Mastering Iliac Crest Bone Graft Harvest: An Intraoperative Masterclass

Key Takeaway
Join us in the OR for a detailed masterclass on iliac crest bone graft harvesting. We'll meticulously cover surgical anatomy, patient positioning, and step-by-step intraoperative execution for both anterior and posterior approaches. Learn to navigate neurovascular risks, utilize precise instrumentation, and manage potential complications, ensuring optimal outcomes for your spinal fusion patients. This guide is designed for fellows seeking to master this essential technique.
Introduction and Epidemiology
The utilization of autogenous bone graft remains the gold standard for achieving arthrodesis in orthopedic and spine surgery. Despite the advent of synthetic bone graft extenders, allografts, and recombinant human bone morphogenetic proteins (rhBMP), autologous iliac crest bone graft (ICBG) uniquely provides the essential triad required for bone healing: osteogenesis (surviving viable osteoblasts and osteoprogenitor cells), osteoinduction (bone morphogenetic proteins and growth factors), and osteoconduction (a structural trabecular scaffold).

Autogenous bone graft can be utilized at any spinal level, via anterior or posterior approaches, as well as in the management of fracture non-unions, delayed unions, and complex joint arthrodesis. The posterior ilium is most frequently harvested for large-volume, nonstructural, cancellous bone graft due to its abundant yield. Conversely, tricortical, structural bone grafts—traditionally utilized for anterior cervical interbody fusions and structural defect reconstructions—are typically harvested from the anterior ilium. While the efficacy of ICBG is undisputed, its epidemiology of use has slightly decreased over the last two decades due to the recognized incidence of donor site morbidity, prompting a rigorous risk-benefit analysis by the operating surgeon.
Surgical Anatomy and Biomechanics
A profound understanding of the osseous, muscular, and neurovascular anatomy of the pelvis is critical to safely executing an iliac crest bone graft harvest while minimizing donor-site morbidity.
Anterior Ilium Anatomy
The anterior ilium presents a concave anterosuperior surface. The anterior iliac crest is thickest at the iliac tubercle, which is located approximately 2 to 3 cm posterior to the anterior superior iliac spine (ASIS). This region provides the optimal site for harvesting a tricortical wedge.

Muscular attachments dictate the surgical planes. The tensor fasciae latae, gluteus medius, and gluteus minimus originate from the lateral aspect of the ilium. These muscles are innervated by the superior gluteal nerve. Medially, the iliacus muscle originates from the inner table. The abdominal musculature (external oblique, internal oblique, and transversus abdominis) attaches to the superior margin of the crest. Because these muscle groups are segmentally innervated, an incision directly over the crest represents a safe, internervous plane.
Neurovascular structures at risk during anterior harvest include:
* Lateral Femoral Cutaneous Nerve (LFCN): Typically courses medial to the ASIS under the inguinal ligament. However, anatomical variants exist where the LFCN crosses lateral to the ASIS, placing it at direct risk during dissection or retractor placement.
* Ilioinguinal Nerve: Courses medially along the inner table of the ilium; at risk if deep medial subperiosteal dissection is performed.

Posterior Ilium Anatomy
The posterior iliac crest provides a significantly larger volume of cancellous bone. The cortical thickness ranges from 14 to 17 mm. The posterior superior iliac spine (PSIS) serves as the primary superficial landmark, often identifiable by a cutaneous dimple in the superomedial gluteal region.

Muscular attachments include the gluteus maximus laterally and the erector spinae and multifidus medially. The lumbodorsal fascia covers this region and must be meticulously repaired to prevent postoperative herniation.
Neurovascular structures at risk during posterior harvest include:
* Superior Cluneal Nerves: These sensory branches of the dorsal rami (L1-L3) pass over the posterior iliac crest approximately 7 to 8 cm lateral to the PSIS. Lateral incisions or excessive lateral dissection place these nerves at high risk for transection or neuroma formation.
* Superior Gluteal Artery and Nerve: These structures exit the pelvis through the greater sciatic foramen. The greater sciatic notch lies approximately 6 to 8 cm deep to the PSIS. Aggressive harvesting directed inferiorly toward the notch can result in catastrophic hemorrhage from the superior gluteal artery, which may retract into the pelvis, complicating hemostasis.

Indications and Contraindications
The decision to utilize ICBG depends on the biologic requirements of the fusion site, the need for structural support, and patient-specific factors.
Operative Indications and Non Operative Alternatives
| Clinical Scenario | Operative Indication for ICBG | Non-Operative / Alternative Graft Management |
|---|---|---|
| Spinal Fusion (Posterior) | High-risk pseudoarthrosis, revision fusion, multi-level deformity correction requiring large volume osteogenic material. | Local autograft (laminectomy bone) combined with allograft or cellular bone matrices. |
| Spinal Fusion (Anterior) | Need for structural tricortical interbody support (e.g., ACDF) without the use of synthetic cages. | PEEK or Titanium interbody cages packed with local bone or demineralized bone matrix (DBM). |
| Fracture Non-union | Atrophic non-unions requiring robust osteoinduction and osteogenesis; segmental defects < 2 cm. | Extracorporeal shockwave therapy (non-operative); Reamer-irrigator-aspirator (RIA) autograft for larger defects. |
| Joint Arthrodesis | Midfoot, hindfoot, or wrist arthrodesis requiring gap filling and biologic stimulation. | Structural allografts, synthetic calcium phosphate cements, or orthobiologics (rhBMP-2). |
| Contraindications | N/A | Prior extensive harvest, local infection, severe osteoporosis, chronic pain syndromes. |
Pre Operative Planning and Patient Positioning
Preoperative assessment must include an evaluation of the patient's bone quality and a review of prior surgical incisions over the pelvic region. Radiographic evaluation (AP and lateral pelvic radiographs, or CT scans if available) helps assess the thickness of the iliac tables and the structural integrity of the pelvis.
Informed consent must explicitly detail the risks of donor site morbidity, including chronic pain, lateral thigh numbness, and cosmetic deformity.

Patient Positioning
Anterior Harvest:
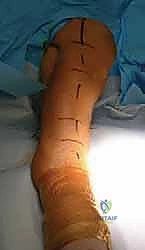
The patient is positioned supine. A bump (rolled towels or a blanket) is placed beneath the ipsilateral ischial tuberosity and hemipelvis. This elevates the hemipelvis, drops the abdominal contents medially, and facilitates unencumbered access to the anterior iliac crest. The ASIS and the iliac tubercle should be carefully palpated and marked.

Posterior Harvest:
The patient is positioned prone on a radiolucent Jackson table or Wilson frame, depending on the primary spinal procedure. Chest and pelvic rolls must be placed to ensure the abdomen hangs completely free, reducing venous pressure and intraoperative bleeding. The PSIS is palpated and marked. The surgical field must be prepped widely to allow for adjustments in the incision trajectory.
Detailed Surgical Approach and Technique
Meticulous surgical technique is paramount to maximizing graft yield while minimizing tissue trauma and subsequent morbidity.
Anterior Iliac Crest Approach
- Incision: A skin incision is made parallel to the iliac crest, centered over the iliac tubercle (the thickest portion of the crest). The incision must begin at least 2 to 3 cm posterior to the ASIS to avoid injury to the LFCN and to prevent postoperative avulsion fractures of the ASIS.
- Superficial Dissection: The subcutaneous tissue is sharply divided down to the fascial layer overlying the iliac crest. Hemostasis is achieved with electrocautery.
- Fascial Incision and Periosteal Elevation: The fascia is incised directly over the midline of the bony crest. Subperiosteal dissection is then performed to expose the lateral wing (outer table) or medial wing (inner table) of the ilium, depending on the graft requirement.
- Tissue Preservation: Care is taken to preserve the fascial edges. A robust fascial cuff must be maintained to facilitate a secure, tension-free closure, which is critical for minimizing postoperative pain and preventing muscle herniation.

Anterior Graft Harvest Techniques
- Tricortical Structural Graft: Parallel transverse cuts are made using an oscillating saw or sharp osteotomes through the inner and outer tables. A basal cut connects the transverse cuts to liberate the wedge.
- Cancellous Harvest (Trapdoor Technique): To preserve the structural contour of the crest and minimize cosmetic deformity, a cortical "trapdoor" is elevated. An osteotome is used to hinge the superior crest cortex. Cancellous bone is then harvested using curettes and gouges from between the intact inner and outer tables. The cortical lid is subsequently reduced and secured.

Posterior Iliac Crest Approach
- Incision: The PSIS is palpated. A vertical incision directly over the PSIS is preferred to minimize the risk of transecting the superior cluneal nerves, which run transversely. Alternatively, an oblique or curved incision may be utilized, provided it remains medial to the cluneal nerve crossing zone (7 to 12 cm anterolateral to the PSIS).
- Fascial Exposure: The subcutaneous tissue is divided to the level of the lumbodorsal fascia and the iliac crest. Using electrocautery, the fascia is incised directly over the bony prominence.
- Subperiosteal Dissection: The gluteus maximus is elevated subperiosteally off the outer table of the ilium. Blunt retractors (e.g., Taylor retractors) are placed. The surgeon must remain vigilant regarding the depth of dissection; staying superior to the sciatic notch is imperative to avoid the superior gluteal neurovascular bundle.

Posterior Graft Harvest Techniques
For large-volume cancellous harvest, the outer table is often fenestrated or a cortical window is removed. Large gouges and curettes are utilized to excavate the cancellous bone extending anteriorly and inferiorly between the tables. Acetabular reamers can occasionally be used for rapid, large-volume extraction in major deformity cases.

Following harvest, meticulous hemostasis is required. Bone wax, gelatin sponges (Gelfoam), or microfibrillar collagen (Avitene) are placed into the defect. A closed suction drain is frequently placed deep to the fascia to prevent hematoma formation.

Complications and Management
Donor site morbidity associated with ICBG harvest is well-documented, with reported complication rates ranging from 10% to 39%. Complications are categorized as major (requiring reoperation or prolonged hospitalization) and minor.

Table of Complications and Management Strategies
| Complication | Incidence | Etiology / Risk Factor | Prevention and Management Strategy |
|---|---|---|---|
| Chronic Donor Site Pain | 15% - 30% | Neuroma, inadequate fascial closure, altered biomechanics. | Prevention: Meticulous fascial closure, trapdoor technique. Management: Multimodal analgesia, local injections, gabapentinoids. |
| Meralgia Paresthetica | 2% - 10% | Injury/traction to the Lateral Femoral Cutaneous Nerve (LFCN). | Prevention: Incision 2-3 cm posterior to ASIS. Management: Often self-limiting; observation, nerve blocks. |
| Cluneal Nerve Neuroma | 1% - 5% | Transection of superior cluneal nerves during posterior approach. | Prevention: Vertical incision over PSIS; avoid lateral dissection >7cm from PSIS. Management: Corticosteroid injections, surgical excision of neuroma. |
| Pelvic Fracture (ASIS/Iliac Wing) | < 1% | Over-harvesting, violation of ASIS, severe osteoporosis. | Prevention: Maintain 3 cm distance from ASIS; avoid deep cortical notching. Management: Protected weight-bearing; rarely requires internal fixation. |
| Superior Gluteal Artery Hemorrhage | < 1% | Dissection entering the greater sciatic notch. | Prevention: Limit deep inferior dissection. Management: Packing, immediate vascular surgery consultation, angiographic embolization. |
| Hematoma / Seroma | 3% - 10% | Bleeding from cancellous bone bed. | Prevention: Bone wax, topical hemostatics, closed suction drain. Management: Evacuation if expanding or causing wound breakdown. |
| Hernia (Lumbar or Abdominal) | < 1% | Failure to close the fascial defect; removal of full-thickness bone. | Prevention: Robust layered fascial closure. Management: General surgery consultation for mesh herniorrhaphy. |

Post Operative Rehabilitation Protocols
Postoperative rehabilitation is primarily dictated by the primary surgical procedure (e.g., spinal fusion, fracture fixation). However, specific considerations regarding the ICBG donor site must be integrated into the protocol.
- Immediate Postoperative Phase (0-2 Weeks):
- Pain management is the primary focus. Multimodal analgesia, including scheduled acetaminophen, NSAIDs (if not contraindicated by the fusion), and short-acting opioids, is utilized.
- Continuous infusion local anesthetic pain pumps (e.g., bupivacaine) placed subfascially at the donor site during closure have shown significant efficacy in reducing early postoperative opioid consumption.
- Mobilization should begin on postoperative day one. Weight-bearing status is determined by the primary surgery, but patients should be counseled that ambulation may exacerbate donor site pain due to the pull of the gluteal and abdominal musculature on the healing fascial repair.

-
Subacute Phase (2-6 Weeks):
- Suture or staple removal typically occurs at 14 days.
- Patients are encouraged to perform gentle active range of motion of the hip and core.
- Desensitization techniques can be employed if superficial hyperesthesia is noted around the incision.
-
Long-term Rehabilitation (>6 Weeks):
- Focus shifts to core strengthening and gluteal rehabilitation to restore normal pelvic biomechanics and gait kinematics.
- Persistent pain beyond 3 to 6 months requires evaluation for potential neuroma formation or unrecognized pelvic stress fracture.
Summary of Key Literature and Guidelines
The academic discourse surrounding ICBG versus alternative graft materials is extensive. While orthobiologics have revolutionized fusion surgery, ICBG remains the benchmark.
- Boden et al. established the fundamental biologic superiority of autograft in achieving posterolateral spinal fusion, highlighting the necessity of viable osteoprogenitor cells which are absent in allografts.
- Dimond et al. evaluated the morbidity of the posterior iliac crest harvest, quantifying the incidence of chronic pain and establishing the anatomical safe zones regarding the cluneal nerves and the sciatic notch. Their work forms the basis of modern anatomical harvesting guidelines.
- Kurz et al. provided a comprehensive review of anterior iliac crest complications, specifically detailing the biomechanical risks of ASIS avulsion fractures and the necessity of preserving a 3 cm bony bridge anteriorly.
- Recent systematic reviews comparing ICBG to rhBMP-2 in spinal fusion demonstrate comparable fusion rates. However, while rhBMP-2 eliminates donor site morbidity, it introduces unique complication profiles, including heterotopic ossification, radiculitis, and significantly higher costs. Consequently, major orthopedic and neurosurgical guidelines continue to support ICBG as a highly efficacious, cost-effective standard of care, particularly in revision scenarios or resource-stratified environments.
You Might Also Like