Full Question & Answer Text (for Search Engines)
Question 1:
All of the following have been used as viral vectors for gene delivery except:
Options:
- Adeno-associated virus
- Rotavirus
- Herpes simplex virus
- Lentivirus
- Retroviral vector
Correct Answer: Rotavirus
Explanation:
A retroviral vector derived from the Moloney murine leukemia retrovirus is among the best-developed viral vectors. Other viral vectors include adenovirus, adeno-associated virus, and herpes simplex virus. Novel vector systems based on lentivirus, a type of retrovirus, which includes human immunodeficiency virus (HIV), are being developed.
Question 2:
The principle of homologous recombination in gene therapy is used to:
Options:
- Replace a defective gene by a wild-type gene
- Suppress the expression of a mutant gene
- Supplement a wild-type gene
- Alter the expression of a mutant gene
- Replacement of a defective gene by a normal gene
Correct Answer: Replacement of a defective gene by a normal gene
Explanation:
Novel approaches to treating genetic diseases involve gene repair or replacement rather than gene supplementation. One such approach is based on homologous recombination (replacement of a defective gene by a normal gene).
Question 3:
The virus associated with most immune reactions is:
Options:
- Adeno-associated virus
- Guttedâ adenovirus
- Adenovirus
- Retrovirus
- Herpes simplex virus
Correct Answer: Guttedâ adenovirus
Explanation:
Adenoviral vectors can cause inflammatory reaction due to immune activation, an event linked to the first death related to gene therapy. This occurred in September 1999 at the University of Pennsylvania in a clinical trial in which an 18-year-old patient received infusion of over a trillion adenoviral vectors directed to his liver, which triggered a systemic inflammatory response that became uncontrollable, leading to organ failure and death. Newer generation gutted or gutlessâ adenovirus vectors are nonimmunogenic.
Question 4:
Compared to ex vivo gene delivery system, the in vivo system is:
Options:
- Technically complex
- Target specific
- Safer
- Less invasive
- More invasive
Correct Answer: Less invasive
Explanation:
Two basic strategies exist for gene delivery. Direct, or in vivo, gene therapy involves direct introduction of vectors into the body. Indirect, or ex vivo, gene therapy involves removal of target cells from the body, vector introduction by incubation of the cells in vitro, and reimplantation. The in vivo system is less invasive.
Question 5:
The gene that has been studied in greatest detail for application in osteoarthritis is:
Options:
- p-53
- Interleukin (IL)-13
- Tissue inhibitors of metalloproteinases-4
- IL-Receptor antagonist
- BMP-2
Correct Answer: IL-Receptor antagonist
Explanation:
Gene therapy has been suggested as a means of delivering sustained therapeutic levels of anti-arthritic gene products to diseased joints. Local gene delivery to the synovial tissue is preferred for osteoarthritis and other conditions affecting a few joints. It is less suited to address the extra- articular components of systemic conditions, such as rheumatoid arthritis. The gene that has been studied in greatest detail encodes the human IL-1 receptor antagonist (IL-Ra).
Question 6:
The osteoinductive potential of LIM mineralization protein (LMP)-1 gene has been studied for clinical application in:
Options:
- Fracture repair
- Spinal fusion
- C artilage regeneration
- Ligament healing
- Meniscal injury
Correct Answer: Spinal fusion
Explanation:
Identification of LIM mineralization protein-1 (LMP-1), a novel intracellular protein, is a step forward in osteoinductive proteins. Unlike BMP, which is a secreted protein that binds to cell-surface receptor to initiate a response, LMP-1 is an intracellular signaling molecule. Boden transfected bone marrow cells from rats ex vivo with LMP-1 gene using a DNA plasmid vector and used them during posterior thoracic and lumbar spine fusion in rats.
Question 7:
The gene studied for application in osteoporosis and wear-induced osteolysis is:
Options:
- Osteoprotegerin (OPG)
- Bone morphogenetic protein (BMP)
- Transforming growth factor-b1
- LMP-1
- IL-receptor antagonist
Correct Answer: Osteoprotegerin (OPG)
Explanation:
Various cytokines and cytokine antagonists hold promise as new therapeutic agents for osteoporosis. Baltzer et al showed that intramedullary injection of Ad-IL-1Ra gene in a murine ovariectomy model strongly reduced the loss of bone mass. Using a similar model, Bolon et al studied the effect of adenovirus-mediated transfer of osteoprotegerin, which showed more bone volume with reduced osteoclast numbers in axial and appendicular bones after 4 weeks compared to sham-operated mice.
Question 8:
Gene transfer to a cell using viral vectors is called:
Options:
- Transduction
- Transfection
- Transformation
- C onjugation
- Augmentation
Correct Answer: Transduction
Explanation:
In vivo gene delivery involves the direct injection of vectors containing the genes into the body with the expectation that they will reach and transduce the target cell.
Question 9:
Which of the following genes has been shown to stimulate proteoglycan synthesis for prevention of disk degeneration:
Options:
- LMP-1
- BMP-7
- Decorin
- TGF-b1
- OPG
Correct Answer: TGF-b1
Explanation:
Intervertebral disk degeneration has been associated with a progressive decrease in proteoglycan content of nucleus pulposus. The potential application of gene therapy for prevention of disk degeneration is to increase or maintain the proteoglycan content of nucleus pulposus. Thompson et al reported that addition of TGF-b1 to canine disk tissue in culture stimulated in vitro proteoglycan synthesis.
Question 10:
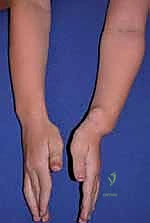
This patient has numerous (> 6) café au lait spots (Slide). The most likely diagnosis is:
Options:
- Fibrous dysplasia
- Osteofibrous dysplasia
- Neurofibromatosis 1
- Mazabraudâ s syndrome
- Osteogenesis imperfecta
Correct Answer: Neurofibromatosis 1
Explanation:
Neurofibromatosis is an autosomal dominant condition that occurs in a peripheral and central form. The peripheral type is more common and called neurofibromatosis 1 (NF1). The central type is characterized by bilateral acoustic neurofibromatosis (NF2). The clinical presentation is variable. Patients may either have a severe form of NF1 with hundreds of neurofibromas in the skin or they may have only cafa-au lait spots and deep neurofibromas that are easily apparent. Demographics of NF1 include: 1. Autosomal dominant with high degree of penetrance 2. C hromosomal abnormality - 17, NF1 gene (encodes neurofibromin) 3. Diagnostic criteria - two or more of the following:
Six or more cafu au lait spots Two or more neurofibromas of any type or one plexiform neurofibroma Freckling in the axillary or inguinal area Optic glioma Two or more Lisch nodules Bone lesion First-degree relative with NF1
Question 11:
This patient has numerous (> 6) cafa au lait spots (Slide). Which of the following describes the correct inheritance pattern:
Options:
- Autosomal recessive
- Autosomal dominant with low degree of penetrance
- Autosomal dominant with high degree of penetrance
- X-linked recessive
- X-linked dominant
Correct Answer: Autosomal dominant with low degree of penetrance
Explanation:
Neurofibromatosis is an autosomal dominant condition that occurs in a peripheral and central form. The peripheral type is more common and called neurofibromatosis 1 (NF1). The central type is characterized by bilateral acoustic neurofibromatosis (NF2). The clinical presentation is variable. Patients may either have a severe form of NF1 with hundreds of neurofibromas in the skin or they may have only cafa au lait spots and deep neurofibromas that are easily apparent. Demographics of NF1 include: 1. Autosomal dominant with high degree of penetrance 2. C hromosomal abnormality - 17, NF1 gene (encodes neurofibromin) 3. Diagnostic criteria - two or more of the following: Six or more cafa au lait spots Two or more neurofibromas of any type or one plexiform neurofibroma Freckling in the axillary or inguinal area Optic glioma Two or more Lisch nodules Bone lesion First-degree relative with NF1
Question 12:
The bone graft used in the Grice procedure for the treatment of neurogenic valgus feet should be placed:
Options:
- Between the cuboid and calcaneus
- Among the metatarsal bones
- In the sinus tarsi parallel to the axis of the tibia
- In the calcaneus after the osteotomy
- None of the above
Correct Answer: In the sinus tarsi parallel to the axis of the tibia
Explanation:
In 1945, Grice developed the use of subtalar extra-articular arthrodesis as a treatment for paralytic valgus feet. Grice demonstrated that blocking the tarsal sinus opening prevents the calcaneus from rotating posterolaterally and thus blocks the heel of a foot from shifting into the valgus position. A bone block must be placed at such an angle in the tarsal sinus that when posterolateral migration of the calcaneus is attempted, the graft compresses. If a graft is placed too far forward, then the posterolateral movement of the calcaneus increases insertional distance between blocked areas, the graft collapses, and the foot goes into valgus.
Question 13:
A patient with myelomeningocele has good quadriceps function, fair hamstring motion, and no active ankle movement. He has bilateral clubfoot. His motor level is:
Options:
Correct Answer: L4
Explanation:
The hamstrings are innervated at a level just proximal to the anterior tibialis muscle (with the highest innervated ankle motor at L5). Therefore, the patientâ s motor level is best estimated at L4.
Question 14:
In a type 1 Monteggiaâ s fracture, the position of reduction is:
Options:
- Flexion of the elbow and supination of the forearm
- Flexion of the elbow and pronation of the forearm
- Extension of the elbow and pronation of the forearm
- Extension of the elbow and supination of the forearm
- Extension of the elbow and midposition of the forearm
Correct Answer: Flexion of the elbow and supination of the forearm
Explanation:
Type 1 Monteggis fracture is associated with an anterior dislocation of the radial head and an apex anterior fracture of the ulna. Type 1 Monteggi s fracture is best treated by flexion and supination. The same maneuvers that reduce the ulna will also stabilize the radial head.
Question 15:
What is the approximate risk of growth disturbance of distal radial Salter II fractures:
Options:
Correct Answer: 15%
Explanation:
Although distal radial physeal fractures are common, growth disturbance is rare with a 1% occurence. Growth disturbance poses a challenge for follow- up, but physicians should at least mention the risk to patients.
Question 16:
Which of the following fracture situations would be most appropriate for internal fixation vs. attempted closed reduction:
Options:
- A 7-year-old girl with 35° angulation of greenstick radius and ulna fracture
- A 7-year-old boy with 35° angulation of complete radius and ulna fracture
- A 9-year-old girl with 30° angulation of complete radius and ulna fracture
- A 12-year-old boy with 25° angulation of complete radius and ulna fracture
- A 15-year-old girl with 25° angulation of complete radius and ulna fracture
Correct Answer: A 15-year-old girl with 25° angulation of complete radius and ulna fracture
Explanation:
Remodeling potential is significantly decreased at skeletal maturity. The first four scenarios represent skeletally immature patients. The 15-year-old girl should be treated like an adult to achieve the most acceptable result. All other patients deserve an attempt at closed reduction.
Question 17:
All of the following may be signs and symptoms of a tethered cord except:
Options:
- Back pain
- Leg pain
- Meryonâ s sign
- Increasing contracture
- Increasing motor weakness
Correct Answer: Meryonâ s sign
Explanation:
A tethered cord is common in patients with myelomeningocele. A tethered cord occurs due to adhesion of the dysplastic distal cord to its surrounding structures. The onset of a tethered cord may be exacerbated by closure of the open cord. Signs and symptoms of a tethered cord may include back pain, leg pain, increasing motor weakness, and increasing contracture. Alternate explanations for some of these signs and symptoms exist as well. An adult with Meryon's sign may drop a child he or she is holding due to weakness of the pectorals and latissimus muscles. Meryon's sign is also common in patients with myelomeningocele who have a C hiari's malformation. In this case, the patient with myelomeningocele does not experience weakness of the pectorals and latissimus muscles due to a tethered cord. Meryon's sign also occurs in some myopathies.
Question 18:
A 15-year-old patient with osteogenesis imperfecta (OI) is examined due to increasing knee flexion contractures and generalized muscle tightness of the lower extremities. The most likely explanation for these symptoms is:
Options:
- Spondylolysis
- Scoliosis
- Osteoarthritis associated with OI
- Basilar invagination
- Disuse
Correct Answer: Basilar invagination
Explanation:
Patients with OI have a significant risk of basilar invagination. In patients with OI the skull settles around the foramen magnum and cervical spine, causing the brainstem to become indented. Signs and symptoms include increased spasticity (described here as muscle tightness), contractures, hyperreflexia, clonus, respiratory depression, and changes in voice or swallowing. Basilar invagination is most common in type IV OI. Although osteoarthritis is more common in patients with OI than in the general population at a given age, the 15-year-old patient in this case is too young to develop osteoarthritis. Spondylolysis would not produce this constellation of symptoms unless associated with severe listhesis.
Question 19:
A 6-year-old boy with osteogenesis imperfecta has had three fractures of his proximal femur resulting in progressive bowing, which has now reached 70°. He has pain in his thigh and a sclerotic stress line at the apex of the bow. The best treatment is:
Options:
- C losed osteoclasis and spica cast
- Osteoclasis and external fixator
- Osteotomy and plate fixation
- Osteotomy and internal fixation with an expandable rod
- Observation
Correct Answer: Osteotomy and plate fixation
Explanation:
As bowing becomes greater, the likelihood of a re-fracture increases. The presence of a lucent sclerotic line and pain increases the risk of re-fracture. Intramedullary fixation is preferred to plate fixation because plate fixation increases the risk of stress risers. Expandable rods that bridge the entire bone from one epiphysis to the other are the best treatment for excessive bowing. Examples include the Bailey Dubow or the Fassier rods.
Question 20:
A 10-year-old boy steps on a nail. The nail is promptly removed and inspected in the emergency department. No evidence of foreign material is found in the patientâ s foot. One week later, the boy develops increased pain and swelling in his foot with inability to bear weight. Plain films show no abnormality. The appropriate next step of treatment would be:
Options:
- Irrigation and debridement of the foot
- Magnetic resonance imaging (MRI) of the foot
- Bone scan
- C omputed tomography scan
- Repair of flexor tendon laceration
Correct Answer: Magnetic resonance imaging (MRI) of the foot
Explanation:
Penetrating injuries to the sole of the foot commonly inoculate bacteria to the deep spaces of the foot. Pseudomonas, other gramnegative organisms, and Staphylococcus are examples of bacteria that commonly can become inoculated. An MRI would help to localize the site and stage of the infection. The MRI determines whether the surgeon should aspirate the infection and treat it with antibiotics or operatively debride the infection. Pseudomonas often requires debridement.

 Six or more cafu au lait spots Two or more neurofibromas of any type or one plexiform neurofibroma Freckling in the axillary or inguinal area Optic glioma Two or more Lisch nodules Bone lesion First-degree relative with NF1
Six or more cafu au lait spots Two or more neurofibromas of any type or one plexiform neurofibroma Freckling in the axillary or inguinal area Optic glioma Two or more Lisch nodules Bone lesion First-degree relative with NF1