Mastering Axillary Space Resections: An Intraoperative Guide to Complex Tumor Excision and Neurovascular Preservation
Key Takeaway
Welcome, fellows, to an immersive masterclass on axillary space exploration and tumor resection. This complex region, housing vital neurovascular structures, demands meticulous technique. We'll navigate the intricate anatomy, from muscular boundaries to the brachial plexus and axillary vessels, ensuring precise tumor excision while preserving limb function. Our focus: comprehensive preoperative planning, exact patient positioning, and a granular, step-by-step intraoperative execution, emphasizing critical pearls and pitfalls for successful limb-sparing outcomes.
Introduction and Epidemiology
The axilla represents a complex anatomic crossroad that frequently serves as a site for both primary soft tissue sarcomas and metastatic disease. Sarcomas in this region typically originate from the robust musculature defining the axillary space, including the pectoralis major, latissimus dorsi, teres major, and subscapularis. Occasionally, primary malignant tumors arise directly from the neurovascular structures traversing the axilla, presenting as malignant peripheral nerve sheath tumors (MPNST), neurofibrosarcomas, or leiomyosarcomas of the axillary vessels. Rarely do primary sarcomas develop within the axillary fat pad itself.
More frequently, orthopedic oncologists encounter massive, matted metastatic deposits within the regional lymph nodes requiring radical resection. Recurrent breast carcinoma and metastatic melanoma are the most common culprits. Historically, the surgical management of massive axillary tumors was limited to forequarter amputation. However, significant advancements in multi-planar radiographic imaging, neoadjuvant chemoradiation protocols, and microvascular reconstructive techniques have revolutionized our approach, making limb-sparing resections the standard of care for appropriately selected patients.
The epidemiology of primary axillary tumors heavily favors soft tissue sarcomas in the adult population, with undifferentiated pleomorphic sarcoma (UPS), myxofibrosarcoma, and liposarcoma representing the most frequently encountered histologic subtypes. Synovial sarcoma, despite its nomenclature, often arises in the periarticular soft tissues of the shoulder girdle and axilla in young adults. MPNSTs are particularly noteworthy in this anatomic region due to the dense concentration of the brachial plexus; these tumors may arise sporadically or in the setting of neurofibromatosis type 1 (NF1), where they often demonstrate aggressive biologic behavior and a high propensity for both local recurrence and distant metastasis.
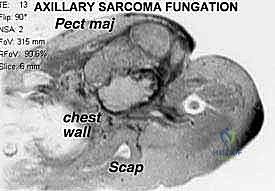
Metastatic disease to the axilla, while primarily the domain of surgical oncology and breast surgery, frequently necessitates the expertise of the orthopedic oncologist when tumor volume dictates en bloc resection of adjacent musculoskeletal or neurovascular structures. The axillary lymph node basin is the primary drainage site for the upper extremity, the breast, and the superficial tissues of the thoracoabdominal wall above the level of the umbilicus. Consequently, advanced melanomas of the upper extremity or trunk, as well as neglected or recurrent breast carcinomas, can present as fungating, neurovascularly invasive axillary masses.
The paradigm shift from ablative surgery to limb salvage in the upper extremity mirrors the evolution seen in lower extremity sarcoma management, albeit with unique challenges. The upper extremity's primary function is spatial positioning of the hand; thus, preserving a insensate, flail limb via a technically successful limb salvage procedure offers no functional advantage over amputation and may indeed represent a significant detriment to the patient's quality of life. Therefore, the decision-making process in axillary tumor surgery is inexorably linked to the anticipated functional outcome, dictating a meticulous, individualized approach to each patient.
Surgical Anatomy and Biomechanics
General Axillary Boundaries
A profound understanding of axillary anatomy is the cornerstone of safe oncologic resection in this region. The axilla is a truncated, pyramid-shaped space situated between the lateral chest wall and the proximal upper extremity.
- Apex: Formed by the convergence of the clavicle anteriorly, the superior border of the scapula posteriorly, and the outer border of the first rib medially. This forms the cervicoaxillary canal, the critical conduit for structures passing from the root of the neck into the arm.
- Anterior Wall: Composed of the pectoralis major and minor muscles, enveloped by the clavipectoral fascia. The clavipectoral fascia is a dense fibrous sheet extending from the clavicle to the axillary fascia, splitting to enclose the subclavius and pectoralis minor muscles.
- Posterior Wall: Formed by the subscapularis superiorly, and the teres major and latissimus dorsi inferiorly. The posterior wall extends further inferiorly than the anterior wall.
- Medial Wall: Defined by the upper four to five ribs and their corresponding intercostal muscles, overlaid by the serratus anterior muscle. The long thoracic nerve descends along the superficial aspect of the serratus anterior, making it vulnerable during deep medial dissections.
- Lateral Wall: A narrow boundary formed by the intertubercular sulcus of the humerus, housing the coracobrachialis and the short head of the biceps brachii.
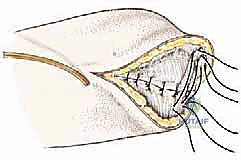
The Infraclavicular Brachial Plexus
The neurovascular bundle is the most critical structure within the axillary space. The lateral, posterior, and medial cords of the brachial plexus are named according to their spatial relationship to the second part of the axillary artery, deep to the pectoralis minor.
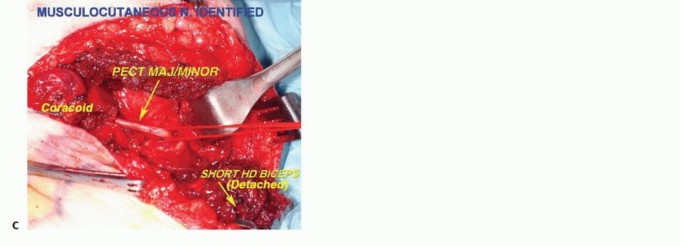
- Lateral Cord: Gives rise to the musculocutaneous nerve and the lateral root of the median nerve. The musculocutaneous nerve is typically the first major nerve encountered during anterior exploration, piercing the coracobrachialis just distal to the coracoid process. It provides motor innervation to the anterior compartment of the arm and continues as the lateral antebrachial cutaneous nerve.
- Posterior Cord: Gives rise to the upper and lower subscapular nerves, the thoracodorsal nerve, the axillary nerve, and the radial nerve. The axillary nerve courses posteriorly through the quadrangular space (bounded by the teres minor, teres major, long head of the triceps, and surgical neck of the humerus), intimately related to the inferior capsule of the glenohumeral joint. The radial nerve continues posteriorly to the axillary artery before exiting the axilla through the triangular interval.
- Medial Cord: Gives rise to the medial pectoral nerve, the medial brachial cutaneous nerve, the medial antebrachial cutaneous nerve, the ulnar nerve, and the medial root of the median nerve. Due to its medial and superficial position along the neurovascular sheath, the ulnar nerve is highly susceptible to compression or direct invasion by tumors expanding from the inferior axillary space.

Axillary Vasculature and Lymphatics
The axillary artery is a direct continuation of the subclavian artery, transitioning at the lateral border of the first rib. It is divided into three parts by the pectoralis minor muscle, yielding critical branches:
- First Part: Proximal to the pectoralis minor. Gives rise to the superior thoracic artery.
- Second Part: Posterior to the pectoralis minor. Gives rise to the thoracoacromial trunk and the lateral thoracic artery.
- Third Part: Distal to the pectoralis minor. Gives rise to the subscapular artery (the largest branch, which divides into the circumflex scapular and thoracodorsal arteries), and the anterior and posterior circumflex humeral arteries.
The axillary vein lies medial and slightly anterior to the axillary artery. It is formed by the confluence of the basilic and brachial veins at the lower border of the teres major. The cephalic vein joins the axillary vein in the deltopectoral groove just distal to the clavicle.
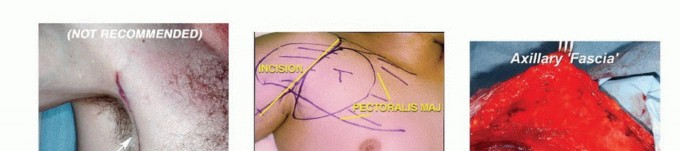
The lymphatic drainage of the axilla is anatomically categorized into three levels based on their relationship to the pectoralis minor muscle, a classification critical for both oncologic staging and surgical planning:
* Level I: Lymph nodes located lateral to the lateral border of the pectoralis minor.
* Level II: Lymph nodes located posterior to the pectoralis minor.
* Level III: Lymph nodes located medial to the medial border of the pectoralis minor, extending up to the apex of the axilla.
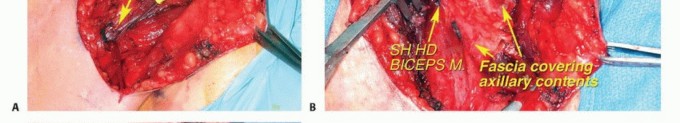
Biomechanical Implications of Muscular Resection
En bloc resection of axillary tumors frequently mandates the sacrifice of major shoulder girdle musculature. The biomechanical consequences must be anticipated.
Resection of the pectoralis major results in a predictable weakness in shoulder adduction and internal rotation. However, compensatory hypertrophy of the anterior deltoid and coracobrachialis often mitigates severe functional impairment, provided the axillary and musculocutaneous nerves remain intact.
Sacrifice of the latissimus dorsi, a common requirement for large posterior axillary tumors, leads to deficits in forceful extension, adduction, and internal rotation of the humerus. While activities of daily living are generally well-tolerated, high-demand activities (e.g., pushing up from a chair, crutch ambulation) will be noticeably compromised.
Loss of the deltoid muscle (due to axillary nerve sacrifice or direct tumor invasion) is far more devastating, resulting in a profound inability to actively abduct the shoulder, severely limiting upper extremity spatial positioning. In such scenarios, regional muscle transfers (e.g., latissimus dorsi or pectoralis major transfer) or glenohumeral arthrodesis may be required to restore a stable fulcrum for distal extremity function.
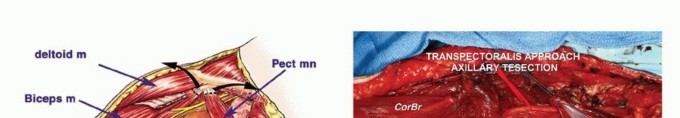
Indications and Contraindications
The decision to proceed with limb-sparing axillary resection versus forequarter amputation requires a nuanced evaluation of tumor biology, anatomic extent, and patient-specific factors. The primary objective is complete macroscopic and microscopic tumor extirpation (R0 resection) while preserving a functional and painless upper extremity.
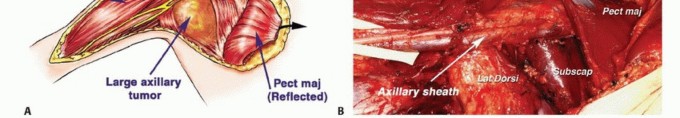
Criteria for Limb Salvage
Limb salvage is indicated when an en bloc resection can be achieved with negative margins without compromising the critical neurovascular structures required for distal limb viability and function. Involvement of a single major motor nerve (e.g., radial or musculocutaneous nerve) is not an absolute contraindication to limb salvage, as tendon transfers or nerve grafting can often restore acceptable function.
Similarly, isolated involvement of the axillary artery or vein can be managed with segmental resection and interposition grafting, provided the surrounding soft tissue envelope is adequate to cover the vascular reconstruction. The advent of advanced microvascular techniques has significantly expanded the boundaries of resectability in the axilla.
Contraindications to Limb Conserving Surgery
Absolute contraindications to limb salvage include:
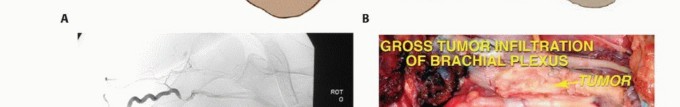
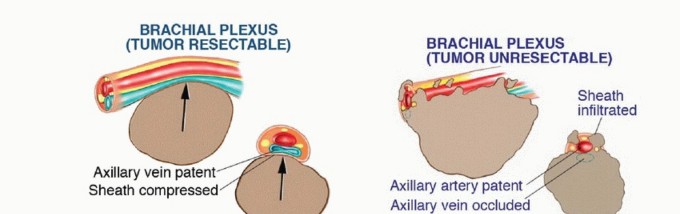
1. Involvement of the entire brachial plexus, where resection would result in a completely flail and insensate limb.
2. Extensive vascular involvement precluding reconstruction, particularly when combined with significant neural compromise.
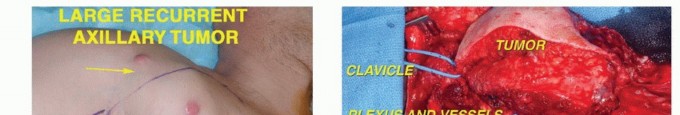
3. Massive tumor ulceration or fungation with secondary infection that precludes safe soft tissue coverage.
4. Inability to achieve negative surgical margins without sacrificing critical structures necessary for a functional limb.
Relative contraindications include severe medical comorbidities precluding lengthy reconstructive surgery, advanced age with poor baseline baseline functional status, and patient preference for a definitive, single-stage ablative procedure.
| Indication Category | Operative (Limb Salvage) Criteria | Non-Operative / Ablative (Amputation) Criteria |
|---|---|---|
| Tumor Margins | Anticipated R0 resection achievable while preserving critical neurovascular structures. | Inability to achieve R0 resection without rendering the limb flail or ischemic. |
| Brachial Plexus | Displacement without invasion, or involvement of a single resectable/reconstructable cord/branch. | Circumferential encasement or direct invasion of multiple cords/trunks. |
| Vascular Structures | Displacement, or isolated involvement amenable to segmental resection and bypass grafting. | Extensive encasement of artery and vein precluding safe bypass, or combined massive neurovascular involvement. |
| Soft Tissue Envelope | Adequate local tissue or availability of regional/free flaps for coverage of vessels and nerves. | Massive fungating tumors, severe radiation necrosis, or lack of reconstructive options. |
| Distant Metastasis | Oligometastatic disease responding to systemic therapy, or isolated primary tumor. | Widely disseminated, progressive metastatic disease with short life expectancy (palliative focus). |
Pre Operative Planning and Patient Positioning
Advanced Imaging Modalities
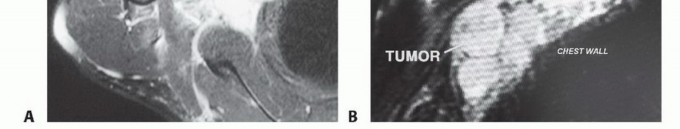
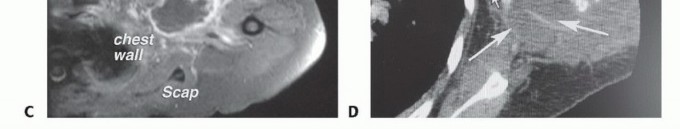
Meticulous preoperative planning is the sine qua non of successful axillary tumor resection. Magnetic Resonance Imaging (MRI) with and without intravenous gadolinium contrast is the gold standard for evaluating soft tissue sarcomas. T1-weighted images provide excellent anatomic detail and delineate the tumor's relationship to the axillary fat pad and muscular boundaries. Fluid-sensitive sequences (T2-weighted fat-suppressed or STIR) highlight peritumoral edema, which often harbors microscopic satellite lesions and must be included within the resection volume.
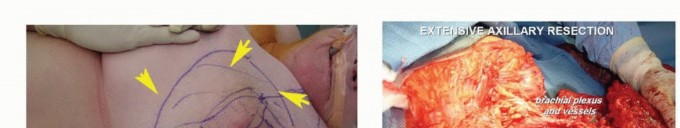
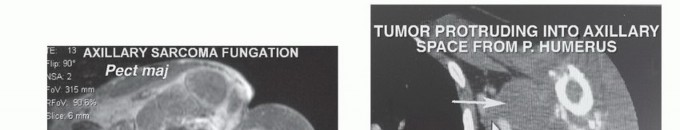
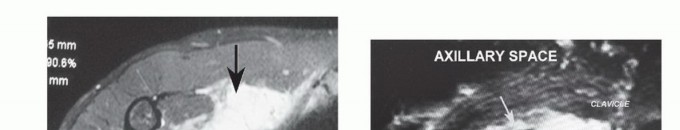
For tumors in close proximity to the axillary vessels, MR Angiography (MRA) or Computed Tomography Angiography (CTA) is essential to assess for vascular displacement, encasement, or luminal narrowing. Evidence of vascular invasion dictates the need for vascular surgery consultation and preparation for interposition grafting.
Electromyography (EMG) and Nerve Conduction Studies (NCS) may be utilized adjunctively if there is clinical evidence of brachial plexopathy, helping to establish a baseline and differentiate between compression and direct neural invasion. Furthermore, a staging CT of the chest, abdomen, and pelvis, or a whole-body FDG-PET/CT, is mandatory to rule out distant metastatic disease prior to undertaking a massive local resection.
Biopsy Principles in the Axilla
A definitive histologic diagnosis must be established prior to definitive resection. Core needle biopsy is the preferred modality. The biopsy tract must be carefully planned by the operating surgeon so that it can be excised en bloc with the tumor specimen. In the axilla, the biopsy tract should typically be placed along the planned extensile deltopectoral or axillary crease incision. Trans-compartmental biopsies or biopsies that traverse uninvolved neurovascular structures must be strictly avoided to prevent tumor seeding and upstaging of the local disease.
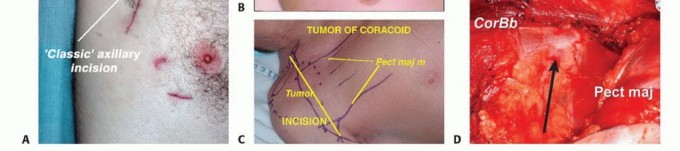
Patient Positioning and Operating Room Setup
Proper patient positioning is critical to provide unhindered access to the anterior, inferior, and posterior aspects of the axilla. The patient is typically positioned supine on a standard operating table. A bump or sandbag is placed under the ipsilateral scapula to elevate the shoulder girdle and allow the arm to fall into extension.
The entire forequarter, including the chest wall to the sternal midline, the neck up to the mandible, and the entire upper extremity down to the fingertips, is prepped and draped free. This allows for intraoperative manipulation of the arm, which is essential for visualizing different aspects of the axillary space. The arm may be supported on an arm board or held by an assistant.
If vascular reconstruction is anticipated, the ipsilateral or contralateral lower extremity (from groin to ankle) must also be prepped and draped for potential great saphenous vein harvesting. A multidisciplinary approach is often required, and the operating room should be configured to accommodate orthopedic oncology, vascular surgery, and plastic/microvascular surgery teams.
Detailed Surgical Approach and Technique
Incision Planning and Superficial Dissection
The surgical approach to the axilla must be extensile. The standard incision is an extended deltopectoral approach. The incision begins at the junction of the middle and lateral thirds of the clavicle, courses distally along the deltopectoral groove, and extends across the anterior axillary fold into the medial aspect of the arm along the medial border of the biceps brachii. For exceptionally large tumors or those extending to the apex of the axilla, the incision can be extended proximally along the superior border of the clavicle (supraclavicular extension) or distally along the mid-axillary line.
Skin flaps are elevated in the sub-fascial plane. The cephalic vein is identified within the deltopectoral groove and typically retracted laterally with the deltoid muscle. The pectoralis major muscle is exposed. Depending on the tumor's location and required margins, the pectoralis major may be retracted medially, partially resected, or entirely detached from its humeral insertion and reflected medially to expose the clavipectoral fascia.
Proximal Vascular Control
Before manipulating the tumor mass, proximal vascular control must be established. The clavipectoral fascia is incised, exposing the pectoralis minor muscle. If the tumor is intimately involved with the pectoralis minor, the muscle is taken en bloc with the specimen. Otherwise, the pectoralis minor is tenotomized at its coracoid insertion and reflected medially.

This maneuver exposes the axillary sheath containing the axillary artery, vein, and brachial plexus. Proximal control of the axillary artery and vein is obtained at the lateral border of the first rib. Vessel loops are placed around the vessels. In cases of massive apical tumors where proximal control below the clavicle is impossible, a supraclavicular approach or even a partial claviculectomy may be required to expose the subclavian vessels prior to their entry into the axillary space.

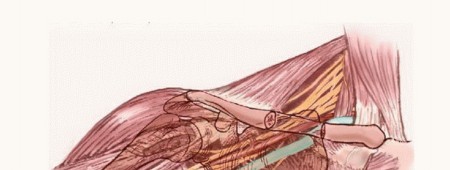
Brachial Plexus Dissection and Mobilization
Once vascular control is secured, the brachial plexus is systematically identified and mobilized. Dissection proceeds from known, normal anatomy towards the tumor margin.
The musculocutaneous nerve is identified laterally as it enters the coracobrachialis. The median nerve is formed by the confluence of its medial and lateral roots anterior to the axillary artery and is traced distally. The ulnar nerve is identified medially.

Dissection of the posterior cord and its branches (radial and axillary nerves) requires retraction of the axillary artery and vein. The radial nerve is identified posterior to the artery, and the axillary nerve is traced as it dives posteriorly into the quadrangular space.
If the tumor abuts a nerve without direct invasion, the nerve can often be spared by meticulous epineural dissection. The use of loupe magnification or an operating microscope is highly recommended during this phase. Intraoperative nerve stimulation can be invaluable in identifying distorted neural structures.

Tumor Extirpation and Margin Assessment
With the critical neurovascular structures protected or deliberately isolated for en bloc resection, the tumor is mobilized from its muscular attachments. The dissection remains strictly outside the reactive pseudocapsule, taking a cuff of normal tissue (muscle, fascia, or fat) to ensure negative margins.
The branches of the axillary artery and vein supplying the tumor (e.g., subscapular, circumflex humeral vessels) are meticulously ligated and divided. Bipolar electrocautery and surgical clips are preferred to prevent postoperative hematoma.
Once the tumor is completely mobilized, it is delivered from the wound. The surgical bed is copiously irrigated. Suspect areas on the tumor bed are marked and sent for frozen section analysis to confirm negative margins before proceeding with reconstruction.
Vascular and Soft Tissue Reconstruction
If segmental resection of the axillary artery or vein was necessary, vascular reconstruction is performed immediately. Autologous reversed great saphenous vein is the conduit of choice for arterial reconstruction due to its superior patency rates and resistance to infection compared to synthetic grafts (e.g., PTFE). Venous reconstruction is more controversial but is generally recommended to minimize postoperative limb edema, especially if collateral venous drainage has been compromised.
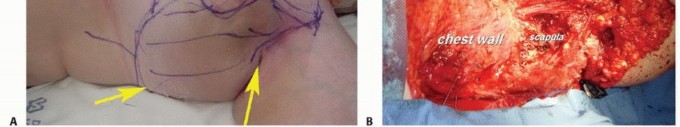
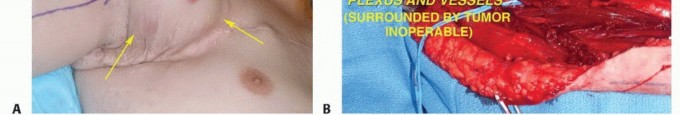
Adequate soft tissue coverage of the neurovascular
Clinical & Radiographic Imaging


You Might Also Like