Orthopaedic Board Review: High-Yield Clinical MCQs
Orthopaedic Board Review: High-Yield Clinical MCQs
This module contains 50 advanced orthopedic multiple-choice questions meticulously developed to mirror the American Board of Orthopaedic Surgery (ABOS) Part I and AAOS OITE examinations. These questions are comprehensively derived from the clinical teaching case: Orthopaedic Surgery Board Review: High-Yield MCQ Bank.
Comprehensive Exam
00:00
Start Quiz
Question 1
A 55-year-old patient with end-stage renal disease presents with diffuse bone pain. Laboratory studies reveal significantly elevated parathyroid hormone (PTH) levels. Which of the following best explains the primary mechanism for the elevated PTH in this patient?
Explanation
Correct Answer: Impaired renal degradation and clearance of PTH
The kidney is the primary organ responsible for the metabolic clearance and degradation of parathyroid hormone (PTH). In patients with chronic kidney disease (CKD) or end-stage renal disease, impaired renal function leads to decreased clearance of PTH, contributing to secondary hyperparathyroidism. Additionally, failing kidneys cannot adequately convert 25-hydroxyvitamin D to its active form (1,25-dihydroxyvitamin D), leading to hypocalcemia, which further stimulates PTH secretion.
Question 2
A 6-year-old boy sustains a widely displaced extension-type supracondylar humerus fracture. He subsequently develops severe, unrelenting forearm pain exacerbated by passive finger extension. If left untreated, this condition will most likely progress to a contracture primarily involving which of the following muscle groups?
Explanation
Correct Answer: Wrist flexors and forearm pronators
The patient is presenting with signs of acute compartment syndrome, a feared complication of supracondylar humerus fractures. If untreated, the ischemia leads to muscle necrosis and subsequent fibrosis, known as Volkmann's ischemic contracture. The deep flexor compartment of the forearm (specifically the flexor digitorum profundus and flexor pollicis longus) is most severely affected due to its proximity to the anterior interosseous artery and median nerve, leading to a classic flexion contracture of the wrist and fingers.
Question 3
During the reparative phase of secondary fracture healing in a diaphyseal tibia fracture treated with a cast, a soft callus forms. Which of the following biological processes is primarily responsible for the initial stabilization of the fracture site during this specific phase?
Explanation
Correct Answer: Proliferation of chondrocytes and production of a cartilaginous matrix
Secondary fracture healing occurs in stages: hematoma formation (inflammation), soft callus formation (reparative), hard callus formation, and remodeling. The soft callus phase is characterized by endochondral ossification, where mesenchymal stem cells differentiate into chondrocytes that produce a cartilaginous matrix. This cartilage bridges the fracture gap and provides initial semi-rigid stabilization before being replaced by woven bone (hard callus).
Question 4
A 22-year-old basketball player sustains an inversion ankle sprain while landing from a jump. The ankle was in a plantarflexed position at the time of injury. Which of the following ligaments is the primary restraint to anterior translation of the talus within the mortise in this specific foot position?
Explanation
Correct Answer: Anterior talofibular ligament
The anterior talofibular ligament (ATFL) is the weakest of the lateral ankle ligaments and the most commonly injured in an inversion sprain. Biomechanically, when the ankle is in plantarflexion, the ATFL is taut and serves as the primary restraint to anterior translation of the talus. The calcaneofibular ligament (CFL) becomes the primary restraint when the ankle is in dorsiflexion.
Question 5
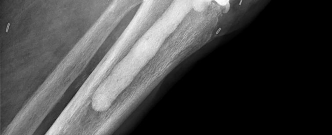
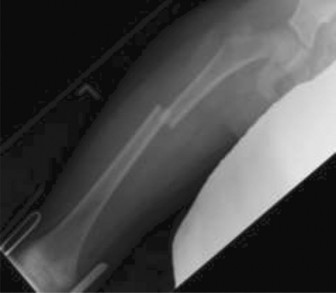
A 15-year-old boy presents with progressive distal thigh pain. Radiographs reveal a mixed lytic and sclerotic lesion in the distal femoral metaphysis with a 'sunburst' periosteal reaction and Codman's triangle. A biopsy is performed. Which of the following histological findings is required to confirm the most likely diagnosis?
Explanation
Correct Answer: Production of osteoid matrix by malignant mesenchymal cells
The clinical and radiographic presentation (sunburst pattern, Codman's triangle, metaphyseal location in an adolescent) is classic for osteosarcoma. The defining histological hallmark required for the diagnosis of osteosarcoma is the production of malignant osteoid (unmineralized bone matrix) directly by malignant mesenchymal cells. Small round blue cells describe Ewing sarcoma, while lobules of cartilage describe chondrosarcoma.
Question 6
A 45-year-old man presents with acute onset of severe low back pain radiating down the posterolateral aspect of his left leg to the dorsum of his foot. Physical examination reveals 3/5 strength in great toe extension and decreased sensation over the first dorsal web space. The patellar and Achilles tendon reflexes are symmetric and 2+. Which of the following nerve roots is most likely compressed?
Explanation
Correct Answer: L5
This patient presents with a classic L5 radiculopathy. The L5 nerve root supplies motor innervation to the extensor hallucis longus (great toe extension) and provides sensory innervation to the dorsum of the foot, specifically the first dorsal web space. The L4 root is associated with the patellar reflex and anterior tibialis (ankle dorsiflexion), while the S1 root is associated with the Achilles reflex, gastrocnemius (ankle plantarflexion), and sensation to the lateral aspect of the foot.
Question 7
A 13-year-old obese male presents with a 3-week history of left groin pain and a limp. On examination, as the left hip is passively flexed, it obligatorily externally rotates. Radiographs confirm a slipped capital femoral epiphysis (SCFE). Relative to the capital femoral epiphysis, in which direction is the femoral neck (metaphysis) typically displaced in this condition?
Explanation
Correct Answer: Anterior and superior
In a Slipped Capital Femoral Epiphysis (SCFE), the capital femoral epiphysis remains anatomically seated within the acetabulum while the femoral neck (metaphysis) displaces. Because the epiphysis effectively 'slips' posterior and inferior relative to the neck, the biomechanical reality is that the femoral neck displaces anterior and superior relative to the epiphysis. This creates the classic external rotation deformity seen clinically.
Question 8
A 30-year-old woman sustains a closed, displaced midshaft humerus fracture after a fall. On initial examination, she is unable to actively extend her wrist or fingers. Sensation is decreased over the dorsal aspect of the first web space. Which of the following is the most appropriate initial management for this specific neurological deficit?
Explanation
Correct Answer: Observation and supportive splinting
The patient has a radial nerve palsy, which is the most common neurological injury associated with midshaft humerus fractures. In the setting of a closed fracture, the vast majority of these injuries are neuropraxias that will resolve spontaneously over 3 to 4 months. The standard of care is observation and supportive splinting (e.g., a wrist extension splint) to prevent contractures. Immediate exploration is generally reserved for open fractures, penetrating trauma, or palsies that develop after closed reduction.
Question 9
A 24-year-old man falls on an outstretched hand and presents with anatomic snuffbox tenderness. Radiographs reveal a non-displaced fracture through the waist of the scaphoid. He is placed in a thumb spica cast. The high risk of avascular necrosis and nonunion in this fracture pattern is primarily due to the retrograde blood supply to the proximal pole. Which of the following vessels provides this critical blood supply?
Explanation
Correct Answer: Dorsal carpal branch of the radial artery
The scaphoid has a precarious retrograde blood supply. The primary blood supply enters the distal pole of the scaphoid via branches of the radial artery, specifically the dorsal carpal branch, and flows proximally. A fracture through the waist of the scaphoid can disrupt this retrograde flow, leaving the proximal pole ischemic and at high risk for avascular necrosis and nonunion.
Question 10
A 75-year-old woman sustains a displaced intracapsular femoral neck fracture. She is at high risk for developing avascular necrosis of the femoral head due to disruption of its primary blood supply. Which of the following arteries is the predominant source of vascularity to the weight-bearing portion of the adult femoral head?
Explanation
Correct Answer: Medial circumflex femoral artery
The medial circumflex femoral artery (MCFA) is the dominant blood supply to the adult femoral head. It gives rise to the lateral epiphyseal artery, which supplies the critical weight-bearing superolateral portion of the femoral head. Displaced intracapsular femoral neck fractures frequently tear these retinacular vessels, leading to a high incidence of avascular necrosis. The artery of the ligamentum teres provides a negligible amount of blood supply in adults.
Question 11
A 6-year-old boy sustains an extension-type supracondylar humerus fracture with posterolateral displacement of the distal fragment. Based on the typical displacement pattern, which of the following physical exam findings is most likely to be present if the most commonly associated nerve injury occurred?
Explanation
Correct Answer: Inability to flex the distal interphalangeal joint of the index finger
In extension-type supracondylar humerus fractures, the direction of distal fragment displacement dictates the nerve most at risk. Posterolateral displacement of the distal fragment causes the proximal fragment to displace anteromedially, putting the median nerve (specifically the anterior interosseous nerve, AIN) at greatest risk. The AIN innervates the flexor pollicis longus (FPL) and the flexor digitorum profundus (FDP) to the index and middle fingers. An AIN palsy presents as an inability to flex the IP joint of the thumb and the DIP joint of the index finger (making an 'A-OK' sign is impossible). Posteromedial displacement puts the radial nerve at risk.
Question 12
The medial circumflex femoral artery (MCFA) provides the primary blood supply to the adult femoral head. During a posterior approach to the hip (Moore or Southern approach), the main branch of the MCFA is most at risk of iatrogenic injury during the surgical release of which of the following structures?
Explanation
Correct Answer: Quadratus femoris muscle
The medial circumflex femoral artery (MCFA) is the dominant blood supply to the femoral head. Its ascending branch runs deep to the quadratus femoris and along its superior border. During a posterior approach to the hip, releasing the quadratus femoris too far medially or aggressively can result in iatrogenic injury to the MCFA, potentially compromising the blood supply to the femoral head and increasing the risk of avascular necrosis.
Question 13
A 22-year-old male sustains a proximal pole scaphoid fracture. The high risk of avascular necrosis and nonunion in this specific region is primarily due to the retrograde intraosseous blood supply derived from branches of which of the following arteries?
Explanation
Correct Answer: Radial artery
The scaphoid receives its primary blood supply from the dorsal carpal branch of the radial artery. The blood vessels enter the scaphoid at the dorsal ridge near the waist and supply the bone in a retrograde fashion (from distal to proximal). Because of this retrograde flow, fractures at the proximal pole of the scaphoid frequently disrupt the blood supply to the proximal fragment, leading to a high incidence of avascular necrosis and nonunion.
Question 14
A 10-year-old sustains a Salter-Harris Type II fracture of the distal radius. Through which specific histologic zone of the physis does the fracture line primarily propagate before exiting through the metaphysis?
Explanation
Correct Answer: Zone of hypertrophy
Physeal fractures, including Salter-Harris types, typically propagate through the zone of hypertrophy. This zone is biomechanically the weakest area of the growth plate because the chondrocytes are enlarged (hypertrophic) and the extracellular matrix is relatively sparse. The fracture line usually spares the reserve and proliferative zones, which is why growth potential is often maintained in Type I and II fractures, provided the blood supply is intact.
Question 15
A 15-year-old male is diagnosed with conventional osteosarcoma of the distal femur. Which of the following tumor suppressor gene mutations is most strongly associated with the pathogenesis of this primary bone malignancy?
Explanation
Correct Answer: RB1
Osteosarcoma is strongly associated with mutations in the RB1 (retinoblastoma) and TP53 (Li-Fraumeni syndrome) tumor suppressor genes. Patients with hereditary retinoblastoma (germline RB1 mutation) have a significantly increased risk of developing osteosarcoma. EXT1 is associated with multiple hereditary exostoses (osteochondromas), NF1 with neurofibromatosis, GNAS with fibrous dysplasia, and APC with familial adenomatous polyposis (and Gardner syndrome, which includes osteomas).
Question 16
A 3-month-old female is being treated with a Pavlik harness for developmental dysplasia of the hip (DDH). During a follow-up visit, the parents report that the infant has stopped kicking her leg on the treated side. On examination, there is an absence of active knee extension. This complication is most likely due to which of the following positioning errors?
Explanation
Correct Answer: Excessive hip flexion
The Pavlik harness is used to treat DDH by maintaining the hips in flexion and abduction. However, improper application can lead to severe complications. Excessive hip flexion (typically >120 degrees) can compress the femoral nerve against the inguinal ligament, leading to a transient femoral nerve palsy, which presents as an inability to actively extend the knee. Conversely, excessive hip abduction places the medial circumflex femoral artery at risk, potentially causing avascular necrosis (AVN) of the femoral head.
Question 17
A 45-year-old male sustains an acute Achilles tendon rupture during a tennis match. The rupture most commonly occurs in a hypovascular 'watershed' region. Approximately how far proximal to the calcaneal insertion is this zone located?
Explanation
Correct Answer: 2 to 6 cm
The Achilles tendon has a hypovascular zone located approximately 2 to 6 cm proximal to its insertion on the calcaneus. This 'watershed' area receives less blood supply compared to the proximal and distal portions of the tendon, making it the most susceptible region to degeneration and acute rupture, particularly in middle-aged individuals engaging in episodic athletic activities.
Question 18
A 42-year-old avid cyclist presents with numbness in the small finger and ulnar half of the ring finger, consistent with Guyon's canal syndrome. Which of the following structures forms the lateral boundary of this anatomic canal?
Explanation
Correct Answer: Hook of the hamate
Guyon's canal (the ulnar tunnel) is a fibro-osseous tunnel at the wrist through which the ulnar nerve and artery pass. The boundaries are: the volar carpal ligament (roof), the transverse carpal ligament and pisohamate ligament (floor), the pisiform (medial wall), and the hook of the hamate (lateral wall). Compression here, often seen in cyclists ('handlebar palsy'), affects the ulnar nerve.
Question 19
A 28-year-old farmer sustains a highly contaminated open tibial shaft fracture with extensive soft tissue stripping and a 12 cm laceration after a tractor accident. According to classic evidence-based guidelines, which of the following intravenous antibiotic regimens is most appropriate for initial management?
Explanation
Correct Answer: First-generation cephalosporin, an aminoglycoside, and high-dose penicillin
This is a Gustilo-Anderson Type III open fracture with heavy farm/soil contamination. Standard protocol for Type I and II open fractures includes a first-generation cephalosporin (e.g., cefazolin). For Type III fractures, an aminoglycoside (e.g., gentamicin) is added for expanded Gram-negative coverage. When there is farm, soil, or standing water contamination, high-dose penicillin is classically added to cover anaerobic organisms, specifically Clostridium species, to prevent gas gangrene.
Question 20
The anterior cruciate ligament (ACL) is composed of two distinct functional bundles. Which of the following statements correctly describes the biomechanical role of the anteromedial (AM) bundle?
Explanation
Correct Answer: It is tightest in flexion and primarily resists anterior tibial translation.
The ACL consists of the anteromedial (AM) and posterolateral (PL) bundles, named for their tibial insertion sites. The AM bundle is tightest in knee flexion and is the primary restraint to anterior tibial translation. The PL bundle is tightest in knee extension and is the primary restraint to rotatory loads (pivot shift). Understanding this anatomy is crucial for anatomic ACL reconstruction techniques.
Question 21
The primary blood supply to the adult femoral head is derived from the medial circumflex femoral artery (MCFA). Which specific branch of the MCFA provides the majority of this perfusion, and what is its anatomical relationship to the hip joint?
Explanation
Correct Answer: B
The lateral epiphyseal artery, a terminal branch of the medial circumflex femoral artery (MCFA), provides the majority of the blood supply to the adult femoral head. It courses posterosuperiorly along the femoral neck within the retinacular folds before penetrating the head. Disruption of this specific vascular pathway is the primary cause of avascular necrosis following displaced femoral neck fractures.
Question 22
A 6-year-old boy sustains a severe extension-type supracondylar humerus fracture. He subsequently develops untreated compartment syndrome leading to Volkmann's ischemic contracture. Which of the following muscle groups in the forearm is typically the most severely affected by this ischemic process?
Explanation
Correct Answer: C
Volkmann's ischemic contracture most severely affects the deep volar compartment of the forearm. The flexor digitorum profundus (FDP) and flexor pollicis longus (FPL) are the most profoundly affected muscles due to their central location and reliance on the anterior interosseous artery, which is highly susceptible to ischemic compromise during severe swelling.
Question 23
During the reparative phase of secondary fracture healing, a soft callus forms to stabilize the fracture site. Which of the following best describes the predominant collagen type synthesized during this specific stage, and the primary cell type responsible?
Explanation
Correct Answer: B
The soft callus phase of secondary fracture healing is characterized by the formation of cartilaginous tissue. Chondrocytes proliferate in the hypoxic environment of the fracture gap and synthesize a matrix predominantly composed of Type II collagen. This soft callus is later replaced by woven bone (Type I collagen) during the hard callus phase via endochondral ossification.
Question 24
Guyon's canal syndrome involves compression of the ulnar nerve at the wrist. Which of the following structures forms the floor of this anatomical canal?
Explanation
Correct Answer: B
Guyon's canal is a fibro-osseous tunnel at the ulnar aspect of the wrist. The roof is formed by the volar carpal ligament. The floor is formed by the transverse carpal ligament (flexor retinaculum) and the pisohamate ligament. The medial (ulnar) boundary is the pisiform, and the lateral (radial) boundary is the hook of the hamate.
Question 25
Slipped Capital Femoral Epiphysis (SCFE) typically presents with posterior and inferior displacement of the epiphysis relative to the femoral neck. Through which specific histological zone of the physis does this failure primarily occur?
Explanation
Correct Answer: C
In SCFE, the mechanical failure and subsequent slippage occur primarily through the zone of hypertrophy of the physis. This zone is structurally the weakest because it lacks the abundant collagen matrix found in the proliferative zone and has not yet been reinforced by the calcification seen in the zone of provisional calcification.
Question 26
A 45-year-old farmer sustains a highly contaminated open tibial shaft fracture after his leg is caught in a tractor mechanism (Gustilo-Anderson Type III). In addition to immediate surgical debridement and a first-generation cephalosporin, which of the following antibiotic regimens is most appropriate to add for this specific injury profile?
Explanation
Correct Answer: B
For a Gustilo-Anderson Type III open fracture, broad-spectrum coverage including a first-generation cephalosporin and an aminoglycoside (like gentamicin) or a third-generation cephalosporin is standard to cover Gram-positive and Gram-negative organisms. Because this is a farm injury with gross soil/fecal contamination, there is a high risk of Clostridium infection, necessitating the addition of Penicillin.
Question 27
A 15-year-old male is diagnosed with osteosarcoma of the distal femur, characterized radiographically by a 'sunburst' pattern. Which of the following genetic mutations is most strongly associated with the pathogenesis of this primary bone tumor?
Explanation
Correct Answer: D
Osteosarcoma is strongly associated with mutations in tumor suppressor genes, most notably RB1 (associated with hereditary retinoblastoma) and TP53 (associated with Li-Fraumeni syndrome). The t(11;22) translocation is seen in Ewing sarcoma. EXT mutations are linked to multiple hereditary exostoses (osteochondromas). GNAS1 is associated with fibrous dysplasia. The t(X;18) translocation is seen in synovial sarcoma.
Question 28
A patient presents with an L5 radiculopathy due to a paracentral disc herniation at L4-L5. Which of the following physical examination findings is most specific to an isolated L5 nerve root deficit?
Explanation
Correct Answer: B
An L5 radiculopathy classically presents with weakness in the extensor hallucis longus (great toe extension), weakness in ankle dorsiflexion (tibialis anterior, though L4 also contributes), and sensory deficits over the dorsum of the foot, specifically the first dorsal web space. The Achilles reflex is mediated by S1, and the patellar reflex is mediated by L4.
Question 29
The anterior cruciate ligament (ACL) is the primary restraint to anterior tibial translation. It is composed of two distinct functional bundles. Which of the following statements correctly describes the biomechanical behavior of these bundles during knee range of motion?
Explanation
Correct Answer: B
The ACL consists of the anteromedial (AM) and posterolateral (PL) bundles. Biomechanically, the AM bundle is tight in knee flexion and is the primary restraint to anterior translation at 90 degrees of flexion. The PL bundle is tight in knee extension and is the primary restraint to rotatory loads and anterior translation in near-full extension.
Question 30
A 3-month-old female is being treated with a Pavlik harness for developmental dysplasia of the hip (DDH). During a follow-up visit, the physician notes that the infant is no longer actively extending her knee on the treated side. Which of the following positioning errors in the harness is the most likely cause of this complication?
Explanation
Correct Answer: C
The Pavlik harness maintains the hip in flexion and abduction. Excessive hip flexion (typically greater than 120 degrees) can cause compression of the femoral nerve against the inguinal ligament, leading to a transient femoral nerve palsy. This presents clinically as an inability to actively extend the knee due to quadriceps weakness. Conversely, excessive abduction is associated with avascular necrosis (AVN) of the femoral head.
Question 31
A 6-year-old boy sustains a severe extension-type supracondylar humerus fracture. Despite closed reduction and percutaneous pinning, he develops unrecognized compartment syndrome leading to Volkmann's ischemic contracture. Which of the following muscle groups is typically the most severely affected by the ischemic necrosis in this condition?
Explanation
Correct Answer: B
Volkmann's ischemic contracture is the classic sequela of untreated compartment syndrome in the forearm, often following supracondylar humerus fractures. The deep volar compartment is the most susceptible to ischemia due to its central location and vascular supply pattern. Consequently, the flexor digitorum profundus (FDP) and flexor pollicis longus (FPL) are the most severely affected muscles, leading to the characteristic flexion deformities of the fingers and thumb.
Question 32
During the reparative phase of secondary fracture healing, a soft callus forms to bridge the fracture gap. Which of the following biological conditions most strongly favors the differentiation of mesenchymal stem cells into chondrocytes rather than osteoblasts during this phase?
Explanation
Correct Answer: B
Secondary fracture healing involves soft callus formation via endochondral ossification. The fracture hematoma and early reparative tissue are relatively avascular, resulting in a hypoxic environment (low oxygen tension). This hypoxia, combined with moderate mechanical strain (interfragmentary motion), drives mesenchymal stem cells to differentiate into chondrocytes to form the cartilaginous soft callus. High oxygen tension and rigid stability would instead favor direct (primary) bone healing or intramembranous ossification.
Question 33
A 15-year-old male presents with a painful, enlarging mass in his distal femur. Radiographs demonstrate a destructive metaphyseal lesion with a 'sunburst' periosteal reaction. Biopsy confirms osteosarcoma. Mutations in which of the following pairs of tumor suppressor genes are most strongly implicated in the pathogenesis of this patient's primary bone malignancy?
Explanation
Correct Answer: C
Osteosarcoma is the most common primary malignant bone tumor in adolescents. It is strongly associated with mutations in the RB1 (retinoblastoma) and TP53 (Li-Fraumeni syndrome) tumor suppressor genes. Loss of heterozygosity or mutation in these genes disrupts normal cell cycle regulation, leading to uncontrolled osteoblastic proliferation and malignant transformation.
Question 34
The anterior cruciate ligament (ACL) is the primary restraint to anterior tibial translation. It is composed of two distinct functional bundles. Which of the following statements accurately describes the biomechanical behavior of these bundles during knee range of motion?
Explanation
Correct Answer: B
The ACL consists of the anteromedial (AM) and posterolateral (PL) bundles, named for their tibial insertion sites. Biomechanically, the AM bundle tightens during knee flexion, providing primary restraint to anterior translation in the flexed position. Conversely, the PL bundle tightens during knee extension and is the primary restraint to rotatory loads (such as those tested during a pivot shift) when the knee is near full extension.
Question 35
A 45-year-old male presents with foot drop and numbness over the dorsum of his left foot. To clinically differentiate an L5 radiculopathy from a common peroneal nerve palsy, the examiner should test the strength of which of the following muscles?
Explanation
Correct Answer: D
Both L5 radiculopathy and common peroneal nerve palsy can cause foot drop (weakness of the tibialis anterior and extensor hallucis longus) and numbness over the dorsum of the foot. However, the tibialis posterior muscle is innervated by the tibial nerve but receives its segmental innervation primarily from the L5 nerve root. Therefore, weakness in foot inversion (tibialis posterior function) indicates an L5 radiculopathy, whereas normal inversion strength points to an isolated common peroneal nerve lesion.
Question 36
A 12-year-old obese male presents with a painful limp and an obligate external rotation of the hip during flexion. Radiographs confirm a slipped capital femoral epiphysis (SCFE). The mechanical failure of the physis in this condition predominantly occurs through which of the following histologic zones?
Explanation
Correct Answer: C
Slipped capital femoral epiphysis (SCFE) involves the displacement of the proximal femoral epiphysis relative to the metaphysis. The biomechanical failure and slippage occur almost exclusively through the zone of hypertrophy of the physis. This zone is structurally the weakest because it lacks the abundant collagenous matrix found in the proliferative zone and the calcified matrix found in the zone of provisional calcification.
Question 37
A 22-year-old male falls on an outstretched hand and sustains a non-displaced fracture of the proximal pole of the scaphoid. He is at a high risk for avascular necrosis (AVN) and nonunion. This risk is primarily due to the scaphoid's retrograde blood supply, which predominantly enters the bone at which of the following anatomical locations?
Explanation
Correct Answer: C
The scaphoid has a tenuous, retrograde blood supply. The major blood supply (70-80%) comes from branches of the radial artery that enter the bone at the dorsal ridge (distal to the waist) and flow proximally. Because of this retrograde flow, fractures at the waist or proximal pole disrupt the blood supply to the proximal fragment, significantly increasing the risk of avascular necrosis and nonunion.
Question 38
A 3-month-old female is being treated with a Pavlik harness for developmental dysplasia of the hip (DDH). During a follow-up visit, the parents report that the infant has stopped kicking her right leg. On examination, there is an absence of active knee extension on the right side. This complication is most likely due to which of the following improper harness adjustments?
Explanation
Correct Answer: C
The Pavlik harness is the standard initial treatment for DDH in infants under 6 months. Proper positioning is crucial. Excessive flexion of the hip (caused by anterior straps being too tight) can compress the femoral nerve against the inguinal ligament, leading to a transient femoral nerve palsy. This manifests clinically as decreased kicking and absent active knee extension. Conversely, excessive abduction (posterior straps too tight) increases the risk of avascular necrosis of the femoral head.
Question 39
Acute hematogenous osteomyelitis in children most commonly localizes to the metaphysis of long bones. Which of the following anatomical features of the pediatric metaphysis is the primary reason for this specific localization?
Explanation
Correct Answer: B
In children, the metaphysis is the most common site for acute hematogenous osteomyelitis. The nutrient artery branches into small arterioles that form sharp, hairpin loops at the physeal border before emptying into large venous sinusoids. This anatomical arrangement causes sluggish, turbulent blood flow, which allows blood-borne bacteria to settle and proliferate in an area with relatively low local phagocytic activity.
Question 40
In an adult patient sustaining a displaced intracapsular femoral neck fracture, the primary blood supply to the femoral head is severely compromised. Which of the following vessels provides the majority of the arterial supply to the adult weight-bearing dome of the femoral head?
Explanation
Correct Answer: B
In adults, the primary blood supply to the femoral head comes from the medial circumflex femoral artery (MCFA). The MCFA gives rise to the lateral epiphyseal arteries (also known as the posterosuperior retinacular vessels), which penetrate the capsule and supply the majority of the weight-bearing dome of the femoral head. The artery of the ligamentum teres (derived from the obturator artery) provides a negligible supply in adults, making the head highly susceptible to avascular necrosis following a displaced femoral neck fracture.
Question 41
The kidney is the primary organ responsible for the clearance of parathyroid hormone (PTH). In a patient with end-stage renal disease, impaired clearance and altered vitamin D metabolism most commonly lead to which of the following secondary bone pathologies?
Explanation
Correct Answer: Secondary hyperparathyroidism
Impaired renal function leads to decreased phosphate excretion and decreased 1-alpha-hydroxylase activity (lowering active Vitamin D). This causes hypocalcemia, which stimulates the parathyroid glands to overproduce PTH, leading to secondary hyperparathyroidism and renal osteodystrophy.
Question 42
Volkmann's ischemic contracture is a feared complication of supracondylar humerus fractures in children. Which of the following muscle groups is most susceptible to the initial ischemic insult in this condition?
Explanation
Correct Answer: Deep flexors of the forearm
Volkmann's contracture results from untreated compartment syndrome of the forearm, typically following brachial artery compromise. The deep flexor compartment, specifically the flexor digitorum profundus (FDP) and flexor pollicis longus (FPL), is the most severely affected due to its central location and vulnerability to ischemia.
Question 43
During the reparative phase of secondary fracture healing, a soft callus is formed. Which of the following collagen types is predominantly synthesized during this specific stage of callus formation?
Explanation
Correct Answer: Type II collagen
The soft callus phase of fracture healing is characterized by the formation of cartilaginous tissue by chondrocytes. The predominant collagen in this cartilaginous soft callus is Type II collagen. As the soft callus undergoes endochondral ossification to become a hard callus, Type I collagen becomes predominant.
Question 44
A 45-year-old male presents with an L5 radiculopathy due to a paracentral disc herniation at L4-L5. Which of the following physical examination findings is most specific for isolating an L5 motor deficit?
Explanation
Correct Answer: Weakness in great toe extension
The L5 nerve root primarily innervates the extensor hallucis longus (EHL), which is responsible for great toe extension. Testing EHL strength is the most specific motor test for L5 radiculopathy. Ankle dorsiflexion (tibialis anterior) is also L5 but has L4 contribution. The Achilles reflex is S1, and the patellar reflex is L4.
Question 45
Stable, non-displaced scaphoid fractures are at risk of nonunion due to the bone's precarious blood supply. Which of the following best describes the primary arterial supply to the proximal pole of the scaphoid?
Explanation
Correct Answer: Dorsal carpal branch of the radial artery entering distally and flowing retrogradely
The primary blood supply to the scaphoid comes from the dorsal carpal branch of the radial artery, which enters the bone at the dorsal ridge near the distal pole and flows retrogradely to supply the proximal pole. This retrograde blood supply makes proximal pole fractures highly susceptible to avascular necrosis and nonunion.
Question 46
Developmental dysplasia of the hip (DDH) has several known risk factors, including breech presentation. What is the primary biomechanical mechanism by which breech positioning in utero increases the risk of DDH?
Explanation
Correct Answer: Forced hip extension and adduction restricting normal acetabular development
Breech presentation forces the fetal hips into extreme flexion and limits abduction (often forcing adduction or extension depending on the exact breech type, but primarily restricting the normal flexed/abducted posture). This mechanical restriction prevents the femoral head from properly seating and stimulating the development of a deep, concentric acetabulum.
Question 47
The medial circumflex femoral artery (MCFA) is the dominant blood supply to the adult femoral head. Which specific branch of the MCFA is most critical for perfusing the weight-bearing superolateral aspect of the femoral head?
Explanation
Correct Answer: Lateral epiphyseal artery
The lateral epiphyseal artery system, which arises from the posterosuperior retinacular branches of the medial circumflex femoral artery (MCFA), provides the majority of the blood supply to the weight-bearing superolateral portion of the femoral head. Injury to these vessels during a femoral neck fracture leads to avascular necrosis.
Question 48
Paget's disease of bone is characterized by disorganized bone remodeling and a 'mosaic' pattern on histology. Which of the following represents the primary cellular abnormality that initiates the pathogenesis of this disease?
Explanation
Correct Answer: Hyperactive, multinucleated osteoclasts
The initial phase of Paget's disease is characterized by a marked increase in osteoclastic bone resorption. The osteoclasts in Paget's disease are abnormal, being larger and containing many more nuclei than normal osteoclasts. This intense resorption is followed by a disorganized, chaotic osteoblastic response, leading to the characteristic 'mosaic' woven bone.
Question 49
A 25-year-old male sustains a posterior hip dislocation in a motor vehicle collision. He subsequently demonstrates a foot drop. Which specific neural structure is most likely injured?
Explanation
Correct Answer: Peroneal division of the sciatic nerve
Posterior hip dislocations are frequently associated with sciatic nerve injuries (up to 10-20% of cases). The peroneal (fibular) division of the sciatic nerve is much more commonly injured than the tibial division because it is tethered at the sciatic notch and positioned more laterally and superficially, making it vulnerable to stretch or direct compression by the displaced femoral head.
Question 50
A Salter-Harris Type II fracture involves the physis and extends through the metaphysis. The characteristic metaphyseal bone fragment that remains attached to the epiphysis is known by which of the following eponyms?
Explanation
Correct Answer: Thurston-Holland fragment
In a Salter-Harris Type II fracture, the fracture line travels through the physis and exits through the metaphysis. The triangular piece of metaphyseal bone that breaks off and remains attached to the epiphyseal fragment is classically referred to as the Thurston-Holland fragment.
You Might Also Like