fat (which has high signal intensity on T1-weighted images) layers superiorly, serum layers centrally, and red blood cells layer inferiorly. This finding is highly indicative of an intra-articular fracture, which allows marrow fat to escape into the joint space.
Question 43
A 3-year-old boy presents with a limp and refusal to bear weight on the right leg. He is afebrile but has limited internal rotation. An AP pelvis radiograph is shown. The right teardrop distance measures 11 mm, while the left measures 8 mm. What is the most definitive next step in management to determine the etiology?
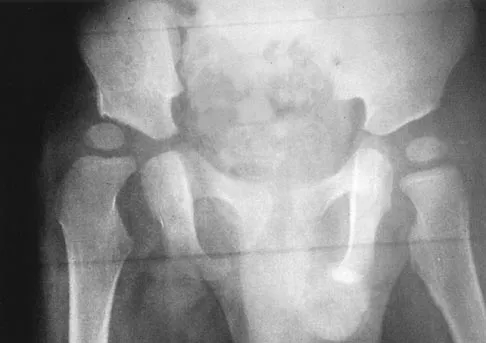
Explanation
Correct Answer: B
The widened teardrop distance (a difference of >2 mm compared to the contralateral side) indicates a significant joint effusion. In a child presenting with refusal to bear weight and limited motion, septic arthritis must be urgently ruled out. Hip aspiration is the most definitive test to differentiate septic arthritis from transient synovitis by obtaining fluid for cell count, Gram stain, and culture.
Question 44
A 7-year-old boy with a known history of Legg-Calve-Perthes disease presents with worsening pain and a limp. An AP radiograph in maximum abduction is shown. The failure of the lateral epiphysis to slide under the acetabular edge with abduction is known as hinge abduction. This biomechanical phenomenon is most likely to result in which of the following?

Explanation
Correct Answer: B
The radiograph demonstrates hinge abduction, where the extruded, enlarged lateral portion of the femoral head hinges against the lateral acetabular margin during abduction. This prevents the femoral head from seating concentrically in the acetabulum, thereby preventing the acetabulum from acting as a spherical mold to remodel the femoral head during the healing phase of Legg-Calve-Perthes disease.
Question 45
A 55-year-old male heavy laborer complains of progressive loss of elbow extension and pain at the extremes of motion. A lateral radiograph is shown. Which of the following surgical interventions is most appropriate for this patient if conservative management fails?

Explanation
Correct Answer: C
The patient has primary degenerative arthritis of the elbow, characterized by osteophytes on the coronoid and olecranon, loose bodies, and pain at terminal extension. The most appropriate surgical treatment for a high-demand patient (such as a heavy laborer) is the removal of loose bodies, excision of impinging osteophytes, and capsular release (performed either open or arthroscopically). Total elbow arthroplasty is contraindicated in heavy laborers due to strict permanent lifting restrictions.
Question 46
An 8-month-old infant is noted to have a congenital spinal deformity as shown in the clinical photograph. Neurologic examination is normal. Which of the following screening tests is most highly recommended to identify the most common associated extraspinal anomaly in this patient?
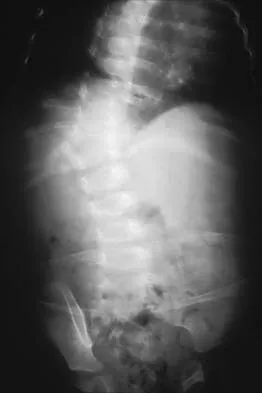
Explanation
Correct Answer: B
The patient has congenital scoliosis. Approximately 60% of patients with congenital vertebral anomalies have associated abnormalities in other organ systems. The most common associated extraspinal anomalies are genitourinary (occurring in up to 37% of patients), such as renal agenesis, duplication, or ectopia. Therefore, a renal ultrasound is the most appropriate and least invasive initial screening test.
Question 47
A 38-year-old woman presents with severe, sharp pain in the third webspace of her foot, 18 months after undergoing a dorsal neurectomy for a Morton's neuroma. Examination reveals a positive Mulder's click and exquisite tenderness on the plantar aspect. If surgical intervention is chosen, what is the most reliable approach and procedure?
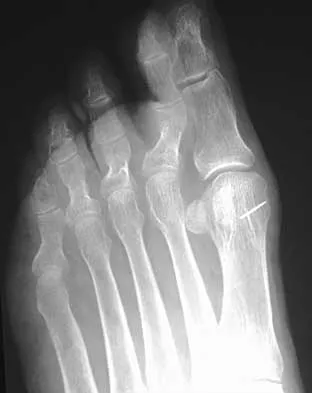
Explanation
Correct Answer: B
Recurrent Morton's neuroma is typically due to a stump neuroma located in the weight-bearing area resulting from an initial resection that was too distal. The most reliable surgical treatment is a revision neurectomy to resect the nerve more proximally, moving the stump out of the weight-bearing zone. A plantar approach is preferred for revision surgery as it allows excellent visualization of the nerve proximal to the deep transverse metatarsal ligament and avoids the dorsal scar tissue from the index procedure.
Question 48
A 22-year-old collegiate volleyball player experiences deep shoulder pain and a 'dead arm' sensation during serving. An arthroscopic image is shown. Which of the following treatments provides the best chance for return to pre-injury level of play?

Explanation
Correct Answer: D
The image shows a Type II SLAP lesion, characterized by detachment of the superior labrum and biceps anchor from the superior glenoid. In a young, competitive overhead athlete, arthroscopic repair of the SLAP lesion using suture anchors is the treatment of choice to restore the stabilizing function of the biceps anchor and allow return to sports. Tenodesis or tenotomy is generally reserved for older patients or those with chronic, degenerative changes.
Question 49
A 45-year-old man sustained a distal radius fracture treated with cast immobilization. He subsequently developed severe shoulder stiffness. After 6 months of physical therapy, his forward elevation is 130 degrees, but external rotation at the side is limited to 5 degrees. Which of the following structures is most likely contracted and requires arthroscopic release?
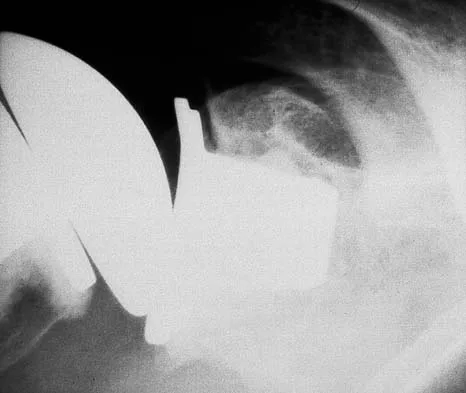
Explanation
Correct Answer: C
Isolated or disproportionate loss of external rotation with the arm at the side is the clinical hallmark of a contracted rotator cuff interval, which includes the coracohumeral ligament and the superior glenohumeral ligament. Arthroscopic release of the rotator cuff interval is the treatment of choice when conservative management fails to restore external rotation.
Question 50
A 19-year-old female collegiate soccer player sustains a noncontact twisting injury to her knee, resulting in an ACL tear. Which of the following factors is considered the most significant modifiable contributor to the higher incidence of ACL tears in female athletes compared to males?
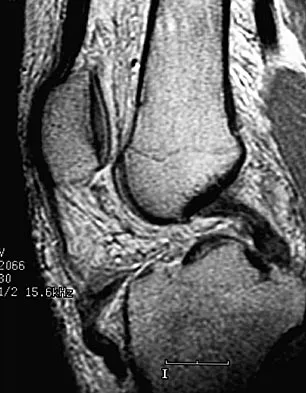
Explanation
Correct Answer: D
While anatomic (notch width, Q-angle) and hormonal factors have been implicated in the higher rate of ACL tears in females, neuromuscular factors (such as landing biomechanics, decreased hamstring-to-quadriceps strength ratio, and altered muscle activation patterns) are considered the most significant and, importantly, modifiable risk factors. Neuromuscular training programs have been shown to effectively reduce the incidence of ACL tears in female athletes.
You Might Also Like