The Swashbuckler Approach to the Distal Femur: A Comprehensive Surgical Guide
Key Takeaway
The Swashbuckler approach, popularized by Starr et al., is a highly utilitarian surgical technique for complex distal femur fractures. By utilizing a lateral parapatellar arthrotomy and elevating the vastus lateralis without violating the quadriceps tendon, it provides unparalleled exposure of the femoral condyles. This approach is particularly indicated for AO/OTA Type C intra-articular fractures requiring precise anatomical reduction and locking plate osteosynthesis.
Introduction to the Swashbuckler Approach
The management of complex, comminuted, and intra-articular fractures of the distal femur (AO/OTA Type 33-B and 33-C) presents a formidable challenge to the orthopedic surgeon. Achieving anatomical reduction of the articular block while preserving the delicate soft-tissue envelope of the metadiaphysis is the cornerstone of successful osteosynthesis.
Historically, standard lateral approaches provided inadequate visualization of the medial femoral condyle and the intercondylar notch, often necessitating highly morbid extensile exposures or dual incisions. To circumvent these limitations, Starr et al. popularized the Swashbuckler Approach. This modified anterior approach combines a lateral parapatellar arthrotomy with the elevation of the vastus lateralis muscle. By reflecting the entire extensor mechanism medially without splitting the quadriceps tendon, the surgeon gains unparalleled, panoramic visualization of the distal femoral articular surface.
This comprehensive guide details the indications, biomechanical principles, preoperative planning, and step-by-step surgical execution of the Swashbuckler approach, integrating modern concepts of locking plate fixation and minimally invasive plate osteosynthesis (MIPO).
Indications and Contraindications
Primary Indications
The Swashbuckler approach is highly versatile and is indicated for a variety of complex distal femoral pathologies:
* AO/OTA Type 33-C Fractures: Complete articular fractures with metaphyseal comminution. The approach allows for direct visualization and reduction of the articular block (condyles) before bridging the metaphyseal segment.
* AO/OTA Type 33-B Fractures: Partial articular fractures, particularly those involving coronal plane shear fractures (Hoffa fragments) of the lateral or medial condyles.
* Distal Femoral Malunions and Nonunions: Provides the necessary exposure for intra-articular osteotomies, callus takedown, and complex deformity correction.
* Periprosthetic Fractures: Supracondylar fractures above a total knee arthroplasty (TKA), where visualization of the implant-bone interface is critical.
Contraindications
- Severe Medial Soft Tissue Compromise: If the medial soft tissue envelope is severely traumatized, subluxating the patella medially may exacerbate tissue necrosis.
- Isolated Medial Condyle Fractures: A direct medial approach is more appropriate and less invasive for isolated medial pathology.
- Active Infection: Overlying cellulitis or active intra-articular sepsis precludes the use of this extensile approach for elective reconstruction.
Surgical Anatomy and Biomechanics
The Extensor Mechanism and Vastus Lateralis
The Swashbuckler approach exploits the internervous and intermuscular planes of the lateral thigh. The vastus lateralis is enveloped by the fascia lata and the lateral intermuscular septum. By dissecting the vastus lateralis off the lateral intermuscular septum and elevating it anteriorly, the entire anterior and lateral aspects of the distal femur are exposed.
Surgical Warning: The perforating branches of the profunda femoris artery pierce the lateral intermuscular septum to supply the vastus lateralis. These vessels must be meticulously identified, isolated, and ligated during the elevation of the muscle. Failure to do so can result in severe postoperative hematoma, acute blood loss, or compartment syndrome.
Biomechanics of Locking Condylar Plate Fixation
Following articular reduction, fixation is typically achieved using a Locking Condylar Plate (LCP). Locking plates act as fixed-angle constructs, which are biomechanically superior in osteoporotic bone and comminuted fractures.
* Articular Block: The distal locking screws provide a stable scaffold, preventing varus/valgus collapse of the condyles.
* Metaphyseal Bridging: By utilizing the plate as an extramedullary splint across the comminuted metaphysis, the surgeon preserves the fracture hematoma and periosteal blood supply, promoting secondary bone healing via callus formation.
Preoperative Planning and Patient Positioning
Imaging and Templating
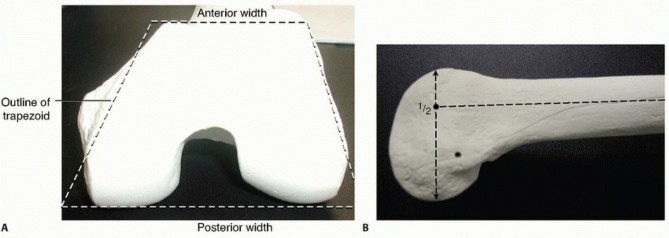
Standard orthogonal radiographs (AP and lateral) of the entire femur and knee are mandatory. A fine-cut Computed Tomography (CT) scan with 2D and 3D reconstructions is critical for identifying coronal shear fragments (Hoffa fractures), intercondylar comminution, and the exact trajectory of the fracture lines. Preoperative templating ensures the correct plate length and screw trajectory are selected.
Patient Positioning
- Table: Place the patient supine on a fully radiolucent operating table to allow unimpeded fluoroscopic imaging in both AP and lateral planes.
- Knee Positioning: Place a sterile bump, roll, or radiolucent triangle under the ipsilateral knee. Maintaining the knee in 30 to 60 degrees of flexion relaxes the deforming force of the gastrocnemius muscle, which typically pulls the distal articular fragment into extension (recurvatum deformity).
- Tourniquet: The use of a sterile tourniquet is highly debated.
Clinical Pearl: Use a tourniquet only if strictly necessary. Inflating a tourniquet on the proximal thigh can tether the quadriceps muscle, making medial retraction of the extensor mechanism and patella significantly more difficult, thereby limiting distal articular exposure.
Step-by-Step Surgical Technique
1. The Incision
- Make a longitudinal incision starting proximally over the lateral aspect of the distal femur, extending distally to the midline, and curving slightly to cross the patella and terminate at the tibial tubercle.
- The length of the proximal extension depends on the degree of metaphyseal comminution and the planned length of the plate.
2. Superficial Dissection and Fascial Incision
- Extend the incision directly down through the subcutaneous tissue to the fascia of the quadriceps and the iliotibial (IT) band.
- Incise the quadriceps fascia in line with the skin incision.
- Sharply dissect the quadriceps fascia off the vastus lateralis muscle laterally, continuing until you reach its inclusion with the IT band.
3. Deep Dissection and Muscle Elevation
- Retract the IT band and the lateral fascia laterally. Continue the deep dissection down to the linea aspera and the lateral intermuscular septum.
- Begin elevating the vastus lateralis muscle off the lateral intermuscular septum, working from distal to proximal.
- Ligation of Perforators: As the vastus lateralis is elevated, carefully identify the perforating vessels from the profunda femoris. Clamp, divide, and securely ligate or cauterize these vessels to expose the entire lateral and anterior distal femur.
4. The Arthrotomy
- Distally, incise the lateral parapatellar retinaculum, separating it from the vastus lateralis.
- Perform a standard lateral parapatellar arthrotomy to enter the knee joint.
- Place a blunt retractor (such as a Hohmann or Z-retractor) under the vastus lateralis and vastus medialis.
- Gently subluxate and displace the patella medially. This maneuver, combined with the proximal elevation of the vastus lateralis, "opens the book" of the distal femur, providing a spectacular, unobstructed view of both the lateral and medial femoral condyles, as well as the intercondylar notch.
5. Articular Reduction
- Irrigate the joint to remove hematoma and osteochondral debris.
- Anatomically reduce the articular fragments. Use pointed reduction forceps, dental picks, or K-wires as joysticks.
- Provisional fixation is achieved with multiple smooth K-wires.
- Definitive fixation of the articular block is typically performed using independent, countersunk 3.5mm or 4.5mm cortical lag screws, placed anterior-to-posterior (for Hoffa fragments) or lateral-to-medial. Ensure these screws do not interfere with the planned trajectory of the distal locking screws of the condylar plate.
Locking Condylar Plate Fixation and MIPO Techniques
Once the articular block is reconstituted, it is effectively converted into an extra-articular fracture (AO/OTA Type 33-A). The next phase is attaching the articular block to the femoral diaphysis.
Locking condylar plate fixation is the gold standard for buttressing multifragmentary distal femoral fractures, bridging highly comminuted zones, and treating malunions. Current implants offer the stability of fixed-angle devices while allowing for biologically appropriate, minimally invasive placement.
Minimally Invasive Plate Osteosynthesis (MIPO)
For extensive metaphyseal comminution, opening the entire fracture zone devitalizes the bone fragments and increases the risk of nonunion. Instead, a MIPO technique is utilized.

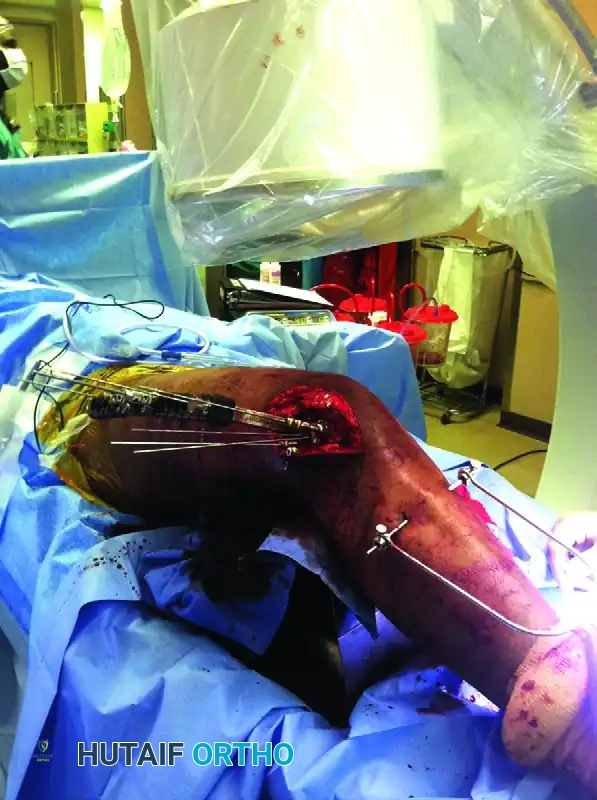
As demonstrated in the surgical setup above, MIPO allows for accurate fixation while minimizing further biological insult to the comminuted metaphyseal zones.
Key Elements of the MIPO Setup:
1. Proximal Tibial Traction: Note the proximal tibial traction pin and bow in the image. This is a critical adjunct. Applying skeletal traction through the proximal tibia allows the surgeon to restore axial length and correct rotational alignment indirectly, without stripping the fracture site.
2. Submuscular Plate Insertion: The locking plate is slid submuscularly (deep to the vastus lateralis) from the distal articular exposure proximally along the lateral shaft of the femur.
3. Targeting Outriggers: Specially designed radiolucent outriggers (jigs) are attached to the distal end of the plate. These outriggers permit precise, percutaneous targeting for proximal screw fixation.
4. Fluoroscopic Verification: Intraoperative fluoroscopy is used extensively to confirm the restoration of the mechanical axis, correct plate positioning, and ensure that proximal screws are centrally located within the femoral diaphysis.
Pitfall: When bridging a comminuted segment, ensure the plate is long enough. A general rule is to have a plate span ratio of 2:1 to 3:1 relative to the fracture length, with at least 3 to 4 widely spaced bicortical locking screws in the proximal diaphyseal segment to prevent stress risers and hardware failure.
Closure and Postoperative Protocol
Meticulous Closure
Proper closure is vital to ensure normal patellofemoral tracking and prevent postoperative extensor lag.
* Thoroughly irrigate the joint and the submuscular space.
* Place a closed-suction drain in the intra-articular space and/or the submuscular space if significant dead space or oozing is present.
* Retinacular Repair: Meticulously repair the lateral parapatellar arthrotomy and the lateral retinaculum using heavy, absorbable sutures (e.g., #1 or #2 Vicryl). Ensure the patella tracks centrally within the trochlear groove.
* Fascial Closure: Suture the quadriceps fascia and the iliotibial band back into their anatomical positions.
* Close the subcutaneous tissues and skin in a standard layered fashion.
Postoperative Rehabilitation
The rehabilitation protocol must balance the need for early joint mobilization to prevent stiffness with the necessity of protecting the fracture fixation.
* Phase 1 (0-6 Weeks): The knee is placed in a hinged knee brace. Continuous Passive Motion (CPM) or active-assisted range of motion (ROM) exercises are initiated immediately to prevent intra-articular adhesions. Weight-bearing is strictly restricted to toe-touch or non-weight-bearing (NWB) depending on the degree of comminution and bone quality.
* Phase 2 (6-12 Weeks): Progressive partial weight-bearing is initiated based on radiographic evidence of bridging callus. Active quadriceps strengthening is emphasized.
* Phase 3 (>12 Weeks): Transition to full weight-bearing as tolerated once clinical and radiographic union is achieved.
Potential Complications
- Knee Stiffness: The most common complication following distal femur fractures. Early, aggressive ROM is the best prevention.
- Nonunion/Hardware Failure: Often a result of inadequate plate length, insufficient proximal fixation, or excessive soft-tissue stripping.
- Patellar Maltracking: Can occur if the lateral retinaculum is closed too tightly or if the articular block is reduced in a malrotated position.
Conclusion
The Swashbuckler approach represents a masterclass in surgical anatomy, offering an elegant solution to the complex problem of distal femoral articular fractures. By combining the extensile, joint-sparing exposure of the Swashbuckler technique with the biological preservation of MIPO locking plate osteosynthesis, orthopedic surgeons can achieve rigid anatomical reduction, promote rapid biological healing, and maximize functional outcomes for their patients.
You Might Also Like