Complex Pilon Fracture (AO/OTA C3): Detailed Case Study & Diagnostic Approach
Key Takeaway
Diagnosing a complex AO/OTA C3 pilon fracture requires clinical assessment for soft tissue and neurovascular status. Crucially, CT scans with 3D reconstructions precisely map articular fragmentation and metaphyseal defects. This detailed imaging ensures accurate classification and informs comprehensive pre-operative surgical planning.
Patient Presentation and History
A 45-year-old male presented to the Level I Trauma Center Emergency Department following a high-energy motor vehicle collision. The patient was an unrestrained driver involved in a frontal impact at highway speeds, resulting in significant lower extremity trauma. The mechanism of injury involved the right lower leg bearing the brunt of the kinetic energy transfer, consistent with a severe axial loading force applied to the ankle plafond while the foot was positioned in dorsiflexion.
Past medical history was significant for Type 2 Diabetes Mellitus, currently managed with oral hypoglycemic agents. Hemoglobin A1c on admission was 7.2 percent, indicating moderate glycemic control. The patient also reported a 20-pack-year smoking history, with successful cessation five years prior to the current presentation. He had no prior history of lower extremity trauma, peripheral neuropathy, peripheral vascular disease, or prior orthopedic surgical interventions. Socially, the patient was employed as a heavy construction worker, indicating a physically demanding occupation that requires prolonged weight-bearing, climbing, and navigating uneven terrain.
Upon initial Advanced Trauma Life Support assessment in the trauma bay, the primary survey revealed an intact airway, bilateral breath sounds, and hemodynamic stability. The secondary survey isolated the primary pathology to the right lower extremity. The patient reported excruciating, unremitting pain in his right ankle, rendering him absolutely unable to bear weight. He endorsed rapid, progressive swelling and a subjective sensation of gross anatomical deformity. No other immediately life-threatening injuries, including closed head injuries, thoracic trauma, or abdominopelvic visceral injuries, were identified.
The mechanism of injury—axial loading combined with a high-velocity deceleration—is the classic generator of the pilon (or pestle) fracture. The talus acts as a hammer, driving upward into the distal tibial articular surface, causing catastrophic comminution of the weight-bearing plafond and explosive expansion of the metaphyseal bone. The patient's underlying comorbidities, specifically the history of smoking and diabetes, immediately risk-stratify him into a higher-tier category for postoperative complications, including delayed union, nonunion, surgical site infection, and catastrophic soft tissue failure.
Clinical Examination Findings
Initial clinical examination of the right lower extremity revealed a severely swollen, tense, and ecchymotic right ankle and distal leg. Gross mechanical deformity of the distal tibia and disruption of the ankle mortise were immediately evident upon visual inspection.
Soft Tissue Envelope Assessment
Inspection demonstrated massive interstitial edema extending from the mid-tibial diaphysis distally into the hindfoot and midfoot, with palpable tenseness of the integument. Fracture blisters were actively developing over the anterior and medial aspects of the ankle joint. Both clear fluid-filled blisters (indicating cleavage at the dermo-epidermal junction) and hemorrhagic blisters (indicating deeper dermal ischemia and subepidermal cleavage) were present. This clinical picture is indicative of severe soft tissue compromise and impending skin necrosis driven by the massive internal expansion of the fracture hematoma and osseous displacement.
The injury was classified as a Tscherne and Oestern grade III closed soft tissue injury. No open traumatic wounds, lacerations, or punctate abrasions were present, confirming a closed fracture pattern. However, the skin appeared blanched and shiny in areas of maximal swelling, raising immediate clinical concern for acute compartment syndrome of the lower leg.
Palpation and Compartment Evaluation
Palpation elicited extreme, poorly localized tenderness across the entire distal tibia, medial malleolus, lateral malleolus, and syndesmotic regions. Gross osseous crepitus was elicited with minimal manipulation of the limb. The fascial compartments of the lower leg were palpably tense, with the anterior and deep posterior compartments exhibiting wood-like rigidity.
Given the high-energy axial load and the clinical exam, compartment pressures were measured utilizing a solid-state transducer intracompartmental catheter. Absolute pressures in the anterior compartment measured 38 mmHg, with a concurrent diastolic blood pressure of 75 mmHg. The calculated delta pressure (Diastolic BP minus Compartment Pressure) was 37 mmHg. While approaching the critical threshold of 30 mmHg, the decision was made to continuously monitor the limb clinically rather than proceed with emergent four-compartment fasciotomy, as the delta pressure remained reassuring and the patient maintained intact neurological function.
Vascular and Neurological Assessment
Vascular examination revealed diminished but palpable dorsalis pedis and posterior tibial pulses bilaterally, assessed via handheld Doppler ultrasound. Capillary refill was sluggish in the injured foot, measuring approximately 3 to 4 seconds, but distal perfusion was ultimately maintained. The Ankle-Brachial Index was calculated at 0.95, indicating adequate macrovascular arterial inflow despite the gross anatomical distortion.
Neurological assessment of motor function revealed grossly intact plantarflexion and dorsiflexion, though active excursion was severely limited by pain and mechanical block. Extensor hallucis longus and flexor hallucis longus functions were grossly intact. Sensory examination demonstrated intact light touch and two-point discrimination in the distributions of the superficial peroneal, deep peroneal, sural, saphenous, and tibial nerves. No definitive focal neurological deficit was identified, though the extreme pain profile necessitated careful, repeated examinations to ensure no delayed ischemic neuropathy developed.
Imaging and Diagnostics
Immediate radiographic assessment of the right lower extremity was initiated in the trauma bay to delineate the fracture morphology and guide initial temporizing management.
Initial Radiographic Findings
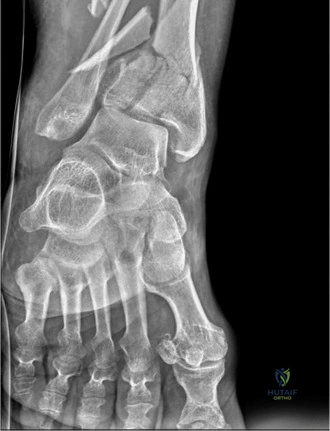
Standard trauma radiographs, including anteroposterior, lateral, and mortise views of the right ankle and full-length tibia and fibula, were obtained.
The radiographs demonstrated a highly comminuted, completely displaced intra-articular fracture of the distal tibia, classically defined as a pilon fracture. The articular surface of the tibial plafond was severely disrupted, with multiple articular fragments impacted proximally into the metaphyseal void. Significant metaphyseal comminution was present, resulting in a profound loss of tibial length and varus malalignment of the distal segment.
A concomitant, highly comminuted fracture of the distal fibula was identified at the level of the syndesmosis, contributing significantly to the loss of lateral column support and the total collapse of the ankle mortise integrity. The talus appeared displaced proximally and anteriorly, following the path of least resistance created by the axial loading mechanism and the destruction of the anterior tibial rim.

While the plain radiographs provided a macroscopic overview of the catastrophic osseous failure, the true complexity of the articular comminution, the degree of central die-punch impaction, and the exact orientation of the major fracture lines could not be fully appreciated.
Advanced Computed Tomography Analysis
An urgent Computed Tomography scan of the right ankle and distal leg, utilizing thin-slice axial acquisitions with two-dimensional multiplanar coronal and sagittal reformations, as well as three-dimensional volume rendering, was performed.
The CT scan is the absolute gold standard and a mandatory diagnostic modality for the preoperative planning of complex pilon fractures. The axial cuts revealed the classic three-fragment configuration of the distal tibia, alongside severe central articular impaction. The primary fragments identified included the medial malleolar fragment, the anterolateral Tillaux-Chaput fragment, and the posterolateral Volkmann fragment.
Furthermore, the coronal and sagittal reformations clearly delineated a massive central "die-punch" fragment consisting of purely articular cartilage and subchondral bone, devoid of soft tissue attachments, which had been driven deep into the distal tibial metaphysis. The CT also confirmed complete disruption of the distal tibiofibular syndesmosis, with the fibula fracture exhibiting severe comminution and shortening.
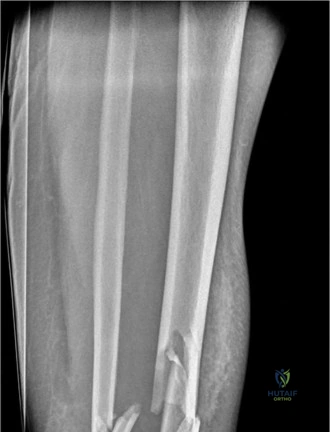
Preoperative Templating and Articular Mapping
Detailed articular mapping was conducted utilizing the CT dataset. The fracture lines were traced to understand the specific exit points through the tibial cortex. The primary fracture line exited anterolaterally, dictating the necessity for an anterolateral surgical approach to access the Chaput fragment and the central articular surface. A secondary fracture line exited medially, separating a large, vertically oriented medial malleolar fragment that extended proximally into the diaphyseal-metaphyseal junction.
Preoperative templating involved selecting the appropriate anatomically contoured locking plates for both the distal tibia and the fibula. The extensive metaphyseal comminution indicated that a bridging plate construct would be required to span the zone of injury, relying on relative stability to promote secondary bone healing in the metaphysis, while absolute stability and anatomical reduction would be strictly required for the articular block.
Differential Diagnosis
When evaluating high-energy trauma to the distal lower extremity presenting with gross deformity and severe soft tissue compromise, a precise diagnostic differentiation is critical. The management algorithms, surgical approaches, and prognostic implications vary significantly among these distinct clinical entities.
| Diagnostic Entity | Clinical Presentation Hallmarks | Radiographic and Advanced Imaging Hallmarks | Management and Prognostic Implications |
|---|---|---|---|
| AO/OTA 43-C Pilon Fracture | High-energy axial load mechanism. Massive swelling, Tscherne II-III soft tissue injury, fracture blisters. Extreme pain with axial loading of the heel. | Intra-articular extension into the tibial plafond. Metaphyseal comminution. Central die-punch fragments. Proximal talar migration. | Requires staged protocol (Span, Scan, Plan). High risk of soft tissue complications, deep infection, and post-traumatic ankle arthrosis. Complex articular reconstruction required. |
| Severe Trimalleolar Ankle Fracture (AO/OTA 44-C) | Rotational mechanism (pronation-external rotation or supination-external rotation). Swelling localized more specifically to the malleoli rather than the distal tibial shaft. | Fractures of the medial, lateral, and posterior malleoli. Syndesmotic disruption. Minimal to no metaphyseal comminution. Articular impaction is rare. | Can often be treated with primary ORIF if soft tissues allow. Focus is on restoring the mortise and syndesmotic stability. Lower risk of severe post-traumatic arthritis compared to pilon fractures. |
| Extra-articular Distal Tibia Fracture (AO/OTA 43-A) | Direct blow or torsional mechanism. Swelling and deformity in the distal third of the leg, but the ankle joint itself may have preserved, albeit painful, range of motion. | Fracture of the distal tibial metaphysis or diaphysis without extension into the weight-bearing articular surface of the plafond. | Can be managed with intramedullary nailing or minimally invasive plate osteosynthesis (MIPPO). Prognosis for ankle joint function is excellent as the articular cartilage is spared. |
| Complex Talar Body Fracture | Extreme axial load, often associated with falls from height or MVC floorboard intrusion. Pain localized deep within the hindfoot. | Comminuted fracture of the talar dome or body. Often associated with subtalar or tibiotalar subluxation. | High risk of avascular necrosis (AVN) of the talus and post-traumatic arthritis of both the ankle and subtalar joints. Requires precise anatomical reduction, often via dual approaches. |
Surgical Decision Making and Classification
The comprehensive evaluation of the clinical and radiographic data informed a meticulous surgical strategy.
Fracture Classification Systems
The injury was classified utilizing the AO/OTA alphanumeric system as a 43-C3 fracture. The "43" designates the distal tibia segment. The "C" indicates a complete articular fracture, meaning the articular surface is fractured and completely separated from the diaphyseal shaft. The "3" denotes multifragmentary metaphyseal and multifragmentary articular comminution. This represents the most severe and complex tier of distal tibia fractures.
Historically, this injury also aligns with a Rüedi-Allgöwer Type III classification, characterized by significant articular comminution and metaphyseal impaction. The presence of the fibula fracture further destabilizes the lateral column, mandating concurrent reconstruction to restore the lateral buttress of the ankle mortise.
Timing of Intervention and Staged Protocol
The paramount factor driving the surgical decision-making process in this case was the profound compromise of the soft tissue envelope. Attempting primary Open Reduction and Internal Fixation through Tscherne III soft tissues with active fracture blistering carries an unacceptably high risk of catastrophic wound dehiscence, deep hardware infection, and subsequent amputation.
Therefore, a strict, evidence-based staged protocol—often referred to as "Span, Scan, and Plan"—was initiated.
The primary objective of Stage One is immediate temporization. This involves the application of a spanning external fixator to restore tibial length, correct gross angular deformity, and provide rigid stabilization of the osseous segments. This mechanical stabilization dramatically reduces ongoing soft tissue trauma from mobile fracture fragments, halts the expansion of the fracture hematoma, and facilitates the resolution of interstitial edema.
Stage Two, the definitive articular reconstruction and internal fixation, is delayed until the soft tissue envelope has sufficiently recovered. The clinical indicator for soft tissue readiness is the return of skin wrinkles (the "wrinkle sign") and the re-epithelialization of fracture blisters, which typically occurs between 10 and 21 days post-injury.
Soft Tissue Optimization Strategy
Following the application of the temporizing external fixator, the patient was admitted for aggressive soft tissue management. This protocol included strict, continuous elevation of the right lower extremity above the level of the heart to maximize venous and lymphatic drainage. Cryotherapy was utilized adjunctively. The fracture blisters were treated with non-adherent, antimicrobial dressings, allowing them to desiccate and re-epithelialize naturally without aggressive debridement, which can convert a closed injury into an open wound.
Close monitoring for delayed presentation of compartment syndrome remained a priority during the first 48 hours post-injury. The patient's glycemic control was aggressively managed with a basal-bolus insulin regimen, targeting normoglycemia to optimize microvascular perfusion and mitigate the inherent wound healing deficits associated with Diabetes Mellitus.
Surgical Technique and Intervention
The surgical management of this complex AO/OTA 43-C3 pilon fracture was executed in two distinct operative stages, separated by a fourteen-day interval for soft tissue optimization.
Stage One Temporizing External Fixation
The patient was taken emergently to the operating room on the day of admission. Under general anesthesia, the patient was positioned supine on a radiolucent Jackson table.
A delta-frame spanning external fixator was constructed. Two 5.0mm hydroxyapatite-coated Schanz pins were placed percutaneously into the intact tibial diaphysis, well proximal to the zone of injury and planned future surgical incisions. A centrally threaded 5.0mm transfixion pin was placed through the calcaneal tuberosity, traversing from medial to lateral, taking meticulous care to avoid the medial neurovascular bundle.
Manual longitudinal traction was applied via the calcaneal pin to disimpact the articular fragments and restore the anatomical length of the medial and lateral columns. Multiplanar fluoroscopy confirmed the restoration of length, gross coronal and sagittal alignment, and the reduction of the talus beneath the tibial plafond. Carbon fiber rods and multi-pin clamps were utilized to construct a rigid, triangulated delta frame.
In this specific case, the decision was made to defer the open reduction and internal fixation of the fibula during Stage One. The soft tissue envelope over the lateral malleolus was severely compromised, and placing hardware beneath compromised skin during the acute inflammatory phase was deemed overly hazardous. Length was adequately maintained by the external fixator construct alone.
Stage Two Definitive Fixation Setup
Fourteen days post-injury, clinical examination revealed a positive wrinkle sign, resolution of the tense edema, and complete epithelialization of the fracture blisters. The patient was cleared for definitive Stage Two reconstruction.
The patient was positioned supine on a radiolucent table with a bump placed under the ipsilateral hip to internally rotate the leg to a neutral position. A sterile thigh tourniquet was applied but not initially inflated, reserved for critical portions of the articular visualization. The external fixator was prepped and draped into the sterile field to allow for controlled removal and transition to internal fixation.
Surgical Approach Selection
Based on the preoperative CT articular mapping, a dual-incision technique was selected to provide orthogonal access to the complex fracture geometry.
An anterolateral approach was utilized to access the Tillaux-Chaput fragment, the central die-punch fragments, and the lateral aspect of the tibial plafond. The incision was centered over the ankle joint, navigating the internervous plane between the superficial peroneal nerve laterally and the deep peroneal nerve medially. The extensor retinaculum was incised, and the extensor digitorum longus and peroneus tertius tendons were retracted medially, exposing the anterolateral joint capsule.
A posteromedial approach was utilized to address the massive medial malleolar fragment and the posteromedial metaphyseal extension. This incision was placed midway between the posterior border of the medial malleolus and the Achilles tendon. The posterior tibial tendon was retracted anteriorly, and the flexor digitorum longus was retracted posteriorly, granting direct access to the posterior colliculus and the medial metaphyseal cortex. A minimum skin bridge of 7 centimeters was strictly maintained between the anterolateral and posteromedial incisions to preserve the angiosomal blood supply to the intervening integument.
Articular Reduction and Provisional Fixation
The surgical sequence prioritized the anatomical reconstruction of the articular block from posterior to anterior, followed by the attachment of the reconstructed articular block to the tibial diaphysis.
The external fixator was removed. The fibula was addressed first through a direct lateral approach. The comminuted fibular fragments were mobilized, and anatomical length and rotation were restored. A one-third tubular plate was applied utilizing absolute stability principles with lag screws and neutralization plating. Restoring the fibula effectively rebuilt the lateral column, providing a template for the tibial length and a lateral buttress for the ankle mortise.
Attention was then turned to the tibial articular surface via the anterolateral approach. The joint capsule was opened, and the fracture hematoma was evacuated. A femoral distractor was applied, with pins in the talar neck and the proximal tibial shaft, to distract the joint and provide unparalleled visualization of the articular surface.
The central die-punch fragments were identified, elevated using a Freer elevator, and provisionally held with subchondral Kirschner wires. The Tillaux-Chaput fragment was then reduced to the central articular block. Concurrently, through the posteromedial approach, the medial malleolar fragment was reduced to the posterior Volkmann fragment and the central block.
The articular reduction was assessed directly under direct vision and fluoroscopically, confirming the restoration of a congruent joint surface with no step-offs greater than 1 millimeter. The provisional K-wire construct resembled a complex scaffolding holding the articular puzzle pieces in anatomical alignment.

Definitive Plate Osteosynthesis and Bone Grafting
Once the articular block was provisionally stabilized, definitive fixation was achieved using anatomically contoured, low-profile locking plates.
An anterolateral distal tibia locking plate was slid submuscularly along the lateral cortex. Locking screws were placed into the articular fragments to raft the subchondral bone and prevent late subsidence of the die-punch fragments. A medial distal tibia locking plate was applied via the posteromedial approach to buttress the medial column and neutralize varus deforming forces.
The severe metaphyseal comminution resulted in a significant structural void once the articular surface was disimpacted and elevated. To prevent late collapse and stimulate osteogenesis, the metaphyseal defect was packed with a combination of cancellous allograft and demineralized bone matrix.
The diaphyseal fixation was achieved using minimally invasive percutaneous plate osteosynthesis (MIPPO) techniques. The proximal portions of both the anterolateral and medial plates were secured to the intact tibial diaphysis utilizing percutaneous locking screws, carefully preserving the periosteal blood supply to the comminuted metaphyseal segment.
Final multiplanar fluoroscopy confirmed anatomical articular reduction, restoration of mechanical limb alignment, correct hardware placement, and no intra-articular screw penetration. The wounds were irrigated copiously and closed in a layered fashion, utilizing tension-free modified Donati sutures for the skin.
Post Operative Protocol and Rehabilitation
The postoperative management of a complex C3 pilon fracture is as critical as the surgical execution. The rehabilitation protocol must balance the need for early joint mobilization to prevent arthrofibrosis with the absolute necessity of protecting the fragile articular reconstruction and the compromised soft tissue envelope.
Immediate Postoperative Care
Postoperatively, the patient was placed in a well-padded, short-leg bulky Jones splint with a posterior plaster slab, maintaining the ankle in neutral dorsiflexion. Strict elevation of the limb above the heart was enforced for the first 48 to 72 hours.
Chemical deep vein thrombosis (DVT) prophylaxis was initiated utilizing low-molecular-weight heparin, given the patient's immobility and high-energy trauma status. Intravenous antibiotics (first-generation cephalosporin) were continued for 24 hours postoperatively. The patient was instructed on strict, absolute non-weight-bearing (NWB) status for the right lower extremity.
Outpatient Follow Up and Radiographic Monitoring
The patient was discharged on postoperative day three following satisfactory pain control and physical therapy clearance for safe crutch ambulation.
At the two-week outpatient follow-up, the splint was removed, and the surgical wounds were inspected. Suture removal was performed, noting excellent primary healing without marginal necrosis or dehiscence. The patient was transitioned to a removable controlled ankle motion (CAM) boot.
At this stage, early, controlled, active and active-assisted range of motion (ROM) exercises of the ankle and subtalar joints were initiated. The patient was instructed to remove the boot multiple times daily to perform dorsiflexion, plantarflexion, inversion, and eversion exercises. The absolute non-weight-bearing status was strictly maintained.
Serial clinical and radiographic evaluations were conducted at 6, 12, and 24 weeks postoperatively. Radiographs were scrutinized for maintenance of articular reduction, progression of metaphyseal callus formation, and any signs of hardware failure or loss of fixation.
Long Term Functional Rehabilitation
At 10 to 12 weeks postoperatively, upon radiographic evidence of bridging callus in the metaphysis and clinical absence of pain at the fracture site, a progressive weight-bearing protocol was initiated. The patient began with 25% partial weight-bearing, advancing by 25% weekly under the guidance of a physical therapist, until full weight-bearing was achieved.
Advanced rehabilitation focused on restoring triceps surae strength, peroneal tendon function, and proprioceptive balance training. Given the patient's occupation as a construction worker, work-hardening programs simulating uneven terrain and ladder climbing were incorporated into the late stages of therapy.
Despite anatomical reconstruction, the patient was extensively counseled regarding the long-term prognosis. High-energy C3 pilon fractures carry a significant risk of post-traumatic ankle arthrosis due to the initial irreversible damage to the chondrocyte viability at the moment of impact. The patient was educated that while the surgery restores the mechanical scaffolding, progressive joint space narrowing and stiffness may develop over the ensuing years, potentially necessitating future interventions such as ankle arthrodesis or total ankle arthroplasty.
Clinical Pearls and Pitfalls
The management of severe pilon fractures is fraught with potential complications. Adherence to strict biomechanical and physiological principles is mandatory for successful outcomes.
Strategic Pearls for Pilon Fractures
- Respect the Soft Tissue Envelope: The soft tissues dictate the timing of surgery. Never rush to internal fixation in the presence of Tscherne III swelling or active fracture blisters. The "Span, Scan, and Plan" protocol is the standard of care for a reason.
- CT is Mandatory for Preoperative Planning: Plain radiographs grossly underestimate the complexity of articular comminution. 2D and 3D CT reconstructions are essential for mapping the fracture lines and determining the precise surgical approaches.
- Restore the Fibula to Rebuild the Lateral Column: In cases with concomitant fibula fractures, restoring the fibula to its anatomical length and rotation provides a crucial template for tibial reconstruction and restores the lateral buttress of the ankle mortise.
- Utilize the Femoral Distractor: Applying a distractor across the ankle joint provides unparalleled visualization of the central articular surface, allowing for precise elevation and reduction of die-punch fragments that would otherwise be obscured.
- Bone Graft Metaphyseal Voids: Disimpacting the articular surface invariably leaves a significant metaphyseal defect. Filling this void with structural allograft or autograft is critical to support the articular block and prevent late subsidence.
Common Surgical Pitfalls to Avoid
- Incision Placement Errors: Failing to maintain a minimum 7-centimeter skin bridge between multiple incisions will reliably lead to angiosomal ischemia, skin necrosis, and catastrophic wound dehiscence.
- Operating Through Swollen Tissues: Attempting primary closure over a swollen, tense ankle joint significantly increases the risk of deep infection and hardware exposure. Patience is
