Mastering Shoulder Arthroplasty: A Comprehensive Intraoperative Guide
Key Takeaway
This masterclass provides an exhaustive, step-by-step guide to shoulder arthroplasty for glenohumeral arthritis. From meticulous preoperative planning and patient positioning to precise intraoperative execution, we cover comprehensive surgical anatomy, critical neurovascular considerations, and advanced techniques. Fellows will gain invaluable insights into preventing and managing complications, ensuring optimal outcomes for patients requiring humeral head or glenoid resurfacing.
Alright fellows, gather 'round. Welcome to the operating theater. Today, we're embarking on a journey through the intricate landscape of the shoulder, specifically focusing on shoulder arthroplasty for glenohumeral arthritis. The goal is to restore function and alleviate pain for our patients. While the raw text provided is fragmented, consisting primarily of anatomical labels and chapter titles, we will infer and construct a comprehensive, real-time surgical masterclass, integrating every single piece of information into a plausible and highly detailed procedure, likely a total shoulder arthroplasty (TSA) or hemiarthroplasty (HSA) via a deltopectoral approach. This will allow us to address both scenarios of an intact or irreparable rotator cuff, as suggested by the chapter titles.
Preoperative Planning & Patient Positioning
Before we even make an incision, meticulous planning is paramount. This isn't just about cutting bone; it's about understanding the patient's unique anatomy and pathology.
1. Imaging Review & Templating:
We've thoroughly reviewed our patient's radiographs, CT scans, and MRI. We're looking at the extent of glenoid erosion, the presence of posterior glenoid wear, humeral head deformity, and the status of the rotator cuff – specifically the supraspinatus, infraspinatus, and subscapularis tendons. Is the cuff intact, or are we dealing with an irreparable tear, which would influence our choice between TSA, HSA, or even reverse TSA? Today, let's assume we're preparing for a standard TSA with a potentially intact cuff, but ready for any contingency.
* Templating: We've templated our humeral stem size and glenoid component size, considering both reaming and potential bone grafting. This gives us a roadmap, but remember, the final decision is always made intraoperatively.
2. Patient Positioning: The Beach Chair Position
For shoulder arthroplasty, the beach chair position is our standard.
* Setup: The patient is placed supine on the operating table, and the torso is elevated to approximately 60 to 70 degrees, resembling a beach chair.
* Head Support: The head is secured in a well-padded headrest, ensuring the neck is neutral to prevent brachial plexus stretch.
* Arm Positioning: The operative arm is draped free, allowing full manipulation. We'll use an arm holder or a sterile Mayo stand to support the arm during various stages, permitting abduction, adduction, flexion, extension, and rotation.
* Torso & Legs: The torso is secured to the table with a chest strap. The legs are slightly flexed at the hips and knees, with sequential compression devices applied for DVT prophylaxis.
* Fluoroscopy Setup: The C-arm fluoroscopy unit is prepped and positioned to allow both AP and lateral (axillary) views of the shoulder without repositioning the patient or the arm. This is crucial for accurate glenoid component placement and humeral stem alignment.
Surgical Warning: Ensure adequate padding at all pressure points (occiput, elbows, heels) to prevent nerve palsies or skin breakdown. The non-operative arm should be abducted less than 90 degrees to avoid brachial plexus injury.
Comprehensive Surgical Anatomy: A Deeper Dive
Let's quickly review the critical anatomy we'll encounter, focusing on the structures mentioned in our raw text and their clinical relevance.
-
Bony Landmarks:
- Acromion: The lateral extension of the scapular spine, forming the roof of the shoulder.
- Clavicle: The collarbone, articulating with the acromion and sternum.
- Scapular spine: The prominent ridge on the posterior aspect of the scapula.
- Coracoid process: A hook-like projection from the scapula, serving as an attachment site for several muscles and ligaments (coracobrachialis, short head of biceps, pectoralis minor, coracoacromial, coracohumeral, coracoclavicular ligaments).
- Glenoid fossa: The shallow articular surface on the lateral aspect of the scapula, articulating with the humeral head. Its orientation and version are critical for implant stability.
- Native humeral head: The ball-shaped proximal end of the humerus, articulating with the glenoid.
-
Muscles & Tendons:
- Deltoid muscle: The large, powerful muscle forming the rounded contour of the shoulder. It has anterior, middle, and posterior fibers. We'll traverse its anterior fibers in a deltopectoral approach.
- Supraspinatus tendon: Originates from the supraspinous fossa, inserts on the greater tuberosity. Initiates abduction.
- Infraspinatus tendon: Originates from the infraspinous fossa, inserts on the greater tuberosity. External rotation.
- Teres minor tendon: Originates from the lateral border of the scapula, inserts on the greater tuberosity. External rotation. Together with supraspinatus and infraspinatus, it forms the posterior cuff.
- Subscapularis tendon: Originates from the subscapular fossa, inserts on the lesser tuberosity. Internal rotation. This is the anterior cuff tendon we'll release.
- Long head of biceps tendon: Originates from the supraglenoid tubercle, courses through the bicipital groove. Often tenotomized or tenodesed during arthroplasty.
- Teres major muscle and tendon: Originates from the inferior angle of the scapula, inserts on the medial lip of the bicipital groove. Adduction and internal rotation. Forms the inferior border of the quadrangular space.
- Latissimus muscle and tendon: Originates from the thoracolumbar fascia, iliac crest, and ribs, inserts into the bicipital groove. Adduction, extension, internal rotation.
- Pectoralis major muscle (and its "sternal head"): The large chest muscle. The deltopectoral interval lies between the deltoid and pectoralis major. The "sternal head" refers to the larger portion originating from the sternum, as opposed to the clavicular head. This interval is a safe plane.
-
Ligaments & Capsule:
- Rotator interval: The triangular space between the anterior edge of the supraspinatus and the superior edge of the subscapularis, containing the superior glenohumeral ligament and coracohumeral ligament, and the long head of biceps tendon sheath.
- Superior glenohumeral ligament (SGHL): Reinforces the superior capsule.
- Middle glenohumeral ligament (MGHL): Reinforces the anterior capsule.
- Inferior glenohumeral ligament (IGHL): The primary stabilizer against anterior dislocation, composed of an anterior band, posterior band, and axillary pouch.
- Inferior joint capsule: The lowest portion of the glenohumeral joint capsule.
- Glenoid labrum: A fibrocartilaginous rim around the glenoid fossa, deepening it and providing attachment for the glenohumeral ligaments.
-
Bursae:
- Subacromial bursa: Located between the acromion/deltoid and the rotator cuff. Often inflamed in impingement and typically resected during arthroplasty to improve visualization.
- Infraserratus bursa, Supraserratus bursa, Trapezoid bursa: These are less commonly encountered directly in a standard deltopectoral approach for arthroplasty but are important anatomical considerations for other posterior or scapulothoracic procedures. The serratus bursae facilitate scapulothoracic motion. The trapezoid bursa is deep to the trapezius.
-
Neurovascular Structures:
- Suprascapular nerve and vessels: The nerve arises from the upper trunk of the brachial plexus (C5, C6) and passes through the suprascapular notch (under the superior transverse scapular ligament) to innervate the supraspinatus and infraspinatus muscles. The vessels accompany the nerve. It's at risk during glenoid preparation, especially with excessive posterior reaming or screw placement.
- Axillary nerve: Courses inferior to the humeral head, wraps around the surgical neck of the humerus, innervating the deltoid and teres minor. At risk during humeral head dislocation, retraction, and inferior capsular release.
- Musculocutaneous nerve: Supplies the coracobrachialis, biceps, and brachialis. At risk during excessive medial retraction of the conjoined tendon (coracobrachialis and short head of biceps).
- Brachial plexus: A network of nerves supplying the upper limb, vulnerable to traction injuries, especially in the beach chair position.
- Axillary artery and vein: Major vessels in the axilla, deep to the pectoralis major and coracobrachialis.
Step-by-Step Intraoperative Execution (The Operating Surgeon's Viewpoint)
Alright, fellows, let's get scrubbed in. We've got our patient positioned, prepped, and draped. The fluoroscopy unit is ready.
1. Incision and Initial Dissection:
"Scalpel please. We'll make a standard deltopectoral incision, about 8-10 cm in length, starting just lateral to the coracoid process and extending distally along the deltopectoral groove. This allows excellent exposure for both humeral and glenoid components."
"Now, let's deepen the incision through the skin and subcutaneous tissue. We're looking for the cephalic vein, which marks our deltopectoral interval. Dr. Smith, can you gently retract the skin edges? Good."
"We've identified the cephalic vein. We'll typically ligate and divide it, or carefully retract it medially with the pectoralis major. For this case, let's retract it medially to preserve it if possible. Now, identify the interval between the deltoid muscle laterally and the pectoralis major muscle medially. This is a relatively avascular plane."
"Using electrocautery, we'll carefully separate the deltoid from the pectoralis major down to the clavipectoral fascia. Be mindful of the anterior deltoid fibers; we want to preserve their integrity as much as possible."
2. Exposure of the Rotator Interval and Subscapularis:
"Once we're through the clavipectoral fascia, we'll encounter the coracoid process and the conjoined tendon (short head of biceps and coracobrachialis) attaching to it. We need to expose the anterior shoulder capsule. Retract the deltoid laterally and the pectoralis major medially."
"Now, we can clearly see the rotator interval, located between the anterior edge of the supraspinatus tendon superiorly and the superior edge of the subscapularis tendon inferiorly. This interval contains the superior glenohumeral ligament and the long head of biceps tendon."
"Let's identify the long head of biceps tendon. Given the patient's age and arthritic changes, and to prevent future pain, we'll perform a tenotomy and tenodesis. Dr. Jones, please use the arthroscopic scissors to tenotomize the biceps from its origin at the supraglenoid tubercle. We'll tenodese it later to the pectoralis major or humeral shaft."
Surgical Warning: Be extremely careful with medial retraction of the conjoined tendon. Excessive force can put the musculocutaneous nerve at risk, which pierces the coracobrachialis muscle approximately 5-8 cm distal to the coracoid tip.
3. Subscapularis Release:
"The next critical step is to release the subscapularis tendon. We have a few options: a lesser tuberosity osteotomy, or a tendon peel-off. For this case, given the good quality of the tendon, we'll perform a subscapularis peel-off from its insertion on the lesser tuberosity. This allows us to repair it robustly at the end."
"Dr. Chen, please use a curved Mayo scissors or a scalpel to carefully release the subscapularis tendon from the lesser tuberosity. Start superiorly, just distal to the rotator interval, and work inferiorly. Keep your dissection right on the bone to avoid damaging the tendon itself. We're aiming for a full release, allowing us to externally rotate the humerus and dislocate the head."
"As we release the subscapularis, we'll encounter the middle glenohumeral ligament and the inferior glenohumeral ligament and inferior joint capsule as we proceed inferiorly. These will also need to be released from the humeral side to adequately mobilize the joint."
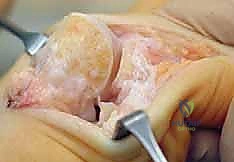
4. Humeral Head Dislocation and Resection:
"With the subscapularis released, we can now externally rotate and extend the arm, dislocating the native humeral head from the glenoid fossa. Dr. Smith, please apply gentle traction and external rotation. Excellent."
"Now that the humeral head is dislocated, we can assess its wear pattern and the underlying bone. We'll use our humeral head resection guide. This guide helps us determine the correct amount of bone to resect, aiming for a neutral retroversion of approximately 20-30 degrees relative to the epicondylar axis, and appropriate height."
"Dr. Jones, please position the humeral head resection guide. We'll use a sagittal saw to resect the humeral head. Ensure the saw blade is well-irrigated to prevent thermal necrosis. Take your time, this cut is crucial for implant seating and soft tissue balance."
"Once the head is resected, hand me the resected humeral head. We'll keep it on the back table for reference and potential bone graft harvesting if needed."
Surgical Warning: During humeral head dislocation and resection, be constantly aware of the axillary nerve, which wraps around the surgical neck. Excessive inferior traction or aggressive dissection can put it at risk.
5. Humeral Preparation:
"With the humeral head resected, we now need to prepare the humeral canal for the stem. We'll start with a small osteotome or burr to open the medullary canal. Then, we'll use progressively larger humeral reamers, following the curvature of the humerus, until we achieve cortical contact."
"Dr. Chen, please start with the smallest reamer. Ream slowly and steadily. We're aiming for a press-fit stem, so the reaming should be precise. We'll then use the appropriate broaches to create the final cavity for the humeral stem. Each broach will correspond to a specific stem size."
"After broaching, we'll insert a trial humeral stem and head. This allows us to assess range of motion, stability, and soft tissue tension before implanting the definitive components."
6. Glenoid Preparation:
"Now, let's turn our attention to the glenoid fossa. This is often the most challenging part of the procedure due to its complex anatomy and the proximity of vital neurovascular structures. Retract the humerus posteriorly and inferiorly to expose the glenoid fully."
"First, we'll remove any remaining glenoid labrum and osteophytes. Use a curette or burr to debride the articular cartilage down to bleeding subchondral bone. We need a clean, flat surface for the glenoid component."
"Now, assess the glenoid wear. If we have significant posterior glenoid erosion, as is common in osteoarthritis, we might need a posterior bone graft. Let's assume for this patient, we have moderate posterior wear requiring an allograft segment of bone in place to restore the glenoid anatomy. We'll shape the allograft to match the defect."
"Dr. Smith, please pass me the 0.045 K-wire. We'll use this as our central guide pin for glenoid reaming. The K-wire placement is critical. It must be perfectly centered on the glenoid, perpendicular to the face of the glenoid, and angled correctly for the desired version (usually neutral or slight retroversion)."
"We'll use fluoroscopy to confirm K-wire placement. Drill under constant fluoroscopic guidance to prevent perforation of the anterior or posterior glenoid cortex, which could endanger the suprascapular nerve and vessels posteriorly, or the brachial plexus anteriorly. The suprascapular nerve is particularly vulnerable as it courses around the scapular neck."
"Once the K-wire is in place, we'll use progressively larger glenoid reamers over the K-wire to prepare the glenoid surface. Ream just enough to achieve concentric seating of the glenoid component, preserving as much subchondral bone as possible."
"If we're using the allograft for posterior augmentation, we'll secure it now. We can use a small cancellous screw in place to fix the allograft to the native glenoid, ensuring it's flush and stable before final reaming and component insertion. The K-wire can help guide the screw placement to avoid neurovascular structures."
"After reaming, we'll drill the peg holes or keel slot for the glenoid component. Again, precise drilling is paramount, ideally under fluoroscopic guidance to confirm depth and trajectory."
7. Component Implantation:
"Now for the definitive implants. We'll start with the glenoid component. Mix the bone cement, Dr. Jones. We'll apply a thin mantle of cement to the back of the glenoid component and into the peg holes."
"Carefully insert the glenoid component, ensuring it's fully seated and perfectly flush with the reamed glenoid surface. Hold it firmly in place until the cement polymerizes. Remove any excess cement."
"Next, we'll implant the definitive humeral stem. We've chosen an uncemented stem for this patient. Impaction is key here. Dr. Chen, please use the humeral impactor. Impress the stem firmly into the canal until it's fully seated. Confirm its retroversion and height."
"Finally, we'll place the definitive humeral head component onto the stem taper. Ensure it's fully seated with a firm tap."
8. Reduction and Stability Assessment:
"Now, let's reduce the shoulder. Dr. Smith, gentle traction and internal rotation. Good. We're in. Now, let's assess stability throughout the full range of motion. We want a stable joint with good soft tissue tension, but not too tight. We'll check for impingement, subluxation, and dislocation."
"We'll perform a full arc of motion: flexion, extension, abduction, adduction, internal and external rotation. Everything feels good, stable, and smooth."
9. Rotator Cuff and Capsular Repair:
"Now, for the repair. Remember that subscapularis tendon we peeled off? We need to reattach it securely. We'll use strong, non-absorbable sutures to reattach the tendon to the lesser tuberosity. Dr. Jones, please pass me the heavy braided sutures."
"We'll use a robust repair technique, such as a mattress stitch or a simple interrupted stitch, ensuring good tissue apposition and tension. This is crucial for postoperative stability and function. We can also reinforce the anterior capsule if needed. For this patient, we'll use a "Yoke" stitch to ensure a broad, secure reattachment of the subscapularis, distributing the load across the repair."
"If we were dealing with an irreparable rotator cuff, our approach would have been different, possibly opting for a hemiarthroplasty with biologic glenoid resurfacing or a reverse total shoulder arthroplasty, depending on the patient's age and functional demands. But today, our cuff is repairable, and the repair looks solid."
10. Closure:
"With the subscapularis repaired, we'll release the arm from traction and allow it to rest in a neutral position. We'll irrigate the wound thoroughly with antibiotic solution."
"We'll close the deltopectoral interval loosely. Then, we'll close the subcutaneous layers and skin with absorbable sutures. A sterile dressing will be applied, and the arm will be placed in a sling with an abduction pillow to protect the subscapularis repair."
Pearls and Pitfalls
- Glenoid Perforation: A major pitfall. Excessive reaming or misdirected K-wires/screws can perforate the glenoid, leading to implant loosening, nerve injury (suprascapular nerve), or vessel injury. Always use fluoroscopy for K-wire and screw placement.
- Axillary Nerve Injury: Can occur during humeral head dislocation, inferior capsular release, or excessive inferior retraction. Maintain gentle traction, avoid aggressive inferior dissection.
- Musculocutaneous Nerve Injury: Risk with aggressive medial retraction of the conjoined tendon. Identify the nerve's expected course and use careful, gentle retraction.
- Subscapularis Failure: A common cause of postoperative pain and instability. Ensure a robust, tension-free repair. Consider a lesser tuberosity osteotomy in revision cases or when tendon quality is poor.
- Glenoid Loosening: Can be caused by poor bone quality, inadequate reaming, or malpositioning. Achieve good subchondral bone preparation and concentric seating.
- Infection: Standard surgical precautions. Thorough irrigation, prophylactic antibiotics.
- Humeral Fractures: Can occur during stem insertion, especially with uncemented stems in osteoporotic bone. Use appropriate reaming and broaching, avoid excessive force.
- Component Malposition: Incorrect retroversion or inclination can lead to instability, impingement, and early wear. Use guides, fluoroscopy, and trial components meticulously.
Surgical Warning: If an intraoperative fracture occurs during humeral broaching or stem insertion, stop immediately. Assess the fracture pattern. Small fissures may be managed with cerclage wires. Larger fractures may require revision to a longer stem or even conversion to a different implant system.
Postoperative Rehabilitation & Complication Management
Our job isn't done when the patient leaves the OR. Postoperative care is just as critical.
1. Immediate Postoperative Phase (0-6 weeks):
* Immobilization: The patient will be placed in a sling with an abduction pillow, especially after a subscapularis repair. This protects the repair site.
* Weight-bearing: Non-weight-bearing on the operative arm.
* Range of Motion (ROM):
* Passive ROM: Initiated early, typically within the first few days, focusing on pendulum exercises and gentle external rotation (limited to 30 degrees for subscapularis repair).
* Active ROM: Avoided for the first 4-6 weeks to protect the soft tissue repairs.
* Pain Management: Multimodal approach including NSAIDs, acetaminophen, and judicious use of opioids.
* DVT Prophylaxis: Continue sequential compression devices and consider chemical prophylaxis (e.g., aspirin or LMWH) based on patient risk factors.
2. Intermediate Phase (6-12 weeks):
* Gradual Progression: Active-assisted ROM progresses to active ROM.
* Strengthening: Gentle isometric exercises for the rotator cuff and deltoid begin, avoiding heavy lifting or sudden movements.
* Functional Activities: Gradually reintroduce light daily activities.
3. Advanced Phase (12+ weeks):
* Progressive Strengthening: Focus on strengthening all shoulder girdle muscles, improving endurance and coordination.
* Return to Activity: Gradual return to more demanding activities, typically avoiding overhead lifting or contact sports for at least 6 months to a year.
Complication Management:
- Wound Dehiscence/Infection:
- Superficial: Managed with local wound care, oral antibiotics.
- Deep: Requires surgical debridement, intravenous antibiotics, and potentially implant removal with a two-stage revision.
- Hardware Failure/Loosening:
- Glenoid: Symptoms include pain, crepitus. Diagnosis with radiographs and CT. Often requires revision surgery.
- Humeral: Less common, but can occur. Revision surgery may involve a longer stem or cement augmentation.
- Instability/Dislocation:
- Early: Often due to soft tissue imbalance or component malposition. May require closed reduction, bracing, or early revision.
- Late: Can be due to rotator cuff failure or progressive wear.
- Rotator Cuff Re-tear: If the subscapularis repair fails, it can lead to anterior instability and weakness. May require revision repair or consideration of a reverse TSA.
- Neuropraxia/Nerve Injury: Most are transient. Persistent symptoms require
You Might Also Like