Transfer of the Extensor Indicis Proprius and Extensor Digiti Quinti Proprius
Key Takeaway
The Fowler tendon transfer utilizes the extensor indicis proprius (EIP) and extensor digiti quinti proprius (EDQP) to restore intrinsic hand function in patients with claw hand deformity. By routing these split tendons volar to the deep transverse metacarpal ligament and inserting them into the radial lateral bands, surgeons can effectively restore metacarpophalangeal flexion and interphalangeal extension. This guide details the biomechanics, surgical technique, and postoperative protocols for optimal outcomes.
Introduction to Intrinsic Tendon Transfers
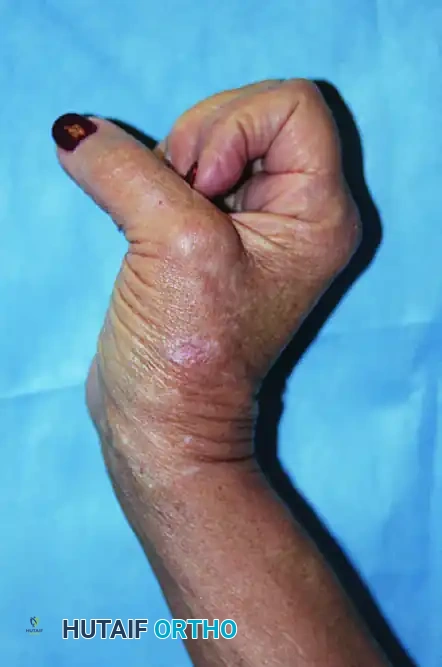
The intrinsic-minus hand, classically presenting as a "claw hand" deformity, is a debilitating condition resulting from the loss of lumbrical and interosseous muscle function. Most commonly caused by ulnar nerve palsy or combined ulnar and median nerve lesions, this neuromuscular imbalance leads to hyperextension of the metacarpophalangeal (MCP) joints and flexion of the proximal and distal interphalangeal (PIP and DIP) joints. The unopposed action of the extensor digitorum communis (EDC) at the MCP joint and the flexor digitorum profundus (FDP) at the IP joints creates a profound functional deficit, severely impairing grip strength, fine motor dexterity, and hand integration.
To restore the delicate biomechanical balance of the hand, numerous tendon transfer techniques have been developed. The Fowler Transfer, utilizing the Extensor Indicis Proprius (EIP) and the Extensor Digiti Quinti Proprius (EDQP)—also known anatomically as the Extensor Digiti Minimi (EDM)—serves as a highly effective method for restoring intrinsic function. By rerouting these expendable extensor tendons volar to the deep transverse metacarpal ligament, the surgeon alters their line of pull, converting them into MCP flexors and IP extensors.
This comprehensive guide details the surgical anatomy, biomechanical rationale, step-by-step operative technique, and postoperative rehabilitation protocols for the Fowler transfer and its notable Riordan modification.
Surgical Anatomy and Biomechanics
A profound understanding of dorsal hand anatomy and intrinsic biomechanics is mandatory for the successful execution of this transfer.
The Donor Motors
- Extensor Indicis Proprius (EIP): The EIP muscle originates from the distal third of the ulna and the interosseous membrane. Its tendon travels through the fourth dorsal extensor compartment alongside the EDC tendons. At the level of the index metacarpal, the EIP tendon is consistently located ulnar and deep to the EDC tendon of the index finger. Its independent muscle belly extends further distally than that of the EDC, aiding in its identification.
- Extensor Digiti Quinti Proprius (EDQP / EDM): The EDQP originates from the lateral epicondyle of the humerus and travels through the fifth dorsal extensor compartment. It typically consists of two tendon slips that insert into the extensor aponeurosis of the little finger. It is located ulnar to the EDC of the little finger (if an EDC slip to the little finger is present).
The Biomechanical Fulcrum
The success of the Fowler transfer relies entirely on altering the vector of the transferred tendons. Normally, the EIP and EDQP are dorsal to the MCP joint axis, acting as extensors. By passing the harvested tendons volar to the deep transverse metacarpal ligament (DTML), the DTML acts as a biomechanical pulley. This volar routing shifts the tendon's line of pull anterior to the MCP joint's axis of rotation, creating a flexion moment at the MCP joint while simultaneously transmitting an extension force to the PIP and DIP joints via the lateral bands.
💡 Clinical Pearl
The deep transverse metacarpal ligament is the critical anatomical structure in intrinsic replacement surgery. Failure to route the tendon volar to this ligament will result in a complete failure of the transfer, as the tendon will continue to act as an MCP extensor, exacerbating the claw deformity.
Preoperative Evaluation and Indications
Indications
- Isolated ulnar nerve palsy with flexible clawing of the ring and little fingers.
- Combined low median and ulnar nerve palsies resulting in a global intrinsic-minus hand.
- Charcot-Marie-Tooth disease or other peripheral neuropathies causing intrinsic wasting.
- Hansen’s disease (Leprosy) with secondary claw hand deformities.
The Bouvier Test
Before selecting the Fowler transfer, the surgeon must perform the Bouvier test.
1. The examiner passively blocks the patient's MCP joints in slight flexion.
2. The patient is asked to actively extend their PIP and DIP joints.
3. Positive Bouvier Test: The patient can fully extend the IP joints. This indicates that the extensor mechanism is intact and the clawing is purely due to intrinsic weakness. A tendon transfer (like the Fowler) is highly indicated.
4. Negative Bouvier Test: The patient cannot extend the IP joints despite MCP stabilization. This indicates secondary joint contractures or central slip attenuation. In this scenario, a simple tendon transfer will fail; the patient requires concurrent PIP joint capsulodesis, arthrodesis, or a different reconstructive approach.
🛑 Pitfall
Performing a Fowler transfer on a hand with fixed PIP flexion contractures (a negative Bouvier test) will result in suboptimal outcomes. Always ensure passive joint suppleness through aggressive preoperative hand therapy before surgical intervention.
Surgical Technique: The Fowler Transfer
The Fowler technique utilizes both the EIP and EDQP to provide four slips of insertion, restoring intrinsic function to all four fingers.
1. Patient Positioning and Anesthesia
- Anesthesia: Regional block (supraclavicular or axillary brachial plexus block) or general anesthesia.
- Positioning: Supine with the operative arm extended on a radiolucent hand table.
- Tourniquet: A well-padded pneumatic tourniquet is applied to the proximal arm and inflated to 250 mm Hg after exsanguination with an Esmarch bandage.
- Preparation: Standard surgical prep and drape from the fingertips to the elbow.
2. Harvesting the Extensor Indicis Proprius (EIP)
- Incision: Make a dorsal longitudinal, slightly curved, or zigzag incision over the radial aspect of the index finger MCP joint, extending proximally over the distal metacarpal.
- Identification: Retract the skin flaps to expose the extensor hood. Identify the EIP tendon. Remember the anatomical rule: the EIP is deep and ulnar to the common extensor tendon (EDC) of the index finger.
- Harvesting for Maximum Length: Dissect the EIP tendon distally to its insertion into the extensor aponeurosis. To obtain the maximum possible length—which is critical because the tendon must reach the lumbrical canal—excise a small, longitudinal strip of the extensor aponeurosis along with the tendon.
- Aponeurosis Repair: Immediately suture the residual defect in the sagittal band and extensor aponeurosis using 4-0 non-absorbable braided sutures (e.g., Ethibond or Ticron). This prevents ulnar subluxation of the remaining EDC tendon during postoperative mobilization.
⚠️ Surgical Warning
If the EIP is harvested too proximally without taking a strip of the aponeurosis, the tendon slips will be too short. This will result in excessive tension upon transfer, leading to a severe intrinsic-plus deformity (swan neck deformity) postoperatively.
3. Splitting and Routing the EIP
- Splitting: Using a Watson-Cheyne dissector or fine tenotomy scissors, split the harvested EIP tendon longitudinally into two equal slips. Extend the split proximally to the musculotendinous junction.
- Routing: Create a pathway from the dorsal incision, passing distally and volarly into the lumbrical canals of the index and middle fingers.
- Passing the Tendon: Pass each slip of the EIP volar to the deep transverse metacarpal ligament.
- Target: Bring the slips out adjacent to the radial lateral bands of the index and middle fingers.
4. Harvesting the Extensor Digiti Quinti Proprius (EDQP)
- Incision: Make a similar dorsal incision over the little finger MCP joint.
- Identification: Identify the EDQP tendon. Verify its identity by applying traction and observing independent little finger extension.
- Harvesting: Free its insertion from the extensor hood, again taking care to harvest maximum length. Ensure the EDC slip to the little finger is intact; if the little finger lacks an EDC slip, harvesting the EDQP will result in a severe extensor lag.
- Splitting and Routing: Split the EDQP tendon into two equal longitudinal slips. Pass each slip volar to the deep transverse metacarpal ligament, directing them toward the radial side of the ring and little fingers.
5. Tendon Insertion and Tensioning (The Bunnell Technique)
- Insertion Site: The slips are attached to the extensor aponeurosis (specifically the radial lateral band) of the index, middle, ring, and little fingers, mimicking the insertion of the lumbrical muscles.
- Weaving: Use the Bunnell technique of tendon weaving. Make a small slit in the lateral band, pass the donor slip through it, and fold it back upon itself.
- Setting the Tension: This is the most technically demanding aspect of the procedure.
- Place the wrist in neutral to 30 degrees of extension.
- Place the MCP joints in 70 to 80 degrees of flexion.
- Place the PIP and DIP joints in full extension.
- Apply moderate tension to the tendon slips—just enough to eliminate slack but not so tight as to cause a rigid intrinsic-plus posture.
- Suturing: Secure the weave with multiple interrupted 4-0 non-absorbable sutures.
- Verification: Release the hand and observe the resting posture. The tenodesis effect should naturally bring the MCP joints into flexion and the IP joints into extension when the wrist is extended.
The Riordan Modification
The classic Fowler transfer utilizes both the EIP and EDQP. However, harvesting the EDQP can occasionally lead to an unacceptable extension lag at the little finger, particularly if the EDC contribution to the fifth digit is anatomically deficient or absent.
To mitigate this risk, Riordan introduced a highly favored modification:
* Single Motor Utilization: The Riordan modification completely spares the EDQP, leaving little finger extension uncompromised.
* EIP as the Sole Motor: Only the EIP is harvested.
* Splitting into Four: If all four fingers require intrinsic replacement, the EIP can be split into four separate slips. However, because the EIP muscle belly is relatively small, splitting it four ways can significantly dilute its force generation.
* Targeted Transfer: More commonly, the Riordan modification is used in isolated ulnar nerve palsy where only the ring and little fingers are clawed (the index and middle fingers retain their median-innervated lumbricals). In this scenario, the EIP is split into two slips, routed volar to the DTML, and inserted into the radial lateral bands of the ring and little fingers only.
💡 Clinical Pearl
When treating a low ulnar nerve palsy, the Riordan modification (using the EIP to motor the ring and little fingers) is often the procedure of choice. It provides excellent MCP flexion force without risking the extensor mechanism of the fifth digit.
Postoperative Care and Rehabilitation
The success of an intrinsic tendon transfer is heavily dependent on strict adherence to postoperative rehabilitation protocols. The postoperative care for the Fowler transfer and its modifications follows the principles established for the modified Bunnell technique.
Phase 1: Immobilization (Weeks 0-4)
- Immediately postoperatively, the hand and forearm are immobilized in a custom-molded dorsal blocking splint or a bulky compressive cast.
- Positioning:
- Wrist: 30 degrees of extension.
- MCP Joints: 70 to 90 degrees of flexion.
- IP Joints: Full extension.
- This "intrinsic-plus" position removes all tension from the newly transferred tendon weaves, allowing for secure biological healing.
- Strict elevation and digital edema control are maintained.
Phase 2: Early Mobilization (Weeks 4-6)
- The rigid cast is removed and replaced with a removable dorsal blocking splint maintaining the same joint angles.
- Active Range of Motion (AROM): The patient initiates active flexion of the MCP and IP joints within the constraints of the splint.
- Passive Extension: Passive extension of the IP joints is encouraged to prevent PIP flexion contractures, provided the MCP joints are kept securely flexed.
- Active extension of the MCP joints is strictly prohibited during this phase to prevent stretching or rupturing the tendon repair.
Phase 3: Progressive Strengthening (Weeks 6-12)
- The dorsal blocking splint is gradually discontinued during the day but may be worn at night for an additional 2-4 weeks.
- The patient begins active MCP extension exercises.
- Neuromuscular re-education is critical. The patient must learn to fire the EIP (originally an index finger extensor) to achieve MCP flexion. Biofeedback and mirror therapy can be highly beneficial.
- Progressive resistance exercises (e.g., putty, grip strengthening) are introduced at week 8.
- Unrestricted activity is typically permitted by 12 weeks postoperatively, provided that adequate motor control and tendon healing have been achieved.
Complications and Management
- Swan Neck Deformity (Intrinsic-Plus Hand): Caused by over-tensioning the transfer. If the tendon is sutured too tightly, the excessive pull on the lateral bands will cause PIP hyperextension and DIP flexion. Management requires prolonged splinting and, if refractory, surgical release or lengthening of the lateral bands.
- Recurrent Clawing: Caused by under-tensioning the transfer, failure to route the tendon volar to the deep transverse metacarpal ligament, or rupture of the repair site during early rehabilitation.
- Extensor Lag: Harvesting the EDQP can result in an extensor lag of the little finger. This is best prevented by confirming the presence of an adequate EDC slip to the little finger prior to harvesting, or by utilizing the Riordan modification.
-
Adhesions: Tendon adhesions along the routing pathway (especially within the lumbrical canal) can restrict excursion. Meticulous hemostasis, atraumatic tissue handling, and timely postoperative therapy are essential preventative measures.
You Might Also Like