Operative Management of Upper Extremity Nerve Entrapments: Ulnar Transposition and Median Nerve Decompression
Key Takeaway
This comprehensive surgical guide details the operative management of upper extremity nerve entrapments, focusing on ulnar nerve transposition and median nerve decompression. Designed for orthopedic surgeons and residents, it provides step-by-step techniques, anatomical considerations, and evidence-based diagnostic protocols for pronator teres and anterior interosseous syndromes. Master the nuances of submuscular transfers, neurolysis, and postoperative rehabilitation to optimize patient outcomes in peripheral nerve surgery.
INTRODUCTION TO PERIPHERAL NERVE SURGERY OF THE UPPER EXTREMITY
The operative management of peripheral nerve entrapments and injuries in the upper extremity demands a profound understanding of micro-anatomy, biomechanics, and precise surgical execution. Peripheral nerves are highly sensitive to traction, friction, and ischemic compression. In the upper extremity, the ulnar and median nerves are particularly susceptible to these pathological forces due to their complex anatomical courses through tight fibro-osseous tunnels and dynamic muscle bellies.
This masterclass provides an exhaustive, evidence-based review of the surgical transposition of the ulnar nerve and the comprehensive management of median nerve pathologies, including Pronator Teres Syndrome and Anterior Interosseous Nerve (AIN) Syndrome.
TRANSPOSITION OF THE ULNAR NERVE
Ulnar nerve entrapment at the elbow (cubital tunnel syndrome) is the second most common compression neuropathy of the upper extremity. When conservative measures fail, or in the presence of advanced motor atrophy, surgical intervention is indicated. Anterior transposition of the ulnar nerve—whether subcutaneous, intramuscular, or submuscular—effectively removes the nerve from the retro-epicondylar groove, eliminating traction during elbow flexion and preventing subluxation.
Biomechanics and Pathoanatomy
During normal elbow flexion, the cubital tunnel volume decreases by nearly 55%, while the ulnar nerve undergoes significant longitudinal excursion (up to 10 mm) and increased intraneural tension. In pathological states, Osborne’s ligament, the arcade of Struthers, or the medial intermuscular septum can act as rigid fulcrums, causing localized ischemia and demyelination. Transposition alters the biomechanical axis of the nerve, placing it anterior to the axis of rotation and thereby neutralizing these tension forces.
Patient Positioning and Preparation
- Positioning: The patient is placed supine with the operative arm abducted to 90 degrees and externally rotated on a radiolucent hand table.
- Tourniquet: A sterile pneumatic tourniquet is applied high on the brachium. Exsanguination is performed carefully, noting that excessive tourniquet pressure or prolonged inflation can exacerbate pre-existing ischemic nerve injury.
- Magnification: Surgical loupes (2.5x to 3.5x) are mandatory for meticulous intraneural dissection and preservation of the vasa nervorum.
Surgical Technique: Anterior Transposition
🔪 Surgical Pearl: Incision and Superficial Dissection
Always anticipate the medial antebrachial cutaneous (MABC) nerve branches. Iatrogenic injury to the MABC is a leading cause of postoperative medial elbow pain and painful neuroma formation. Dissect superficial tissues bluntly and retract MABC branches meticulously.
- Incision: Make a curvilinear incision on the posteromedial surface of the elbow. Begin approximately 7 cm proximal to the medial epicondyle, pass distally and slightly anterior to the epicondyle, and proceed further distally in line with the anatomical course of the ulnar nerve.
- Flap Elevation: Reflect the anterior skin flap to expose the common origin of the flexor-pronator muscle mass.
- Nerve Identification: Identify the ulnar nerve in its groove posterior to the medial epicondyle. Incise Osborne's fascia and free the nerve from surrounding soft tissues. Release the flexor carpi ulnaris (FCU) from its humeral origin on the epicondyle to expose the nerve further distally.
- Branch Preservation: Identify the articular branches (which may be sacrificed) and the critical motor branches to the flexor digitorum profundus (FDP) and FCU. Carefully dissect these motor branches intraneurally up the main trunk to allow adequate mobilization without tethering.
- Mobilization: Dissect any fibrous tissue, osteophytes, or fracture callus from the area adjacent to the retro-epicondylar groove. Gently elevate and remove the nerve from the groove.
- Neurolysis: Carry out an external neurolysis. If there is extensive intraneural scarring or a palpable neuroma-in-continuity, a careful endoneurolysis may be indicated under microscopic magnification.
- Transposition: Draw the nerve over the medial epicondyle to the anterior surface of the elbow. Place it on the surface of the fascia of the flexor-pronator group, securing it beneath the thick subcutaneous fat in this region.
🚨 Surgical Warning: The Arcade of Struthers and Intermuscular Septum
Failure to excise the medial intermuscular septum is the most common cause of failed ulnar nerve transposition. The nerve will kink acutely over the intact septum when transposed anteriorly. Ensure the septum is excised as far proximally as the arcade of Struthers (approximately 8 cm proximal to the epicondyle).
- Stabilization: Place a few interrupted, loose absorbable sutures through the fascia and subcutaneous fat medial to the nerve to create a sling, preventing the nerve from slipping back posterior to the epicondyle.
- Hemostasis: Deflate the tourniquet and achieve meticulous hemostasis before closure. Postoperative hematoma in the transposed bed can lead to severe fibroplasia and recurrent compression.
Alternative: Anterior Submuscular Transposition
If an anterior submuscular transfer is preferred (often indicated in revision surgery, profound ulnar nerve subluxation, or severe ulnar neuropathy with muscle wasting), the flexor-pronator mass must be elevated.

- Place a hemostat beneath the superficial head of the pronator teres, the flexor carpi radialis, the palmaris longus, and the superficial head of the flexor carpi ulnaris. Crucial: Be absolutely certain not to include the median nerve in this clamp.
- Sharply divide the tendinous origin of the medial epicondyle, leaving a 1 cm cuff of tissue for later repair. Retract the flexor mass distally, carefully protecting the small motor branches from both the median and ulnar nerves.
- After placing the fully mobilized ulnar nerve deep to the flexor mass, repair the tendinous origin to the medial epicondyle with robust nonabsorbable sutures (e.g., #1 or #2 braided polyester).
Alternative: Medial Epicondylectomy
As an alternative to formal transposition, a medial epicondylectomy may be performed. This involves subperiosteal elevation of the flexor-pronator origin, osteotomy of the medial epicondyle (taking care not to violate the medial collateral ligament), and reattachment of the soft tissues. This allows the nerve to glide anteriorly without the bony prominence acting as a fulcrum.
Postoperative Care
For subcutaneous transpositions, a soft bulky dressing with a posterior splint is applied. For submuscular transpositions or epicondylectomies, the elbow is immobilized in a posterior splint at a right angle (90 degrees of flexion) with the forearm in neutral rotation for 3 weeks to protect the flexor-pronator repair.
Physical therapy is initiated immediately upon splint removal to restore terminal extension and prevent secondary contractures. Appropriate dynamic or static progressive splinting is continued until sufficient motor function has returned to allow the patient to be free of the brace.
THE MEDIAN NERVE: ANATOMY AND PATHOLOGY
The median nerve is the primary nerve of fine volitional activity in the hand. Injuries to this nerve are profoundly disabling, not only due to the loss of precision pinch and opposition but also because median nerve injuries frequently result in severe, debilitating causalgia (Complex Regional Pain Syndrome Type II) and painful neuromas.
Surgical Anatomy
The median nerve is formed by the junction of the lateral and medial cords of the brachial plexus in the axilla. It is composed of nerve fibers originating from the C6, C7, C8, and T1 nerve roots.
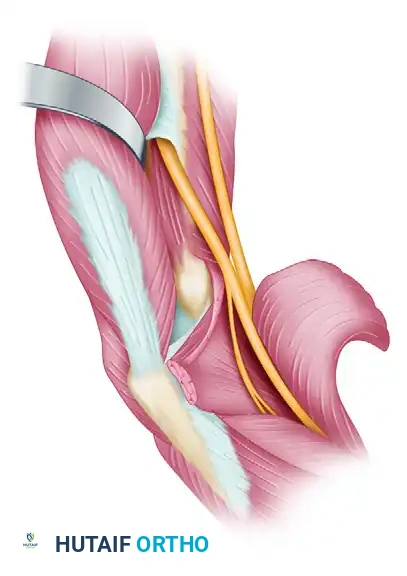
It courses down the brachium adjacent to the brachial artery. In the upper arm, it is relatively superficial and lacks major branches, making it vulnerable to external compression. As it crosses the elbow, it dives between the humeral and ulnar heads of the pronator teres, passing deep to the fibrous arch of the flexor digitorum sublimis (FDS) to enter the forearm.
Mechanisms of Injury and Entrapment
Median nerve injuries are most frequently caused by lacerations, typically occurring in the volar forearm or wrist (e.g., "spaghetti wrist" injuries). Sunderland's extensive research highlighted that in the upper arm, the nerve can be injured by relatively superficial lacerations, excessively tight tourniquets, and humeral shaft fractures. When injured near the axilla, concomitant injuries to the ulnar nerve, musculocutaneous nerve, and brachial artery are highly common.
Proximal Entrapment Sites:
1. Ligament of Struthers: An anomalous fibrous band extending from a supracondylar process of the humerus to the medial epicondyle.
2. Lacertus Fibrosus (Bicipital Aponeurosis): Thickened fascial band at the elbow crease.
3. Pronator Teres: Compression between the two heads, or by a hypertrophic muscle belly.
4. FDS Arch: The fibrous proximal edge of the flexor digitorum sublimis.
Anterior Interosseous Nerve (AIN) Entrapment:
The AIN, a purely motor branch of the median nerve, can be compressed by:
- Tendinous origins of the FDS or pronator teres.
- Variant muscles (palmaris profundus, flexor carpi radialis brevis).
- Accessory muscle slips (Gantzer muscle - accessory head of the flexor pollicis longus).
- Aberrant radial artery or thrombosis of ulnar collateral vessels.
- Enlargement of the bicipital bursa.
At the wrist, the median nerve is highly susceptible to compression within the carpal tunnel, often exacerbated by distal radius fractures, carpal dislocations (e.g., lunate or perilunate dislocations), or severe tenosynovitis.
CLINICAL EXAMINATION OF THE MEDIAN NERVE
Accurate clinical examination requires differentiating true median nerve deficits from substitution movements. Sunderland's works provide an excellent framework for recognizing these compensatory actions.
Motor Examination
The muscles of the forearm and hand supplied by the median nerve that can be tested with relative accuracy include:
- Pronator Teres (PT): Tested by active pronation against resistance with the elbow flexed.
- Flexor Carpi Radialis (FCR): Tested by active wrist flexion; the contracting FCR tendon must be palpated to rule out substitution by the FCU or abductor pollicis longus.
- Flexor Pollicis Longus (FPL): Tested by maintaining the interphalangeal joint of the thumb in flexion against resistance, with the wrist neutral and thumb adducted.
- Flexor Digitorum Sublimis (FDS): Examined separately for each finger while the remaining fingers are held in full passive extension to neutralize the FDP.
- Abductor Pollicis Brevis (APB): Tested by maintaining the thumb in palmar abduction against resistance. Palpation of the contracting muscle belly is essential to differentiate from abductor pollicis longus activity.
Clinical Pearl: Lumbrical Testing
The first and second lumbricals cannot be discretely tested. They are not palpable, and their function (MCP flexion with IP extension) is easily confused with the action of the intact interosseous muscles (ulnar nerve innervated).
Provocative Tests for Pronator Teres Syndrome
When examining a patient with suspected Pronator Teres Syndrome, three specific resistive tests are highly localizing:
1. Pronator Teres Localization: Production of symptoms with pronation of the forearm against resistance while the elbow is flexed and gradually extended.
2. FDS Arch Localization: Independent flexion of the FDS of the long finger against resistance. Reproduction of paresthesias in the radial three and a half digits localizes the entrapment to the fibrous arcade of the flexor sublimis.
3. Lacertus Fibrosus Localization: Flexion-supination of the elbow against resistance reproduces symptoms if the nerve is entrapped by the lacertus fibrosus.
Pronator Compression Test: The examiner applies direct pressure with the thumb just proximal and lateral to the proximal edge of the pronator teres muscle. The rapid onset of pain and paresthesias in the median nerve distribution within 30 seconds is considered a positive test.
Other findings include a positive Tinel sign over the proximal muscle mass, variable weakness in median-innervated extrinsics and intrinsics, and occasionally a visible depression in the contour of the forearm superficial to the lacertus fibrosus. Notably, Nerve Conduction Studies (NCS) and Electromyography (EMG) are frequently normal in Pronator Teres Syndrome, making it a primarily clinical diagnosis.
Anterior Interosseous Syndrome (AIN) Presentation
Typically, the patient presents with deep, aching pain in the proximal forearm lasting for several hours, followed by weakness or paralysis of the FPL, the FDP to the index and long fingers, and the pronator quadratus.
The "OK" Sign Deficit: When the patient attempts to pinch the thumb and index finger together, active flexion of the distal phalanges is impossible, resulting in a flat, pulp-to-pulp pinch rather than a circular "OK" sign.
Variations in presentation usually result from atypical innervation patterns, such as the Martin-Gruber anastomosis. If all FDP muscles are supplied by the AIN, all will be weak. Conversely, if there is overlapping ulnar innervation to the FDP of the long finger, that digit will be spared.
Sensory Examination and Autonomic Changes
Variations in the sensory supply can be confusing, but the classic median nerve distribution includes the volar surface of the thumb, index, and middle fingers, and the radial half of the ring finger.
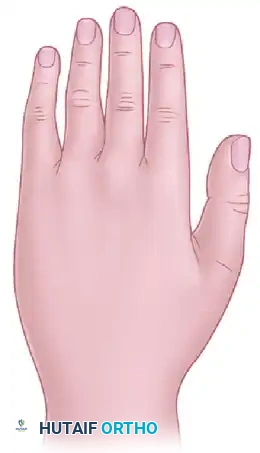
Dorsally, it supplies the distal phalanges of the index and middle fingers. The absolute smallest autonomous zone of the median nerve covers the dorsal and volar surfaces of the distal phalanges of the index and middle fingers.
Objective Sensory Testing:
- Ninhydrin Print Test / Iodine Starch Test: These tests evaluate sudomotor function (sweating). Denervated skin loses sympathetic sudomotor function, resulting in anhidrosis.
- Trophic Changes: In well-established lesions, autonomic changes such as anhidrosis, atrophy of the skin, loss of skin ridges, and narrowing of the digits due to pulp atrophy are highly valuable, objective signs of severe sensory deficit.
OPERATIVE TREATMENT OF MEDIAN NERVE LESIONS
Operative intervention is indicated for refractory entrapment syndromes, space-occupying lesions, and post-traumatic lacerations.
Pronator Teres Syndrome Decompression
Surgical exploration and decompression of the median nerve for refractory Pronator Teres Syndrome is highly effective. Studies by Hartz et al., and Johnson, Spinner, and Shrewsbury report successful symptom relief in 80% to 92% of patients, though some mild persistence of symptoms may remain in up to 66% of patients.
Surgical Approach:
1. An S-shaped incision is made across the antecubital fossa, extending distally over the volar forearm.
2. The lacertus fibrosus is identified and completely divided.
3. The median nerve is traced as it passes between the superficial and deep heads of the pronator teres. The superficial head may be step-cut or Z-lengthened to relieve pressure.
4. The nerve is followed distally to the fibrous arch of the FDS, which is completely released.
5. Any anomalous bands, such as a hypertrophic Gantzer muscle or aberrant vessels, are ligated or excised.
🚨 Diagnostic Pitfall: Double Crush Syndrome
In patients presenting with symptoms of both Carpal Tunnel Syndrome (CTS) and Pronator Teres Syndrome, meticulous attention must be paid to preoperative nerve conduction studies. If the NCS is positive for CTS, we recommend performing a carpal tunnel release first, anticipating that proximal symptoms may resolve. If the NCS is negative for CTS but clinical signs point proximally, proximal median nerve exploration is the initial procedure of choice.
Management of Anterior Interosseous Syndrome
For AIN syndrome, Spinner’s evidence-based algorithm is recommended:
- Spontaneous Onset: If the onset of paralysis is spontaneous (neuritis or idiopathic entrapment), initial treatment is strictly nonoperative (rest, NSAIDs, splinting).
- Surgical Exploration: Indicated in the absolute absence of clinical or EMG improvement after 12 weeks of conservative management. The surgical approach mirrors that of pronator syndrome, with specific attention to the deep fascial bands of the FDS and the origin of the FPL.
- Traumatic Injury: If the AIN injury is caused by a penetrating wound, primary microsurgical repair is recommended immediately.
- Irreparable Injury: In cases of delayed presentation or irreparable nerve destruction, tendon transfers (e.g., Brachioradialis to FPL, and ECRL to FDP) are highly successful in restoring pinch and grip function.
Conclusion
Mastery of upper extremity peripheral nerve surgery requires an intimate knowledge of anatomical variants, precise clinical examination skills, and meticulous surgical technique. Whether performing a complex submuscular transposition of the ulnar nerve or a multi-level decompression of the median nerve, the surgeon's goal remains the restoration of neural gliding and the elimination of ischemic compression, thereby optimizing functional recovery for the patient.
📚 Medical References
You Might Also Like