Elbow Arthroscopy for Degenerative Joint Disease: An Intraoperative Masterclass
Key Takeaway
This masterclass guides fellows through arthroscopic débridement for elbow degenerative joint disease. We'll cover essential anatomy, meticulous patient positioning, and a granular, real-time surgical execution from initial incision to hardware application. Extensive pearls, pitfalls, and postoperative protocols ensure comprehensive learning for managing elbow osteoarthritis with arthroscopy.
Introduction and Epidemiology
Primary degenerative arthritis of the elbow joint is a relatively uncommon condition when compared to osteoarthritis of weight-bearing joints such as the hip or knee. The unique non-weight-bearing biomechanics of the upper extremity generally protect the ulnohumeral and radiocapitellar articulations from early primary degeneration. However, patients who present with primary osteoarthritis of the elbow represent a distinct demographic profile. They are frequently manual laborers, heavy lifters, overhead athletes, and individuals who rely on wheelchairs or crutches for ambulation, effectively converting the upper extremity into a weight-bearing axis.
The pathogenesis of primary elbow osteoarthritis differs significantly from inflammatory arthritides, such as rheumatoid arthritis. While total elbow arthroplasty provides excellent pain relief and improved range of motion in patients with inflammatory arthritis or low functional demands, its use in young, active, or heavy-laboring patients is contraindicated. The constrained or semi-constrained nature of total elbow prostheses in high-demand patients is associated with unacceptably high rates of early aseptic loosening, polyethylene wear, and catastrophic implant failure. Similarly, elbow arthrodesis is highly undesirable for the vast majority of patients, as it sacrifices the functional arc of motion required for activities of daily living and occupational tasks in favor of pain relief.

Historically, open débridement procedures, such as the Outerbridge-Kashiwagi ulnohumeral arthroplasty, have been utilized with good success to address osteophyte impingement and capsular contracture. However, over the past two decades, arthroscopic osteocapsular arthroplasty has gained widespread acceptance among orthopedic surgeons. Arthroscopic débridement adequately addresses the underlying pathologic processes—osteophyte formation, loose bodies, and capsular contracture—while offering the perceived benefits of a minimally invasive approach, superior visualization of the articular compartments, reduced soft tissue trauma, and earlier return to occupational activities. Several large clinical series confirm that arthroscopic outcomes are at least equivalent to open procedures, providing durable relief that does not preclude future reconstructive procedures while minimizing perioperative morbidity.
Surgical Anatomy and Biomechanics
A profound understanding of elbow osseous anatomy, capsuloligamentous structures, and the proximity of neurovascular bundles is paramount for safe and effective arthroscopic management of degenerative joint disease. The elbow is a highly congruent, complex hinge joint composed of three distinct articulations within a single synovial cavity the ulnohumeral joint, the radiocapitellar joint, and the proximal radioulnar joint.
At the distal humerus, the coronoid fossa anteriorly and the olecranon fossa posteriorly serve as critical recesses that accommodate the coronoid process and the tip of the olecranon during terminal flexion and extension, respectively. In the setting of primary degenerative joint disease, reactive bone formation leads to the development of hypertrophic osteophytes within these fossae and on the corresponding articular processes.

Pathoanatomy of Elbow Impingement
The natural history of primary elbow osteoarthritis is characterized by a slowly progressive joint contracture. Loss and fragmentation of articular cartilage lead to the formation of intra-articular loose bodies, which frequently sequester in the olecranon fossa, coronoid fossa, or radiocapitellar gutter.
Mechanical impingement occurs via two primary mechanisms
1. Anterior Impingement Hypertrophic osteophytes on the coronoid process and within the coronoid fossa abut during terminal flexion, leading to anterior mechanical block and pain.
2. Posterior Impingement Osteophytes on the tip of the olecranon and within the olecranon fossa abut during terminal extension, creating a posterior mechanical block.
Concurrently, the anterior and posterior joint capsules become thickened, fibrotic, and contracted. A contracted anterior capsule restricts terminal extension, whereas a contracted posterior capsule restricts terminal flexion. The combination of osseous impingement and capsular contracture results in the classic clinical presentation of terminal motion loss. It is critical to note that the articular cartilage within the mid-arc of the sigmoid notch and trochlea is often relatively preserved in primary osteoarthritis, which explains why patients typically experience pain at the extremes of motion rather than during the mid-arc of movement.
Neurovascular Considerations
The elbow is surrounded by critical neurovascular structures that dictate portal placement and surgical technique. The ulnar nerve traverses posterior to the medial epicondyle within the cubital tunnel and is at significant risk during the establishment of medial portals and during posteromedial capsular release. The radial nerve crosses the radiocapitellar joint anteriorly and is vulnerable during anterolateral portal placement and anterior capsulectomy. The median nerve and brachial artery lie anterior to the brachialis muscle; while protected by the brachialis, aggressive anterior capsulotomy or aberrant portal trajectory can result in catastrophic injury.
Indications and Contraindications
Patient selection is the most critical determinant of success in arthroscopic elbow débridement. The typical patient is a middle-aged male laborer presenting with a painful dominant elbow that worsens with heavy use. Symptoms include progressive loss of terminal flexion and extension, pain localized to the endpoints of motion, and mechanical symptoms such as catching, locking, or painful crepitus.
A thorough physical examination must document the exact arc of motion, the presence of painful crepitus, and any signs of ulnar neuritis. Ulnar nerve irritation is frequently associated with elbow degenerative joint disease due to cubital tunnel stenosis from medial osteophytes or dynamic traction from joint contracture. Documenting preoperative ulnar nerve function is mandatory, as it dictates the need for concurrent endoscopic or open in situ decompression or anterior transposition.
The ideal candidate for arthroscopic débridement has pain primarily at the extremes of motion (impingement pain) rather than pain throughout the functional arc (arthritic pain). Patients with severe mid-arc pain typically have advanced global cartilage loss, and débridement is unlikely to provide satisfactory pain relief.
| Parameter | Operative Indications | Non Operative Indications |
|---|---|---|
| Pain Characteristics | Pain at terminal flexion/extension (impingement) | Mild pain, pain easily controlled with NSAIDs |
| Mechanical Symptoms | Catching, locking, or loose bodies present | Absence of true mechanical locking |
| Range of Motion | Unacceptable loss of functional ROM (outside 30-130 degrees) | Functional ROM maintained |
| Cartilage Status | Preserved mid-arc articular cartilage | Severe global joint space destruction (mid-arc pain) |
| Neurologic Status | Progressive ulnar neuropathy requiring decompression | Normal neurologic examination |
| Prior Treatment | Failure of conservative management (6+ months) | First-line presentation, no prior therapy |
Absolute contraindications to arthroscopic débridement include active intra-articular infection, severe distortion of bony anatomy precluding safe portal placement, and advanced global osteoarthritis in a patient seeking complete pain relief. A relative contraindication is a prior ulnar nerve transposition where the exact location of the nerve is unknown, significantly increasing the risk of iatrogenic transection during medial portal placement.
Pre Operative Planning and Patient Positioning
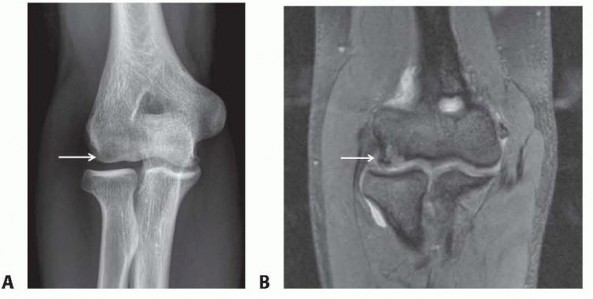
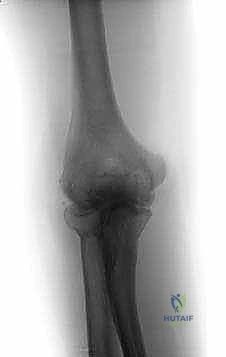
Preoperative evaluation relies heavily on high-quality imaging. Standard plain film radiographs (anteroposterior, lateral, and oblique views) are essential and typically demonstrate joint space narrowing, hypertrophic bony osteophytes, loose bodies, and subchondral sclerosis.

For comprehensive preoperative planning, computed tomography (CT) scans with two-dimensional (2-D) and three-dimensional (3-D) reconstructions are considered the gold standard. 3-D CT allows the surgeon to precisely map the location and volume of osteophytes within the coronoid and olecranon fossae, identify the exact number and location of radiolucent loose bodies, and plan the extent of bony resection required to restore impingement-free motion.
Patient Positioning Options
Arthroscopic elbow surgery can be performed in the lateral decubitus, prone, or supine suspended positions. The choice of position depends on surgeon preference, the specific compartments requiring the most extensive work, and anesthetic considerations.

Lateral Decubitus Position
The lateral decubitus position is highly favored for arthroscopic elbow débridement. The patient is positioned with the operative arm supported over a padded post or suspended via an arm holder. This position allows excellent access to both the anterior and posterior compartments. The shoulder is typically abducted to 90 degrees, and the elbow is allowed to flex freely to 90 degrees and beyond. A non-sterile tourniquet is applied high on the brachium. This setup provides a stable platform for bony resection and allows gravity to assist in joint distraction.
Prone Position
The prone position offers unparalleled access to the posterior compartment and is particularly useful when extensive olecranon fossa clearance or triceps mobilization is required. The arm is draped over a bolster, allowing the elbow to flex to 90 degrees. While posterior access is optimal, airway management is more challenging for the anesthesia team, and anterior compartment work can be slightly more technically demanding due to the orientation of the arm.
Detailed Surgical Approach and Technique
Arthroscopic elbow débridement is a technically demanding procedure that requires meticulous attention to portal placement and a systematic approach to joint clearance. The procedure is typically performed under regional anesthesia (supraclavicular or interscalene block) combined with general anesthesia to ensure complete muscle relaxation.

Joint Distension and Portal Placement
Prior to establishing portals, the joint is maximally distended with 20 to 30 mL of normal saline injected through the soft spot in the center of the anconeus triangle (bordered by the lateral epicondyle, radial head, and olecranon tip). Joint distension displaces the anterior neurovascular structures away from the capsule, increasing the margin of safety during anterior portal placement.
Anterior Compartment Debridement
The proximal anteromedial portal is typically established first. A small incision is made 2 cm proximal and 1 cm anterior to the medial epicondyle. A blunt trocar is advanced anterior to the intermuscular septum, maintaining contact with the anterior humerus to avoid the ulnar nerve posteriorly and the median nerve anteriorly. Once inside the joint, a diagnostic arthroscopy is performed.

Under direct visualization, the proximal anterolateral portal is established using an outside-in technique with a spinal needle. This portal is located 2 cm proximal and 1 cm anterior to the lateral epicondyle. The radial nerve lies in close proximity to this portal; therefore, the incision must be strictly superficial, followed by blunt dissection.
Once both anterior portals are established, the surgeon alternates the arthroscope and working instruments between them. The initial step is often a limited anterior capsulectomy. Using a motorized shaver and radiofrequency ablation wand, the thickened, contracted anterior capsule is excised to expose the coronoid fossa and the coronoid process. Care must be taken to maintain the integrity of the brachialis muscle fibers, which serve as the final barrier protecting the median nerve and brachial artery.

Following capsular release, hypertrophic osteophytes on the coronoid process are resected using an arthroscopic burr. The coronoid fossa is then deepened and cleared of all reactive bone and loose bodies to ensure the coronoid process can fully seat within the fossa during terminal flexion. The radiocapitellar joint is inspected, and any impinging osteophytes on the radial head or capitellum are contoured.
Posterior Compartment Debridement
Attention is then turned to the posterior compartment. The direct posterior and posterolateral portals are established. The direct posterior portal is located 3 cm proximal to the olecranon tip, directly through the triceps tendon. The posterolateral portal is placed just lateral to the triceps tendon, proximal to the olecranon.

The posterior compartment is frequently filled with dense fibrotic tissue, loose bodies, and massive osteophytes. A thorough posterior capsulectomy is performed. The olecranon fossa is cleared of all soft tissue and loose bodies. The hypertrophic osteophytes on the tip and medial/lateral gutters of the olecranon are aggressively resected.
If the olecranon fossa osteophytes are extensive, an arthroscopic Outerbridge-Kashiwagi fenestration (transhumeral portal) can be performed. An arthroscopic burr is used to create a fenestration through the thin bony septum separating the olecranon and coronoid fossae. This connects the anterior and posterior compartments, allowing for decompression of the joint and providing an recess for the olecranon tip to enter during terminal extension, significantly improving range of motion.

Management of the Ulnar Nerve
If the patient has preoperative symptoms of cubital tunnel syndrome, or if extensive posteromedial osteophyte resection is required, the ulnar nerve must be addressed. Depending on surgeon preference and the severity of the neuropathy, this can be managed via an endoscopic in situ decompression or a formal open anterior transposition performed prior to the arthroscopic portion of the procedure.
Complications and Management
While arthroscopic elbow débridement is generally safe, the learning curve is steep, and complications can be severe due to the unforgiving anatomy of the elbow. The overall complication rate is reported to be between 5% and 11%, which is comparable to open débridement procedures.

Neurologic injury is the most dreaded complication. Transient neuropraxias are more common than permanent nerve transections and are often related to over-distension of the joint, prolonged tourniquet time, or aggressive portal placement. Heterotopic ossification is another significant risk, particularly in patients with a history of trauma or prior elbow surgery.
| Complication | Estimated Incidence | Etiology and Risk Factors | Prevention and Salvage Strategies |
|---|---|---|---|
| Ulnar Nerve Injury | 2% - 5% | Medial portal placement, posteromedial retractor use, thermal injury | Maintain trocar on anterior humerus. Consider prophylactic open decompression if severe medial osteophytes exist. Observe for neuropraxia; explore if complete transection suspected. |
| Radial Nerve Injury | 1% - 3% | Anterolateral portal placement, aggressive lateral capsulectomy | Distend joint prior to portal placement. Use blunt dissection. Stay posterior to the radiocapitellar joint line when working laterally. |
| Heterotopic Ossification | 3% - 7% | Aggressive bony resection, capsular tearing, prior trauma | Meticulous lavage of bone debris. Postoperative prophylaxis with Indomethacin or single-dose radiation in high-risk patients. |
| Recurrent Stiffness | 10% - 15% | Inadequate osteophyte resection, poor rehabilitation compliance | Ensure complete clearance of fossae intraoperatively. Aggressive early CPM and static progressive splinting. Revision arthroscopy if mechanical block persists. |
| Infection | < 1% | Standard surgical risk, prolonged operative time | Strict sterile technique. Preoperative antibiotics. Treat with aggressive arthroscopic irrigation and targeted antibiotics if septic arthritis develops. |
Post Operative Rehabilitation Protocols
The success of arthroscopic elbow débridement is heavily dependent on a rigorous and immediate postoperative rehabilitation protocol. The primary goal of rehabilitation is to maintain the range of motion gained intraoperatively and prevent recurrent capsular contracture.

Immediate Post Operative Phase (Days 0 to 7)
Rehabilitation begins in the recovery room. The elbow is typically placed in a bulky soft dressing to minimize hemarthrosis, but rigid immobilization is strictly avoided. Continuous Passive Motion (CPM) machines are frequently utilized immediately postoperative, running continuously while the patient is resting.
If the primary preoperative deficit was a lack of extension, the patient may be fitted with a static progressive extension splint to be worn at night. Conversely, if flexion was the primary deficit, a flexion splint is utilized. Cryotherapy is applied aggressively to manage edema and pain.
Early Active Motion Phase (Weeks 1 to 4)
Active and active-assisted range of motion exercises are initiated within the first 48 hours. Patients are instructed to perform frequent, short bouts of stretching throughout the day. Supervised physical therapy focuses on terminal stretching and mobilization of the radiocapitellar and ulnohumeral joints. Strengthening exercises are generally delayed during this phase to prevent exacerbation of joint inflammation.
Strengthening and Return to Function (Weeks 4 to 12)
Once full, pain-free range of motion is achieved, progressive isometric and isotonic strengthening of the biceps, triceps, and forearm musculature is initiated. Manual laborers and athletes begin work-specific or sport-specific conditioning around 6 to 8 weeks postoperative. Maximum medical improvement following arthroscopic osteocapsular arthroplasty may take up to 6 months, as the joint capsule continues to remodel.
Summary of Key Literature and Guidelines
The academic literature strongly supports the efficacy of arthroscopic débridement for primary degenerative joint disease of the elbow. Foundational studies by Morrey and O'Driscoll established the principles of osteocapsular arthroplasty, demonstrating that resection of impinging osteophytes and release of the contracted capsule reliably restores a functional arc of motion.
Subsequent large-scale arthroscopic series by Savoie, Kelly, and Redfern have validated the minimally invasive approach. These studies consistently demonstrate an average improvement in the arc of motion of 20 to 30 degrees, with the most significant gains observed in terminal extension. Patient satisfaction rates regarding pain relief routinely exceed 85%, particularly in patients whose primary preoperative complaint was impingement pain at the extremes of motion.
Current clinical guidelines recommend arthroscopic débridement as the surgical treatment of choice for young, active patients and manual laborers with primary elbow osteoarthritis who have failed conservative management. While the procedure does not reverse the underlying cartilaginous degeneration, it provides a highly durable result, allowing patients to return to high-demand activities without the catastrophic risks associated with total elbow arthroplasty in this demographic. Future reconstructive options are fully preserved, making arthroscopic débridement an invaluable tool in the orthopedic surgeon's armamentarium for managing the arthritic elbow.
Clinical & Radiographic Imaging











You Might Also Like