Mysterious Fingertip Pain: Orthopedic Diagnosis, Etiology & Management
Key Takeaway
Mysterious fingertip pain stems from elusive etiologies like glomus tumors, digital neuromas, and subtle bone anomalies such as osteoid osteomas. Diagnosis requires a high index of suspicion, meticulous clinical examination, advanced imaging, and a deep understanding of digital surgical anatomy to identify these often overlooked conditions and guide precise management.
Introduction and Epidemiology
"Mysterious fingertip pain" in the orthopedic surgical lexicon refers to persistent, often severe, digital pain where the etiology is not immediately apparent through routine clinical examination or basic imaging. These enigmatic presentations demand a high index of suspicion, meticulous diagnostic workup, and a nuanced understanding of digital pathology. While myriad conditions can cause fingertip pain, those leading to a "mysterious" presentation often involve subtle soft tissue lesions, nerve pathology, or bone anomalies that are easily overlooked. Key conditions frequently presenting in this manner include glomus tumors, digital neuromas, specific nerve entrapments, osteoid osteomas of the phalanx, and early presentations of avascular necrosis or complex regional pain syndrome (CRPS).
Glomus tumors are perhaps the quintessential example of "mysterious" fingertip pain. These benign, highly vascularized tumors originate from modified smooth muscle cells of the glomus body, a specialized neuromyoarterial apparatus involved in thermoregulation. Their prevalence is estimated at 1 to 5 percent of all hand tumors, with a predilection for the subungual region (75 percent), though they can occur in the pulp or periungual areas. They are more common in women, typically affecting individuals between 30 and 50 years of age. Misdiagnosis or delayed diagnosis is common, with an average diagnostic delay of 5 to 7 years, underscoring their "mysterious" nature. The classic clinical triad of severe, paroxysmal pain, cold intolerance, and pinpoint tenderness (Love's test) is often present but may be subtle, particularly in smaller lesions.
Digital neuromas typically arise following trauma or surgery that results in transection or injury to a digital nerve. The regenerating nerve fibers become entrapped within scar tissue, forming a disorganized mass. While post-traumatic neuromas are often linked to a specific injury, spontaneous or less obvious traumatic etiologies can lead to chronic, localized pain that is difficult to ascertain, especially when the neuroma itself is impalpable. The incidence varies significantly depending on the initial injury, but symptomatic neuromas requiring intervention are a recognized sequela.
Osteoid osteomas, while less common in the phalanges, can present as insidious, nocturnal pain relieved by NSAIDs. Their small size and typical lucent nidus can be overlooked on initial radiographs, contributing to diagnostic delay. The pathophysiology involves the production of prostaglandins (specifically PGE2) by the nidus, leading to profound localized pain and adjacent bony sclerosis.
Other less frequent but "mysterious" causes include vascular malformations, digital artery occlusion, subungual exostoses, epidermoid inclusion cysts, and localized occult infections (such as chronic paronychia or deep space micro-abscesses) that possess an atypical presentation. A comprehensive diagnostic approach is critical to unraveling these complex presentations and guiding appropriate management.
Surgical Anatomy and Biomechanics
A thorough understanding of fingertip surgical anatomy is paramount for accurate diagnosis and successful surgical intervention for mysterious fingertip pain. The distal phalanx, nail unit, pulp space, and neurovascular bundles constitute a highly integrated and sensitive functional unit.
Distal Phalanx and Nail Unit Anatomy
The distal phalanx provides the bony support for the nail unit and the tactile pulp. Its volar surface is concave, providing space for the digital pulp. The dorsal surface supports the nail bed.
The nail unit comprises several critical structures:
* Nail Plate: The hard keratinous structure.
* Nail Matrix (Germinal Matrix): Located proximally beneath the proximal nail fold, responsible for producing the nail plate. Injury here leads to permanent nail plate dystrophy.
* Sterile Matrix (Nail Bed): Extends from the germinal matrix to the hyponychium, contributing to nail plate adherence and smoothness. It is highly vascular and richly innervated.
* Eponychium (Proximal Nail Fold): The skin fold covering the proximal nail matrix.
* Hyponychium: The area beneath the free edge of the nail plate, providing a seal against infection and environmental debris.
The Glomus Apparatus
The normal glomus body is a neuromyoarterial receptor primarily located in the reticular dermis of the digits, heavily concentrated in the subungual region. It functions as an arteriovenous anastomosis functioning in temperature regulation. The structure consists of an afferent arteriole, the Sucquet-Hoyer canal (the functional arteriovenous anastomosis lined by cuboidal glomus cells), an efferent venule, intraglomerular reticulum, and a surrounding capsule. Hyperplasia of the glomus cells within the Sucquet-Hoyer canal results in the formation of a glomus tumor.
Digital Pulp and Fibrous Septa
The volar digital pulp is heavily compartmentalized by dense fibrous septa running from the volar dermis to the periosteum of the distal phalanx. This architectural arrangement stabilizes the skin during pinch and grip but creates closed compartments. Consequently, even microscopic space-occupying lesions (such as a tiny glomus tumor or occult micro-abscess) or minor edema can cause exponential increases in compartmental pressure, resulting in disproportionately severe pain.
Neurovascular Arborization
The proper digital arteries and nerves trifurcate near the distal interphalangeal (DIP) joint. The neural branches supply the nail bed, the digital tip, and the volar pulp. The density of sensory receptors—including Pacinian corpuscles (vibration), Meissner's corpuscles (light touch), and free nerve endings (nociception)—is highest in the fingertip. Any mass effect, scar tissue tethering, or iatrogenic injury in this region will trigger profound nociceptive and neuropathic pain pathways.
Indications and Contraindications
The decision to proceed with operative intervention for mysterious fingertip pain hinges on the exhaustion of non-operative modalities and the definitive identification of a surgical target. In conditions like glomus tumors or osteoid osteomas, surgery is the primary definitive treatment. In neuropathic pain syndromes, surgery is reserved for refractory cases.
| Pathology | Operative Indications | Non Operative Indications | Contraindications to Surgery |
|---|---|---|---|
| Glomus Tumor | Confirmed or highly suspected symptomatic lesion; failure of conservative measures; progressive nail dystrophy. | Incidental asymptomatic finding (rare); patient unfit for surgery. | Active local infection; severe unoptimized CRPS (relative). |
| Digital Neuroma | Refractory pain localized to a specific trigger point; failed desensitization and injections; interference with ADLs. | Early post-traumatic hypersensitivity; diffuse pain without a focal trigger point. | Diffuse neuropathic pain lacking a focal target; active CRPS. |
| Osteoid Osteoma | Intractable nocturnal pain; failure of NSAID therapy; impending cortical breakthrough or joint involvement. | Pain adequately controlled with NSAIDs; lesion in a high-risk anatomic zone where morbidity outweighs benefit. | Inability to localize the nidus radiographically. |
| Occult Infection | Abscess formation; osteomyelitis of the distal phalanx; failure of targeted antibiotic therapy. | Cellulitis without fluctuance; early paronychia responsive to soaks and oral antibiotics. | None if surgical drainage is required to prevent tissue necrosis. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is essential to localize the pathology and minimize iatrogenic damage to the complex structures of the fingertip.
Clinical Diagnostic Testing
For suspected glomus tumors, three classic clinical tests are mandatory:
* Love Pin Test: Exquisite, localized pinpoint tenderness when the precise location is pressed with the tip of a paperclip or Kirschner wire.
* Hildreth Ischemia Test: Relief of the pinpoint pain when a proximal tourniquet is inflated to suprasystolic pressures, inducing transient ischemia. This test is highly specific for glomus tumors.
* Cold Sensitivity Test: Exacerbation of severe pain upon immersion of the affected digit in cold water.
Advanced Imaging Protocols
Standard radiographs are the first line of imaging to rule out bony pathology such as osteoid osteoma (lucent nidus with surrounding sclerosis), subungual exostosis, or bony erosion from a soft tissue mass.
When radiographs are negative, high-resolution Magnetic Resonance Imaging (MRI) is the gold standard. For glomus tumors, a dedicated fingertip protocol using a surface coil is required. Glomus tumors typically appear as well-demarcated masses that are hypointense on T1-weighted imaging, markedly hyperintense on T2-weighted imaging, and exhibit avid, homogeneous enhancement following gadolinium administration. High-resolution ultrasound (HRUS) is an alternative, operator-dependent modality that can identify subungual hypoechoic lesions and map digital neuromas.
Patient Positioning and Anesthesia
- Anesthesia: A digital block using a long-acting local anesthetic (e.g., bupivacaine without epinephrine) is typically sufficient. Regional anesthesia or monitored anesthesia care (MAC) may be utilized based on patient anxiety and surgeon preference.
- Positioning: The patient is placed supine with the operative arm extended on a radiolucent hand table.
- Tourniquet: A digital tourniquet (e.g., a sterile glove finger cut and rolled to the base of the digit) or a forearm tourniquet is essential for a bloodless surgical field. Caution must be exercised to track tourniquet time meticulously to prevent ischemic injury.
- Magnification: Surgical loupes (minimum 2.5x to 3.5x) or an operating microscope are strictly required given the microscopic nature of the pathology and the need for precision in nail bed repair.
Detailed Surgical Approach and Technique
The surgical approach is dictated by the precise anatomic location of the lesion. The most common scenario for mysterious fingertip pain is the subungual glomus tumor, requiring a transungual approach.
Transungual Approach for Subungual Lesions
- Nail Plate Removal: A Freer elevator or fine Iris scissors are used to gently separate the nail plate from the underlying sterile matrix and the overlying eponychial fold. The nail plate is carefully extracted and preserved in sterile saline or dilute betadine, as it will be used as a biologic stent postoperatively.
- Matrix Incision: Under loupe magnification, the sterile matrix is inspected. A bluish discoloration or a focal area of elevation often betrays the tumor's location. A longitudinal incision is made directly over the mass. Transverse incisions are strictly avoided as they disrupt the longitudinal growth pattern of the nail and significantly increase the risk of postoperative split-nail deformity.
- Tumor Excision: The sterile matrix is elevated using fine skin hooks. Glomus tumors are typically encapsulated and gelatinous. Using tenotomy scissors or a fine scalpel (No. 15 or 67 blade), the tumor is meticulously shelled out of its bed. Care must be taken to ensure complete excision, as retained microscopic satellites are the primary cause of recurrence.
- Bony Inspection: The underlying distal phalanx is inspected for erosion. If a bony crater is present, it is gently curetted.
- Matrix Repair: The sterile matrix is meticulously reapproximated using 7-0 or 8-0 absorbable sutures (e.g., chromic gut or polyglactin). Perfect anatomic reduction of the matrix is critical to prevent nail dystrophy.
- Nail Plate Replacement: The native nail plate (or a substitute silicone sheet) is fenestrated to allow for hematoma drainage and placed back under the eponychial fold. It is secured with a single non-absorbable suture placed through the distal lateral nail folds.
Lateral Periungual Approach
For lesions located at the lateral margin of the nail unit, a lateral periungual approach may be utilized to spare the central sterile matrix. An L-shaped incision is made along the lateral nail fold, and the flap is elevated to expose the lateral aspect of the distal phalanx and matrix. Following tumor excision, the flap is anatomically reduced.
Volar Approach for Pulp Lesions
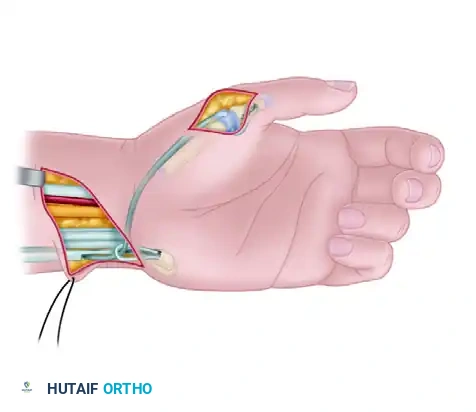
For neuromas or glomus tumors located in the volar pulp, a mid-lateral incision or a volar Bruner (zigzag) incision is utilized. Direct longitudinal incisions over the tactile surface of the volar pad are contraindicated due to the risk of painful scar formation in the primary pinch zone. The fibrous septa are carefully divided to expose the lesion.
Neuroma Resection and Nerve Management
When addressing a painful digital neuroma, the scarred nerve end must be identified and resected back to healthy fascicles. Management of the proximal stump remains controversial and highly variable. Options include:
* Traction Neurectomy: Allowing the nerve to retract into proximal healthy tissue.
* Intramuscular or Intraosseous Burial: Transposing the nerve end into the proximal phalanx or a local intrinsic muscle to shield it from mechanical stimulation.
* Nerve Capping or Wrapping: Utilizing synthetic conduits or vein grafts.
* Targeted Muscle Reinnervation: Emerging techniques involving the transfer of the distal nerve stump to a local motor branch, though less commonly applicable in the distal digit.
Complications and Management
Surgical intervention in the fingertip carries specific risks, primarily related to the delicate anatomy of the nail unit and the dense sensory innervation of the digit.
| Complication | Incidence | Etiology | Management and Salvage Strategy |
|---|---|---|---|
| Nail Dystrophy | 10 to 20 percent | Iatrogenic injury to the germinal matrix; non-anatomic repair of the sterile matrix; transverse matrix incisions. | Prevention is paramount. Established deformity may require secondary nail bed reconstruction using split-thickness sterile matrix grafts from the toes. |
| Tumor Recurrence | 5 to 15 percent | Incomplete excision; presence of unrecognized satellite lesions (multiple glomus tumors occur in 10 percent of cases). | Re-evaluation with contrast-enhanced MRI. Revision excision utilizing wider margins or an operating microscope. |
| Neuroma Stump Pain | 20 to 30 percent | Inadequate resection of the primary neuroma; failure of the chosen stump management technique; mechanical tethering. | Multimodal pain management; desensitization therapy; revision neurectomy with intraosseous burial or capping. |
| Complex Regional Pain Syndrome | 2 to 5 percent | Exaggerated neuroinflammatory response to surgical trauma; inadequate postoperative pain control. | Early recognition. Aggressive physical therapy, stellate ganglion blocks, gabapentinoids, and high-dose Vitamin C. |
| Infection | Less than 2 percent | Contamination of the subungual hematoma or pulp space. | Removal of the stenting nail plate; operative drainage; culture-directed oral or intravenous antibiotics. |
Post Operative Rehabilitation Protocols
Postoperative management is designed to protect the surgical repair while facilitating early mobilization to prevent stiffness and hypersensitivity.
Phase One Early Protection
During the first 10 to 14 days, the digit is protected in a bulky, non-compressive dressing. A dorsal or volar aluminum splint may be applied to protect the DIP joint, depending on the extent of the dissection. The patient is instructed to keep the hand strictly elevated above heart level to minimize throbbing pain and edema. Oral analgesics are utilized, and patients are counseled on the expected timeline of pain resolution.
Phase Two Suture Removal and Desensitization
At the two-week mark, non-absorbable sutures securing the nail plate are removed. The stenting nail plate is left in situ until it is pushed out by the new, growing nail (typically over 3 to 6 months). Gentle, active range of motion (ROM) of the DIP, PIP, and MCP joints is initiated. A formal desensitization program is critical at this stage, involving tactile stimulation with varying textures, fluidotherapy, and gentle massage to normalize sensory input and prevent hypersensitivity.
Phase Three Strengthening and Return to Function
By 4 to 6 weeks, provided wound healing is complete, progressive strengthening is introduced. Patients may return to full occupational and athletic activities as tolerated. For patients who underwent neuroma resection, ongoing monitoring for recurrent trigger points is necessary.
Summary of Key Literature and Guidelines
The academic understanding of mysterious fingertip pain is anchored in several landmark studies and evolving imaging guidelines.
The classic description and surgical management principles of glomus tumors were heavily influenced by the work of Carroll and Berman (1972), who emphasized the necessity of complete excision and the utility of the transungual approach to minimize recurrence. Their foundational work established that microscopic satellite lesions are the primary driver of the historically high recurrence rates.
Diagnostic clinical testing relies heavily on the triad described by Love (1944), who introduced the pin test, and Hildreth (1970), who described the ischemia test. Modern literature confirms that Hildreth's test carries a specificity approaching 100 percent for glomus tumors, making it an indispensable tool in the orthopedic surgeon's clinical armamentarium.
Regarding imaging, contemporary guidelines emphasize the superiority of MRI. Studies by Al-Qattan et al. have demonstrated that high-resolution MRI with gadolinium enhancement yields a sensitivity of over 90 percent for identifying subungual glomus tumors, significantly outperforming ultrasound in differentiating glomus tumors from mucoid cysts, neuromas, and hemangiomas.
For digital neuromas, the literature remains heterogeneous regarding the optimal surgical technique. A systematic review by Eberlin et al. highlights that while no single technique for neuroma management (burial, capping, or simple excision) is universally superior, the prevention of mechanical tethering of the nerve stump is the most critical factor in mitigating postoperative pain.
Ultimately, the successful management of mysterious fingertip pain requires a synthesis of classic clinical acumen, targeted advanced imaging, and meticulous microsurgical technique.
