00:00
Start Quiz
Question 76
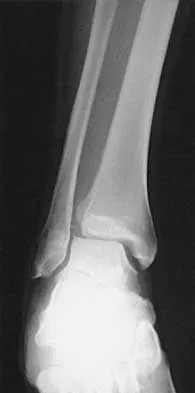
A 47-year-old man ruptured his left patellar tendon and twisted his right ankle in a fall. Initial radiographs of the ankle are unremarkable. One week following repair of the left patellar tendon, he reports increased pain with weight bearing in his right ankle. A follow-up radiograph is shown in Figure 38. Management of the ankle injury should consist of
Explanation
The radiograph reveals disruption of the syndesmosis with lateral displacement of the talus and widening of the medial ankle clear space. No fibular fracture is noted, although radiographs of the entire tibia and fibula are necessary to rule out a more proximal fibula fracture. There is clear instability of the syndesmosis, and surgical stabilization is needed, either by direct repair of the ligaments or more commonly with surgical stabilization of the fibula to the tibia with screws. Functional rehabilitation and early range of motion are indicated with anterior-lateral ankle sprains but not with true instability of the syndesmosis. In anterior syndesmotic injuries in which there are no signs of instability on plain radiographs or with stressing, cast immobilization and protected weight bearing until tenderness subsides is warranted. Long leg cast immobilization is unlikely to be adequate in maintaining reduction of the syndesmosis. Repair of the talofibular ligaments or fibular osteotomy does not address the pathology at the syndesmosis. Chronic syndesmotic disruption is likely to lead to chronic ankle pain and early arthrosis. Wuest TK: Injuries to the distal lower extremity syndesmosis. J Am Acad Orthop Surg 1997;5:172-181.
Question 77
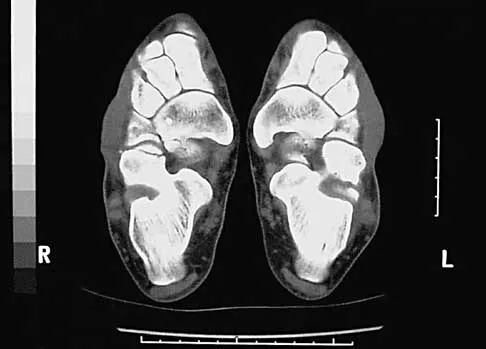
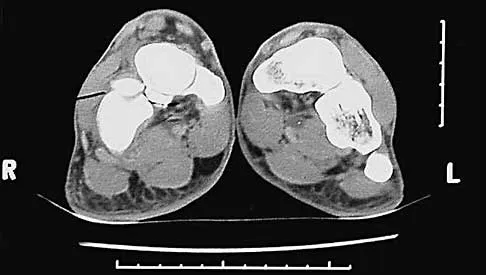
A 45-year-old man reports severe discomfort following a twisting injury to his right ankle and foot. Plain radiographs are negative; however, the CT scans shown in Figures 39a and 39b reveal a fracture. Management should consist of
Explanation
The CT scans show a fracture of the anterior process of the calcaneus that involves less than 25% of the joint surface with minimal to no displacement. The preferred treatment is external immobilization in either a walking cast or, more typically, a removable cast boot. For larger fractures that involve more than 25% of the articular surface with joint incongruity, open reduction and internal fixation may be indicated. Primary calcaneocuboid joint arthrodesis is not warranted because symptoms are rare in most patients. Delayed excision of the fragment is a late reconstructive option if painful nonunion develops. Percutaneous pin fixation is not indicated beceause there tends to be inherent stability in this fracture. Heckman JD: Fractures and dislocations in the foot, in Rockwood CA Jr, Green DP, Bucholz RW, Heckman JD (eds): Rockwood and Green's Fractures in Adults, ed 4. Philadelphia, PA, Lippincott-Raven, 1996, pp 2267-2405.
Question 78
Which of the following complications occurs more commonly after antegrade femoral nail insertion when compared with retrograde insertion?
Explanation
There is no difference between the rates of union, malunion, range of motion of the hip or knee, muscle weakness, or infection for the two types of femoral nail insertion. The only difference is the location of the morbidity, which is around the insertion point of the rod. The antegrade technique has more morbidity about the hip, and the retrograde insertion technique has more morbidity about the knee. Morgan E, Ostrum RF, DiCicco J, McElroy J, Poka A: Effects of retrograde femoral intramedullary nailing on the patellofemoral articulation. J Orthop Trauma 1999;13:13-16. Ricci WM, Bellabarba C, Evanoff B, Herscovici D, DiPasquale T, Sanders R: Retrograde versus antegrade nailing of femoral shaft fractures. J Orthop Trauma 2001;15:161-169. Ostrum RF, Agarwal A, Lakatos R, Poka A: Prospective comparison of retrograde and antegrade femoral intramedullary nailing. J Orthop Trauma 2000;14:496-501.
Question 79
A 24-year-old man has right forearm pain after sliding head first into home plate. Examination reveals that the arm is swollen, but there are no neurovascular deficits or skin lacerations. Radiographs reveal a both-bone forearm fracture. The ulna has an oblique fracture with a 30% butterfly fragment, and the radius is comminuted over 75% of its circumference. In addition to reduction and plate fixation of both bones, management should consist of
Explanation
The patient has a both-bone fracture with a comminuted radial shaft. Open reduction and internal fixation of both bones is the treatment of choice. In the past, Chapman and associates recommended bone grafting radial shaft fractures with more than 30% comminution of the circumference. This has remained the recommendation in most textbooks. More recent studies, where modern biologic plating techniques were used, found that the addition of bone graft to comminuted fractures was not necessary because the union rate did not differ from that of nongrafted comminuted fractures. Anderson LD, Sisk TD, Tooms RE, Park WI III: Compression-plate fixation in acute diaphyseal fractures of the radius and ulna. J Bone Joint Surg Am 1975;57:287-297. Chapman MW, Gordon JE, Zissimos AG: Compression-plate fixation of acute fractures of the diaphyses of the radius and ulna. J Bone Joint Surg Am 1989;71:159-169. Wright RR, Schmeling GJ, Schwab JP: The necessity of acute bone grafting in diaphyseal forearm fractures: A retrospective review. J Orthop Trauma 1997;11:288-294.
Question 80
A 32-year-old woman has an isolated left posterior wall acetabular fracture in which about 25% of the wall surface is involved. Which of the following criteria would indicate the need for surgical reduction and fixation?
Explanation
Fractures with a posterior wall fragment that makes up less than one third of the surface generally are stable. Conversely, fractures with a fragment making up more than 50% of the surface are unstable. Patients with an intermediate fracture fragment should undergo a fluoroscopic examination under sedation or anesthesia to determine if the fragment is truly stable. If so, the patient can be treated nonoperatively and safely mobilized. Tornetta P III: Non-operative management of acetabular fractures: The use of dynamic stress views. J Bone Joint Surg Br 1999;81:67-70.
Question 81
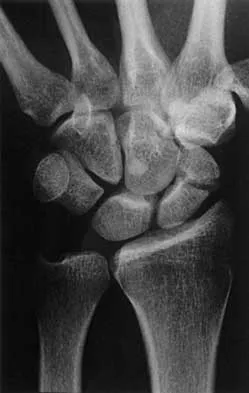
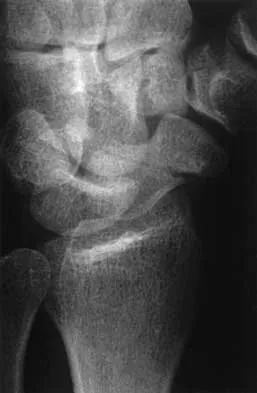
A 25-year-old man reports wrist pain following a motorcycle accident. Examination reveals minimal swelling, slightly limited active range of motion, and point tenderness in the snuff box region. AP and oblique radiographs are shown in Figures 40a and 40b. Management should consist of
Explanation
The radiographs reveal a scaphoid fracture with displacement and comminution and an unstable fracture pattern. Treatment should consist of open reduction and internal fixation. In displaced scaphoid fractures and fractures with unstable fracture patterns, closed reduction is ineffective and is likely to lead to nonunion. Limited intercarpal fusion and proximal row carpectomy are used to correct a variety of traumatic and posttraumatic problems of the wrist. Amadio PC, Taleisnik J: Fractures of the carpal bone, in Green DP, Hotchkiss RN, Pederson WC (eds): Green's Operative Hand Surgery, ed 4. Philadelphia, PA, 1999, pp 809-823. Rettig ME, Kozin SH, Cooney WP: Open reduction and internal fixation of acute displaced scaphoid waist fractures. J Hand Surg Am 2001;26:271-276. Cooney WP, Dobyns JH, Linscheid RL: Fractures of the scaphoid: A rational approach to management. Clin Orthop 1980;149:90-97.
Question 82
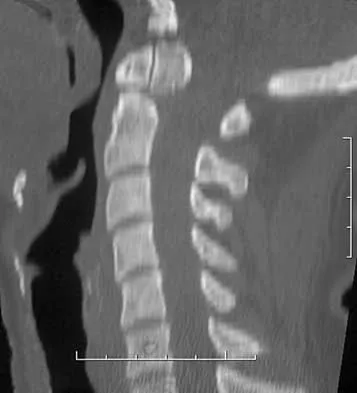
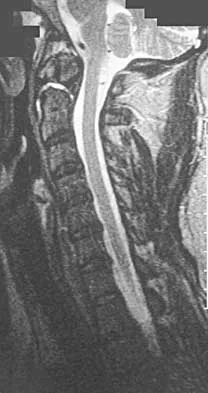
A 42-year-old woman reports that she has low back pain and had a transient loss of consciousness after falling off a horse. She denies having neck pain but notes that she was involved in a motor vehicle accident 2 years ago and had neck pain at that time. Examination reveals full range of motion of the neck and no localized tenderness. The neurologic examination is normal. A lateral radiograph of the cervical spine is obtained. Figures 41a and 41b show CT and MRI scans. What is the most likely diagnosis?
Explanation
The examination findings do not correlate with an acute injury (full range of cervical motion and the absence of pain). Radiographically, the fracture appears old based on the smooth contour of the fracture fragments and the absence of soft-tissue swelling. Flexion-extension radiographs can be obtained to determine potential instability; if present, stabilization and fusion should be considered. Schatzker J, Rorabeck CH, Waddell JP: Non-union of the odontoid process: An experimental investigation. Clin Orthop 1975;108:127-137.
Question 83
What neurologic structure is most at risk when performing intramedullary screw fixation of a fifth metatarsal base fracture?
Explanation
The sural nerve and its terminal branches course through the lateral hindfoot and midfoot area and are directly at risk in surgeries involving the peroneal tendon complex and the fifth metatarsal. The first branch of the lateral plantar nerve originates in the tarsal tunnel region and courses across the plantar heel area to innervate the abductor digiti minimi; it is not at direct risk with fifth metatarsal surgery. The saphenous, superficial peroneal, and deep peroneal nerves are not at risk anatomically with a lateral midfoot incision. Donley BG, McCollum MJ, Murphy GA, Richardson EG: Risk of sural nerve injury with intramedullary screw fixation of fifth metatarsal fractures: A cadaver study. Foot Ankle Int 1999;20:182-184.
Question 84
A 25-year-old man sustained an L1 compression fracture in a fall from his roof. He is neurologically intact and has no other injuries. Radiographs reveal a 25% loss of height anteriorly and 5 degrees of kyphosis at the fracture site. A CT scan reveals no compromise of the posterior column. Management should consist of
Explanation
The patient has a stable fracture that can be initially treated with bed rest, followed by bracing and quick mobilization. The outcome is good and surgery is not required. These fractures can be treated nonsurgically if there is less than 50% compression, 15 degrees of angulation, and intact posterior structures. Cantor JB, Lebwohl NH, Garvey T, Eismont FJ: Nonoperative management of stable thoracolumbar burst fractures with early ambulation and bracing. Spine 1993;18:971-976.
Question 85
A 35-year-old man sustained a 10% compression fracture of the C5 vertebra in a diving accident. Radiographs show good alignment, and examination reveals no neurologic compromise. An MRI scan reveals no significant soft-tissue disruption posteriorly. Management should consist of
Explanation
The patient has a stable flexion-compression injury of the cervical spine. The fracture occurs as a result of compression failure of the vertebral body. If the force continues, a tension failure of the posterior structures occurs, leading to potential dislocation. Immobilization in a rigid cervical orthosis will allow this fracture to heal. Clark CR (ed): The Cervical Spine, ed 3. Philadelphia, PA, Lippincott-Raven, 1998, pp 457-464.
Question 86
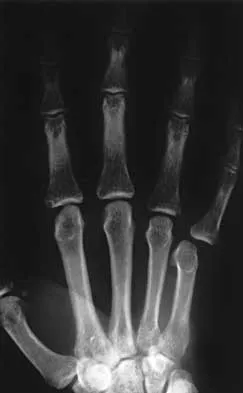
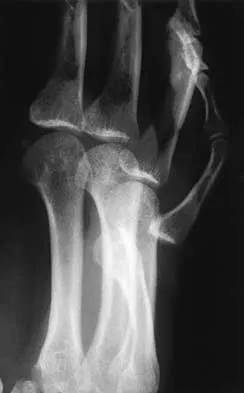
Figures 42a and 42b shows the radiographs of a 20-year-old man who sustained a hyperextension injury to his little finger. Multiple attempts at closed reduction have been unsuccessful. Management should now consist of
Explanation
The radiographs show a complex dislocation of the little finger metacarpophalangeal joint. This is characterized by obvious dislocation on the AP and lateral views and a type of bayonet apposition best visualized on the lateral view. Irreducibility of this injury is caused by displacement of the volar plate that has been traumatically avulsed from its origin on the metacarpal, with subsequent displacement into the metacarpophalangeal joint. This abnormal position of the volar plate causes irreducibility that can be corrected only by open reduction. This can be effected either by dorsal or palmar approaches. Stern PJ: Fractures of the metacarpals and phalanges, in Green DP, Hotchkiss RN, Pederson WC (eds): Green's Operative Hand Surgery, ed 4. Philadelphia, PA, 1999, pp 711-771. Becton JL, Christian JD Jr, Goodwin HN, Jackson JG III: A simplified technique for treating the complex dislocation of the index metacarpophalangeal joint. J Bone Joint Surg Am 1975;57:698-700.
Question 87
A 34-year-old man sustains an extra-articular fracture of the proximal phalanx of his right index finger in a fall. Examination reveals that the fracture is closed and oblique in orientation. Closed reduction and splinting fail to maintain the reduction. Management should now consist of
Explanation
The patient has an unstable oblique fracture of the proximal phalanx that is easily reducible but unstable; therefore, the treatment of choice is closed reduction and percutaneous pin fixation, followed by casting. Closed reduction and percutaneous pin fixation offers a better functional result than open reduction and plate fixation. Repeat closed reduction and buddy taping is inadequate because of the inherently unstable fracture pattern. Buddy taping will allow the dislocation to recur. The other options represent more aggressive surgical techniques than are necessary to treat this fracture. Stern PJ: Fractures of the metacarpals and phalanges, in Green DP, Hotchkiss RN, Pederson WC (eds): Green's Operative Hand Surgery, ed 4. Philadelphia, PA, 1999, pp 711-771.
Question 88
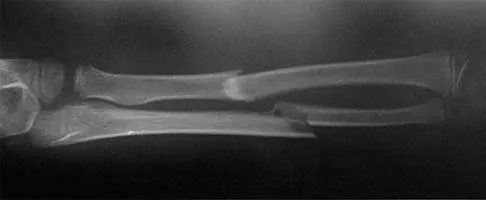
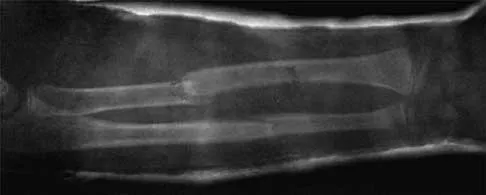
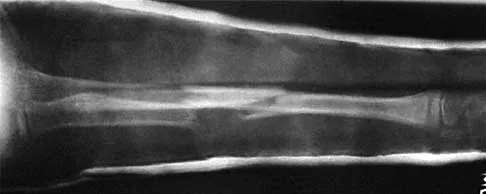
Figures 43a and 43b show the AP and lateral radiographs of the radius and ulna of a 9-year-old patient. The fracture is manipulated and placed in a long arm cast with the elbow flexed to 90 degrees and the forearm to neutral rotation. Figures 43c and 43d show the alignment of the fracture after the manipulation. What is the next most appropriate step in management?

Explanation
By placing the forearm at neutral rotation, as shown in Figures 43c and 43d, the distal fragment has become malrotated by 90 degrees. This is evident by the fact that the bicipital tuberosity is rotated 90 degrees to the radial styloid. Normally, it should be directly opposite (180 degrees) to the radial styloid. The correct alignment was present in the original radiographs shown in Figures 43a and 43b. Another clue to the malrotation in the postreduction radiographs is the difference in the diameters of the opposing radial shafts. To correct this rotational malalignment, the distal fragment needs to be remanipulated into supination so that it is correctly aligned with the supinated proximal radius. Evans EM: Fractures of the radius and ulna. J Bone Joint Surg Br 1951;33:548-561.
Question 89
Which of the following findings is an indication for adjunctive use of high-dose steroids?
Explanation
According to NASCIS III, the high-dose steroid protocol involves infusion of 30 mg/kg methylprednisolone followed by 5.4 mg/kg/h for 24 hours if the patient has sustained a spinal cord injury within the last 3 hours. The drip is continued for 48 hours if administration is started between 3 and 8 hours of the onset of neurologic deficit. No benefit has been conclusively demonstrated with steroids administered beginning 8 hours or longer after injury. Steroid use is not indicated for nerve root deficits, brachial plexus deficits, or gunshot wounds. Kellam JF, Fischer TJ, Tornetta P III, Bosse MJ, Harris MB (eds): Orthopaedic Knowledge Update: Trauma 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 319-328.
Question 90
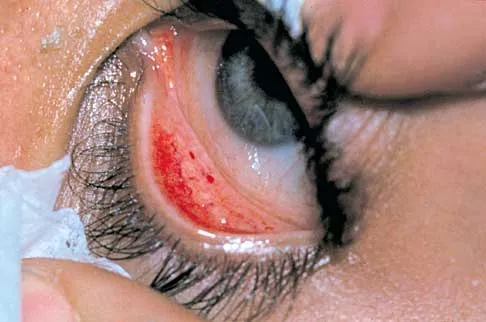
A 22-year-old man sustained a stable pelvic fracture, bilateral femur fractures, and a left closed humeral shaft fracture in a motor vehicle accident. Examination 24 hours after injury reveals that the patient is confused and has shortness of breath. A clinical photograph of his conjunctiva is shown in Figure 44. He has a temperature of 101 degrees F (38.3 degrees C) and a pulse rate of 120/min. Laboratory studies show a hemoglobin level of 8 g/dL, a platelet count of 50,000/mm3, and a PaO2 of 57 mm Hg on 2L of oxygen. What is the most likely diagnosis?
Explanation
The major criteria for the diagnosis of fat embolism syndrome include hypoxemia (PaO2 of less than 60 mm Hg), central nervous system depression, and a petechial rash that is most often located in the axillae, conjunctivae, and palate. The rash is often transient. Tachycardia, pyrexia, anemia, thrombocytopenia, and the presence of fat in the urine are all considered minor criteria. To establish the diagnosis of fat embolism syndrome, one major and four minor signs should be present. Pulmonary embolism, which is the major differential diagnosis, usually is not associated with conjunctival petechia or thrombocytopenia.
Question 91
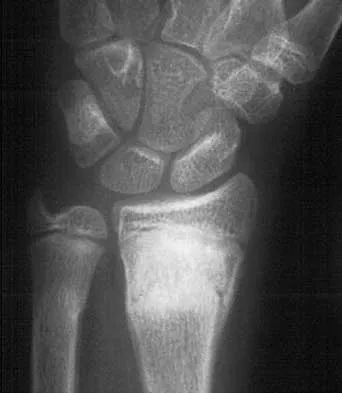
Figure 45 shows the current radiograph of an 11-year-old girl who sustained a simple nondisplaced fracture of the distal radius 4 weeks ago. Management at the time of injury consisted of application of a short arm cast but no manipulation. What is the major concern at this time?
Explanation
The fracture pattern represents a Peterson type I physeal injury, which is a comminuted metaphyseal fracture in which the fracture lines extend up to the physis. Because there is no displacement of the physis and the fracture lines do not cross the physis, there may be a tendency to dismiss this injury as a simple metaphyseal fracture with no significant sequelae. A small percentage of patients (3% in Peterson's series) experience growth arrest. In this patient, a disabling ulnar plus deformity, defined as increased ulnar length in relationship to the distal radius, developed. Peterson HA: Physeal fractures: Part 2. Two previously unclassified types. J Pediatr Orthop 1994;14:431-438.
Question 92
Which of the following is considered the best measure of the adequacy of resuscitation in the first 6 hours after injury?
Explanation
The end point of resuscitation is adequate tissue perfusion and oxygenation. Blood lactate is the end point of anaerobic metabolism. The level of blood lactate reflects global hypoperfusion and is directly proportional to oxygen debt. Two separate prospective studies have verified a significant difference in mortality when blood lactate was used as a measure of resuscitation when compared to traditional parameters (mean arterial pressure, urine output, central venous pressure, and heart rate). Base deficit is a direct measure of metabolic acidosis and an indirect measure of blood lactate levels. It correlates well with organ dysfunction, mortality, and adequacy of resuscitation. It is easy to measure, can be obtained rapidly, and is an excellent assessment of the adequacy of resuscitation. Porter JM, Ivatury RR: In search of the optimal end points of resuscitation in trauma patients: A review. J Trauma 1998;44:908-914.
Question 93
A 26-year-old man sustains a displaced bimalleolar fracture by sliding into second base while playing baseball. Following initial closed reduction and splinting of the fracture, moderate swelling is noted. What is the safest time to perform surgery?
Explanation
Following any closed fracture, the most important determinant for the timing of surgery is the condition of the soft tissues and especially the skin. The best determinant of appropriate soft-tissue condition is the presence of wrinkling of the skin (wrinkle sign) at the site of the incision. A wrinkle sign is present when all the interstitial edema has left the skin; this may take up to 14 to 21 days of elevation. Any abrasion must be epithelialized so that there are no bacteria left at the site. To date, no other method of soft-tissue viability measurement has been shown to be of any clinical benefit. Stover MD, Kellam JF: Articular fractures: Principles, in Ruedi TP, Murphy WM (eds): AO Principles of Fracture Management. Stuttgart, Thieme, 2000, pp 105-119. Hahn DM, Colton CL, Malleolar fractures, in Ruedi TP, Murphy WM (eds): AO Principles of Fracture Management. Stuttgart, Thieme, 2000, pp 559-581.
Question 94
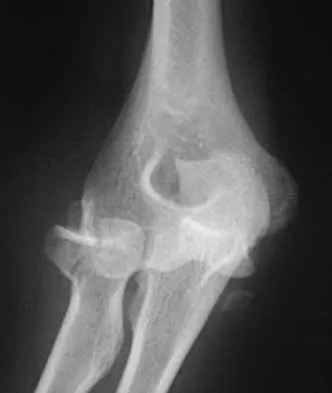
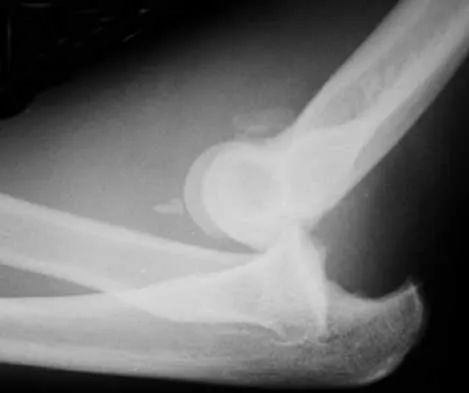
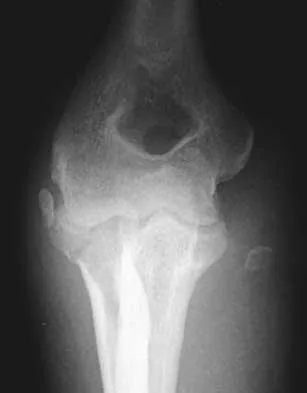
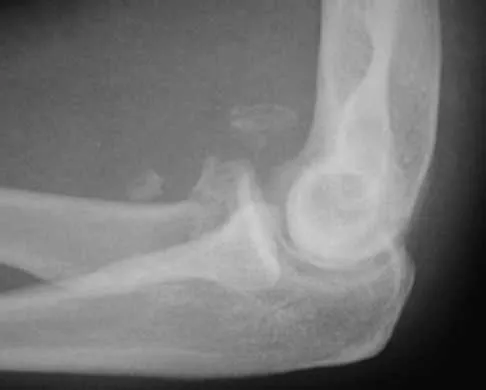
A 28-year-old woman sustained an injury to her dominant right arm after falling off her porch. Examination reveals a deformity at the elbow. She is neurovascularly intact. Figures 46a and 46b show the radiographs obtained before closed reduction, and postreduction radiographs are shown in Figure 46c and 46d. What is the most likely early complication?
Explanation
The patient has a complex fracture-dislocation of the elbow. The radial head is fractured, and there is a displaced coronoid fracture. These associated fractures indicate that the elbow is at high risk for recurrent instability after initial treatment. To prevent this complication, surgical treatment will most likely be required and will consist of some or all of the following: radial head open reduction and internal fixation or replacement, coronoid open reduction and internal fixation, medial and lateral ligament repairs, and even articulated external fixation. This patient was treated with open reduction and internal fixation of the radial head, and the elbow redislocated postoperatively. Ring D, Jupiter JB: Reconstruction of posttraumatic elbow instability. Clin Orthop 2000;370:44-56. O'Driscoll SW: Classification and evaluation of recurrent instability of the elbow. Clin Orthop 2000;370:34-43.
Question 95
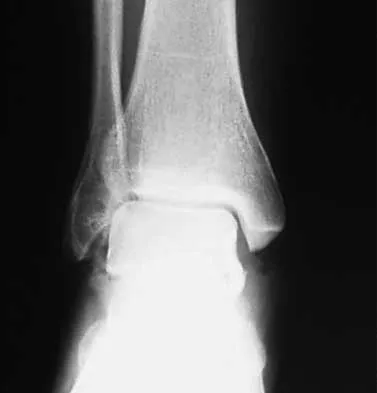
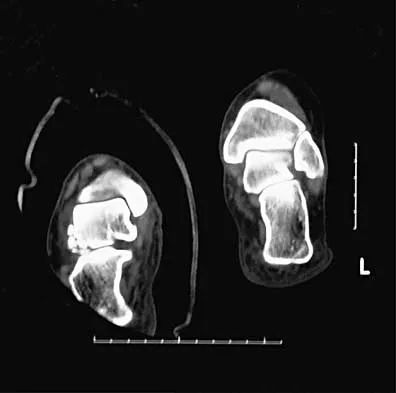
What is the most likely long-term sequela of the injury shown in Figures 47a and 47b?
Explanation
The imaging studies show a comminuted lateral talar process fracture. This injury is often missed on plain radiographs; therefore, CT provides the best method of diagnostic evaluation. The most likely long-term sequela of this injury is subtalar joint arthrosis. Although this injury involves the fibular gutter region, progression to true ankle arthritis is unlikely. There does not appear to be any association with this injury and chronic mechanical instability of the ankle or disruption of the superior peroneal retinaculum and subsequent peroneal tendon instability. Entrapment of the flexor hallucis longus tendon may occur with fractures of the sustentaculum tali but not with injuries of the lateral talar process. Surgical management includes open reduction and internal fixation versus excision; the goal is preservation of the large articular surface fragments. In this patient, there is significant comminution and early fragment excision may be the best option for acute treatment. Tucker DJ, Feder JM, Boylan JP: Fractures of the lateral process of the talus: Two case reports and a comprehensive literature review. Foot Ankle Int 1998;19:641-646.
Question 96
A 16-year-old high school football player has diffuse pain with attempted digital flexion after injuring the ring finger of the dominant hand 1 week ago. Examination reveals that he is unable to flex the distal interphalangeal joint. Management should consist of
Explanation
The patient has an avulsion of the flexor digitorum profundus. Treatment should include surgical exploration and tendon reinsertion. This is not an avulsion of the flexor digitorum superficialis because the patient's deficiency is the inability to flex the distal interphalangeal joint, not the proximal interphalangeal joint. Surgical release of the anterior interosseous nerve is not indicated because the flexor digitorum profundus of the ring finger is innervated by the ulnar nerve. A median nerve contusion causes wrist pain and/or numbness and tingling in the median nerve distribution. Strickland JW: Flexor tendons: Acute injuries, in Green DP, Hotchkiss RN, Pederson WC (eds): Green's Operative Hand Surgery, ed 4. Philadelphia, PA, 1999, pp 1851-1897.
Question 97
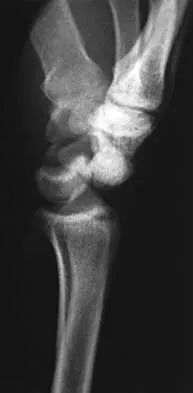
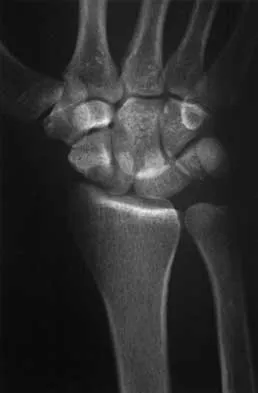
A 25-year-old construction worker lands on his outstretched hand in a fall. The position of his wrist at the time of impact causes a force that leads to hyperextension, ulnar deviation, and intercarpal supination. Radiographs are shown in Figures 48a and 48b. What type of injury pattern is shown?
Explanation
The patient has a transscaphoid dorsal perilunate dislocation. The radiographs clearly define a dorsal dislocation of the capitolunate joint, and the scaphoid fracture component is easily visible on the AP view. A scaphoid fracture alone is an unlikely diagnosis because of the midcarpal dislocation component. The radiocarpal joint is not dislocated because the lunate is sitting in the lunate fossa of the radius. Isolated radiocarpal dislocations are not associated with a midcarpal disruption. While a midcarpal dislocation is a component of a dorsal perilunate dislocation, this diagnosis does not address the scaphoid fracture. A volar lunate dislocation is not seen because the lunate is reduced in the lunate fossa of the distal radius. Volar lunate dislocations are in the spectrum of injury of perilunate dislocations and fracture-dislocations; however, the radiographs show a transscaphoid dorsal perilunate dislocation. Mayfield JK, Johnson RP, Kilcoyne RK: Carpal dislocations: Pathomechanics and progressive perilunar instability. J Hand Surg Am 1980;5:226-241.
Question 98
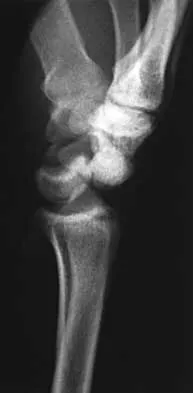
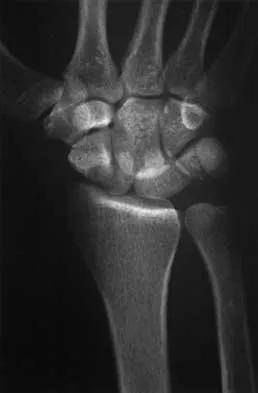
A 25-year-old construction worker lands on his outstretched hand in a fall. The position of his wrist at the time of impact causes a force that leads to hyperextension, ulnar deviation, and intercarpal supination. Radiographs are shown in Figures 48a and 48b. Management should consist of
Explanation
Open reduction and internal fixation is the treatment of choice for accurate reduction of the disrupted intercarpal ligaments. In addition, the displaced scaphoid fracture will require open reduction and internal fixation and possible bone grafting. Closed reduction and long arm casting will not allow accurate reduction of the dislocated intracarpal intervals, and it is unlikely to allow accurate reduction of the scaphoid. The maneuver required to effect closed reduction of a displaced scaphoid fracture will most likely cause the scaphoid lunate interval to displace. Closed reduction with percutaneous pin fixation or with an external fixator is unable to effect anatomic reduction of the injury. Proximal row carpectomy is used as a salvage procedure for a variety of degenerative and posttraumatic problems of the wrist. Kozin SH: Perilunate injuries: Diagnosis and treatment. J Am Acad Orthop Surg 1998;6:114-120. Herzberg G, Comtet JJ, Linscheid RL, Amadio PC, Cooney WP, Stalder J: Perilunate dislocations and fracture-dislocations: A multicenter study. J Hand Surg Am 1993;18:768-779.
Question 99
A 17-year-old boy who fell on a pitchfork in a barn 1 day ago now has a painful, swollen forearm. Examination reveals erythema, exquisite tenderness, and crepitus to palpation of the forearm. He has a pulse rate of 110/min and a blood pressure of 80/60 mm Hg. Radiographs show subcutaneous air and no fractures. Gram stain of wound drainage reveals a gram-positive bacillus. The next most appropriate step in management should consist of
Explanation
The successful treatment of necrotizing soft-tissue infections such as clostridial myonecrosis depends on prompt recognition and aggressive surgical debridement of all involved muscle, fascia, and soft tissue, resecting to a clearly normal healthy, viable margin. The effective antibiotic regimen for clostridial infection is high-dose penicillin; however, necrotizing infections are frequently polymicrobial so initially broad-spectrum antibiotics are indicated. Hyperbaric oxygen therapy may be used as an adjunct to surgical treatment but is insufficient as a primary therapy. Prolonged application of tourniquets and wound closure should be avoided. Pellegrini VD, Evarts CM: Complications, in Rockwood CA Jr, Green DP (eds): Fractures in Adults, ed 3. Philadelphia, PA, JB Lippincott, 1991, pp 365-370. Gerding DN, Peterson LR: Infections caused by anaerobic bacteria, in Shulman ST, Phair JP, Peterson LR, Warren JR (eds): Infectious Diseases, ed 5. Philadelphia, PA, WB Saunders, 1997, pp 416-417.
Question 100
In the management of an open tibia fracture, what factor is considered most important in preventing deep infection?
Explanation
The most important aspect of management of any open fracture, and in particular the tibia, is the degree and the completeness of the debridement of the soft tissue and most importantly, the muscle. The ultimate function is determined by the amount of muscle left, as well as the ability to heal. The amount of necrotic muscle left in the wound also determines the predisposition to infection. The method of fixation, the size of the wound, and the amount of contamination are controlled by the surgeon or the injury and have little to do with the long-term outcome. Initial wound cultures have little predictive value. Clifford P: Open fractures, in Ruedi TP, Murphy WM (eds): AO Principles of Fracture Management. Stuttgart, Thieme, 2000, pp 617-638.
