Surgical Masterclass: Advanced Repair of Athletic Pubalgia with Dual-Layer Mesh Technique
Key Takeaway
This masterclass provides an exhaustive guide to athletic pubalgia repair, focusing on dual-layer mesh techniques. Fellows will gain real-time insights into comprehensive surgical anatomy, meticulous intraoperative execution, and critical pearls for managing complex groin injuries. We cover precise incision, deep dissection, hardware application, and strategies to prevent recurrence, ensuring optimal recovery and return to sport for athletes.
Introduction and Epidemiology
Athletic pubalgia, often interchangeably referred to as a sports hernia or core muscle injury, encompasses a complex spectrum of chronic groin injuries predominantly observed in high-level athletes. The nomenclature surrounding this condition has historically been ambiguous, with terms such as Gilmore’s groin, pubalgia, and sports hernia utilized to describe overlapping clinical entities. In contemporary orthopedic sports medicine, athletic pubalgia is understood as a debilitating condition characterized by chronic groin pain resulting from an occult tear or attenuation of the inguinal floor, specifically involving the transversalis fascia, conjoint tendon, and the aponeurotic insertions of the rectus abdominis and adductor longus, without the presence of a clinically obvious, palpable abdominal wall hernia.
Diagnosis of the underlying etiology of groin pain remains notoriously challenging due to the intricate regional anatomy and the frequent coexistence of multiple pathologies. Intra-abdominal pathology, genitourinary abnormalities, referred lumbosacral pain, and intra-articular hip joint disorders—most notably femoroacetabular impingement (FAI)—must be systematically excluded.
Epidemiologically, athletic pubalgia is most prevalent in sports requiring repetitive, explosive twisting, cutting, and pivoting maneuvers. Consequently, it is disproportionately diagnosed in soccer, ice hockey, rugby, and American football players. The pathogenesis typically involves a sudden, eccentric contraction of the adductor musculature against a fixed lower extremity, often occurring at the myotendinous junction or the aponeurotic insertion. Adductor strains represent the most common cause of groin pain in athletes, and these injuries frequently coexist with structural deficiencies of the lower abdominal wall. Osteitis pubis, characterized by symphyseal pain and joint disruption, is another overlapping entity commonly seen in distance runners and soccer players, further confounding the clinical picture. Stress fractures of the pubic rami, while rare, result from repetitive cyclic loading and must be considered in the differential diagnosis, particularly in endurance athletes.

Surgical Anatomy and Biomechanics
A thorough understanding of the complex three-dimensional anatomy of the groin and anterior pelvis is paramount for the accurate diagnosis and surgical management of athletic pubalgia. The pubic symphysis acts as the central fulcrum for the anterior pelvis, balancing the antagonistic forces of the abdominal musculature pulling superiorly and the adductor musculature pulling inferiorly.
Osseous and Articular Structures
The pubic symphysis is a rigid, nonsynovial, amphiarthrodial joint consisting of layers of hyaline cartilage encasing a central fibrocartilaginous disc. This joint must withstand immense shear forces during athletic activity. The pubic tubercle serves as the critical anchor point for several major tendinous and aponeurotic structures.

Musculotendinous Aponeurotic Plate
The anterior pelvic anatomy is defined by the rectus abdominis-adductor longus aponeurotic plate. The rectus abdominis inserts onto the anterior pubis, while the adductor longus originates just inferior to this insertion. These structures are anatomically contiguous, forming a shared aponeurosis over the anterior pubis. Disruption of this aponeurotic plate alters the biomechanical equilibrium of the pelvis. When the rectus abdominis insertion is attenuated or torn, the unopposed pull of the adductor longus creates an anterior and inferior shear force on the pubic symphysis, leading to chronic pain, secondary osteitis pubis, and further destabilization of the pelvic ring.

Other muscles in and around the groin region, including the rectus femoris, the sartorius, the gracilis, and the abdominal obliques, contribute to the dynamic stability of the region. The posterior inguinal wall consists primarily of the transversalis fascia, along with the conjoint tendon, which is formed by the confluence of the internal abdominal oblique and transversus abdominis aponeuroses. The conjoint tendon inserts onto the pubic tubercle and along the iliopubic tract.

Inguinal Canal and Neurovascular Considerations
The inguinal canal is an oblique cleft in the lower anterior abdominal wall. Its anterior wall is formed by the external oblique aponeurosis, and its floor is formed by the transversalis fascia. In athletic pubalgia, it is this posterior wall (the inguinal floor) that is typically attenuated or torn.

Surgeons must possess an intimate knowledge of the regional neuroanatomy to avoid iatrogenic injury during pelvic floor reconstruction. The three primary nerves of concern are:
1. Ilioinguinal Nerve (L1): Pierces the internal oblique muscle and travels within the inguinal canal, exiting through the superficial inguinal ring to provide sensation to the superomedial thigh and the root of the penis/mons pubis.
2. Iliohypogastric Nerve (T12-L1): Runs superior to the ilioinguinal nerve, piercing the external oblique aponeurosis superior to the superficial ring.
3. Genitofemoral Nerve (L1-L2): The genital branch travels within the spermatic cord, supplying the cremaster muscle and scrotal sensation.


Indications and Contraindications
Surgical intervention for athletic pubalgia is typically considered a diagnosis of exclusion and is indicated only after a comprehensive trial of non-operative management has failed to return the athlete to their pre-injury level of competition.
Operative vs Non Operative Management
| Clinical Scenario | Recommended Management | Rationale |
|---|---|---|
| First-time acute adductor strain | Non-Operative | High rate of healing with conservative therapy, eccentric strengthening, and phased return to play. |
| Chronic groin pain (>8-12 weeks) failing PT | Operative | Indicates structural failure of the rectus-adductor aponeurotic plate or posterior inguinal wall requiring mechanical repair. |
| MRI evidence of rectus avulsion or secondary cleft sign | Operative | High likelihood of persistent biomechanical instability; unlikely to resolve with conservative measures alone. |
| Coexisting symptomatic FAI and Athletic Pubalgia | Operative (Staged or Concurrent) | Addressing only the pelvic floor while ignoring the hip pathology leads to high failure rates due to persistent abnormal pelvic biomechanics. |
| Incidental asymptomatic osteitis pubis on imaging | Non-Operative | Often an adaptive change in high-level athletes; does not warrant surgical intervention in the absence of mechanical symptoms. |
Contraindications to surgical intervention include active systemic or local infection, untreated intra-abdominal pathology (e.g., inflammatory bowel disease, genitourinary malignancy), and the presence of primary, symptomatic intra-articular hip pathology that has not been addressed. Failure to recognize and treat concurrent FAI is a primary cause of failed athletic pubalgia surgery, as the restricted hip internal rotation forces compensatory, deleterious shear stresses across the pubic symphysis.

Pre Operative Planning and Patient Positioning
Clinical Evaluation
The clinical examination must be meticulous. The duration of symptoms is typically months, and the pain is classically resistant to conservative measures. The patient often recalls a sudden, intense pain in the groin during an acute event, followed by chronic, insidious discomfort that worsens with exertion and improves with rest.
Palpation is critical. With increasing experience, the examiner can invaginate the scrotum to palpate the superficial inguinal ring, noting an abnormal, patulous inguinal floor and appreciating exquisite tenderness inside the external ring or directly over the pubic tubercle.
Provocative testing includes:
* Resisted Sit-Up Test: Elicits pain at the rectus abdominis insertion.
* Adductor Squeeze Test: Performed at 0, 45, and 90 degrees of hip flexion to isolate the adductor longus and pectineus.
* Single-Leg Hop Test: Evaluates for pelvic ring instability or stress fractures.

Diagnostic Imaging
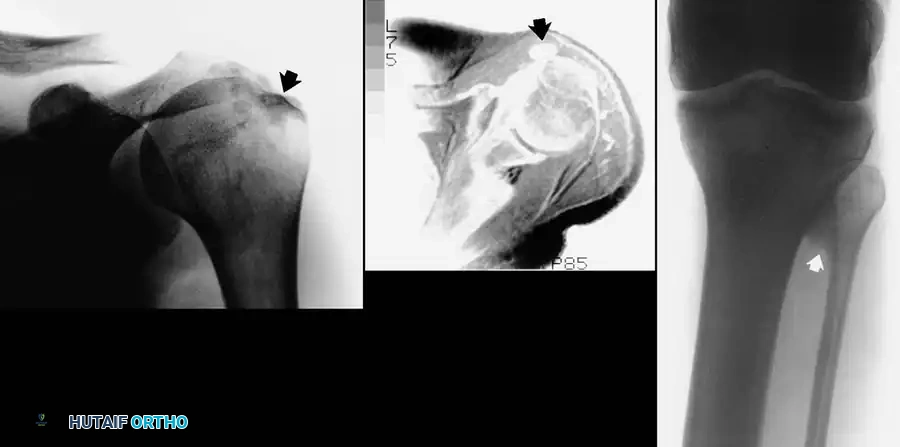
Imaging is essential to rule out competing diagnoses and confirm the structural deficits of athletic pubalgia.
* Radiographs: An AP pelvis, Dunn lateral, and false profile views of the hips are mandatory to evaluate for FAI, osteitis pubis (symphyseal sclerosis, widening, or cyst formation), and subtle avulsion fractures.
* Magnetic Resonance Imaging (MRI): A dedicated athletic pubalgia MRI protocol (high-resolution, small field-of-view fluid-sensitive sequences of the pubic symphysis) is the gold standard. Pathognomonic findings include the "secondary cleft sign" (indicating a tear of the adductor longus/rectus abdominis aponeurosis extending inferiorly), marrow edema in the anterior pubic body, and attenuation of the conjoint tendon.
* Dynamic Ultrasound: Can be utilized to visualize posterior wall ballooning during a Valsalva maneuver and to assess the integrity of the adductor origin dynamically.


Patient Positioning and Anesthesia
The procedure is typically performed under general anesthesia, though regional anesthesia (spinal or epidural) is a viable alternative. The patient is placed in the supine position on a standard radiolucent operating table. For cases requiring concurrent adductor release, the operative leg may be placed in a mild frog-leg position (flexed, abducted, and externally rotated) to place the adductor longus under tension. The abdomen and bilateral lower extremities are prepped and draped in a standard sterile fashion, allowing access from the umbilicus to the mid-thighs.

Detailed Surgical Approach and Technique
Surgical management typically involves an open anterior pelvic floor repair, often combined with an adductor longus tenotomy or fractional lengthening, depending on the preoperative clinical and radiographic findings. While laparoscopic techniques (Totally Extraperitoneal [TEP] or Transabdominal Preperitoneal [TAPP] with mesh placement) are employed by some general surgeons, the open anatomic repair remains the gold standard in orthopedic sports medicine for restoring the biomechanical integrity of the rectus-adductor aponeurotic plate.
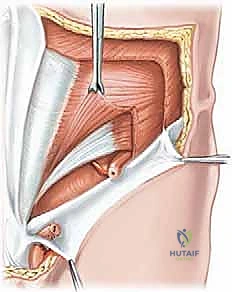
Superficial Dissection and Nerve Identification
- Incision: A 4 to 6 cm oblique incision is made along the Langer lines, centered over the superficial inguinal ring, approximately 2 cm superior and parallel to the inguinal ligament.
- Fascial Dissection: Dissection is carried down through the subcutaneous tissue and Camper's fascia. Scarpa's fascia is sharply incised to expose the external oblique aponeurosis.
- External Oblique Aponeurosis: The external oblique aponeurosis is incised parallel to its fibers, extending from the superficial inguinal ring laterally. Care is taken not to extend the incision too far medially to avoid disrupting the medial crus.
- Nerve Protection: The ilioinguinal nerve is immediately identified on the undersurface of the external oblique aponeurosis or resting on the internal oblique muscle. It is meticulously mobilized and protected with a vessel loop. The iliohypogastric nerve is also identified superiorly and protected.


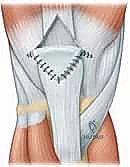
Pelvic Floor and Rectus Abdominis Repair
- Assessment of the Posterior Wall: The spermatic cord (or round ligament in females) is mobilized and encircled with a Penrose drain. The posterior wall of the inguinal canal (transversalis fascia) is inspected. In athletic pubalgia, this fascia is typically found to be attenuated, bulging, or frankly torn near its insertion on the pubic tubercle.
- Rectus Abdominis Reattachment: If the rectus abdominis insertion is partially avulsed, the necrotic or fibrotic margins are debrided. The lateral border of the rectus abdominis is mobilized.
- Transversalis Fascia Plication: The attenuated transversalis fascia is plicated and repaired using heavy, non-absorbable, monofilament suture (e.g., 0 or 2-0 Prolene). The repair begins at the pubic tubercle and extends laterally toward the internal ring, effectively tightening the posterior inguinal wall.
- Conjoint Tendon and Rectus Repair: The inferior edge of the conjoint tendon and the lateral margin of the rectus abdominis are sutured to the inguinal ligament (Poupart's ligament) and the reflection of the external oblique, restoring the dynamic stability of the anterior pelvic ring.
- Mesh Utilization: In cases of severe tissue attenuation or recurrent injuries, a lightweight, macroporous synthetic mesh or biologic graft may be placed in the preperitoneal space or as an onlay to reinforce the repair, though primary tissue repair is preferred in elite athletes to maintain physiologic compliance.


Adductor Longus Tenotomy
Given the antagonistic relationship between the rectus abdominis and the adductor longus, releasing the adductor longus is frequently necessary to decompress the anterior pelvis and protect the abdominal wall repair.
- Incision: A separate 3 cm longitudinal incision is made over the palpable adductor longus tendon at the proximal medial thigh.
- Tendon Isolation: The adductor longus tendon is isolated from the underlying pectineus and the posterior adductor brevis. Care is taken to protect the anterior branch of the obturator nerve, which lies deep to the adductor longus.
- Tenotomy: A fractional lengthening (releasing the tendinous portion while leaving the muscular belly intact) or a complete transverse tenotomy is performed approximately 1 to 2 cm distal to the pubic insertion.
- Closure: The incisions are irrigated copiously. The external oblique aponeurosis is closed over the spermatic cord, recreating the superficial inguinal ring without causing constriction. Subcutaneous tissues and skin are closed in layers.


Complications and Management
While surgical outcomes for athletic pubalgia are generally excellent, with return-to-play rates exceeding 90% in appropriately selected cohorts, complications can occur and must be managed aggressively.
Table of Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology | Salvage Strategy and Management |
|---|---|---|---|
| Nerve Entrapment (Ilioinguinal / Iliohypogastric) | 2% - 5% | Suture entrapment, excessive scar tissue formation, or iatrogenic transection during external oblique opening. | Initial management includes gabapentinoids and targeted diagnostic/therapeutic nerve blocks. Refractory cases require surgical exploration, neurolysis, or selective neurectomy with proximal burying of the nerve stump into the internal oblique muscle belly. |
| Recurrent Groin Pain | 5% - 10% | Failure to address concurrent hip pathology (FAI), premature return to sport, or failure of the primary repair. | Comprehensive re-evaluation including intra-articular hip injections and repeat MRI. If FAI is identified, hip arthroscopy is indicated. If primary repair failed, revision surgery with mesh reinforcement may be necessary. |
| Scrotal / Labial Hematoma | 3% - 7% | Inadequate hemostasis of the cremasteric vessels or superficial epigastric vessels. | Usually self-limiting. Management includes scrotal elevation, ice, and compression. Surgical evacuation is rarely indicated unless expanding rapidly or causing skin necrosis. |
| Adductor Weakness | 1% - 3% | Over-aggressive adductor release or iatrogenic injury to the anterior branch of the obturator nerve. | Prolonged physical therapy focusing on compensatory strengthening of the pectineus, gracilis, and adductor magnus. Nerve injury requires EMG/NCS evaluation. |
| Deep Vein Thrombosis (DVT) | < 1% | Pelvic surgery, localized inflammation, and postoperative immobility. | Standard anticoagulation protocols. Early mobilization is the primary preventative measure. |


Clinical & Radiographic Imaging
























You Might Also Like