00:00
Start Quiz
Question 26
Figure 11 shows the radiograph of an 18-year-old soccer player who reports recurrent lateral foot pain after sustaining an inversion injury. History reveals that 6 months ago he had been treated in a non-weight-bearing cast for a fifth metatarsal fracture. Management should consist of
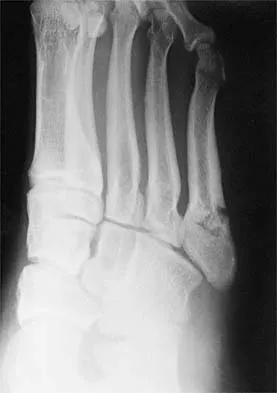
Explanation
Fractures in this area of the fifth metatarsal have a high incidence of delayed union, nonunion, and recurrence with nonsurgical management. In an acute fracture, prolonged casting in a non-weight-bearing cast may allow for healing; however, in the presence of prolonged symptoms, recurrent fracture, and intermedullary sclerosis, surgical treatment is preferred. Surgery most commonly consists of intermedullary fixation or medullary curettage and bone grafting, followed by application of a non-weight-bearing cast. Torg JS, Balduini FC, Zelko RR, Pavlov H, Peff TC, Das M: Fractures of the base of the fifth metatarsal distal to the tuberosity: Classification and guidelines for nonsurgical and surgical management. J Bone Joint Surg Am 1984;66:209-214.
Question 27
Which of the following types of exercise used to increase flexibility is considered most beneficial in increasing joint range of motion?

Explanation
Evidence has shown that PNF is the treatment of choice to increase joint range of motion and flexibility. PNF has the advantage of pushing the patient to stretch a little further when the muscle tendon unit is relaxed by a partner. While isokinetic and eccentric exercises can improve flexibility, and therefore increase range of motion, their main purpose is to increase strength and endurance. Ballistic stretching involves a large load applied rapidly; however, evidence has shown that static stretching, where a low load is applied for a long duration, offers a more significant benefit. Sady SP, Wortman M, Blanke D: Flexibility training: Ballistic, static or proprioceptive neuromuscular facilitation? Arch Phys Med Rehabil 1982;63:261-263. Tanigawa MC: Comparison of the hold-relax procedure and passive mobilization on increasing muscle length. Phys Ther 1972;52:725-735.
Question 28
The view from an anterosuperior portal of the right shoulder shown in Figure 12 reveals which of the following findings?
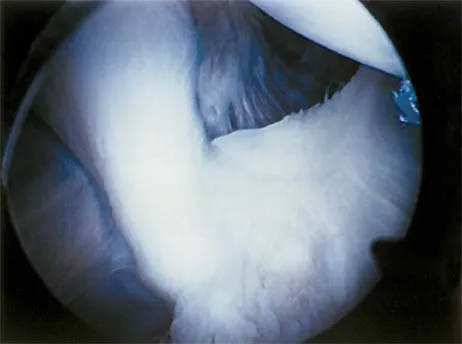
Explanation
The arthroscopic view shows a HAGL lesion. With the arthroscope directed anteroinferiorly, muscular striations of the subscapularis can be visualized through the avulsion site. In vitro strain studies indicate that glenohumeral ligament failure on the humeral side occurs in approximately 25% of patients, while clinically this lesion has been reported in approximately 9% of patients with shoulder instability. Failure to recognize and treat this lesion leads to persistent anterior instability. An ALPSA lesion, a Bankart variant, occurs on the glenoid side and is characterized by a sleeve-like medial retraction and inferior rotation. A Bankart lesion is the classic avulsion of the glenohumeral ligament from the glenoid rim. The subscapularis tendon and the rotator interval are not shown in the figure. Wolf EM, Cheng JC, Dickson K: Humeral avulsion of glenohumeral ligaments as a cause of anterior shoulder instability. Arthroscopy 1995;11:600-607. Bigliani LU, Pollack RG, Soslowsky LJ, Flatow EL, Pawluk RJ, Mow VC: Tensile properties of the inferior glenohumeral ligament. J Orthop Res 1992;10:187-197.
Question 29
An 18-year-old football player has intense pain and is unable to bear weight on the right knee after being tackled from the front. A posterior knee dislocation is reduced on the field. Because the game took place in a remote location, the patient is not examined in the emergency department until 5 hours after the injury. Examination now shows a grossly swollen knee with moderate ischemia in the lower leg. Posterior tibial and dorsalis pedis pulses are diminished. The best course of action should be to
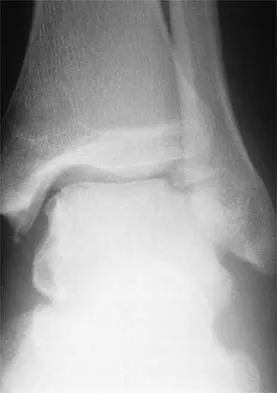
Explanation
Vascular injuries occur in approximately 20% to 35% of knee dislocations, of which one third are posterior. Recognition of the vascular injury is essential. Normal pulses or normal capillary refill do not preclude an arterial injury, and arteriography should be considered in all knee dislocations. If the leg is ischemic, the arteriogram should be circumvented and the patient taken directly to the operating room. The risk of muscle fibrosis, contracture, or vascular insufficiency, and the need for amputation increase significantly when ischemia exceeds 6 hours. This patient has ischemia and is considered a vascular emergency. As such, delays for a thorough examination of the ligament, MRI scans, and even an arteriogram are unwarranted. Concurrent ligamentous repair and reconstruction should be deferred until vascular stability has been achieved. Kremchek TE, Welling RE, Kremchek EJ: Traumatic dislocation of the knee. Orthop Rev 1989;18:1051-1057.
Question 30
A 17-year-old football player is unable to flex the distal interphalangeal (DIP) joint of his ring finger. He states that he injured the finger 6 weeks ago while attempting to tackle another player who pulled free from his grip, but he did not inform his coach at the time of the injury. Current radiographs show an observable fleck of bone volar to the base of the proximal phalanx. Treatment should consist of
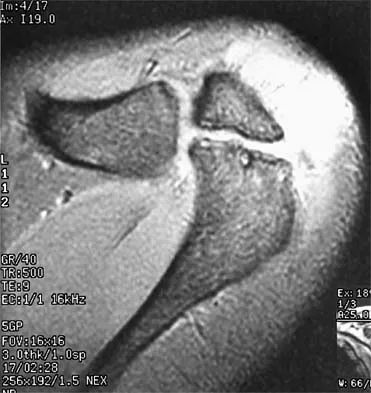
Explanation
Flexor digitorum profundus ruptures are classified into three types. In type I, the tendon retracts into the palm. In type II, the tendon retracts to the level of the proximal phalanx, the vinculum remains intact, and the blood supply is preserved to the tendon. A small fleck of bony fragment observed at the A2 pulley is pathognomonic for a type II rupture. Successful primary repair of the type II rupture has been reported as late as 2 months after the injury. Type III injuries have large fragments of the distal phalanx attached and are caught distally by the A1 pulley. Type III ruptures can be repaired up to several months after the injury. Leddy JP: Avulsions of the flexor digitorum profundus. Hand Clin 1985;1:77-83.
Question 31
A 48-year-old ski instructor dislocates his nondominant shoulder in a fall. Management consisting of application of a sling for 1 week results in improvement in his pain. Follow-up examination 6 weeks after the injury reveals that the patient continues to have difficulty with shoulder elevation. Management should now include
Explanation
Patients who are older than age 45 years and have initial dislocations are at greater risk for tearing the rotator cuff. Patients who are unable to lift the upper extremity or who have continued pain should undergo further evaluation for potential rotator cuff tears; early diagnosis is preferred. Physical therapy or continued use of a sling will be of little benefit. A corticosteroid injection might delay the diagnosis and compromise subsequent rotator cuff repair. Repairing the labrum generally is not necessary in a patient of this age who has an initial dislocation. Hawkins RJ, Bell RH, Hawkins RH, Koppert GJ: Anterior dislocation of the shoulder in the older patient. Clin Orthop 1986;206:192-195.
Question 32
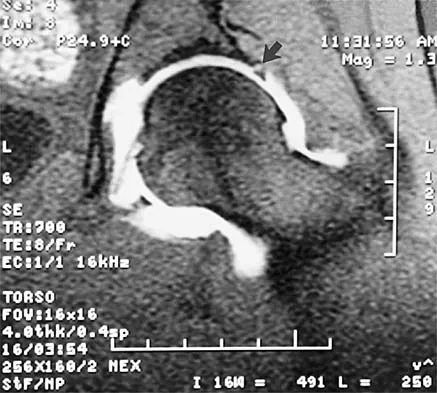
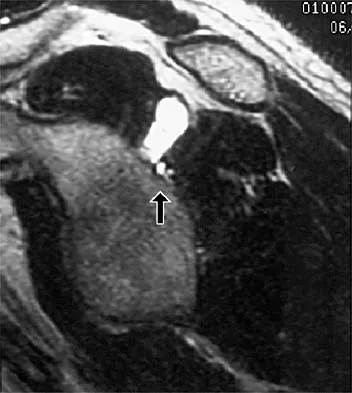
Figure 13 shows the MRI scan of a 29-year-old rock climber who reports increasing shoulder pain and weakness. Based on these findings, atrophy will most likely occur in which of the following muscles?
Explanation
The MRI scan shows a cyst at the spinoglenoid notch. These cysts are often associated with a labral injury, such as a superior labrum anterior and posterior (SLAP) lesion. The suprascapular nerve passes through the suprascapular notch and sends motor branches to the supraspinatus and sensory branches to the capsule. At the spinoglenoid notch, the infraspinatus branch of the suprascapular nerve is compressed by the cyst, leading to isolated infraspinatus atrophy. The teres minor and the deltoid are innervated by the axillary nerve. Fehrman DA, Orwin JF, Jennings RM: Suprascapular nerve entrapment by ganglion cysts: A report of six cases with arthroscopic findings and review of the literature. Arthroscopy 1995;11:727-734. Ianotti JP, Ramsey ML: Arthroscopic decompression of a ganglion cyst causing suprascapular nerve compression. Arthroscopy 1996;12:739-745.
Question 33
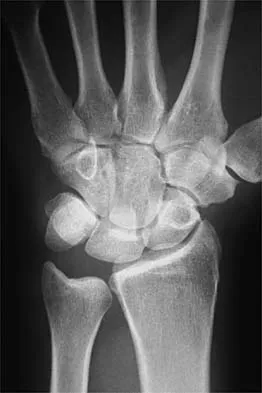
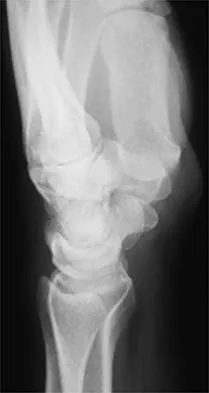
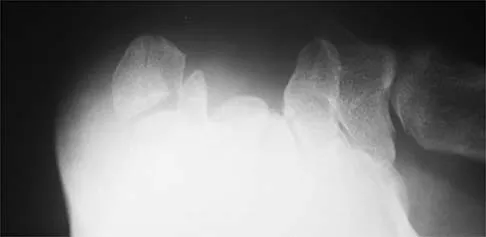
A 46-year-old man has acute tenderness along the ulnar aspect of the wrist after falling on his outstretched hand while playing basketball. Examination reveals tenderness and mild swelling along the volar ulnar aspect of the wrist. Radiogaphs are shown in Figures 14a through 14c. Management should consist of
Explanation
The PA view of the wrist shows a pisiform fracture. Pisiform fractures constitute 1% to 3% of all carpal bone fractures. This fracture can be further evaluated with a carpal tunnel view or a supination oblique view of the wrist. Initial management should consist of immobilization with a short arm cast. If nonsurgical measures fail, bony excision is warranted. Failla JM, Amadio PC: Recognition and treatment of uncommon carpal fractures. Hand Clin 1988;4:469-476.
Question 34
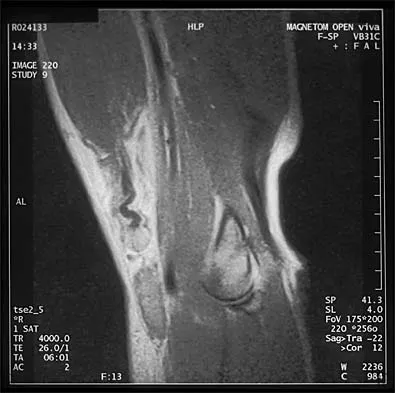
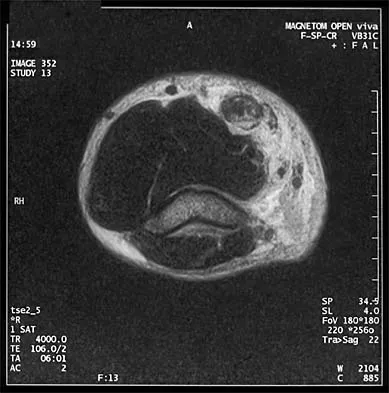
A 32-year-old powerlifter who was performing a dead lift 3 days ago noted a sharp pain in the front of his dominant right arm just after beginning to lower the weight. He now reports pain in the anterior aspect of the arm that worsens when he opens a door. Examination reveals moderate ecchymosis and swelling of the forearm and tenderness in the antecubital fossa. The MRI scans are shown in Figures 15a and 15b. If the injury is left unrepaired, the greatest functional deficit will most likely be the loss of
Explanation
A complete tear of the distal biceps brachii most often occurs from a large, rapid eccentric elbow extension load. A pop or tearing sensation usually occurs, and a palpable defect in the antecubital fossa is often present on examination. The treatment of choice is a direct primary repair by a two-incision technique. If left unrepaired, the most disabling consequence is the loss of forearm supination strength. It is unlikely that significant elbow or forearm motion will be lost if the rupture is left unrepaired and early motion exercises are initiated. Elbow flexion strength tends to return with time, but the loss of forearm supination strength remains problematic. D'Alessandro DF, Shields CL Jr, Tibone JE, Chandler RW: Repair of distal biceps tendon ruptures in athletes. Am J Sports Med 1993;21:114-119.
Question 35
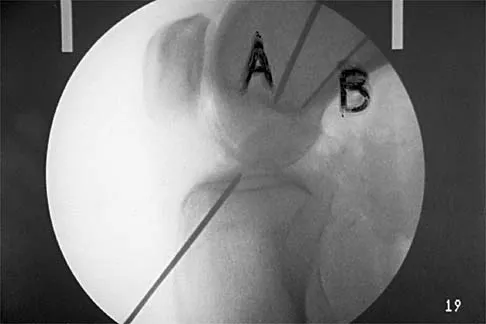
Figure 16 shows the lateral radiograph of a patient who is scheduled to undergo an anterior cruciate ligament (ACL) reconstruction. If the graft is tensioned at 20 degrees of flexion and the femoral tunnel is created by passing a reamer over the guide wire marked "A," the resulting ligament reconstruction will excessively
Explanation
If the femoral tunnel is created using guide wire A, it will be too far anterior in the intercondylar notch. The distance between a central tibial insertion for the ACL and an anterior femoral tunnel will progressively increase as the knee is flexed. Therefore, if the graft is tensioned near extension, the ligament will excessively tighten as the knee flexes past 90 degrees. This will result in restricted knee flexion or failure of the graft as full flexion is gained. There will be little effect on the ligament as it extends from 20 degrees to 0 degrees of flexion. If the graft is tensioned in significant flexion (greater than 60 degrees), it will be excessively loose as the knee fully extends. Daniel DM, Fritschy D: Anterior cruciate ligament injuries, in DeLee JC, Drez D Jr (eds): Orthopaedic Sports Medicine: Principles and Practice. Philadelphia, PA, WB Saunders, 1994, pp 1313-1360.
Question 36
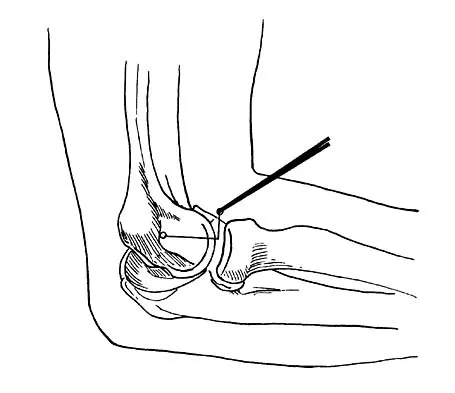
Which of the following nerves is most commonly injured during revision surgery following a Bristow procedure?
Explanation
Because of the previously transferred bone block of coracoid and short arm flexors, the musculocutaneous nerve often scars along the anteroinferior glenohumeral capsule. Mobilization of this tissue places the nerve at greatest risk. The axillary nerve is also potentially at risk, but this is nonspecific to prior surgery, particularly the Bristow procedure. Norris TR: Complications following anterior instability repairs, in Bigliani LU (ed): Complications of Shoulder Surgery. Baltimore, MD, Williams and Wilkins, 1993, pp 98-116.
Question 37
A 17-year-old high school soccer player sustains an anterior cruciate ligament (ACL) tear at the beginning of the season. An MRI scan confirms a complete ACL tear with no meniscal injuries. The patient plans an early return to play and would like to avoid surgery. Therefore, the patient and family should be advised that nonsurgical management consisting of rehabilitative exercises and the use of a functional knee brace will most likely result in
Explanation
While there are athletes who can function at a full level with an ACL tear, they are in the minority. As yet, there is no reliable way to predict the patients who will be able to compensate for the loss of the ACL. Studies have confirmed the risk of recurrent instability and meniscal injury in athletes with an ACL-deficient knee who participate in cutting sports. One study showed that only 12 of 43 patients who attempted rehabilitation and bracing were able to return successfully for the season. Another study showed that 17 of 31 athletes who were able to return to their sport sustained 23 meniscal tears because of recurrent instability. Shelton WR, Barrett GR, Dukes A: Early season anterior cruciate ligament tears: A treatment dilemma. Am J Sports Med 1997;25:656-658.
Question 38
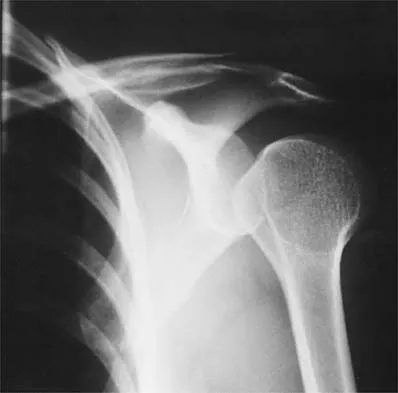
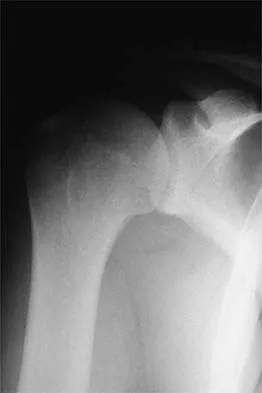
A patient underwent anterior stabilization of the shoulder 6 months ago, and examination now reveals lack of external rotation beyond 0 degrees. The patient has a normal apprehension sign and normal strength, and the radiographs are normal. Based on these findings, the patient is at greater risk for the development of
Explanation
Because the patient's shoulders are overtensioned anteriorly, premature osteoarthritis may develop. This may create obligate translation posteriorly and increase the interarticular pressure of the humeral head against the glenoid. Patients should achieve 20 degrees to 30 degrees of external rotation with the elbow at the side. Late degenerative arthritis following a Putti-Platt procedure is associated with significant restriction of external rotation. This patient's shoulder has a reduced risk of anterior instability, rotator cuff tear, and internal impingement because of the limitation of motion. Hawkins RJ, Angelo RL: Glenohumeral osteoarthritis: A late complication of the Putti-Platt repair. J Bone Joint Surg Am 1990;72:1193-1197.
Question 39
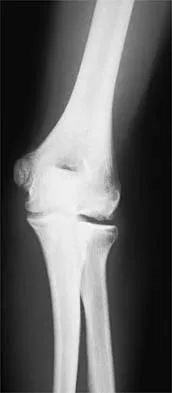
A 13-year-old girl who competes in gymnastics reports the insidious onset of lateral left elbow pain over the past 6 months. She also notes occasional catching episodes in the elbow; however, she denies any history of trauma. Examination reveals tenderness over the lateral epicondyle and extensor muscle origin. The elbow is stable and has full flexion, but lacks 10 degrees of full extension. An AP plain radiograph and an MRI scan are shown in Figures 17a and 17b. Management of the elbow should consist of
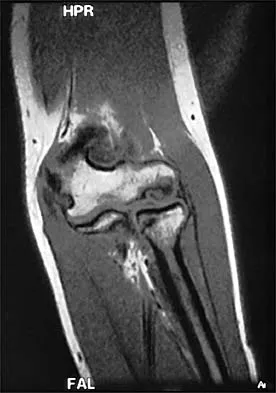
Explanation
The radiograph and MRI scan show osteochondritis dissecans of the capitellum, and the patient's history suggests a loose body. The treatment of choice is arthroscopic removal of the loose body and microfracture of the crater. Excision of the radial head, a cortisone injection, or tennis elbow release does not treat the pathology in the capitellum. Nonsurgical treatment would not relieve the mechanical symptoms of the loose body or promote healing in the crater. Baumgarten TE, Andrews JR, Satterwhite YE: The arthroscopic classification and treatment of osteochondritis dissecans of the capitellum. Am J Sports Med 1998;26:520-530. Jackson DW, Silvino N, Reiman P: Osteochondritis in the female gymnast's elbow. Arthroscopy 1989;5:129-136.
Question 40
A 25-year-old man injures his shoulder while skiing. Examination reveals increased passive external rotation, pain in the cocked position, and a positive lift-off test. What is the most likely diagnosis?
Explanation
A positive lift-off test and increased passive external rotation are diagnostic of a subscapularis tear or detachment. Although a similar injury could produce anterior instability, this will test the integrity of the subscapularis. A locked dislocation has limited passive movement. A ruptured biceps tendon will most likely produce ecchymosis and findings similar to supraspinatus trauma. Internal impingement is not associated with subscapularis weakness. Gerber C, Krushell RJ: Isolated rupture of the tendon of the subscapularis muscle: Clinical features in 16 cases. J Bone Joint Surg Br 1991;73:389-394.
Question 41
A college basketball player is struck in the eye by a player's hand while driving to the basket. Fluorescein evaluation reveals the injury shown in Figure 18. Management should consist of
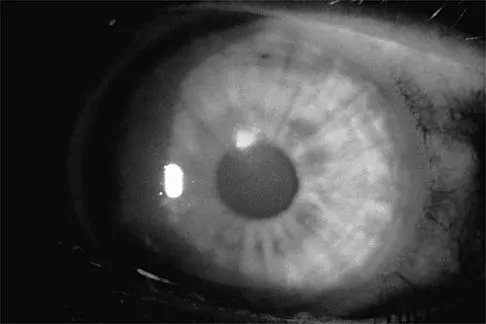
Explanation
The athlete has a corneal abrasion. Fluorescein staining identifies the break in the epithelium when examined with ultraviolet light. Topical antibiotics are used as prophylaxis against secondary bacterial infection, and the patch, applied with the lid closed, is used for comfort and to promote epithelial healing. The accompanying symptoms, including pain, tearing, and photophobia, are usually too intense to allow a return to play. Surgery is reserved for a corneal laceration with associated loss of the anterior chamber. While a proper fundoscopic examination may be a consideration, increased intraocular pressure is not typically associated with this injury. Traumatic hemorrhage in the anterior chamber (hyphema) necessitates strict bed rest during the early phases of healing; examination will most likely reveal the red fluid level of blood settling inferiorly in the anterior chamber. It is often associated with increased intraocular pressure. Brucker AJ, Kozart DM, Nichols CW, et al: Diagnosis and management of injuries to the eye and orbit, in Torg JS (ed): Athletic Injuries to the Head, Neck, and Face. St Louis, MO, Mosby-Year Book, 1991, pp 650-670.
Question 42
In patient selection for meniscal allograft transplantation, which of the following variables has the greatest influence on outcome?
Explanation
Many clinical studies to date show that the extent of arthritis is the most common variable that has the greatest influence on outcome. The success rate of allograft transplantation is significantly diminished in patients who have grade IV chondromalacia of the knee or notable flattening and general joint incongruity. Carter TR: Meniscal allograft transplantation. Sports Med Arthroscopy Rev 1999;7:51-63. Garrett JC: Meniscal transplantation: A review of 43 cases with two- to seven-year follow-up. Sports Med Arthroscopy Rev 1993;2:164-167.
Question 43
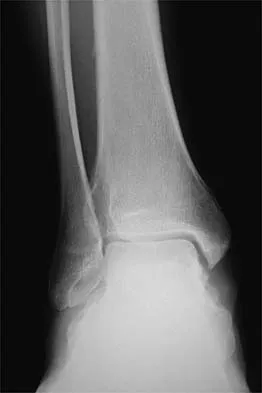
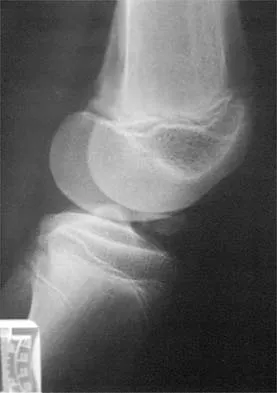
A 10-year-old boy sustained an injury to the left knee. The radiographic findings shown in Figure 19 are most commonly associated with injury to which of the following structures?
Explanation
The radiograph shows a bony avulsion of the ACL attachment site on the tibial spine in this skeletally immature patient. In this age group, injury often results in failure of the bony attachment site rather than the substance of the ligament. Avulsion of the patellar tendon insertion site can occur, but this structure is located at the apophysis of the tibial tubercle. The attachment site of the PCL is much more posterior. In adults, bony avulsion is more commonly associated with PCL injuries than with ACL injuries. When a small bony avulsion of the lateral capsule from the lateral tibial plateau is seen on the AP view, this finding is considered pathognomonic of an ACL injury (Segond sign) in adults. The area of the pes anserinus is anterior and distal; avulsion would be unusual. Baxter MP, Wiley JJ: Fractures of the tibial spine in children: An evaluation of knee stability. J Bone Joint Surg Br 1988;70:228-230. Meyers MH, McKeever FM: Fracture of the intercondylar eminence of the tibia. J Bone Joint Surg Am 1970;52:1677-1684.
Question 44
What is the single most important nutritional factor affecting athletic performance?
Explanation
Maintenance of adequate hydration is the single most important factor affecting athletic performance. While carbohydrate loading may be beneficial for some endurance athletes, the consumption of carbohydrates during exercise does not appear to be beneficial for athletes engaged in events that last less than 1 hour. In general, athletes consuming a balanced diet do not need electrolyte supplementation. Maughan RJ, Noakes TD: Fluid replacement and exercise stress: A brief review of studies on fluid replacement and some guidelines for the athlete. Sports Med 1991;12:16-31.
Question 45
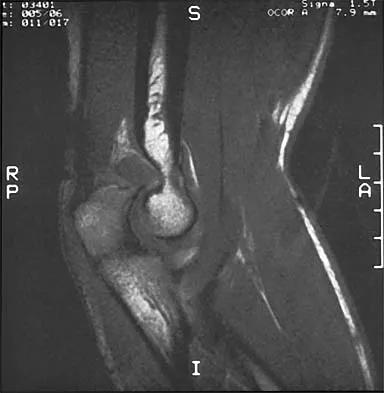
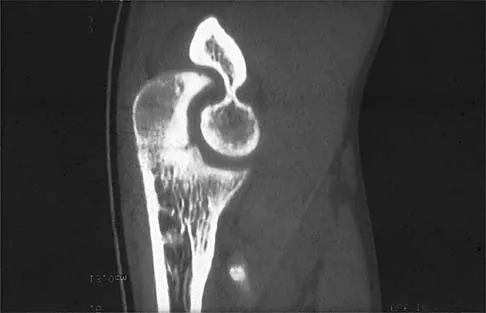
A right-handed 20-year-old college baseball pitcher has had a 6-month history of vague right elbow pain while pitching. Examination reveals full flexion of the elbow and a loss of only a few degrees of full extension. The elbow is stable, but palpation reveals tenderness over the olecranon. Plain radiographs are inconclusive. MRI and CT scans are shown in Figures 20a and 20b. Management should consist of
Explanation
The patient has a stress fracture of the olecranon that occurs with repetitive throwing motions. If the fracture is not displaced, the initial treatment of choice is rest and rehabilitation to maintain elbow motion, followed by aggressive strengthening at 6 to 8 weeks. A light throwing program generally can begin at 8 to 12 weeks. Complete recovery may require 3 to 6 months. If the fracture is displaced or if nonsurgical management fails, surgery is indicated for internal fixation of the stress fracture. Azar FM, Wilk KE: Nonoperative treatment of the elbow in throwers. Oper Tech Sports Med 1996;4:91-99.
Question 46
What is the most common associated pathology in patients who have suprascapular nerve entrapment secondary to ganglion cysts?
Explanation
It is well known that suprascapular nerve entrapment can be secondary to many entities, and its association with ganglion cysts and SLAP lesions has been well documented. Because of a superior labral tear, synovial fluid will leak out of the joint underneath the labrum, causing the cyst and secondary compression of the nerve. Fehrman DA, Orwin JF, Jennings RM: Suprascapular nerve entrapment by ganglion cysts: A report of six cases with arthroscopic findings and review of the literature. Arthroscopy 1995;11:727-734. Iannotti JP, Ramesey ML: Arthroscopic decompression of a ganglion cyst causing suprascapular nerve compression. Arthroscopy 1996;12:739-745.
Question 47
A 27-year-old runner training for his first marathon reports lateral knee pain after an unusually long training run. He states that the most significant pain occurs while running downhill. Examination of the patient while he is laying on the unaffected side reveals increased pain when manual pressure is applied to the lateral femoral epicondylar area during knee range of motion of 30 degrees to 45 degrees. What is the most likely diagnosis?
Explanation
Iliotibial band friction syndrome is one of the most common causes of lateral knee pain in runners. It is caused by increased friction between the iliotibial band and the lateral femoral condyle because of increased tension on the lateral structures. It may be caused by a prominence of the lateral epicondyle or a malalignment of the lower extremity in the runner, including genu varum, tibia vara, heel varus and forefoot supination, or compensating pronation. These structural characteristics can couple with relative muscle imbalance and lead to an altered running gait, enhancing friction between the lateral femoral condyle and the iliotibial band. Management is usually nonsurgical, including stretching of the iliotibial band and strengthening of the hip abductor muscles, with occasional use of cortisone injections or iontophoresis. Noble CA: The treatment of iliotibial band friction syndrome. Br J Sports Med 1979;13:51-54. James SL: Running injuries to the knee. J Am Acad Orthop Surg 1995;3:309-318.
Question 48
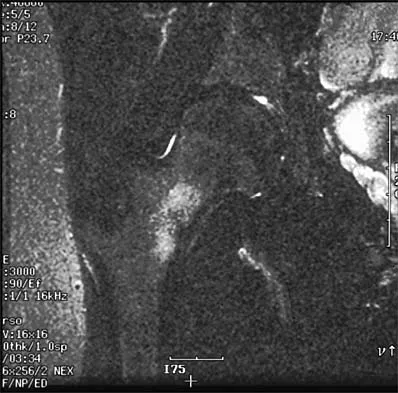
A 30-year-old woman who runs approximately 30 miles a week has had right hip and groin pain for the past 3 weeks. Examination reveals an antalgic gait, limited motion of the right hip, and pain, especially with internal and external rotation. Plain radiographs are normal, and an MRI scan is shown in Figure 21. Management should consist of
Explanation
A stress fracture of the hip is a relatively common problem in endurance sports. These fractures are classified as compression-side, tension-side, and displaced femoral neck fractures. The MRI scan shows a compression-side stress fracture. Compression-side fractures usually occur in the inferior or calcar area of the proximal femur, and non-weight-bearing crutch ambulation for 6 to 7 weeks will most likely result in healing. Once the patient is walking without pain or a limp, activities can be slowly increased. Because tension-side fractures have a high risk of displacement, treatment should consist of immediate internal fixation. Griffin LY (ed): Orthopaedic Knowledge Update: Sports Medicine. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1994, pp 239-253.
Question 49
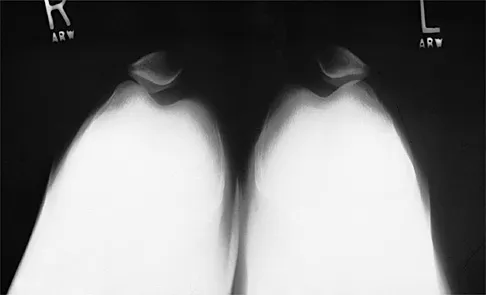
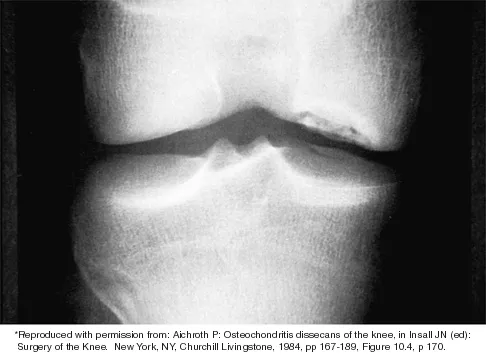
Which of the following primary prognostic factors best predicts the outcome of the knee lesion shown in Figure 22?
Explanation
The patient has osteochondritis dissecans. While location, size, and knee stability are all relevant to the overall prognosis, studies have shown that younger patients with open growth plates have a better prognosis of healing when compared with patients who have closed growth plates. The degree of pain is also relevant to treatment, but it is subjective rather than objective and is not as reliable of a prognostic indicator as age. Stanitski CL: Osteochondritis dissecans of the knee, in Stanitski CL, DeLee JC, Drez D Jr (eds): Pediatric and Adolescent Sports Medicine. Philadelphia, PA, WB Saunders, 1994, vol 3, pp 387-405. Cahill B: Treatment of juvenile osteochondritis dissecans and osteochondritis dissecans of the knee. Clin Sports Med 1985;4:367-384.
Question 50
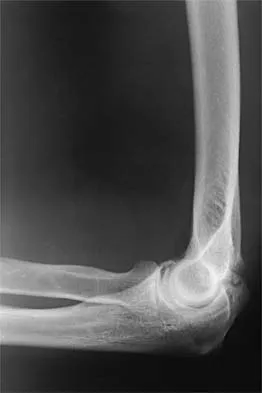
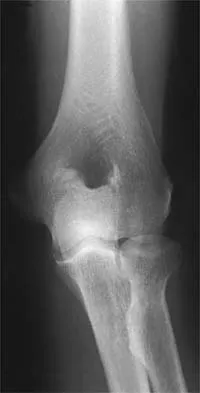
Figures 23a and 23b show the AP and lateral radiographs of the elbow of a 30-year-old professional pitcher. The pathology shown in these studies is most consistent with which of the following conditions?
Explanation
The radiographs show the osteophytic build-up of the posteromedial corner of the elbow that occurs with valgus extension overload in the pitching elbow. This is the result of excessive valgus forces during the acceleration and deceleration phases of throwing. These forces, coupled with medial elbow stresses, cause a wedging of the olecranon into the medial wall of the olecranon fossa. Valgus instability of the elbow may further stimulate osteophyte formation. Repetitive impact of a spur within the olecranon fossa may cause fragmentation and eventual formation of loose bodies. Azar FM, Wilk KE: Nonoperative treatment of the elbow in throwers. Oper Tech Sports Med 1996;4:91-99. Field LD, Savoie FJ: Common elbow injuries in sport. Sports Med 1988;26:193-205.
