Operative Management of Distal Femur Fractures: External Fixation and Unicondylar Reconstruction
Key Takeaway
External fixation serves as a critical damage-control modality for severe, open distal femoral fractures, particularly those complicated by vascular compromise. When managing unicondylar fractures, including coronal Hoffa variants, precise anatomical reduction and rigid internal fixation are mandatory. This guide details the biomechanics, surgical techniques, and conversion protocols essential for optimizing outcomes in complex distal femur trauma.
EXTERNAL FIXATION IN DISTAL FEMORAL FRACTURES
The management of severe, high-energy distal femoral fractures presents a formidable challenge to the orthopaedic surgeon. In the context of polytrauma, severe soft tissue compromise, or gross contamination, immediate definitive internal fixation is often contraindicated. External fixation serves as an indispensable tool, utilized as either a temporary damage-control measure or, less commonly, as a definitive stabilization technique.
External fixation is particularly critical in the presence of severe open distal femoral fractures (Gustilo-Anderson Types IIIB and IIIC) and fractures associated with concomitant popliteal or superficial femoral vascular injuries. In these catastrophic scenarios, rapid skeletal stabilization is a prerequisite for successful vascular repair and soft tissue management.
Indications and Biomechanical Considerations
The primary goal of temporary external fixation is to restore length, alignment, and rotation while providing local traction and allowing mobility for patients with multiple traumatic injuries.
- Damage Control Orthopaedics (DCO): In the hemodynamically unstable polytrauma patient, a rapidly applied external fixator minimizes additional surgical hits, controls hemorrhage from the fracture site, and mitigates the systemic inflammatory response syndrome (SIRS).
- Vascular Injury: Skeletal stability must be achieved prior to or simultaneously with vascular repair to prevent disruption of the vascular anastomosis.
- Severe Soft Tissue Compromise: Open fractures with extensive degloving or contamination require serial debridements. External fixation provides rigid stability without introducing hardware into a contaminated field.
Surgical Warning: If the fracture exhibits a significant intercondylar component (AO Type C), the external fixator must span the knee joint. Attempting to place pins into small, comminuted condylar fragments risks intra-articular penetration, inadequate purchase, and catastrophic failure of the construct.
Surgical Technique: Knee-Spanning External Fixation
The application of a knee-spanning external fixator must be executed with precision to avoid neurovascular injury and to facilitate future conversion to internal fixation.
1. Patient Positioning and Preparation:
The patient is positioned supine on a radiolucent trauma table. The entire lower extremity from the iliac crest to the toes is prepped and draped to allow for unrestricted fluoroscopic access and potential extension of the surgical field.
2. Femoral Pin Placement:
* Two or three 5.0 mm or 6.0 mm half-pins are placed in the anterior or anterolateral aspect of the intact femoral diaphysis, proximal to the fracture zone.
* Safe Zone: Pins should be placed under fluoroscopic guidance. Care must be taken to avoid the suprapatellar pouch, which can extend up to 5-7 cm proximal to the superior pole of the patella. Intra-articular pin placement guarantees septic arthritis.
* A generous stab incision is made, the iliotibial band is split, and the vastus lateralis is bluntly retracted. A tissue protector must be used during drilling to prevent thermal necrosis of the bone and soft tissue entanglement.
3. Tibial Pin Placement:
* Two 5.0 mm half-pins are placed in the anterior or anteromedial aspect of the proximal tibial diaphysis.
* Pins should be placed distal to the tibial tubercle to avoid the joint capsule and the proximal tibial physis (in skeletally immature patients).
4. Frame Assembly and Reduction:
* Carbon fiber rods are utilized to connect the femoral and tibial pins.
* Longitudinal traction is applied to restore limb length. Coronal and sagittal alignment are corrected under fluoroscopic visualization.
* A dual-rod construct (often in a delta or multi-planar configuration) is recommended to maximize biomechanical stiffness, particularly in heavy patients or those with severe instability.
Postoperative Protocols and Conversion Strategies
A major advantage of temporary external fixation is that it allows for superior computed tomography (CT) evaluation of the distal femoral fracture. Without the artifact generated by bulky internal plates or intramedullary nails, the surgeon can meticulously map coronal shear fractures, articular comminution, and bone voids, thereby formulating a precise preoperative plan for definitive fixation.
Clinical Pearl: The 14-Day Rule. Conversion from a temporary external fixator to definitive internal fixation (plate osteosynthesis or intramedullary nailing) must ideally be performed within 14 days. Prolonged external fixation exponentially increases the risk of pin track colonization and subsequent deep infection upon conversion.
Early conversion from a spanning external fixator to an intramedullary nail or locking plate is highly safe and effective in patients with multiple injuries, provided the soft tissue envelope has adequately recovered and systemic physiology is optimized.
Salvage Fixation:
If a patient is placed in a spanning external fixator and remains medically unfit for internal fixation within the 14-day window of safety, the temporary frame must be revised. The spanning fixator can be converted to a definitive small wire (Ilizarov) fixator or a hybrid fixator.
* This method is strictly reserved for salvage in severe, unsalvageable soft-tissue injuries or delayed presentations.
* Complications: Definitive external fixation of the distal femur is associated with a 1% to 10% deep infection rate. Furthermore, it universally results in significant knee stiffness. However, it is crucial to recognize that this stiffness is primarily dictated by the severe nature of the initial trauma (articular scarring, quadriceps fibrosis) rather than the method of fixation itself.
CONDYLAR FRACTURES OF THE FEMUR
While high-energy trauma often results in complex, multi-fragmentary fractures, isolated condylar fractures present a distinct biomechanical and surgical challenge. These injuries require meticulous attention to articular congruity and absolute stability.
Unicondylar Fractures of the Femur (AO Type B)
Unicondylar fractures of the distal femur (AO/OTA Type 33-B) are partial articular fractures where one part of the articular surface remains in continuity with the femoral diaphysis. They occur less frequently than their supracondylar (Type A) or complete articular intercondylar (Type C) counterparts.
These fractures are typically the result of axial loading combined with varus or valgus stress. Concomitant injuries to the ipsilateral extremity—such as tibial plateau fractures, patellar fractures, or ligamentous disruptions—are present in approximately one-third of patients, necessitating a high index of suspicion during the initial evaluation.
Classification of Unicondylar Fractures
The AO/OTA classification divides Type B fractures into three distinct categories based on the anatomical plane of the fracture:
* Type B1: Sagittal fracture of the lateral condyle.
* Type B2: Sagittal fracture of the medial condyle.
* Type B3: Coronal fracture of the anterior or posterior condyle (commonly known as a Hoffa fracture).
Clinical Evaluation and Advanced Imaging
Accurate diagnosis hinges on a comprehensive radiographic evaluation. A standard trauma series is often insufficient to fully characterize the articular involvement.
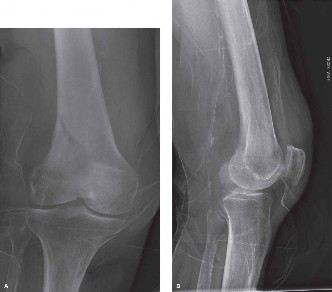
- Standard Radiographs: Anteroposterior (AP) and lateral views of the femur and knee are mandatory.
- Specialized Views: Tangential patellar (skyline) and tunnel (notch) views are necessary to accurately diagnose associated injuries to the patellofemoral joint and to visualize osteochondral fragments within the intercondylar notch.
- Computed Tomography (CT): A CT scan with 2D and 3D reconstructions is an absolute necessity for surgical planning. Coronal fractures of the posterior condyle (Hoffa fractures) are notoriously difficult to identify on standard AP radiographs and can be easily missed or underestimated on lateral views due to the overlap of the intact condyle. CT accurately defines the size, displacement, and comminution of the articular fragments.
Nonoperative Management
Nondisplaced unicondylar fractures can theoretically be treated nonoperatively. This involves strict non-weight-bearing mobilization in a hinged knee brace locked in extension for 4 to 6 weeks, followed by a graduated range of motion protocol.
Pitfall: Nonoperative management carries a high risk of secondary displacement due to the deforming forces of the gastrocnemius and the inherent instability of the articular shear fragment. Patients must be followed closely with weekly radiographs for the first month. Any loss of reduction is an absolute indication for surgical intervention.
Surgical Management of Displaced Unicondylar Fractures
Displaced unicondylar fractures require prompt surgical fixation. The goals of surgery are anatomical reduction of the articular surface, rigid internal fixation to allow early mobilization, and prevention of post-traumatic osteoarthritis.
Surgical Approaches
The choice of surgical approach is dictated by the specific condyle involved and the fracture pattern:
* Lateral Parapatellar Approach: The workhorse approach for Type B1 (lateral condyle) fractures. It provides excellent visualization of the lateral articular surface and the lateral metaphysis.
* Medial Subvastus or Medial Parapatellar Approach: Utilized for Type B2 (medial condyle) fractures. The subvastus approach spares the quadriceps tendon, facilitating faster postoperative rehabilitation.
* Swashbuckler Approach: A modified anterior approach that involves elevating the vastus lateralis off the linea aspera. It is highly effective for complex lateral condyle fractures with significant posterior extension or associated metaphyseal comminution.
Fixation Techniques
Because unicondylar fractures are intra-articular, the biomechanical principle of absolute stability must be applied. This is achieved through interfragmentary compression and buttress plating.
1. Sagittal Fractures (Type B1 and B2):
* Reduction: The articular surface is anatomically reduced under direct vision and temporarily held with pointed reduction forceps.
* Lag Screw Fixation: Interfragmentary compression is achieved using 4.5 mm or 6.5 mm partially threaded cancellous lag screws placed perpendicular to the fracture plane.
* Buttress Plating: Lag screws alone are biomechanically insufficient to withstand the shear forces of weight-bearing. A contoured locking or non-locking plate must be applied to the affected cortex (lateral for B1, medial for B2) to function as an anti-glide or buttress plate. The plate neutralizes axial loads and prevents proximal migration of the condylar fragment.
2. Coronal Fractures (Type B3 / Hoffa Fractures):
Hoffa fractures represent a unique biomechanical challenge. The posterior condylar fragment is subjected to immense shear forces during knee flexion, driven by the pull of the gastrocnemius muscle and the articulation of the tibial plateau.
- Approach: A lateral or medial approach is used depending on the affected condyle. For severe posterior comminution, a posterior approach (e.g., posteromedial or posterolateral) may occasionally be required.
- Fixation: The gold standard for Hoffa fractures is fixation with multiple anterior-to-posterior (AP) or posterior-to-anterior (PA) lag screws.
- Biomechanical Superiority: PA directed screws are biomechanically superior as they are placed perpendicular to the fracture line and engage the dense bone of the anterior metaphysis. However, PA screw placement requires extensive posterior dissection. Therefore, AP directed screws (often headless compression screws or countersunk 3.5/4.5 mm cortical screws) are more commonly utilized.
- If AP screws are used, the screw heads must be countersunk below the articular cartilage to prevent iatrogenic damage to the patella or tibial plateau during knee range of motion.
- In cases of osteoporotic bone or large Hoffa fragments, supplementary posterior buttress plating may be necessary to prevent shear failure.
Postoperative Rehabilitation
Regardless of the fixation method, the postoperative protocol must balance the need for fracture healing with the prevention of knee stiffness.
* Early Motion: Continuous passive motion (CPM) or active-assisted range of motion is initiated within 24 to 48 hours postoperatively to nourish the articular cartilage and prevent intra-articular adhesions.
* Weight-Bearing: Patients are typically restricted to toe-touch or non-weight-bearing for 8 to 12 weeks, depending on radiographic evidence of callus formation and the security of the initial fixation.
* Thromboprophylaxis: Standard deep vein thrombosis (DVT) prophylaxis is mandatory until the patient is fully mobile.
By adhering to strict biomechanical principles—whether utilizing damage-control external fixation for catastrophic trauma or executing precise articular reconstruction for unicondylar fractures—the orthopaedic surgeon can maximize functional recovery and minimize the devastating complications associated with distal femoral injuries.
You Might Also Like