Acromioclavicular Joint Dislocations: Comprehensive Evaluation and Surgical Management
Key Takeaway
Acromioclavicular (AC) joint dislocations require meticulous clinical and radiographic evaluation to determine the optimal treatment strategy. While low-grade injuries are managed conservatively, high-grade dislocations in active patients necessitate surgical intervention. Modern operative management favors anatomic reconstruction of the coracoclavicular ligaments using autograft and suture tape augmentation, ensuring biomechanical stability and mitigating the risks of hardware migration associated with historical fixation methods.
INTRODUCTION AND BIOMECHANICS
Acromioclavicular (AC) joint dislocations represent a common orthopedic injury, frequently sustained during contact sports or high-velocity trauma following a direct blow to the superior aspect of the acromion with the arm adducted. The stability of the AC joint relies on a complex interplay of static and dynamic stabilizers. The acromioclavicular ligaments provide primary restraint to anterior-posterior translation, while the robust coracoclavicular (CC) ligaments—comprising the conoid and trapezoid—are the primary stabilizers against superior-inferior translation.
The conoid ligament, situated posteromedially, primarily resists superior translation of the clavicle. The trapezoid ligament, located anterolaterally, resists axial compression. Disruption of these structures leads to predictable patterns of instability, necessitating a thorough clinical and radiographic evaluation to guide management.
CLINICAL FINDINGS AND EVALUATION
The clinical presentation of an AC joint injury is typically characterized by localized pain, focal swelling, and an observable deformity over the superior shoulder.
Physical Examination
Patients often present supporting the injured arm in an adducted position to relieve tension on the AC joint. Palpation reveals point tenderness directly over the articulation. In higher-grade injuries, a gross step-off is palpable and visible, representing the superiorly displaced distal clavicle relative to the acromion.
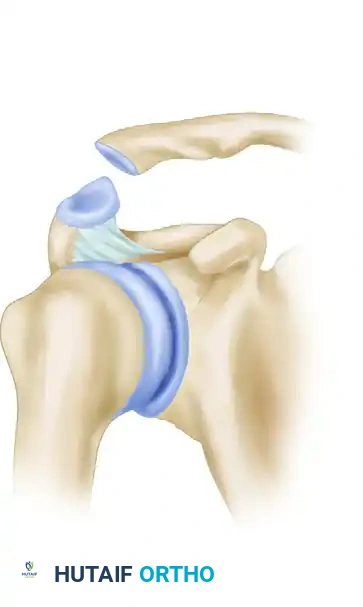
Figure 1: Clinical presentation of an acromioclavicular dislocation demonstrating a visible step-off deformity without the application of traction weights.
The distal clavicle is often highly mobile; it can be ballotted inferiorly (the "piano key" sign), though it will immediately spring back to its superiorly displaced position once pressure is released.
Clinical Pearl: Always assess the sternoclavicular joint and the entire clavicular shaft to rule out concomitant fractures or bipolar clavicle injuries, which drastically alter the surgical algorithm.
Radiographic Assessment
Standard radiographic evaluation must include an anteroposterior (AP) view of the shoulder, an axillary lateral view, and a Zanca view (AP view with a 10° to 15° cephalad tilt) to accurately profile the AC joint without superimposition of the scapular spine.
If the acromioclavicular ligament is torn but the coracoclavicular ligaments remain intact (Grade II injury), anteroposterior instability is the predominant finding. On the AP projection, widening of the AC joint is noted, but vertical displacement is minimal.
To detect further instability and differentiate between subtle grades of injury, stress radiography is highly valuable. This is achieved by suspending 10 to 15 lb (4.5 to 6.8 kg) of weight from both of the patient’s wrists.
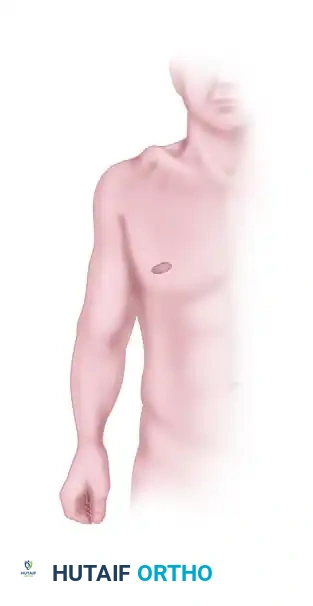
Figure 2: Stress view of the acromioclavicular joint. Weights are suspended from the wrist to unmask latent coracoclavicular instability.
Surgical Warning: Weights must be tied or strapped to the patient's wrists rather than held in the hands. Having the patient actively grip the weights causes reflex contraction of the biceps, deltoid, and rotator cuff musculature, which can artificially reduce the AC joint and mask the true degree of instability.
With the patient standing erect, bilateral AP radiographs are obtained simultaneously for comparison.
* Subluxations: The lateral end of the clavicle is displaced superiorly (or the scapula and arm are displaced inferiorly) by less than or equal to one-half the thickness of the clavicle.
* Dislocations: The distal clavicle is displaced by a distance equal to or greater than its entire thickness.
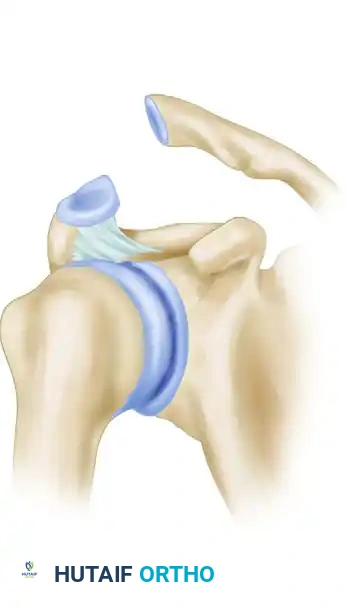
Figure 3: Pathoanatomy of a moderate acromioclavicular dislocation, illustrating disruption of the AC capsule with partial or complete CC ligament involvement.
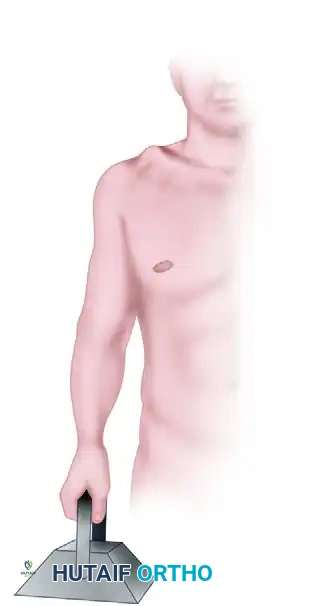
Figure 4: Severe acromioclavicular dislocation demonstrating complete rupture of both the acromioclavicular and coracoclavicular ligamentous complexes, resulting in gross superior displacement of the clavicle.
NON-SURGICAL MANAGEMENT
Type I and Type II injuries (and select Type III injuries in low-demand patients) are satisfactorily treated non-surgically.
Conservative Protocol
- Acute Phase: Application of ice, use of mild analgesics (NSAIDs), and immobilization with a sling for comfort.
- Rehabilitation Phase: Early range-of-motion (ROM) exercises are initiated as soon as pain permits, typically within 7 to 14 days, to prevent adhesive capsulitis.
Advantages and Disadvantages of Closed Treatment
The primary advantage of closed management is the avoidance of surgical morbidity. When successful, closed techniques yield a stable joint and satisfactory shoulder function. However, non-surgical management is not without significant drawbacks.
Disadvantages of Non-Surgical Treatment:
* Skin pressure and potential ulceration from aggressive strapping or bracing techniques (historically used Kenny-Howard splints).
* Recurrence or persistence of the cosmetic deformity.
* The necessity of wearing a sling or brace for up to 8 weeks in some protocols.
* Poor patient compliance due to discomfort.
* Interference with activities of daily living (ADLs).
* Loss of shoulder and elbow motion, particularly in older patients.
* Soft tissue calcification (CC ligament ossification).
* Late acromioclavicular osteoarthritis.
* Late muscle atrophy, weakness, and fatigue of the shoulder girdle.
To mitigate these complications, close clinical observation on a regular basis is necessary, and complete patient cooperation is essential.
OPERATIVE MANAGEMENT
Surgical intervention is generally reserved for high-grade dislocations (Types IV, V, and VI) and acute Type III injuries in young, active patients, manual laborers, or overhead athletes. Most procedures that reduce and fix the AC joint should be reserved for patients younger than 45 years old.
DePalma’s anatomical dissections demonstrated that early degenerative changes develop in the AC joint by the third decade of life, with significant arthrosis present by the fourth decade. Therefore, in older patients with painful, chronic AC dislocations and pre-existing degenerative changes, distal clavicle excision (Mumford procedure) is strongly recommended as an adjunct or standalone procedure.
Core Requirements of AC Joint Surgery
Regardless of the specific technique employed, any surgical procedure for AC dislocation must fulfill three fundamental requirements:
1. Exposure and Débridement: The AC joint must be adequately exposed, and the interposed meniscus or degenerative disc material must be débrided.
2. Ligamentous Restoration: The coracoclavicular and acromioclavicular ligaments must be repaired or anatomically reconstructed.
3. Stable Reduction: A rigid, stable reduction of the AC joint must be obtained and maintained during biological healing.
Historical and Alternative Surgical Options
Historically, numerous procedures have been devised, broadly divided into five categories:
1. AC Reduction and Fixation: Transarticular wire fixation (smooth or threaded Kirschner wires). Note: This is largely abandoned due to the high risk of catastrophic hardware migration into the thoracic cavity.
2. AC Reduction + CC Fixation: Utilizing heavy non-absorbable sutures, metallic/bioabsorbable anchors, or screws (Bosworth screw) between the clavicle and coracoid.
3. Combined AC and CC Fixation.
4. Distal Clavicle Excision: Often combined with ligament reconstruction.
5. Dynamic Muscle Transfers: The Dewar and Barrington procedure involves transferring the coracoid process (with the attached conjoint tendon) to the clavicle to dynamically hold the lateral end of the bone in position.
Pitfall: Coracoclavicular fixation devices depend entirely on an intact coracoid process. Preoperative advanced imaging (CT scan) may be warranted if a concomitant coracoid base fracture is suspected, as this contraindicates standard CC suspension techniques.
PREFERRED SURGICAL TECHNIQUE: ANATOMIC RECONSTRUCTION (MAZZOCCA ET AL.)
Our preferred method for treating high-grade, acute, and chronic AC joint dislocations is the anatomic reconstruction technique described by Mazzocca et al. This procedure reconstructs both the conoid and trapezoid ligaments independently, restoring the native biomechanics of the shoulder girdle.
This technique alleviates concerns over hardware migration, the inadequacy of native AC ligaments for primary repair, and non-anatomic positioning. Biomechanical studies have definitively demonstrated that this anatomic reconstruction provides superior fixation strength and stiffness compared to traditional pin fixation or modified Weaver-Dunn procedures.
Indications
- Acute Grade IV, V, VI dislocations.
- Acute Grade III dislocations in high-demand patients.
- Chronic, symptomatic AC joint instability.
- Unstable distal third clavicle fractures (Neer Type II), utilizing appropriate drill holes.
Preoperative Preparation and Positioning
- The patient is placed in the beach-chair position with the head secured.
- The operative arm is draped free to allow full manipulation. A pneumatic arm positioner may be utilized.
- Ensure the C-arm fluoroscopy unit can easily access the shoulder in both AP and axillary planes.
Step-by-Step Surgical Approach
1. Incision and Exposure
Make a curvilinear incision starting 3.5 cm medial to the distal clavicle, following the lines of Langer, extending distally to the tip of the coracoid process.
Dissect through the subcutaneous tissue to expose the deltopectoral fascia. Develop the deltopectoral interval, retracting the cephalic vein laterally with the deltoid.
2. Coracoid Preparation
Identify the coracoid process. Carefully release the coracoacromial (CA) ligament if necessary for exposure, though preserving it is preferred if possible. Expose the base of the coracoid, ensuring clear visualization of the medial and lateral borders to facilitate safe passage of the graft and sutures.
3. Distal Clavicle Resection
Distal clavicular resection (approximately 8 to 10 mm) is performed routinely to correct altered AC joint biomechanics and prevent late postoperative impingement or arthrosis. Use an oscillating saw to make a perpendicular cut. Débride the AC joint of any remaining meniscal tissue.
4. Graft Preparation
An autologous semitendinosus graft is harvested from the ipsilateral knee. The graft is whipstitched at both ends using high-strength non-absorbable sutures. The reconstruction is preferably augmented with a synthetic suture tape to provide immediate mechanical stability while the biological graft incorporates.
5. Clavicular Tunnel Drilling
Two tunnels are drilled in the distal clavicle to anatomically mimic the insertions of the conoid and trapezoid ligaments:
* Conoid Tunnel: Drilled approximately 4.5 cm medial to the distal end of the clavicle, positioned slightly posterior to the midline of the clavicular axis.
* Trapezoid Tunnel: Drilled approximately 2.5 cm medial to the distal end of the clavicle, positioned slightly anterior to the midline.
6. Graft Passage and Fixation
Pass a suture shuttle under the base of the coracoid from medial to lateral. Use this to shuttle the semitendinosus graft and the augmenting suture tape beneath the coracoid.
* The medial limb of the graft (conoid) is passed superiorly through the medial clavicular tunnel.
* The lateral limb of the graft (trapezoid) is passed superiorly through the lateral clavicular tunnel.
Reduce the AC joint anatomically. This is often facilitated by an assistant applying an upward force on the elbow while applying a downward force on the clavicle. Once anatomic reduction is confirmed fluoroscopically, the suture tape is tied securely over the bony bridge between the two tunnels (or secured with cortical buttons). The semitendinosus graft limbs are then sutured to each other and to the surrounding periosteum to complete the biological fixation.
7. Closure
Meticulously repair the deltotrapezial fascia over the clavicle. This is a critical step to prevent hardware prominence and provide an additional layer of dynamic stability. Close the subcutaneous tissue and skin in a standard layered fashion.
POSTOPERATIVE REHABILITATION PROTOCOL
Successful outcomes depend heavily on strict adherence to postoperative rehabilitation.
- Weeks 0-6: The patient is immobilized in a sling. Only passive range of motion (PROM) is permitted. Forward flexion and abduction are strictly limited to 90° to prevent excessive stress on the healing graft. No active internal rotation or cross-body adduction.
- Weeks 6-12: The sling is discontinued. Active-assisted and active range of motion (AROM) are initiated. Scapular stabilization exercises are emphasized.
- Weeks 12-16: Progressive strengthening begins. Isotonic exercises for the deltoid, rotator cuff, and periscapular musculature are introduced.
- Months 4-6: Return to sport-specific activities and heavy manual labor is permitted once full, painless ROM and symmetric strength are achieved.
COMPLICATIONS OF SURGICAL MANAGEMENT
While surgical intervention provides superior biomechanical restoration, the surgeon must be acutely aware of potential complications. Difficulties and problems associated with surgical methods include:
- Infection: Superficial or deep surgical site infections.
- Anesthetic Risk: Standard risks associated with general anesthesia and interscalene blocks.
- Hematoma Formation: Due to the highly vascular nature of the deltopectoral interval.
- Scar Formation: Hypertrophic scarring, particularly with incisions violating Langer's lines.
- Recurrence of Deformity: Due to graft stretching, suture failure, or non-compliance with the postoperative sling.
- Hardware Complications: Metal breakage, migration (especially with historical K-wires), and loosening.
- Suture Failure: Breakage or loosening of fixation sutures.
- Clavicular Complications: Erosion or iatrogenic fracture of the distal clavicle through the drill holes (stress risers).
- Postoperative Stiffness: Pain and limitation of motion, particularly if rehabilitation is delayed.
- Secondary Procedures: Required for the removal of symptomatic hardware.
- Late AC Arthritis: If distal clavicle excision was not performed or if reduction was non-anatomic.
- Soft Tissue Calcification: Heterotopic ossification of the CC ligaments (usually clinically insignificant but radiographically prominent).
Surgical treatment permits direct inspection of the injury, removal of fracture fragments or interposed tissue obstructing reduction, and anatomical restoration. When executed meticulously, modern anatomic reconstruction techniques allow for the resumption of shoulder motion earlier and with greater long-term stability than is possible with closed techniques or historical non-anatomic operations.
📚 Medical References
- s: comparative results following operative treatment with and without primary distal clavisectomy, Am J Sports Med 5:258, 1977.
- Brucker PU, Gruen GS, Kaufmann RA: Scapulothoracic dissociation: evaluation and management, Injury 36:1147, 2005.
- Buckerfi eld CT, Castle ME: Acute traumatic retrosternal dislocation of the clavicle, J Bone Joint Surg 66A:379, 1984.
- Bundens WD, Cook JI: Repair of acromioclavicular separations by deltoid-trapezius imbrication, Clin Orthop 20:109, 1961.
- Cook FF, Tibone JE: The Mumford procedure in athletes: an objective analysis of function, Am J Sports Med 16:97, 1988.
- Copeland S, Kessel L: Disruption of the acromioclavicular joint: surgical anatomy and biological reconstruction, Injury 11:208, 1980.
- Darrow JC Jr, Smith JA, Lockwood RC: A new conservative method for treatment of type III acromioclavicular separations, Orthop Clin North Am 11:727, 1980.
- DePalma AF: Surgical anatomy of acromioclavicular and sternoclavicular joints, Surg Clin North Am 43:1541, 1963.
- Dewar FP, Barrington TW: The treatment of chronic acromioclavicular dislocation, J Bone Joint Surg 47B:32, 1965.
- Dias JJ, Steingold RF, Richardson RA, et al: The conservative treatment of acromioclavicular dislocation: review after fi ve years, J Bone Joint Surg 69B:719, 1987.
- Dumontier C, Sautet A, Man M, et al: Acromioclavicular dislocations: treatment by coracoacromial ligamentoplasty, J Shoulder Elbow Surg 4:130, 1995.
- Ejeskär A: Coracoclavicular wiring for acromioclavicular joint dislocation: a ten-year follow-up study, Acta Orthop Scand 45:652, 1974.
- Eskola A, Vainionpää S, Korkala S, et al: Four-year outcome of operative treatment of acute acromioclavicular dislocation, J Orthop Trauma 5:9, 1991.
- Féry A, Sommelet J: Dislocation of the sternoclavicular joint: a review of 49 cases, Int Orthop 12:187, 1988.
- Fukuda K, Craig EV, An KN, et al: Biomechanical study of the ligamentous system of the acromioclavicular joint, J Bone Joint Surg 68A:434, 1986.
- Galpin RD, Hawkins RJ, Grainger RW: A comparative analysis of operative versus nonoperative treatment of grade III acromioclavicular separations, Clin Orthop Relat Res 193:150, 1985.
- Gerber C, Rockwood CA Jr: Subcoracoid dislocation of the lateral end of the clavicle: a report of 3 cases, J Bone Joint Surg 69A:924, 1987.
- Gillespie HS: Excision of the outer end of the clavicle for dislocation of the acromioclavicular joint, Can J Surg 7:18, 1964.
- Gurd FB: The treatment of complete dislocation of the outer end of the clavicle, Ann Surg 113:1094, 1941.
- Guttmann D, Paksima NE, Zukerman JD: Complications of treatment of complete acromioclavicular joint dislocation, Instr Course Lect 49:407, 2000.
- Heinig CF: Retrosternal dislocation of the clavicle: early recognition, x-ray diagnosis, and management, J Bone Joint Surg 50A:830, 1968.
- Hobbs DW: Sternoclavicular joint: a new axial radiographic view, Radiology 90:801, 1968.
- Horn JS: The traumatic anatomy and treatment of acute acromioclavicular dislocation, J Bone Joint Surg 36B:194, 1954.
- Jacobs B, Wade PA: Acromioclavicular-joint injury: an end-result study, J Bone Joint Surg 48A:475, 1966.
- Jalovaara P, Päivänsalo M, Myllylä V, et al: Acute acromioclavicular dislocations treated by fi xation of the joint and ligament repair or reconstruction, Acta Orthop Belg 57:296, 1991.
- Jay GR, Monnet JC: The Bosworth screw in
You Might Also Like
