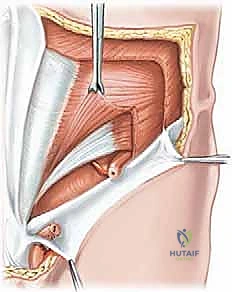
Adductor Longus Tenotomy: An Intraoperative Masterclass for Chronic Groin Pain

Key Takeaway
This masterclass details adductor longus tenotomy for chronic groin pain in athletes. We cover essential surgical anatomy, meticulous preoperative planning, and a step-by-step intraoperative guide, emphasizing precise technique and nerve protection. Fellows will learn to navigate common pitfalls, manage complications, and guide patients through a structured postoperative rehabilitation program for optimal recovery and return to sport.
Introduction and Epidemiology
Definition and Clinical Spectrum
Groin injuries represent a significant and complex diagnostic challenge in sports medicine, accounting for approximately two to five percent of all athletic injuries. Within this broad spectrum of pathology, adductor longus related groin pain emerges as the most frequently encountered clinical entity. The differential diagnosis for groin pain in the elite athlete is notoriously extensive, encompassing intraarticular hip pathology, osteitis pubis, athletic pubalgia, and genitourinary abnormalities. Precise isolation of the adductor longus as the primary pain generator is critical for implementing an effective therapeutic algorithm.
Adductor longus pathology predominantly manifests in athletes participating in high velocity kicking sports, such as soccer, and in disciplines demanding rapid, high torque directional changes, including ice hockey, rugby, and American football. The clinical presentation is generally dichotomized into acute and chronic phases. Acute adductor related groin pain typically represents a musculotendinous junction strain, though complete avulsions of the adductor longus origin from the pubis can occur in rare, high energy scenarios. Conversely, chronic adductor pain frequently presents as an isolated enthesopathy or concomitantly with the pre hernia complex, commonly referred to as athletic pubalgia or a sports hernia.
Incidence and Demographics
Epidemiological data indicates a strong male predilection for adductor related groin pain, largely reflecting the demographic distribution in high risk sports. Prior adductor strain is the single most significant independent risk factor for future injury. Furthermore, biomechanical screening has demonstrated that an adductor to abductor muscle strength ratio of less than eighty percent is highly predictive of future adductor strains. Recognizing these epidemiological patterns is essential for orthopedic surgeons and sports medicine physicians when designing preseason screening and targeted injury prevention protocols.

Surgical Anatomy and Biomechanics
Osteology and Musculotendinous Origins
A profound understanding of the anterior pelvic osteology and the complex myotendinous architecture is paramount for accurate diagnosis and surgical intervention. The adductor longus is a robust, fan shaped muscle originating from the anteromedial aspect of the superior pubic ramus, immediately inferior to the pubic tubercle. It extends distally to insert on the linea aspera of the posterior femur.
The origin of the adductor longus is anatomically unique, consisting of a direct attachment of both tendinous structures and muscular fibers directly to the periosteum of the pubis. The proximal tendon possesses a notably narrow cross sectional area, which concentrates mechanical stress during eccentric loading. This proximal tendon is readily identifiable on the anterior surface of the muscle belly, transitioning via an oblique musculotendinous junction. Conversely, the proximal posterior surface is typically entirely muscular in origin. A frequently encountered anatomical anomaly involves muscle fibers forming the lateral five to eleven millimeters of the anterior origin, a variation that must be recognized during surgical release.

Neurovascular Supply
The adductor longus is innervated by the anterior division of the obturator nerve. The obturator nerve arises from the lumbar plexus (L2, L3, L4), traverses the obturator foramen, and bifurcates into anterior and posterior divisions. The anterior division descends anterior to the adductor brevis and posterior to the pectineus and adductor longus, providing motor innervation to these structures. Surgical approaches to the proximal adductor longus must meticulously respect this neurovascular anatomy to prevent iatrogenic denervation of the medial compartment of the thigh. Vascular supply is derived primarily from the deep femoral artery and its medial circumflex femoral branch.
Kinematics and Pathomechanics
The pathogenesis of chronic adductor strains and their frequent association with athletic pubalgia is rooted in the complex biomechanics of the pelvic ring. The rectus abdominis and the adductor longus share a confluent fascial attachment at the pubic symphysis, forming the rectus abdominis adductor longus aponeurotic plate. This structural continuity means that forces generated by the lower extremity are directly transmitted to the anterior abdominal wall.
Pathology typically arises in athletes utilizing powerful, ballistic muscle actions. A classic mechanism involves a rapid transition from a posteriorly rotated trunk and planted foot, with simultaneous hip extension and abduction, to a sudden, explosive anterior trunk rotation coupled with hip flexion and adduction. This exact kinematic sequence is observed during an in step soccer kick or the recovery phase of a hockey stride. These actions subject the adductor longus origin to immense eccentric loads followed by forceful concentric contraction. Over time, repetitive microtrauma leads to chronic tendinosis, enthesopathy, and potential microtearing of the aponeurotic plate. Furthermore, subtle degrees of pelvic instability or symphyseal micro-motion may exacerbate this sheer stress, leading to the clinical manifestation of the pre hernia complex.
Indications and Contraindications
Diagnostic Criteria and Clinical Evaluation
The decision to proceed with operative intervention for adductor related groin pain requires a meticulous clinical evaluation. Patients typically present with localized pain over the adductor longus origin that is exacerbated by sport specific activities. Physical examination hallmarks include profound tenderness at the inferior pubic ramus and pain with resisted hip adduction, particularly when tested in zero degrees and forty five degrees of hip flexion. The single adductor test and the bilateral adductor squeeze test are highly sensitive provocative maneuvers.
Operative management is rarely indicated for acute musculotendinous strains, which possess a robust capacity for intrinsic healing. Even in the rare instance of a complete adductor longus avulsion from the pubis, nonoperative management remains the preferred initial strategy, as functional deficits are often minimal following structured rehabilitation. However, chronic adductor enthesopathy that is refractory to prolonged conservative management, or adductor pathology presenting concomitantly with a functionally limiting sports hernia, warrants surgical consideration.

Nonoperative Versus Operative Management
| Clinical Scenario | Recommended Management Strategy | Key Considerations and Rationale |
|---|---|---|
| Acute Musculotendinous Strain (Grade I to III) | Strict Nonoperative Management | High healing potential via conservative measures. Focus on progressive loading and eccentric strengthening. |
| Complete Proximal Avulsion | Primary Nonoperative Management | Surgical repair is rarely indicated. Functional outcomes are generally excellent with structured rehabilitation. |
| Chronic Isolated Enthesopathy | Exhaustive Conservative Trial | Minimum of three to six months of physical therapy, core stabilization, and judicious corticosteroid or PRP injections. |
| Refractory Chronic Enthesopathy | Operative Intervention | Adductor tenotomy or fractional lengthening indicated after failure of comprehensive conservative protocols. |
| Concomitant Athletic Pubalgia | Combined Operative Intervention | Pelvic floor repair combined with adductor release to address the entire rectus abdominis adductor longus aponeurotic plate. |
| Significant Hip Osteoarthritis | Relative Contraindication to Surgery | Groin pain is likely referred from the intraarticular hip joint. Address the primary joint pathology first. |
Pre Operative Planning and Patient Positioning
Imaging Modalities
Advanced imaging is indispensable for preoperative planning and for differentiating adductor pathology from other causes of groin pain. Plain radiography, including an anteroposterior pelvis and flamingo views, is utilized to assess for osteitis pubis, symphyseal instability, and cam or pincer morphology indicative of femoroacetabular impingement.
Magnetic Resonance Imaging is the gold standard for evaluating the adductor origin and the rectus abdominis aponeurosis. High resolution, non contrast MRI of the pelvis should include T1 weighted, T2 weighted, and fat suppressed short T1 inversion recovery sequences. In a mature pelvis, the fibrocartilage of the symphysis pubis develops a central fluid filled cleft, which manifests as a central focus of high signal intensity on T2 and STIR imaging. Pathologic findings include marrow edema at the pubic tubercle, thickening or partial tearing of the adductor longus tendon, and the "secondary cleft sign." The secondary cleft sign represents an abnormal extension of fluid signal from the symphysis pubis laterally into the adductor longus origin or superiorly into the rectus abdominis insertion, indicating a macroscopic tear of the aponeurotic plate.

Anesthesia and Positioning
Surgical intervention for adductor related groin pain can be performed under general anesthesia or regional anesthesia, depending on patient comorbidities and surgeon preference. Regional anesthesia provides excellent postoperative pain control but may interfere with immediate postoperative neurological assessments.
The patient is positioned supine on a standard radiolucent operating table. The operative lower extremity is prepped and draped free to allow for dynamic intraoperative manipulation. The hip is typically positioned in a "frog leg" posture, utilizing approximately forty five degrees of hip flexion, forty five degrees of abduction, and maximal external rotation. This positioning places the adductor longus under tension, facilitating identification of the proximal tendon and rendering the surgical planes more accessible. A sterile tourniquet is generally not required, though meticulous hemostasis is mandatory to prevent postoperative hematoma formation.
Detailed Surgical Approach and Technique
Surgical Anatomy and Incision
The surgical approach for an adductor longus tenotomy requires precise identification of the superficial landmarks. The pubic tubercle is palpated, and the prominent, cord like origin of the adductor longus is identified immediately inferior to it. A longitudinal incision, approximately three to five centimeters in length, is centered over the palpable proximal tendon, beginning just distal to the inguinal crease. Alternatively, a transverse incision aligned with the Langer lines can be utilized for superior cosmetic outcomes, though it provides slightly less extensibility.
Dissection proceeds sharply through the skin and subcutaneous tissues. Camper fascia and Scarpa fascia are sequentially incised. Superficial veins, including branches of the external pudendal vessels, are frequently encountered in this layer and must be carefully cauterized or ligated to prevent postoperative hematoma. Deep to Scarpa fascia, the deep investing fascia of the thigh is encountered and incised longitudinally in line with the adductor longus fibers.

Deep Dissection and Adductor Release
Once the deep fascia is opened, the epimysium of the adductor longus is exposed. The surgeon must clearly delineate the medial and lateral borders of the proximal tendon. Blunt dissection is utilized to sweep the surrounding adipose tissue and identify the internervous plane. It is critical to differentiate the adductor longus from the more medially located gracilis and the deeper adductor brevis.
A right angle clamp is carefully passed posterior to the adductor longus tendon, remaining strictly superficial to the adductor brevis fascia. This maneuver isolates the adductor longus while protecting the anterior division of the obturator nerve, which courses deep to the longus and anterior to the brevis.
The release can be performed as a complete tenotomy or a fractional lengthening, depending on the severity of the contracture and the presence of concomitant pathology. For a complete release, the tendinous portion of the adductor longus is transected approximately one to two centimeters distal to its insertion on the pubis. The surgeon must ensure that the muscular fibers, which often attach directly to the periosteum laterally, are also adequately released. Following transection, the muscle belly will retract distally. The underlying adductor brevis must remain intact to preserve baseline adductor strength and pelvic stability.
Concurrent Procedures for Athletic Pubalgia
In cases where chronic adductor enthesopathy is accompanied by athletic pubalgia, an isolated adductor tenotomy is often insufficient, as it fails to address the destabilization of the anterior pelvic ring. In these instances, the procedure is combined with a reinforcement or repair of the rectus abdominis insertion and the posterior inguinal wall.
If a combined approach is utilized, the general surgeon or specialized orthopedic surgeon will address the abdominal wall pathology first, often utilizing a mesh repair or primary fascial plication, followed immediately by the adductor release. This comprehensive approach restores the equilibrium of the rectus abdominis adductor longus aponeurotic plate, alleviating the pathological sheer forces acting across the pubic symphysis. Following the release, the wound is irrigated copiously, and meticulous hemostasis is confirmed. The deep fascia is left open to prevent compartment syndrome, and the subcutaneous tissue and skin are closed in a standard layered fashion.
Complications and Management
Intraoperative and Postoperative Risks
While adductor tenotomy is generally considered a safe and highly effective procedure, specific anatomical risks must be mitigated through meticulous surgical technique. The most devastating intraoperative complication is iatrogenic injury to the anterior division of the obturator nerve. This occurs if dissection strays deep to the adductor longus or if the adductor brevis fascia is inadvertently violated. Nerve injury results in profound weakness of hip adduction and sensory deficits over the medial thigh.
Postoperative hematoma is the most common complication, given the highly vascular nature of the medial thigh musculature and the rich venous plexus surrounding the external genitalia. Meticulous intraoperative hemostasis and the judicious use of a closed suction drain in highly vascularized cases can mitigate this risk. Infection is rare but requires standard aggressive management if superficial or deep space involvement is suspected.

| Complication | Estimated Incidence | Prevention and Management Strategies |
|---|---|---|
| Postoperative Hematoma | Three to Five Percent | Meticulous intraoperative electrocautery. Ligation of external pudendal branches. Consider short term closed suction drainage. Manage with compressive dressings; surgical evacuation rarely needed. |
| Obturator Nerve Injury | Less than One Percent | Maintain dissection strictly superficial to the adductor brevis. Use blunt dissection when passing instruments posterior to the adductor longus tendon. |
| Superficial Surgical Site Infection | One to Two Percent | Standard perioperative intravenous antibiotics. Chlorhexidine skin preparation. Treat with culture directed oral antibiotics. |
| Prolonged Adductor Weakness | Two to Four Percent | Ensure the adductor brevis and magnus are entirely preserved during the release. Implement a rigorous, phased postoperative strengthening protocol. |
| Recurrence of Groin Pain | Five to Ten Percent | Accurate preoperative diagnosis is crucial. Ensure concomitant athletic pubalgia or intraarticular hip pathology (FAI) was not missed. May require revision surgery or pelvic floor repair. |
Post Operative Rehabilitation Protocols
Acute Phase Recovery
The postoperative rehabilitation protocol following an adductor tenotomy is designed to facilitate tissue healing while preventing severe contracture of the retracted muscle belly. During the initial acute phase (weeks zero to two), the primary goals are pain control, edema reduction, and the restoration of basic mobility. Patients are typically allowed to weight bear as tolerated with the assistance of crutches, weaning off the assistive devices as their antalgic gait resolves.
Immediate postoperative interventions include cryotherapy and gentle, pain free passive range of motion. Aggressive stretching of the adductor compartment is strictly contraindicated during this phase to prevent hematoma formation and disruption of the healing inflammatory matrix. Isometric contractions of the quadriceps, hamstrings, and gluteal musculature are initiated to maintain lower extremity neuromuscular control.
Return to Play Criteria
The intermediate phase (weeks two to six) focuses on restoring full, symmetric range of motion and initiating progressive resistance training. Stationary cycling and aquatic therapy are excellent modalities for promoting cardiovascular fitness without subjecting the healing adductor complex to high sheer forces. Concentric strengthening of the adductors is introduced gradually, beginning with submaximal isometrics and progressing to isotonic exercises using resistance bands or light cable weights.
The advanced phase (weeks six and beyond) is dedicated to sport specific functional rehabilitation. The core objective is to restore the adductor to abductor muscle strength ratio to greater than eighty percent, which is the established benchmark for minimizing reinjury risk. Eccentric loading protocols for the adductor longus are critical during this phase, as eccentric strength is vital for decelerating the lower extremity during high velocity kicking and skating.
Return to play is permitted when the athlete demonstrates pain free, full range of motion, symmetrical adductor strength on dynamometer testing, and the ability to complete sport specific agility drills, such as cutting, pivoting, and maximum effort striking, without apprehension or biomechanical compensation. Most elite athletes return to full competition between eight and twelve weeks postoperatively.
Summary of Key Literature and Guidelines
Evidence Based Outcomes
The academic understanding of adductor related groin pain has evolved significantly over the past two decades, moving away from vague terminologies toward precise anatomical diagnoses. The Doha agreement meeting on terminology and definitions in groin pain in athletes represents a landmark consensus, standardizing the classification of groin pain into distinct clinical entities: adductor related, iliopsoas related, inguinal related, and pubic related groin pain. This standardization is critical for interpreting outcomes in the orthopedic literature.
Historically, the literature has strongly supported nonoperative management for acute adductor strains. Studies utilizing MRI to grade acute strains have demonstrated that even high grade tears at the musculotendinous junction heal predictably with structured rehabilitation, with athletes returning to play in an average of four to eight weeks.
For chronic adductor enthesopathy, surgical outcomes have been extensively documented. Literature reviews assessing isolated adductor tenotomy report success rates ranging from seventy five to ninety percent in appropriately selected athletes. However, prominent sports medicine surgeons have increasingly highlighted the biomechanical interplay between the adductor longus and the rectus abdominis. Contemporary studies demonstrate that when adductor tenotomy is combined with a pelvic floor repair in patients exhibiting signs of the pre hernia complex, return to play rates exceed ninety percent, with a significantly lower incidence of recurrent groin pain compared to isolated adductor release.
Ultimately, successful management of adductor related groin pain requires a rigorous adherence to evidence based diagnostic criteria, an exhaustive trial of targeted nonoperative therapies, and precise surgical execution when conservative measures fail. Continuous advancements in high resolution imaging and biomechanical screening will further refine the indications for operative intervention, optimizing outcomes for the elite athletic population.
You Might Also Like