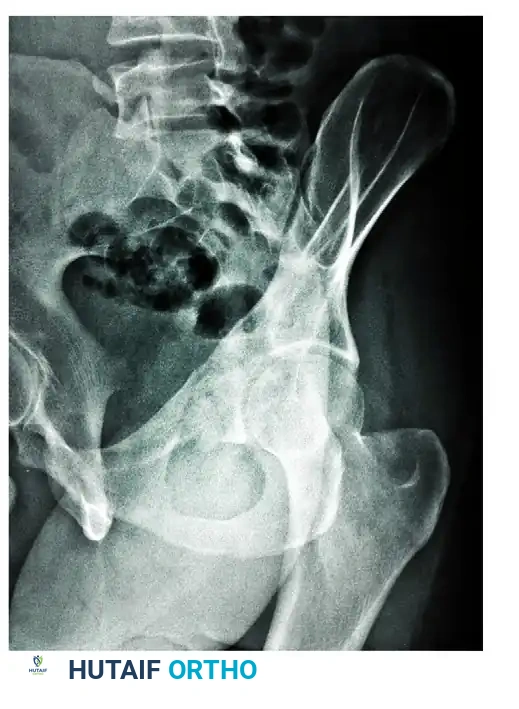
Operative Management of Pelvic and Acetabular Malunions and Nonunions
Key Takeaway
The operative management of pelvic and acetabular malunions is a formidable surgical challenge requiring meticulous preoperative planning and advanced reconstructive techniques. Late correction is technically demanding and associated with higher complication rates than acute fracture management. Indications for intervention include intractable pain, pelvic instability, sitting imbalance, and significant leg-length discrepancy. Successful outcomes depend on precise patient selection, comprehensive radiographic evaluation, and individualized, multi-stage surgical strategies to restore pelvic ring biomechanics.
Introduction to Pelvic and Acetabular Deformities
The late correction of pelvic and acetabular deformities represents one of the most formidable challenges in orthopedic trauma surgery. Even with the advent of modern, standardized protocols for the acute management of pelvic ring disruptions and acetabular fractures, malunions and nonunions continue to occur. These complications frequently result in profound functional disability, chronic pain, and significant alterations in biomechanics.
Late correction is inherently more difficult, less successful, and associated with a markedly higher incidence of complications compared to the management of acute pelvic fractures. Consequently, the initial anatomical reduction and rigid stabilization of acute pelvic injuries remain of paramount importance to prevent the sequelae of malunion and nonunion. When late reconstruction is justified, it must be undertaken exclusively by highly experienced pelvic surgeons operating within specialized tertiary referral centers.
Clinical Pearl: The primary goal of pelvic reconstruction is not necessarily perfect anatomical restoration—which is frequently impossible in the chronic setting—but rather the restoration of a stable, painless pelvic ring, equalization of limb length, and correction of sitting imbalance.
Pathoanatomy and Biomechanics
Acetabular Malunions
Malunions of the pelvis in which surgical correction is most frequently justified are those involving the acetabulum. The hallmark of acetabular malunion is the incongruity of the articular surface, which rapidly precipitates post-traumatic osteoarthritis.
* Central Dislocation: A common sequela of unreduced transverse or T-type fractures, leading to medial migration of the femoral head (protrusio acetabuli).
* Structural Deficiencies: Malunion often leaves the anterior or posterior columns structurally deficient, complicating future arthroplasty.
* Osteonecrosis: Avascular necrosis of the femoral head or the acetabular fracture fragments may occur, particularly following posterior fracture-dislocations.
Pelvic Ring Malunions and Nonunions
Pelvic ring nonunions do not universally cause pain; however, severe malunions—most commonly involving the posterior sacroiliac (SI) complex—are highly symptomatic.
* Cranial Displacement: Vertical shear injuries that heal in a displaced position result in cranial migration of the hemipelvis. A displacement of 1 cm or more typically leads to a clinically significant leg-length discrepancy (LLD), sitting imbalance (due to asymmetrical ischial tuberosity height), and a prominent, painful sacrum when the patient is supine.
* Rotational Deformities: Severe internal or external rotational malunions alter the vector forces across the hip joint and lumbar spine, leading to secondary mechanical back pain and gait efficiency loss.
* Visceral Impingement: Pelvic tilt fractures or displaced superior pubic rami can erode into the perineum or impinge upon the bladder, causing urinary frequency, dyspareunia, or vaginal wall impingement.
Clinical Evaluation and Patient Selection
Patient selection is the cornerstone of successful pelvic reconstruction. The surgeon must conduct a rigorous clinical evaluation to differentiate between pain originating from a pelvic nonunion/malunion, post-traumatic osteoarthritis of the hip, or concomitant lumbosacral spine pathology.
Indications for Surgical Intervention
Surgical treatment of pelvic malunions is indicated for:
1. Intractable posterior or anterior pelvic pain directly attributable to instability or malreduction.
2. Gross pelvic instability (clinically or radiographically demonstrated).
3. Sitting imbalance due to ischial height discrepancy.
4. Symptomatic limb shortening (cranial displacement > 1 cm).
5. Visceral compromise (e.g., vaginal wall or bladder impingement).
6. Severe cosmetic deformities secondary to limb shortening and malrotation.
Surgical Warning: Posterior pelvic pain of uncertain etiology, or pain primarily driven by chronic lumbosacral nerve root injury, is highly unlikely to improve with pelvic osteotomy and realignment. Concomitant lumbar injuries must be thoroughly evaluated and ruled out as the primary pain generator prior to pelvic surgery.
Patient Counseling and Expectations
Patients must possess realistic expectations and fully comprehend the magnitude of the proposed surgery. They must accept the known risks, which include:
* Loss of reduction or hardware failure.
* Iatrogenic nerve injury (particularly the L5 and S1 nerve roots).
* Vascular injury (corona mortis, superior gluteal artery, internal iliac branches).
* Persistent nonunion.
* Significant, potentially life-threatening blood loss.
* Strict compliance with 3 to 5 months of restricted weight-bearing postoperatively.
Radiographic Assessment
A comprehensive imaging protocol is mandatory to delineate the complex, multiplanar nature of pelvic deformities.
Standard Radiography
- Anteroposterior (AP) Pelvis: Evaluates overall symmetry, LLD, and cranial displacement. Limb shortening is quantified by comparing the cranial displacement of the acetabular roof on the affected side with the contralateral normal side, using a line perpendicular to the midline of the sacrum.
- Judet Views (45-degree internal/obturator and external/iliac oblique): Essential for assessing the integrity of the anterior and posterior acetabular columns.
- Inlet View (40-degree caudal): Assesses anterior-posterior translation and internal/external rotational deformities of the hemipelvis.
- Outlet View (40-degree cephalad): Evaluates vertical translation (cranial/caudal migration) and flexion/extension deformities of the hemipelvis.
- Single-Leg Standing AP (Flamingo Views): Right and left single-leg standing radiographs are highly useful for detecting dynamic instability across the pubic symphysis and SI joints.
Advanced Imaging
- Computed Tomography (CT): A fine-cut pelvic CT scan is non-negotiable. It provides critical information regarding the extent of fracture union, the presence of bridging callus, and the exact location of nonunions.
- Three-Dimensional (3D) CT Reconstruction: Invaluable for spatial orientation and preoperative templating. 3D models allow the surgeon to visualize the deformity in its entirety and plan the precise location and angle of corrective osteotomies.
Preoperative Planning for Acetabular Reconstruction
Before attempting acetabular reconstruction, the surgeon must systematically evaluate four critical elements:
1. Location and Condition of Segments: Assess the viability of the different segments of the acetabular articular surface and the structural integrity of the bony columns supporting them.
2. Femoral Head Wear: Determine the extent of chondral damage or mechanical wear on the femoral head.
3. Degree of Osteoarthritis: Evaluate joint space narrowing, subchondral sclerosis, and cyst formation.
4. Osteonecrosis: Identify any avascular necrosis of the femoral head or acetabular fragments.
Treatment Modalities for Acetabular Malunion
The treatment varies based on injury severity, deformity, disability, and patient age.
* Arthrodesis: When hip motion is severely limited and painful, and the patient is young or has an occupation requiring prolonged standing or heavy labor, hip arthrodesis remains a viable, durable treatment of choice.
* Total Hip Arthroplasty (THA): For older patients, or those with sedentary occupations, THA is indicated. However, THA in the setting of acetabular malunion is highly complex. It frequently requires structural bone grafting, trabecular metal augments, or custom triflange components to address column deficiencies and restore the anatomical hip center of rotation.
Surgical Techniques for Pelvic Ring Reconstruction
Operative correction of pelvic deformity requires individualized, bespoke surgical plans. The approach depends on whether the pathology is a nonunion without deformity, or a complex malunion requiring multiplanar correction.
Management of Nonunions Without Deformity
Pelvic nonunions lacking significant deformity can typically be managed with a one-stage or two-stage procedure. The risks and surgical approaches are akin to those of acute fracture surgery. In situ decortication, robust autologous bone grafting (e.g., from the iliac crest or reamer-irrigator-aspirator system), and rigid internal fixation are the mainstays of treatment.
The Three-Stage Procedure for Complex Malunions
For malunited or severely malaligned fractures, a three-stage procedure is highly recommended to mobilize the hemipelvis and provide the maximal amount of deformity correction.
Stage 1: Anterior Release (Patient Supine)
- Approach: A Pfannenstiel, ilioinguinal, or anterior intrapelvic (Stoppa) approach is utilized depending on the location of the anterior malunion.
- Procedure: The malunited superior and inferior pubic rami, or the pubic symphysis, are osteotomized. Callus is resected to fully mobilize the anterior ring. Care must be taken to protect the bladder, spermatic cord/round ligament, and the corona mortis.
- Temporary Closure: The anterior wound is temporarily closed, and the patient is repositioned.
Stage 2: Posterior Release, Reduction, and Fixation (Patient Prone)
- Approach: A posterior vertical or curvilinear incision is made over the posterior superior iliac spine (PSIS) and sacrum.
- Procedure: The malunited sacroiliac joint or sacral fracture is exposed. An osteotomy is performed through the malunion site. Extensive soft tissue release, including the sacrotuberous and sacrospinous ligaments, may be required to mobilize the hemipelvis.
- Reduction: Heavy skeletal traction (via a distal femoral pin) or specialized pelvic reduction clamps (e.g., Jungbluth clamps) are used to pull the hemipelvis distally and correct rotational deformities.
- Fixation: Once the posterior ring is anatomically aligned or maximally improved, rigid fixation is applied. This is typically achieved using iliosacral screws, transiliac-transsacral screws, or posterior tension band plating. Robust bone grafting of the posterior osteotomy site is mandatory.
Stage 3: Anterior Fixation (Patient Supine)
- Procedure: The patient is returned to the supine position. The anterior wound is reopened. With the posterior ring stabilized, the anterior ring is now rigidly fixed using symphyseal plates or retrograde medullary superior ramus screws.
Pitfall: Attempting to correct a severe, chronic cranial migration (>2-3 cm) acutely during a single surgical setting places extreme tension on the lumbosacral plexus. For severe shortening and internal rotation, a two-stage correction utilizing a period of heavy skeletal traction (2-3 weeks) after the initial osteotomy has been reported to minimize neurological complications prior to definitive fixation.
Alternative Procedures
- Leg-Length Equalization: Patients presenting with a leg-length discrepancy but lacking other pelvic symptoms (no pain, no sitting imbalance) should be spared the morbidity of a pelvic osteotomy. These patients are best treated with standard methods of limb-length equalization, such as contralateral epiphysiodesis (in skeletally immature patients), limb lengthening procedures, or simple shoe lifts.
- Sacroiliac Arthrodesis: For chronic, isolated sacroiliac pain caused by subtle instability or post-traumatic SI joint arthritis that is not relieved by conservative treatment (physical therapy, SI joint injections), an isolated SI joint arthrodesis is the treatment of choice.
Postoperative Protocol and Rehabilitation
The postoperative management of pelvic reconstruction patients is as critical as the surgery itself.
* Weight-Bearing: Patients must be strictly compliant with restricted weight-bearing (toe-touch or non-weight-bearing on the affected side) for a minimum of 3 to 5 months, depending on the quality of bone, rigidity of fixation, and radiographic evidence of union.
* Thromboprophylaxis: Given the extensive nature of the surgery and prolonged immobility, aggressive deep vein thrombosis (DVT) prophylaxis (e.g., low molecular weight heparin or direct oral anticoagulants) is mandatory unless contraindicated.
* Radiographic Monitoring: Serial radiographs are obtained at 6 weeks, 12 weeks, and 6 months to monitor for loss of reduction, hardware failure, and progression of bony union.
Outcomes and Complications
The surgical correction of pelvic malunions is a high-risk endeavor, but it can yield highly satisfactory results in properly selected patients.
In a landmark comprehensive study of 437 pelvic malunions, Kanakaris et al. reported the following outcomes:
* Union Rate: Averaged 86% following reconstructive surgery.
* Pain Relief: Achieved in 93% of patients, underscoring that correction of instability and malalignment effectively addresses the primary pain generators.
* Patient Satisfaction: Reached 79%.
* Functional Return: Despite high rates of union and pain relief, return to a preinjury level of activity was reported in only 50% of patients. This statistic must be explicitly discussed with the patient during preoperative counseling to ensure realistic expectations.
Complications remain frequent and include:
* Infection (particularly in posterior approaches due to proximity to the perineum).
* Neurological deficits (L5/S1 root stretch injuries during distal traction).
* Heterotopic ossification.
* Hardware prominence requiring subsequent removal.
Conclusion
The management of pelvic and acetabular malunions demands a profound understanding of pelvic biomechanics, advanced imaging interpretation, and masterful surgical technique. While the complication rates are higher than in acute trauma settings, meticulous multi-stage reconstructive procedures can successfully restore pelvic stability, correct severe deformities, and provide substantial pain relief for this highly debilitated patient population.
You Might Also Like