Mastering Infection and Microbiology: A Guide to Diagnosis & Treatment
Key Takeaway
Learn more about Mastering Infection and Microbiology: A Guide to Diagnosis & Treatment and how to manage it. Infection and microbiology study how bacteria, like *Staphylococcus aureus MRSA*, cause diseases. Infections arise when pathogens colonize favorable environments in susceptible hosts, leading to conditions like cellulitis and erysipelas. Key clinical findings include erythema, pain, and fever, often requiring broad-spectrum antibiotics and sometimes surgical management. Prevention is also crucial.
Mastering Infection and Microbiology A Guide to Diagnosis & Treatment
Introduction and Epidemiology
Musculoskeletal infections represent a formidable challenge in orthopedic surgery, carrying significant morbidity, mortality, and socioeconomic burden. These infections can manifest in various forms, including osteomyelitis, septic arthritis, prosthetic joint infection (PJI), and soft tissue infections. The incidence of certain infections, such as PJIs, continues to rise with the increasing volume of arthroplasty procedures. A deep understanding of the underlying microbiology, host-pathogen interactions, and principles of surgical and antimicrobial management is paramount for orthopedic surgeons.
The initial management strategy for musculoskeletal infections often hinges on distinguishing between empirical and definitive treatment. Empirical treatment is initiated based on clinical findings, patient history, and presumed common pathogens, often before culture results are available. Staphylococcus species (e.g., S. aureus, coagulase-negative staphylococci) and Streptococcus species remain the predominant organisms encountered in skin, soft tissue, and bone infections. Conversely, definitive treatment is guided by final culture and sensitivity results, allowing for targeted antimicrobial therapy. Surgical intervention is frequently a cornerstone of treatment, involving thorough debridement of necrotic or infected tissue, drainage of contained infections, and restoration of vascularity where compromised.
Understanding bacterial virulence factors is crucial for effective diagnosis and treatment. These factors contribute to a pathogen's ability to establish infection, evade host defenses, and resist antimicrobial agents. Key virulence mechanisms include antibiotic resistance, increased surface adhesion, biofilm formation, and toxin production, all of which significantly impact the clinical course and complexity of orthopedic infections.
Anatomical and Biomechanical Considerations in Orthopedic Infection
The unique anatomical and biomechanical environment of the musculoskeletal system profoundly influences the pathogenesis, diagnosis, and management of infections. Unlike highly vascularized soft tissues, bone possesses a complex vascular supply, which can be easily disrupted by trauma, surgery, or inflammation, creating avascular segments that are difficult for antibiotics and host immune cells to penetrate. The presence of foreign bodies, such as orthopedic implants, further alters the local environment, providing inert surfaces for bacterial adhesion and biofilm formation.
In long bones, the metaphyseal region, rich in sinusoidal capillaries, is a common site for hematogenous osteomyelitis in children. In adults, osteomyelitis often results from direct inoculation during trauma or surgery, or from contiguous spread from an adjacent soft tissue infection. The anatomy of joints, with their synovial lining, presents a closed space that can rapidly be destroyed by enzymatic degradation in septic arthritis, necessitating urgent decompression and debridement. Articular cartilage is highly susceptible to irreversible damage from bacterial enzymes and inflammatory mediators.
The biomechanics of bone healing and implant stability are intrinsically linked to infection. Infection can disrupt the delicate balance of bone remodeling, leading to osteolysis, non-union, and pathological fractures. In the presence of implants, bacteria can colonize the implant surface, forming a robust biofilm that renders systemic antibiotics largely ineffective and compromises the mechanical integrity of the bone-implant interface. The creation of dead space following debridement is another critical biomechanical consideration, as it can serve as a nidus for recurrent infection if not adequately managed with local antibiotics, muscle flaps, or bone grafts.
The vascularity of the soft tissue envelope surrounding bone and implants is critical for both host defense and antibiotic delivery. Compromised vascularity, often seen in open fractures, radiation injury, or chronic wounds, significantly increases infection risk and impedes healing. Furthermore, the biomechanical forces acting on bone and implants necessitate stable fixation to promote healing, but in the presence of infection, this stability can be compromised, leading to loosening or failure. Surgical approaches must consider internervous planes to minimize iatrogenic damage, but in the context of infection, extensive debridement may necessitate broader exposure and potential sacrifice of anatomical structures to achieve source control.
Indications and Contraindications
The decision to proceed with surgical intervention for musculoskeletal infections is complex, balancing the risks of surgery against the potential for disease progression, functional impairment, and systemic complications. Surgical indications are generally centered on source control, debridement of infected and necrotic tissue, and reconstruction where necessary. Contraindications are typically relative, often related to the patient's overall medical status, but can also include situations where non-operative management is clearly superior or surgical risk outweighs potential benefit.
Operative Indications for Musculoskeletal Infections
Surgical intervention is indicated in most orthopedic infections where there is a collection of pus, devitalized tissue, or an infected foreign body.
- Septic Arthritis: Urgent irrigation and debridement (I&D) to remove purulent material and preserve articular cartilage.
- Acute Osteomyelitis: Debridement of necrotic bone and drainage of abscesses, especially when medical management fails or signs of progression exist.
- Chronic Osteomyelitis: Definitive surgical debridement of sequestra, involucrum, and necrotic soft tissue, often requiring multiple stages and dead space management.
- Prosthetic Joint Infection (PJI):
- Acute PJI (within 3-4 weeks of implantation or acute hematogenous spread): Debridement, antibiotics, and implant retention (DAIR) in selected cases.
- Chronic PJI: One-stage or two-stage exchange arthroplasty, or resection arthroplasty/arthrodesis for severe cases or compromised hosts.
- Necrotizing Soft Tissue Infections: Aggressive and often serial surgical debridement of all non-viable tissue is life-saving.
- Deep Soft Tissue Abscesses: Incision and drainage.
- Open Fractures with Contamination: Initial debridement and irrigation, with potential for repeat debridements.
- Infected Hardware: Removal of infected implants, especially in the presence of active infection that cannot be controlled with antibiotics alone.
Non Operative Indications for Musculoskeletal Infections
Non-operative management, primarily with antibiotics, is appropriate in select cases.
- Early, Uncomplicated Hematogenous Osteomyelitis: Particularly in children, without evidence of abscess formation or widespread bone necrosis.
- Cellulitis without Abscess: Superficial skin and soft tissue infections without deep involvement or purulent collections.
- Viral or Fungal Infections (selected cases): While some fungal infections may require debridement, initial management is often antifungal therapy.
- Patients Unfit for Surgery: Those with severe comorbidities where the risks of anesthesia and surgery significantly outweigh the potential benefits, provided infection control is achievable with antibiotics.
- Minor, Localized Infections: Superficial wound infections responsive to local care and oral antibiotics.
| Operative Indications | Non-Operative Indications |
|---|---|
| Septic Arthritis | Early, uncomplicated hematogenous osteomyelitis (pediatric) |
| Acute Osteomyelitis with abscess/sequestrum | Cellulitis without abscess formation |
| Chronic Osteomyelitis (sequestrum, involucrum) | Superficial wound infections |
| Acute PJI (DAIR for selected cases) | Selected fungal infections responsive to antifungals |
| Chronic PJI (One/Two-stage exchange, resection arthroplasty) | Patients with severe medical comorbidities precluding surgery (relative) |
| Necrotizing Soft Tissue Infections | Minor, localized infections responsive to antibiotics |
| Deep soft tissue abscesses | |
| Open fractures with significant contamination | |
| Infected hardware not amenable to retention |
Pre Operative Planning and Patient Positioning
Thorough pre-operative planning is critical for optimizing outcomes in musculoskeletal infection cases. This includes comprehensive diagnostic workup, patient optimization, and meticulous surgical strategy.
Diagnostic Workup
- Clinical Assessment: Detailed history, physical examination focusing on signs of inflammation, pain, systemic toxicity, and localizing findings.
- Laboratory Studies: Complete blood count (CBC), erythrocyte sedimentation rate (ESR), C-reactive protein (CRP) are baseline markers. Procalcitonin may assist in differentiating bacterial from non-bacterial inflammation.
- Microbiological Studies:
- Blood Cultures: Essential for detecting bacteremia, especially in hematogenous infections.
- Aspirates/Biopsies: Direct aspiration of fluid (e.g., joint fluid, abscess) or bone biopsy for Gram stain, culture, and sensitivity. This is paramount for definitive diagnosis and guiding targeted antibiotic therapy. The original seed content emphasizes the transition from empirical to definitive treatment based on these results.
- Tissue Specimens: Multiple tissue samples from distinct locations within the infected site improve diagnostic yield, especially for PJI.
- Imaging:
- Radiographs: Initial assessment for bone changes (e.g., periosteal reaction, osteolysis, sequestrum).
- Magnetic Resonance Imaging (MRI): Highly sensitive for soft tissue edema, abscesses, marrow changes in osteomyelitis, and differentiating infection from other pathologies.
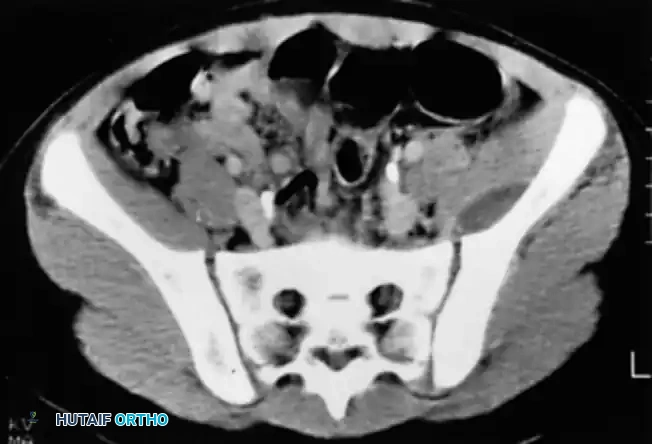
- Computed Tomography (CT): Excellent for delineating bone destruction, sequestra, involucrum, and planning complex debridements.
- Nuclear Medicine Scans (e.g., Technetium-99m bone scan, Gallium-67 scan, Indium-111 labeled leukocyte scan, FDG PET/CT): Useful for localizing infection, especially in complex cases or when hardware is present, although specificity can be an issue.
Patient Optimization
- Medical Clearance: Assess and optimize comorbidities (e.g., diabetes control, nutritional status, cardiac/pulmonary function).
- Antibiotic Stewardship: Initiate empirical antibiotics based on suspected pathogens, local epidemiology, and patient risk factors (e.g., MRSA risk). The seed content highlights Staphylococcus and Streptococcus as common organisms, and the importance of considering antibiotic resistance (e.g., bla gene, mecA gene for MRSA). This initial therapy can be adjusted to definitive treatment upon culture results.
- Anemia Correction: Address anemia if present to optimize oxygen delivery and healing.
- Nutritional Support: Malnutrition compromises immune function and healing; consider pre-operative nutritional supplementation.
Patient Positioning
Patient positioning must allow for complete access to the infected area and potential donor sites for flaps or grafts, while maintaining patient safety and comfort. General principles include:
- Sterile Field: Broad preparation and draping to allow for extension of incisions or secondary procedures.
- Tourniquet: Often utilized in extremity surgery to optimize visualization and reduce blood loss during debridement, though caution is advised in cases of poor vascularity.
- C-arm Access: Ensure fluoroscopic access for precise localization and evaluation during debridement and reconstruction.
Detailed Surgical Approach and Technique
The surgical management of musculoskeletal infections is centered on the principles of source control, debridement, dead space management, and optimization of the local environment for healing. While specific approaches vary by anatomical location and infection type, the underlying tenets remain consistent.
General Principles of Surgical Debridement
- Excision of All Non-Viable Tissue: This is the most critical step. Bone, soft tissue, and foreign material that are necrotic, inflamed, or contain biofilm must be meticulously removed until healthy, bleeding tissue is encountered. This directly addresses the "débridement of dead tissue" principle from the seed content.
- Biofilm Disruption: The glycocalyx-biofilm-slime-polysaccharide capsule, as described in the seed content, provides a protective barrier for bacteria, rendering them highly resistant to antibiotics and host defenses. Surgical debridement aims to physically remove this biofilm from implant surfaces and surrounding tissues. This often requires aggressive scraping, brushing, or removal of the colonized implant.
- Drainage of Contained Infections: Abscesses and purulent collections must be thoroughly drained. This may involve opening fascial compartments, joint capsules, or intramedullary canals.
- Restoration of Vascularity: Where possible, attempts should be made to improve blood supply to the infected area. This may involve revascularization procedures or the use of well-vascularized soft tissue flaps to bring healthy tissue with immune cells and antibiotics into the wound.
- Specimen Collection: Multiple tissue samples from different sites (e.g., implant-bone interface, deepest infection, soft tissue margins) should be sent for Gram stain, aerobic/anaerobic cultures, and sensitivity testing. This informs definitive antibiotic therapy.
Specific Surgical Techniques by Infection Type
Septic Arthritis
- Arthroscopic Irrigation and Debridement: Preferred for most peripheral joints (knee, shoulder, ankle, wrist) due to minimally invasive nature, excellent visualization, and thorough lavage. Synovial debridement and removal of fibrin clots are performed.
- Open Arthrotomy: Reserved for hip septic arthritis (difficult to visualize arthroscopically), recalcitrant cases, or joints with extensive destruction requiring more aggressive debridement.
Osteomyelitis
- Acute Hematogenous Osteomyelitis: Often initially managed with antibiotics. Surgical intervention (cortical fenestration, drainage) is indicated if a subperiosteal abscess develops, medical management fails, or signs of impending soft tissue rupture are present.
- Chronic Osteomyelitis: Requires radical surgical debridement of all infected and necrotic bone (sequestrum) and surrounding granulation tissue (involucrum) until healthy, bleeding bone is exposed. This often creates a significant dead space that needs management.
- Saucerization: Wide unroofing of the infected bone to convert a cavity into a shallow saucer, allowing for easier healing and obliteration of dead space.
- Bone Defect Management: Following debridement, defects may be managed with antibiotic-impregnated beads (PMMA), bone graft (autograft/allograft), or vascularized bone flaps, depending on size and location.
Prosthetic Joint Infection (PJI)
- Debridement, Antibiotics, and Implant Retention (DAIR): Appropriate for acute PJIs (<3-4 weeks post-op or acute hematogenous) without well-fixed components or extensive necrosis. Involves extensive synovectomy, irrigation with pulsed lavage, removal of all modular components, and exchange of polyethylene liners. The implant is retained.
- One-Stage Exchange Arthroplasty: Removal of all components, thorough debridement, and immediate reimplantation of new components, usually with antibiotic-loaded cement. Indicated for well-controlled infections with known, susceptible organisms and good soft tissue coverage.
- Two-Stage Exchange Arthroplasty: The gold standard for chronic PJI.
- Stage 1 (Resection Arthroplasty): Removal of all components, extensive debridement of infected bone and soft tissues. Placement of an antibiotic-impregnated cement spacer. This allows for local delivery of high-dose antibiotics and treatment of the infection in the interim.
- Stage 2 (Reimplantation): After a period of systemic antibiotics and normalization of inflammatory markers, the spacer is removed, and a new prosthesis is implanted.
- Resection Arthroplasty/Arthrodesis/Amputation: Salvage options for recurrent, intractable, or highly virulent PJIs, especially in immunocompromised patients or those with severe bone loss.
Dead Space Management and Wound Closure
- Antibiotic Delivery: Local delivery systems (e.g., antibiotic-impregnated PMMA beads or cement) are critical adjuncts, providing high concentrations of antibiotics at the infection site, especially beneficial against biofilm-producing organisms.
- Soft Tissue Coverage: Adequate soft tissue coverage is essential. This may require local muscle flaps, rotational flaps, or free tissue transfer, especially after extensive debridement or in areas of poor vascularity.
- Drains: Suction drains are often used post-operatively to evacuate hematoma and seroma, preventing dead space and potential recurrence.
- Primary vs. Delayed Primary Closure: Wounds may be closed primarily if clean and viable. Delayed primary closure is often preferred after aggressive debridement, allowing for repeat debridement (second-look surgery) and ensuring no residual infection before definitive closure.
Complications and Management
Musculoskeletal infections and their treatment are associated with a wide array of complications, ranging from local wound issues to systemic manifestations and persistent disability. Effective management requires early recognition, aggressive intervention, and often a multidisciplinary approach.
Common Complications of Musculoskeletal Infections and Their Surgical Management
| Complication | Incidence (General) | Salvage / Management Strategies ## Master Infection and Microbiology A Guide to Diagnosis & Treatment
Musculoskeletal Infections Overview
Musculoskeletal infections present a critical challenge to orthopedic surgeons, often leading to significant morbidity and functional impairment. These infections encompass a broad spectrum, including osteomyelitis, septic arthritis, prosthetic joint infection (PJI), and soft tissue infections. Accurate and timely diagnosis, coupled with appropriate medical and surgical management, is paramount for optimal patient outcomes. The foundational principles of treatment involve a strategic progression from empirical to definitive therapies.
Empirical treatment is initiated based on clinical presentation, risk factors, and the presumed pathogen profile, prior to the availability of culture and sensitivity data. For musculoskeletal infections, Staphylococcus species (e.g., Staphylococcus aureus, coagulase-negative staphylococci) and Streptococcus species are the most frequently encountered organisms. This initial broad-spectrum coverage aims to control the infection rapidly while awaiting specific microbiological identification. Definitive treatment, conversely, is guided by the conclusive results of culture and sensitivity testing. This allows for de-escalation or modification of antimicrobial therapy to a narrower-spectrum agent, thereby optimizing efficacy, minimizing resistance development, and reducing drug-related toxicities. Surgical intervention is a cornerstone of musculoskeletal infection management, focusing on key principles: thorough drainage of purulent collections, aggressive débridement of necrotic or devitalized tissue (bone, soft tissue, and foreign material), and measures to restore local vascularity to facilitate host defenses and antibiotic delivery.
Bacterial Virulence and Antibiotic Resistance Mechanisms
Understanding bacterial virulence factors is crucial for appreciating the pathogenesis of musculoskeletal infections and for formulating effective treatment strategies. These factors enable bacteria to colonize, invade, and cause damage to host tissues while evading immune responses and resisting antimicrobial agents.
Antibiotic Resistance Plasmid Mediated Mechanisms
Antibiotic resistance, often mediated by mobile genetic elements such as plasmids, represents a significant hurdle in infection control. Plasmids can transfer resistance genes between bacteria, contributing to the rapid spread of antimicrobial resistance.
- β-Lactamase (bla gene): The presence of the bla gene encoding for β-lactamase enzymes confers resistance to penicillin in staphylococcal species. These enzymes hydrolyze the β-lactam ring, inactivating penicillins and related antibiotics.
- Penicillin-Binding Protein 2a (mecA gene): The mecA gene encodes for an altered penicillin-binding protein (PBP2a), which has a low affinity for most β-lactam antibiotics. This mechanism is responsible for methicillin resistance in Staphylococcus aureus (MRSA), rendering standard penicillins, cephalosporins, and carbapenems ineffective against these strains. The emergence of MRSA has profoundly impacted empirical antibiotic choices and infection control protocols in orthopedics.
Increased Surface Adhesion and Biofilm Formation
Bacterial adhesion to host tissues and inert surfaces, particularly orthopedic implants, is a critical step in the initiation and perpetuation of musculoskeletal infections.
- Fibronectin Binding Protein (fnb gene) in Staphylococcus aureus: The fnb gene encodes for fibronectin-binding proteins (FnBPs), which mediate the attachment of S. aureus to host extracellular matrix proteins such as fibronectin. This significantly enhances bacterial adherence, not only to biological tissues but also to prosthetic materials like titanium orthopedic implants, forming an essential component of biofilm initiation.
Glycocalyx Biofilm Slime Polysaccharide Capsule
The formation of a glycocalyx, often referred to as biofilm, slime, or polysaccharide capsule, is a preeminent virulence factor, especially in implant-associated infections. Biofilms are complex communities of bacteria encased in a self-produced extracellular polymeric substance (EPS) matrix, which adheres to biotic or abiotic surfaces.
- Improved Attachment to Inert Surfaces: The EPS matrix provides a robust scaffold, significantly improving bacterial attachment to inert surfaces such as joint prostheses, plates, screws, and external fixator pins. This strong adhesion makes complete eradication challenging.
- Protection from Desiccation: The biofilm matrix provides a hydrated microenvironment, protecting bacteria from environmental stressors, including desiccation, contributing to their survival outside the host.
- Cell Protection from Phagocytosis: The physical barrier of the biofilm matrix offers substantial protection to embedded bacteria from host immune cells, particularly phagocytes. This inhibition of phagocytosis is a major mechanism by which bacteria persist in chronic infections.
- Hides PAMPs: The biofilm can obscure pathogen-associated molecular patterns (PAMPs), reducing recognition by host immune receptors.
- Protects Bacteria from Toxic Enzymes/Chemicals: The EPS matrix acts as a diffusion barrier, impeding the penetration of antibiotics, antiseptics, and host antimicrobial enzymes and reactive oxygen species, further contributing to bacterial survival and recalcitrance.
Bacterial Toxins
Bacterial toxins are potent virulence factors that can cause direct tissue damage, disrupt host cellular processes, and modulate immune responses, leading to systemic illness and severe local pathology.
- Protein A (S. aureus): Protein A, located on the surface of S. aureus, is a potent antiphagocytic factor. It binds to the Fc region of immunoglobulin G (IgG) molecules, orienting the antibody "upside down" and preventing effective opsonization and subsequent phagocytosis by macrophages and neutrophils. This allows S. aureus to evade humoral immunity.
- M Protein (Group A Streptococcus pyogenes): M protein, a fibrillar protein found on the surface of group A Streptococcus pyogenes, is a major virulence factor inhibiting phagocytosis. It does so by binding to host complement regulatory proteins, thereby inhibiting the activation of the alternative complement pathway on the bacterial cell surface. This prevents the deposition of C3b, a crucial opsonin, and protects the bacteria from complement-mediated killing.
- Endotoxin (Gram-Negative Lipopolysaccharide Capsules): Endotoxins are lipopolysaccharides (LPS) that form an integral part of the outer membrane of gram-negative bacteria. Upon bacterial lysis, LPS is released and can trigger a potent inflammatory response in the host. This can lead to systemic inflammatory response syndrome (SIRS), septic shock, disseminated intravascular coagulation (DIC), and multi-organ failure.
- Exotoxins: Exotoxins are soluble proteins secreted by bacteria, often acting at sites distant from the infection.
- Clostridium perfringens Lecithinase (Alpha Toxin): This phospholipase is the primary virulence factor in Clostridium perfringens, the causative agent of gas gangrene. It hydrolyzes lecithin in cell membranes, leading to extensive tissue destruction (myonecrosis), hemolysis of red blood cells, and increased vascular permeability. Clinically, this manifests as rapidly progressing gangrene with crepitus and systemic toxicity.
- Clostridium tetani Tetanospasmin: This neurotoxin produced by Clostridium tetani is responsible for tetanus. Tetanospasmin travels retroaxonally to the central nervous system, where it blocks the release of inhibitory neurotransmitters (glycine and gamma-aminobutyric acid) at the spinal motor neurons. This results in disinhibition of motor neurons, leading to sustained muscle spasms, rigidity (e.g., "lockjaw" or trismus), and opisthotonus.
- Clostridium botulinum Botulism Toxin: This potent neurotoxin produced by Clostridium botulinum blocks the release of acetylcholine at the neuromuscular junction. This leads to flaccid paralysis. In infants, this can manifest as "floppy baby syndrome." Medically, attenuated forms of botulinum toxin are used therapeutically for muscle spasticity (e.g., cerebral palsy) and cosmetic applications.
- Community-Associated MRSA (CA-MRSA) Panton-Valentine Leukocidin (PVL) Cytotoxin: PVL is a pore-forming cytotoxin produced by certain strains of CA-MRSA. It creates pores in the membranes of leukocytes, particularly neutrophils, leading to cell lysis. PVL is associated with severe necrotizing skin and soft tissue infections, including severe cellulitis, abscesses, and necrotizing pneumonia, contributing to rapid tissue destruction and increased virulence in CA-MRSA infections.
Post Operative Rehabilitation Protocols
Rehabilitation following surgical management of musculoskeletal infections is a critical, often protracted, process that must be meticulously planned and executed. The primary goals are to restore function, prevent stiffness, and facilitate healing while protecting the surgical site and ensuring infection eradication. Rehabilitation protocols must be individualized, considering the extent of debridement, bone and soft tissue reconstruction, implant stability, and the patient's overall medical status.
Early Post Operative Phase
- Wound Care and Infection Control: Meticulous wound care is paramount. Regular dressing changes, monitoring for signs of infection recurrence (erythema, swelling, discharge), and adherence to antibiotic regimens are essential. Wound dehiscence or seroma formation can necessitate further intervention.
- Pain Management: Aggressive pain management is crucial for patient comfort and participation in therapy.
- Immobilization/Protection: Depending on the surgical procedure and stability of bone/soft tissue reconstruction, the affected limb may require immobilization (e.g., splint, brace, cast) to protect healing tissues and optimize revascularization. This is particularly important after extensive bone debridement or flap reconstruction.
- Early Range of Motion (ROM): For septic arthritis or PJI cases where implants are retained or exchanged and stable, early, gentle, passive, or active-assisted ROM exercises may be initiated to prevent joint stiffness and maintain articular cartilage health. However, this must be carefully balanced against wound integrity and implant stability. In cases of extensive bone debridement or compromised soft tissue, ROM may be delayed.
- Weight Bearing: Weight-bearing restrictions are common, especially after bone debridement, bone grafting, or joint exchanges. These restrictions are gradually advanced based on radiographic evidence of bone healing, implant stability, and pain levels.
Intermediate Post Operative Phase
- Progressive ROM and Strengthening: As healing progresses, ROM exercises are advanced, and a progressive strengthening program is initiated. This targets muscles weakened by disuse, surgical insult, or infection.
- Gait Training: If lower extremity is involved, gait training with assistive devices (crutches, walker) progresses from partial to full weight bearing as tolerated and indicated by healing.
- Edema Management: Compression garments, elevation, and manual lymphatic drainage may be used to manage persistent edema, which can impair function and healing.
- Scar Management: Techniques such as massage, silicone sheeting, and stretching are employed to improve scar pliability and prevent contractures, especially after extensive soft tissue debridement or flap surgery.
Late Post Operative Phase and Return to Function
- Advanced Strengthening and Proprioception: Focus shifts to higher-level strengthening, endurance training, and proprioceptive exercises to prepare for return to daily activities, work, or sports.
- Functional Training: Activity-specific training to simulate occupational or recreational demands.
- Psychosocial Support: Patients undergoing treatment for chronic musculoskeletal infections often face significant psychosocial challenges. Depression, anxiety, and fear of recurrence are common. Psychological support, patient education, and a collaborative approach with the patient's primary care physician are integral to successful long-term rehabilitation.
- Long-Term Monitoring: Continued clinical and laboratory monitoring (ESR, CRP) is often necessary for months to years to detect signs of infection recurrence. This is particularly true for PJI, where late recurrence remains a concern.
Throughout the rehabilitation process, close communication between the surgeon, physical therapist, and infectious disease specialist is paramount to ensure that functional goals align with the biological realities of infection eradication and tissue healing. Any signs of infection recurrence necessitate immediate re-evaluation and potential re-intervention.
Summary of Key Literature and Guidelines
The management of musculoskeletal infections is continuously evolving, driven by advancements in microbiology, imaging, surgical techniques, and antimicrobial therapies. A thorough understanding of current literature and established guidelines is essential for evidence-based practice.
Key literature highlights the critical role of multidisciplinary teams, typically including orthopedic surgeons, infectious disease specialists, microbiologists, and rehabilitation specialists, for optimizing patient outcomes in complex infections like PJI and chronic osteomyelitis. High-level evidence supports the two-stage exchange arthroplasty as the gold standard for chronic PJI, achieving infection eradication rates of 85-95% in many series. However, research continues on the efficacy of one-stage exchange in selected cases, with studies suggesting comparable success rates when strict inclusion criteria are met (e.g., known susceptible organism, good soft tissue, well-preserved bone stock).
Regarding osteomyelitis, literature consistently emphasizes radical surgical débridement as the cornerstone of treatment, followed by targeted, long-duration antibiotic therapy. Studies investigating antibiotic-impregnated polymethylmethacrylate (PMMA) beads and cement spacers demonstrate their effectiveness in achieving high local antibiotic concentrations and aiding dead space management, particularly for chronic osteomyelitis and PJI. The role of vascularized flaps for soft tissue coverage and bone reconstruction after extensive débridement is also well-established in the literature, improving healing rates and reducing recurrence, especially in challenging defects or immunocompromised patients.
Guidelines from professional organizations such as the Musculoskeletal Infection Society (MSIS), Infectious Diseases Society of America (IDSA), and the American Academy of Orthopaedic Surgeons (AAOS) provide invaluable frameworks for diagnosis and treatment. These guidelines offer recommendations on:
- Diagnostic Criteria: Standardized definitions for PJI, including synovial fluid analysis (cell count, differential, alpha-defensin), tissue histopathology, and culture criteria.
- Antimicrobial Selection: Recommendations for empirical antibiotic regimens based on common pathogens and resistance patterns, with detailed guidance on switching to definitive therapy based on culture results. The guidelines underscore the importance of susceptibility testing, particularly concerning MRSA (mecA gene) and β-lactamase producing organisms (bla gene).
- Surgical Management Algorithms: Detailed algorithms for managing various types of musculoskeletal infections, including when to consider DAIR, one-stage, or two-stage exchange for PJI, and the extent of débridement required for osteomyelitis.
- Duration of Antibiotic Therapy: Evidence-based recommendations for the duration of intravenous and oral antibiotic courses, often ranging from 6 weeks to several months, depending on the infection type, organism, and surgical success.
- Role of Biofilms: These guidelines increasingly acknowledge the profound impact of biofilm formation on treatment outcomes and emphasize the need for surgical removal of colonized implants and thorough débridement to disrupt the biofilm matrix.
- Prevention Strategies: Recommendations for perioperative antibiotic prophylaxis, glycemic control, and nutritional optimization to minimize infection risk.
Continuous engagement with current research, participation in national and international consensus groups, and adherence to evolving guidelines are critical for orthopedic surgeons to deliver the highest standard of care in the challenging field of musculoskeletal infection management. The dynamic nature of bacterial resistance and new therapeutic modalities necessitates lifelong learning and adaptive practice.
